The provision of procedural services by general practitioners (GPs) and hospital-based generalist doctors has been and remains an essential component of medical service delivery in rural and remote Australia1,2. However the number of rural GPs offering procedural services and the complexity of these services has been in gradual decline over the last three decades1-5. The reasons for this decline are multiple and include: increasing specialisation, centralisation of services, inadequate caseload, staff shortages, access to and expense associated with continuing medical education and locum relief, credentialing processes, fear of litigation and insurance expenses, family and social considerations and an ageing rural workforce1,5-7.
Few studies have looked at the issues directly relevant to recently qualified GPs, and how these impact on the use of procedural skills. Anecdotal reports in Australia suggest that a large proportion of doctors leave procedural practice soon after training, moving into either non-procedural rural general practice or undertaking alternative specialist training. A postal census of obstetrics-trained GPs in Victoria found that 31% had never been involved in procedural obstetric practice, 49% had previously provided procedural services, and only 20% were currently involved in procedural practice8. Experience has also suggested that if training is not immediately followed by a year of procedural consolidation with appropriate mentoring and support in a rural area, the risk of losing confidence and skills is high. There is concern that once doctors stop providing procedural services they are unlikely to recommence2.
Advanced Rural Skills Training (ARST) allows a general practice registrar or Rural Generalist to broaden their skills and capacity beyond the normal scope of general practice training. Advanced Rural Skills Training is also known as Advanced Specialised Training; however, for brevity the former term will be used throughout this article. The training may be procedurally based (allowing for credentialing within rural hospitals) such as anaesthetics, emergency medicine, obstetrics and gynaecology or surgery9. The skills may also be non-procedural, such as Aboriginal and Torres Strait Islander health, internal medicine, mental health, paediatrics, population health or remote practice9. An Advanced Specialised Training year is a required component of the Australian College of Rural and Remote Medicine (ACRRM) training program and an ARST post is an optional addition for the Royal Australian College of General Practitioners (RACGP) program3. These both involve 12 months in an accredited training post with additional curriculum content, experience and assessment that can be undertaken at various times within these training programs9.
With recent increases in ARST posts, increasing numbers of doctors joining the Rural Generalist Pathway (Queensland Health) and a continuing deficit of rural GPs, it is timely to investigate the outcomes of ARST. This project aimed to:
- describe where GPs practice in the 5 years after ARST
- describe the proportion of doctors using their advanced rural skills
- measure doctors' ratings of the quality of support and how critical the year directly following training is in future career choices
- measure the association between support and use of advanced rural skills.
A cross-sectional, postal survey of all doctors who had completed ARST in Queensland between 1995 and June 2009, was designed. General practice colleges (RACGP and ACRRM), the three Queensland regional training providers and one national training provider were approached in order to identify eligible doctors. Data were collected on a three-page, structured questionnaire which was mailed either directly by the training providers or by the research team (where access to names and addresses of potential participants was provided). Questionnaires returned because of incorrect address were (where possible) re-addressed and posted by Health Workforce Queensland. One reminder questionnaire was sent to each eligible doctor approximately 2 weeks after the initial mailing. Two training providers declined to mail the questionnaires but did provide the number of their registrars who had completed ARST. An electronic version of the questionnaire was established and advertised in an RACGP newsletter to increase the response rate.
Participants were asked about their practice history (location, type of organisation, use of advanced rural skills) in the 5 years directly following their most recently completed ARST post. Advanced rural skills training was classified as 'single procedural' (completion of one procedural ARST post), 'single non-procedural', 'multiple procedural' (completion of two or more procedural ARST posts) or 'multiple mixed' (one or more procedural and one or more non-procedural ARST posts). Use of advanced skills was determined via a combination of self-report and research team assessment. 'Not using skills' was coded where advanced procedural skills were only being used in emergencies or limited to skills reasonably expected to be practiced by a GP without ARST. 'Occasional use of skills' was self-reported.
