Hospitals are part of a comprehensive system of services that together contribute to the nations' health outcomes. Australia has a mix of public and private hospitals and they account for approximately one-third of the healthcare gross domestic product. While governments have assumed the responsibility of delivering public hospital services in Australia to ensure equity of access, private hospitals do not have the same degree of service obligations and most of them operate on a for-profit basis1.
Dental health services in Australia are largely privately financed with almost 80% of the total expenditure met through out-of-pocket payments or private health insurance, with approximately $4 billion spent annually directly by patients2.The direct costs have led to differential access to dental care with the lower socioeconomic groups being least likely to access care3,4. Australia ranks high globally in terms of the degree of inequality in access to health care, especially dental care5. This can be attributed to its vast geographic land mass and significant socioeconomic gradient within the population. Dental service patterns in Australia also shows a sharp contrast between patients receiving care in the public and private sector; while extractions are more common in public hospitals, restorative and preventive treatments are more commonly provided in private hospitals6.
With significant improvements in dental health, it is assumed that dental disease would no longer be responsible for significant hospitalisation rates. However, in Western Australia, oral health conditions are still responsible for a large number of hospital episodes and are a significant cost to the State. Removal of impacted teeth comprises approximately 37% of all hospitalisations for oral health related conditions in Western Australia and the total costs for this procedure contributes to approximately 27% of all hospitalisation costs for oral health related conditions7. Most of the patients hospitalised for the removal of these impacted teeth are young (between the age group of 15-24 years), reside in metropolitan areas, seek treatment in a private hospital and are privately insured7. It has also been reported in the literature that hospitalisations for removal of impacted teeth were more common in the higher socioeconomic groups of the society who could afford private health insurance, while the lower socioeconomic groups, including Indigenous Australians residing in rural and remote areas, had fewer admissions for removal of these impacted teeth in Western Australia8.
With this background, this study developed a national projection of rates of hospitalisation for surgical removal of impacted teeth for Australia using Western Australian statistics.
The geographic projection model was developed based on previously published approaches, allowing the model to be sustainable at all levels, from health service regions through to a nationwide level9.
Baseline Western Australia data
Every episode of discharge from all private and public hospitals in Western Australia for the financial years 1999/2000 to 2008/2009 indicating hospitalisation for removal of impacted teeth as the principal oral condition, as classified by the International Classification of Disease-tenth Australian Modification (ICD-10AM), was included in the study: these data were pooled to form the base data for this analysis10. Hospitalisation data were obtained from the Western Australian Hospital Morbidity Data System (HMDS) under appropriate ethical data release. The diagnoses of all types of impacted and embedded teeth were included in the analyses. Primary place of residency at the time of hospitalisation, age and health insurance status were also analysed. Indigenous cases have not been used in this study as they constitute less than 0.5% of the total number of cases.
Population data
Australian population data were obtained from the Australian Bureau of Statistics' (ABS) last national Census (2006). Data were obtained by age, health insurance status and socioeconomic status, Socio-Economic Indexes for Areas (SEIFA) category. SEIFA is the nationally accepted coding for socioeconomic advantage and disadvantage in Australia developed by the ABS. This index uses income, housing, employment, education and others as a basis for quantifying socioeconomic standards in different areas. Categories for SEIFA are: most disadvantaged (deciles 1, 2), above average disadvantaged (deciles 3, 4), average disadvantaged (deciles 5, 6), below average disadvantaged (deciles 7, 8) and least disadvantaged (deciles 9,10). Each category comprises approximately 20% of the Australian population.
