Intellectual disability (ID) is an issue of importance in Australia because it affects 3% of the population1. More than 90% of people with ID live in the community and rely primarily on their GP for primary health care (PHC).
The Australian Association of Developmental Disability Medicine and other advocacy and medical organisations lobbied the Australian Government early in the last decade to fund annual health screening for people with ID2,3. In response to these efforts, the Australian Government through its publicly funded universal healthcare system Medicare, introduced specific items in the Medicare Benefits Schedule (MBS) in July 2007. The items allow GPs to provide comprehensive health assessments for people with ID at no cost to the patient, either at the surgery or through a home visit. The MBS defines eligibility in the following way4:
A person is considered to have an ID if they have significantly sub-average general intellectual functioning (two standard deviations below the average intelligence quotient [IQ]) and would benefit from assistance with daily living activities.
The annual comprehensive health assessment (ACHA) for people with ID provides for a regular review of the person's physical, psychological and social functioning. It allows for the appropriate involvement of the person's carer, support worker and/or case manager5. Following the introduction of ACHA for people with ID in July 2007, in the first 18 months 8700 people with ID received the assessment in Australia. There were some early successes in terms of GPs' enhanced capacity to detect important health problems in this population group6.
To place this Medicare initiative in context, it is part of a series of reforms introduced over a decade (documented on the Australian Government's Department of Health and Ageing website7), initially called Enhanced Primary Care but now Chronic Disease Management (CDM)8. Health assessments were funded for various population groups, such as the 'kids' health check' and a health check for refugees and humanitarian entrants7. In 2010, Medicare item numbers for CDM were overhauled and item numbers were related to the duration of the consultation, rather than the particular category of health check. This did not affect eligibility criteria for the different assessments. Medicare has retained the eligibility criteria and the recommended health check proforma for health assessment for a person with ID on the MBS website4.
The genesis of this study was a concern that the inequity in access to health services in rural communities might limit uptake of the health assessments in rural South Australia. There continues to be a maldistribution of health professionals favouring metropolitan centres9, and this inequity is increasing10. Primary care clinicians' hours of work are also longer the more remote their location10. Compared with those in metropolitan centres, the rural population has 20% higher reported rate of fair or poor health, and 10% higher mortality11. It seems likely that people with ID, who have comparatively less influence and voice, would experience greater problems with access, and an even higher risk of poor health outcomes. The sources of 'double disadvantage' arising from having a disability and living in a regional or remote community were identified in a 1997 study12.
This article presents the findings of a qualitative study that explored the take-up of ACHAs for people with ID in urban Adelaide and the Riverland region of rural South Australia.
The study used complexity theory as a theoretical perspective which assumes that general practice is an open complex adaptive system where changes in practice emerge as a result of the interactions of local agents13. The aim of this research was to gain a better understanding of whether and how people with ID access ACHAs. Sub-questions were: Which rural general practice characteristics affect access? and How is the role of general practice in delivering ACHAs viewed by people with ID and by doctors14.
Sampling
Theoretical sampling of interview participants was used to ensure the views of rural doctors and people with ID from rural and urban settings were captured. Data were triangulated through the inclusion of perspectives from managers of disability services and from carers and support workers (identified collectively as carers) in both rural and urban settings to clarify factors specific to rural areas.
Data collection
Semi-structured interviews of 20 min to one hour were conducted with people with ID and their carers in a rural town and in an outer suburb of Adelaide. Participants were asked about their experience with accessing health care, and with Medicare ACHAs in particular. Rural doctors from a number of towns and practices were also interviewed to find out how they perceived the Medicare ACHAs. All participants were sent information about the Medicare items relating to ACHAs for people with ID. Rural doctor participants also received a copy of the Medicare health assessment proforma4.
Data analysis
All interviews were audiotaped, transcribed, de-identified, numbered randomly and coded with pseudonyms for people with ID, and abbreviations for doctors (D), carers and support workers (C), and supported accommodation manager (M). These documents were analysed using thematic analysis, through a manual, paper-based process that included open coding, selective coding and constant comparison.
Additional theoretical sampling of participants allowed further development and saturation of themes15. Preliminary groupings were reviewed before further analysis to finalise the major themes emerging from the data. These themes were then used to review the original transcripts to ensure representation. For example, a preliminary grouping was made of coding where rural location was specifically mentioned. The codes were then refined into categories such as codes that related to rural community connectedness or the difficulty of getting to Adelaide. Once preliminary categorisation was complete, the categories were reassessed under seven prominent themes that were significant in answering the question, while outlier categories were set aside.
