In rural Australia, GPs form the frontline for provision of medical services. Besides responsibilities for primary care via private practice, rural doctors often provide emergency and inpatient services for rural hospitals.
Those rural doctors who have achieved a level of training approved by the Joint Credentialing Committee in Anaesthesia (JCCA) or equivalent experience are deemed capable of providing anaesthetic services for elective surgery in rural Australia as a GP-Anaesthetist (GPA). The 2010 Rural Health Workforce National Minimum Data Set reported 6467 rural doctors in Australia, of whom 861 have procedural skills in fields such as obstetrics, surgery and anaesthetics. Of these, there were an estimated 448 rural doctors with anaesthetic skills in Australia1. In addition to elective anaesthesia, these doctors may be called upon to provide airway support for emergency patients. Meanwhile rural doctors without specific anaesthetic credentialing may also be required to manage an airway as part of an emergency medicine roster.
Difficult airways, whether in the elective or emergency setting, must be managed effectively by the GPA. A difficult airway has been defined by the Australian and New Zealand College of Anaesthetists (ANZCA) as the 'clinical situation in which a conventionally trained anaesthetist experiences difficulty with mask ventilation, difficulty with tracheal intubation, or both'2. Difficult mask ventilation has been reported in 5% of cases, with impossible mask ventilation in 0.15%3. Difficult intubation may occur in as many as 1% to 3% of elective anaesthesia cases and up to 14% of emergencies (the latter including prehospital intubations)4.
Airway problems and lack of equipment were highlighted in the 2011 UK National Audit Project No 4 (NAP4) report, the recommendations of which guide the profession5. Algorithms such as those from the UK's Difficult Airway Society (DAS) exist for such circumstances, necessitating the use of specific airway equipment at defined stages6.
The ANZCA has defined the minimum requirement for basic airway equipment in operating suites and other anaesthetising locations in its 2008 Technical Document T01, Recommendations on Minimum Facilities for Safe Administration of Anaesthesia in Operating Suites and Other Anaesthetising Locations7. This document states that equipment for managing difficult intubations must be readily available in all locations where endotracheal intubation is electively performed. Subsequent to this document, ANZCA provided recommendations on the availability of difficult airway equipment (DAE) in all areas where airways are managed8.
Unfortunately there are no 100% reliable predictors of a difficult airway. A meta-analysis of over 50 000 patients suggested that a combination of both Mallampati score and thyromental distance is the most reliable method of predicting difficult laryngoscopy9. This approach is only 36% sensitive and 87% specific, meaning that unanticipated difficult airways will still occur. Experienced anaesthetists know that the unanticipated difficult airway can catch the unwary at any time and that to be ill-prepared invites disaster. Rural GPAs may encounter unanticipated difficulties with intubation on a routine list even with case-selection to avoid anticipated difficulties. Additionally the case mix in rural Australia often necessitates emergency airway management, which may pose additional hazards (eg unfasted, maxillofacial injuries, anaphylaxis, cervical collar).
Thus GPAs need to have access to an appropriate range of DAE and to apply appropriate difficult airway management algorithms effectively. The range of DAE needs to be an appropriate balance between both the relative infrequency of difficult airway (whether ventilation or intubation) and the consequences of mismanagement, against factors such as ease of use, ongoing training requirements and cost.
This survey was conducted in January 2012 and was directed to rural GP proceduralists delivering anaesthesia in Australia, questioning the availability of DAE in their location, their access to ongoing training and inviting comments on the practice of rural anaesthesia as perceived by respondents.
Invitations to complete an online survey were made to all members on the databases of the Rural Doctors Association of Australia (RDAA) and of the state-based Rural Doctor Workforce Agencies, targeting GPs in rural areas as defined by the Australian Standard Geographical Classification of Rural Areas (ASGC-RA). This includes Inner Regional (RA2), Outer Regional (RA3), Remote (RA4) and Very Remote (RA5) regions of Australia. Respondents were asked to indicate whether they were a GPA or an 'occasional intubator' (a rural doctor who may be required to manage the airway without formal anaesthetic credentials; such doctors typically participate in an emergency on-call roster).
The survey consisted of four sections: (i) demographics; (ii) questions relating specifically to equipment and training for management of the difficult airway based on current ANZCA recommendations8; (iii) other areas of relevance to rural anaesthesia (including involvement in prehospital care); and (iv) access to anaesthetic upskilling.
Responses were entered into a Numbers spreadsheet (Apple Inc, Cupertino, CA, USA) and analysed using Statistical Package for Social Sciences v15.0 (www.spss.com). The Fisher's exact test was used, with a p-value <0.05 considered significant. Demographic data were compared with the 2010 Rural Health Workforce National Minimum Data Set to determine representation of GPAs from each state and survey response rate. As there were no data for the number of rural GPs who provide emergency medicine service (and hence are likely 'occasional intubators'), these and other non-GPA responses were excluded from further analysis. A few respondents elected to provide their contact details in addition to comments. While comments were collated for analysis, identifying information was deleted. All participants gave consent for participation and use of anonymised comments to open-ended questions.
