Chronic disease is the leading cause of death and disability in Australia1 and the leading cause of mortality in the world, representing 63% of all deaths2. Worldwide, 346 million people are diagnosed as having diabetes3. In Australia diabetes is one of the top 10 leading causes of death, and as an underlying cause of death contributes to 28% of deaths4. The prevalence of diabetes in Australia is 7.5%5,6 and its incidence is escalating6. Therefore, effective approaches to the management and prevention of diabetes are important, with General Practitioners (GPs) being at a key point of intervention in service provision7.
Strategies to improve the inequitable provision of health services to rural and remote Australians8 that address the poorer health status of rural Australians compared with their urban counterparts are now government priorities9, as evidenced by the recent National Strategic Framework for Rural and Remote Health10. The paucity of the rural health workforce is a long standing and complex issue with multiple flow-on effects11. The number of full time equivalent (FTE) medical practitioners in inner regional locations (186 per 100 000) is approximately half that in major cities (332 per 100 000)12. Consistent with this, the number of specialists in inner regional locations (54 FTE per 100 000) is also approximately half that of major cities (116 FTE per 100 000)12. The current initiative, the Rural and Remote Health Workforce Innovation and Reform Strategy13 endeavours to address these issues, while the Medical Specialist Outreach Assistance Program an incentive program for specialists to provide outreach services, is of longer standing14.
While telemedicine has the potential to make a contribution to the provision of specialist services, there are known barriers for rural practice15. It is the more traditional outreach clinic that is the focus of the Physician in Practice Clinic (PIPC).
While shared care through specialist outreach clinics, where the specialist attends to see patients in an outreach setting and sends a report to the referring physician, is a traditional approach to the management of chronic disease, it has mixed results16. The model of specialist outreach that reflects the joint consultation between GP and specialist (with both present) central to the outreach clinic (the subject of this article), is typically described as a 'multifaceted' specialist outreach clinic, and has been found to improve patient access, outcomes and service use17. With this approach not only does joint consultation occur between the specialist and GP, but typically education sessions for primary caregivers or enhanced patient care are also provided. An investigation of the literature revealed that in more than 150 studies cited in systematic reviews of the specialist outreach model17-20, only one publication reported a model consistent with PIPC17. Therefore, while the PIPC model is not unique, it could be considered uncommon. While GP education is rarely a focus of the specialist outreach model, this is a key element of PIPC.
While comparative literature is limited, it shows some support for this model of care. One of the systematic reviews reported a randomised controlled trial of the joint consultation model in orthopaedic surgery21. Here significantly fewer specialist referrals and diagnostic actions occurred in the intervention group compared with the control group, more patients in the intervention group were symptom free after one year, and the clinical knowledge of GPs improved significantly21. A New Zealand study in paediatrics reported that GPs who attended six-weekly joint sessions highly valued the joint consultation and perceived this to be like a short refresher course22. In addition it was reported that multiple GPs frequently attended the joint consultation which extended the learning opportunity, and that after each consultation a discussion was held on general paediatric care and specific paediatric problems, which built further knowledge.
Physician in Practice Clinic
This is an innovative approach to the management of chronic disease that focuses on the education of GPs by an endocrinologist conducting patient consultations jointly with the GP at the GP's rooms. Expectations are that improved patient outcomes will result in the long term due to: better educated and more confident GPs; easier service access for patients; and reduced waiting lists. For the endocrinologist, in the longer term this may reduce waiting lists through more targeted referrals.
The Clinic is facilitated and overseen by the Toowoomba Division of General Practice, with participating practices conducting a Clinic approximately every 6 months. The endocrinologist, GP and the patient attend a 30 minute consultation by appointment. Prior to referral to the Clinic the GP reviews the patient and, where necessary, updated tests are undertaken. The GP presents key points from the patient's history and clinical questions that require exploration. A specialist opinion is offered and a management plan developed with the patient. The goal is for the GP to provide continued care with input from the specialist as required, but decisions about case responsibility are made on a case by case basis. The Clinic runs for half a day; initially monthly, then becoming fortnightly to meet demand by GPs; it is usually followed by a lunch time forum where practice staff are invited to pose questions to the specialist. The specialist is employed by the Toowoomba Hospital and the GPs claim their attendance time from Medicare (as is usual practice). This article reports on the perceived educational benefits of PIPC, identified by a sample of GPs involved in the Clinic. The aim of the article is to articulate what benefits the GPs have reported, as a measure of the effectiveness of the program.