Meaningful and respectful inclusion of people with ID
Interviewing people with ID involves some challenges similar to that of providing their healthcare. The researchers set out with the intention of privileging the voices of people with ID as an important aspect of the methodology, which was consistent with the health equity focus of the study. The researchers noted that there were clear parallels between what is considered good practice in terms of health professionals' respectful communication, health service provision to people with ID, and principles of respectful inclusion in research.
First, participants gave their informed consent wherever able, with the carer as witness or if not able, the accommodation manager consented to their supported participation prior to the interview. The interviewer for this study [HB], who had little prior work or social experience with people who had severe or profound ID, took added steps to respectfully and actively include people with ID by: (i) ensuring the presence of a support person to assist in framing questions as well as interpreting responses; (ii) seeking to make the participant comfortable while gauging their level of cognition through the consent process and friendly conversation; (iii) framing questions that the participant could meaningfully answer (eg 'Do you remember going to see the doctor, what do you remember about it?') which often prompted discussion between the person with ID and their carer and provided richer contextual data; (iv) addressing questions directly to the person first; and (v) asking the participant's permission to direct a question to a carer if needing help to interpret a response.
Finally the data analysis involved an iterative process of interviews, self-reflection and discussion among the researchers about the data and to what extent particular responses should be included, to ensure that the voices of people with ID were neither overlooked nor overstated. Data were considered important to the study question where they illustrated the complexity of providing care as one of the benefits of comprehensive annual screening and where participants' comments or non-verbal communication revealed something of their experience of the health system, again, as context for this study. In summary, while not all participants could contribute to the same degree in terms of understanding the intent of the research, to the extent that they could understand and answer questions facilitated by the carer, this was experienced by the interviewer as valid and genuine participation and is presented as such in the results and discussion.
An example is provided of how the interviewer sought to ask questions directly (to Amanda) in a way that could be understood; and how the carer-proxy facilitated (Fig1). While it is often unclear whether Amanda understood questions because she often simply agreed, she sometimes expressed concern or a contrary opinion.

Figure 1: Example of the interviewer's direct questions and the carer-proxys' facilitation.
Ethics approval
The research was approved by Flinders University Social and Behavioural Research Ethics Committee; approval number 4358.
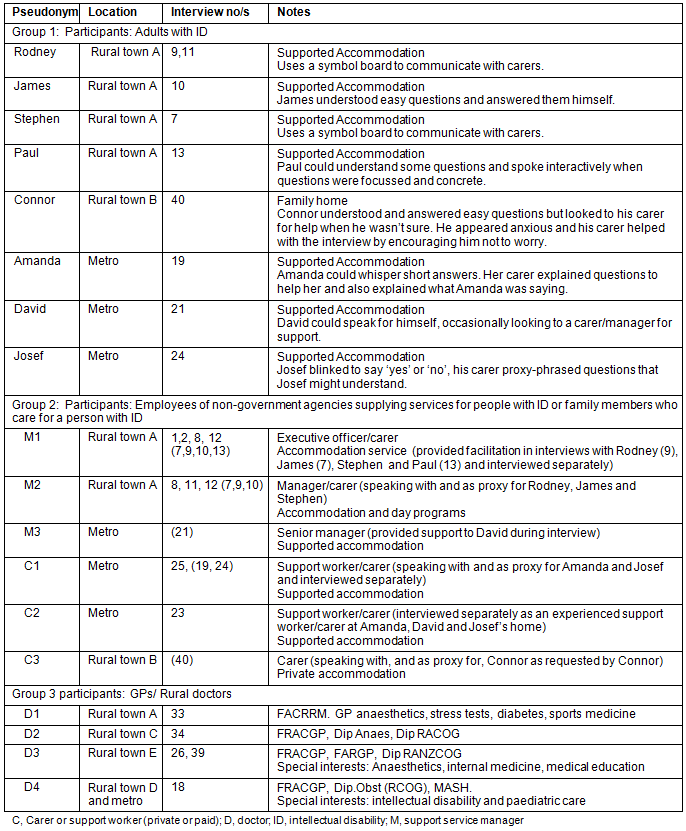
Eighteen participants were interviewed and their relevant background information is provided (Table 1). As described, carers acted as interpreters and/or proxies for either the participant or the interviewer, to facilitate the interview. When interview numbers are given in brackets, this indicates the involvement of the carer as a proxy and/or support, rather than a participant in that particular interview. Within the results tables and text, the examples given from the data are referenced by a code representing the participant and the interview: for example M1-7, where M1 is the participant identifier and 7 is the interview number from which the quote was sourced.