Rate calculations
The West Australian dataset was then analysed to determine the rates of hospitalisation for removal of impacted teeth for insured and uninsured patients for the four age groups: 15-19, 20-24, 25-29 and 30-34 years in each of the five SEIFA-defined categories. Ages <14 years and >35years were not included as the selected age groups comprised almost 80% of all cases reported7. The variables of age, health insurance status and SEIFA category were used as risk indicators7. A total of 40 distinct rates were computed dependent on the mix of the variables health insurance (two sub-sets), age (four sub-sets) and SEIFA (five sub-sets). The percentages of private health insurance status of the population among the different age groups were obtained from the ABS website11. Statistical Package for the Social Sciences v15 (SPSS Inc; www.spss.com) was used to produce the required population-based rates. This approach is consistent with that applied previously9.
Geographic boundaries
Australia is divided geographically into statistical local areas (SLAs) by the ABS. The SLA is the base spatial unit used to collect and disseminate statistics other than those collected from the population censuses. The SLA is the smallest unit defined in the Australian Standard Geographical Classification (ASGC). Statistical local areas cover the whole of Australia without gaps or overlaps, and there are a total of 1353. Boundary files for each SLA were obtained from the ABS.
Model development
Population data across each of the 1353 SLAs were distributed by age, health insurance status and SEIFA. Using Excel v2003 (Microsoft; Redmond, WA, USA), the hospitalisation rate for each population subset derived from the Western Australian morbidity data was applied across Australia to the appropriate population subset (age, health insurance status, SEIFA) within each SLA.
The fully integrated database was then geo-coded using ArcGIS v10(ESRI; Redlands, CA, USA) to allow the visualisation of the fully integrated data model.
Ethics approval
Ethics approval was from the Human Research Ethics Committee from The University of Western Australia (#RA/4/1/5502).
Validation of the model
The mathematical model was validated by comparing projected Western Australian rates of hospitalisation with real reported data in Western Australia. It was known from the morbidity dataset that in Western Australia over the 10-year period (1999/2000 to 2008/2009) an average of 8810 hospitalisations occurred per annum, with 7106 (80%) of these happening within the 15-34 years age-group. Consequently, the mathematical modelling approach developed and presented in this study to calculate the projected numbers of Western Australian total hospitalisations for the removal of impacted teeth produced an outcome that was within 10% of the reported (real) data for Western Australia.
Overall rates
The extrapolation of the Western Australian rates to the whole of Australia gave an age-adjusted rate of approximately 1300 persons per 100 000 undergoing hospitalisation for the removal of impacted teeth. Overall it is predicted that almost 62 000 patients per annum would have undergone removal of their impacted teeth under general anaesthesia during the study period in the whole of Australia. With the average Diagnosis Related Group (DRG) cost of this procedure being approximately $1300, it can be predicted that almost $80 million per annum was spent on this procedure in the whole of Australia.
A clear rural-urban divide with the age-adjusted rates (AAR) being higher in the metro-city SLAs when compared to the rural-remote SLAs is shown using maps (Fig1). A 25 km buffer was drawn around the metro General Post Offices (GPOs) to compare the rates between those residing closer to the city and those away from it. Approximately 37% of the SLAs were within the 25 km buffer and approximately 63% of them were outside the buffer zone. A clear contrast is shown with higher rates noted in those SLAs closer to the city when compared to those away from it (Fig2). Age-adjusted rates were calculated for those within the city buffer, which was 1363 per 100 000 persons when compared to 1175 outside the buffer zone.
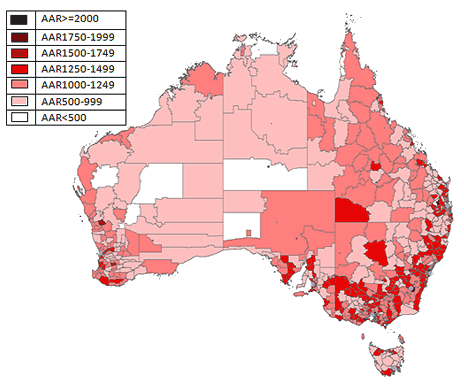
Figure 1: Geographic modelling of projected age-adjusted rates for patients
undergoing hospitalisation for removal of impacted teeth in Australia.
