Serious long-term recruitment and retention problems among rural health workers have contributed to inequitable health service access for rural communities1. In response, new healthcare models with flexible workforce roles are emerging, including Expanded Scope of Practice (ESP) paramedic roles2,3.
The research team collaborated with the Australasian Council of Ambulance Authorities and four Australian ambulance services to develop and complete the study. It aimed to identify trends in the evolving practice of rural paramedics and to determine the key characteristics, roles and expected outcomes for a rural ESP model.
Key factors driving the dialogue on ESP for paramedics are4-7:
- increasing demand in emergency departments
- decreasing home visiting by medical practitioners
- paramedics' emerging professionalization.
Major stakeholders in North America and the UK are beginning to promote and embrace ESP roles. In the USA the EMS Agenda for the Future envisions Emergency Medical Services (EMS) undertaking a community-based health management role that is fully integrated with the overall health system4. This concept has been further developed to specifically focus on rural and frontier EMS8,9.
The Joint Royal Colleges and Ambulance Liaison Committee has set the agenda for expanding paramedic practice in the UK10 and the emergency care practitioner role has emerged. In this instance, paramedics have been given additional assessment, treatment and referral skills to deal with a range of minor injuries and falls cases11,12.
There is mounting evidence that the roles of rural paramedics are continuing to evolve in response to the factors identified in this study. Most recently, ESP paramedics have been proposed as a means of maintaining emergency department services in the small rural hospitals of Nova Scotia13 and they have been working with nurses and physicians to support isolated communities14. Australian models built on the foundations of workforce flexibility and integration have been trialled in an urban area of New South Wales, rural Western Australia and in remote northern Queensland15.
These new paramedic models incorporate the 'chain of survival' concept, while increasing the depth of treatment and clinical decision-making, and include more primary healthcare activities than in traditional paramedic roles16. Any changes to paramedic roles must be well considered with care taken to ensure that any expansion does not compromise emergency response, and that appropriate educational programs are in place17. In the event of rural ESP models being embraced as part of an integrated healthcare system, their introduction needs to be closely scrutinized to ensure that changes have positive public health outcomes5.
A multiple case study method was used to examine four initiatives where each ESP role provided a distinct case for description and analysis. This approach allowed researchers to capture the complex and interconnected place of paramedics in rural communities. Multiple case sampling allowed increased confidence in the findings as examples of ESPs, their benefits and other characteristics were found18. All ambulance services providing full emergency health services in Australia were invited to participate via the Australasian Council of Ambulance Authorities. Four State-based ambulance services in south-eastern Australia elected to participate, each proposing up to two case studies as examples of rural ESP. The research team further selected the initiatives on the basis of maximising variety.
The sampling framework incorporated one purposively selected case per partner ambulance service. In each case three sources of data were collected and analysed: semi-structured interviews with up to 17 key informants in each of the four ambulance services; observation of key processes and events; and review of documents which described the paramedic role and the available organizational and educational support. Informants included paramedics, ambulance volunteers, nurses, doctors and members of the community. Interviews were conducted during 2005 and 2006 with further research and analysis taking place concurrently and also following completion of the fieldwork phase of the data collection.
Paramedic research assistants collected data using an interview guide; interviews were taped and transcribed. The chief investigators mentored these research assistants and in some cases accompanied them during the early stages of the fieldwork. Data were triangulated to guard against interviewer bias or inaccuracy18.
Inductive data analysis of each case was undertaken within a conceptual framework that had been developed prior to data collection (Fig1), with discussion about suitable themes and data categories taking place throughout the data collection process. Finally, cross-case analysis, highlighting common features of the extended roles was undertaken.
Ethics approval
Human Ethics approval was obtained from Charles Sturt University (Approval No. 2005/021) and interview participants gave consent for interviews; confidentiality was assured.
