Authentic early experience (AEE) is now common in basic medical education. Placing students in clinical contexts appears to enhance the relevance and integration of foundation sciences to medical practice1,2, complement simulated learning by providing opportunities to practise clinical and communication skills3,4, and raise awareness of a wider range of potential career pathways, notably in primary care and rural practice1. Further, these early experiences may commence the important professional acculturation transition from student to doctor5,6. At least anecdotally, they offer 'vocational testing' for students, with the majority gaining affirmation of their career choice and a minority realising that they are unsuited to a medical career. These placements are accepted well by students, teachers and patients2,7. From a management perspective, early placements have opened up previously unused supervision capacity, particularly outside of large academic hospitals, as programs seek a relevant clinical caseload to support their curricula8.
There can, however, also be unintended consequences. Placement providers sometimes feel poorly prepared for more junior learners and struggle to meet their expectations9. Early experiential learning sometimes appears disconnected from the curriculum and its assessment10. Students sometimes do not feel welcome or are unclear about expected outcomes, perhaps because of under-confidence or inexperience in adult learning11,12. Occasionally students feel traumatised after confronting challenging situations, such as death, for the first time10,11. There may also be concerns about patient safety if students act beyond their level of training without appropriate supervision. However, most of the evidence comes from student and teacher perception surveys7, and it is unclear how well grounded AEE is from the perspective of educational theory. The more general topic of experiential learning is best supported by situated learning theory13, but this may be more relevant to senior clinical placements, when few would challenge the need for substantial clinical experience that synthesises theory and practice as preparation for the transition to junior doctor5.
With the recent (and continuing) expansion of health professional education at basic, postgraduate and specialist levels to meet workforce needs14, healthcare facilities are becoming crowded with learners from several health professions at all levels, and there is strong competition for the available learning resources. The value of 'mainstream' healthcare facilities (hospitals and general practices) may be less clear for more junior students who do not yet have much knowledge of health science or systems and have not yet developed their clinical skills12. It is therefore worth considering what impact this expansion is having on the efficient utilisation of this valuable, yet finite, resource15,16. This article reports an analysis of the utilisation of Australia's healthcare system for early clinical placements, and aims to assist planning future medical education.
This study involved a secondary analysis of de-identified data obtained from the Medical Schools Outcomes Database & Longitudinal Tracking (MSOD) project, a collaboration of all Australian medical schools that collects periodic data from medical students and medical schools for the purpose of tracking the outcomes of basic medical education17. Data from medical students is collected via questionnaires administered at entry, exit, and postgraduate years (PGY) 1, 3, 5 and 8 (currently data is available only up to PGY 1), and medical schools provide annual data about placements and electives. The data obtained for this study concerned clinical placements in the first half of Australian medical courses in the 2009 academic year and included data from all 18 Australian medical schools, and so was able to provide a comprehensive national overview. The 'first half' of medical programs was defined as Years 1 and 2 for the four-year graduate-entry schools and Years 1, 2 and 3 for the five- and six-year standard-entry schools. Specific data obtained included the duration of clinical placements, the setting of the placements (hospital, GP, community health, Indigenous health, and other), and their location by postcode and town name (domestic or international). These data were aggregated by category to provide a detailed description of the utilisation of the health-care system at the time of maximal growth in basic medical education. In order to gain an understanding of the impact of all clinical placements, data was also obtained on the total number of clinical placements in all settings for all years during 2009.
Ethics approval
This analysis was covered by the MSOD project, which has approval by ethics committees at all participating universities (see http://www.medicaldeans.org.au/medical-schools-outcomes-database/for-participants/university-human-research-ethics-compliance).
Responses were received for 5117 of 7740 students (66.9%) enrolled in Years 1 and 2 (standard and graduate entry combined) and Year 3 (standard entry only). A total of 16 711 (99.6%) domestic and 67 (0.4%) international clinical placements were reported during 2009. International placements had a slightly shorter duration than domestic placements, but were so few that they were not a significant source of early clinical placements and may have been an elective for the more adventurous students. The data are summarised in Table 1.