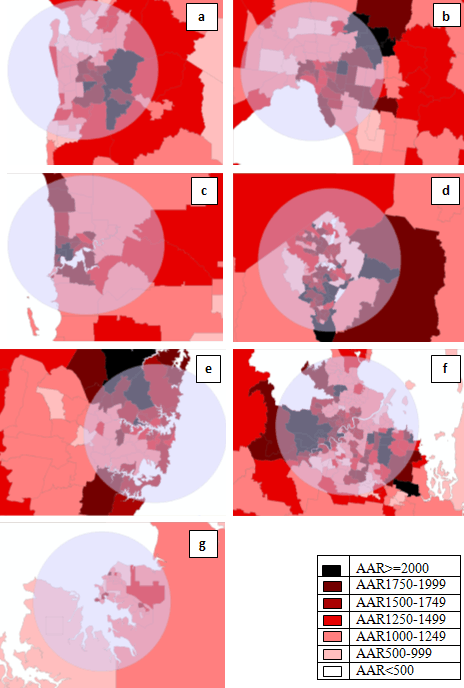
Figure 2: High magnification maps of the metropolitan areas of (a) Adelaide, (b) Melbourne, (c) Perth, (d) Canberra,
(e) Sydney, (f) Brisbane and (g) Darwin overlaid with 25 km buffer (blue shading). The differing levels of red (see key)
are different estimated age-adjusted rates (AAR) of patients undergoing hospitalisation for the removal of impacted teeth.
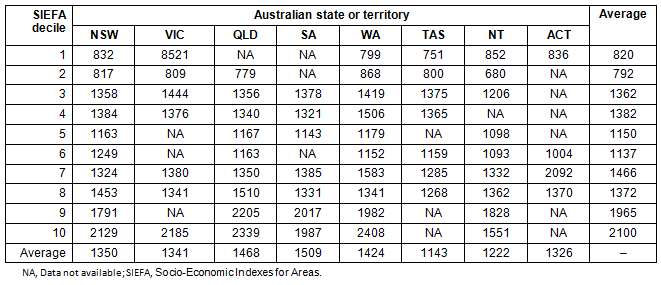
Comparison of the estimated number of total cases and insured cases among the different SEIFA deciles also shows a marked variation (Fig3). The highest numbers of cases are estimated as expected in the SEIFA deciles 9 and 10, which represent the least disadvantaged populations. On comparison of projected AARs per 100 000 among the different SEIFA deciles (Fig4), the AARs in deciles 9 and 10 (least disadvantaged) are almost three times greater than the AARs in deciles 1 and 2 (most disadvantaged). The estimated AARs in the eight Australian states show a somewhat similar pattern, except for Tasmania, where the rates are mostly lower than the other states (Table 1).
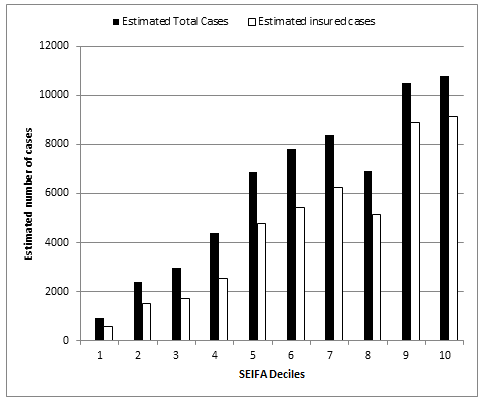
Figure 3: Comparison of estimated numbers of total and insured cases undergoing hospitalisation for
removal of impacted teeth in each Socio-Economic Indexes for Areas (SEIFA) decile per annum in Australia.
