Supplying and maintaining an adequate medical workforce in rural and remote areas has been a long-standing challenge in Australia. In an endeavour to address this challenge, the regionally-located James Cook University (JCU) established a medical school in 1999 with a mission to address the health needs of its region, producing graduates not only capable of undertaking internship anywhere in Australia or New Zealand, but also with competencies relevant to rural, remote and tropical medicine and the health of Indigenous Australian communities1.
The school's pioneers designed a 6 year medical program based on the available evidence about initiatives that may better prepare doctors to work in rural and remote locations. These included: a selection process with ambitious targets for regional and rural background student numbers; curriculum and assessment practices developed in collaboration with rural community representatives; increased engagement with Aboriginal and Torres Strait Islander health issues and peoples; more frequent and longer clinical placements in small rural and remote settings; and recruitment of Faculty with substantial rural/remote experience2-5. Similar models have been adopted by several other new medical schools around the world6.
The JCU School of Medicine enrolled its first cohort in 2000, and by 2001 reported substantial progress towards implementing the model7. The program obtained accreditation by the Australian Medical Council in 2005, and by early 2011 had graduated 6 cohorts with a total of 445 students. Throughout this period the School achieved or exceeded rural enrolment targets, with 66% from designated rural areas across the whole of Australia, based on the Australian Standard Geographical Classification Remoteness Area (ASGC-RA) index8, and 69% of students from northern Australia - north of the Tropic of Capricorn from Rockhampton across to the Western Australian coast (Fig1). This high regional and rural representation reflects a process that includes an assessment of genuine interest in rural, remote, Indigenous and tropical medicine in written statements and interviews, and adjustment of academic scores for the 'rurality' of applicants' 12 years of schooling9. A final decision on admission is made via a combination of the scores from adjusted academic performance and interview.
Students undertake a 6 year MBBS course characterised by significant rural exposure, content, and mentorship from Year 1, strategies shown to play an important role in attracting medical practitioners to rural areas10. No student spends time in a capital city teaching hospital unless on an elective placement, and all students undertake a minimum 20 weeks of placement in small rural or remote towns - well above that occurring in other Australian medical schools at the time - with further opportunities available for extended rural experience.
The establishment of the JCU medical program occurred in the context of a doubling of medical schools and medical school places in Australia since the year 2000. Just under half of this expansion has occurred in regional Australia, and there has been concurrent establishment of outpost clinical schools in rural and remote locations11. JCU was the first of 9 new medical schools, one of a few that are oriented to meeting rural workforce needs. These and other policy measures are evidence of the community and political importance of strategies to deliver a rurally-oriented medical workforce.
There is as yet, however, little firm evidence that Australia's rural medical education initiatives have resulted in long-term improvement in the rural and remote medical workforce12. Many evaluations of the effect of rural undergraduate placements measure intentions rather than workforce outcomes13-16, reflecting the 10-15 year duration of training from entering medical school to becoming a recognised specialist.
The JCU Medical School has been established for approximately 12 years. This article reports a study of progress towards achieving the School's mission of positively influencing graduates' rural career intentions. Graduates' career intentions for the first 6 graduating student cohorts are explored and compared with similar data from other medical schools in Queensland and the rest of Australia. In addition, the actual internship locations of JCU graduates are reported, providing a more accurate picture of likely career choices than from earlier intention data.
Study protocol and survey
Two data sources were used to address different components of the study. The data on career intentions and intern year locations for the first 6 graduating JCU cohorts were from the annual, in-house exit surveys between 2005 and 2010 of students about to graduate. This written survey sought information on: preferred geographical location of future medical practice; location of internship; preferred medical career specialty (and whether they had changed this intention during the course); and intention to work in a rural area on course commencement (and if they had changed this intention). Students gave informed consent to participate and were free to decline or withdraw at any stage. Ethical approval for the study was obtained from the JCU Human Research Ethics Committee (# H1804).
The data for other medical schools was a secondary analysis of de-identified data obtained from the Medical Schools Outcomes Database & Longitudinal Tracking (MSOD) project, a collaboration of all Australian medical schools that collects periodic data from medical students and medical schools for the purpose of tracking the outcomes of basic medical education17. This analysis was covered by the MSOD project, which has approval by ethics committees18 at all participating Universities (see http://www.medicaldeans.org.au/medical-schools-outcomes-database/for-participants/university-human-research-ethics-compliance).
