Although Australia is recognised as one of the safest countries in which to give birth or to be born1 with a high-quality healthcare system rating well internationally2, maternity care in Australia is not meeting the needs of all Australian women, especially those in rural and remote areas3-5. In particular, rural and remote families experience higher rates of maternal deaths6, rural women have significantly higher rates of neonatal deaths and remote women have higher rates of foetal deaths7. Moreover, maternal mortality rates for Indigenous women are more than two and a half times as high as for other women8, and Indigenous women have a higher rate of foetal death and neonatal death9.
The Rural Doctors Association of Australia reported that rural communities across Australia have experienced on-going loss of maternity units for more than a decade, forcing thousands of women to travel to distant centres to give birth10. There are three main interrelated reasons for losing these units. The first is shortages in healthcare workforce11 which is the major factor that has led to the closure of 50% of rural maternity units across Australia since 199510. In Australia, workforce shortages of maternity and healthcare professionals is worsening5. The second reason is safety and quality considerations10. Difficulties in recruiting and retaining obstetric specialists in rural areas undermine anaesthesia and caesarean delivery capabilities and raise concerns on the safety and quality of birthing services11. Finally, cost considerations affect the decision to close small maternity units in rural areas10,12 when health authorities and hospitals anticipate savings from shutting down such services.
Losing obstetric services in rural areas has many impacts on rural communities. Research has shown negative effects on the wellbeing of mothers and their babies who have to leave their community and travel to a larger centre to obtain obstetric services13-15. Moreover, women who have to travel great distances to access maternity services encounter stress, financial burdens, social disruption and lack of continuity of care4,16. In addition, the loss of maternity services affects the sustainability of rural communities; for as Klein et al recognised, maternity and newborn care are the lynchpins for sustainable communities medically, socially and economically12.
The Rural Doctors Association of Australia noted that rural communities have been put under increasing pressure as more and more rural maternity units have been closed by the state governments and this situation shows no sign of improvement17. To deal with these dilemmas, small rural birthing units without caesarean delivery capabilities have been implemented in a few rural communities across Tasmania. In these communities, GP obstetricians and midwives look after low-risk women from the antennal to postnatal period. Women who are classified high risk still need to travel to major hospitals for antenatal checks and deliveries.
While statistical data and other quantitative studies on the outcomes of small rural hospitals without obstetric services can provide evidence on the safety of this model of care, other factors should be also considered when planning for future health services. For this reason, this study considers the views of maternity healthcare professionals on this model of care, with the aim of providing insightful recommendations to policy-makers and the Tasmanian State Government on the future implementation of this model of care in rural settings.
This study is part of a larger study which focused on maternity services for rural women and elicited the views of women through surveys and interviews and of maternity health professionals through interviews18. This article reports the views of health professionals on the model of small maternity units without caesarean section capabilities. A qualitative approach using semi-structured interviews was employed to investigate the experience of maternity health professionals in Tasmania, Australia. The study used a grounded theory approach for its data analysis. According to Glaser and Strauss, grounded theory is a qualitative approach designed to facilitate the systematic analysis of data in order to generate new theories, explanations and interpretations19. Data are coded and categorised as the researcher begins to see patterns emerge. Theory is developed throughout the research process as data interpretation takes place and comparison of that interpretation is made with new data that are collected20.
All transcribed material was analysed sentence by sentence and coded for the participant's meanings. Initial open coding of the data used differing codes, which were then organised into categories. The data were then repeatedly re-analysed to reassess the content and confirm the findings. QSR-NVivo v9.0 (www.qsrinternational.com) software was used in the analysis to organise transcripts and codes. Quotations were referenced according to the participant's profession and an assigned number.
Research questions
Three research questions were formulated to achieve the aim of the study:
- What are the difficulties that women in rural areas face when local hospitals do not provide maternal health services from the views of maternity health professionals?
- What are rural women's expectations of maternity care from the views of maternity health professionals?
- What are the views of health professionals on small maternity units without caesarean delivery capabilities in rural settings?