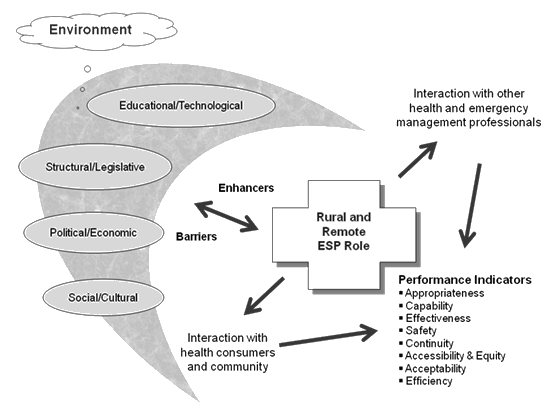
Figure 1: Conceptual framework for Beyond Emergency Response Project.
Case studies
Data from multiple sites in four states, South Australia, Tasmania, New South Wales and Victoria (Fig2), provided information on aspects of healthcare delivery in rural areas across south-eastern Australia. While the study locations presented a diversity of topographic and geographic features, communities in the case studies shared many common characteristics. These included their small size and isolation from major health services, difficulty in recruiting and retaining health professionals, low caseloads and associated risks of paramedic de-skilling, and a reliance on volunteers and/or sole paramedics in emergency health services.
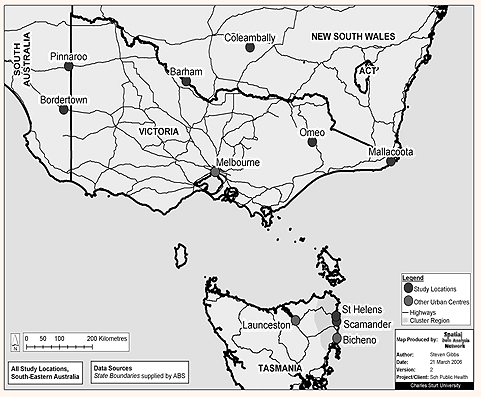
Figure 2: Case study locations in south-eastern Australia.
The South Australian case study was based in Bordertown located near the Victorian border, with limited application at Pinnaroo and two other rural hospitals. In this case the ambulance service is contracted to supply an intensive-care paramedic for rural hospitals' emergency departments within the area when a medical practitioner is unavailable. Paramedics work closely with nursing staff, operate within their existing clinical practice guidelines and consult with the ambulance service medical officer as required. A significant feature of the program is that the paramedic role has changed from the traditional 'scoop and run' or 'shifting the problem' to one that requires more assessment, stabilisation and treatment19.
In Tasmania the case study was located in Scamander and serviced the north-eastern region. Paramedics work as autonomous practitioners operating in partnership with local volunteer ambulance units, hospitals, medical practitioners and the regional community. The role requires strong teamwork, clear communication and understanding between the paramedics, volunteers and other health professionals. In this example the paramedics have the flexibility to extend their roles and adapt to the small communities in which they practice20.
The New South Wales case study covered areas surrounding the small towns of Coleambally and Barham. An overwhelming characteristic of this case study at the time was the lack of any significant change in the roles and interactions of the paramedics, despite their keenness (shared with other health professionals) for some innovation that could help the local health system operate more effectively.
A non-traditional model of service delivery had been developed in Victoria with local communities and other interested parties in the towns of Omeo and Mallacoota21. This expanded role integrated a paramedic into the community to provide public health and pre-hospital care education to the community and other healthcare providers, and supported the volunteer ambulance system.
Limitations
Inclusion of the specific cases was dependent on the willingness of ambulance services to participate in the study. While there was a potential danger that only exemplar examples would be volunteered to the research team, the nominated cases proved to be very diverse and at different stages of development. Participants were independently interviewed and their confidentiality was assured to encourage frank and open responses.
The case studies form the basis of the rural model of practice described later that incorporates a mixture of features that modify the roles and required knowledge, skills and attitudes of rural paramedics. These results, when viewed through the conceptual framework (Fig1), describe some of the environmental influences on the development of the model and how its introduction may impact on paramedics' interactions with rural communities and other health professionals.
Four overarching themes emerged from the data:
- Community engagement
- Clinical response
- Scope of practice extension
- Educational requirements.
Key components of these themes contributed toward the development of the rural expanded scope of practice (RESP) model for paramedics, described below. Other aspects of the findings have been reported previously11,21,22.
