Attracting, training and retaining GPs in rural communities has long been the subject of intense interest and concern in medical and political circles. Indeed, there has been much research into determining the career intentions of Australian-trained doctors to work in rural locations1,2. Moreover, government reviews and policy decisions, including the decentralisation of GP training and the ten-year moratorium (a strategy to place overseas-trained doctors in rural locations) have attempted to address GP training and chronic rural and remote workforce shortages3-7.
In an environment of continuing GP shortages in rural Australia, this study examined whether the decentralised model of GP training results in the retention of doctors in rural areas. Specifically, the study explored the influence of the decentralised model of GP training on the retention of 61 doctors who trained with Bogong Regional Training Network (BRTN) in rural locations in North-east Victoria and southern New South Wales between 2004 and 2009. While this preliminary work provides a snapshot of retention rates of doctors in the Bogong region, it also forms part of a longitudinal study that is tracking the location of doctors trained by the BRTN over a longer timeframe.
Decentralised model of GP training
In 1998, the then Minister for Health Michael Wooldridge initiated a ministerial review of GP training. Central to that review was continuing concern about the serious doctor shortfall in rural and remote Australia and the need to prioritise medical vocational training. In particular the review noted the Government's concern about a '...chronic undersupply of rural doctors' in all states and territories8.
After wide industry and community consultation, the review noted that GPs and expert stakeholders were calling for substantial changes in the way GP training was managed and delivered8. It recommended dissolution of the centralised Royal Australian College of General Practitioners (RACGP) model of training in favour of a decentralised approach that would attract GPs to rural areas and therefore foster greater equity of provision of medical services in rural Australia.
In 2001 General Practice Education and Training (GPET) was formed to manage GP training via a consortium of 21 regional training providers (RTPs)9. The RTPs began delivering training to GP registrars in 200410. Between 2004 and 2009, 1610 Australian medical graduates and 564 international medical graduates became fellows of the RACGP through GPET (GPET; pers. comm; 2010). Of these, 61 GP registrars completed their training with BRTN and 57 of this group gained their RACGP Fellowship (the remaining four were awaiting fellowship when this study was conducted).
Ten-year moratorium
Introduced in 1997, the moratorium was an attempt to reduce a perceived oversupply of generalist doctors in metropolitan areas11. This amendment to the Health Insurance Act 1973, denied international medical graduates and some overseas-born, Australian-trained doctors access to a Medicare provider number and, therefore, access to government funded rebates, except under certain circumstances12. However, in order to address a serious doctor shortage in rural and regional Australia, exemptions to Section 19AB of the Act enabled these doctors to claim Medicare rebates provided they completed an accredited GP training program and practised in a designated 'area of need' or place of workforce shortage for a period of up to 10 years13,14. As a result, doctors who migrate are more likely than non-medical migrants to locate in regional and rural areas15. In 2002 there were 1303 international medical graduates with 'Section 19AB exemptions'16, and in 2010 there were 657617.
Data from the Interactive Registrar Information System (IRIS), the GP Registrar Information Management and Education system (GPrime) and paper files were used to construct a comprehensive socio-demographic profile of former registrars.
Semi-structured telephone and face-to-face interviews were conducted with GPs to explore career path decisions. Semi-structured interviews allowed the flexibility to explore different circumstances of sub-sets of respondents. The data were analysed to identify and more closely examine emergent themes associated with GP career decisions.
Of 61 prospective interviewees, current practice addresses were found for 51 doctors. The remaining 10 doctors could not be contacted by phone or email. Practice managers were contacted by telephone and the research project explained. 'Invitations to participate' were then sent to each doctor and follow-up phone calls made to liaise with practice managers to schedule interview times. In June and July 2009, 27 of the 51 doctors contacted agreed to participate in 10 min telephone interviews. Three additional doctors participated in individual, one-hour, face-to-face interviews to further explore themes of interest. Each doctor was offered a small honorarium for participating. Interviews were conducted with 30 of the total of 51 doctors contacted, a response rate of 58.8%.
Ethics approval was not obtained for this study because the data upon which the analysis is based formed part of a routine quality control process for the BRTN. Participation was voluntary and participant anonymity was assured.
Population profile
More than 36% (n=22) of the doctors in the study were Australian-born, none of whom identified as Aboriginal or Torres Strait Islander. The remaining 64% (n=39) were born overseas (Table 1), principally in Bangladesh, Iraq, Malaysia, China and India, reflecting the national migration trend data of overseas trained doctors in Australia18.