Because this research conforms with the ethical standards established by the NHMRC for quality assurance, research ethical approval was not sought.
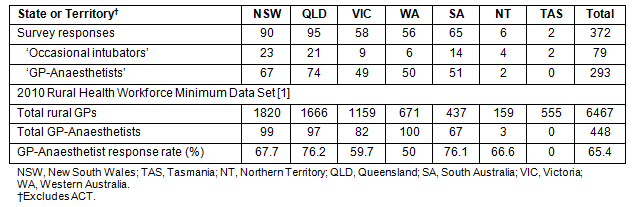
A total of 372 completed surveys were received from doctors in RA 2-5, of whom 293 (79%) identified themselves as GPAs, the remaining 79 (21%) being 'occasional intubators'. Existing data suggests there are 6467 doctors in rural Australia (RA 2-5), with 816 (12%) being proceduralists and 448 (7%) having anaesthetic credentials1. It is unknown how many rural doctors provide emergency medicine services, making the denominator for 'occasional intubators' impossible to determine. Given the majority of survey respondents were GPAs, where the denominator of 448 is known, only responses from this group were analysed (293/448, 65% response rate). Distribution of GPAs was comparable with data from the 2010 Rural Health Workforce National Minimum Data Set (Table 1).
Table 1: Survey response rate for rural doctors by state or territory1
Demographics
Of 293 responses from GPAs, 83% were male. The median age of respondents was 46.4 years (interquartile range 32-61). All GPA respondents were rurally based (RA2 23%, RA3 49%, RA4 18% and RA 5 10%). Of these, 51% received their anaesthetic training in the state where they resided currently, with 13% training interstate and 35% training overseas. As a group they were experienced, with duration of GPA status ranging from 1 to 40 years (mean 15.6 years, 180 of 293 respondents [61%] with >10 years experience). There were no significant differences in respondents between states or ASGC-RA with regard to demographics.
Difficult airway equipment
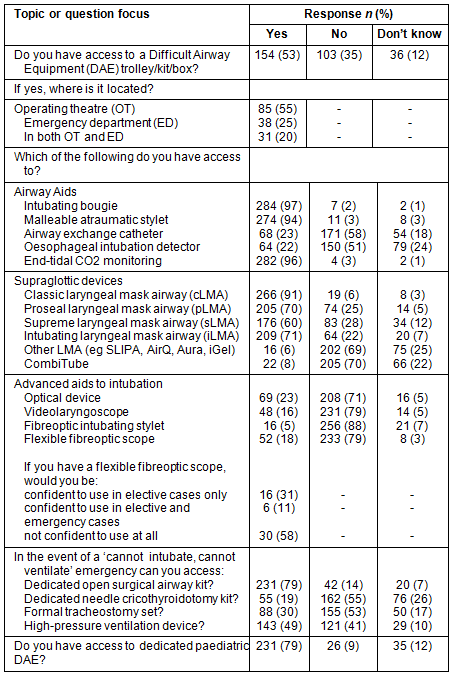
Only 154 of GPAs (53%) indicated that they had access to a dedicated difficult airway trolley or box. The remainder either did not have access to dedicated DAE (35%) or did not know (12%). Further responses regarding the availability and range of difficult airway equipment for GPAs are summarised (Table 2).
Table 2: GP-anaesthetist responses to questions regarding the availability of difficult airway equipment in rural Australia, n = 292
Anaesthesia in rural areas
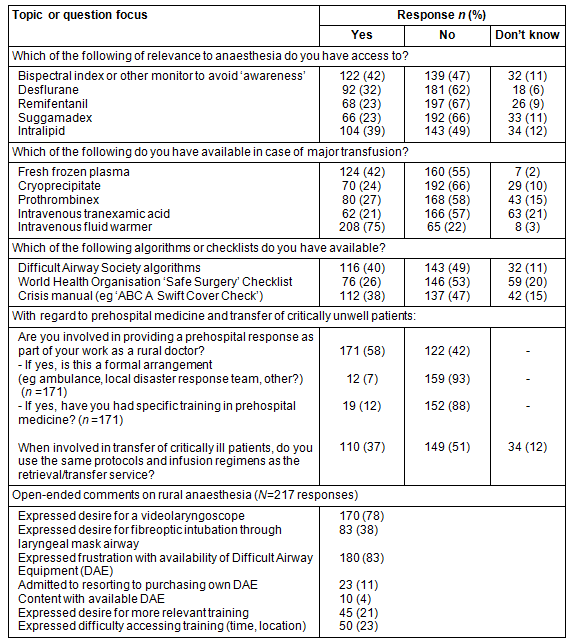
Responses to closed-ended questions regarding the availability of other items usually available to metropolitan anaesthetists, and GPA involvement in prehospital medicine are indicated (Table 3), along with a summary of open-ended questions inviting comment on the practice of rural anaesthesia in Australia.