Sampling and data collection
Participants were recruited using purposive sampling strategies including recruitment through third parties. Between February and May 2011, key managers of hospitals and health centres across Tasmania were contacted to assist in participant recruitment.
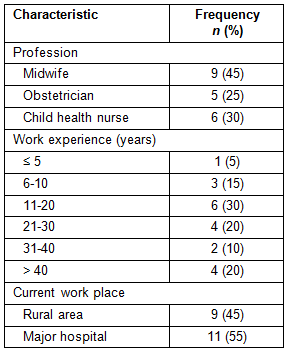
The selection criteria for the interviews were that the participants are maternity healthcare providers and currently employed by the health system in Australia or Tasmania. Approximately 28 health professionals who met the criteria were invited to participate in the study and 20 accepted. Key characteristics of the participants are provided (Table 1). The participants were asked to complete an anonymous questionnaire about their background prior to commencement of the interviews. The interviews took 20-30 min to complete. All the interviews were conducted in rooms in the hospitals or in health centres and tape-recorded. All participants provided written consent to participate and for the interviews to be audio-recorded, prior to participation.
Table 1: Key characteristics of the participants
Data analysis
Audio-recorded interviews were transcribed verbatim in Microsoft Word. Transcripts were then checked against interview playback for errors or omissions. After quality assurance, the transcripts were imported into QSR-Nvivo v9 for analysis. The transcripts were systematically and manually analysed in QSR-Nvivo using open, axial and selective coding methods until theoretical saturation of the data was achieved.
Ethics approval
Ethics approval for the study was granted by the Tasmanian Social Sciences Human Research Ethics Network (#H10967).
Three main categories emerged:
- Women's difficulties in rural areas (with 4 subcategories: access issues, disruption, anxiety and travel related issues).
- Women's expectation of maternity care.
- Maternity units without caesarean delivery capabilities.
Women's difficulties in rural areas
Access issues: When maternity services are not available in the local community, women have to travel to access the required services. Thus, in order to avoid travelling, women are less likely to attend all their appointments. In addition, they are less likely to travel to see health professionals even if they have concerns about their pregnancy. According to the health professionals interviewed, these are regarded as inadequate care for women.
Every time they have an antenatal visit, it is a huge event ...so it probably means that they are less likely to go and see someone for minor concerns. They would wait until they are really unwell or really concerned before they make the effort to come. Travelling puts a lot of strains on the women. Thus, they are less likely to attend all of their appointments and to come in if they have got concerns. (Obstetrician 1)
Furthermore, the results from the interviews with health professionals reveal that when the local hospital does not provide maternal health services, women have to rely on their GPs. However, with the current workload of GPs in rural areas, they may not be available to provide care for the pregnant women. As a result, women may not get proper antenatal care in their local communities.
They rely on their GPs. We all know that the GP services are stretched to their maximum at the moment; therefore I suspect that there are a number of women out there do not get adequate care antenatally and simply because they can't get into a doctor or there is not a doctor available. Consequently, they are disadvantaged because of the lack of services in the rural areas. (Midwife 4)
Disruption: When maternity services are not available for women in rural areas, health professionals could see that women may face many difficulties including disruption from their support network and their home environment.
If they have got other families that the first big hurdle is that they have to leave home and leave their support network and leave maybe their other children, the same access problem to good quality care if they have to travel. The financial problems come into it again but probably mostly the disruption from their support network and their home environment. (Midwife 7)
Being separated from the support of locally based family and friends can be an issue for women if they are required to stay in the hospital for a length of time.
Given the often brief time spent in a maternity hospital these days, perhaps being separated from the support of locally based family and friends is not such an issue. However, it certainly would be if the woman is required to stay in the hospital either antenatally or postnatally for any length of time. (Child and Family health nurse 2)
Anxiety: Being away from their familiar environment and social network can cause stress and anxiety to women. Women from rural areas can find being away from home especially difficult. They often feel 'isolated' and 'lonely' as they are separated from their partners, other children and families while remaining in hospital following childbirth.
