Timor-Leste is a small lower-middle income country1. Its land area of 14 874 km2 covers half the island of Timor in the Timor Sea, to the north of Australia. It has a population of 1 066 582, of whom 70% live in rural areas2 and 40% live below the poverty line3. Social and health indicators are poor, with high rates of infant and maternal mortality3. The capital, Dili, forms one of 13 administrative districts.
Since gaining independence in 2002, the new government has faced many challenges in rebuilding infrastructure and services that were almost totally destroyed in the mass violence that accompanied the withdrawal of Indonesian forces that occupied the former Portuguese colony from 1975 to 19994. Continuing low-level civil conflict has further hampered development efforts. The chronic shortage of health professionals, who are mainly concentrated in urban centers5, has also contributed to difficulties in delivering high quality and accessible health care to rural communities6.
Faced with many other pressing health issues, including infectious diseases, it is perhaps not surprising that the eye health workforce and eye care services are inadequate7. Lack of access to preventive or curative eye care services leaves many people vision impaired. Distance and near vision impairment affected 25%8 and 32%9 of people aged 40 years and over, respectively in 2005. Cataract and uncorrected refractive error caused more than 90% of all distance vision impairment8.
An objective of the National Eye Health Strategy 2006-2011 was to improve access to eye services for all, including primary eye care, refractive error correction and cataract surgery10,11. The traditional vision screening outreach model involved periodic visits by international and local (Dili-based) teams to district hospitals.
This article reports on the first year of operation of an alternative approach whereby transport and support were provided to a trained eye health nurse in a rural district, enabling him to provide outreach services to rural and remote communities at the sub-district level. The aim was to determine if access to eye care services in rural areas of Timor-Leste could be improved through a district-based outreach service. A motorbike was provided for the Eye Care Nurse (ECN) based at Covalima District Hospital to deliver eye care services to sub-district community health centers on a regular basis. Covalima district was selected as the pilot site due to its remote location and geographical challenges to accessing services. Moreover, the ECN had shown dedication and an interest in providing outreach eye care since commencing services in 2003.
Setting
Covalima is 178 km (5-6 hours travel by road) from Dili. It has 7 sub-districts and a total population of approximately 60 000 people, more than half of whom live outside the main sub-district and population centre of Suai Town2. When travelling to and from Dili, most people depend on public transport, which is expensive and often unreliable due to bad weather and poor roads. There is no public transport within the sub-districts.
The only ECN is based at the Covalima District Hospital in Suai Town. Prior to this project, regulations restricted all hospital-based staff to provide care to patients during working hours on the hospital premises. Thus, people who lived outside the town area and could not travel to the hospital could not access eye services; only basic health care services were available at village health posts.
Preparation
The project was conducted as a partnership between the Ministry of Health, the Covalima District Hospital and The Fred Hollows Foundation New Zealand (FHFNZ, an international non-government organization working in eye health), in accordance with a signed letter of agreement. Prior to its commencement, the Ministry requested that all hospitals grant special dispensation for the ECN to deliver outreach services to sub-districts in coordination with the District Health Services. This was arranged by Suai Hospital and Covalima District Health Service.
Intervention
The project was incorporated as part of the broader health service under the hospital's annual action plan. Visits by the ECN to different rural communities supplemented the clinical eye care and eye health counselling services provided at the hospital-based eye clinic. Outreach activities included vision screening and spectacle dispensing for the community and primary school children, as well as health promotion activities focused on nutrition and hygiene. Patients identified with operable cataract were informed of the date of the next surgical outreach in Suai Town, and conditions beyond the scope of management of the ECN were referred to the hospital in Dili. Spectacle supply for the project was managed by local non-government organization Fo Naroman Timor-Leste as part of the National Spectacle Program12.
The FHFNZ funded the motorbike and running costs and employed the project coordinator (SP) who provided project training and supportive supervision to the ECN, as well as project monitoring and evaluation. Monthly supervisory visits allowed early identification and prompt response to areas in need of attention.
