The Northern Territory (NT) provides a fascinating setting for learning in allied health practice, and each year students from universities all over Australia undertake placements in allied health workplaces here. These placements occur under the umbrella of work-integrated-learning (WIL), which are university learning activities that bridge formal classroom learning with professional practice and are often workplace-based1. Work-integrated-learning placements are a universal part of allied health professional (AHP) preparation programs, and are known to positively influence career choices and the recruitment of health professional students to rural and remote sites2-4. This recruitment strategy is often employed in the NT where allied health workforce shortages are problematic. A link between student supervision and increased job satisfaction, professional development, and retention of rural allied health professionals in the workforce has also been shown and is relevant to workforce and service delivery planning5-7.
Work-integrated-learning placement programs are, nevertheless, resource-intensive and place demands on healthcare organisations that are often under-resourced and stretched to capacity8. Logistically, remote placements are complicated, expensive, and require high staff to student ratios to ensure quality and safety9-12. These issues compound the social and psychological challenges of geographic isolation, transient workforce, and disease-burdened populations experienced by potential supervisors working in remote settings3. Although student WIL programs are crucial for the perpetuation of the workforce, the viability of WIL programs is dependent on the capacity and willingness of healthcare organisations and staff to provide supervision.
Information regarding the demographics, qualifications, career motivations, and teaching workloads of AHPs in the NT is limited and out-of-date13,14. This research project was motivated by the need to characterise the AHP workforce, and in particular, better understand its capacity for student supervision to inform planning, implementation, and improvement of remote WIL programs. This study sought to identify the characteristics of NT AHPs and their participation in, and capacity for the supervision of students in the workplace. Allied health professionals' satisfaction, motivations, and career intentions were also investigated.
Under the recommendation of Services for Australian Rural and Remote Allied Health (SARRAH), a national study of the AHP workforce was initiated through the University Departments of Rural Health (Rural Allied Health Workforce Survey, RAHWS)15. The RAHWS survey instrument was revised (available on request) to suit the NT context, integrating NT Department of Health and Families data priorities and key student supervision considerations. Piloting of the adapted survey ensured that relevant local information was captured.
The allied health professions eligible for this study were based on the 'Framework for the Classification of the Allied Health Workforce'16 which defines rural and remote allied health and categorises the professions based on qualification/skills level and direct impact on the health outcomes of consumers. This study included non-medical and non-nursing health professions that provide direct therapeutic and diagnostic health services across the NT.
All NT AHPs who met the inclusion criteria above were invited to participate. Online (SurveyMonkey; www.surveymonkey.com) and hardcopy surveys were distributed over a 3 month period (2008/2009) using overlapping recruitment strategies (eg respondents may have received multiple invitations to participate) to ensure maximum coverage of the dispersed and transient target population. Strategies included email distribution through key professional contacts within the Department of Health and Families, professional associations and directories. Snowball recruitment was encouraged.
Responses were entered into a secure electronic database either directly (electronic submissions) or manually (from hard copy). Statistical analysis was conducted using SPSS v17 (www.spss.com) and Microsoft Excel 2007. Analysis excluded cases where data were incomplete or unintelligible. Missing data were imputed from existing data and a 'no response' category included where appropriate. Demographic, professional, and training factors were compared using χ2 and ANOVA tests, as appropriate. The Shapiro-Wilks test was used to evaluate skew within a sample.
Ethics approval
Ethics approval was obtained from the Menzies School of Health Research, Charles Darwin University (#HREC-07/87).
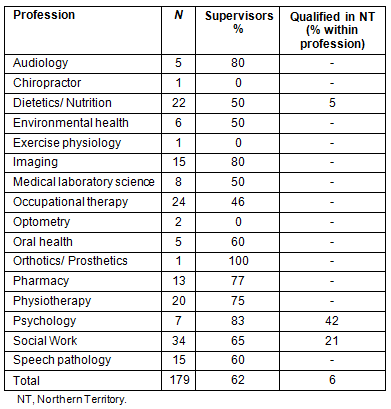
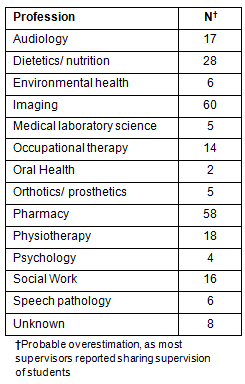
After data cleaning the final sample size (n) was 179. This represents an estimated acceptable 40% response rate. For the purposes of this article, the sample was divided into two categories (supervisors/non-supervisors) based on their (Yes/No) response to the question: 'Do you participate in the supervision of students on professional placements in your workplace?' The distribution of respondents across professions and the percentage who supervised is shown (Table 1).