Semi-structured interviews were selected to allow for the discovery of meaning and an understanding of the participants' viewpoints23. This approach elicits the personal and social context of beliefs and feelings through spontaneous responses that are specific and concrete24. It was therefore ideal for eliciting from the GPs the educational benefits they believed they had received, if any. The interview guide contained predominantly open-ended questions. Content focused on what educational benefits had occurred related to clinical knowledge, how useful this was to patients and in learning how to work with the specialist.
Sample
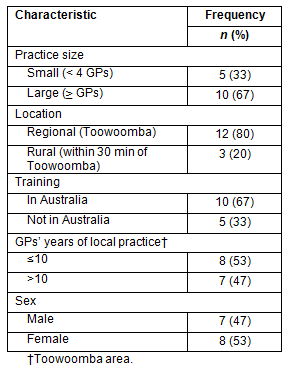
A purposive sample of 15 GPs involved in the Clinic, which operated in the Toowoomba region, Queensland, Australia, were recruited over a seven-month period as the Clinics occurred. Participants were recruited from each of the nine practices involved in the Clinics held between March and October 2010; each participant had been involved in one Clinic. For most of the practices this was the first time they had been involved in a Clinic but two practices had been involved in a pilot of the program. To ensure diversity in the sample, and to investigate for possible differences between characteristics, GPs were selected according to rural/regional location, practice size, sex, location of medical training and time practicing locally (Table 1), without weighting or stratification. All participating practices are Inner regional25. For the purposes of this article, Toowoomba practices are defined as 'regional' and the two other practices, both located within 30 km of Toowoomba, are defined as 'rural'. The Toowoomba population was approximately 140 000, while the rural centres had populations of approximately 4500 and 1700, respectively26.
In order for the sample to resemble the GPs involved in the Clinic, the characteristics the sample was selected on (ie rural/regional location etc) closely matched the proportions of those with these characteristics who were involved in the Clinic. Participation in the evaluation of the effectiveness of PIPC, that this article reports on in part, was a condition of entry to the Clinic program. All practices and therefore GPs were notified by the Division of General Practice when the evaluation commenced, and what would be required was outlined. A list of GPs who were involved in the Clinic was provided by practice managers. Those who met the inclusion criteria were contacted and invited by the research team to participate in the study; all invitees participated. When written consent had been provided by the GP, a digitally recorded interview took place, usually at the GP's practice. Anonymity and confidentiality are ensured, with only the research team knowing the identity of participants, because data were de-identified following collection, and reporting occurs only at the group level.
Table 1: Characteristics of the practices and GPs interviewed (n=15)
Ethics approval
Ethical approval for the conduct of this study was obtained from the University of Queensland Behavioural and Social Sciences Ethical Review Committee (#2010000620) and from the University of Southern Queensland's Ethics Committee.
Data collection and analysis
While a constructivist ontology underpins the choice of methodology, there is no explicit theoretical basis with the data collection process. However the approach is consistent with grounding the analysis in the data with the constant comparative method and theoretical saturation of Grounded Theory. Data analysis occurred concurrently with data collection and demonstrated after 15 interviews that there was little new information emerging and theoretical saturation had been reached.
A research assistant was employed to conduct the project, which included conducting the interviews. The research assistant was previously unknown to participants. Interviews took between 15 and 30 minutes. The period between Clinic attendance by the GP and data collection was, for the majority of participants, approximately 6 weeks, but for one it was 4 months and another 6 months. The interviews were professionally transcribed then thematically analysed by the first author using QSR NVivo v9 (www.qsrinternational.com); inductive analysis was used to identify concepts, sub-themes and themes. This interpretation occurred within the context of the study.
An issue that emerged early in the data collection process was the interviewees' overwhelmingly positive responses regarding the Clinic. This was despite the research team seeking a critique of the project through the interview process. Because no changes were required to the interview guide nor the process, the procedure was maintained. This positive response continued and resulted in no contradictory data.
While a member check or other strategy to test for trustworthiness was not conducted, the results reported are consistent with PIPC results in the Toowoomba Division of General Practice annual census of activities and programs, a funding requirement. The purpose of the census is to provide accurate and timely information on the General Practice workforce Australia-wide for strategic planning activities, as well as to inform local Division planning.
Of the 15 GPs interviewed, 10 were from large practices; 12 worked in a regional location (Toowoomba); 10 were trained in Australia (the remainder were not); eight had been practising locally (in the Toowoomba area) for up to 10 years; and eight were female (Table 1). Whereas these numbers reflected the proportions of GPs in PIPC with these characteristics, there are differences between these and national and state data. In Queensland 79.7% of employed medical practitioners are Australian trained27, whereas this was so for only 66.7% of Clinic GPs; however, this disparity could reflect that conditionally registered medical practitioners are not included in Queensland registration data. In Queensland 33.2% of employed medical practitioners were female, whereas 53.3% of those involved in the Clinics were female27.