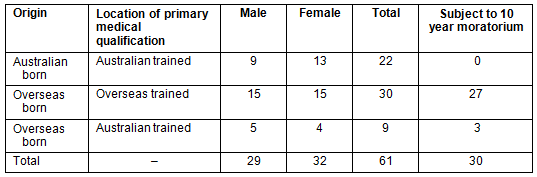
A total of 52% of doctors in the study were women and more than 80% of the doctors were aged between 30 and 44 years, the remainder being between 45 and 56 years. All Australian-born doctors and nine overseas-born doctors gained their primary medical qualifications in Australia (Table 1). Almost 72% (n=28) of overseas-born doctors gained their primary medical qualification in their country of origin. Of a total of 30 international medical graduates, 25 were subject to the ten-year moratorium. Three of the nine overseas-born, Australian medical graduates were also subject to the moratorium.
Table 1: Birth location, location of primary medical qualification, gender and moratorium status
At the end of 2009, more than 42% (n=24) of the 57 GPs who had completed their vocational training remained in rural general practice, 32% (n=18) in the Bogong region. Of the remaining 58% (n=33), 19 doctors were practising in inner metropolitan areas and seven were located in suburbs more than 25 km from the centre of a capital city. One doctor was living rurally but not practising medicine, and six individuals were unable to be located (Table 2).
The results of this study show that there was a statistically significant relationship between a doctor's country of birth and remaining in rural practice, with almost three-quarters (73% n=16) of the Australian-born respondents and almost one-quarter (23% n=8) of the overseas-born respondents remaining in rural practice after fellowship (χ² = 13.68 p<0.001).
Table 2: Location of GPs in 2009

Of the nine overseas-born, Australian-trained medical graduates, only one remained in rural practice and of the 26 doctors subject to the moratorium who had completed their vocational training, only 27% (n=7) stayed in rural practice (data not shown).
Most doctors who stayed in rural practice after fellowship generally remained in or near one of the towns in which they had completed a placement or where they had completed extended or advanced skills training.
What brought them to rural practice?
The majority of the Australian-born doctors in this study chose rural practice because they or their partners had experienced rural or semi-rural environments and were familiar with rural culture and a rural lifestyle. Some were influenced by having a spouse with a rural background, familial connections or opportunity for spouse employment:
He coaxed me to move up to the country with him. ...I said to my husband, that if I hated it we will have to go back, or if I missed my family too much but it worked out well and we are...planning to stay here permanently. (Australian-born GP)
Others had chosen to embark on rural practice long before they completed their registrar training. For some it was part of a long-term plan and, importantly, their choice was influenced by the type of medicine practised:
I came here, because of...the procedural hospital work, the emergency work, the orthopaedic work. ...It all seemed like a really exciting job. (Australian-born GP)
For the overseas-born cohort, the training location was primarily determined by the requirements of the ten-year moratorium. Many of the overseas-born doctors were from urban backgrounds; were unfamiliar with rural life or rural general practice and typically had little knowledge of the Bogong region. For these doctors, 'chance' was an important factor in selecting a location for training:
I didn't know much about the area. It was not an informed decision, I just made the decision without any consideration of what it would be like. (Overseas-born GP)
Nearly one-quarter (23% n=8) of overseas-born doctors chose to remain in rural general practice after gaining their fellowship. This group did not select rural general practice as a deliberate career choice. However, they found the experience of living and working in a rural environment both challenging and rewarding. The following comment provides insight into the importance of the rural training experience in retaining overseas-born registrars after fellowship:
If I didn't come here to train, I wouldn't be in the country. It is the experience of being in a rural community that gives you an understanding of what it is like. If you didn't experience it, you wouldn't even consider coming to a rural practice. I was forced to go rural because of the ten-year moratorium. (Overseas-born GP)
Why did some GPs leave rural practice?
A total of 45% (n=26) of the study cohort left rural general practice soon after attaining their FRACGP, most relocating to metropolitan practice. Four were Australian-born and 22 were overseas-born doctors. Eight of the nine overseas-born, Australian-trained doctors relocated to metropolitan practices in Australian cities. This study found that relocation was predominantly due to:
- the opportunity for specialist training
- the importance of being close to extended family members who were city based
- perceptions of better educational opportunities for children in city schools and universities
- lack of cultural support networks for themselves and their spouses in rural towns.