Women can feel very isolated when there is a need to be admitted to a large medical institution and it means being separated from her family. This can cause her high levels of anxiety particularly if she is concerned for other children at home. (Midwife 2)
Travel related issues: When health services for expecting mothers are absent locally, women often have to travel to larger hospitals to access care. This creates many issues for women and families including time, expense and transport facilities.
They need to plan for all unexpected outcomes, burden of travel, more with further to go - more time and more expense and need transport facilities. (Child and family health nurse 1)
The travel related issues are not only about the transport and accommodation expenses but also the risk of giving birth en route due to the distance between the local hospital and a major hospital.
There is a risk of childbirth because of the long trip to the closest midwifery hospital to [rural town name]. (Midwife 3)
In addition, there is also a risk that women might choose to give birth at home or in the local hospital which does not have standard maternity services because they want to stay in their local community.
They also tend to opt for other options. They are more inclined to give birth to a baby at home or in a local hospital which does not have specific maternity services because they want to be around with their family. (Obstetrician1)
Women's expectation of maternity care
This section presents the health professionals' perspectives of women's expectation of maternity care. Health professionals were asked about their understanding of women's expectation of maternity services especially women in rural and remote areas. Most agreed that women, regardless of where they live in urban or rural areas, expect to have a safe environment for themselves and their babies, access to services and quality services.
Safety/access to services: According to the health professionals interviewed, when it comes to maternal health care, women have great concern over the safety of themselves and their babies. Women want to be informed of their pregnancy and their babies. They expect to have readily accessible maternity services to be ensured of the safety of themselves and their babies.
They want to know about information about their pregnancy. The women want to know that their babies are normal. They expect that there will be someone at any time to pick up their problems and they expect readily accessible maternity services. (Obstetrician 1)
Safety is one of the most important things that women expect. Health professionals suggested that maternity services need to be flexible and available close to their homes particularly, so that they can remain close to their supported network.
All mothers expect the safety of themselves/their babies to be paramount. Maternity services need to be flexible, available close to their homes particularly so that they can remain close to other children/family members, which ensure that they feel supported and that those people can be involved as much as possible. (Midwife 3)
Another expectation health professionals often observed among rural women was being able to access to services. Certain services are only available in urban areas and are therefore difficult for rural and remote women to access.
One area of women's expectation that has not been met for a long time is in postnatal care. A lot of women are aware that we have an extended midwifery service but a lot of them find it difficult to access especially if they live in rural areas. (Obstetrician 5)
Antenatal education is often available in major hospitals but limited in many rural areas. Participants observed that women expect to have this service accessible in their communities.
I think women expect to be able to access maternity services... but things like antenatal classes, education type do not get done because those resources are limited in rural areas. (Midwife 4)
Quality services: The health professional participants observed that quality of care is another of women's expectations of maternity services, such as not being inconvenienced by cancelled or late appointments.
Most women have the same expectation that they are going to have good service. They don't want to be mucked around especially if they are from rural areas. It is easy for people who live in towns as they can come back later on sometimes. But it is certainly not the case for women in rural areas. (Midwife 5)
Another aspect of quality care that women expect is that they do not want to be kept waiting for long for their appointment.
They expect that 'my appointment is at 3 o'clock and therefore I get in it at 3 o'clock'... In here we actually give them really good care, just as they expect their appointment at 3 o'clock and they don't want to wait. (Midwife 4)
From the health professionals' point of view, another expectation women often have is that they will be listened to by health professionals and involved in their own care. A breakdown in communication between the women and their caregivers was noted and it was believed that this may have been due to the closure of the local services to which postnatal women were once transferred to rest for a few days after delivery.