Quotes are used to illustrate the educational benefits themes and sub-themes that emerged from the analysis. The GPs are identified by a number in brackets (#n) with their relevant characteristics as in Table 1. The themes are: new knowledge; interactive learning; knowledge used quickly; knowledge generalised; and increased confidence. These themes can be categorised as immediate and longer term benefits. Immediate benefits are those that participants reported happening during the joint consultation. There are: the acquisition of new knowledge; the interactive nature of the learning; and being able to use the knowledge quickly. Longer term benefits are those acquired after the joint consultation. These are: knowledge generalised; and increased confidence. For ease of explanation the immediate benefits are reported first, followed by longer term benefits. Text that best represents the theme or sub-theme has been selected, but with the goal of giving examples from a variety of participants.
Marked differences in the frequency of mention for a theme or sub-theme are listed according to a GP characteristic (Table 2). This quantification of qualitative data reflects the positivist origins of Grounded Theory28 and Strauss and Corbin's29 emphasis on verification, rather than Glaser and Strauss's30 focus on the discovery of theory. How this benefits the analysis is by highlighting in what ways GPs with these characteristics received educational benefits from their involvement in PIPC. These same results are reported headed by GP characteristics (Table 3). Due to the small numbers in some of the categories these results need to be interpreted with caution. The rationale for inclusion, particularly with the rural/regional category, is that the Division of General Practice was seeking feedback in all dimensions with a view to tailoring the program, if required. In addition it is well-documented that service provision is more costly when travel is required (in this case for the endocrinologist) and that rurally based practitioners have poorer access to professional development.
Table 2: Frequently mentioned themes and sub-themes by GP characteristics
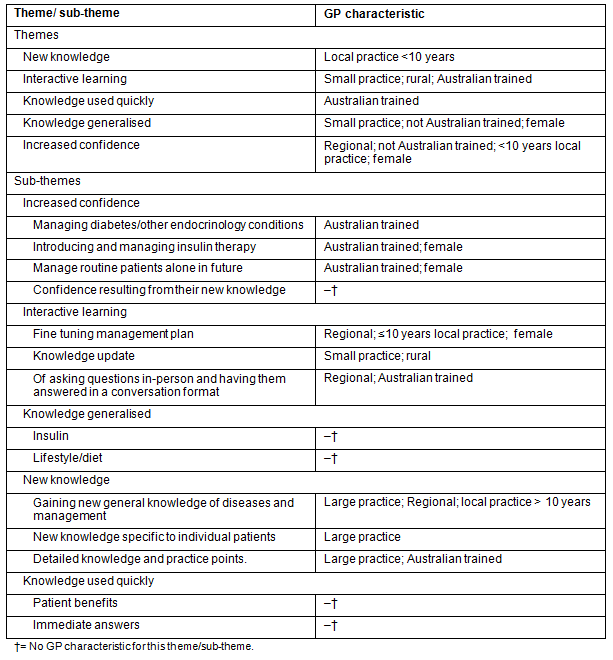
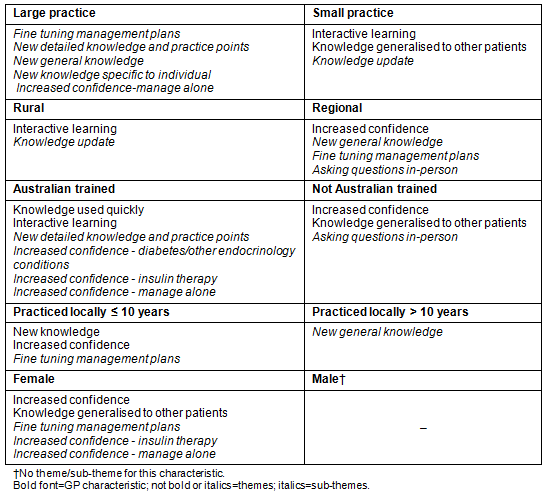
Table 3: Themes and sub-themes according to specific GP characteristics
Immediate benefits
The three themes, new knowledge, interactive learning, and knowledge used quickly are all benefits GPs reported receiving during or immediately following the joint consultation with the endocrinologist.
