Remote Area Nurses (RANs) work in the most geographically isolated parts of Australia, in predominantly Indigenous communities1. These communities are typically the most socially disadvantaged and 'health poor' people in Australia2-4. In addition, these communities often experience high levels of violence5.
Remote Area Nurses are mostly women1, sometimes work alone and are almost universally required to provide after-hours medical assistance6,7. Remote Area Nurses are members of small teams, often working with Aboriginal health workers and off-site GPs. They work in Aboriginal communities, mining, farming and tourism communities and off-shore Islands. The scope and variety of locations of practice, creates situations of increased risk of violence unique to remote area nursing4. This risk is greatly enhanced by the typically solitary nature of the work and lack of support resources within the community5.
Although much has been written about the phenomenon of occupational violence and nursing, literature specific to RANs is scarce. The seminal work by Fisher et al in 19958 and follow-up study by Opie et al9 point to an increase in violence towards RANs over the previous 13 years. Two-thirds of the nurses in the follow-up study reported concern for their personal safety. Violent incidents included verbal aggression and obscene behaviour, property damage, physical violence, sexual harassment/abuse, telephone threats and stalking6. Violence is cited as a significant stressor for RANs and is a contributing factor to the frequency of staff turnover in remote areas5. Evidence highlights that the retention of experienced RANs provides benefits in terms of patient and community outcomes through continuity of service, and that it is fiscally beneficial to all10. Therefore, addressing the issue of violence towards RANs benefits not only the nurses themselves, but also the health of the community.
Australian occupational health and safety legislation states that employers have a responsibility to provide a safe workplace for their employees11,12. However, many RANs feel under-prepared to deal with issues of violence and some have felt unsupported by their employer following a violent incident6. Understanding how to assess, estimate and evaluate the risk of violence in a variety of settings is vital to safe practice13.
A risk management approach which encompasses the overall process of hazard identification, risk assessment, developing control measures, implementation and evaluation, is commonly used as a framework to systematically address the issue of occupational violence6,14-16. Determining appropriate measures to manage the risk of violence must begin with the hazards identified by the risk assessment as the highest priority14. The role of the four main characters in a violent incident should be explored, namely: environment, nurse, client and organisation17. For the purposes of this study: 'environment' refers to the physical practice environment, for example the clinic; 'nurse' refers to the RAN; 'client' could be either the patient or bystander and may be more than one person; and the 'organisation' refers to the external structure within which the nurse is practising and includes the employing organisation and the community.
The purpose of this study was to identify and describe hazards within the RAN workplace from the perspective of experienced RANs. The viewpoint from experienced RANs has not been documented previously, despite the detailed and specialist insight it can provide.
This article describes part of the results of a Delphi study that was conducted in the second half of 201018. The aim of the study was to facilitate consensus among expert RANs about the identification and priority of hazards following a risk management approach. Suggestions for addressing these hazards were also identified and will be reported elsewhere. The Delphi method entails several rounds of questionnaires which progressively refine knowledge and opinion and aims to reach consensus from the participants19. This study involved three rounds.
Thirty-two potential panel members were identified by the researcher and a respected academic in the field of Australian remote health practice. Panel nomination was based on extended length of practice as a RAN, geographical representation and active involvement in the RAN community. Elected state representatives of the Council of Remote Area Nurses Australia and health centre managers were also included.
Ten RANs who had been nominated agreed to form the expert panel. A single representative from the states Western Australia, Tasmania, Queensland and South Australia, along with six RANs from the Northern Territory made up the panel. Eight participants were government employees. Eight were female. The average length of time spent working as a RAN was 13.2 years (range 4-25 years) although this increased to 16.7 years (range 4-30 years) when duration of time spent involved in remote health issues, including management and education, were also considered.
Both email and an online survey were the mediums of data collection. This provided low-cost access to the RAN population distributed across Australia's remote regions.
Three rounds were conducted with all questionnaires pilot tested prior to survey. The first and third rounds consisted of open-ended questions and were completed via email. In the first round, the panel was asked to consider two broad questions: 'What is it about Remote Area Nursing that contributes to violent incidents? and 'What can be done about it?', as a stimulus for generating a list of potential hazards. Content analysis of the data from the open-ended questions facilitated the emergence of themes20. A literature search was then conducted based on these themes and some additional items were added for panel consideration. These items were summarised and reduced in consultation with the research team to 125 hazard items.