Women expect to be active participants in their birthing experience and expect to have their wishes considered. The main criticism I hear from women about maternity services is where there has been a breakdown in communication. There was probably a higher expectation of being able to get more of a rest when postnatal women returned to [name of the local hospital] for a few days. However, this service ceased several years ago due to insufficient midwives available to be rostered on for all shifts. (Child and Family health nurse 2)
Maternity units without caesarean delivery capabilities
In view of current concerns in rural areas across Australia in general and Tasmania in particular (ie shortage of health professionals and cost considerations), maternity units without caesarean section services could be regarded as a model of care for low-risk women in rural areas. However, the data analysis from the health professionals' interviews suggested differing opinions on this mode of intrapartum care.
Ensuring the safety: Health professionals in the study only supported this model of care provided those units have appropriately trained medical staff and a good back-up system to deal with unexpected emergency situations.
Yes, absolutely, providing that they have got appropriately trained staff and good back up and emergency care or ambulance care, good protocol for transferring people out of there if things are not looking so good. (Midwife 7)
'Town A' (an rural town mentioned by many health professionals in this study) is 63 km from a major hospital referred to by many health professionals as providing maternity services without caesarean delivery capabilities. According to the participants, midwives are able to work alongside with GPs to provide care for low-risk women in rural areas without caesarean delivery support. However, they could only see this occurring in very few places in Tasmania.
The GPs look after women and do normal deliveries. They only see low-risk women; anything that is high risk comes in here (the major hospital). But as long as the GPs are willing to do it and we are trained to do it. Midwives are always able to deliver a normal low-risk woman. They closed everything [else] down. So people do not have their option. (Midwife 4)
The health professional who worked at the local hospital in Town A explained how the small maternity unit in her area worked without caesarean delivery support.
Any complications or lack of progress in labour is identified early to allow for the woman to be transported to [the major hospital] where more specialised care is available should this be required. (Midwife 3)
Sustainability concern: The health professionals who support this model of care were aware of the current health workforce shortages and often expressed concern about sustainability. They had concerns about staffing, equipment and how to run a maternity unit with only midwives and GPs and how to make sure it meets the required standard.
Possibly, but I am not sure how sustainable this is. For example, maintaining rosters with midwives on each shift. What happens with short notice sick leave, and can annual leave be covered? How well will the midwives be supported with specific professional development opportunities? What access will these women have to obstetricians and paediatricians? How well will equipment be maintained? How will changes in practice be communicated and standards of care audited? Will the local GPs be the admitting doctor and if so, how will this sit with their professional indemnity? Many questions - and no doubt more if I think a little longer! (Child and Family Health Nurse 2)
Safety concern: Although there are some health professionals who support small maternity units without caesarean delivery capabilities, 13 of the 20 participants did not advocate it because of safety concerns. Even though they seemed to support this model of care, they still stressed that a low-risk woman does not mean 'no' risk.
I think so, as long as she has all the routine screens done so we know she is low-risk. However, it does not mean she does not have any risk. (Midwife 6)
Another practitioner saw a great potential for a small suitably staffed rural maternity unit but not without caesarean delivery capabilities. According to most of the participants, the need for a caesarean section can happen without warning and therefore a small unit should have the facilities and staff to cope in such a situation.
Women give birth in all sorts of places - a small suitably staffed rural maternity unit sounds great. I think every small rural maternity unit should have the facilities and staff to cope with a caesarean section, as the need for a section can happen without warning. (Midwife 2)
In order to ensure the safety of the mothers and babies, it was suggested that women should always give birth in a unit with obstetric services.
As I said, 80% of births could go very smoothly but there is always the unexpected. If a woman is going to give birth, there should always be a facility for caesarean section. (Obstetrician 2)
Another reason given by health professionals for not supporting small maternity units without caesarean section capabilities was the concern about the quality and safety of services. They cited frequent instances where women suffered adverse outcomes in such units.