The MSOD Exit Questionnaire data from 2009 to 2010 were obtained to compare graduate career intentions of graduates from other Australian medical schools with those from JCU. These data were chosen for three reasons: the years match most closely the JCU exit data; they were the most recently available MSOD data; and they were the first years that a majority of medical schools were included in the MSOD project. However, data were available for only 8 metropolitan-based medical schools: two in Queensland and six in other Australian states. None of the other new rurally-oriented medical schools had graduated any students by 2009, and three well-established schools had not yet joined the MSOD project. Hence, data from only 9 of the then 12 medical schools with comparable data were included in this study, comprising 66% of the Australian domestic medical graduate output in 2009 and 201011. The data appear to be representative of the Australian context because the mix of graduates from the leading 'group of eight' universities in the comparator sample was similar to that from all Australian schools other than JCU (76% vs 71%), as was the proportion of graduates from the 'new' medical programs established since the year 2000 (23% vs 20%).
Participants self-defined their preferred geographical location of practice in the JCU and MSOD exit surveys into five categories: capital city; major urban centre (population >100 000); regional city or large town (25 000-100 000); smaller town (<25 000); and international.
Internship locations in both surveys were categorized using the Australian Standard Geographical Classification Remoteness Area (ASGC-RA) classification system8, using the RA categories: RA1 - Major Cities of Australia; RA2 - Inner Regional Australia; RA3 - Outer Regional Australia; RA4 - Remote Australia; RA5 - Very Remote Australia.
Analysis