Table 3: Responses relating to equipment, medical supplies and protocols available to GP-anaesthetists in rural Australia, n = 292 (unless otherwise indicated)
Ongoing training
Of GPAs, 209 (71%) indicated that they had accessed anaesthetic upskilling in the previous 12 months, with 149 (72%) attending a course or conference, 22 (10%) a clinical attachment and 36 (18%) attending both. Of courses attended in the past three years, the Early Management of Severe Trauma (EMST) course was most popular (102 indicated attendance on either provider course [48] or refresher course [54]), along with the Advanced Paediatric Life Support (APLS) course (92 responses). Also popular were Rural Emergency Skills Training (REST, 74 responses), Emergency Life Support (ELS, 56 responses) and various state-based training initiatives (86 responses). The Effective Management of Anaesthetic Crises (EMAC), a specific courses dealing with anaesthetic emergencies and human factors was only attended by 26 respondents. However, 130 GPAs (44%) indicated that they had attended a course dealing with 'the difficult airway' in the past 3 years. Comments included difficulty accessing such courses due to distance and inability to arrange locum cover.
Discussion
This study has surveyed the rural GPA workforce in Australia to question the availability of equipment and training in difficult airway management. Respondents were also invited to make comments on anaesthesia from a rural perspective. Key findings include the paucity of access to a dedicated DAE trolley or box for rural GPAs (53%) and the range of airway equipment available. Less than 25% of GPAs reported access to an optical (23%) or video (16%) indirect laryngoscope, despite the plethora of such devices now available to the wider anaesthetic community. Open-ended comments from 217 GPAs suggested frustration with the availability of DAE (83%), with a desire for equipment to allow indirect techniques such as optical or videolaryngoscopy (78%) and a means of fibreoptic intubation through a laryngeal mask (38%). Eleven percent of GPAs had purchased their own DAE. Only 4% were content with the range of DAE available to them. The GPAs were often involved in prehospital medicine, with 58% attending out-of-hospital incidents. Such responses are appropriate for GPAs with skills in airway management and may value-add to care delivered by paramedics, many of whom may be volunteers in in rural and remote areas. Importantly only 7% of GPAs reported a formal arrangement, suggesting that such responses are ad hoc. Only 12% had received formal training in the prehospital environment.
Problems in the availability of DAE in Australasian hospitals have been previously reported. In 2008 Eley et al surveyed rural anaesthetists in Queensland and reported a wide variety in the availability and type of DAE10. They recommended the standardisation of equipment across rural hospitals, supported by access to difficult airway workshops delivered in rural areas. An audit of New Zealand metropolitan anaesthetic departments reported deficiencies in DAE and championed the need for quality assurance and implementation of airway guidelines in Australasia11. In Australasia, the ANZCA has made specific recommendations on the availability, storage and quality assurance of DAE8,12. Importantly none of the survey respondents indicated the full availability of DAE as outlined in ANZCA guidelines. The lack of such equipment may make following such guidelines problematic. These results are in stark contrast to a 2009 survey of vocationally registered Fellows of the Australasian College of Anaesthetists (FANZCAs) in Queensland, Australia which reported almost universal availability of DAE trolleys/boxes and 94% satisfaction of respondents with the equipment therein13. Even so, the authors noted that clinical circumstances and patient pathology are often impossible to change, but external factors can be controlled. Such factors include decision-making with respect to an anticipated difficult airway, availability of appropriate equipment, currency in the use of that equipment and access to assistance.
It would seem that the lessons applicable to patients in the care of metropolitan specialist anaesthetic practice do not apply to rural patients and the GPAs who look after them, often in challenging circumstances.
Limitations
It is uncertain how many GPAs there are in Australia, with no record maintained by state-based rural doctor workforce agencies or rural doctor associations. Indeed data are conflicting and incomplete. The JCCA had 122 rural doctors registered in the 2008-2011 triennium for maintenance of clinical standards for anaesthesia, but such registration is not mandatory for GPAs (P Garrad, pers comm, 2012). Data from the Australian College of Rural and Remote Medicine (ACRRM) and the Royal Australian College of General Practitioners (RACGP) indicates 470 and 386 rural doctors, respectively, are enrolled in the Rural Procedural Grants Program (RPGP) for anaesthesia. It is uncertain how many of these are actively providing anaesthetic services in the bush, or the extent of overlap between ACRRM and RACGP enrolments. Medicare Australia declined to provide a statistic for the number of doctors registered for the anaesthetic-component of rural procedural grants in 2012. Although invitations to complete the survey were distributed to doctors on the databases of the RDAA and state Rural Workforce Agencies, it is possible that some GPAs were not invited. The most recent National Rural Health Workforce Minimum Data Set indicates 448 GPAs in RA2-51. Maintenance of a dedicated rural proceduralist database would aid future research into this cadre.