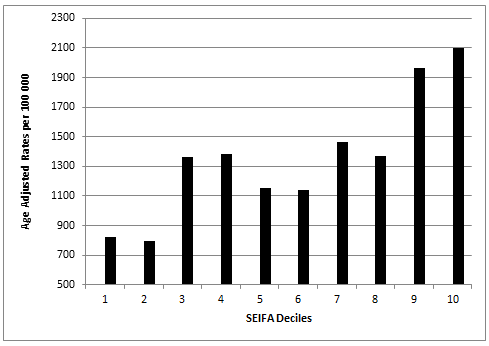
Figure 4: Comparison of the projected age-adjusted rates for patients undergoing hospitalisation for
removal of impacted teeth in each Socio-Economic Indexes for Areas (SEIFA) decile in Australia.
Table 1: Comparison of projected age-adjusted rates for patients
undergoing hospitalisation for removal of impacted teeth in the different Australian states
Discussion
The projections of Western Australian derived rates of hospitalisation to the whole of Australia using this innovative approach produced some very interesting insights. A definite rural-urban divide was found. If this was a purely disease-driven care, then an even geographic distribution would be expected. However, these results can be attributed to a number of factors: the strong socioeconomic gradient within the Australian population and therefore the ability to afford private health insurance as dental treatment is mostly private12; the concentration of specialists, general dental practitioners and hospitals in urban areas13,14; and the need to seek treatment15. This again leads to the issue of accessibility to dental services in rural and remote communities and the effect of the 'pay for services' system in affording dental treatment. The behavioural model for the use of health services that was used to interpret the national health data in the USA also highlights the contribution and importance of different factors at both individual and community levels, which include age, gender, ethnicity, education, socioeconomic level, health status, health beliefs, dental insurance, smoking status and dental anxiety16. The high prevalence of the procedure of hospitalisation for the removal of impacted teeth in urban centers could be a reflection of these factors. It is also important to note that the Indigenous cases have not been used in this study and therefore it is a projection of only the non-indigenous rates.
An Australian study based on the National Health Survey in 2001, which studied the factors associated with dental service attendance in young adults, found that those living in a major city and young adults with private health insurance were more likely to have visited a dental professional than those living in other geographic areas or without private health insurance5. The results of our study also show a similar pattern. The increase in dental service attendance led to increased provision of services in urban areas.
The cost for this procedure is another issue to be considered. It has been reported in the literature that most impacted teeth are third molars and there exists a huge controversy surrounding the prophylactic extraction of these teeth for different reasons, including orthodontic treatment and prevention of future pathology17,18. Longitudinal studies have shown that extraction of unerupted third molars in young patients undergoing orthodontic treatment to prevent future crowding of lower incisors is not evidence based19. Many of these third molars that remain impacted when young continue to erupt with age and it has been shown that retaining a third molar is more cost effective20. Also, some countries such as the England and Scotland have introduced guidelines governing the extraction of third molars, following which there has been a significant reduction (by almost 50%) in the number of patients being referred for third molar extractions, thereby reducing costs significantly21,22. Although most of the surgical extractions for impacted teeth in Australia are performed under general anaesthesia, a small number are performed in private dental clinics. The exact proportion of these is unknown, although it is estimated at less than 10%.
The results of this study suggest two important but contrary issues. One, the unavailability of these services to those residing outside the metro areas or their inability to afford these services. The second, questioning the very nature of this procedure and its costs, which is so focused for those residing in urban centers.
The basic objective of any healthcare system is to improve and maintain health outcomes for the population. Therefore, a complete understanding of the use of dental services is of the utmost importance for proper resource allocation and utilisation. The findings of this study can be used to inform health policy to guide proper allocation of resources and target services to benefit the community, especially those residing in rural and remote areas in a vast country such as Australia.
References
1. Australian Institute of Health and Welfare Dental Statistics and Research Unit. Oral health of health cardholders attending for dental care in the private and public sectors. Cat. no. DEN 196. Canberra, ACT: AIHW, 2009.
2. Productivity Commission. Public and private hospitals. Research report. Canberra, ACT: Productivity Commission, Australian Government, 2009.
