Accommodation use and needs vary according to oncology patients' age, disease, treating institution and country of residence1,2. The types of accommodation most often used by families of cancer patients include private facilities (with family or friends), accommodation provided by charitable organizations (usually with shared, or communal, facilities), hotels/motels and the hospital ward itself1,2. Some research has investigated the types of accommodation preferred by families of adult oncology patients and reported that communal-style accommodation provides positive social opportunities3, allows the formation of social bonds with others2-4 and facilitates the interaction of family members with staff4. However, reported negative aspects of this type of facility include families missing the home environment3,5,6, separation from other family members3, and a loss of the family's existing social network and privacy6.
Important considerations specific to the accommodation needs of families of pediatric cancer patients include maintaining proximity to the rest of the family (including other children) as well as staying close to hospital to facilitate proper patient management7,8. Given the rarity and geographical dispersion of childhood cancer diagnoses, treatment options can be limited in rural or regional areas3. Travelling large distances from home to hospital can directly impact patient care because treatment side effects (eg nausea) can be exacerbated with travel9.
Objectives
The objectives of this study were to explore:
- The accommodation utilized by families of pediatric oncology patients treated at Sydney Children's Hospital (SCH), Australia.
- The financial burden of accommodation and travel, travel time and mode of transport.
- Parents' accommodation preferences and appraisals of bedside, self-contained and communal facilities.
Study invitations were sent to parents of SCH oncology patients who had completed treatment within the past 5 years. The semi-structured telephone interview schedule (Appendix I) was developed by a multidisciplinary medical and allied health team. In order to survey a variety of opinions, parents were invited if they had utilized accommodation on the hospital campus (the ward, or at Ronald McDonald House (RMH), Randwick), private homes, hotels/motels; or if they had stayed at their own home. Interviews were recorded, transcribed verbatim and coded line-by-line9,10. Coding was facilitated by QSR NVivo v8 (www.qsrinternational.com). Rurality of family residences was assessed using the ASGC (Australian Standard Geographical classification) remoteness ratings, which categorize areas according to their distance from 'service centers' across Australia.
Ethics approval
The study received ethical approval (#08/057).
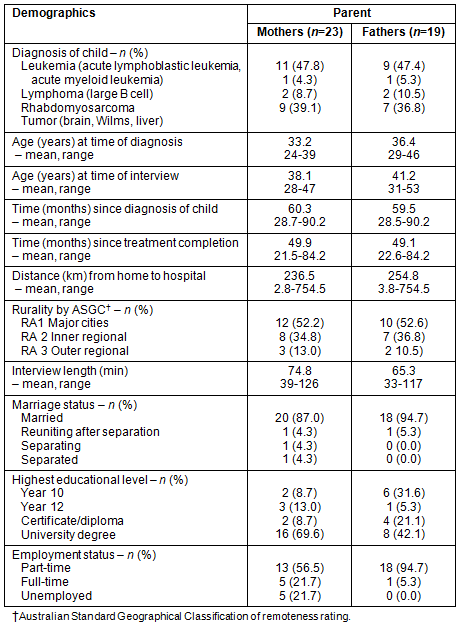
Forty-two families were invited. Of these, parents from 25 families opted-in (see Table 1 for demographics). Contact was lost with two families, resulting in interviews for 23 mothers and 19 fathers from 23 families (n=42; response rate of 57.5%). Nine families stayed at their own residence during treatment (mean distance from SCH for these families was 15.4 km), while 14 families required accommodation. Of these, 13 stayed at RMH for at least some of their child's treatment (mean distance from SCH: 370.8 km). These 14 families were divided into three groups for further comparison where appropriate (3 'local' families who resided in a major city within 100 km of the hospital, but who still required accommodation, with a mean distance of 82.22 km from SCH; 8 'inner regional' (IR) families with a mean distance of 396.75 km from SCH; and 3 'outer regional' (OR) families with a mean distance of 547.4 km from SCH). Of the 13 families who reported staying at RMH, 10 were IR (n=3) and OR (n=7) families. Two IR/OR families also used private accommodation, and three IR and one OR father remained at home (away from Sydney) to care for other children, visiting the hospital occasionally.