The first group of eight participants were people with ID from the following three locations: two rural towns (A and B) which are both more than 200 km from Adelaide (the nearest major urban centre) with populations of less than 10 000 people; and an outer suburb of Adelaide. Participants also included five employees of not-for-profit supported accommodation services located in rural town A and Adelaide, and one parent-carer (rural town B). The third group of participants, rural doctors, included a doctor (D1) from one of these rural towns (A) and another (D2) from a town of similar size in the same region (C). The third (D3) lives and practices in a small rural town (D) closer to the outskirts of Adelaide, as does the fourth doctor (D4 in town E), who also practises in Adelaide. Recruitment of doctors was challenging principally due to the workforce demands of rural practice. One doctor from each of a number of practices was purposively sampled to ensure a broad range of experience.
Table 1: Participants' relevant background information
Seven broad themes emerged relating to the role of the Medicare health assessment for people with ID, doctors and carers. A description is presented of the first three themes relating to the nature of rural communities and rural practice (Table 2). Each theme is presented with an outline of its sub-categories and the interviews in which the categories were coded.
Table 2: The nature of rural communities and rural practice

Theme 1: The healthcare barriers that all rural people experience have a greater impact on people with ID
For people with ID, the well-known barriers to health care in rural areas have a bigger impact. Rural patients often have a long wait to see a preferred doctor and for some people with ID, who may particularly benefit from seeing someone they are familiar with or who is comfortable communicating with people with ID, choice of doctor may not be offered, especially in times of workforce crisis. Other important factors include the need to be accompanied by a carer on trips to city specialists and the difficulty in sourcing appropriate and affordable accommodation.
A GP in the metro area, if he feels he needs specialist expertise, is more likely to say, 'Oh what I'm going to do is refer you to Modbury to the Centre for Intellectual Disability Health'. A rural GP has no ability to do that because it involves travel and overnights etc. [M1-1]
Theme 2: Rural communities provide connection, cohesion, consistency and comfort
Despite the disadvantages already outlined, several participants described the rural context as having advantages for people with ID. Rural communities were recognised as characterised by personal connections. Rural people with ID were described as more likely to remain in the same community, and they were visible, and recognised within the community. There was a sense of familiarity and continuity of relationships because people know each other in smaller towns. Doctors were also seen as and felt themselves to be part of the community. There was a perception that people with ID felt comfortable in familiar, less complex surroundings and had more help from local people. Both doctor-patient rapport and relationships among health and disability personnel were perceived as better by rural participants, as a consequence of these connections.
Funnily enough there's a lot more continuity rurally... The people don't change as often, the staff don't change as often, there's less mobility of the patients. [D4-18]
Theme 3: The way rural doctors practice
Doctors described that they most frequently assist patients who come to them with a specific reason of their own, and the doctor manages the medical care from there. Rural doctors, in the absence of specialists, expect to manage a broad range of health conditions in their community. The three exclusively rural doctors described responsibility for the health care of people with ID in their community in these terms and did not suggest that initiation and management of medical care for people with ID differed from the care given to any other patient. When discussing whether there was a need for special-interest care in ID health, these three doctors suggested that it was preferable for people to attend their local practice rather than to have one local sub-specialist provide care solely for people with ID.
I would always prefer people to go to their own doctor because you're looking at more than just the intellectual disability. There's a lot of fragmentation of medicine now, and I think that's the beauty of GP Management Plans is that you're bringing all the problems together. [D2-34]
By contrast, the ID special-interest doctor [D4-18] described the benefits of a more tailored approach to care and portrayed his own care for people with ID as a proactive, iterative process of gaining the patient's trust and gathering their medical history with cooperation from carers.
One rural carer suggested that it didn't matter whether care was provided by special-interest GPs or by generalist doctors as long as they had the specific skills and knowledge to give effective health care to people with ID. Two people with ID voiced satisfaction with the care they received from doctors when they were treated with respect and listened to.
Yep, they ask me if there's anything else and I usually tell them. It's good when they do that. [Paul -13]
Other (proxy) participants expressed the complexity of communication:
Q: Yep. And was the doctor, could you understand what he was saying to you?