The hazard items formed the basis of the second round online survey which required the panel to prioritise the hazard items by way of a five-point Likert scale ranging from 'not a hazard' to 'extreme hazard'. Data analysis weighted the Likert scale in an ordinal manner and then calculated the mean for each item. Mean values were calculated as follows: Not a hazard=0; Minor Hazard=1; Moderate Hazard=2; Major Hazard=3; Extreme Hazard=4. The items with the highest mean represented the greatest hazard. Results were then assessed for consensus among the panel with a 70% level of agreement indicating consensus19.
The third round sought clarification of several issues identified in the preceding two rounds. This article focuses primarily on the results from rounds one and two. One question, however, asked in round three is directly relevant to this article: 'How is information about community members with a history of violence passed on from one health provider to another?'
Presentation of the data to the panel and provision for comments at each stage of data collection, increased the validity of data analysis and increased the reliability of findings presented21. The first author followed a process of 'bracketing' to identify bias that may be present as a result of her previous experience as an RAN21.
Ethics approval
Ethics approval was provided by Edith Cowan University, Human Ethics Committee (#5364) and anonymity of panel respondents was maintained throughout the research process22,23. All participants gave informed consent.
Round one: open-ended questions
The panel identified a large number of hazards in the practice of remote area nursing. These items were sorted and classified according to the characteristics of violence, namely: the environment; the nurse; the client; and the organisation (including community) in which the interaction takes place. Items were further grouped according to similar themes that emerged during the analysis process
Round two: online survey
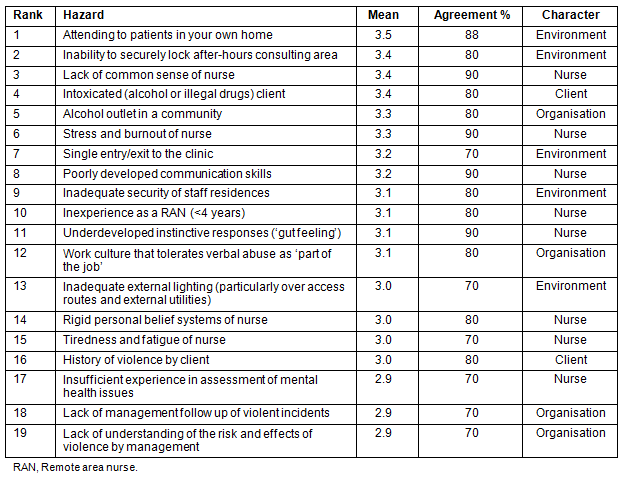
The highest ranking hazards as identified by the panel in the online survey are shown, as is the percentage of panel members who rated the hazard as 'major' or 'extreme' (Table 1). The 'character' column (Table 1) indicates the hazards position within the sub-categories of nurse, client, environment and organisation.
Environment
Environmental factors such as attending to patients in a RAN's private residence and inadequate security locks in the consulting area were considered the hazards of greatest risk to RANs. These were closely followed by only a single entry/exit, and poor security features of staff housing and inadequate security lighting.
Nurse
Nursing attributes including lack of common sense, stress and burnout, poorly developed communication skills and inexperience were ranked as the top hazards for RANs. The panel discussed how long it took to be considered an 'experienced' RAN. They agreed that it took on average 4 years to reach this level, although some panel members recognised that experience is gained at different rates. Rigid personal beliefs were identified as evidence of a lack of cultural awareness or cultural safety preparation. As described by one panel member:
Successful RANs are culturally safe practitioners. They have taken the trouble to see the health service from the community's point of view, learning and understanding the history and the attitudes involved. They also appreciate the power they have by virtue of their position and profession... (Panel member 08)
Tiredness and fatigue, particularly for nurses working in single nurse posts, was seen to:
...contribute to nurses missing cues, and perhaps being less tolerant which could lead to clients being more aggressive. (Panel member 03)
Inexperience in mental health assessment was also considered to be a significant hazard.