Table 1: Distribution of respondents across
professions, role in supervision, and portion trained locally
Demographics & participation in supervision
Eighty-four percent of the AHPs in this study were Australian-born; 97% had Australian citizenship, and 80% were female. The average age of respondents was 40.2 years with a range of 23-68 years (SD 11) and significant positive skew (0.947; p<0.05). Most reported having grown up in a capital city or large metropolitan area (73%), while 20% claimed rural and 7% remote upbringing. Only 2% reported being of Aboriginal or Torres Strait Islander descent (NT Indigenous population, 2006: 30%17). Only 6% of respondents had obtained their allied health qualification in the NT, and 8% were trained in a country other than Australia.
In the 12 months prior to the study 62% of the sample had supervised students; the median proportion of supervisors in each profession was 60% (Table 1). Supervisors, who were on average 41.6 years of age, were slightly older than non-supervisors (p<0.05, 3.41 years mean difference). Female and male AHPs in the NT were equally likely to have supervised students.
Workplace & experience
The allied health workforce was concentrated in the capital city, as evidenced by the majority of respondents (67%) reporting working in ASGC R3 (Outer Regional; Table 2)18. Most respondents (70%) worked in the public sector (25% private, 5% non-government organisations [NGOs]). Supervisors were similarly distributed across sectors (77% public, 20% private, 3% NGOs). Neither of the two supervisors who worked primarily in an RA5-Very Remote region were public sector employees.
Years of experience is shown (Fig1). Overall, respondents reported an average of 14.2 years experience in their profession (SD 10), and 6.7 years in their current positions (SD 6). Experience was positively skewed towards fewer years of experience (0.749, p >0.05) with a quarter of respondents having 5 years or less experience. Supervisors had an average of 15.2 years experience, higher than non-supervisors (12.1 years; p<0.1). There was no measurable difference between groups in 'time worked in current position'.
Respondents' work-time was divided across multiple organisational roles: individual patient clinical care (40%), clinical services management tasks (17%), teaching and training (12%), non-individual clinical care (10%), research related activities or travel (6%), travel linked to management or care (5%), or other duties (10%). Organisational roles and time distribution for supervisors are shown (Fig2A), as is their satisfaction with the amount of teaching responsibilities (Fig2B).
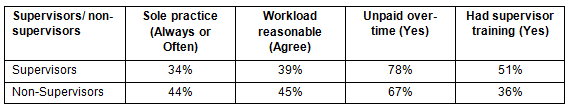
Supervisors and non-supervisors were equally likely to always or often work in a sole practice environment (38%, Table 3). Supervisors, however, tended to be more likely to report working unpaid overtime (p<0.1), and were more likely to have had training in supervising or mentoring students (p=0.05).
Table 2: Geographic and workplace sector distribution of supervisors and non-supervisors
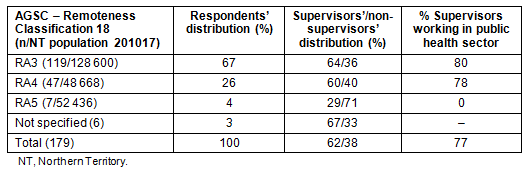
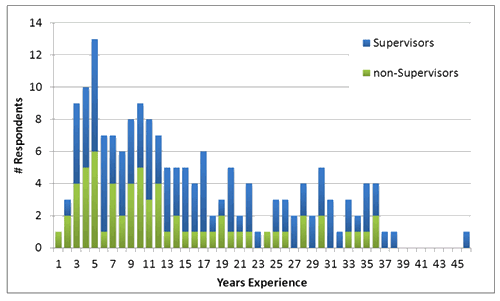
Figure 1: Years of experience (imputed from: years since qualifying in profession).