M: Yep. [Stephen]
Q: Okay, that's good. Did he understand what you wanted to tell him?
M: Yep. [Stephen]
Carer: There was a fair amount of me explaining things that the doctor was saying to [Stephen], and vice a versa, and I'd have to say that, it wasn't an easy process to go through, because Dr [name] does have quite an accent and even I had problems picking up some of the things he was saying, so yeah, there was some issues there with communication. [M2-7]
An overview of the themes relating to challenges for implementation is given (Table 3). Each theme is presented with an outline of categories coded under it and the participants whose comments were coded.
Table 3: Challenges for implementation
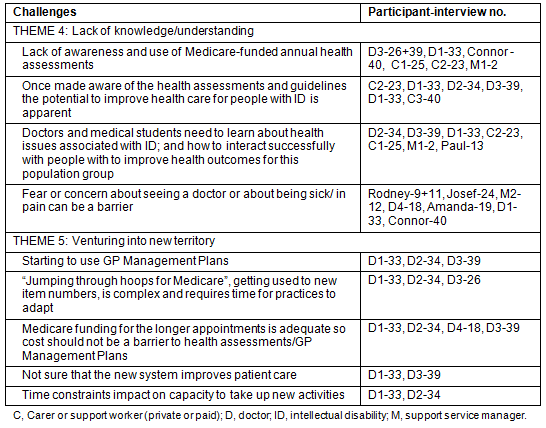
Theme 4: Lack of knowledge/understanding
Though the majority of people with ID and their carers in this study were not aware of the ACHAs, they were quick to identify the assessments' potential benefits. Health assessments were perceived as reassurance for carers that new health problems would be detected early and appropriate management could then occur. The opportunity for medication review was also seen as a benefit.
Few doctors were familiar with the ID-specific health assessments, although all were utilising CMD Plans to some extent. Doctors acknowledged that they did not have specific expertise in disability, and rural carers/support workers saw this as an issue because access to specialist services was reported as limited. Two doctors referred to patients they saw who suffered from dementia or mental illness (and not ID) although being asked quite specifically about ID in the interview. This suggested that they did not see many people with ID, and that in thinking about the care they provided, saw mental health and aged care as appropriate examples. It was acknowledged by doctors and carers that there were also gaps in doctors' awareness of disability services. Doctors did not automatically have awareness of, or referral to, disability services as part of their role. However, it was also seen as more likely in rural areas for doctors to know someone with expertise or interest in ID that they could contact for information and further support. Carers felt that doctors could take a more proactive stance in coordinating access to services that could improve their patients' quality of life.
Other important factors affecting the implementation of ACHAs were any that made a trip to the doctor arduous or anxiety-provoking for the person with ID or their carer.
Field note: Rodney was pleased to be interviewed but quickly became anxious, agitated and easily distracted onto other topics and concerns. Some of his anxiety was apparently triggered by talking about visiting the doctor and having his blood pressure tested which was an unpleasant recollection. [interview with Rodney, M1 and M2]
Several carers, from both rural and metropolitan sites, expressed a need for doctors to have more training in effective and respectful communication with and management of health issues for people with ID. Two GPs and two carers agreed that exposing medical students to people with ID would increase familiarity with and ability to provide appropriate care for people with ID (although whether or how this should be introduced into medical education was not an area of investigation in this study):
If they've got greater exposure to intellectually disabled people, then they'll learn more about it, just simply by the exposure... [D1-33]
Theme 5: Venturing into new territory
It was apparent that the broader Medicare changes concerning the introduction of CDM and its predecessor Enhanced Primary Care had impacted on practices, and that these Medicare items were being used to provide services to patients with a chronic disease. Within the framework of CDM, rural doctor participants had mixed feelings about whether taking a proactive approach to managing the health of people with ID would benefit patients and ultimately lead to better health outcomes.
If you were looking after a Down Syndrome child of yours in the community, then would one of these [ACHAs] change our management? It may or it may not. It may potentially bring it to [our] attention that we hadn't immunised them properly. So there may well be a change in the way we manage it because simply, having done this. [ D1-33]
However, the GPs acknowledged that people with ID and ID service providers were likely to value them and they considered how ACHAs might be useful.
I think, recognising that an intellectual disability in itself leads you to poorer health outcomes could be a trigger, if you like, almost mandating or making it easy for people with intellectual disabilities to have comprehensive health assessments and plans. [D3-39]
The principal barrier to undertaking ACHAs was that rural doctors are very busy. While the new CDM package has been refined and developed with the goal of addressing rural time constraints, doctors still need to be able to work through the practical aspects of implementation and to make decisions about what to prioritise.