Client
Intoxicated clients and those with a history of violence ranked 4th and 16th, respectively, as likely to contribute to RANs' risk. The dynamic nature of violence was also recognised by a panel member who stated:
We need to be aware of the reasons people can be violent; intoxication,.. pain, frustration, biochemical derangement etc. (Panel member 08)
Organisation
Hazards that were perceived to be related to the employing organisation or community included the presence of an alcohol outlet within the community and a work culture that accepts violence as an unavoidable aspect of nursing practice. One panel member stated:
There are situations tolerated by RANs, perhaps due to isolation or the Indigenous clientele that would never be tolerated in another workforce. (Panel member 13)
Lack of understanding and action on the part of management in regard to violent incidents were also identified by the panel as significant hazards. Stories were told of hazards being identified to management and safety audits being completed and then several years later, none of the recommendations had been actioned. One comment highlighted this point:
In my experience policies around workplace violence do more to protect management than it does to protect staff on the ground. (Panel member 03)
Responses from the panel pointed to lack of support within the community as a significant area of concern for RANs. Specifically, the panel stated their objection to single nurse posts and communities without a police presence on the grounds of increased risk of violence towards the RANs within those communities. Support within the community extended beyond the police and health service:
...it is imperative that meaningful relationships are fostered with Aboriginal health workers, traditional healers, community leaders and...specific groups [such as the] women's group. (Panel member 01)
Table 1: Priority hazards as identified by expert panel. Mean values were calculated as follows:
Not a hazard=0, Minor Hazard=1, Moderate Hazard=2, Major Hazard=3, Extreme Hazard=4.
The items with the highest mean represented the greatest hazard.
Round three - history of violence
Identifying community members with a history of violence was mentioned in the first round. The second round confirmed this history as increasing the risk posed by the client. However, it was not known how this information was passed between health staff, particularly new or relieving staff.
The panel stated that this information was rarely passed on and that there was no standardised way of documenting or handing over information about history of violence to other health professionals. Occasionally, notes were made in the patient's medical file or with an 'alert' sticker. Some health services have computerised records and an alert can be included as part of an individual's file. One panel member suggested having photos or a list of known violent offenders in the staff office to inform new staff members of those in the community with a history of violence.
However, panel members were concerned about labelling clients as violent, as this may adversely affect their care in the future or violate their right to privacy.
Discussion
Violent incidents in this study were found to be characterised by the interplay of four main characters: the environment, the nurse, the client and the organisation17. The character most relevant to that hazard was identified (Table 1).
Environment
Attending to patients in the RAN's home was seen by most experts as an extremely hazardous situation and providing good security measures at the staff residence was considered a vital aspect of maintaining the personal safety of RANs. This situation, specific to RAN practice, has been identified as an issue of concern previously6 and there has been at least one serious assault in a RAN's accommodation where the poor level of security provided was implicated24.
Issues relating to building design and maintenance were also considered to be significant hazards for RANs. An inability to safely lock the clinic, having a single exit and inadequate external lighting were most commonly ranked as major or extreme hazards. Maximising the safety of a community clinic may include: limiting access to the building after hours by keeping a minimum number of keys in circulation, keeping the building neat and tidy with vegetation cleared well back from access routes, and maintaining bright security lighting to eliminate hiding places and discourage loitering25.
Assessment of the work environment either by the nurses themselves, with training and support or an independent assessor should be considered a priority by employers.
Nurse
The panel indicated that inexperience as a RAN was a significant hazard and that experienced RANs were better protected from violence due to their knowledge and respect of the community and its culture. Aspects of experience include: length of service as a RAN, well developed communication skills and 'gut feeling', common sense, clinical confidence and culturally safe practice. It is not known empirically if 'experience' is a protective factor for RANs, or if experienced RANs report less violence.
However, common sense and intuition are considered vital skills in assessing the risk of violence. These skills may reflect attention to the 'markers' of risk such as: general appearance (eg 'rough looking'), sex (male), greater physical size/strength, illicit drug use, age (young), psychiatric illness, predictability and presence of companions26. In addition, expert nurses are considered to have '...mature practical knowledge about what to expect of particular patient populations' (p.153)27. This knowledge sparks early recognition when things go awry27. Level of experience as an indicator of vulnerability to violence, is pertinent when considered with recent workforce data that shows the most common length of time spent as a RAN was 2 months and the average was 3.2 years28. This may, at least in part, be an explanation for the rise in incidence of violence reported by Opie et al9. However, it is not known if experienced RANs actually experience less violence. Further research exploring the relationship between RAN experience and incidence of violence could provide guidance for education and recruitment of RANs.