Evaluation
Baseline and ongoing data on patients accessing eye services at the hospital were extracted from routine monthly reports. A project monitoring form was designed to capture elements such as patient demographics, number of patients seen and spectacles dispensed, number of health promotion participants, and costs. The Organization for Economic Co-operation and Development (OECD) evaluation framework with modifications suggested by Chianca13 was used to assess if the outreach program met the criteria of relevance, effectiveness, efficiency, impact and sustainability.
The data reported here were collected during the first 12 months of the project's operation, from June 2009.
Activities
In the year before this project, 564 patients were screened and 360 spectacles were dispensed, all at the hospital. No health promotion activities were conducted.
During the project period, 55 outreach visits were conducted throughout the 7 sub-districts (Table 1). In total 1405 people participated in outreach vision screening and 777 were dispensed spectacles. Almost half of those screened (47.9%; n=673) and receiving spectacles (47.6%; n=370) were female. In addition, the ECN conducted 39 health promotion activities, with 540 men, 573 women, 900 boys and 837 girls participating across all sub-districts. The ECN also provided vision screening at 21 schools, screening 966 boys and 853 girls. No children screened were identified as requiring spectacle dispensing or referral.
Table 1: Eye health services provided in Covalima District for 12 months from June 2009
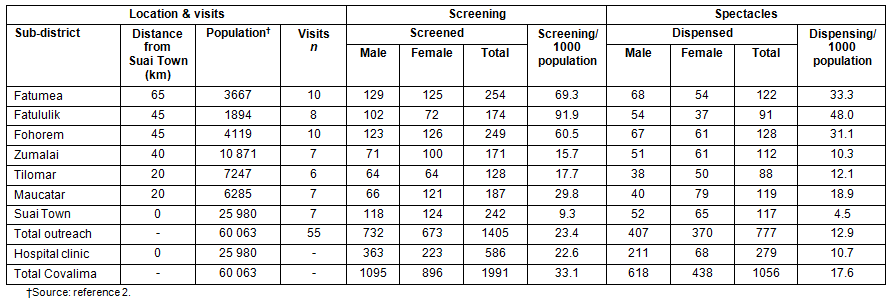
When not providing outreach services, the ECN screened 586 people who presented to the eye clinic at the hospital, and he dispensed spectacles to 279 people. Including both hospital and outreach services, 1991 people were screened, 3.5-times as many people as in the preceding 12 months, while 2.9-times as many people received spectacles.
Women accounted for 38.1% (n=223) of the hospital consultations and received 24.3% (n=68) of all spectacles dispensed there (Table 1). Female participation in screening (Χ2=16.2, df=1, p<0.001) and spectacle dispensing (Χ2 =45.7, df=1, p<0.001) was statistically significantly higher on outreach compared with the hospital.
There was considerable variation across sub-districts in the proportion of the population who received eye health services (Table 1). Excluding Suai Town, the vision screening rate ranged from 15.7/1000 population in Zumalai to 91.9/1000 population in Fatululik. Suai Town had the lowest proportion of people receiving vision screening through outreach (9.3/1000); however, when the consultations at the hospital clinic were included (22.6/1000) the ratio became 31.9/1000 population. These results were not unexpected. Zumalai sub-district has the largest population after Suai Town and is widespread with poor roads. During a monitoring visit, the Zumalai Community Health Centre chief requested expansion of the outreach service to health posts in the sub-district. This was not possible during the project period due to lack of roads or unfavorable road conditions.
Cost
The salaries of the ECN and the project coordinator were borne by their employers regardless of this project, so have not been included in cost calculations. Further, supervision and mentoring activities were undertaken opportunistically in conjunction with other activities, so the additional costs for these (borne by FHFNZ) were low, and also not included in these calculations.
The major expense of this project was therefore the motorbike, which cost US$2,025. Running costs, including fuel and maintenance, totaled $1,191 over the 12 months. These costs were relatively modest and would compare favorably with the tangible and intangible costs involved in an outreach eye care team from Dili or elsewhere making visits to Suai Town for vision screening. As visiting teams do not usually venture beyond Suai Town, rural people are required to travel to receive eye care from them, which is prohibitively expensive or logistically difficult for many.