Location was coded using the Rural, Remote, Metropolitan Area (RRMA) seven-point classification system (www.aihw.gov.au). Attitudinal questions about quality of support and how critical the year directly following training is in future career choices, were rated on a five-point rating scale. Descriptive statistics were prepared for practice history information and attitudinal ratings. A χ2 test was used to analyse the association between support and use of skills. SPSS v17.0 software was used for data analysis (www.spss.com).
Ethics approval
Ethical approval for the study was granted through the James Cook University Human Research Ethics Committee (#H3424).
Response rate, Advanced Rural Skills Training and current practice
Information supplied by colleges and training providers indicated that 118 doctors were eligible to be included in the study. Sixty-one completed questionnaires were returned resulting in a response rate of 51.7%, unadjusted for those who did not receive a questionnaire.
Respondents had completed a range of procedural and non-procedural training posts and these are tabulated (Table 1). Some respondents (15, 24.6%) had completed two or more posts. The most common posts were: obstetrics and gynaecology (23, 37.7%), anaesthetics (11, 18%), the combination of anaesthetics and obstetrics and gynaecology (7, 11.5%) and Aboriginal and Torres Strait Islander health (7, 11.5%). Six respondents (9.9%) had or were currently undertaking training with another specialist college. This was generally, but not always, similar to their ARST.
The majority (37, 60.6%) were using skills related to their ARST at the time of study and an additional 2 (3.3%) were using these skills occasionally. The remainder were not using their advanced rural skills. The percentage of respondents currently using their skills within each type of ARST is given (Fig1). Those who had completed a single non procedural (9, 90%) or multiple procedural posts (7, 70%) were more likely to be currently using their skills compared with those who had completed a single procedural (21, 58.3%) or multiple mixed training posts (2, 40%). Of those currently using their skills, 31 (81.6%) were practicing in a location classified as RRMA 4-7. In comparison, 11 (50%) of those not using their skills were located in a RRMA 4-7 location.
Table 1: Type of Advanced Rural Skills Training completed by respondents
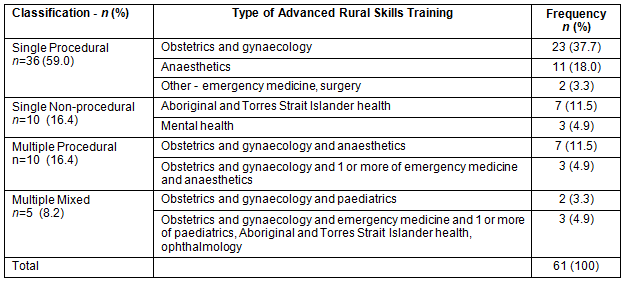

Figure 1: Current use of skills within type of Advanced Rural Skills Training (ARST).
Practice history and use of advanced skills
All respondents had practice history for at least one year after training. Fifty-eight respondents had 2 years of practice history, 49 had 3 years, 40 had 4 years and 36 (59%) had practice history for a full 5 years after training. The most common organisations in which respondents practice during the first 5 years after ARST (Y1-Y5) were: public hospital (including primary health care & specialty clinics); private general practice; a combination of public hospital and private general practice; remote flying services; and Aboriginal Medical Services. Other organisation types included: private hospital; private general practice sub-specialty; university; and non-government organisations. The percentage working in public hospitals declined gradually from 27 (44.3%) in the first year after training (Y1) to 9 (25.7%) 5 years after training (Y5) (Fig2). In comparison, the percentage working in private general practice (Y1 = 12, 19.7%; Y5 = 10, 28.6%) and remote flying (Y1 = 4, 6.5%; Y5 = 5, 14.3%) increased over the first 5 years after training.