Data were coded numerically and entered into the computerized statistical package SPSS release 19 (www.spss.com). Frequency analyses were conducted to compare JCU medical school data with Queensland MSOD data. Confidence intervals for odds ratios (OR) were estimated using the Woolf (logit) method19, and p-values calculated using two-tailed Fisher's exact χ2 tests. Content analysis was conducted on the free text data gathered as reasons students had given for changing their intentions to work rurally and to work overseas.
A total of 292 Year 6 JCU MBBS students out of a possible 445 completed the exit survey from 2005 to 2010, an overall response rate of 66%. Response rates across the years were: 2005 (50/58, 86%); 2006 (15/72, 21%); 2007 (44/67, 66%); 2008 (55/67, 82%); 2009 (57/83, 69%); and 2010 (71/98, 72%). Queensland MSOD data was derived from a total of 720 participants from other Queensland schools and a total of 1457 participants from 6 universities from all Australian states except Tasmania.
Major outcomes for the 6 JCU graduate cohorts, compared with graduates from the comparator universities from Queensland and elsewhere, are summarised in tables showing preferred geographic location, the medical specialty that students were most interested in pursuing at graduation, and the geographic area (ASGC-RA index)8 for the Australian city or town where JCU graduates had been accepted to undertake an internship (Tables 1-3, respectively).
Table 1: Preferred geographic location of future medical practice at graduation from medical school
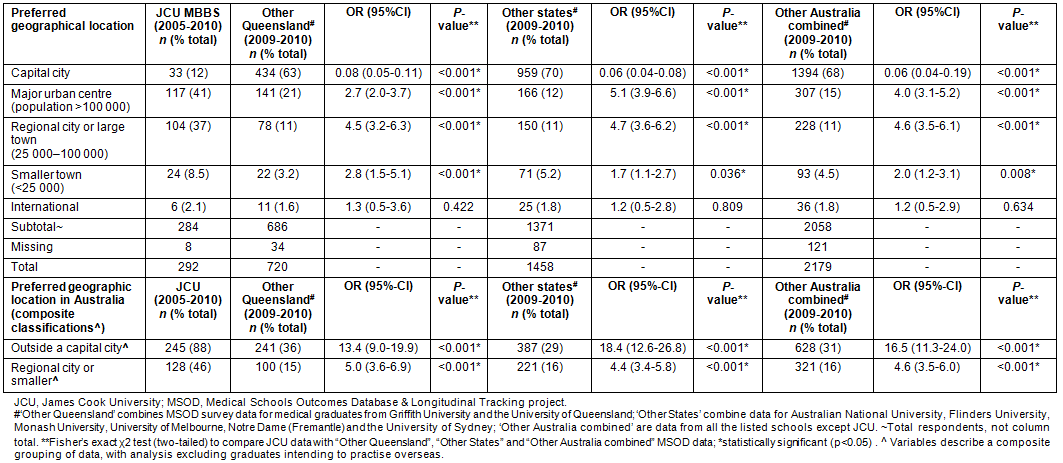
Table 2: Preferred medical career specialty at graduation from medical school
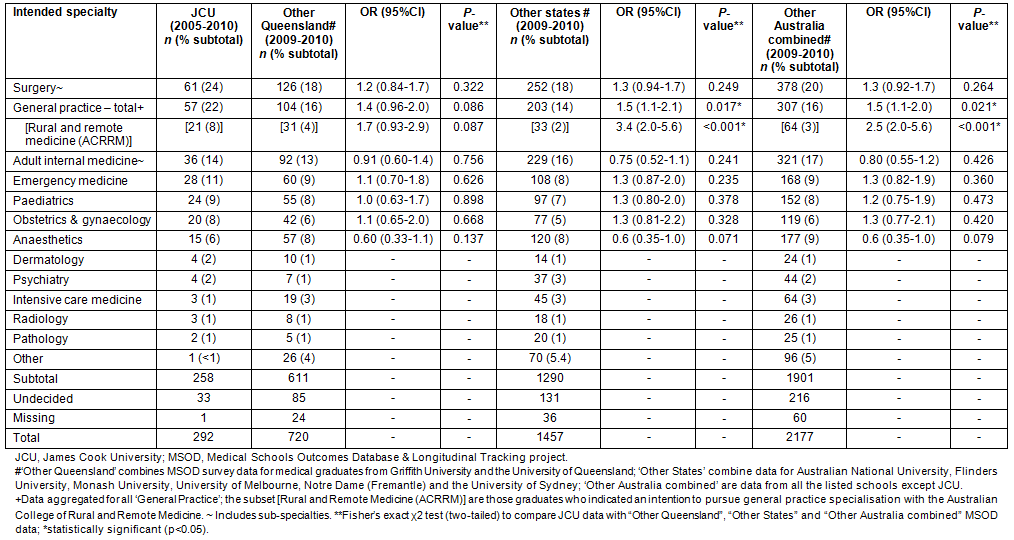
Table 3: Geographic classification (Australian Standard Geographical Classification Remoteness Area index) of city or town where medical graduates are to undertake internship
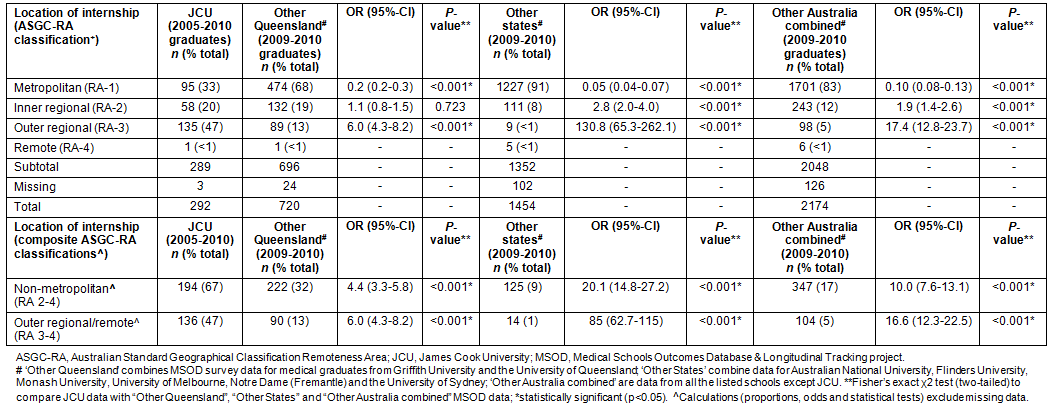
Internship practice location for 289 JCU MBBS graduates from 2005-2010 is also displayed (Fig1). Fifty-two percent of JCU graduates undertook internships in northern Australia, in particular: Townsville (32%), Cairns (14%), Mackay (5%) and Darwin (1%). A further 8% of graduates undertook their internship in Nambour, 3% in Toowoomba, and 2% in Rockhampton - all Queensland Inner Regional locations.
