Allied health research suggests that workforce development in rural Australia occurs in an ad hoc fashion, often without sufficient planning to meet the needs of the local communities1. Rural and remote communities are typically underserviced by allied health professionals and the discipline of dietetics is no exception. The dietetic workforce in Australia is unevenly spread across the country, with 32% of the rural population being serviced by 24% of the workforce2. In the geographical area under investigation, a survey of allied health staff in 2006 found that the average number of dietitians per 100 000 population was 8.4, slightly better than the average for all regional areas in Australia of 7.7 per 100 0003, but lower than the national average of 13 dietitians per 100 0004. It has been reported that some rural areas are better staffed than others and that there is an uneven growth across the country2. Dietetic services in rural areas of the state New South Wales (NSW) are typically based in the public sector, with limited private practice services available5.
Recruitment and retention issues for dietitians in rural areas have been reported elsewhere by the present authors6. Recruitment to rural areas has improved with an increase in the number of pre-entry dietetic programs since 1991; however, retention of staff remains an issue2. The development of dietetic positions in rural areas has not previously been investigated. The growth of allied health services in rural Australia has occurred due to five main categories of funding: (i) specific Commonwealth or State funding; (ii) allocations based on population ratios; (iii) qualitative demand from stakeholders; (iv) utilisation data; and (v) needs-based methods using population and health outcomes1. The key factors that lead to increased funding and the development of dietetic positions in rural areas are unknown. The purpose of this study was to describe dietetic services in selected rural areas and to determine the barriers to and drivers for the development of rural dietetic staffing.
Site selection
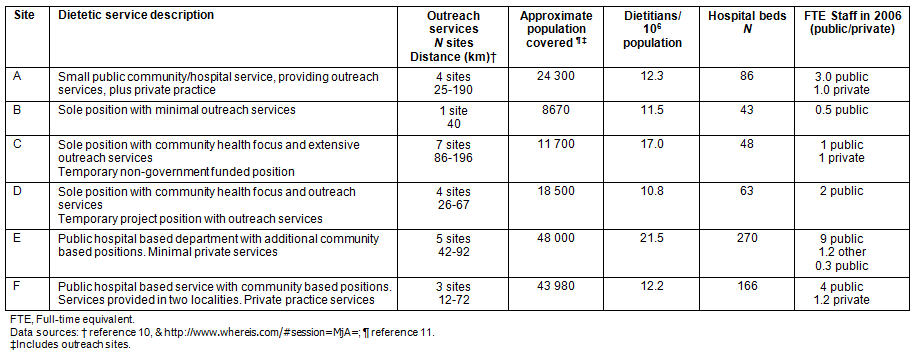
Six rural sites from the Hunter New England Health (NHEH) service area of NSW were selected for a case study examination of the development of dietetic positions in the local area over a 15 year period (1991-2006). The six sites were chosen because they represented different models of dietetic service delivery within the same geographical and health service region. Models of dietetic service delivery included a mix of public hospital and community based services with variable private services, as described (Table 1).
Ethics approval
Ethics approval for the study was granted by the Hunter New England Human Research Ethics Committee and the University of Newcastle Human Research Ethics Committee. Individual sites have not been identified to protect the anonymity of participants.
Methodology
A sequential explanatory mixed methods approach was used with quantitative (document searches) and qualitative (semi-structured individual interviews) data collection7. Data triangulation was conducted to achieve a more complete analysis and to determine the convergence and divergence of the data8. This process involves the examination of data from several sources to build justification for the themes7. Multiple sources of information were utilised, including written records where available, and information compared across the interview transcripts to obtain valid data.
Part A: Quantitative data collection and analysis
Document searches were conducted on de-identified human resource records at each of the six sites, to collect data on demographic data, job descriptions, start and end dates of employment, salary classifications, job titles, location of employment and periods of position vacancies. Quantitative human resource data were tabulated, and counts and proportions were used to summarise developments over a 15 year period.
Part B: Qualitative data collection and analysis
Individual interviews were conducted with key informants from the public and private sector, including dietitians, dietetic managers, health service managers and other people of influence (such as project managers and team leaders). Semi-structured interview protocols were developed, after a review of the literature on the rural dietetics workforce. Questions centred on the development of positions because no previous research has investigated the development of the dietetic workforce in rural areas. Participants were recruited using purposive, non-probability sampling. Professionals identified as being currently employed in the six sites were invited to participate. The snowballing recruitment technique was then used to further identify potential participants.