In the first year after training 8 (13.1%) worked in large rural centres (RRMA 3), 5 (8.2%) in small rural centres (RRMA 4), 16 (26.2%) in other rural areas (RRMA 5), 7 (11.5%) in remote centres (RRMA 6), 17 (27.9%) in other remote areas (RRMA 7) and the remainder (8, 14.1%) in various locations or 'overseas'. Other remote areas (RRMA 7) were the most common location of practice in the first 5 years after training and this was closely followed by other rural areas (RRMA 5).
There was a decreasing percentage of doctors using their advanced skills over the 5 years directly following training, with a large decrease at year one (Y1) and then gradual decreases from year three (Y3) (Fig3). In the first year after training 46 (75.4%) doctors used their skills (either regularly or occasionally), this remained steady at 45 (77.6%) in Y2 and then decreased to 35 (71.4%) in Y3, 27 (67.5%) in Y4 and 22 (61.1%) in Y5. In the first 5 years after ARST, eight respondents (13.1%) returned to procedural practice after ceasing practice for at least one year. In every case this coincided with a move to a more rural or remote setting. Among those with practice history for the full 5 years after training, 16 (44.4%) used their skills continuously, 15 (41.7%) used their skills in some but not all years, 5 (13.9%) never used their skills.
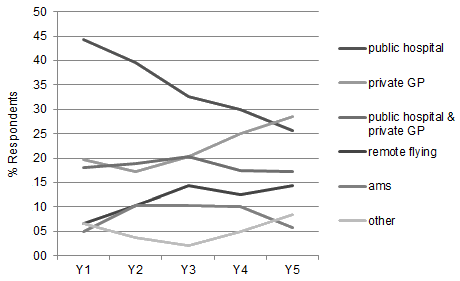
Figure 2: Type of organisation after Advanced Rural Skills Training.
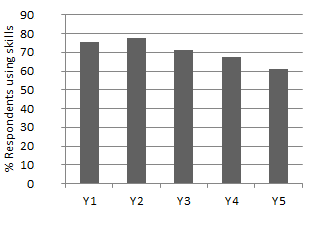
Figure 3: Use of advanced rural skills after Advanced Rural Skills Training.
Ratings of the year directly following training
The year directly following ARST was rated as 'very critical' in their future career choices by 25 (41%) respondents and as 'critical' by 17 (27.9%) respondents. Eight (13.1%) rated the first year as 'moderately critical' and 11 (18%) as 'slightly critical' or 'not at all critical' to future career choices.
Ratings of the quality of support received in the year directly following ARST were not normally distributed. There were peaks at both 'very good support' (13, 23.2%) and 'very poor support' (12, 21.4%); however, almost half (26, 46.4%) rated the support they received as either 'good' or 'very good'.
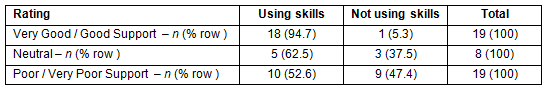
There was a statistically significant association between ratings of support in the year directly following training and whether doctors were using their skills 3 years after training (χ2 = 8.715, df = 2, p = 0.013). Doctors were more likely to be using their advanced rural skills 3 years after training if they had reported 'good' or 'very good' support in the year directly following training, compared with those who reported poor support (Table 2).
Table 2: Rating of support in Y1 and use of Advanced Skills in year 3
Discussion
This study has shown that almost two-thirds of GPs who have completed ARST in Queensland are currently using their advanced rural skills. This figure is much higher than that reported by Loy et al among obstetric-trained GPs8. However these studies are not directly comparable because of the inclusion of all ARST options (including non-procedural), differences in State healthcare systems and possible under-representation of those who have moved to metropolitan areas. However, both studies show a reduction in use of skills starting directly after training8. Overall the reduction in use of advanced rural skills in the first 5 years roughly matched the movement of the majority from public hospital practice into private general practice and remote flying practice. This pattern is reflective of the divide between public and private services in Queensland's healthcare system.
This study also confirms the critical nature of experiences in the year directly following ARST in future career decisions and use of advanced skills. It is concerning therefore that over one-third of trainees experienced 'very poor' or 'poor' support. Strategies to formalise or ensure support in this 'consolidation year' are needed to improve this situation, especially for procedural doctors.