Hospitals in areas such as [name of Tasmanian rural town] and [name of Tasmanian rural town] provide care but it's not sufficient and this can unfortunately lead to substandard care. We had a case several days ago when a woman came in after delivery, bleeding since 9 am and she came around 7 pm, and she was bleeding for 10 hours. I would say this is substandard care. And we see this once every few months, not once a year. So things like bleeding can be a problem for local hospitals probably due to lack of many deliveries and lack of proper training. (Obstetrician 3)
Discussion
What can these findings tell us about the difficulties of women when their local hospital does not provide birthing services from the maternity care providers' views? According to the interviewed health professionals, rural women face challenges in accessing services and in travel related issues, as well as experiencing disruption and stress. These findings are consistent with the larger study which interviewed and surveyed rural women18 suggesting that the absence of maternity care services causes financial burden to rural families and communities in the form of travel costs, accommodation, childcare costs, loss of income and other expenses. In addition, women often face social disruption because they are removed from their social network and separated from family members in order to give birth in an unfamiliar hospital. Moreover, women face the risk of giving birth before arriving at a major hospital18. This is supported by other studies that have interviewed and surveyed women4,16,21. These challenges cause stress, fear and anxiety4,16,21,22 to the women and their families. Most recent research has found that women living in communities without access to local maternity services are 7.4 times more likely to experience stress and anxiety compared with women in communities with local services22. These negative feelings have been linked with adverse outcomes for mothers and babies13-15. As mentioned, one reason for closing small rural maternity units is cost savings. Hospitals, health authorities and health departments assume that it will be cost-effective to shut down rural maternity units. However, the findings from the present study and the literature suggest that the closure of these services shifts costs and risk from the healthcare system to rural families and communities in the form of travel cost, accommodation, childcare cost, and stress, fear and anxiety.
In these rural contexts, the model of providing small maternity units without caesarean delivery capabilities in rural communities reduces the travel needs for the women and their families. Under this model of care, low-risk women can access services in their local communities for antenatal check-ups, labour and delivery services and postnatal checks. Consequently, the difficulties associated with travel such as extra costs, disruption, anxiety, stress and risk of labouring and birthing en route are be minimised. Moreover, this model of care is likely to meet women's expectation of quality of care due to the small size of the maternity units. In a small hospital with few incidents of births, women would be less likely to have to wait for the services and more likely to have continuity of care. However, with the current availability of human resources in rural communities in Tasmania, there are concerns over the viability of this model of care, including how to ensure sufficient staff to cover the services in small rural communities with few incidents of births and to ensure the standard of care. This is supported by Canadian literature suggesting that rural maternity units without caesarean section capability are particularly vulnerable to closure23,24. According to Lynch et al, in 1986 communities with and without caesarean section capability were able to provide care for 78% and 55%, respectively, of local women giving birth; in 2000 these numbers had fallen to 61% and 35%24. In fact, the unit without caesarean section capability that was only performing 35% of local deliveries in 2000 ceased maternity services entirely in the same year. Kornelsen et al pointed out that the sustainability of most non-specialist-led services is in question from a health human resource perspective25. This is an issue in Australia where there is a declining number of GPs who are willing to practise obstetrics26. The closure of the local hospital, difficulty in maintaining skills and the stress of always being on call27 are some of the reasons that GPs cease practising obstetrics.
The findings of the study reveal the health professionals' concerns not only about the sustainability of small rural birthing services without caesarean capabilities but also about the safety of this model. This is supported by an UK study that suggested health professionals voiced their concern about the sustainability of intrapartum care in remote units and believed that the safety and quality of local service were threatened due to the loss of medical cover28. Although small rural birthing services without operation wards would meet the women's expectation with regard to access to services, their expectations of other aspects of maternal services are not likely be met under this model of care. Not having caesarean capabilities in small rural maternity units means that in emergency situations the safety of the women and the babies will largely depend on the transfer and ambulance system. Most, if not all, health professionals in the present study noted that the need for a caesarean section can happen without warning and in these situations transport time is very critical to saving mothers' and babies' lives. In addition, this model of care is supposed to provide care for low-risk women but according to our participants, changes in women's risk status can also happen at any time. Research has found that 55% of pregnancies ending in perinatal death have no identifiable risk factors at the beginning of pregnancy, and that 28% have no risk factors identifiable at the onset of labour29. There are also concerns that available maternity units in rural Tasmania fail to provide women standard care due to the lack of experience in handling deliveries and proper training. Therefore, maternity units not equipped and staffed to deal with unexpected emergencies in childbirth would not be safe for the women and babies.