Probably the main negatives that we have with any of these is actually, primarily based on time and being able to have the time to do that. That's probably, primarily a structure of how we work, rather than anything else. [D1-33]
An overview of the themes relating to evidence of progress is given (Table 4). Again, each theme is presented with an outline of its categories and list of participants with comments coded to these sub-themes.
Table 4: Evidence of progress

Theme 6: The practice nurse as knowledge holder, facilitator and implementer of care
The three solely rural doctors were providing chronic disease management using Medicare Item 721, the GP Management Plan. For each GP this involved a practice nurse making an initial assessment and drawing up a plan before the patient was seen by the doctor for the equivalent of (or not much longer than) a standard consultation, so that doctors were still able to see the same number of patients. Two of the doctors had used these plans for patients with ID.
We can still do them [GP Management Plans] in an appointment, or maybe a double appointment, but since the nurses do so much of the work for us it cuts down our time commitment dramatically, and they spend a lot of time discussing the issues that we don't often have time to discuss, like diet, exercise and things like that. [D2-34]
The increasing reliance on the practice nurse in CDM was seen by rural doctors as a source of hope that other health assessments could be progressively introduced as nurses worked through the implementation of the various components of the Medicare system.
Theme 7: The health communication triangle
The interaction between doctor, patient and carer as advocate/interpreter is fundamental to effective care. It works when the person with ID is supported to speak or communicate their own feelings and needs; the carer advocates for client-centred care; the carer uses their own knowledge of the person's history and capabilities to convey relevant information; and the doctor, with the help of the carer, is able to diagnose, prescribe and refer effectively in line with their patient's diagnosis and preferences.
A person with ID often relies on a carer/support worker to identify when they need to see a doctor and to organise taking them there. The majority of participants reported that a carer who knows the person very well and is sensitive to their needs and priorities could make a substantial difference to outcomes on a number of levels. A strong theme was the varying capacity for a person with ID to verbalise or to comprehend when something feels wrong.
Carers can assist the doctor by interpreting the person's body language and behaviour, potentially influencing the person to accept an intervention that is causing them concern, and reassuring the person about what is happening.
I had a toothbrush in my pocket and said, 'Open your mouth' and the client did and the doctor said 'Oh I've never seen anything', and I said 'Would you open your mouth for a wooden stick? I wouldn't.' You need to use things that are familiar to the clients so you need to actually set up the appointment to ensure success [be]cause the GP doesn't know. They deal with a whole bunch of people. [M1-1]
They can also make decisions about whether a doctor's behaviour towards the person with ID is appropriate and respectful. If not, they reported choosing whether to intervene or find a different doctor, or accept the situation if that is in the person's best interest. The manager and carers' stories about medical appointments suggested that despite challenges and dilemmas they were determined to secure the best possible care for their clients.
Well that's where you really need someone that's gone with the person that will speak up and be assertive, because otherwise, yeah you can't just stand back, you've got to really speak up for the client... [C1-25]
Rural doctors also commented that carers have an important role in, and make valuable contributions to the health assessment.
The rapport between the client and their carer, and the client and me, as the doctor is so much part of that whole process. [ D1-33]
Several participants commented on the benefit of carers providing a very detailed and comprehensive history because some people with ID cannot do this verbally. The patient having their own copy of their health record (which may be held for them by a carer/support worker) was considered beneficial so that other healthcare providers could add to it. The facilitation of patient empowerment through carer involvement was also suggested.
And the patients really do appreciate that now, when they do travel or see somebody or another health worker, they can just hand over this document which explains things to them and they find that very useful. [D2-34].
Discussion
Why don't people know about the health assessments?
This study found that since ACHAs were introduced in 2007, knowledge about their existence or benefits for people with ID had not reached many clients or their carers in either rural or urban settings. The only source of information about the health assessments uncovered by the researchers was that provided on state and Commonwealth Government health websites. A recent South Australian study confirmed that there are still barriers to internet use which indicate a 'digital gradient' where internet use correlates negatively with low income, low literacy, unemployment and housing status among other factors16. This suggests that complementary means of communication may be necessary to reach people with ID and their carers effectively.