Interviews were conducted over an 11 month period by the first author until a saturation point was achieved with the emerging themes, with participants recruited from all sites and levels of management. Informed consent to obtain de-identified documents and to conduct individual interviews was obtained from participants. The taped interviews were transcribed by a research assistant and the accuracy was checked and corrected against the original recording by the interviewer. Participants were invited to review their transcripts.
Qualitative data from the document searches and interviews were collated and entered into the NVivo 7 program v.8 (www.qsrinternational.com). Themes were coded into common categories, using a constant comparison inductive approach9. This approach involves inspecting and comparing data that arises in a single case and comparing with other cases9. These themes were independently validated by the second author. Extracts from interview transcripts were edited, using standard transcription conventions where needed, to ensure anonymity and clarity. Each quote was labelled according to position, employment status, interview ID number and site of employment. For example, the following label (dietitian, currently employed, 4C) denotes a quote from participant four who is currently employed in Site C.
Participants
Forty key informants agreed to participate in the in-depth semi-structured interview. Participants included 28 dietitians (past and present), three dietetics managers and nine managers. The majority of participants was female (87.5%) and three of the five participating male subjects were in dietetic positions. A summary of the dietetic service and staffing details is provided for each site (Table 1).
Table 1: Dietetic service and staffing levels at six rural sites10,11
Quantitative workforce data
The dietetic workforce across the six sites, increased by a net of 22.6 full-time equivalent (FTE) positions, a 5.6-fold increase over the 15 years. Increases in dietetic staffing for the six sites separated into 5 year periods for the study period (1991-2006) are shown (Fig1). In the cases of sites D, E and F, the largest increase in dietetic positions occurred in the last 5 years.
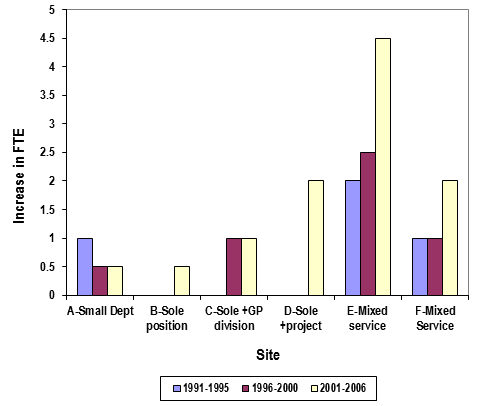
Figure 1: Increase in dietetic staffing across the six sites for health service and Division of GP services.
Qualitative thematic analysis
The main themes arising from the interviews in relation to the development of positions and the barriers to and drivers for a best practice dietetic service are reported (Table 2). Funding for additional dietetic positions has typically been achieved in the study sites through gradual increases, opportunistic situations or ad hoc funding, or through strategic lobbying by champions. Key themes will be discussed and supported by quotes from the participants.
Table 2: Summary of themes for the development of positions

General lack of funds and competing priorities for funding: A general lack of public funds was identified as the main barrier to attracting additional funds or reallocating funds to dietetic staffing in rural areas. The scarcity of additional funding and the limited access to this funding at a local health service level was reported in a number of sites.
Well I think funding has been the largest barrier...the funding base is at a marginal level and so the full cost of running those services has been greater than the funding provided. I think the other barrier is probably more around the inability to shift resources internally within an area of service with great ease. (Manager, currently employed, 40A-F)
The lack of funding within the local health service cluster was identified as a barrier to the development of any further dietetic positions despite identified needs for the service.
...the reason that they couldn't employ any more dietitians was because there was no money, the cluster had no money and they were in the red and that there is no way that they could create a permanent position. (Dietitian, past, 23D)
Managers often realised and agreed there was a need for additional dietetic services; however, they were faced with the reality of there being no additional funding available and no other services that could be reduced.
There haven't been a lot of specific opportunities for dietetic services to push their case over the last 5 to 10 years...dietetic services hasn't necessarily been one of the sub-groups that have been able to lobby and advocate for money... (Manager, currently employed, 38F)
Competing priorities for the funding dollar was a common reason given for extra dietetic positions not being funded. Dietetics was seen by managers as not being a 'needy area' and not being a high enough priority to attract its own funding.
... if you go to take money from somewhere you've actually got to take it from someone else ... so you have to say well what service are we going to decrease to increase your service and really the answer is, none, because we can't afford to do that. (Manager, currently employed, 24A)
The long-term nature of dietetic interventions and patient outcomes were perceived to be an issue, especially given the focus on acute hospital services for much of the enhancement funding.