Specialisation: Two Australian-born doctors took the opportunity to build on previous training experiences. Both had undertaken advanced rural skills posts with BRTN and were furthering their specialist training in city hospitals. One has since relocated in the Bogong region as a specialist anaesthetist. However, anecdotal evidence from discussions with practice managers suggest that two overseas-born doctors that the researchers were unable to locate had also pursued specialist training in capital cities.
Proximity to family: Lack of familiarity with rural living and isolation from family and friends for overseas-born doctors was a major reason for relocating to metropolitan areas. While many respondents considered the challenge and diversity of rural general practice far more appealing than metropolitan practice, the importance of close contact with city based relatives and friends took precedence over personal job satisfaction:
I was attracted to a city practice mainly because my family and friends were all in the city. (Overseas-born, overseas-trained GP)
Educational opportunities: Overseas-born doctors were of the view that their children would have more opportunities in life if they were educated in the city. When asked what influenced him to relocate to a metropolitan practice, one doctor remarked:
Kids' schooling. Schooling in the [town name] area was not going to be satisfactory. There was a lack of choice of good schools. (Overseas-born GP)
While this view was fairly typical of the overseas-born doctors in this study, it was not the case for Australian-born doctors. They were more likely to educate their children in local primary and secondary schools and then accept that their offspring would move to a capital city when they began their university studies.
Support networks: Several overseas-born respondents had experienced difficulties adapting to life in small rural communities. Many towns are not as culturally diverse as larger regional or metropolitan centres so social networks and activities are hard to establish. Even overseas-born doctors who remained in rural practice after fellowship commented that isolation from city based family and friends, and lack of locally sourced Hal-al and Asian food and cultural activities were problematic. Similarly, and associated with distance from family, was the lack of suitable support networks for the spouses of doctors in rural towns:
My wife didn't cope with a rural environment. She was born in the city. We were both born overseas in the city. We had no family support in the rural town because our family were all in Melbourne. My wife couldn't adapt to a rural lifestyle. (Overseas-born, Australian trained GP)
What sustains doctors in rural practice?
While the triggers for attracting and deciding to remain in rural practice for Australian and overseas-born doctors may be different, both groups agree on what sustains them in rural practice once that decision is made:
- a preference for a rural lifestyle and a fondness for rural people and communities
- the diversity and challenge of rural practice
- the ability to provide holistic patient care.
Rural lifestyle, rural people and communities: A desire for a rural lifestyle and a connection to rural people and their communities together with proximity to Melbourne were the most frequent reasons that Australian and overseas-born respondents offered for remaining in rural practice Many expressed an aversion to the fast pace of city life, traffic congestion, and the impersonal nature of suburban living. Several respondents commented on the slower pace of country living and the positive aspects of developing a strong sense of community. One respondent noted:
The satisfaction of rural practice is tremendous. Working in a close-knit community is really good. You feel part of the community. (Australian-born GP)
Another respondent described country people as more 'down to earth' and more 'genuine' than city people. He enjoyed their openness and candour and felt he understood the issues facing many farming families. Another respondent in a small rural town, when asked why he had remained in the town where he trained, said:
The town. The people here. Facilities including the hospital. Friendly staff [and] proximity to Melbourne [state capital]. (Overseas-born GP)
Diversity and challenge of rural practice: Both Australian and overseas-born respondents commented that a benefit of rural practice is having a good mix of different types of patients and being required to have a range of skills to deal with 'whoever comes in the door'. They argued that there is a greater variety of medical conditions to manage than in metropolitan practice and believed they had more autonomy in treating patients, especially in emergency medicine.