An obvious potential source of information regarding ACHAs is the doctors themselves. However, this research revealed that rural doctors were also largely unaware that there are specific eligibility criteria to allow people with ID to access ACHAs, although information was included in Medicare bulletins that go to all medical practices. One reason might be the large number of other Medicare changes preceding and following the introduction of this particular health assessment, and the time it has taken for general practices to implement them.
General practitioners' lack of expert knowledge about ID may be another contributing factor. Three of the four doctors interviewed did not have expertise in ID. Only one rural doctor participant who had a special interest in ID, said he recommended the annual health assessments to clients. No other doctors in this study had considered how patients with ID could benefit from this Medicare initiative. Although the study sample size was small, these findings correspond with other studies which show that GPs do not have good knowledge of the health needs of people with ID, despite acknowledging their responsibility toward these patients17. People with ID can make an appointment through the Centre for Disability Health (CDH) in Adelaide. The CDH clinics use comprehensive health assessments for their patients, but the distance and complexity of travel to Adelaide, as well as prioritisation of clients with more complex needs, make access difficult for people in the Riverland region.
While it appears there is more work to be done before rural doctors will routinely offer health assessments to people with ID, they did report occasionally using GP Management Plans for these patients. This was specifically for the purpose of CDM, as for any at-risk patient, rather than an ACHA. Significantly, they did not see an automatic need to differentiate the model of care for people with ID from that of other patients. A tension emerged in the doctors' responses between the desire to treat people with ID the same as any other patient and their recognition that health assessments might support tailored care to detect health problems that might otherwise be missed, because of the patient's reduced ability to assess and seek advice about their own health status.
Progress in chronic disease management and the PHC model
On the positive side, when informed about the ACHA for people with ID, doctors agreed that the Medicare scheduled items made adequate allowance for the cost of assessing and planning for high-need patients, including the time for practice nurses to do the screening.
The implementation of so many Medicare changes in relatively few years presents serious challenges for rural general practices, which tend to be small businesses. Rural doctors, who are 'time poor', may have reason to avoid or delay new schemes they are not immediately equipped to implement due to capacity issues. Doctors emphasised a preference for simplicity, with one standardized format for CDM planning that could be used with any patient.
There was a general sense that the CDM model was met with some reluctance. Doctors perceived it as a departure from the traditional approach to consultation when patients had a specific health concern. Despite misgivings, the rural doctors in this study were beginning to take on the CDM model, and employ and train practice nurses in PHC health screening and planning. The findings suggested that, with appropriate information and training and effective coordination of services, nurses and other health professionals may become more proactive in encouraging people with ID to have annual health assessments by their doctor.
Other implications of being rural for access to health assessments
Rural doctors expressed some scepticism, suggesting that comprehensive health assessments for people with ID might not lead to better health outcomes for their patients. This may in part be due to their recognition of the lack of health services in rural areas. Access to city-based specialists and tertiary hospital care was predictably identified as a barrier to effective tailored health care by both rural carers and doctors, as in similar studies18,19. While rural location is not a barrier to having a comprehensive health assessment, the resulting care plan can be compromised if the doctor is unable to refer patients to specialists.
Despite this, the present study found that rural doctors are able to use their local connections to address healthcare needs as flexibly as possible with the services available. Where there was evidence that a particular doctor took a more active interest, became better informed and provided more tailored care for their patient with ID, it was not clear whether the advocacy of service providers and carers was a factor in the level of interest and awareness of the doctor, or whether they had sought out doctors who were more likely to invest time and energy in their clients. Further investigation into what motivates doctors to improve their care for people with ID may be helpful.
When rural participants were asked whether 'being rural' was a disadvantage in accessing health care they described rural communities as places that fostered stability and familiarity, which were seen as major assets when it came to the interests of people with ID. Participants saw marked benefits in being part of smaller rural communities, where people with ID were both visible and valued within the community, and where there was greater potential for linkages between rural doctors and disability organisations. There was also a sense of comfort because rural communities were perceived as less crowded and confusing than suburbia. In the context of rural people with ID being perceived as having a double disadvantage12, this important finding recognises the importance of stable relationships in the provision of health care and quality of life for people with ID.
More effective inclusion of carers in GP consultation
This study found that doctors reported frustration when a support worker did not know the patient well, could not interpret the patient's behaviour and body language or help the person understand what the doctor wanted to communicate, or did not have the person's medical history or health summary. Conversely, support workers reported seeking out doctors who are able to recognise and include them appropriately and effectively, and who above all are respectful to the person with ID.