Of 372 survey respondents, 293 identified themselves as a GPAs, the remainder being 'occasional intubators'. The latter were excluded from further analysis as the total number of 'occasional intubators' was unknown, but potentially includes all rural GPs. There are estimated to be over 6000 rural doctors in Australia1 and hence the response rate for 'occasional intubators' was insufficient. Assuming that the Minimum Data Set is reliable, a response rate of 293/448 (65.4%) for GPAs represents a better than expected response for an online survey. Any survey is subject to responder bias, but it is encouraging that the demographics of respondents were representative of the target population, using available published data.
It should be noted that responses were analysed for individuals, not for institutions. There may be duplication in responses for GPAs working in the same hospital, leading to bias in results. However, in a difficult airway crisis it is the GPA who is responsible for ensuring awareness of what equipment is available and the knowledge of how to use it. Hence individual responses are valuable because 'don't know' or 'no' responses are important negatives even if another GPA from the same institution reported otherwise. Put simply, if a doctor thinks that a certain piece of equipment is lacking, or does not know, then it is unlikely to be used in a crisis even if the equipment is available. Further work is recommended in this regard, with either a survey of individual hospitals or an audit driven by the health units themselves.
Clinical implications
Given the potentially catastrophic consequences of a difficult airway, it would seem mandatory for the rural doctor workforce to have access to appropriate equipment and training in difficult airway management, more so when specialist backup is several hundred kilometres or hours away.
The UK's Difficult Airway Society has published recommended algorithms for unexpected difficult intubation in a variety of circumstances, with these algorithms offering alternative plans which require certain equipment6. The DAS guidelines run through four main plans (Plans A, B, C & D) in cases of unexpected difficult intubation. A summary of the DAS plans is presented (Fig1). Importantly the DAS algorithms call for availability of specific equipment for each plan in crisis management.
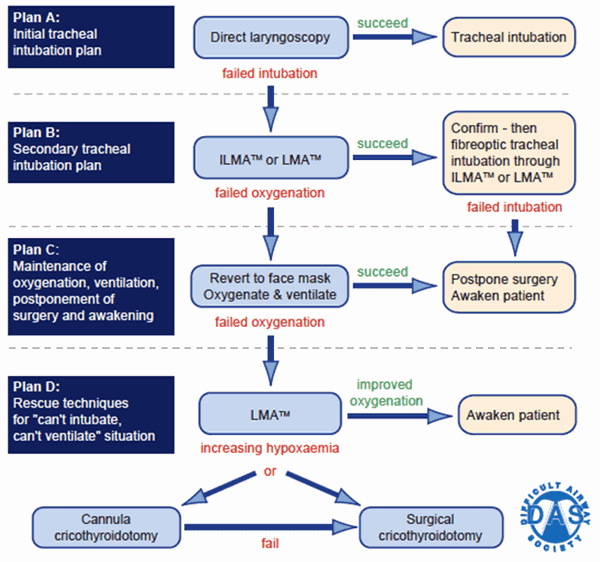
Figure 1: Summary of Difficult Airway Society UK (DAS UK) algorithm for difficult airways. Reproduced with the permission of the Difficult Airway Society (UK).
The DAS algorithms are designed to facilitate a safe approach to difficulties during intubation. Certain categories of equipment are needed for each stage (alternative means of laryngoscopy, classic or intubating laryngeal mask airways, fibreoptic intubation devices and equipment to create a surgical airway and deliver oxygen through it). Difficulties with bag-mask ventilation should also be anticipated and require adjunct equipment such as nasal and oral pharyngeal airways, a means to detect end-tidal carbon dioxide and a means to detect inadvertent oesophageal intubation.
Difficult Airway Society algorithms: Plan A (the initial tracheal intubation plan) allows for up to four attempts at intubation (three in rapid sequence intubation). Each attempt requires changes such as patient position, use of different laryngoscope blade or operator as well as the use of adjuncts, such as stylet or bougie, before announcing failure. Newer devices such as optical or videolaryngoscopes have a role at this stage. Such devices may improve the Cormack-Lehane grade at laryngoscopy, thus making a 'difficult' intubation 'easy'14. Less than 25% of GPAs reported access to an optical (23%) or video (16%) indirect laryngoscope.