Stress and fatigue appeared to contribute significantly to the risk of violence with 90% of the panel considering the risk as major or extreme. Remote Area Nurses experience high levels of distress related to a lack of infrastructure and the high acuity of their patients7. High staff turnover and inadequate numbers and skill mix of staff in communities is also a significant stressor for RANs5. Remote Area Nurses use less sick leave and work 2 days more per week than their metropolitan counterparts because there is no-one to cover for them1. Staff who are tired and under pressure may be less likely to recognise behaviours that may be precursors to a violent incident and they may not be able to employ the patience, calmness and communication skills needed to diffuse an aggressive situation29. The recruitment of adequately prepared and experienced RANs should be a priority. Retention of RANs using a variety of strategies including personal and professional support appears to be a priority if a reduction in violence is to be realised.
The panel considered RANs with rigid belief system to be at increased risk of violence. This item recognises the different context of nursing practice in remote areas compared with the metropolitan context. City nurses adapting to the very different remote context may experience culture shock30. This is exacerbated by living in the community that they work in. Cross-cultural adjustment may cause significant anxiety, confusion and emotional distress and may compromise clinical care and cultural safety30,31. 'Cultural safety' is a term used to describe nursing care that maintains a person's cultural integrity and recognises that the nurse's own culture impacts on nursing practice32. Culturally safe practice is particularly important in remote areas because the health service provided is generally the only option for residents.
While the panel identified shortcomings of the nurse as 'hazards' it is important to note that lack of preparation and support, combined with high job demands are organisational hazards and outside the control of the individual nurse. Remote Area Nurses who experience violence in the workplace must always be seen as victims of a traumatic event6.
Client
The panel agreed that intoxication with alcohol, petrol sniffing and to a lesser extent marijuana were the most significant risk factors to consider during a violence risk assessment. Mental illness was identified by the panel as a significant hazard with the qualifier that intoxication and non-compliance with a treatment regime further increased the risk. The effects of alcohol, drug abuse and mental illness on the risk of violence posed by a client is well established in the literature29,33.
Clients with a history of violence were identified by the panel as a significant hazard that increased the risk of violence; however, the panel only showed moderate support for documenting clients with a history of violence even though this is highly significant in terms of risk assessment33,34. Further investigation with the aim of creating a process of identifying community members who may pose additional risk due to a history of violence, and also upholds a client's right to privacy, is warranted.
Organisation
The organisation within which RANs work was considered in this study to include both the employer and the broader community context. Communities with an alcohol outlet were considered to be higher risk communities, as were single nurse posts and communities without access to immediate police back up.
A work culture that tolerates verbal abuse was identified as a significant organisational hazard. Under-reporting of violent incidents, a lack of understanding from management, as well as dishonesty about the risk and effects of violence were seen to contribute to this culture. A culture of acceptance that verbal abuse is 'part of the job' contributes to the risk of violence in that it encourages the 'context of silence' that surrounds violence in the remote area nursing workplace6. Adopting an attitude that verbal aggression does not affect the RAN personally, may appear to be protective for some RANs but it may also discourage reporting and discussion among RANs about the effects of verbal aggression, because doing so may be seen as 'weak'. Under-reporting of violent incidents was recognised as a hazard by the panel and well documented in the literature6,35,36. Lack of action from management when hazards are identified and lack of evidence of a commitment to violence prevention initiatives were seen as organisational hazards. One of the reasons cited for the under-reporting of violent incidents is the belief that 'nothing will be done about it anyway'35. Organisations may be considered to be contributing to the incidence of violence by reinforcing the context of silence.
Analysis of organisational policies and procedures related to aggression management and reporting, along with education programs and resources aimed to assist management in changing organisational culture, may counter the context of silence that currently exists.