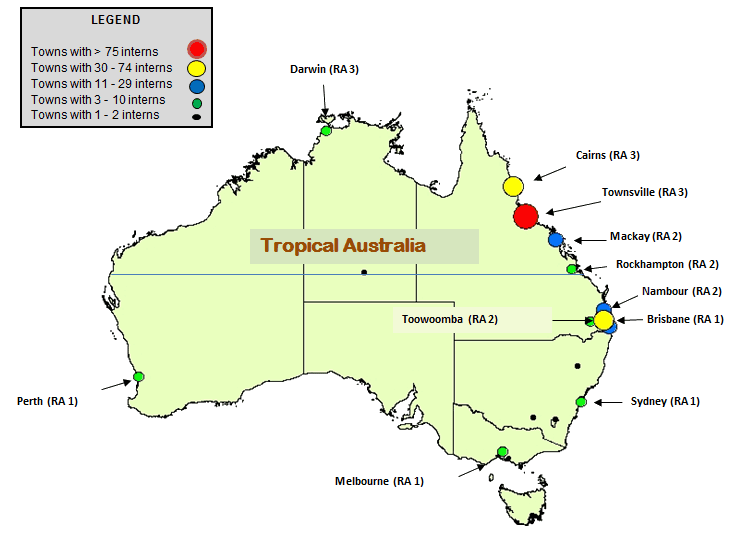
Figure 1: Location (city or town) of where JCU MBBS graduates (n=289) were accepted for internship between the years 2006 and 2011. Size and colour of the circle represents the number of JCU MBBS interns who spent the majority of a calendar year in that city or town. Large red circle = Townsville (>75 interns); yellow circles = Cairns and Brisbane (30-74 interns); blue circles = Mackay, Nambour and the Gold Coast (11-29 interns); green circles = Rockhampton, Darwin, Toowoomba, Perth, Sydney and Melbourne (3-10 interns); black dots = 1 or 2 interns. RA, Remoteness area (Australian Standard Geographical Classification).
The JCU Exit Survey explored, in an open-ended question, whether students reportedly changed their most-preferred medical specialty and/or intention to work rurally and overseas since commencing the course, and main reason for this change. Overall, 50% of JCU graduates (143 of 284) changed their choice of postgraduate discipline over the duration of the course, almost all (92%) as a result of exposure to different disciplines during clinical and rural placement experiences.
At entry to the course, 197 (68%) of JCU graduates intended to work 'in a rural area' and this increased to 220 (76%) by graduation, with 117 students overall changing intentions to work rurally during the course. Of these 117, 102 (87%) indicated they now wanted to do some rural practice, with almost two-thirds (64) wanting to have a rural-urban mix ('urban for a while and rural for a while'; reason not specified), 23 intended to now work rurally because of positive experiences during rural placement, 10 wanted to work rurally because 'there are more career opportunities working rurally', and 5 because of 'increased interest in rural medicine'. Only 15 students changed their intention to no longer wanting to work rurally at graduation, with reasons given including: 'intended training and career opportunities only available in metropolitan areas' (7 students); 'new partner' and/or 'family commitments' (5); 'placement experiences raised my awareness of a lack of clinical support in rural practice' (2); 'over-exposure to rural [in the JCU MBBS curriculum]' (2); and, 'want to work in a big city for a while' (1).
Only 3 students intended to work at least sometime overseas at the start of the course, increasing to 91 (31%) by graduation. Ninety of the 91 graduates changed their intention either because of increased knowledge of overseas work opportunities (79 students) or a personal desire to help people in low-income countries (11 students).
Discussion
This study shows that JCU medical graduates appear to prefer different geographic locations of future medical practice and different specialty interests than those from other Australian medical schools in this study, as was predicted by the design of the program. At graduation, almost nine in ten JCU graduates intended to practise outside capital cities, compared with approximately one-third of graduates from elsewhere (Table 1). Just under half of the JCU graduates intended to work in rural towns or small regional towns and centres (population <100 000), compared with one in six from the comparator schools. Both larger regional and smaller rural and remote locations in Queensland (along with other rural and remote areas in Australia) could expect workforce benefits from JCU graduates.