Respondents reflected that the diversity of general practice, which included emergency and procedural work, was essential for skills development and provided far greater levels of job satisfaction than they would have if they worked in general practice in a metropolitan environment:
The greater the variety of cases and conditions, the better it is for skills development and job satisfaction. ...This variety of exposure to a range of medical issues and problems makes you use your brain and clinical skills to the max. (Australian-born GP)
Holistic patient care: A third important element that sustained Australian and overseas-born GPs' interest in rural practice was a commitment to provide holistic, 'cradle to grave' patient care. Continuity of care and understanding the issues and problems facing whole families played a significant role in providing high levels of patient care and job satisfaction for rural GPs:
When I worked in big city hospitals you saw people as patients and they were gone again; you didn't have that on-going continuity that you can get in a rural setting. (Australian-born GP)
The positive aspects of being a doctor in a small town outweighed the disadvantages for those that wished to stay. One doctor expressed a strong sense of duty to the individuals and communities he served:
As a citizen, as an Australian citizen, I think that we also have some moral responsibility to give some support to the community. I think that is a good idea. To use your skill as well; it is a very good opportunity. (Overseas-born GP)
Discussion
Has the decentralised model of GP training resulted in the retention of doctors in rural areas? Yes. But the extent to which the model has influenced GP retention rates is a complex issue. This is particularly true in light of the multidimensional nature of health care in Australia19, and the interrelationships between work related and personal/lifestyle satisfaction factors in the overall social, political, economic and cultural environment20. This study has revealed that there is a positive association between rural training and rural retention for some doctors. At the conclusion of this study, 42% of doctors who trained with BRTN remained in the region. Separate data shows that in the Bogong region between 2004 and 2010, the full-time workload equivalent GP-to-population ratio fell from 1:166921 to 1:126222 adding weight to the notion that the decentralised training model has had a positive impact on the workforce in the Bogong region.
Consistent with the literature23-25, the majority of the Australian-born doctors in this study chose rural practice because they or their partners had experienced rural or semi-rural environments and were familiar with rural culture and a rural lifestyle. This study also found that Australian-born doctors are significantly more likely to remain in rural practice after completing training than their overseas-born colleagues. For Australian-born doctors, informed choice drew them to rural general practice. They came to the region to train predominately because they were familiar with rural life, they or their spouses had rural backgrounds or connections, and many had a preference for procedural work. This is consistent with contemporary Australian studies, which indicate that not only does a rural lifestyle, rural people and communities exert a strong influence on the choice of location for medical registrars26, but a rural background24,27 and the challenge of procedural practice28 are strong predictors of the decision to practice in a rural environment.
Australian-born, Australian trained medical graduates are self-selecting individuals. They are not subject to the moratorium or compelled to locate in a rural environment. Because they have the opportunity to train and locate in specific rural locations by informed choice rather than chance, it might be expected that they will remain in rural general practice after fellowship, as did nearly three-quarters of the doctors in this study.
The literature is clear that prospective registrars with rural backgrounds and/or associations are more likely to be attracted to and remain in rural practice after fellowship than registrars with urban backgrounds. This study confirms Australian-born doctors are more likely than recently arrived overseas-born colleagues to have a 'rural connection' and to be familiar with rural community life. In this regard there is a need to recognise the importance of rural suitability as a selection criterion when engaging in the GP registrar recruitment process.
However, the choice of most overseas-born doctors is influenced by the requirement to train in the rural pathway and work in an area of workforce shortage. Consistent with Reed et al's study into barriers to employment of overseas trained doctors29, this study found overseas-born doctors are more likely to select a rural location on the basis of proximity to a capital city in order to remain close to extended family members. In this sense they are attracted to a particular region more by chance than choice.
Similarly, Alexander and Fraser note that an important factor in the retention of overseas trained doctors in rural practice relates to educational facilities for children and work opportunities for partners30. This study concurs, finding that relocation to metropolitan practice after training was predominantly due to lack of cultural and familial support networks and perceptions of limited employment and educational opportunities for spouses and children.
Although the ten-year moratorium is discriminatory31, its intent is to bring medical services to designated areas of need in rural, remote and outer metropolitan regions. This has been an effective catalyst in bringing overseas-born doctors to rural and regional centres32. However, while 'obligation strategies' are common throughout the world33 and may provide a degree of workforce stability for a limited time20, they do not necessarily keep doctors in rural communities. With only 27% of the doctors subject to the moratorium staying in rural practice, this study has once again demonstrated that doctors who wish to relocate to urban centres for family, educational or other reasons do so after fellowship, even if it means practising medicine on the fringes of capital cities, and those doctors who want to work in rural areas do so and tend to stay there - as with nearly-three quarters in this cohort.