Although the study sample included 11/20 health professionals who practised in major hospitals compared with those from rural areas, there were no major differences in the perspectives of these two groups regarding women's expectations of maternity care and perceptions of safety in rural maternity units. However, obstetricians were more likely to oppose this model of care. In contrast, midwives were more likely to support small maternity units without caesarean capabilities. This may be due to the underlying theoretical perspectives of each profession. Obstetricians are more likely to be influenced by the medical model in which childbirth requires medical control and monitoring in order to guarantee safety30. The views of midwives more closely adhere to a social model in which childbirth is seen as a natural physiological event, and the majority of pregnant women will have a normal and safe childbirth with little or no medical intervention; while those women who not expected to have a normal childbirth can be predicted and selected31.
The findings from the interviews with 20 maternity health professionals who have experience in providing care for rural women revealed that providing low-intervention style birthing services in rural areas can minimise the difficulties for low-risk women. These women could be offered the choice to receive care in their local communities and thus not have to travel and meet associated costs. Furthermore, being able to stay in the community to give birth enables the women to have the support of their families and social networks which minimizes stress, fear and anxiety.
Regarding women's expectations of maternity care, they want access to care, the assurance of safety for themselves and their babies and quality services. The model of small rural birthing units without caesarean capabilities would provide women access to services and some degree of quality care. However, this model may not meet women's expectations of safety, nor would it guarantee sustainability. Finally, although a few low-intervention style, rural maternity units already exist in Tasmania, they may not meet women's safety expectations in the case of an emergency.
The findings of this study have provided some insights for policy-makers and the state government when planning of the future of this model of care. It is recommended that safety and sustainability issues should be considered when this model of care is to be implemented in other rural communities. While further consideration is needed for small birthing centres in the rural communities, antenatal and postnatal services should be provided in these units to minimise travel needs and to meet the access needs of rural women.
References
1. Australian Government Department of Health and Ageing. Improving Maternity Services in Australia. (Online) 2008. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/maternityservicesreview-discussionpaper (Accessed 10 May 2012).
2. Australian Institute of Health and Welfare. Safety and quality of health care. (Online) 2008. Available: http://www.aihw.gov.au/safequalityhealth/index.cfm (Accessed 10 May 2012).
3. Alston M, Allan J, Dietsch E, Wilkinson J, Shankar J, Osburn L et al. Brutal neglect: Australian rural women's access to health services. Rural and Remote Health 6(1):475. (Online) 2006. Available: www.rrh.org.au (Accessed 10 May 2012).
4. Roach S, Downes S. Caring for Australia's most remote communities: obstetric services in the Indian Ocean Territories. Rural and Remote Health 7: 699. (Online) 2007. Available: www.rrh.org.au (Accessed 10 May 2012).
5. Department of Health and Ageing. Improving maternity services in Australia: Report of the Maternity Services Review. Canberra, ACT: Australian Government Department of Health and Ageing, 2009.
6. Kildea S, Polack W, Barclay L. Making Pregnancy Safer in Australia: The importance of maternal death review. Australian and New Zealand Journal of Obstetrics and Gynaecology 2008; 48: 130-136.
7. Australian Institute of Health and Welfare. Rural, regional and remote health-indicators of health. Canberra, ACT: AIHW 2005.
8. Australian Institute of Health and Welfare. Maternal deaths in Australia 2003-2005. Canberra, ACT: AIHW 2007.
9. Australian Institute of Health and Welfare. Australia's Mothers and Babies 2005. Canberra, ACT: AIHW 2007.
10. Rural Doctors Association of Australia. Maternity services for rural Australia. Canberra, ACT: Rural Doctors Association of Australia, 2006.