Plan B of the DAS algorithm requires an alternative intubation strategy. Devices such as the intubating laryngeal mask airway (iLMA) may allow blind passage of an endotracheal tube. Plan B also refers to fibreoptic intubation through such a conduit allowing greater success than blind passage. It was surprising that 18% of respondents had access to a flexible fibreoptic scope for intubation, given the relative expense of such items compared with other equipment (units are typically in the tens of thousands of dollars). However only 11% of those with access to fibreoptic scopes would be confident to use in an emergency, with 58% stating they were not confident to use in either elective or emergency situations. The ANZCA guidelines for difficult airway management also include reference to availability of fibreoptic intubation. It may appear hard to reconcile DAS and ANZCA guidelines with respondents lack of access to such equipment and the reluctance to use in any but elective cases. However it must be appreciated that fibreoptic intubation is considered an advanced skill and is mainly used to facilitate awake intubation for an anticipated difficult airway. It is likely that GPAs, with a relatively low caseload and training that is necessarily abridged, would not be experienced in fibreoptic use. One can argue that it is prudent for GPAs to avoid this technique and for resource-limited rural hospitals to consider investment in other less expensive equipment. While this is certainly true for the majority of GPAs who would never consider an awake fibreoptic intubation, the use of a fibreoptic device to allow intubation through an iLMA conduit is a relatively simple technique and could be employed by GPAs.
Plan C is utilised when intubation attempts have failed and emphasises the importance of the maintenance of oxygenation and awakening of the patient. Suxamethonium is the agent of choice to induce paralysis in an RSI (unless a contraindication exists) due to its relative short duration of action, thereby affording the possibility of patient regaining spontaneous ventilation within minutes. Rocuronium, an aminosteroid neuromuscular blocker, may be used as an alternative to suxamethonium, giving similar rapid intubating-conditions at a dose of 1.2 mg/kg. The longer duration of rocuronium poses a hazard if the airway cannot be secured as the patient will not regain spontaneous ventilation for many tens of minutes. However its effects can be reversed with suggamadex, allowing use of rocuronium for RSI with a faster onset-offset profile than traditional suxamethonium. Only 23% of respondents reported availability of suggamadex, with the remainder either not knowing (11%) or reporting unavailable (66%). This may reflect practice patterns (hospitals not using rocuronium would not need to carry suggamadex, although it also reverses the effects of vecuronium, another aminosteroid neuromuscular blocker). Given the increasing use of rocuronium in cases where suxamethonium is contraindicated, a similar increase in use of suggamadex by GPAs could be advocated. Financial constraints may be an issue.
The DAS algorithm does not specifically address the issue of a failed rapid sequence intubation in a patient where awakening is not an option (eg head injury with loss of protective airway reflexes in a remote clinic requiring intubation and retrieval), other than suggesting progression to Plan D (rescue techniques for 'can't intubate, can't ventilate'). Some retrieval experts, recognising the significant differences between elective and emergency intubation, have advocated the use of rocuronium for such intubations, on the basis that waking the patient is not an option and longer duration of paralysis will aid attempts to secure the airway. If passage of an endotracheal tube is impossible, use of an LMA as a conduit for fibreoptic intubation with either malleable stylet or flexible scope may offer a valid rescue technique (M Le Cong, pers comm, 2012). This may be a lifesaving manoeuvre for isolated rural GPAs when the airway of a critically unwell patient must be secured without access to specialist help and where awakening is not an option, without progression to the psychologically-challenging creation of a surgical airway. Relatively simple and low cost fibreoptic intubation devices are available and may be realistic adjuncts to allow intubation through a LMA in such situations14. These are discussed below.
Plan D calls for the rapid establishment of a surgical airway. Thankfully this crisis is rare, with the 'cannot intubate, cannot ventilate' (CICV) scenario occurring in 1:10 000 elective anaesthesia cases, but higher in other situations such as emergency airway management (P Baker, pers comm, 2012). No accurate data are available for the incidence of CICV in Australia, nor for incidence of CICV in the rural GPA setting. Unfortunately, problems with CICV have been noted in Coronial reports and yet a modicum of preplanning and provision of simple equipment can be lifesaving in this emergency.
Despite the relative infrequency of a CICV crisis, rural GPAs with their responsibility for frontline emergency care and without immediate access to specialist backup, may be unfortunate enough to encounter this scenario on rare occasions and will be required to manage it appropriately. Two main techniques are recommended, either needle or surgical cricothyroidotomy. Further discussion of the merits of either is beyond the scope of this paper, but suffice it to say such procedures require ready access to both equipment, well-briefed personnel and familiarity with the techniques involved15. The fact that only 19% of GPAs had a dedicated needle cricothyroidotomy kit and 79% a surgical kit begs the question as to whether GPAs and supporting staff are truly prepared for the infrequent but critical CICV crisis.