Our study found that there was a significant relationship between place of birth and remaining in rural practice, with almost three-quarters (73% n=16) of the Australian-born respondents and almost one-quarter (23% n=8) of the overseas-born respondents remaining in rural practice after fellowship (χ² = 13.68 p<0.001). In contrast, the location of primary medical qualification (Australia or overseas) was less influential. Of the nine overseas-born, Australian trained medical graduates, only one has remained in rural practice. It is likely that overseas-born doctors who complete their medical degree in Australia have more characteristics in common with their overseas-born, overseas-trained counterparts than they do with their Australian-born colleagues.
While the decentralised training environment has had a positive influence on GP retention rates in the Bogong region, particularly for Australian-born graduates, there are cultural and regulatory differences between Australian and overseas-born doctors that profoundly influence the decision to locate and remain in rural communities. An understanding of these differences is essential if policy-makers are to maximise the retention of both groups of GPs in rural communities.
Evidence from this study suggests that decisions about location may be made early in the GP career-path, decision-making phase. Thus it is vital in order to create early exposure to careers in rural general practice through marketing general practice to school children, including the children of overseas-born migrants, and embracing introductory programs such as the Prevocational General Practice Placements Program (PGPPP). It is also important to maintain opportunities for rural based decentralised training to accommodate the wave of Australian-trained medical students who are approaching graduation. To this end, the development of specific rural training programs such as the Rural Generalist Pathway need more support.
Many of the overseas-born doctors in this study, even those who have returned to the cities, stated that they would not have been exposed to the benefits of rural medicine or contemplated remaining in rural practice had it not been for the regulatory framework that compelled them to locate in rural centres. For those who stayed, training, living and working in a rural environment was an important influencing factor in their decision to remain in rural practice. Although they did not have substantial prior exposure to rural community life or knowledge of North-east Victoria, they indicated that the quality of the training experience and their experience of life in rural Australia unlocked opportunities and provided them with choices they previously did not know existed. In forcing registrars to train in the rural pathway, the ten-year moratorium has facilitated the experience of country life and rural medicine that would not otherwise be considered or imagined. As Lee et al noted, the experience of rural training can impact positively on individuals' decision to remain in rural practice34.
It is unlikely that Australia's need for overseas trained doctors will diminish in the foreseeable future32,35. This group, including overseas-born, adult migrants who gain their primary medical qualifications in Australia, require different types of support and assistance during GP training if they are to remain in rural locations. It is well documented that social isolation and acculturative stress is problematic for overseas-born health professionals working in Australian rural communities36, and there are growing calls for greater levels of clinical and cultural support networks for overseas-born doctors37,38. Researching the specific support needs of overseas-born doctors and their families in order to minimise the isolation and challenges associated with living and working in a rural environment is essential if they are to be retained in rural communities.
While this study represents a snapshot of the effect of decentralised GP training in the Bogong region, it is part of a longitudinal study that is examining the causal relationship between decentralised training and longer-term retention of doctors in rural and regional practice. The results of that study should contribute further to practical policy outcomes for governments and training providers.
Limitations
While this article has revealed a positive association between rural training and rural retention, the population studied was limited to quite a small cohort of doctors trained in the Bogong region of North-east Victoria and southern New South Wales, Australia. The overseas-born doctors had migrated to Australia as adults, were generally from urban, non-English speaking backgrounds and thus may not be representative of migrants who arrived as children or those from western, English-speaking cultures or rural environments.
A further limitation of this study is the lack of historical data available on the recruitment and numbers of GPs trained in the pre-regionalised environment, making direct comparisons between pre- and post-regionalisation situations difficult.
The decentralised training model has had a positive influence on retention rates in rural practice in the Bogong region. There are cultural and regulatory differences between Australian- and overseas-born doctors that profoundly influence the decision to locate and remain in rural communities with Australian-born doctors significantly more likely to remain in rural practice after completing training. For Australian-born doctors, informed choice draws them to rural general practice; while for overseas-born doctors, chance, is a major contributing factor that influences their decisions to locate in the region. This study supports the continued development of decentralised and rural-specific training pathways for Australian doctors as an effective method of attracting and retaining doctors to rural Australia during and after general practice training.
Acknowledgements
The authors acknowledge the support of Bogong Regional Training Network which funded the research project, the doctors who gave their time and offered their insights at interview, and the practice managers for their administrative assistance.
References
1. Somers GR, Strasser R, Jolly B. What does it take? The influence of rural upbringing and sense of rural background on medical students' intention to work in a rural environment. Rural and Remote Health 7: 706. (Online) 2007. Available: www.rrh.org.au. (Accessed 14 May 2012).