The specific Medicare item number for comprehensive health assessment for people with ID was initially introduced to promote active involvement of the carer/support worker in a medical consultation5. Although the original item number has since been incorporated in the generic comprehensive health assessment item number, tools to support the health communication triangle between patient with ID, carer and doctor are still available on the Medicare website4. Four state governments in Australia have purchased a tool called the Comprehensive Health Assessment Program (CHAP) which is designed to assist recall, communication and transfer of information experienced by adults with ID, their carers and their GPs20,21. Such tools could further assist doctors to use the ACHAs in South Australia by promoting active involvement of carers; supporting the knowledge and health literacy of carers; and improving the transfer of information between the health and disability sectors and within the health sector.
Education and training for primary healthcare providers
This study revealed that rural doctors inevitably have some patients with ID; however, they are not equipped with specific skills and knowledge and rely on their generic skills, and do not necessarily identify people with ID as a priority group for preventative PHC. There is now a substantial body of research that confirms the value of annual health assessments in improving health outcomes for people with ID20,22,23. The Medicare funded ACHAs provide an opportunity for people with ID to live well and protect themselves from disease. If rural doctors are offered training and an opportunity to trial ACHAs they may appreciate the potential offered and be inspired to find ways to manage the administrative demands, leading to higher rates of annual screening. A 2009 study showed that when GPs received training, their use of GP Management Plans increased from very low to 20% above the national average24. Some medical schools such as Monash University now incorporate health care for people with ID in their curriculum25.
Though this study was small, its findings correlate with other studies into health access and screening for people with ID. There is a need for further research into targeted promotion and implementation of health assessments for people with ID. Evaluation and ID-specific training for doctors and medical students may further assist diffusion of both training and regular, effective screening.
Finally, having limited experience in ID, the authors found that meaningful inclusion of people with ID presented ethical challenges in how data was collected and interpreted. Our experience leads us to conclude that inclusion of people with severe and profound disabilities was justified because each participant contributed through their presence, their unique methods of engaging with the interviewer and their carer and support staff and through what they were unable to say, which allowed insight into the challenges they experienced when dealing with health professionals. This experience heightened the authors' understanding of the lives of people with ID and as a result they have become better advocates for people with ID.
People with ID in this study had not had an opportunity to access ACHAs. Rural people's access to effective generic healthcare was complicated by rural workforce issues and remoteness from major hospitals and specialised disability health services. Despite these frustrations, rural people with ID valued living in the country. The study found that rural people with ID enjoy greater social connectedness and more stability than city people. The authors recommend that these assets of rural community life should be harnessed when designing rural health promotion strategies and systems for people with ID.
Rural doctors need to be made aware of the evidence that routine health assessments improve health outcomes for people with ID. Many rural communities lack specialised disability health services, making it particularly important that rural doctors are supported to provide and promote ACHAs to ensure that the full benefit of this policy is realised for people with ID. The rural doctors in this study rightly saw that they had responsibility for the healthcare of people with ID in their communities. They felt that their practices were adequately remunerated to provide ACHAs but that they could be incorporated into normal appointment scheduling with appropriate input from practice nurses and carers. They identified continued support to employ and train practice nurses as an important element of the PHC model. Education about the benefits and effective use of the ACHAs for key stakeholders, including people with ID and their carers, health professionals and organisations that provide services for people with ID, may help the rural uptake of ACHAs.
Acknowledgements
This study was funded through a Flinders University Health Sciences research grant. The authors acknowledge Ruth Firstbrook, former CEO Lifestyles Assistance and Accommodation Service, who contributed significant expertise and guidance in carrying out the research; Dr Kwame Mfodwo, Monash University and Lucy Atkinson, Flinders University who proofread and provided comments on the readability and presentation.
References
1. Australian Institute of Health and Welfare. Disability in Australia: Intellectual Disability. Canberra, ACT: AIHW, 2008.
2. Lennox NG, T TM. Comment on Health care for people with intellectual disability. Medical Journal of Australia 2008; 189(2): 90.
3. Royal Australian College of General Practitioners. RACGP calls for increased support for Medicare services for people with disability (Media release). Melbourne, VIC: RACGP, 4 March 2005.
4. Australian Government Department of Health and Ageing. Medicare Benefits Schedule: Health Assessment for People with an Intellectual Disability fact sheet. Canberra, ACT: Commonwealth of Australia, 2011.