Theme 1 - Community engagement
During the study, many interviewees raised the possibility of extending or acknowledging the ESP of paramedics in terms of interaction with their local communities.
It is a combined role and you also extend that further to outside of the branch and there is more community involvement and more involvement with other health organisations and emergency organisations up here as well. So it seems it is quite a broad range of tasks as opposed to being somebody who is on the road all the time. (Paramedic respondent)
A earlier publication of the authors demonstrated that ESPs encourage community engagement and promote the health of rural communities by increasing community response capacity22. They link communities more closely to ambulance services, and facilitate health promotion and illness prevention work at the community level. For example, in some settings ESPs increase community response capacity by providing first-aid training for community members, and they increase the capacity and sustainability for ambulance volunteers through their clinical and educational support. Interviewees noted the increase in volunteer capacity and confidence, and the way they were able to extend their skills:
Obviously the education of the volunteers. They're obviously much more confident, and capable than they ever were before there was a paramedic here. (Health professional respondent)
The ESPs can also generate higher numbers of volunteers:
... it didn't matter how much we appealed or how many advertisements we put in our magazines we couldn't get them. Then the paramedic comes and mate, [s/he] is knocking them back ... (Community respondent)
In addition to their 'life saving' role, paramedics can and often do have positive roles in promoting healthy lifestyles and preventing death and injury through public education programs. These features are based on the view that paramedic care can be an integral part of the local community and integrated into the healthcare system, with professional staff sharing roles that best utilise their skills and knowledge:
Compared to nursing or hospital [situations] the paramedic gets more of an insight into the patient's overall condition, medical as well as social. The paramedic can see more of the requirements for other resources as many patients are elderly, live alone, have lost a partner, have many different social aspects that may not be witnessed in hospital or by other medical staff. (Paramedic respondent)
Paramedics in an ESP role undertake health promotion and illness prevention work, targeted to fit the needs of local communities:
... there is probably not much point in us you know, going out into the community and teaching things like jelly fish stings and envenomation etc etc. but out here there is an enormous relevance for things like organophosphate poisoning which you very rarely see in the major centres, but which you very often see out here ... (Paramedic respondent)
The study findings show that committee membership is common amongst ESPs living in rural towns, where they are involved in activities from Road Safety Task Force Committees to key social and sporting groups. This type of community engagement meant some ESPs both stood out as community leaders and represented health as key stakeholders:
[S/he] is also on our road safety committee, and has designed a mock crash, again, showing the youth what can happen, a big part of our planning. (Community respondent)
While having a job description that included expectations about community interactions facilitated community engagement, it was probably more important that the ESP had good communication skills:
The personality and the way in which the person works is as important to me as that high level of clinical skills that they have because I am really so happy that we have got a fellow like [name deleted] appointed to [town]. If it was someone who had a high level of clinical skills but wasn't such a good communicator, the position I don't think would be as effective. (Volunteer respondent)
Theme 2 - Clinical response
There was strong agreement that paramedics in rural settings need a wide range of traditional paramedic skills to effectively deal with any emergency cases that are encountered.