2. Eley D, Baker P. Will Australian rural clinical schools be an effective workforce strategy? Early indications of their positive impact on intern choice and rural career interest. Medical Journal of Australia 2007; 187(3): 166-167.
3. Deloitte Access Economics. Review of the Rural Medical Workforce Distribution Programs and Policies. Canberra, ACT: Department of Health and Ageing, 2011.
4. Holsgrove G, Jolly B, Jones A, Southgate L. Alternative Approaches to Vocational Training for General Practice: final report of the London hospitals consultancy team. Canberra, ACT: Department of Human Services and Health, 1996.
5. Australian Government. Health Insurance Amendment Bill (No 2) 1996. Explanatory Memorandum. Canberra, ACT: Australian Government, 1996.
6. De Boer R, Boxall A, Biggs A, Buckmaster L, Gardner-Garden J, Jolly R. The interim report of the National Health and Hospitals Reform Commission - a summary and analysis. Research Paper 24 2008-09. Social Policy Section, Parliament of Australia, 2009. Available: http://www.aph.gov.au/About_Parliament/Parliamentary_Departments/Parliamentary_Library/pubs/rp/rp0809/09rp24 (Accessed 9 May 2012).
7. Australian Government Department of Health and Ageing. Report on the Audit of the Health Workforce in Rural and Regional Australia. Canberra, ACT: Commonwealth of Australia, 2008.
8. Department of Health and Aged Care. General practice education: the way forward. Final report of the Ministerial review of general practice training. Canberra, ACT: Commonwealth of Australia, 1998; vii-viii, 1, 85.
9. Australian General Practice Training. What is GPET? (Online) 2009. Available: http://www.agpt.com.au/PoliciesPublications/AboutGPET/ (Accessed 14 May 2012).
10. General Practice Education Australia. Transfer to a Regional Training Provider at the end of the 2003 training year. Letter to registrars. Brisbane, QLD: Royal Australian College of General Practitioners, 2003.
11. Hawthorne L, Birrell B. Doctor Shortages and their impact on the quality of medical care in Australia. People and Place 2002; 10(3): 55.
12. Commonwealth of Australia. Health Insurance Amendment Bill (No 2) 1996. Supplementary Explanatory Memorandum. Canberra, ACT: Commonwealth of Australia, 1996.
13. Medicare Australia. Forum. New Legislation. Newsletter of the Health Insurance Commission 1997; 8(1): no pp.
14. Rural Health Workforce Australia. Will more medical places result in more rural GPs? Melbourne, VIC: Rural Health Workforce Australia, 2008; 6.
15. Hawthorne L, Hawthorne G, Crotty B. The Registration and Training Status of Overseas Trained Doctors in Australia. Final Report. Melbourne, VIC: Faculty of Medicine, Dentistry and Health Sciences, The University of Melbourne, 2007; 58.
16. Medical Training Review Panel, Department of Health and Ageing. Medical Training Review Panel: thirteenth report. (Online) 2010. Available: www.health.gov.au/internet/main/publishing.nsf/Content/work-pubs-mtrp-13 (Accessed 14 May 2012).
17. Medical Training Review Panel, Department of Health and Ageing. Medical Training Review Panel: fourteenth report. (Online) 2011. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/work-pubs-mtrp-14 (Accessed 14 May 2012).
18. Hawthorne L, Birrell B, Young D. The retention of Overseas Trained Doctors in General Practice in Regional Victoria. Melbourne, VIC: Rural Workforce Agency, 2003; 33-34.
19. Acil Tasman. Evaluation of the regionalization of general practice vocational training. Report for the Department of Health and Ageing. Canberra, ACT: Department of Health and Ageing, 2005.
20. Humphries J, Wakerman J, Pashen D, Buykx P. Retention strategies and incentives for health workers in rural & remote areas: What works? Canberra, ACT: Australian Primary Health Care Research Institute, ANU College of Medicine, Biology & Environment, School of Rural Health, Monash University, Bendigo, Centre for Remote Health Alice Springs, Mt. Isa Centre for Rural and Remote Health, 2009; 9.
21. Primary Health Care Research & Information Service (PHC RIS). Key Division of General Practice characteristics 2002-2003. (Online) 2004. Available: http://www.phcris.org.au/products/asd/keycharacteristic/index.php (Accessed 9 May 2012.