11. National Association of Specialist Obstetricians and Gynaecologists. Submission to Maternity Services Review. Sydney, NSW: NASOG, 2008.
12. Klein M, Christilaw J, Johnston S. Loss of maternity care: the cascade of unforeseen dangers. Canadian Journal of Rural Medicine 2002; 7(2): 120-1201.
13. Kornelsen J, Moola S, Grzybowski S. Does distance matter? Increased induction rates for rural women who have to travel for intrapartum care. Journal of Obstetrics and Gynaecology Canada 2009; 31(1): 21-27.
14. Sontheimer D, Halverson LW, Bell L, Ellis M, Bunting PW. Impact of discontinued obstetrical services in rural Missouri: 1990-2002. Journal of Rural Health 2008; 24(1): 96-98.
15. Nesbitt T, Connell F, Hart G, Rosenblatt R. Access to Obstetric Care in Rural Areas: Effect on Birth Outcomes. American Journal of Public Health 1990; 80: 814-818.
16. Kornelsen J, Grzybowski S. Safety and community: the maternity care needs of rural parturient women. Journal of Obstetrics and Gynaecology Canada 2005; 27(6): 554-561.
17. Rural Doctors Association of Australia. Rural Doctors Welcome Maternity Services Review Report. Canberra, ACT: RDAA, 2009.
18. Hoang H. Maternity Care and Services in Rural Tasmania: the Perspectives of Rural Women and Health Professionals (PhD thesis). University of Tasmania, 2012.
19. Glaser BG, Strauss AL. The discovery of grounded theory. Strategies for qualitative research. Mill Valley, CA: Sociology Press, 1967.
20. Strauss A, Corbin J. Basics of qualitative research: techniques and procedures for developing grounded theory. Newbury Park, CA: Sage, 1990.
21. Dietsch E, Shackleton P, Davies C, Alston M, McLeod M. 'Mind you, there's no anaesthetist on the road': women's experiences of labouring en route. Rural and Remote Health 10: 1371. (Online) 2010. Available: www.rrh.org.au (Accessed 10 May 2012).
22. Kornelsen J, Stoll K, Grzybowski S. Stress and anxiety associated with lack of access to maternity services for rural parturient women. Australian Journal of Rural Health 2011; 19: 9-14.
23. Iglesias S, Tepper J, Ellehoj E, Barrett B, Hutten-Czapski P, Luong K et al. Rural surgical services in two Canadian provinces. Canadian Journal of Rural Medicine 2006; 11(3): 207-217.
24. Lynch N, Thommasen H, Anderson N, Grzybowski S. Does having cesarean section capability make a difference to a small rural maternity service? Canadian Family Physician 2005; 51: 1238-1239.
25. Kornelsen JG, Iglesias S. Is rural maternity care sustainable without general practitioner surgeons? Canadian Journal of Rural Medicine 2006; 11(3): 218-220.
26. NSW Health Department. The NSW Framework for Maternity Services. Sydney, NSW: NSW Health Department, 2000.
27. Innes K, Strasser R. Why are general practitioners ceasing obstetrics. Medical Journal of Australia 1997; 166: 276-277.
28. Tucker J, Hundley V, Kiger A, Bryers H, Caldow J, Farmer J et al. Sustainable maternity services in remote and rural Scotland? A qualitative survey of staff views on required skills, competencies and training. Quality and Safety in Health Care 2005; 14(1): 34-40.
29. Högberg U, Wall S, Wiklund D-E. Risk Determinants of Perinatal Mortality in A Swedish County, 1980-1984. Acta Obstetricia et Gynecologica Scandinavica 1990; 69(7-8): 575-579.
30. Savage W. A Savage Enquiry, Who Controls Childbirth? London: Virago Press; 1986.
31. Oakley A. Who cares for women? Science versus love in midwifery today. In: E Teijlingen, G Lowis, P McCaffery, M Porter (Eds). Midwifery and the Medicalization of Childbirth: Comparative Perspectives. New York: Nova Science, 1999.