In some instances, it was reported that ESPs have managed to link communities more strongly to other health services by encouraging the use of air ambulance services for eligible, instead of only critically ill, patients. They had increased the general community knowledge about when to use the air ambulance:
I don't think anyone ever realized that we could just do it so easily ... I think everyone was very reluctant to ever call an air ambulance ... (Community respondent)
While many of the interviewees argued that patients and rural communities would benefit if paramedics located some distance from major centres learnt and practiced a wider range of skills that are more often seen in hospital emergency departments, others had reservations about the feasibility of this suggestion:
It may well be and clearly that there would be health efficiencies to be had if these people could have minor suturing and minor medical treatment effected at local level instead of them being transported some distance to the nearest A & E centre ... (Paramedic respondent)
How far the skills will extend needs to be considered - they may be juggling too many hats. But it may be a good thing for all professions to broaden their outlook and have some overlap with each other. (Health professional respondent)
In spite of these challenges, the paramedics indicated a desire to use their time and skills effectively:
... it's less harmonious in a way when you get three people on duty sitting around here all day in this little office and we haven't had a job now, we had one job in four days. Now that's frustrating. You get a job comes in during the day and there's three on, obviously everyone wants to go. Well you just can't do that. (Paramedic respondent)
One barrier to the introduction of new roles comes from the way that paramedics and others continue to see their role as primarily one of 'emergency response'. These attitudes have been found to be a barrier to paramedic role innovation in Australia23,24:
People don't quite understand the roles that our bureaucracies give us particularly well, in that they don't understand that ambulance officers or the Ambulance Service is primarily concerned with the provision of emergency care. (Paramedic respondent)
Further, some respondents were concerned about the difficulty of maintaining existing paramedic skills in low workload areas and others questioned whether the introduction of more skills may create more problems:
There is a potential for loss of these skills in areas of low workloads. Confidence and performance may drop simply due to a low caseload even if skills level does not. Giving extra skills may not be a solution to this. (Health professional respondent)
Theme 3 - Scope of practice extension
Some respondents could see how modest extensions in paramedic scopes of practice would complement the roles of other rural health professionals and in some cases fill service gaps. The most obvious examples being when doctors cannot provide after-hours services or when there are no doctors located in small isolated communities:
The government is always stating they can't get doctors, so to train paramedics to higher skills when a doctor can't do a house visit would be good. For example with antibiotics, treating minor injuries, this would be better done at home rather than waste valuable hospital resources. (Paramedic respondent)
The other thing is that if we do get an injury that needs a couple of stitches we have to travel all the way to [regional centre] about one hour twenty from here then you have to get back. It would be good if the ambulance could put stitches in and look after wounds so that we didn't have to travel all the way to [regional centre]. (Community respondent)
One of the medical practitioner respondents felt that the introduction of the new paramedic role had personally been a major retention factor because of the assistance it provided in after hours medical coverage.
Having [the ESP] here has been an enormous bonus to us, the practice. I mean before [the ESP] came I was on the verge of leaving the practice. (Medical respondent)
While most interviewees offered positive support for the ESP roles, some respondents did raise role boundary issues. One general practitioner had the view that it would have negative impacts on the health system as a whole:
If a patient cannot get to a GP in a taxi then they are obviously sick enough to be in hospital. Sending a paramedic is not going to help. I do not believe in them expanding their role into other things, but am happy to have them assist when needed. Paramedics should not step out of their boundaries and into the role of medicine otherwise doctors will stop working except between the hours of 9 to 5. (Medical respondent)
Another doctor was concerned about how nurses would react to the ESP role impinging on 'nursing work':
Dressings and when I say basic care, I don't mean that derogatory or anything, but that type of care, the nurses would be very threatened if somebody came in and did that. This organization, I believe would impact because it would be taking work away. So I suppose it sits in the back of my mind, initially when all this started, how it was going to impact on the nursing staff, the organization, our funding bodies. So that was my concern. I am not too concerned now, unless the role changes of course. (Medical respondent)
Theme 4 - Educational requirements
Evolution of ESP roles raises a number of educational challenges. These include identifying the new knowledge and skills required, finding the means to provide continuing education for the paramedics and volunteers, and the value of interprofessional education:
Respondents suggested specific education and training was needed for ESPs such as wound dressing techniques. For example, elderly patients with skin tears may be better treated if paramedics applied the correct dressings and techniques in the first instance. Skills maintenance and access to continuing education for both paramedics and volunteers was of concern, especially for those skills that are rarely used:
I see extended scope as more intricate stuff rather than the day to day stuff that we do. The only thing that I would see is that [s/he] may get bored, because someone with all those skills and whether they use them, with the amount of critical incidents that occur here, you would have to question someone so highly skilled and your normal paramedic has to fit the role. (Health professional respondent)
Volunteer ambulance officer respondents welcomed the advent of ESPs and saw opportunities for their own professional development and extensions to their own skill sets:
Before, we used to hand the patient onto the paramedics from town and the paramedic would go on with the patient so we wouldn't see anyone cannulated or any advanced care. Now it is better because our skills have become more advanced by being able to help out more, for example helping to set up for cannulation or with IVs. (Volunteer respondent)
Those paramedics already working with volunteer ambulance officers welcomed suggestions to enhance their capabilities within regulatory and legal constraints:
There are things the volunteers could develop in such as IVs, but there would be a risk of litigation. If possible the paramedics could be involved in getting the volunteers more involved with greater skills such as IVs, and doing more to assist the paramedics. I feel the volunteers could be more involved with the permanent paramedics ... (Paramedic respondent)
Paramedic respondents recognised the potential tensions related to the blurring of professional boundaries that are inherent in the ESP roles and they related how interprofessional education had improved communication and teamwork with other health professionals:
Protocols need to be aligned and agreed upon between various situations: [nurses] were initially apprehensive as my treatment did not parallel what they were used to from local GP. But they learnt from the experience and were happy. Patient recovered very well. (Paramedic respondent)
Discussion
A rural model
These findings highlight key elements of the development of ESP roles, and the benefits and issues that accompany them. They were used to inform a RESP model containing four key components.