3. Brennan DS, Luzzi L, Roberts-Thomson KF. Dental service patterns among private and public adult patients in Australia. BMC Health Services Research 2008; 8: 1.
4. Jamieson LM, Thomson WM. Adult oral health inequalities described using area-based and household-based socioeconomic status measures. Journal of Public Health Dentistry 2006; 66(2): 104-109.
5. Van Doorslaer E, Clarke P, Savage E, Hall J. Horizontal inequities in Australia's mixed public/private health care system. Health Policy 2008; 86(1): 97-108.
6. Brennan D, Spencer AJ. Trends in private dental service provision in major city and other Australian locations. Australian Journal of Rural Health 2007; 15: 189-195.
7. George RP, Kruger E, Tennant M. Hospitalisation for the surgical removal of impacted teeth: Has Australia followed the international trends? Australasian Medical Journal 2011; 4(8): 425-430.
8. George R, Kruger E, Tennant M. The geographic and socioeconomic distribution of in-hospital treatment of impacted teeth in Western Australia: a 6-year retrospective analysis. Oral Health and Preventive Dentistry 2011; 9(2): 131-136.
9. Kruger E, Heitz-Mayfield LJA, Perera I, Tennant M. Geographic modelling of jaw fracture rates in Australia: a methodological model for healthcare planning. Dental Traumatology 2010; 26(3): 217-222.
10. National Centre for Classification of Health. The international classification of diseases and related health problems, 11th revision, Australian modification (ICD-10-AM), Volume 1-5. Lidcombe, NSW: National Centre for Classification in Health, 2000.
11. Australian Bureau of Statistics. Private health insurance, Australia 2004-5, cat. no. 4815.0.55.001. Canberra, ACT: ABS, 2006.
12. Schwarz E. Access to oral health care an Australian perspective. Community Dentistry and Oral Epidemiology 2006; 34: 225.
13. Brennan D, Spencer AJ. Trends in private dental service provision in major city and other Australian locations. Australian Journal of Rural Health 2007; 15: 189-195.
14. Spencer AJ, Tuesner DN, Cartner KD, Brennan DS. The dental labour force in Australia: the position and policy directions. Australian Institute of Health and Welfare cat. no. POH 2. Canberra, ACT: AIHW (Population oral health series no. 2), 2003.
15. Slack-Smith LM, Mills CR, Bulsara MK, O'Grady MJ. Demographic, health and lifestyle factors associated with dental service attendance by young adults. Australian Dental Journal 2007; 52(3): 205-209.
16. Andersen RM. Revisiting the behavioral model and access to medical care: does it matter? Journal of Health & Social Behavior 1995; 36: 1-10.
17. Hugosen A, Kugelberg CF. The prevalence of third molars in a Swedish population. An epidemiologic study. Community Dental Health 1988; 5: 121-138.
18. Chu FCS, Li TKL, Lui VKB, Newsome PRH, Chow RLK, Cheung LK. Prevalence of impacted teeth and associated pathologies - a radiographic study of the Hong Kong Chinese population. Hong Kong Medical Journal 2003; 9: 158-163
19. Kruger E, Thomson WM, Konthasinghe P. Third molar outcomes from age 18 to 26: findings from a population-based New Zealand longitudinal study. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology 2001; 92: 150-155.
20. Mettes DTG, Nienhuijs MMEL, van der Sanden WJM, Verdonschot EH, Plasschaert A. Interventions for treating asymptomatic impacted wisdom teeth in adolescents and adults. Cochrane Database of Systematic Reviews 2005; 18(2): CD003879. DOI: 003810.001002⁄ 14651858.
21. Scottish Intercollegiate Guidelines Network. Management of unerupted and impacted third molar teeth. Edinburgh: SIGN, 1999.
22. National Institute for Clinical Excellence. Guidance on removal of wisdom teeth. London: NICE, 2000.