New knowledge: New knowledge was acquired from the PIPC program. Notably all doctors in the study spoke of gaining new knowledge. The sub-themes that emerged within new knowledge are: gaining new general knowledge of diseases and management; new knowledge specific to individual patients; and detailed knowledge and practice points. The general knowledge and practice points from the lunch time forums were seen as complementing the specific and detailed information elicited during patient consultations.
Those who had practiced locally for up to 10 years were more likely than those who had practiced longer to mention acquiring new knowledge, and those from large practices were more likely than those from small practices to comment on each of the sub-themes within new knowledge. However it was regional doctors and those who had practiced locally for more than 10 years who were more likely than their counterparts to mention the acquisition of new general knowledge; Australian trained doctors were more likely than those not trained in Australia to speak of acquiring detailed knowledge and practice points. There were no differences for the sex of the doctor.
The following quote illustrates the benefits of the lunch time forum for new general knowledge.
... we had the opportunity to ask all sorts of other questions too ... which was certainly very useful. ... last time we got into vitamin D which is quite topical at the moment and osteoporosis which wasn't a part of my case load that I put up, so that was quite interesting and useful (#13 Large practice; regional; >10 years local practice).
This comment highlights new detailed knowledge acquisition:
... the fellow that has the total pancreatectomy, in how to look at the blood sugars and how to adjust according to the short acting and the long acting ... so just to understand how we are looking at the drops and the pre and post of a certain meal or over the whole day and which one to look for when you are adjusting and which one to adjust (#15 Australian trained).
Interactive learning: The interactive nature of the learning was an important ingredient of the education. A key aspect of PIPC is the presence of the specialist at the GP-patient consultation. While more than three-quarters of participating GPs mentioned the benefits of interactive learning, it was rural doctors, those in small practices and Australian trained doctors who were more likely than their counterparts to mention this. Other differences emerging in the sub-themes were: fine tuning management plans; receiving updated knowledge; and benefits of asking questions in-person and having them answered in a conversation format.
While the rural doctors and those in small practices tended to speak predominantly about having their knowledge updated, the regional doctors were more likely to speak about the benefits of being able to ask questions in-person and fine tune their management plan. All those who mentioned the benefits of having questions answered in this interactive setting were Australian trained; those with up to 10 years local practice and female doctors only, spoke of fine tuning their management plan. The following quote is an example of knowledge updating:
We quickly discussed how we picked it up, how we managed it, what is the different classifications of thyroid cancer, what's the outcome for the patient, which one is dangerous, which one is not. So we actually quickly ran through five cancers in 10 minutes and that way you are getting a full recap of therapy available (#2 Rural, small practice).
This quote details the fine tuning of a management plan:
... often I know the basic points to start with, but it's then being given education and an idea of a particular plan for that scenario, but also for that individual patient. So it allowed us, or allowed me in particular, to feel much more confident to continue to manage that patient in the community (#11 Regional; female; more than 10 years of local practice; Australian trained).
The benefits of being able to ask questions in-person and have them answered is highlighted in the following quote:
... for the 'Can I just ask you what I should be considering?' And sometimes those things only take 2 minutes when the physician is here in the rooms because we can pull up the chart, pull up the medications, pull up their results and then can say, 'Bang, bang, bang' and you're fine, that's great, where to try to explain it via phone is too difficult and the only other way then would be a referral (#12 Australian trained; regional).
Knowledge used quickly: An important educational benefit was how quickly the new knowledge could be used. Almost two-thirds of the GPs spoke of being able to use their new knowledge quickly. The sub-themes are: patient benefits; immediate answers. This refers to how the patient benefited because the GP had questions answered immediately. The only differences in GP characteristics is that Australian trained doctors were more likely than those not Australian trained to speak of using their new knowledge quickly.
The following quote highlights how this worked at one Clinic, with emphasis on how quickly the patient receives treatment with this model of care when compared with the traditional approach. In addition this comment mentions the additional benefit for the patient, convenience of access.
... a lot of my people are very complicated and it takes a bit of getting your head around what's going on for them ... I've got a lady who had an operation, the operation went really well, but she got complications, she just did not do well afterwards and she was really, really sick and losing weight and she went to see the surgeon privately who said, 'Look you really, really need a gastroscopy'. Twelve months later she's got the appointment to go and see about the gastroscopy. Now after a year of being really, really sick she's starting to feel just a little bit better and doesn't want to have the thing in case it upsets her. So I mean there's the sort of thing that can happen in the public system where people have got a need to go and see someone and then it becomes quite complex to get them there and then by the time they get there, the clinical picture has changed ... on the day, you are with the specialist, you are seeing the patient, and this is how it is today, is quite different to sort of sending someone off into the 'never-never' where in 9 month's time they might arrive at someone's front door and they say, 'Well, what did Dr X really think because I can't see what he's talking about'. You know? (#7 Australian trained).