Further, chosen internship locations for JCU medical graduates are consistent with the rural career intent data (Table 3). Two-thirds of JCU medical graduates undertook internships outside an Australian metropolitan centre, compared with one in six from comparator schools. Approximately half the JCU graduate internships were in outer regional or remote locations compared with only 5% elsewhere. While over half of JCU graduates undertook internship in northern Australia (the region they had trained in), they also accepted internships in other rural and regional locations nationally, suggesting a general positive rural workforce impact (Fig1). However, the proportion of JCU graduates undertaking internship in a metropolitan area (33%) is higher than the 12% who indicated a wish to ultimately practise in such locations, suggesting that factors such as training pathways, availability of posts (internship allocation is currently state-based), and the desire for a metropolitan life- or work-experience may influence internship choice. Further exploration of this issue is needed, because an association between rural internship and medical graduate rural practice has been reported14,20-22. Hence, it may be important to expand postgraduate training opportunities more in regional and rural than in metropolitan areas.
Data on intended field of medical specialisation (Table 2) revealed that JCU medical students at graduation had a greater career interest in general practice and rural medicine compared with graduates from other Australian schools, although not in comparison with other Queensland schools, suggesting that the more decentralised Queensland context may be different. In other respects, JCU graduates' specialty career preferences were similar to those of medical graduates elsewhere. The degree to which these intentions translate to definitive career choices remains to be seen, because half the JCU graduates in the exit survey changed their choice of postgraduate discipline during the course and not all graduates were yet in formal postgraduate training programs. However, while medical students tend to commence their medical education without a clear view on their intended careers and only limited knowledge about some specialties from the popular media23, the JCU program ensures that graduates are aware of the careers aligned to the specific rural, remote and Indigenous health interests of the university.
It is not possible from these data to determine the impact of individual rural medical education initiatives on career outcomes, but it is possible to state that the combination of initiatives including selection, curriculum, assessment and role modelling appear to have resulted in different outcomes from those of the comparator metropolitan schools. It is likely that entering students are more aware of rural and regional career possibilities and more attracted to a non-metropolitan lifestyle. During the program, they follow a curriculum delivered in non-metropolitan contexts, and are exposed almost exclusively to non-metropolitan medical practice and professional role models. It is interesting to note that the proportion of JCU students intending to work rurally increased over the course from 68% at entry to 76% at graduation; this is positive news for Australia's underserved rural and remote communities. The proportion of JCU graduates interested in working overseas (almost one-third) is worthy of further exploration. While the extent to which this will translate into practice is not known, the outcome is consistent with the humanitarian themes of the JCU program.
Limitations
There are some limitations to this study. Surveys of career intention have limited predictive power, although the different profile of responses between JCU graduates and others nonetheless suggest that desired workforce outcomes are likely. The response rate of the second graduating cohort was low (21%), due to the timing that year of questionnaire administration, but the overall response rate of 66% is reasonable. Comparative MSOD data was available for only two other Queensland and six other national schools in 2009-2010, none of which had a whole-of-school focus on rural medical education. All schools were, however, participating in a range of Government-funded rural initiatives, albeit differently and none to the degree that the JCU program offers. Inclusion of data, when available, from other new schools with a strong rural focus is recommended in future research. Finally, the information on whether or not impending graduates changed their intention to work rurally and to work overseas over the course duration is obtained solely from the exit survey; thus, these recollections are subject to recall bias.
Early trends from the first six cohorts to graduate from the JCU School of Medicine suggest that the school appears on track to meet its mission to address the workforce needs of northern and rural Australia. Most graduates have been accepted to undertake their internship in Queensland, and are much less likely to want to work in metropolitan areas than graduates from other Queensland and Australian medical schools, with nearly all graduates preferring larger non-metropolitan, outer regional and rural centres.
The JCU graduates are interested in a broad range of specialties, and are more likely than other graduates to be interested in general practice and rural medicine. Long-term studies will be needed to fully understand the workforce impact of the first of Australia's 'new' medical schools. The data provide further evidence to support continued investment in the decentralisation of medical education. Additional positive benefits for rural workforce might be expected as graduates from other rurally-oriented medical schools commence vocational training.
Acknowledgements
The research on which this article is based used data provided by the Medical Schools Outcomes Database (MSOD) Project, Medical Deans Australia and New Zealand. The authors are grateful to the Australian Government Department of Health and Ageing for funding the project from 2004 to 2011, to Health Workforce Australia for funding from 2011 onwards and to the medical students, graduates and doctors who participated.