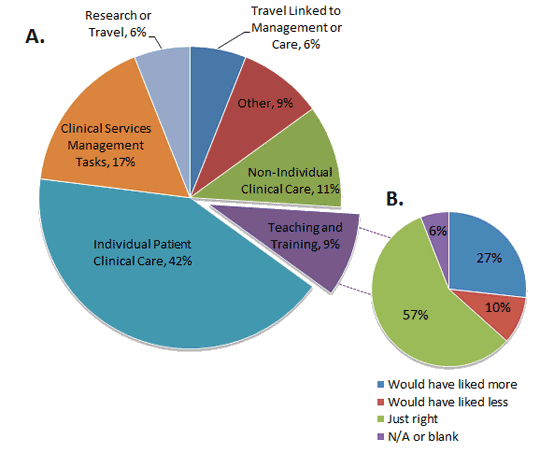
Figure 2: A. Supervisors' distribution of time in organisational roles;
B. Satisfaction with the amount of teaching responsibilities over last 12 months.
Table 3: Comparison of respondents on sole practice, workload, overtime and supervision training
Student supervision responsibilities
The supervisors reported supervising 247 students from 18 universities in the previous 12 months. Ninety-two per cent of supervisors reported teaching students at the undergraduate level across a range of disciplines (Table 4) for placements of 2 days or longer. The majority (60%) reported sharing the supervision with another supervisor.
Half of the supervisors surveyed were satisfied with the amount of supervisory responsibility they had (Fig2B). Almost 30% of supervisors would have liked to do more teaching while 33% of non-supervisors responded that they would like more supervision responsibilities. Supervisors estimated that they allocated 9% of their weekly work time to teaching or supervising. Half of the supervisors reported having had training in supervision or mentoring; of the supervisors who had not received training, 67% reported a need for training. Supervisors and non-supervisors were equally likely to report a need for supervisor/mentor training.
Table 4: Reported number of students supervised
Career motivation and intentions
Income, type of work, and work-life balance were the most frequently selected factors attracting AHPs to their current positions (Fig3). Housing affordability was least frequently selected.
Supervisors and non-supervisors were equally likely to have received a promotion (40% Yes) or salary increase (34% Yes) in their current jobs. Only 22% worked with an aide or therapy assistant. As is shown (Table 5), the majority of AHPs reported having more than 5 days of continuing professional development (CPD) training in the previous 10 months (responses were similar between supervisors and non-supervisors). University or University Department of Rural Health was most commonly listed as the provider of CPD programs.
Seventy-nine percent of the whole sample reported that they were 'Satisfied' or 'Extremely Satisfied' in their current roles. Of the 131 professionals who reported high job satisfaction, 79 (60%) had supervisory responsibilities; however, student supervision was not correlated to job satisfaction in this study. Eighty-one percent of supervisors and 76% of non-supervisors reported being satisfied or extremely satisfied in their current positions (Table 6). Almost half of respondents (8/17) who had < 5 years experience and did not currently supervise students indicated they would have liked to have more student supervisory responsibilities.
The majority (67.5%) of AHPs in the sample reported an intention to leave their current positions in 5 years or less. Notably, those who had student supervision responsibilities were significantly less likely to report an intention to leave than non-supervisors (p<0.01). Of the non-supervisor cohort, 77% reported an intention to leave in 5 years or less. Both supervisors and non-supervisors most commonly cited 'family reasons' as the motivator for leaving; other reasons are listed (Table 7; respondents were able to select more than one reason for leaving).
A strong relationship was identified between lower job satisfaction and intention to leave in the short-term (Fig4). The AHPs who were satisfied or extremely satisfied with their jobs were significantly less likely to report an intention to leave within 5 years (p<0.05).
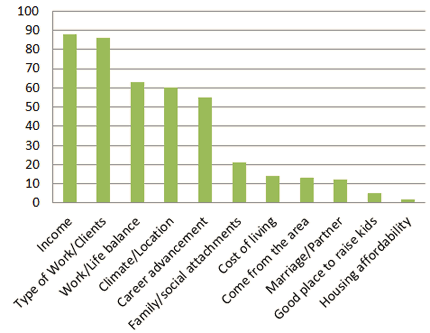
Figure 3: Factors that attracted allied health professionals to current positions.
Table 5: Estimate of continuing professional development time
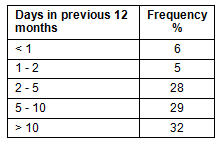
Table 6: Job satisfaction of respondents
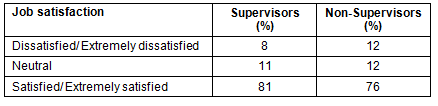
Table 7: Retention time frames and motivation
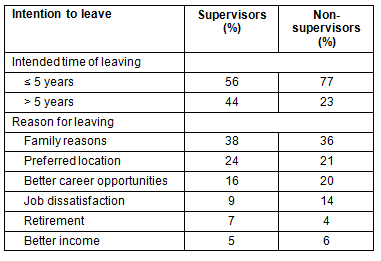
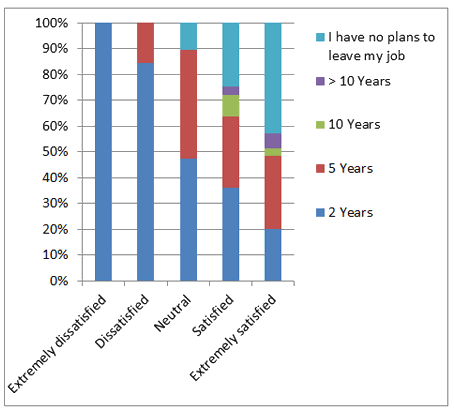
Figure 4: Correlation between job satisfaction and reported intention to leave current job.