Longer term benefits
The three themes, knowledge generalised, increased confidence, and improved relationships and reduced referrals are all benefits GPs reported receiving at some time after the joint consultation with the endocrinologist.
Knowledge generalised: A key asset of the new knowledge was that it could be used with other patients. Two-thirds of the sample spoke of having used their new knowledge from PIPC with other patients. The sub-themes are: insulin and lifestyle/diet. The majority of comments described how the practitioners used their new knowledge about the introduction and management of insulin therapy with other patients. Some comments were also made by doctors about using their new knowledge to educate patients about the lifestyle and dietary aspects of diabetes management.
Doctors not trained in Australia, females, and those from small practices were proportionally more likely than their counterparts to speak of applying their new knowledge to other patients. There were no differences in the sub-themes. The following two quotes illustrate how these GPs have applied their new knowledge of insulin to other patients:
... certainly been more confident in using the insulin and increasing the insulin dosages and extending the regime of insulin.
Q: So how many patients would you have had the opportunity to apply that new knowledge to ...?
A: ... 20 to 30 patients I would guess (#5 Small practice; Australian trained; male).
... we always learned if they are unstable ... send to endocrinologist for second opinion and they always introduce insulin, but now it's different, so we can as Dr X told, you can introduce insulin (#14 Small practice; female; not Australian trained).
GPs trained in countries other than Australia and female doctors spoke about a broader range of applications of knowledge than their counterparts. The following comment details a range of conditions managed:
Particularly with thyroid problems, vitamin D, parathyroid, calcium problems in post-menopausal women really which I see a lot of, and adolescents with polycystic ovarian syndrome ... that's a large group of my population of age of the patients that I see, so yes, it's definitely helped me to commence a management plan and commence initial management with those patients that I'm seeing on a regular basis (#11 female; Australian trained).
Increased confidence: A follow-on effect of the new knowledge was an increase in confidence. As with knowledge generalised, two-thirds of the GPs spoke of their confidence increasing as a result of their involvement in PIPC. The sub-themes are: increased confidence in managing diabetes and other endocrinology conditions; more confident introducing and managing insulin; their confidence resulting from their new knowledge; and feeling able to manage routine cases alone next time.
Regional doctors, females, doctors not trained in Australia and those who had practised locally for up to 10 years were more likely than their counterparts to speak of their confidence being increased as a result of their participation in PIPC. However, Australian trained doctors were more likely than those not Australian trained to mention the sub-themes of increased confidence in managing diabetes and other endocrinology conditions, more confident introducing and managing insulin, and feeling able to manage alone next time. Only female doctors mention the sub-themes of being more confident introducing and managing insulin and feeling able to manage alone next time. So, female doctors who were Australian trained were more likely than their counterparts to mention the sub-themes of increased confidence in managing diabetes and other endocrinology conditions, more confident introducing and managing insulin and feeling able to manage alone next time.
In the following comment the GP describes her greater confidence in managing a similar problem alone in future:
I mean if I come across the same situation again now I think I probably would be able to sort of deal with it myself this time (#10 Female; Australian trained; up to 10yrs local practice).
This quote illustrates increased confidence to introduce and manage insulin therapy:
Oh, I would say increasing my confidence in my capacity to manage, particularly diabetes, because they were the cases that I brought, and in hearing the case discussion, the lunch time discussion regarding endocrinological conditions, then, so that more general increase in confidence as well (#3 Female; Australian trained).
Improved relationships and reduced referrals: A benefit with the potential for a long term effect was the improved relationships between the GPs and specialist, and the GPs reporting making fewer referrals. The GPs spoke about the positive changes in their relationship with both the endocrinologist and the specialist outpatients department at the hospital. Most GPs stated they felt more comfortable contacting the endocrinologist after their face-to-face contact at the joint consultation. Some GPs also felt they better understood the process and resources of the hospital. The GPs believed patients benefited from the Clinic through reduced specialist referrals, including those to specialists other than the endocrinologist.
Summary
In summary, at least two-thirds of study participants commented in each of the five themes, with all participants reporting they acquired new knowledge. While the GPs were unequivocal in their praise of this model of service delivery, some dimensions of PIPC had more educational benefits than others depending on the characteristics of the doctor (Table 3).