References
1. Hays RB. A new medical school for regional Australia. Medical Journal of Australia 2000; 172(8): 362-363.
2. Hunt DD, Norris T, Ballweg R. The University of Washington WAMI program: 25 years of experience with manpower shortages in rural areas. Australian Journal of Rural Health 1995; 3: 152-158.
3. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
4. McDonald J, Bibby L, Carroll S. Recruiting and retaining general practitioners in rural areas: improving outcomes through evidence-based research and community capacity building. Evidence-based review: Final Report. Ballarat, VIC: Centre for Health Research and Practice, University of Ballarat, 2002.
5. Verby JL, Newell JP, Andresen SA, Swentko WM. Changing the medical school curriculum to improve patient access to primary care. JAMA 1991; 266: 110-113.
6. Tesson G, Curran V, Pong RW, Strasser R. Advances in rural medical education in three countries: Canada, The United States and Australia. Education for Health 2005; 18(3): 405-415.
7. Hays RB. Rural initiatives at the JCU School of Medicine: a vertically integrated regional/rural/remote medical education provider. Australian Journal of Rural Health 2001; 9(Suppl): S2-5.
8. Australian Bureau of Statistics. ASGC Remoteness Classification: purpose and use. Census paper # 03/01. Canberra, ACT: Commonwealth of Australia, 2003.
9. Hays RB, Bower AJ. Modifying academic ranking of rural and remote medical school applicants. Medical Journal of Australia 2001; 174: 371-372.
10. Somers G, Strasser, R. Do rural mentors, rural undergraduate clubs and rural rotations increase the medical student's intention to practise in the country. In: Proceedings, Australian College of Rural and Remote Medicine, Scientific Form; 30 April 2002; Melbourne, VIC; 90-94.
11. Australian Government. Medical Training Review Panel, Fifteenth Report. Canberra, ACT: Commonwealth of Australia, Feb 2012. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/work-pubs-mtrp-15 (Accessed 31 July 2012).
12. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: www.rrh.org.au (Accessed 31 July 2012).
13. Worley PS, Prideaux DJ, Strasser RP, Silagy CA, Magarey JA. Why we should teach undergraduate medical students in rural communities. Medical Journal of Australia 2000; 172: 615-617.
14. Rolfe IE, O'Connell DL, Pearson SA, Dickinson JA. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Australian and New Zealand Journal of Medicine 1995; 25: 512-517.
15. Hays RB, Nichols A, Wise A, Adkins P, Craig M, Mahoney M. Choosing a rural practice career in Queensland. Australian Journal of Rural Health 1995; 3(4): 171-174.
16. Walker JH, DeWitt DE, Pallant JF, Cunningham CE. Rural origin plus a rural clinical school placement is a significant predictor of medical students' intentions to practise rurally: a multi-university study. Rural and Remote Health 12: 1908. (Online) 2012). Available: www.rrh.org.au (Accessed 31 July 2012).
17. Humphreys JS, Prideaux D, Beilby JJ, Glasgow NJ. From medical school to medical practice: a national tracking system to underpin planning for a sustainable medical workforce in Australasia. Medical Journal of Australia 2009; 191(5): 244-245.
18. Medical Deans Australia and New Zealand. University Human Research Ethics Compliance. (Online) no date. Available: http://www.medicaldeans.org.au/medical-schools-outcomes-database/for-participants/university-human-research-ethics-compliance. (Accessed 31 July 2012).
19. Woolf B. On estimating the relation between blood group and disease. Annals of Human Genetics 1955; 19: 251-253.
20. Bowman RC, Penrod JD. Family practice residency programs and the graduation of rural family physicians. Family Medicine 1998; 20: 288-292.
21. Pathman DE, Steiner BD, Jones BD, Konrad TR. Preparing and retaining physicians through medical education. Academic Medicine 1999; 74(7): 810-820.
22. Rosenthal TC, McGuigan MH, Anderson G. Rural residency tracks in family practice: graduate outcomes. Family Medicine 2000; 32(3): 174-177.
23. Maudsley G, William L, Taylor D. Medical students' and prospective medical students' uncertainties about career intentions: cross-sectional and longitudinal studies. Medical Teacher 2010; 32(3): E143-E51.