Discussion
This study is the most recent and comprehensive analysis of the AHP workforce in the NT13,14. The data help characterise the workforce, their capacity and preparation for student supervision, and career motivations. This study describes a workforce that is predominantly female, Australian trained (although not in the NT), middle working-age, with significant (>14 years) professional experience. Northern Territory AHPs are, on average, younger and less experienced than in allied health workforces elsewhere in Australia19,20. Experience was positively skewed toward fewer years, with half of the sample reporting having less than 11 years experience, and almost a quarter having less than 5 years. This study shows that most professionals supervise students but require more training in supervision, and - of significant concern - a high proportion of the workforce intends to leave their current positions in the near future. These findings support the argument for greater resourcing and efforts toward training and retaining AHPs who supervise students in remote workplaces.
The finding that only 6% of the total sample had undertaken their allied health qualification in the NT illuminates an important factor affecting recruitment. Most of the allied health training courses are not available in the NT. Residents move interstate to obtain their qualification and potentially form relationships and networks that prevent them from returning to the NT. Likewise, NT workforce planners have to rely on the AHP workforce of other states for sufficient AHPs.
The lack of local training AHP courses also has a potential negative impact particularly on Aboriginal and Torres Strait Islanders, who are underrepresented in the NT AHP workforce relative to population. While minority health professionals are far more likely than others to locate their practice in areas where they serve minority patient populations, research has shown that they are also more likely to provide culturally competent care21,22. Successful recruitment of Indigenous people into the allied health professions should be prioritized by allied health training programs nationally, and must be a key consideration in the development of local programs in the NT.
The challenge of recruiting professionals to the NT has significant implications for workforce planning and the retention of professionals, as noted elsewhere23. Based on the present data, AHPs are attracted to the NT by the promise of interesting work, good pay and opportunities for career advancement, as well as a high quality of life (work-life balance) in a favourable climate. In response to the question 'what attracted you to your current position', most respondents cited 'income' and/or 'type of work'; however, further qualitative investigation is needed to explain the 'type of work' that attracts AHPs. Free text responses to this question included reference to the adventure and excitement anticipated in working in the NT and the opportunities for cross-cultural experiences. A caveat on using novelty as a recruitment motivator is sounded by Hall et al, who found unintended consequences when recruitment was based on adventure: the retention rate was less than 5 years24. In light of the significant cost of recruitment25, strategies should target professionals who are more likely to stay.
The present findings about recruitment vary from the trend in published literature, which cites social reasons (eg proximity to family) as a predominant recruitment factor of health professionals, to a rural site26,27. The explanation for this difference may lie in the fact that most of the professionals in the present study were trained - and likely have social ties - outside the NT, a factor which the authors propose then reduces their length of stay. The notion that social ties impact retention has been proposed previously by Hall et al24, who noted that retention is improved when local communities take a role in integrating and supporting new recruits.
Earlier studies have shown a strong relationship between lower job satisfaction and turnover of health workforce28; similarly, it was found that professionals who expressed dissatisfaction with their current roles intended to leave within 5 years. In the NT, three factors combine to form a stressful work environment: the population is small and dispersed over a wide geographical area; the population carries a disproportionate disease burden29; and the NT has the lowest AHPs to population ratio in Australia30. The present sample was predominantly Darwin-based (ASGC RA 318); thus, service delivery to remote communities required extensive time in travel, and a substantial amount of sole practice. The professional context observed fits Wakerman's definition of remote practice: '...characterised by geographical, professional and, often, social isolation of practitioners; a strong multidisciplinary approach; [and] overlapping and changing roles of team members' (p210)31. Although the challenges of the work environment were evident and a link was found between satisfaction and turnover, few respondents in the present study cited job dissatisfaction as the key driver of their intention to leave.