Relevance
The people of Timor-Leste are poor and the country has a rugged terrain and little transport infrastructure. Providing a motorbike for the ECN to use in rural outreach was relevant to both the travelling conditions and the setting. It addressed some of the barriers to utilization of eye health services faced by those living in rural areas5. Being from the area, the ECN could speak the local language and was knowledgeable about local issues, unlike outreach teams from the capital or overseas-based international agencies. This project addressed the main causes of vision impairment in Timor-Leste in accordance with the Eye Health Strategy: primarily uncorrected refractive error and presbyopia (access to affordable spectacles), as well as cataract (referred for surgery). In keeping with a primary health care approach, health promotion activities focusing on nutrition and hygiene were incorporated in outreach visits.
Effectiveness
The high number of patients seen on outreach visits was facilitated by the ECN who provided a schedule of visits to all 7 sub-district community health centers in advance. This enabled the community health center nurses to inform the public about the date and place of the next outreach eye care service.
The visiting plan for the first 6 months, which did not take population numbers and geography into consideration, stipulated an equal number of visits to each sub-district and did not allow extra time for more populous places or reaching more remote areas. This was addressed in the plan for the second 6 months but the provision of services across sub-districts remained inequitable. The fact that very few of the school students screened had vision problems suggests that those with problems may be kept at home and that there is a need to find alternative methods of identifying them14.
Efficiency
The project made better use of the ECN's skills and time than when he was restricted to practice in the hospital. In the preceding 2 years he saw, on average, 2-3 eye patients per day at the hospital. During this project he saw, on average, 4 patients on the days that he was at the hospital and 26 patients per day on outreach. Allocating the cost of the motorbike over the 3 years of its anticipated useable life, the non-salary costs of this project for the first year were $1,866. On outreach visits 1405 people were seen, at an average cost of $1.30 per person. In addition, school vision screening and eye health promotion activities were conducted. If the recipients of these services are included in the cost calculations, the cost per project beneficiary reduced to $0.44 each.
Impact
The project provided a three-fold increase in vision screening services, as well as enabling improved eye health knowledge and awareness opportunities for rural people in Covalima. The project also provided people with access to affordable spectacles within their sub-districts, and most likely an consequential improvement in vision. In addition, vision screening enabled the early detection and management of eye problems, which may lead to improved outcomes through more timely referral to specialized eye services.
Sustainability
The project was implemented in an environmentally responsible way. Clear guidelines about motorbike maintenance were provided to minimize pollution and prolong the life of the motorbike.
Following the evaluation of the project, this eye health outreach service was integrated into annual outreach plans and budgets at the district level. In addition, the political support by the hospital and health services, and the cultural appropriateness of the provision of this public health service by local personnel added to its sustainability.
Conclusion
Providing eye health services to people in rural areas of post-conflict and still fragile states such as Timor-Leste, where the infrastructure and health workforce are very limited, is a major challenge. This pilot project demonstrates what can be achieved when a Ministry of Health (central and district level) and non-government organizations (international and local) work in partnership to support a dedicated health care provider.
The positive outcomes were achieved following an incremental, 'little steps'15 approach. The planning and implementation of a pilot project in a single site was carefully documented. Thereafter an evaluation using an international development framework was conducted prior to reaching a decision on continuation and expansion. Appropriate scaling down of support from FHFNZ as the Ministry of Health takes more responsibility for monitoring and mentoring will be critical for the sustainability of the project. Continuing the project with the same focus on opportunistic monitoring and coordination will keep costs down.
The dedication of the ECN who managed a heavy workload and difficult travel conditions was essential to the project's success. Ongoing support and regular monitoring, with a monthly visit or phone call from the project coordinator were also critical to ensure service quality and to maintain motivation of the ECN. The ECN's engagement and communication with community health center chiefs and other health workers supported project coordination with other community health initiatives and events, and improved awareness and support of eye health services. Ongoing training was required during the project as learning needs became apparent. This focused on patient-centered care, improving communication skills and the collection of monitoring data.
Several thousand rural dwellers previously unable to access eye care services have now utilized these services. Importantly, in addition to meeting the five evaluation criteria of relevance, effectiveness, efficiency, impact and sustainability, the project resulted in significantly greater gender equity among eye health service beneficiaries. To improve equitable access to eye health services across the 7 sub-districts in future, the visiting schedule will need to take into account factors such as population size and dispersion and travelling conditions.