Limitations
Bias may have been present in the selection of the panel for this Delphi study, and the generalisability of results was limited due to the descriptive nature of the study, and the fact that the majority of participants resided in the Northern Territory.
Prioritising hazards according to a risk management process involves more than just identifying the most extreme hazards. The likelihood and consequences of a hazard occurring must also be considered when allocating resources or implementing control measures14. Further research is required in order to identify control measures and priorities for resource allocation in each workplace.
This study sought to document the opinions of a panel of expert RANs in order to identify and describe hazards that contribute to an increased risk of violence in their workplace. Documentation and analysis of the knowledge and insights of RANs in regard to this phenomenon has not previously been conducted and, as a result, this study adds to understanding the phenomenon of violence towards RANs.
The working environment presents risks to RANs as some consultations occur outside of the clinic environment and building design and security features are vital considerations for RAN safety. Experience as a RAN appears to be an important factor in the incidence of violence as is the level of stress and fatigue experienced by RANs. Remote Area Nurses appear to be concerned about the increased risk of violence when consulting with intoxicated clients, particularly those with mental health issues or a history of violence. Organisational responsibility includes managing the risk of violence through establishing a process of reporting and action where hazards are identified. Challenging a culture of acceptance of violence within the workplace is an important role for the organisation.
Identifying hazards is the first step in a risk management process. Further research is needed to identify measures that may reduce the risk of violence towards RANs. Implementation of strategies to reduce stress and improve retention of RANs may deliver reductions in the level of violence experienced in the RAN workplace.
Further research that considers the impact of violence on victims and the costs incurred by organisations is warranted. Assessments of employers policies, responses and compliance with occupational health and safety legislation may provide evidence to encourage the urgent action that is required to halt the unacceptable burden of violence carried by RANs.
Acknowledgements
The expert panel who generously provided their time and knowledge to this research is acknowledged, as is Lesley Andrew for her input into the original research project.
References
1. Lenthall S, Wakerman J, Opie T, Dunn S, MacLeod M, Dollard M et al. Nursing workforce in very remote Australia, characteristics and key issues. Australian Journal of Rural Health 2011; 19(1): 32-37.
2. Smith JD. Australia's rural and remote health: a social justice perspectiv, 2nd edn. Melbourne, VIC: Tertiary Press, 2007.
3. Dowd T, Johnson S. Remote area nurses - on the cutting edge. Collegian 1995; 2(1): 36-40.
4. Cramer J. Amorphous practice: nursing in a remote Indigenous community of Australia. In: E Willis, V Smye, M Rameka (Eds). Advances in Contemporary Indigenous Healthcare. Sydney, NSW: Content Management, 2006; 191-202.
5. Lenthall S, Wakerman J, Opie T, Dollard M, Dunn S, Knight S et al. What stresses remote area nurses? Current knowledge and future action. Australian Journal of Rural Health 2009; 17(4): 208-213.
6. Fisher J, Bradshaw J, Currie BA, Klotz J, Robins P, Searle KR et al. Violence and Remote Area Nursing. Australian Journal of Rural Health 1996; 4(3): 190-199.
7. Ellis I, Kelly K. Health infrastructure in very remote areas: an analysis of the CRANA Bush Crisis Line Database. Council of Remote Area Nurses of Australia. Australian Journal of Rural Health 2005; 13(1): 1-2.
8. Fisher J, Bradshaw J, Currie BA, Klotz J, Robins P, Searle KR et al. "Context of Silence". Violence and the Remote Area Nurse. Rockhampton, QLD: Central Queensland University,1995.
9. Opie T, Lenthall S, Dollard M, Wakerman J, MacLeod M, Knight S et al. Trends in workplace violence in the remote area nursing workforce. Australian Journal of Advanced Nursing 2010; 27(4): 18-23.
10. Buykx P, Humphreys J, Wakerman J, Pashen D. Systematic review of effective retention incentives for health workers in rural and remote areas: towards evidence-based policy. Australian Journal of Rural Health 2010; 18(3): 102-109.
11. Armstrong F. Keeping nurses safe: an industry perspective. Contemporary Nurse 2006; 21(2): 209-211.
12. National Health and Medical Research Council. When it's right in front of you. Assisting health care workers to manage the effects of violence in rural and remote Australia. Canberra, ACT: Commonwealth of Australia, 2002.