A lot of our outcomes are long-term, so trying to justify that to management is quite difficult at times. (Dietitian manager, currently employed, 6E).
Dietetics, along with other allied health professions, was seen as an additional or optional service, rather than something that was essential to acute hospital care.
The biggest problem is often allied health is seen as a little bit of a luxury and it is much easier to justify nursing or medical extra positions. (Dietitian manager, currently employed, 6E)
Some dietetic services were unable to attract additional funding for an increase in dietetic staffing despite the expansion of other health services.
We were never enhanced to go along with the expansion of the hospital services. We just stayed the same ... and it was always seen as ... they were never going to enhance the hours for the position. (Dietitian, past, 9A)
Current health issues that were attracting health funding (such as obesity) were seen to provide potential future funding for dietetics.
Competing priorities is one of the biggest things and getting dietetics high enough on the agenda to rate allocation of funding in it's own right. Maybe with obesity being identified as a major health issue, that will start to turn around a little bit. (Manager, currently employed, 38F)
Champions for strategic increases in funding: Sites where a 'champion' existed were generally successful in obtaining funding for increased positions through lobbying and repeated submissions for additional funding. Champions included dietitian managers and non-dietitians. Champions who could obtain the support of local management were able to make progress with submissions for funding at an area health service level.
Without management on side, you don't get anywhere. You can agitate all you like and it doesn't get you anywhere so really the first job of the dietitians is to then convince management ... that the need is there and show that demand and go from there in terms of business cases and funding proposals... (Dietetics manager, currently employed, 6E)
Health priorities at a local level needed local management support to be considered at area health service level for potential funding.
Number one it has got to be prioritised within the cluster, then it goes to the Area where it is then prioritised, so it just wasn't prioritised at that time ... it was obvious that there was no service provision and that it was a strong submission, so there was nothing to argue against it, it was very obvious that we needed a dietitian. (Manager, past, 31D)
Persistence and continuity were key factors in obtaining funding for additional positions. 'I had to do a lot of fighting for every position that we got...' (dietitian manager, past, 17E). Champions who remained employed in one area for an extended period of time were best placed to be aware of the needs of the community, the management structure and processes as well as having close working relationships with management.
[I] went to all levels of management that I possibly could, I eventually got the Executive Officer of the hospital onside, after lobbying management for 6 months, we got a 0.5 position created. (Dietitian, past, 9A)
Developing good working relationships with managers at various levels and having a high profile was an advantage in the lobbying process for development of positions.
...being around for a long time is actually quite an advantage, having been here with a lot of the managers for a long time has actually helped me a lot ... they know me as a clinician as well and so they know that I am actually quite passionate about the service and that I have the clients' best interests at heart. I am not just trying to empire build and build a bigger service, so I guess that's an advantage... (Dietitian manager, currently employed, 6E)
Being able to demonstrate a demand for services was a key factor in submissions made to management in order to justify the need for additional positions.
...it was the demand for the services that you needed to establish before you got those positions and talking to the right people and getting other people to ask for your services... (Dietitian, past, 7E)
Crisis situations in terms of service demands were a useful time to lobby management. A crisis situation provided impetus for change, even when there had been previous difficulties in obtaining funds.
Site B was reaching crisis point so something really, really had to be done which was actually a prime time to go to senior management and argue that case with them. (Dietitian manager, currently employed, 6E)
In some cases a crisis situation provided an opportunity to approach management for extra funding:
I think when it reaches crisis and services are cut and then they will respond so it's almost like, rather than proactive it's a reactive measure. (Dietitian, past, 16A).
One way champions were able to obtain funding was to ensure that the users of dietetic services were paying for the services they were receiving. This required a knowledge of the funding sources, health service management roles and lobbying skills. New graduates in rural positions are not always well equipped to deal with these management issues. In sites with a high turnover of new graduates and no long-term experienced staff, little was being done to progress the situation or change funding sources.
It was a matter of looking at the funding and where it was all coming from ... and who pays ... we got them to ... agree that they would pay 0.5 because in their budget there was a little bit of leeway and they were meant to be providing some allied health services and of course they weren't paying for it (Dietitian manager, currently employed, 6E, speaking in area advisor role)
Ad hoc and opportunistic funding: Funding for positions was often obtained through opportunistic situations that arose or ad hoc funding arrangements. The availability of an unemployed or under-employed dietitian provided an incentive to try to create a position when funding was accessible. Typically these, predominantly female dietitians, moved to the area due to their partner's work or were new graduates returning to their local home town looking for work after graduation.