The DAS plans relate specifically to difficult intubation and CICV situations. It should be noted that difficulties may be encountered with bag-mask ventilation, with insertion and ventilation via supraglottic devices, or with misplacement of the endotracheal tube. Adjunct devices such as oro- and naso-pharyngeal airways, supraglottic devices such as laryngeal masks and the combitube, as well as means to detect end-tidal CO2 and to detect inadvertent oesophageal intubation are invaluable. The vast majority of GPAs reported that simple adjuncts such as bougie, stylet, classic LMA and end-tidal CO2 monitoring were available to them, which is reassuring. Very few had access to an oesophageal detection device or combitube. All of these adjuncts are relatively cheap and valuable aids in airway management.
Access to equipment and training: Responses from GPAs indicated that they did not enjoy access to the same range of anaesthetic paraphernalia as one might expect in a tertiary centre. Availability of items such as suggamadex (to reverse rocuronium) and intralipid (to treat local anesthetic toxicity) were reported by less than 40% of respondents. The GPAs reported similar rates for access to desflurane, remifentanil and BIS (bispectral) monitoring, although the need for these will be determined by case mix. Access to blood products is always problematic in rural areas, with it impractical to store blood and blood products in smaller centres, particularly those without general surgery capabilities. Reassuringly 75% of GPAs reported access to a fluid warmer, which may go at least some way to avoiding hypothermia in cases of major transfusion. Only 21% of GPAs reported access to intravenous tranexamic acid, a relatively cheap adjunct for initial management of major haemorrhage in trauma. There was no correlation with the availability of these items and state or ASGC-RA.
The majority of GPAs had been able to access upskilling in the previous 12 months, whether via a course/conference, clinical attachment or both. Of courses attended in the previous 3 years, EMST, APLS and REST courses were most represented. None specifically addresses difficult airway management in depth, although the EMST provider course does offer a chance to practice surgical techniques including scalpel cricothyroidotomy on an animal model. Forty-four percent of respondents had accessed a difficult airway course in previous three years. Comments suggested difficulties in organising locum relief and the need for interstate travel for such courses. There may be scope for locally delivered high-fidelity courses targeted at GPAs in the future, although it was encouraging that 86 respondents had accessed a course delivered in their home state.
Prehospital care: Involvement in prehospital care was reported by 58% of GPAs. Looking to models overseas, the British Association for Immediate Care Scheme (BASICS) enlists doctors with such skills to support paramedics in the prehospital environment, even though transport times and population densities in the UK are more favourable than in Australia16. New Zealand has a similar scheme (Primary Response In Medical Emergencies, PRIME) for rural doctors17. Criticism has been levelled at metro-centric 's-emergency plans' that rely on retrieval services and overlook local rural doctors with procedural skills, such as the Kerang train crash disaster in rural Victoria18. While recognising that the experts in prehospital medicine are trained paramedics and retrievalists, it seems that rural doctors are being called to respond to such incidents, but such responses are ad hoc and without appropriate training. In Australia there are well-documented difficulties for rural patients with critical injuries to enter into a system of care in a timely manner19.
There is scope in Australia to utilise GPAs, with skills in airway management and resuscitation, as a coordinated response. Any such scheme would require appropriate training, equipment and audit. However, such schemes exist in the UK and New Zealand and would seem intuitively suited to Australia where population densities are low, paramedics may be volunteers without advanced airway skills, and distance for the retrieval service to travel may be long.
Suggestions for rural anaesthetists
Given the distances involved to specialist care and the high likelihood of GPAs being required to manage difficult airways with no back-up, it would seem mandatory for rural hospitals to ensure the availability of and training in appropriate equipment. It is difficult to reconcile the fact that none of the survey respondents had access to DAE as outlined by ANZCA.
Concordance between rural hospitals in DAE would facilitate ease of use by locums and retrieval service, as well as affording an economy of scale in the purchase, maintenance and cycling of stock. Any equipment purchased should be resilient, affordable, appropriate for use in the rural environment and preferably standardised. A difficulty is that such equipment is infrequently used and historically has been expensive to purchase, something which cash-strapped rural hospitals may be likely to question. Such equipment may also require special training both for initial skills acquisition and for maintenance.
Unfortunately there is no single 'magic' device to guarantee successful management of the difficult airway. The plethora of devices available and their individual 'quirks' means that selection of DAE can be problematic, although 'hands-on' experience via difficult airway courses can be invaluable. One caveat is that possession of a variety of devices may detract from key skills of maintaining oxygenation, ventilation and avoiding trauma to the airway. One astute responder noted that good familiarity with a small range of commonly used options is much more efficient and safer to organise/find/assemble/replace/troubleshoot than a supermarket shelf full of 'toys' from the sales representatives. Although it is true that airway complications are relatively infrequent, the consequences of mismanagement can be catastrophic. One respondent noted that it took four years and neonatal death to get decent anaesthetic monitoring and established procedures for failed intubation in their rural hospital.