In the present study, retention was linked to performing student supervision because supervisors were less likely to report an intention to leave their current position compared with non-supervisors. Interestingly, fewer years experience did not appear to deter an interest in supervision.
The majority of professionals in the present sample had supervision and training roles for students on WIL placements. Most participants responded that their time commitment to the role was 'just right' or that they would like a greater supervision role; however, they also identified a need for training. This highlights the importance of nurturing constructive university-workplace relations and the regular provision of supervision training1. Reasons for the low level of training for supervision and the impact of supervising a student without training have not yet been assessed but may relate to the high turnover of staff where supervision and training programs have not been conducted locally or frequently. Supervising students in the remote context requires additional skills, resources, and planning. Increased training and resourcing (ie appointment of local placement coordinators and allied health WIL supervisors) may be an effective strategy in addressing these issues.
Study limitations
The response rate for the survey was estimated to be 40%. High workload in the sample population, or concerns about maintaining anonymity due to small workforce numbers may have precluded a higher response rate. Pharmacy, social work and psychology were the most difficult professions to quantify, due to factors including employment outside of the health sector, a less well-networked professional structure, potential inaccuracies in registration board listings, and low use of email in workplaces. Nevertheless, the authors are confident that representative sampling was achieved, that the survey design limited the risk of discovery failure, and that the results are of importance to workforce planning.
Work-integrated learning placements in the NT must be supported as part of recruitment and retention strategies for the allied health workforce. It has been argued that offering student placements in the NT will provide a pipeline of professionals who understand the unique health service requirements of the NT. However, the finding of widespread intentions to leave current positions suggests the retention of professionals who can provide student training is a significant concern. In addition, these results illuminate the need for increased professional development for supervisors. Comprehensive, targeted support programs should be aimed at reducing professional workload and increasing training, recognition, and remuneration for supervising students. Such programs may help stem the skills drain, and improve the preparedness of future remote AHPs. Based on the study findings and the authors' previous work, models of supervisor recruitment and support should focus on professionals not currently teaching, complemented with strategies to overturn the perception that supervision equates to workload overburdening, and mechanisms to develop supportive networks that encourage retention. In addition, higher level responsibility and support for student supervision in workplaces is required, ideally from directors and senior managers, ensuring that student supervision is incorporated into core business and strategic planning.
References
1. Patrick C-J, Peach D, Pocknee C, Webb F, Fletcher M, Pretto G. The WIL (Work Integrated Learning) report: a national scoping study (Final Report). Brisbane, QLD: Australian Learning and Teaching Council, 2008.
2. Laurence CO, Williamson V, Sumner KE, Fleming J. "Latte rural": the tangible and intangible factors important in the choice of a rural practice by recent GP graduates. Rural and Remote Health 10: 1316. (Online) 2010. Available: www.rrh.org.au (Accessed 5 November 2012).
3. Dunbabin JS, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: www.rrh.org.au (Accessed 5 November 2012).
4. Eley D, Young L, Baker P, Wilkinson D. Developing a rural workforce through medical education: lessons from down under. Teaching and Learning in Medicine 2008; 20: 53-61.
5. McDonnel Smedts A, Lowe MP. Clinical training in the top end: impact of the Northern Territory Clinical School, Australia, on the Territory's health workforce. Rural and Remote Health 7: 723. (Online) 2007. Available: www.rrh.org.au (Accessed 5 November 2012).
6. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14: 14-19.
7. Shannon SJ, Walker-Jeffreys M, Newbury JW, Cayetano T, Brown K, Petkov J. Rural clinician opinion on being a preceptor. Rural and Remote Health 6: 490. (Online) 2006. Available: www.rrh.org.au (Accessed 5 November 2012).
8. Northern Territory Government. Northern Territory Submission to the Productivity Commission Health Workforce Study. In: Health and Community Services (Ed.). Darwin, NT: Health and Community Services, 2005.
9. Jones GI, Alford KA, Russell UJ, Simmons D. Removing the roadblocks to medical and health student training in rural hospitals in Victoria. Australian Journal of Rural Health 2003; 11: 218-223.
10. Chaytors RG, Spooner GR. Training for rural family medicine: a cooperative venture of government, university, and community in Alberta. Health and Community Services 1998; 73: 739-742.
11. van Diepen K, MacRae M, Paterson M. Use of clinical placements as a means of recruiting health care professionals to underserviced areas in Southeastern Ontario: part 2 - community perspectives. Australian Journal of Rural Health 2007; 15: 29-34.