- Rural community engagement
- Emergency response
- Situated practice
- Primary health care.
Rural community engagement: Rural community engagement encompasses extended roles for paramedics in health and emergency service planning and development, along with a more active community role in primary health care such as health education and screening. This role enrichment can have significant benefits for communities. For these roles to succeed paramedics require enhanced knowledge and understanding of rural health issues as well as having the skills to deal with specific ambulance service issues, such as the leadership, management and support of volunteers.
Emergency response: Emergency response includes the traditional role of responding to medical incidents or providing support to volunteer and first responder services. Such response is still a highly valued component of the paramedic role and one which will evolve as paramedics extend their knowledge base and take advantage of technological developments.
Situated practice: Situated practice can take place in either out-of-hospital or institutional settings and is an area where the data suggest there is great potential. Central to this extension of practice scope is the ability to competently assess, treat and release or refer patients when appropriate, or transport patients to hospitals. More use may be made of paramedic knowledge and skills in some medical clinics and hospitals. These 'adjunct' roles may include assistance with airway management, blood pressure measurement and venesection, assisting with the management of 'difficult' patients and the stabilisation of patients. There may also be scope for these minor injury roles to be extended beyond basic first aid in occupational settings such as mines and factories, and in extreme field situations, such as bush fires, wars and major disasters8. However, professional boundary issues may arise with other health professions and RESPs may need organisational support to develop positive interdisciplinary relations.
Primary health care: Primary healthcare integration would see paramedics taking an active and acknowledged role with other health professionals in providing a 'first point of contact' when people have a health problem25. Potential activities that could be integrated and coordinated by paramedics include activities such as health promotion and preventative services, and the treatment of minor injuries12,14.
The RESP model
The RESP model recognises the way its four components are intertwined with other elements of a rural health system. As the data highlight, role changes can bring out issues around professional boundaries and how this model needs to balance key elements of the health system and participant aspirations (Fig3). These include a commitment to population health, high quality clinical care based on the available research evidence, robust quality improvement systems, and responsible fiscal management. In the differing contexts of rural Australia the key components of the RESP model will have varying degrees of salience according to local conditions and needs. It is conceived as a flexible model that has the capacity to grow and develop to fit local circumstances, and avoid the danger of being a 'one hat, fits all' model. Like any abstract model its elements can be adapted to the needs and aspirations of specific communities, paramedics and other interested parties.
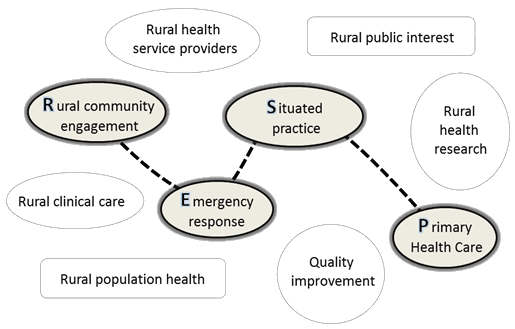
Figure 3: Integrating RESP into the rural healthcare system.
The RESP model has historical links to ambulance service tradition and practice throughout Australia where volunteers formed the genesis of most civilian ambulance systems26. More recently, paramedics have been progressively shifting their education to universities, undertaking research, pressing for occupational registration and forming strong bonds with the established health professions6. They are seen as an emerging health profession27 that is in the process of framing their own professional identity28-30.