The position was roughly created for me I think as an opportunistic role. I had moved back to my country town and home and there wasn't a position ... the dietitian at Community Health ... applied for a grant to do project work ... so I obviously was going to apply for the job. (Dietitian, currently employed, 28C)
At a number of sites, dietitians reported using the funding for long-term, unfilled allied health positions to create new dietetic positions.
I think the funding came from...a little bit of surplus from an empty position [other allied health position] that couldn't be filled. (Dietitian, currently employed, 5E).
Opportunities were also created by applying for project funding that led to funding for a full-time position.
Initially it was a grant we won... to do an Aboriginal health project and that was...incorporated into my budget as one of my FTEs and I was given funding from [health service sector], as recurrent funding in my budget to actually continue that position. (Dietitian manager, currently employed, 6E)
Deliberately denying a service due to a lack of staffing: Dietetic staffing was sometimes reduced due to dietitians withdrawing established but unfunded services to particular parts of the health service. Increasing demands for dietetic services was placing pressure of dietitians to reduce or re-orientate their services. Dietitians responded to unreasonable workloads by deliberately reducing some patient services. This was, in part, to alert management to the pressure they were facing in providing services to an ever-increasing client base.
...we withdrew services from the Diabetes Centre and that really got the attention of the CEO ... it was an outpatient service ... the job that I had been employed to do was an inpatient based role, so inpatients were the priority. (Dietitian, past, 7E)
This strategy was successful in raising awareness among management and allowed for a review of the staffing situation, particularly after complaints from other health professionals and/or clients.
I recall that the hospital dietitian did cut back some services to show how great the need was ... I think this is partly where the enhancement funding came from for ... a diabetes dietitian. (Dietitian, past, 25F)
Discussion
The findings from this study have important implications for the development of dietetic staffing in rural areas. The positions in these sites developed in an ad hoc and opportunistic way with some areas developing higher staffing ratios than others. Increases were not based on population size or other possible benchmarks such as hospital bed numbers, rates of chronic disease or best practice guidelines for individual conditions. The average dietetic staffing level across the six sites was 12.3 per 100 000, which is more than the 8.4 per 100 000 found in an allied health study3 conducted in the same geographical area in 2005. This difference between the studies is likely to be due to the poor response rate (50%) of the 2005 study compared with 71% for the present study.
Sites that were successful in consistently increasing staffing sought additional funding through several sources. Competing priorities and a general lack of funds, were the major barriers to increased staffing, even when service demand was well established. The attitude of managers to the services provided by dietitians and their perception of the importance of the dietitian's role may influence their decision to fund additional positions. Developing a high profile with local management was a key factor that assisted in negotiations for additional funding. Further research is required to determine if these factors are similar for other rural areas and health service settings.
In a recent systematic review of the literature on primary health care services in rural and remote areas by Humphreys et al, adequate funding and champions to support these services was identified as the key to ensuring sustainable rural health services12. Despite the need for preventative and primary healthcare services to address the chronic disease burden experienced in rural Australia13, funding for non-acute services is limited and generally appears to have a lower priority than acute and emergency services. Dietetic services are disadvantaged in this funding system by being perceived as non-acute .
In order to ensure more equitable access to dietetic services in rural Australia, a range of strategies are required. Dietitians are competing with other health professions for limited funds and those who are proactive and committed to pursuing funds are likely to be more successful in establishing positions in a system where funding is often ad hoc. The professional association, the Dietitians Association of Australia, could take a lead role in providing training and advice for rural dietitians on successful approaches and strategies for increasing dietetic resources and services in rural areas. Given that a lack of funds and competing priorities inhibited the growth of rural dietetic positions, it is important that submissions for additional staff funding are timely and linked to health service priorities, draw on evidence and are underpinned by data wherever possible. Lobbying by the profession at state and federal levels may be more effective in the long term, given the limited capacity of funding at the local level.
Recent changes to the structure and function of local health services through the development of Local Health Districts and Medicare Locals will have implications for the future development of the rural dietetics workforce. Current health reforms14 may support the future development of the dietetic workforce; however, workforce planning is dependent on accurate workforce data and this has been lacking2. Poor staff retention levels have implications for future workforce planning and this continues to be an issue for the rural dietetics workforce6. Further growth of the private sector has been identified as a way to address gaps in the public sector dietetics workforce5. The role of Medicare Locals in the coordination of primary health care delivery to address local health needs and service gaps15 may assist in the strengthening of private dietetic services in rural areas.