Increased confidence in clinical practice was the most comprehensively reported benefit of PIPC involvement with four of the five GP characteristics represented (Table 2). This is followed by interactive learning and knowledge generalised with three GP characteristics represented in each. It is noteworthy that two of the three benefits where at least three of the five GP characteristics are represented, are longer term benefits: increased confidence and knowledge generalised. Therefore, while there are differences within and between themes and sub-themes, the longer term benefits appear to accrue more generally.
The perceived educational benefits of PIPC are listed according to GP characteristic (Table 3). This demonstrates that the educational benefits reported varied by characteristic, and within each characteristic. There were differences according to location of practice. Rural doctors reported an immediate benefit, by identifying the interactive nature of the learning as key. This result is consistent with rural doctors being known to suffer from professional isolation31. In contrast, regional doctors reported the longer term benefit of increased confidence in their clinical practice as a result of the program. There were also contrasts between the place of receiving medical training, categories. Australian trained doctors reported two immediate benefits: being able to use the knowledge they acquired from PIPC quickly, and the interactive nature of the learning. However doctors not trained in Australia reported two longer term benefits: the increased confidence they have, and being able to use this new knowledge with other patients. Female doctors reported two longer term benefits: increased confidence and being able to generalise the knowledge to other patients. For the other two characteristics a combination of immediate and longer term benefits were reported. Those in small practices reported the immediate benefit of the interactive nature of the learning and the longer term benefit of being able to generalise the new knowledge to other patients. Those who had practised locally for up to 10 years reported an immediate benefit from the acquisition of new knowledge, and the longer term benefit of increased confidence.
The results from the Toowoomba Division of General Practice annual census of activities and programs reflect the benefits reported in PIPC. A questionnaire was emailed to all general practices in the Division, with several weekly reminders, resulting in a 62.5% response rate. The questions asked were: (i) Have you hosted a PIPC? (ii) If 'yes', was it of value? Why? (iii) If 'yes', would you host another? Why? (iv) If 'no' would you like to host a clinic? Why?. Of the 14 comments about usefulness, the educational benefits for the GP were the most frequently mentioned reason. Of those who had hosted a Clinic, 88% indicated they would host another. When asked why, of the 11 comments, most referred to the educational benefits for GPs. Of the 57% who had not hosted a Clinic but indicated they would do so, the most common reason given was for the educational benefits they anticipated.
Discussion
While reviews of specialist outreach models of care report mixed findings, this novel approach to specialist outreach, focused on the education of GPs to achieve improved long-term patient outcomes demonstrates some strengths. The GPs reported educational benefits from interactive learning, acquiring new knowledge from the joint consultation, being able to use it quickly and being able to generalise this knowledge to other patients. They also reported other benefits: increased confidence in their practice, and improved professional relationships and reduced referrals to the endocrinologist. The PIPC appears to have achieved its key aims of better educated and more confident GPs.
While the PIPC model (joint consultation) is rarely reported in the literature, the results of this evaluation are consistent with the few published studies. The GPs in the PIPC reported improved clinical knowledge as did those in a randomised controlled trial (RCT)21, and they highly valued the joint consultation as was reported in a study from New Zealand22. However specialist outreach clinics, without the joint consultation dimension, report benefits for GPs that are also reported with PIPC. One of these benefits is the increase in knowledge (in ophthalmology), but only for 38% of participants32,33; whereas in PIPC all study participants reported acquiring new knowledge. The improved relationships reported by GPs in PIPC were also found in a study of paediatricians34, and in a systematic review19.
The PIPC GPs believed a patient benefit would be reduced referrals and some reported that this had occurred already, with patients themselves reporting a range of benefits35. This resulted from the GPs' increased knowledge and therefore greater capacity to treat, obviating the need for referral at least on some occasions. This was a finding of the RCT21, with reduced and more targeted referrals in ophthalmology32, and across disciplines33.
The results of this aspect of the evaluation of PIPC demonstrate that GPs believe they have received significant educational benefits and that, in turn, their patients have benefited. While definitive conclusions cannot be drawn from this small study, its strength is the detail and nuanced account provided. Corroborating data is provided from two sources. First from the Toowoomba Division of General Practice annual census where the predominant value of PIPC was considered to be the educational benefits for GPs. Second, a patient satisfaction evaluation of PIPC reported substantial practical patient benefits, where two-thirds considered it an 'excellent' service, and patient comments indicated that they felt they benefited from the improved knowledge their GP obtained through the joint appointment with the specialist35. While the in-depth analysis to sub-theme level, of the educational benefits and the GP characteristics associated with these benefits, provides a rich description of how the knowledge is acquired and used to the advantage of both practitioner and patient, it is the broader thematic analysis that gives some indication of how PIPC could be targeted in future.