Melding existing paramedic models and this emerging professionalism into a new, practical and acceptable model is potentially useful in diverse rural and remote settings where greater use can be made of mixed staffing configurations. This would ideally see RESP roles integrated into teams with community volunteers or first responders, and other health professionals. The essential difference between the RESP model and the widespread urban oriented models used in some rural locations is its extension beyond the well accepted chain of survival's four links (early access, early CPR, early defibrillation and early advanced care) at the site of the emergency event31. The RESP model is also well suited to rural areas with high ambulance 'down-time' and where a demonstrated dearth of other health professionals is evident.
A significant strength of the RESP model is that it draws social and political support from members of the public, volunteers and healthcare professionals who work with and alongside paramedics. This feature may make the RESP model more resilient and less prone to 'capture' by any single stakeholder group such as local hospitals and labour unions. This broader paramedic role may also improve the recruitment and retention to rural areas of paramedics who are looking for enhanced personal and professional satisfaction that can come from roles that extend beyond the traditional emergency response of ambulance services.
Through their education and continuing professional development, paramedics will need to develop improved patient assessment, specific treatment skills and broader clinical decision-making skills. These new paramedics will need to be nurtured through the establishment of a responsive organisational culture and structure that encourages them to respond flexibly to local epidemiologically defined realities that will vary from place to place and may not match centrally framed policy initiatives6,32.
The key feature of the RESP model is its capacity to integrate the existing ambulance systems (including volunteer ambulance models) with public health and social service agencies, primary care providers and other healthcare facilities to ensure that patients are referred to or transported to the most appropriate and cost-effective facility. These characteristics ensure that paramedic care occurs as part of a seamless health system that provides patients with well-organized and high quality care.
The extent to which paramedics are able to become engaged in primary healthcare activities depends on their education and training6, their legal status, and their availability after fulfilling their primary functions in emergency medical care and transportation. Given the large number of paramedic programs now offered in Australian universities, paramedics are educationally well placed to expand their practice beyond emergency response33. Paramedics in Australia are not currently registered as health professionals and this may have some impact on their capacity to fully embrace some of the expanded roles that are emerging throughout the country34-36.
Since the completion of this research project there have been further developments that support the RESP paramedic model. In remote Western Australia, St John Ambulance has trialled and is now implementing a large community paramedic program37. It will provide on-the-ground support in the local community to maximise the number of volunteers and to provide an extended scope of practice where the provision of such services is not viable through the traditional health model3,38. Also, the Ambulance Service of New South Wales has entered into a partnership arrangement with an area health service to enhance local services, with paramedics taking a more active role in emergency departments, health promotion activities, primary health care and medication management during inter-facility transfers3,23.
The description and analysis of this innovative model has set strategic directions for paramedic ESP roles in rural Australia and elsewhere15. The RESP model has the capacity to facilitate a higher quality and more equitable emergency health system for rural communities. This has occurred in several of the case study sites through an increased use of ambulance service resources and through an increase in the clinical and other specialist capabilities of paramedics and volunteer staff.
Introduction of these types of flexible and innovative models need to be based on the values, priorities and capacity of the communities they serve. For the model to provide extended benefits to communities and volunteers, community interaction goals should be clearly defined and paramedics need appropriate leadership and networking skills39. It is clear from previous studies that well developed interpersonal skills and the ability to build relationships with local and regional stakeholders are important and that poor skills in these areas can create conflict and staff retention difficulties3,21,40.
This study demonstrated that paramedics can contribute to an improvement in healthcare service provision and that further expansion of their role may be possible. Many respondents in this study recognised that paramedics' previous professional experience provides them with the knowledge, skills and experience to undertake broader roles than had previously been possible. However, to be effective and sustainable it must be underpinned by a robust education system that provides paramedics with broad knowledge, understanding, skills and professional attitudes that will enable them to operate as independent practitioners41. Emerging rural paramedic roles, such as those described by the RESP model, are more likely to succeed if targeted interprofessional education programs involving paramedics and other health professionals are encouraged and supported. While the diversity among rural communities precludes recommending a single solution, a commitment to learning and solving problems together in a cooperative working environment has the potential to produce a culture of innovation and flexibility that can effectively respond to the needs of individual rural communities.