One-quarter of recently qualified GPs did not use their skills in the year directly following training. Possible reasons include: lack of intention to practice, inadequate career planning, mismatch between practice type or location and ARST, timing of ARST within broader general practice training means skills cannot be used immediately. It seems essential that doctors receive support as a continuum before, during and after training.
Encouraging doctors to rejoin the procedural rural workforce has been suggested as a solution to current workforce shortages8,10. Findings from this study provide some hope that this is possible, especially among those recently qualified and with appropriate support and supervision. Systems to allow ongoing identification of doctors with ARST would be essential to enable this re-engagement and could possibly occur through an independent peer network or alumni, or through a collaborative arrangement between the RACGP and ACRRM. It would also allow monitoring of training outcomes, peer mentoring, provision of ongoing support and implementation of workforce strategies.
This study of outcomes from advanced rural skills training in Queensland has shown that the majority of GPs and Rural Generalists are using their advanced procedural and non-procedural skills. However, based on the experiences of recently qualified doctors, there is room for improvement using strategies such as:
- training and career planning support to ensure the progression of advanced trained doctors directly into an appropriate practice after training
- extending formal support mechanisms into the first year after training
- improved opportunities to practice advanced skills, including addressing the divide between public and private sectors
- opportunities and systems to encourage doctors to re-engage and re-skill in advanced procedural or non procedural practice could be implemented by colleges, training providers and health departments to help support recently qualified GPs in using their advanced rural skills.
Acknowledgements
The authors acknowledge the Rural Generalist Pathway Program, Queensland Health for providing the funding for this project. They also acknowledge Ms Catherine Sharpe, Research Assistant, for her role in data collection and analysis. Dr Denis Lennox and A/Prof Tarun Sen Gupta provided assistance in project design.
References
1. Robinson M, Slaney GM, Jones GI, Robinson JB. GP proceduralists: 'the hidden heart' of rural and regional health in Australia. Rural and Remote Health 10: 1402. (Online) 2010. Available: www.rrh.org.au (Accessed 2 December 2011).
2. Australian College of Rural and Remote Medicine. Barriers to the maintenance of procedural skills in rural and remote medicine. Brisbane, QLD: Australian College of Rural and Remote Medicine Research Project, 2002.
3. Campbell DG, Greacen JH, Giddings PH, Skinner LP. Regionalisation of general practice training - are we meeting the needs of rural Australia? Medical Journal of Australia 2011; 194(11): S71-74.
4. Pashen D, Murray R, Chater B, Sheedy V, White C, Eriksson L et al. The expanding role of the rural generalist in Australia - a systematic review. Brisbane, QLD: Australian College of Rural and Remote Medicine, 2007.
5. Stratigos S, Nichols, A. Procedural rural medicine: strategies towards solutions. Kingston, ACT: Rural Doctors Association of Australia and Australian College of Rural and Remote Medicine, 2002.
6. Glazebrook RM, SL Harrison. Obstacles to maintenance of advanced procedural skills for rural and remote medical practitioners in Australia. Rural and Remote Health 6: 502. (Online) 2006. Available: www.rrh.org.au (Accessed 2 December 2011).
7. Davie MJ. General practitioner anaesthesia survey 2006. Anaesthesia and Intensive Care 2006; 34(6): 770-775.
8. Loy CS, Warton RB, Dunbar JA. Workforce trends in specialist and GP obstetric practice in Victoria. Medical Journal of Australia 2007: 186 (1): 26-30.
9. General Practice Education and Training Limited. Australian General Practice Training. Guide for GP Registrars 2009. Canberra, ACT: General Practice Education and Training Limited, 2008.
10. Willcock SM. Getting back into the emergency department: diversifying general practice while relieving emergency medicine workforce shortages. Medical Journal of Australia 2008; 189 (2): 113-114.