New airway devices are available, putting both videolaryngoscopy and fibreoptic intubation within reach of rural GPAs and 'occasional intubators' for a modest budget of under $4,000. Regular training with such equipment on elective lists, cost-sharing and standardisation between health units and rigorous equipment selection guided by end-users would facilitate their ease of use in an emergency.
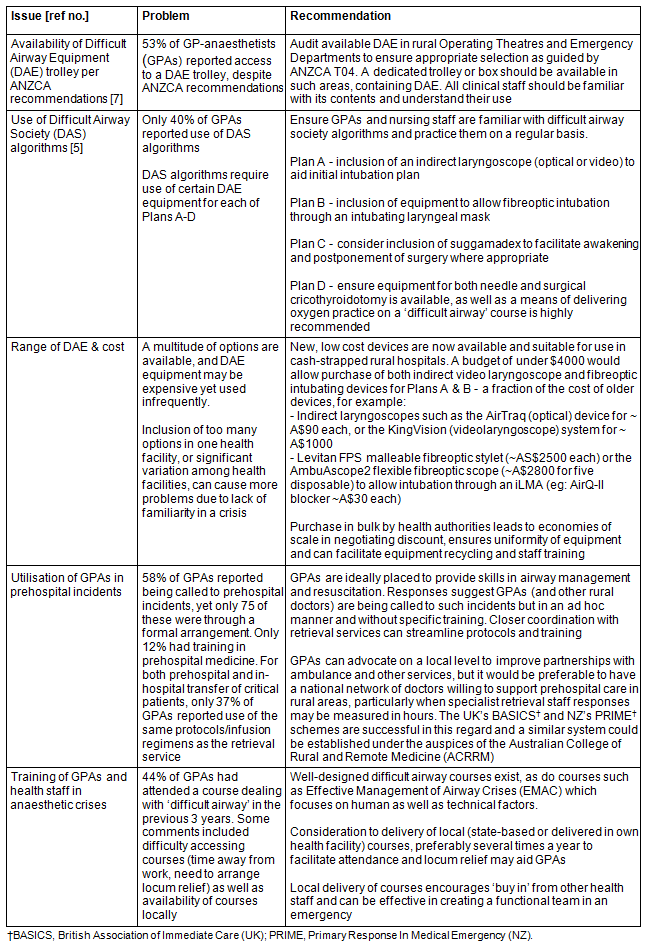
A pragmatic approach is outlined (Table 4) to the problems of DAE and related issues for rural GPAs and health administrators when trying to balance cost against necessity.
Table 4: Recommendations for rural GP-anaesthetists and rural hospitals in Australia6,8
In addition to the availability of DAE, equal importance should be placed on understanding the human factors in airway crisis management. It is no use having DAE if healthcare staff do not know where to find it, how to use it, and have not received training in airway crisis management. There is potential for locally delivered courses aimed not just at GPAs, but also associated health staff, particularly nursing staff, in rural operating theatres and emergency departments.
It should be remembered that any rural doctor providing emergency care may be called upon to manage the airway, more so in areas where GPAs are not immediately available. It behoves all rural doctors working in such environments to be familiar with airway management, with DAS algorithms and DAE. Similarly, health authorities must ensure that appropriate equipment and staff training is in place wherever an airway may need to be managed. The availability of newer devices makes this a realistic possibility, although the abundance of choice may seem overwhelming and cause confusion. Standardisation of equipment and training will be key, ideally with expert commentary guiding concordance in the selection of DAE between rural hospitals and the retrieval services that service them.
Despite the existence of well-publicised algorithms for difficult airway management and the need for specific equipment to manage the difficult airway, Australian GPAs report difficulty accessing essential equipment for these infrequent but life-threatening events. This is surprising in light of recommendations from the Australian and New Zealand College of Anaesthetists. The consequences of difficulty in airway management can be catastrophic. Equipment needs must be balanced against important considerations including ease of use, initial and ongoing training, and cost. Suggestions for affordable equipment and ongoing training for rural GPAs are made. The involvement of GPAs in prehospital responses occurs in the absence of formal arrangements and with a dearth of training. There is scope to improve rural prehospital responses in Australia, utilising the advanced skills of GPAs in resuscitation and airway management.