While not articulated explicitly in the PIPC program documentation, inherent in the program goals is the notion of progressive change over time. The results of the evaluation are consistent with this. The analysis of themes that were associated with the GP characteristics demonstrates two categories of benefit: immediate and longer term. The immediate benefits of acquiring new knowledge, through in-person interaction with the specialist and using this information during the joint consultation, were reported most by rural doctors, those in small practices, Australian trained doctors and those who had practiced locally for up to 10 years. While generalisations cannot be drawn from this small qualitative study, it appears that rural doctors and those in small practices may receive fundamental educational benefits from participating in PIPC. Therefore targeting practices with these characteristics could be considered in future. In addition, while the PIPC program is not hailed as a professional development opportunity, it was identified by some participants as being convenient and cost-effective professional development. The difficulty of accessing continuing medical education and professional isolation are both recognised barriers to the retention of rural doctors31, so PIPC appears to be making a contribution to this workforce issue. Therefore this element has the potential to assist recruiting in rural practices.
An important finding of this study is the comprehensive reporting of longer term benefits due to involvement in PIPC. Those who most frequently report the longer term benefits of generalising the new knowledge to other patients and increased confidence from having the new knowledge spans all GP characteristics, but not all dimensions within. The dimensions of the characteristics reporting these benefits are: small practices; regional practices; doctors not Australian trained; those who had practiced locally for up to 10 years; and female doctors. The key result here is that such a broad range of GPs are reporting the generalisability of the new knowledge; and generalising the new knowledge is a key aspect of PC's goal of improving health outcomes for rural Australians in the longer term. Future PIPC programs could build on this result by targeting the dimensions of the characteristics in GPs who did not report this benefit.
It is clear that this novel but easily replicated approach to specialist outreach in the management of chronic disease, has the potential to improve health outcomes, and ultimately contribute to addressing the health and health service inequalities experienced in rural communities. Through the provision of continuing education for rural and regional GPs there is the additional potential to make a positive contribution to the well-known retention barriers of professional isolation and poor access to continuing education. While it is unlikely that the proportion of specialists in rural Australia will increase markedly, PIPC is a model that demonstrates how this scarce resource can be effectively utilised. Based on the early success of PIPC, two other specialties now use this model to provide services. While prudence is required in applying the results of this study, it does provide clear evidence of goal attainment, and importantly how the program could be targeted for greater effect.
Acknowledgements
The authors acknowledge the work of Ms Donna Boucher, Project Officer. The project the material is drawn from was funded by GP Connections, the Toowoomba Division of General Practice.
References
1. Department of Health and Ageing. Chronic disease. Canberra, ACT: Department of Health and Ageing, 2011.
2. WHO. Health topics - Chronic diseases. Geneva: WHO. (Online) 2011. Available: www.who.int (Accessed 28 August 2011).
3. WHO. Diabetes - Fact sheet No. 312. Geneva: WHO. Available: www.who.int.
4. AIHW. Australia's Health 2008. Cat. no. AUS 99. Canberra, ACT: Australian Institute of Health and Welfare, 2008 (Accessed 28 August 2011).
5. Dunstan DW, Zimmet PZ, Welborn TA, Cameron AJ, Shaw J, de Courten M et al. The Australian Diabetes, Obesity and Lifestyle Study (AusDiab)-methods and response rates. Diabetes Research and Clinical Practice 2002; 57: 119-129.
6. Dunstan D, Zimmet P, Welborn T, Sicree R, Armstrong T, Atkins R et al. Diabesity & Associated Disorders in Australia - 2000. The Accelerating Epidemic. The Australian Diabetes, Obesity and Lifestyle Study (AusDiab). Melbourne, VIC: International Diabetes Institute, 2001.
7. Britt H, Miller GC, Charles J, Henderson J, Bayram C, Valenti L et al. General practice activity in Australia 1999-00 to 2008-09. General practice series no. 26. Canberra, ACT: University of Sydney and Australian Institute of Health and Welfare, 2009.
8. Humphreys J, Wakerman J. Primary health care in rural and remote Australia: achieving equity of access and outcomes through national reform. A discussion paper commissioned by the National Health and Hospitals Reform Commission. Bendigo, VIC & Alice Springs, NT: Monash School of Rural Health & Centre for Remote Health, 2011.
9. AIHW. Rural, regional and remote health: indicators of health status and determinants of health. Rural Health Series no. 9. Canberra, ACT: Australian Institute of Health and Welfare, 2008.