Acknowledgements
The Australasian Council of Ambulance Authorities Inc funded the Beyond Emergency Response research project. They also facilitated the cooperation of the Ambulance Service of New South Wales, Rural Ambulance Victoria, Tasmanian Ambulance Service and the South Australian Ambulance Service to provide examples of initiatives and provide paramedic research associates to undertake the field research.
References
1. Humphreys J, Wakerman J, Wells R, Kuipers P, Jones J, Entwistle P. "Beyond workforce": a systematic solution for health service provision in small rural and remote communities. Medical Journal of Australia 2008; 188(8): S77-S80.
2. Productivity Commission. The Health Workforce. Research Report. Canberra, ACT: Australian Government, 2005.
3. Council of Ambulance Authorities. Expanding roles: An Australasian overview of emerging paramedic models of care. Adelaide, SA: Council of Ambulance Authorities, 2008.
4. National Highway Traffic Safety Administrator. Emergency Medical Services Agenda for the Future. Washington, DC: National Highway Traffic Safety Administrator, 1996.
5. Mason S, Knowles E, Freeman J, Snooks H. Safety of paramedics with Extended Skills. Academic Emergency Medicine 2008; 15: 607-612.
6. Joyce CM, Wainer J, Piterman L, Wyatt A, Archer F. Trends in the paramedic workforce: a profession in transition. Australian Health Review 2009; 33(4): 533-540.
7. Woollard M. The Role of the Paramedic Practitioner in the UK. Journal of Emergency Primary Health Care 2006; 4(1): 990156 (article no).
8. McGinnis K. Rural and Frontier Emergency Medical Services: Agenda for the Future. Kansas City: National Rural Health Association; 2004.
9. Wingrove G, Laine S. Community Paramedic: A New Expanded EMS Model. DOMAIN 2008: issue unknown: 32-37.
10. Joint Royal Colleges Ambulance Liaison Committee. The future role and education of paramedic ambulance service personnel (emerging concepts). (Online) 2000. Available: www.jrcalc.org.uk/publications_emerging.html (Accessed 29th February 2012).
11. Cooper S, Barrett B, Black S, Evans S, Real C, Williams Cet al. The emerging role of the emergency care practitioner. Emergency Medicine Journal 2004; 21(5): 614-618.
12. Mason S, Wardrope J, Perrin J. Developing a community paramedic practitioner intermediate care support scheme for older people with minor conditions. Emergency Medicine Journal 2003; 20: 196-198.
13. Ross J. The Patient Journey Through Emergency Care in Nova Scotia: A Prescription for New Medicine. Halifax, NS: Nova Scotia Government, 2010.
14. Martin-Misener R, Downe-Wamboldt B, Cain E, Girouard M et al. Cost effectiveness and outcomes of a nurse practitioner-paramedic-family physician model of care: The Long and Brier Islands study. Primary Health Care Research & Development 2009; 10: 14-25.
15. Blacker N, Pearson L, Walker T. Redesigning paramedic models of care to meet rural and remote community needs In: Proceedings, 10th National Rural Health Conference, 17-20 May 2009; Cairns, QLD; NRHA, 2009.
16. Ball L. Setting the scene for the paramedic in primary care: a review of the literature. Emergency Medicine Journal 2005; 22: 896-900.
17. O'Meara P, Walker J, Stirling C, Pedler C, Tourle D, Davis V et al. The rural and regional paramedic: moving beyond emergency response. Bathurst, NSW: Charles Sturt University, 2006.
18. Yin RK. Case Study Research: design and methods, 2nd edn. Thousand Oaks, CA: Sage, 1994.
19. Sefrin P. "Scoop and Run" or "Stay and Play". The Internet Journal of Rescue and Disaster Medicine 1998; 1(1). Available: http://www.ispub.com/journal/the-internet-journal-of-rescue-and-disaster-medicine/archives.html .