13. Wright NMJ, Dixon CAJ, Tompkins CNE. Managing violence in primary care: an evidence-based approach. British Journal of General Practice 2003; 53(492): 557-562.
14. Grammeno G (Ed.). Planning Occupational health and safety. A guide to OHS risk management, 8th edn. Sydney, NSW: CCH Australia, 2009.
15. Northern Territory Government. Remote Health Branch - Agression Management Policy. Darwin, NT: Northern Territory Government, 2005; 1-2.
16. WorksafeWA. Prevention and management of aggression in health services. A handbook for workplaces. Perth, WA, 2009; 95.
17. Viitasara E, Menckel E. Developing a framework for identifying individual and organizational risk factors for the prevention of violence in the health-care sector. Work 2002; 19(2): 117-123.
18. McCullough KM. Violence towards remote area nurses: a Delphi study to develop a risk management approach. Perth, WA: Edith Cowan University, 2011.
19. Beretta R. A critical review of the Delphi Technique. Nurse Researcher 1996; 3(4): 79-89.
20. Polit D, Hungler B. Nursing Research Principles and Methods, 6th edn. Philadelphia, PA: JB Lippincott, 1999.
21. Koch T. Establishing rigour in qualitative research: the decision trail. Journal of Advanced Nursing 2006; 53(1): 91-100.
22. Waltz CF, Strickland OL, Lenz ER. Measurement in Nursing and Health Research, 3rd edn. New York: Springer, 2005.
23. Adler M, Ziglio E. Gazing into the Oracle : the Delphi method and its application to social policy and public health. London: Jessica Kingsley, 1996.
24. Opie T, Lenthall S, Dollard M. Occupational stress in the remote area nursing profession. In: J Langan-Fox, C Cooper (Eds); Handbook of Stress in the Occupations. London: Edward Elgar, 2011.
25. Wilkinson J, Huntington A. The personal safety of district nurses: a critical analysis. Nursing Praxis in New Zealand 2004; 20(3): 31-44.
26. Magin P, Adams J, Joy E, Ireland M, Heaney S, Darab S. General practitioners' assessment of risk of violence in their practice: results from a qualitative study. Journal of Evaluation in Clinical Practice 2008; 14(3): 385-390.
27. Benner P, Tanner C, Chesla C. Expertise in Nursing Practice, 2nd edn. New York: Springer, 2009.
28. Rickard G. Registered Nurse Workforce in Very Remote Australia. In: Proceedings, 28th Annual CRANAplus Conference; 13-16 October 2010; Adelaide, SA, 2010.
29. Ferns T, Cork A, Rew M. A&E nursing. Personal safety in the accident and emergency department. British Journal of Nursing 2005; 14(13): 725-770.
30. Muecke A, Lenthall S, Lindeman M. Culture shock and healthcare workers in remote Indigenous communities of Australia: what do we know and how can we measure it? Rural and Remote Health 11: 1607. (Online) 2011. Available: www.rrh.org.au (Accessed 27 March 2012).
31. Morgan S. Orientation for general practice in remote Aboriginal communities: a program for registrars in the Northern Territory. Australian Journal of Rural Health 2006; 14(5): 202-208.
32. Eckermann A, Dowd T, Chong E, Nixon L, Gray R, Johnson S. Binan Goonj Bridging Cultures in Aboriginal Health, 3rd edn. Sydney, NSW: Elsevier, 2010.
33. Sands N. An ABC approach to assessing the risk of violence at triage. Australasian Emergency Nursing Journal 2007; 10(3): 107-109.
34. Luck L, Jackson D, Usher K. STAMP: components of observable behaviour that indicate potential for patient violence in emergency departments. Journal of Advanced Nursing 2007; 59(1): 11-19.
35. Ferns T. Under-reporting of violent incidents against nursing staff. Nursing Standard 2006; 20(40): 41-45.
36. Luck L, Jackson D, Usher K. Survival of the fittest, or socially constructed phenomena? Theoretical understandings of aggression and violence towards nurses. Contemporary Nurse 2006; 21(2): 89-101.