Table 1: Summary of demographics of participants
Accommodation information and booking
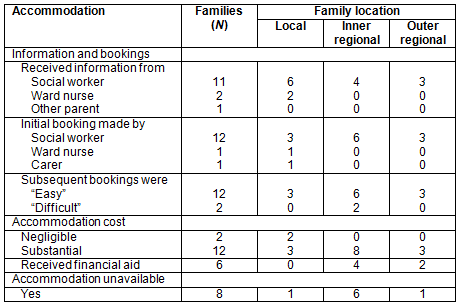
As listed in Table 2, IR and OR parents received accommodation information from social workers (n=7) and other parents (n=1). Twelve families had their initial booking at RMH coordinated by their social worker (local=3, IR=6, OR=3) and in each case reported that subsequent bookings were satisfactory. However, two parents (from different families) appraised the RMH booking system poorly due to the lack of advanced guaranteed booking. Six IR and one OR family reported at least one occasion in which they were unable to be accommodated at RMH. Five families reported that it was more difficult to book accommodation when the child was on less intensive therapy (in line with RMH selection criteria that prioritize new diagnoses).
Table 2: Summary of responses to accommodation-related questions
Financial
All IR and OR families (n=11) reported that accommodation costs were a significant burden (with a minimum cost of A$200 and a maximum of $600 cost per person per trip). Despite this cost, only four IR and two OR families reported receiving financial aid for travel. These families were required to pay their travel costs upfront and funds were claimed back later.
We ended up hiring accommodation close to the hospital which was really hard actually because at the time we were ... building a house, we were renting a unit in [home town] and then we were also renting a place in Sydney and neither of us were working. (Mother, 38 years; home 110.4 km from hospital).
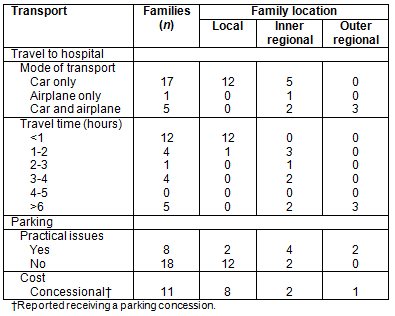
Families most commonly travelled by car (22/23 families). All mothers from OR areas reported travelling by airplane on occasion. Further travel-related information is provided (Appendix II).
Accommodation preferences and improvement suggestions
Accommodation preferences information is provided (Appendix III). When asked to describe their most preferred option, seven out of 11 IR and OR mothers and three out of nine fathers chose a self-contained unit as their first preference. One mother and three fathers from IR and OR areas chose communal living, with an ensuite room. Two IR and one OR mother reported preferring to stay on the ward over all other options. One father from an IR area nominated a hotel or motel as most preferred.
Home
Nine out of 12 'local' families stayed at their residence during treatment and were, unsurprisingly, satisfied with their accommodation experience. Despite living within 100 km of the hospital, three families reported using RMH or other accommodation options during their child's treatment to minimize their travel time to the hospital. One mother and one father from separate local families reported a need for additional assistance with daily chores, and one father reported a need for baby-sitting services for healthy siblings. Two mothers reported a need for more contact with other parents of children with cancer, and one mother and one father desired additional outreach assistance from nurse staff.
Ward
All parents reported staying overnight on the ward at some time during their child's treatment. Positives of staying by their child's bedside included being close to the patient (19M [mothers]; 12F [fathers]), knowing what was happening with treatment (4M;1F), being able to watch or assist the nurses (1M;1F), and the supportive environment (2F). Negatives included the uncomfortable bedding (12M;16F), ward noise (7M;6F), lack of privacy (6M;5F) and limited showering or cooking facilities (3M;1F).