22. Primary Health Care Research & Information Service (PHC RIS). Key Division of General Practice characteristics 2009-2010. (Online) 2011. Available: http://www.phcris.org.au/products/asd/keycharacteristic/index.php Accessed 20 April 2012).
23. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9: 1083 (Online) 2009. Available: www.rrh.org.au (Accessed 7 May 2012).
24. Australian Medical Workforce Advisory Committee. Career decision making by postgraduate doctors. AMWAC Medical Careers Surveys, 2004. Main Report. Sydney, NSW: AMWAC 2005; 187-191.
25. Humphreys J, Walkerman J, Wells R, Kuipers P, Jones J, Entwistle P et al. Improving Primary Health Care workforce retention in small rural and remote communities: how important is ongoing education and training? Melbourne, VIC: Australian Primary Health Care Research Institute, School of Rural Health Monash University, Centre for Remote Health, Flinders and Charles Darwin Universities, Menzies Centre for Health Policy, 2007; 9.
26. Lawrence CO, Williamson V, Sumner KE, Fleming J. "Latte rural": the tangible and intangible factors important in the choice of a rural practice by recent GP graduates. Rural and Remote Health 10: 1316. (Online) 2010. Available: www.rrh.org.au (Accessed 12 May 2012).
27. Ward A, Kamien M. Career choices and practice locations of medical students. Project 654. General Practice Evaluation Program (GPEP). Perth, WA: University of Western Australia, 2000.
28. Robinson M, Slaney GM, Jones GI, Robinson JB. GP Proceduralists: 'the hidden heart' of rural and regional health in Australia. Rural and Remote Health 10: 1402. (Online) 2010. Available: www.rrh.org.au. (Accessed 9 May 2012).
29. Reed M, Reed C, Forwood A, Camakaris B. Barriers to Employment of International Medical Graduates within the Victorian Public Health System. Research Report. Melbourne, VIC: Medical Workforce - Service and Workforce Planning, Department of Human Services, 2008; p 45.
30. Alexander C, Fraser JD. Education, training and support needs of Australian trained doctors and international medical graduates in rural Australia: a case of special needs? Rural and Remote Health 7: 681. (Online) 2007. Available: www.rrh.org.au (Accessed 9 May 2012).
31. General Practice Registrars Australia. Federal Election Statement 2007. Breathing new life into general practice. (Online) 2007 Available: http://www.gpra.org.au/sites/default/files/docs/GPRA%20election%20statement%202007.pdf (Accessed 9 May 2012).
32. Rural Health Workforce Australia. Submission to the Health Standing Committee. Parliamentary Inquiry into Overseas Trained Doctors. The 10-Year Moratorium. (Online) 2011. Available: http://www.rhwa.org.au/site/index.cfm?display=32639 (Accessed 9 May 2012).
33. Frehywot S, Mullan F, Payne PW, Ross H. Compulsory service programmes for recruiting health workers in remote and rural areas: Do they work? Bulletin of the World Health Organisation 2010: 88: 264-370.
34. Lee Y, Barnard A, Owen C. Initial evaluation of rural programs at the Australian National University: understanding the effects of rural programs on intentions for rural and remote medical practice. Rural and Remote Health 11: 1602. (Online) 2011. Available: www.rrh.org.au (Accessed 9 May 2012).
35. House of Representatives Standing Committee on Health and Ageing. Lost in the Labyrinth: Report on the inquiry into registration processes and support for overseas trained doctors. Canberra, ACT: Parliament of the Commonwealth of Australia, 2012.
36. Le Q, Elmer S, Kilpatrick S. Adapting to rural communities by overseas born health professionals. In: Proceedings, Rural health: the place to be,10th National Rural Health Conference; 17-20 May 2009; Cairns, QLD; 2009.
37. Australian College of Rural and Remote Medicine. ACRRM submission to the House of Representatives Standing Committee on Health and Ageing. Inquiry into Registration Processes and Support for Overseas Trained Doctors. (Online) 2011. Available: www.acrrm.org.au/reviews-and-submissions (Accessed 9 May 2012).
38. Royal Australian College of General Practitioners. RACGP Submission to the House of Representatives Standing Committee on Health and Ageing: Inquiry into Registration Processes and Support for Overseas Trained Doctors. Melbourne, VIC: RACGP, 2011.