A potential limitation of this study is that the information provided by managers may have been influenced by the fact that the interviewer works as a dietitian in the study area; however, the interviewer is not employed in the public health system and was not previously known to the health service managers interviewed for this study. To overcome this potential limitation, multiple sources of information were utilised, including written records (where available), and information was compared across the interview transcripts to obtain valid data. The generalisability of the findings may be limited due to different funding arrangements in other states and territories of Australia. It is noted that the effectiveness of the current dietetics workforce was not assessed in this study and that innovations to the existing workforce may achieve improvements in service delivery without changes in staffing levels.
This research demonstrates an inconsistent approach to the development of dietetic positions in rural areas of Australia. In underserviced rural areas, a systematic, planned approach to the development of dietetic positions is needed. The development of dietetic positions in rural areas is limited by a general lack of funds and competing priorities. This is particularly as issue in the primary healthcare setting when acute services take priority for funding. Champions for the development of positions can be effective in increasing positions, particularly when they have management support.
Acknowledgements
The authors thank the dietitians and mangers who participated in this research. This research was supported by a Primary Health Care Research Education and Development Small Grant in Aid provided through the University Department of Rural Health Northern NSW, The University of Newcastle.
References
1. Struber J. Recruiting and retaining allied health professionals in rural Australia: why is it so difficult? Internet Journal of Allied Health Sciences and Practice 2(2): 1-13. (Online) 2004. Available: http://ijahsp.nova.edu/articles/Vol2num2/struber_rural.htm (Accessed 10 March 2011).
2. Brown LJ, Capra S, Williams LT. Profile of the Australian dietetic workforce 1991-2005. Nutrition and Dietetics 2006; 63(3): 166-178.
3. Smith T, Cooper R, Brown L, Hemmings R, Greaves J. Profile of the rural allied health workforce in Northern New South Wales and comparison with previous studies. Australian Journal of Rural Health 2008; 16(3): 156-163.
4. Australian Institute of Health and Welfare. Health and community services labour force. National health labour force series 42, cat no. HWL 43. Canberra, ACT: Australian Government Publishing Service, 2006.
5. Brown L, Mitchell L, Williams L, Macdonald-Wicks L, Capra S. Private practice in rural areas - an untapped opportunity for dietitians. Australian Journal of Rural Health 2011; 19(4): 191-196.
6. Brown L, Williams L, Capra S. Going rural but not staying long: recruitment and retention issues for the rural dietetic workforce in Australia. Nutrition and Dietetics 2010; 67(4): 294-302.
7. Creswell JW. Research design: qualitative, quantitative and mixed methods approaches, 3rd edn. Thousand Oaks, CA: Sage, 2009.
8. Creswell JW, Plano Clark V. Designing and conducting mixed methods research. Thousand Oaks, CA: Sage, 2007.
9. Silverman D. Interpreting qualitative data, 3rd edn. Thousand Oaks, CA: Sage, 2006.
10. New South Wales Health. Services and facilities. Sydney, NSW: NSW Health, 2008. Available: http://www.hnehealth.nsw.gov.au/services_and_facilities (Accessed 26 March 2011).
11. Australian Bureau of Statistics. 2006 Census data by location. Canberra, ACT: AusStats, 2008. Available: http://www.censusdata.abs.gov.au/ABSNavigation/prenav/PopularAreas?&collection=Census&period=2006&&navmapdisplayed=true&javascript=true&textversion=false.{Verified (Accessed 12 March 2011).
12. Humphreys J, Wakerman J, Wells R, Kuipers P, Jones J, Entwistle P. Beyond workforce: a systematic solution for health service provision in small rural and remote communities. Medical Journal of Australia 2008; 188(8): S77-S80.
13. Hunter New England Health. Area Healthcare Services Plan. New Lambton, NSW: Hunter New England Health, 2006.
14. Health Workforce Australia. National Health Workforce Innovation and Reform Strategic Framework for Action 2011-2015. (Online) 2011. Available: https://www.hwa.gov.au/sites/uploads/hwa-wir-strategic-framework-for-action-201110.pdf (Accessed 9 December 2011).
15. National Rural Health Alliance. Rural Issues Paper on Medicare Locals. (Online) 2010. Available: http://nrha.ruralhealth.org.au/cms/uploads/factsheets/Fact-Sheet-29-medicare-locals.pdf (Accessed 9 December 2011).