After the first 12 months of this project, the Ministry of Health and FHFNZ agreed to expand this rural outreach model, providing local ECNs with a motorbike, training and support in another three districts. This expansion will likely be accompanied by the usual challenges related to scaling up, such as ensuring quality and equity, as well as ensuring sustainability beyond the involvement of FHFNZ. This pilot project did not have the resources to assess changes in community knowledge and practice in terms of eye health or improvements in vision. These are important measures for ongoing monitoring and evaluation. Identifying ways to ensure other ECNs are similarly motivated and committed to the eye health program objectives is likely to be necessary. Further, it is probable that health system strengthening will be required to ensure the project remains adequately supported by realistic and ongoing financing, leadership and management16.
Acknowledgements
The authors acknowledge the dedication and hard work of Covalima ECN Mr Bernadino Pires, as well as the help and support of the Timor-Leste Ministry of Health, Covalima Hospital Director, Fo Naroman Timor-Leste, Irim Tolentino, Lucy Lee and Karen Hobday.
References
1. World Bank Country Database. Data: Timor-Leste. (Online) 2012. Available: http://data.worldbank.org/country/timor-leste (Accessed 21 January 2012).
2. National Statistics Directorate, Ministry of Planning and Finance, Government of the Democratic Republic of Timor-Leste. Timor-Leste National Census of Population and Housing 2010: Preliminary Report. Dili: Government of the Democratic Timor-Leste, 2010.
3. United Nations Development Programme Human Development Report 2010. The real wealth of nations: pathways to human development. New York: UNPHDR, 2010.
4. Earnest J, Beck M, Connell L (Eds). Rebuilding Education and Health in a Post-Conflict Transitional Nation: Case Studies from Timor-Leste. Rotterdam: Sense, 2008.
5. Palagyi A, Ramke J, du Toit R, Brian G. Eye care in Timor-Leste: a population-based study of utilization and barriers. Clinical and Experimental Ophthalmology 2008; 36(1): 47-53.
6. Zwi AB, Blignault I, Glazebrook D, Correia V, Bateman Steel CR et al. Timor-Leste Health Care Seeking Behaviour Study. Sydney, NSW: University of New South Wales, 2009.
7. Palagyi A, Brian G, Ramke J. Training and using mid-level eye care workers: early lessons from Timor-Leste. Clinical and Experimental Ophthalmology 2010; 38(8): 805-811.
8. Ramke J, Palagyi A, Naduvilath T, du Toit R, Brian G. Prevalence and causes of blindness and low vision in Timor-Leste. British Journal of Ophthalmology 2007; 91(9): 1117-1121.
9. Ramke J, du Toit R, Palagyi A, Brian G, Naduvilath T. Correction of refractive error and presbyopia in Timor-Leste. British Journal of Ophthalmology 2007; 91(7): 860-866.
10. Ministry of Health, Government of the Democratic Republic of Timor-Leste. National Eye Health Strategy 2006-2011. Dili: Government of the Democratic Republic of Timor-Leste, 2006.
11. Ramke J, Ximenes D, Williams C, du Toit R, Palagyi A, Brian G. An eye health strategy for Timor-Leste: the result of INGDO-government partnership and a consultative process. Clinical and Experimental Ophthalmology 2007; 35(4): 394.
12. Ramke J, Williams C, Ximenes J, Ximenes D, Palagyi A, du Toit R et al. A public-private partnership to provide spectacles for Timor-Leste. Community Eye Health 2007; 20(63): 54.
13. Chianca T. The OECD/DAC Criteria for International Development Evaluations: An Assessment and Ideas for Improvement. Journal of MultiDisciplinary Evaluation 2008; 5(9): 41-51.
14. Ramke J, du Toit R, Roberts B, Pereira S, Hobday K. Vision screening of children attending primary school in rural Timor-Leste. Clinical and Experimental Ophthalmology 2011; 39(4): 377-378.
15. Umar N, Litaker D, Terris DD. Toward more sustainable health care quality improvement in developing countries: the "little steps" approach. Quality Management in Health Care 2009; 18(4): 295-304.
16. Mangham LJ, Hanson K. Scaling up in international health: what are the key issues? Health Policy and Planning 2010; 25(2): 85-96.