Self-contained accommodation
Reported positives included cooking or showering facilities (8M;10F), the ability to 'get away from everything' (7M;2F), privacy (5M;2F), independence (2M;2F), the ability to maintain a regular lifestyle (4F), and not having to worry about infection (2M;1F). Parents' most commonly cited negatives were social isolation (3M;7F), cost (4M;3F) and distance from hospital (5M).
Communal living
Key positives of communal style accommodation included meeting others (12M;9F), proximity to hospital (5M;1F), privacy (3M;1F), and access to children's play area (1M;3F). Negatives included interacting with parents who did not understand oncology-specific needs (3M;6F), lack of ensuite in some rooms (3M;4F), being surrounded by sickness (4M;1F), small rooms (3M;1F) and lack of privacy (4F). Parents were also concerned by infection risks (2M;F1), and noise from other families (2F).
Discussion
Parents provided positive appraisals of the accommodation options offered to families attending SCH for pediatric cancer treatment. However, several IR and OR families expressed dissatisfaction in their ability to access accommodation when required or to receive booking confirmations in an adequate timeframe. The majority of parents (from local, IR and OR areas) would prefer to stay close to the hospital, a preference of family members of adult patients as well1,11. The importance of close proximity for families of pediatric oncology patients is reinforced by research that suggests that better decisions are made by medical staff and treatment adherence is better in families staying near hospital7,8,12-14.
Self-contained accommodation (near hospital) was the most highly endorsed accommodation option for both IR and OR families, particularly by mothers. Self-contained accommodation was, however, frequently unavailable. Although communal accommodation was often not the option most preferred by families, this type of accommodation may meet the needs of some families for whom isolation is a concern. This is consistent with Payne et al. who reported that communal living allows isolated families to develop a social or support network4. However, parents reported the lack of ensuites in communal accommodation as a major unmet practical need. This, and other, concerns (eg exposure to other sick children) may be addressed in communal facilities by dedicating an oncology-specific area. Both IR and OR families also reported greater difficulties accessing accommodation when on maintenance therapy. While priority needs to be given to patients with greater clinical need, this is an important finding not reported previously. Families who have completed their initial treatment may be caught off-guard by the need to book alternate accommodation, despite the importance of continued medical care at this time.
The major costs reported included the cost of travel and accommodation for families living large distances from their treating center, rather than the patient's direct medical costs1. In line with our findings, adult cancer patients also report difficulty paying upfront for accommodation, even when this cost will be reimbursed1. Previous studies have reported poorer outcomes for pediatric cancer patients living in rural or remote locations15 and also warn that families from rural or remote areas may be less likely to seek needed help15.
Clinical implications
The financial burden of accommodation and travel is a major source of stress for families from IR and OR areas, and is not matched by available financial assistance1. Where possible, clinicians may ease this burden by providing flexible care, including scheduling appointments that allow families to fly to and from their appointment on the same day. Given the rarity of childhood cancer, it is not cost-effective to duplicate services outside of tertiary hospitals. However, further development of shared care models, in which primary oncologists liaise with local hospitals whenever possible, would be valuable. There is a need for greater access to accommodation tailored to suit the needs of regional families. Data suggests that appropriate accommodation (delivered well) can reduce length of hospital admission (due to outpatient care and faster recovery)7,8,12,13. Further investigation of the psychological or medical impact of access to different types of accommodation is warranted.
Limitations
A strength of this study is that it rigorously documented the needs of both local (or 'urban'), and IR and OR families from the perspective of both parents. The qualitative framework provided ample, nuanced data in an under-researched area. The sample size was however, small, and included parents at a single site, limiting transferability. The study was also limited by its reliance on retrospective accounts.
With a large percentage of families travelling long distances for treatment at SCH, it is important to assess their accommodation needs and experiences. Although parents positively appraised the accommodation options they utilized, they also provided useful suggestions for enhancing the experiences of future families. There is a clear need for greater access to accommodation specifically tailored to suit the needs or preferences of families from rural and remote locations.