20. Mulholland P, O'Meara P, Walker J, Stirling C, Tourle V. Multidisciplinary Practice in Action: The Rural Paramedic - It's Not Only Lights and Sirens Journal of Emergency Primary Health Care 2009; 7(2): 990312.
21. O'Meara P, Kendall D, Kendall L. Working together for a sustainable urgent care system: a Case Study from South Eastern Australia. Rural and Remote Health 4: 312. (Online) 2004. Available: www.rrh.org.au (Accessed 15 February 2012).
22. Stirling C, O'Meara P, Peddler D, Tourle V, Walker J. Engaging Rural Communities in Health Care Through a Paramedic Expanded Scope of Practice. Rural and Remote Health 7: 839. (Online) 2007. Available: www.rrh.org.au (Accessed 15 February 2012).
23. Neumayer B, Malone G. Collaboration of the delivery of rural health services between NSW Ambulance and Greater Southern Area Health Services. In: Proceedings, 10th National Rural Health Conference, 17-20 May 2009; Cairns, QLD; NRHA, 2009.
24. Paramedics Australasia. Consultation Response on National Health Workforce Innovation and Reform Strategic Framework for Action (Framework). Ballarat, VIC: Paramedics Australasia, 2011.
25. Vuori H. Health for all, primary health care and general practitioners. Journal of the Royal College of General Practitioners 1986; 36(290): 398-402.
26. Howie-Willis I. The Australian ambulance system: a historical introduction. In: P O'Meara, C Gribich (Eds); Paramedics in Australia: Contemporary challenges of practice. Sydney, NSW: Pearson Education Australia, 2009; 1-27.
27. Sheather R. Professionalisation. In: P O'Meara, C Gribich (Eds); Paramedics in Australia: Contemporary challenges of practice. Sydney, NSW: Pearson Education Australia, 2009; 62-83.
28. O'Meara P. So how can we frame our identity? Journal of Paramedic Practice 2011; 3(2): 5.
29. McDonnell AC. The search and development of professionalism in "Ambulance": A multidisciplinary journey. Journal of Emergency Primary Health Care 2009; 7(4): 990390.
30. Woollard M. Professionalism in UK paramedic practice. Journal of Emergency Primary Health Care 2009; 7(4): 990391.
31. Jacobs I, Callanan V, Nichol G, Valenzuela G, Mason T, Jaffe P et al. The Chain of Survival. Annals of Emergency Medicine 2001; 37(4): S5-S16.
32. Raven S, Tippett V, Ferguson J-G, Smith S. An Exploration of expanded paramedic healthcare roles for Queensland. Brisbane, QLD: Australian Centre for Prehospital Research, University of Queensland, 2006.
33. Willis E, Williams B, Brightwell R, O'Meara P, Pointon T. Road-ready paramedics and the supporting sciences curriculum. Focus on Health Professional Education 2010; 11(2): 1-13.
34. Fitzgerald G, Bange R. Defining a Regulatory Framework for Paramedics: A Discussion Paper. Journal of Emergency Primary Health Care 2007; 5(2): 990253.
35. Eburn M, Bendall JC. The provision of Ambulance Services in Australia: a legal argument for the national registration of paramedics Journal of Emergency Primary Health Care 2010; 8(4): 99014.
36. Australian College of Ambulance Professionals. Meeting the Challenge. Submission to National Health and Hospitals Reform Commission, 2008.
37. O'Meara P. Community paramedic program for rural and remote areas. Health Matters. Melbourne, VIC: Victorian Healthcare Association, 2011.
38. Joyce G. St John Ambulance Inquiry - Implementation of Recommendations. Perth, WA: Government of Western Australia, 2010.
39. Reeve C, Pashen D, Mumme H, De La Rue S, Cheffins T. Expanding the role of paramedics in northern Queensland: An evaluation of population health training. Australian Journal of Rural Health 2008;16: 370-375.
40. Fahey C, Walker J, Lennox G. Flexible, Focused Training Keeps Volunteer Ambulance Officers. Journal of Emergency Primary Health Care 2003; 1(1-2): 990017 (article no).
41. O'Meara P. The maturation of the paramedic profession through international scholarship. International Journal of Paramedic Practice 2011; 1(2): 2-3.