10. Australian Government. National Strategic Framework for Rural and Remote Health. (Online) 2012. Available: www.ruralhealthaustralia.gov.au (Accessed 7 September 2012).
11. Yan W, Cheng TC, Scott A, Joyce CM, Humphreys J, Kalb G et al. Medicine in Australia: Balancing Employment and Life (MABEL). Australian Economic Review 2011; 44(1): 102-112.
12. AIHW. Medical labour force 2007. Canberra, ACT: Australian Institute of Health and Welfare, 2009.
13. Australian Government. Rural and Remote Health Workforce Innovation and Reform Strategy. (Online) 2012. Available: www.hwa.gov.au (Accessed 7 September 2012).
14. Australian Government. Medical Specialist Outreach Assistance Program. (Online) 2011. Available: www.health.gov.au (Accessed 7 September 2012).
15. Moffatt J, Eley D. Barriers to the up-take of telemedicine in Australia - a view from providers. Rural and Remote Health 11: 1581. (Online) 2011. Available: www.rrh.org.au (Accessed 7 September 2012).
16. Smith S, Allwrights S, O'Dowd T. Effectiveness of shared care across the interface between primary and specialty care in chronic disease management. Cochrane Database Systematic Review 2007; 18(3): CD004910.
17. Gruen R, Weeramanthri T, Knight S. specialist outreach clinics in primary care and rural hospital settings. Cochrane Database of Systematic Reviews 2003; 4: Art. no. CD003798.
18. Sibbald B, McDonald R, Roland M. Shifting care from hospitals to the community: a review of the evidence on quality and efficiency. Journal of Health Service Research & Policy 2007; 12(2): 110-117.
19. Powell J. Systematic review of outreach clinics in primary care in the UK. Journal of Health Services Research and Policy 2002; 7(3): 177-183.
20. Smith SM, Allwright S, O'Dowd T. Does Sharing Care Across the Primary-Specialty Interface Improve Outcomes in Chronic Disease? A Systematic Review. American Journal of Managed Care 2008; 14(4): 213-124.
21. Vierhout W, Knottnerus J, van Ooij A, Crebolder H, Pop P, Wesselingh-Megens A et al. Effectiveness of joint consultation sessions of general practitioners and orthopaedic surgeons for locomotor-system disorders. Lancet 1995; 346(8981): 990-994.
22. Marsh GN, Tompkins AB. Paediatric Care in General Practice: an Experiment in Collaboration. BMJ 1969; 2: 106-108.
23. Denzin NK, Lincoln YS, editors. Handbook of Qualitative Research. London: Sage, 1995.
24. Kvale S. Interviews: an introduction to qualitative research interviewing. Thousand Oaks: Sage, 1996.
25. AIHW. A guide to remoteness classifications. Canberra: Australian Institute of Health and Welfare, 2004.
26. ABS. 2011 Census Quick Stats. (Online) 2012. Available: www.censusdata.abs.gov.au (Accessed 2 September 2012).
27. AIHW. Medical labour force 2007. Canberra, ACT: Australian Institute of Health and Welfare, 2009.
28. Charmaz K. Grounded Theory. Objectivist and Constructivist Methods. In: NK Denzin, YS Lincoln (Eds). Handbook of Qualitative Research. Thousand Oaks: Sage, 2000; 509-535.
29. Strauss A, Corbin J. The Basics of Qualitative Research. California: Sage, 1990.
30. Alvesson M, Skoldberg K. Reflexive Methodology. New Vistas for Qualitative Research. London: Sage, 2000.
31. McDonald J, Bibby L, Carroll S. Recruiting and Retaining General Practitioners in Rural Areas: Improving Outcomes through Evidence-Based Research and Community Capacity-Building Evidence-Based Review: Final Report. Ballarat, VIC: University of Ballarat, 2002.
32. Gillam SJ, Ball M, Dunne H, Cohen S, Prasad M, Vafidis G. Investigation of benefits and costs of an ophthalmic outreach clinic in general practice. British Journal of General Practice 1995; 45: 649-652.
33. Bowling A, Stramer K, Dickinson E, Windsor J, Bond M. Evaluation of specialists' outreach clinics in general practice in England: process and acceptability to patients, specialists, and general practitioners. Journal of Epidemiology & Community Health 1997; 51: 52-61.
34. Spencer NJ. Consultant paediatric outreach clinics - a practical step in integration. Archives of Disease in Childhood 1993; 68: 496-500.
35. Hossain D, Moffatt J, Hansford G. Perceived value of the Physician in Practice Clinic approach to patients. International Journal of Health Promotion and Education 2012; 50(4): 194-202.