12. Schofield D, Keane S, Fletcher S, Shrestha U, Percival I. Loss of income and levels of scholarship support for students on rural clinical placements: A survey of medical, nursing and allied health students. Australian Journal of Rural Health 2009; 17: 134-140.
13. Eastaway J, Campbell N. Position Paper on Allied Health Clinical Education and Training in the Northern Territory. Darwin, NT: Department of Health & Community Services. Northern Territory Government, 2004. Available: http://digitallibrary.health.nt.gov.au/prodjspui/handle/10137/78 (Accessed 28 October 2011).
14. Campbell N, Smedts A, Lowe S, Keane S. The Northern Territory Allied Health Workforce Study. Final report. Darwin, NT: Northern Territory Clinical School, 2010. Available: http://www.flinders.edu.au/medicine/fms/sites/northern_territory_clinical_school/documents/Research%20Publications/The%20Northern%20Territory%20Allied%20Health%20Workforce%20Study.pdf (Accessed 5 November 2012).
15. Keane S, Smith TN, Lincoln M, Wagner SR, Lowe SE. The rural allied health workforce study (RAHWS): background, rationale and questionnaire development. Rural and Remote Health 8: 1132. (Online) 2008. Available: www.rrh.org.au (Accessed 5 November 2012).
16. Lowe S, Adams R, O'Kane A. A framework for the categorization of the Australian Health Workforce. Canberra, ACT: SARRAH, 2007.
17. Australian Bureau of Statistics. Regional Population Growth, Australia. Catalogue no. 32180ds0005_2001-10. Canberra, ACT: ABS, 2011.
18. Australian Bureau of Statistics. ABS Views on Remoteness. Commonwealth of Australia. Catalogue no. 1244.0. Canberra, ACT: ABS, 2001.
19. Keane S, Smith T, Lincoln M, Fisher K. Survey of the rural allied health workforce in New South Wales to inform recruitment and retention. Australian Journal of Rural Health 2011; 19: 38-44.
20. Fitzgerald K, Hornsby D, Hudson L. A study of allied health professionals in rural and remote Australia. Canberra, ACT: SARRAH, 2000.
21. Davidson RC, Montoya R. The distribution of services to the underserved. A comparison of minority and majority medical graduates in California. Western Journal of Medicine 1987; 146: 114-117.
22. Gabard DL. Increasing minority representation in the health care professions. Journal of Allied Health 2007; 36: 165-175.
23. Struber J. Recruiting and Retaining Allied Health Professionals in Rural Australia: Why is it so difficult? Internet Journal of Allied Health Sciences and Practice 2004; 2(2). Available: http://ijahsp.nova.edu/articles/Vol2num2/struber_rural.htm (Accessed 28 October 2011).
24. Hall DJ, Garnett ST, Barnes T, Stevens M. Drivers of professional mobility in the Northern Territory: dental professionals. Rural and Remote Health 7: 655. (Online) 2007. Available: www.rrh.org.au (Accessed 5 November 2012).
25. Humphreys J, Wakerman J, Kuipers P, Wells R, Russell DP, Siegloff S et al. Improving workforce retention: Develping an integrated logic model to maximise sustainability of small rural and remote health care services. In: Institute APHCR (Ed.). Canberra, ACT: Australian Primary Health Care Research Institute, 2009.
26. Solomon P, Salvatori P, Berry S. Perceptions of important retention and recruitment factors by therapists in northwestern Ontario. Journal of Rural Health 2001; 17: 278-285.
27. Stewart SR, Pool JB, Winn J. Factors in recruitment and employment of allied health students: Preliminary findings. Journal of Allied Health 2002; 31: 111.
28. Thomas Y, Dickson D, Broadbride J, Hooper L, Hawkins R, Edwards A et al. Benefits and challenges of supervising occupational therapy fieldwork students: Supervisors; perspectives. Australian Occupational Therapy Journal 2007; 54: s2-s12.
29. Vos T, Barker B, Begg S, Stanley L, Lopez AD. Burden of disease and injury in Aboriginal and Torres Strait Islander Peoples: the Indigenous health gap. International Journal of Epidemiology 2009; 38: 470-477.
30. Lowe S, O'Kane A. Northern Territory Allied Health Workforce Report. Canberra, ACT: SARRAH, 2004.
31. Wakerman J. Defining remote health. Australian Journal of Rural Health 2004; 12: 210-214.
Correction: A correction was made to the Results section of the Abstract. 20% replaced by 30% on 21 February 2013.