Acknowledgements
The authors thank Jordana McLoone who assisted with the development of the interview schedule, Sarah Ellis who provided administrative assistance throughout the project, and Jennifer Cohen who provided clinical guidance for the project development - all from Sydney Children's Hospital. The Behavioural Sciences Unit at Sydney Children's Hospital, is supported by the Kids with Cancer Foundation.
References
1. McGrath P, Seguerra J. The patient transit assistance scheme: a consumer's perspective. Australasian Journal of Rural Health 2000; 8(1): 232-238.
2. Wilkes LM, White K, Mohan S, Beale B. Assessing metropolitan cancer care services: practical needs of rural families. Journal of Psychology Oncology 2006; 24(2): 85-101.
3. Hegney D, Pearce S, Rogers-Clark C, Martin-McDonald K, Buikstra E. Close, but still too far. The experience of Australian people with cancer commuting from a regional to a capital city for radiotherapy treatment. European Journal of Cancer Care (Engl) 2005; 14: 75-82.
4. Payne S, Jarrett N, Jeffs D, Brown L. Implications of social isolation during cancer treatment. The implications of residence away from home during cancer treatment on patients' experiences: a comparative study. Health and Place 2001; 7(1): 273-282.
5. Martin-McDonald K, Rogers-Clark C, Hegney D, McCarthy A, Pearce S. Experiences of regional and rural people with cancer being treated with radiotherapy in a metropolitan centre. International Journal of Nursing Practice 2003; 9: 176-118.
6. Wrubel J, Acree M, Goodman S, Folkman S. End of living: maintaining a lifeworld during terminal illness. Psychology and Health 2009; 24(10): 1229-1243.
7. Enand M. The impact of Ronald McDonald Houses on their partner Children's Hospitals. Portland, OR: University of Portland, 2004.
8. van Linschoten CP, Reuter E. A home away from home: summary of the report on the study of the 'use and necessity of the Ronald McDonald House'. Chicago, IL: Argo Institute/Groningen University, 1996.
9. Miles MB, Huberman AM. Qualitative data analysis: An expanded sourcebook, 2nd edn. London: Sage, 1994.
10. Denzin JM, Lincoln YS: Handbook of qualitative research. London: Sage, 1994.
11. McGrath P. Accommodation for patients and carers during relocation for treatment for leukaemia: a descriptive profile. Supportive Care in Cancer 1999; 7: 6-10.
12. Mission Measurement. Literature review in support of: Ronald McDonald House Charities. Portland, OR: Mission Measurement, 2007.
13. Stangroom C. An investigation into the value created by Ronald McDonald House Charities to its partner Children's Hospitals in Australia. Melbourne, VIC: Monash University, 2007.
14. Ronald McDonald House Charities. Available: www.rmhc.org.au/. (Accessed 18 December 2011).
15. Aitken TJ, Hathaway G. Long distance related stressors and coping behaviors in parents of children with cancer. Journal of Pediatric Oncology Nursing 1993; 10(1): 3-12.
________________________
Appendix I: Sample questions from the semi-structured interview schedule

Appendix II: Responses to travel-related questions summary
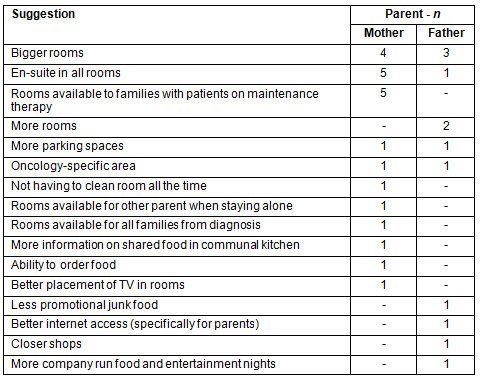
Appendix III: Spontaneous suggestions for improvement of accommodation
at Ronald Macdonald House, Randwick