5. Australian Government Department of Health and Ageing. MBS Annual Health Assessment for People with an Intellectual Disability: Questions and Answers. Canberra, ACT: Commonwealth of Australia. (Online) 2010. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/mbsprimarycare-qandaintelldisability (Accessed 8 July 2013).
6. Simpson J. Medicare health checks reveal hidden suffering! Intellectual Disability Australasia 2009; 30(2). Available: http://search.informit.com.au/documentSummary;dn=706643469800131;res=IELHEA (Accessed 25 November 2012).
7. Australian Government Department of Health and Ageing. History of key MBS primary care initiatives 1999-2009. Canberra, ACT: Commonwealth of Australia. (Online) 2009. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/mbsprimarycare-History (Accessed 8 July 2013).
8. Australian Government Department of Health and Ageing. Removal of Enhanced Primary Care (EPC) terminology. Canberra, ACT: Commonwealth of Australia. (Online) 2010. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/mbsprimarycare-removalofepc (Accessed 8 July 2013).
9. Australian Government Department of Health and Ageing. Report on the Audit of Health Workforce in Rural and Regional Australia. Canberra, ACT: Commonwealth of Australia, 2008.
10. NRHA. Development and distribution of the health workforce. Contract no. 9. Canberra, ACT: National Rural Health Alliance, 2009.
11. NRHA. Fact Sheet: Measuring the metropolitan-rural inequity. Canberra, ACT: National Rural Health Alliance, 2010.
12. Gething L. Sources of double disadvantage for people with disabilities living in remote and rural areas of New South Wales, Australia. Disability and Society 1997; 12(4): 513-531.
13. Plsek P, Greenhalgh T. Complexity science: The challenges of complexity in health care. BMJ 2001; 323(7313): 615-618.
14. Rhydderch M, Elwyn G, Marshall M, Grol R. Organisational change theory and the use of indicators in general practice. Quality in Health Care 2004; 13(3): 213-217.
15. Strauss A, Corbin J. Basics of Qualitative Research: Techniques and Procedures for Developing Grounded Theory, 2nd edn. Thousand Oaks, CA: Sage, 1998.
16. Newman LA, Biedrzycki K, Baum F. Digital Technology Access and Use among Socially and Economically Disadvantaged Groups in South Australia. Journal of Community Informatics 2010; 6(2). Available from: http://ci-journal.net/index.php/ciej/article/view/639 (Accessed 27 May 2012).
17. Iacono T, Humphreys J, Davis R, Chandler N. Health care service provision for country people with developmental disability: an Australian perspective. Research in Developmental Disabilities 2004; 25(3): 265-284.
18. Iacono T, Davis R, Humphreys J, Chandler N. GP and support people's concerns and priorities for meeting the health care needs of individuals with developmental disabilities: A metropolitan and non-metropolitan comparison. Journal of Intellectual & Developmental Disability 2003; 28(4): 353-367.
19. Humphreys J, Wakerman J. Primary health care in rural and remote Australia: achieving equity of access and outcomes through national reform. A discussion paper commissioned by the National Health and Hospitals Reform Commission. Bendigo, VIC & Alice Springs, NT: Monash School of Rural Health & Centre for Remote Health, 2011.
20. Lennox N, Rey-Conde T, Cooling N. Comprehensive health assessments during de-institutionalization: an observational study. Journal of Intellectual Disability Research 2006; 50(10): 719-724.
21. Lennox N, Bain C, Rey-Conde T, Purdie D, Bush R, Pandeya N. Effects of a comprehensive health assessment programme for Australian adults with intellectual disability: a cluster randomized trial. International Journal of Epidemiology 2007; 36(1): 139-146.
22. Cooper S-A, Morrison J, Melville C, Finlayson J, Allan L, Martin G et al. Improving the health of people with intellectual disabilities: outcomes of a health screening programme after 1 year. Journal of Intellectual Disability Research 2006; 50(9): 667-677.
23. Robertson J, Roberts H, Emerson E, Turner S, Greig R. The impact of health checks for people with intellectual disabilities: a systematic review of evidence. Journal of Intellectual Disability Research 2011; 55(11): 1009-1019.
24. Pierce D. Identifying and addressing barriers to the use of enhanced primary care plans for chronic disease in rural practices. Australian Journal of Rural Health 2009; 17(4): 220-221.
25. Centre for Developmental Disability Health Victoria. Undergraduate - Curriculum. Melbourne: Monash University. (Online) 2007. Available: http://www.cddh.monash.org/undergraduate-curriculum.html (Accessed 8 July 2013).