Acknowledgments
The author acknowledges the advice of Dr Paul Baker (FANZCA, New Zealand) and Dr Minh le Cong (FACRRM, Royal Flying Doctor Service, Queensland) for background information in the preparation of this manuscript. Pam Garrad (JCCA), Pauline Curtis (RACGP) and Mark Knibbs (ACCRM) are thanked for attempting to clarify the number of GP-anaesthetists in Australia. The Rural Doctors Association of Australia and the individual state Rural Doctor Workforce Agencies of Queensland, New South Wales, Victoria, Western Australia, Tasmania and the Northern Territory kindly forwarded survey invitations to rural doctors on their membership lists.
References
1. Health Workforce Queensland and New South Wales Rural Doctors Network. Medical practice in rural and remote Australia: Combined Rural Workforce Agencies National Minimum Data Set report as at 30th November 2010. (Online) 2010. Brisbane, QLD: Health Workforce Queensland. Available: http://web.healthworkforce.com.au/downloads/Publications/MDS%20Report%202010_National_2010.pdf (Accessed 1 February 2012).
2. ANZCA. Strategic Plan. (Online) no date. Available: http://www.anzca.edu.au/ (Accessed 25 September 2012).
3. Kheterpal S, Martin L, Schanks AM, Tremper KK, Wong E, Ng Y-Y. Prediction and outcomes of impossible mask ventilation: a review of 50,000 anaesthetics. Anesthesiology 2009; 110: 891-897.
4. Wong E, Ng Y-Y. The difficult airway in the emergency department. International Journal of Emergency Medicine 2008; 1(2): 107-111.
5. Cook TM, Woodall N, Frerk C.Fourth National Audit Project. Major complications of airway management in the UK: results of the Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society. Part 1: anaesthesia. British Journal of Anaesthesia 2011; 106: 617-631.
6. Henderson J, Popat MT, Latto IP, Pearce AC, Difficult Airway Society. Difficult Airway Society guidelines for management of the unanticipated difficult intubation. Anaesthesia 2004; 59(7): 675-694.
7. Australian and New Zealand College of Anaesthetists. T01 Recommendations on minimum facilities for safe administration of anaesthesia in operating room suites and other anaesthetising locations. (Online) 2008. Available: http://www.anzca.edu.au/resources/professional-documents/t1.html (Accessed 1 January 2012).
8. Australian and New Zealand College of Anaesthetists. Ps56 Guidelines on equipment to manage a difficult airway during anaesthesia. (Online) 2012. Available: http://www.anzca.edu.au/resources/professional-documents/documents/professional-standards/pdf-files/PS56-guidelines-on-equipment-to-manage-a-difficult-airway-during-anaesthesia.pdf (Accessed 6 October 2012).
9. Shiga T, Wajima Z, Inoue T, Sakamoto A. Predicting difficult intubation in apparently normal patients: a meta-analysis of bedside screening test performance. Anesthesiology 2005; 103: 429-437.
10. Eley V, Lloyd B, Scott J, Greenland K. Availability of difficult airway equipment to rural anaesthetists in Queensland, Australia. Rural and Remote Health 8: 1020 (Online) 2008. Available: www.rrh.org.au (Accessed 19 September 2012).
11. Baker PA, Hounsell GL, Futter ME, Anderson BJ. Airway management equipment in a metropolitan region: an audit. Anaesthesia and Intensive Care 2007; 35: 563-569.
12. Baker PA, Flanagan BT, Greenland KB, Morris R, Owen H, Riley RH et al. Equipment to manage a difficult airway during anaesthesia. Anaesthesia and Intensive Care 2011; 39: 16-34.
13. Zugai, BM, Eley, V, Mallitt, KA, Greenland, KB. Practice patterns for predicted difficult airway management and access to airway equipment by anaesthetists in Queensland, Australia. Anaesthesia and Intensive Care 2010; 38(1): 27-32.
14. Timmermann A. Supraglottic airways in difficult airway management: successes, failures, use and misuse. Anaesthesia 2011; 66(Suppl2): 45-56.
15. Paix BR, Griggs WM. Emergency surgical cricotyyroidotomy: 24 successful cases leading to a simple 'scalpel-finger-tube' method. Emergency Medicine Australasia 2012; 24: 23-30.
16. British Association for Immediate Care (BASICS UK). Home page. (Online) no date. Available: http://www.basics.org.uk (Accessed 1 February 2012).
17. Hore T, Coster G, Bills J. Is the PRIME (Primary Response In Medical Emergencies) scheme acceptable to rural general practitioners in New Zealand? Journal of the New Zealand Medical Association 2003; 116(1173): 420.
18. Anon. Kerang medics ignored. The Age, 14 July 2011. (Online) 2011. Available: http://www.theage.com.au/victoria/kerang-medics-ignored-20110713-1hebl.html (Accessed 1 February 2012).
19. Fatovich DM, Phillips M, Langford SA, Jacobs IG. A comparison of metropolitan vs rural major trauma in Western Australia. Resuscitation 2011; 82: 886-890.