Table 1: Years 1-3 domestic and international clinical placements
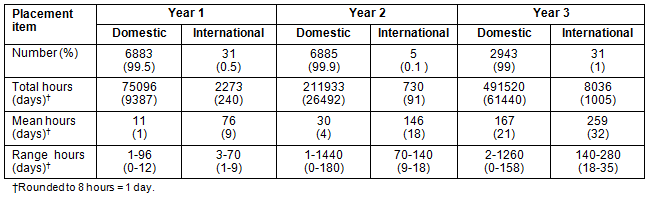
Focusing on the domestic placements, there were totals of 6883 (Year 1), 6986 (Year 2) and 2943 (Year 3) placements, representing totals, respectively, of 9387, 26 492 and 61 440 days of clinical placements. Placements increased in duration from Year 1 to Year 3, with mean durations, respectively, of 1, 4 and 21 days (ranges of 0.2-15, 0.2-180, and 0.2-180 days). On average, each student had 3.3 domestic early clinical placements during 2009, occupying a total of 97 319 days of clinical supervision and patient access in the Australian healthcare system. Placements were in a wide range of settings, including hospitals (81%), general practices (7%), community settings (7%), Indigenous health clinics (1%) and 'other' settings (4%). The setting 'other' was not clearly defined and may reflect coding confusion by medical schools, but, on closer examination of location data, were mostly (about two-thirds) in combinations of small hospital, general practice and other community settings in regional and rural communities. The other third were mostly quite short (1-3 hour) placements in large cities, perhaps including a wider range of health and social care settings. Approximately 1% of data was missing. The duration in most categories was bi-modal. Shorter placements were mostly in urban settings, whereas longer placements were mostly in regional and rural settings. These data are summarised (Tables 2-4).
Table 2: Year 1 domestic clinical placements in undergraduate and graduate programs according to category
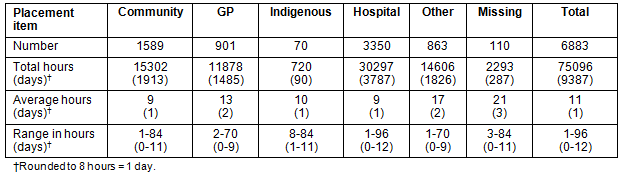
Table 3: Year 2 domestic clinical placements in undergraduate and graduate programs according to category

Table 4: Year 3 domestic clinical placements in undergraduate programs according to category
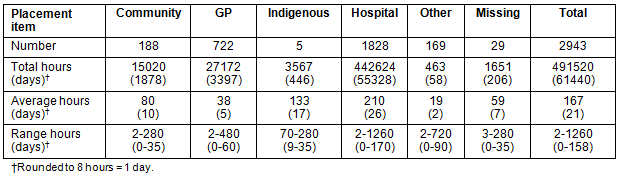
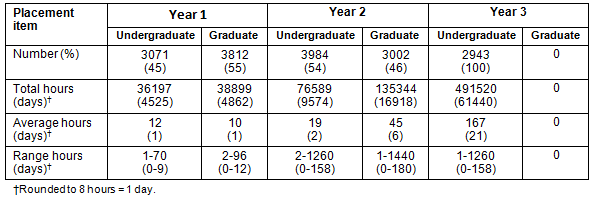
A comparison of the clinical placements of standard- and graduate-entry schools is provided (Table 5). In Year 1, the pattern of use is similar - large numbers of brief (mean of 1 day) placements, although the total duration of placements in standard-entry schools is greater. In Year 2, graduate-entry placements are longer, although less numerous, and with approximately equal utilisation by graduate and standard-entry schools. In Year 3, only the standard-entry schools have early clinical placements, but they have more intensive (total of 61 440 days) and longer (mean of 21 days) placements at a time when all schools have students in clinical placements for 100% of the final two academic years.
Table 5: Years 1-3 domestic standard and graduate-entry school comparison
The total number of domestic placements during 2009 in all settings for all years was 32 845, occupying 4 816 933 hours (602 117 days) of health system time. Hence, early clinical placements were responsible for about 16% of all clinical placement time in the Australian healthcare system.
Discussion
With the expansion of basic medical education, these data indicate that students are present in healthcare settings for at least about 600 000 days spread over approximately 200 working days each academic year, Considering that data from about one-third of students was not retuned, the figures are likely to be higher. A substantial proportion of placements appears to be in rural communities, where expansion of medical education has been promoted. The chances of patients encountering medical students, particularly in the public hospitals and general practice, are likely to be high, particularly in the light of other studies showing that only about half of inpatients are available for student interactions18. Therefore, although it is difficult to determine an optimal ratio of student to patient encounters, Australia's healthcare system, including regional and rural communities, appears to be utilised heavily for clinical placements. This study suggests that early clinical placements are responsible for about 16% to this load, using capacity in a wide range of hospital and community facilities. Hospitals and general practices carry the heaviest load, but substantial capacity is provided by a range of community facilities that are not general practice. Indigenous health facilities, considering their small number, are also providing a substantial number of placements and may be heavily utilised. Longer placements are more common in regional and rural communities, perhaps reflecting the trend towards the longitudinal integrated clerkship model offered by some rural-oriented programs.
What is not clear from the data is precisely what medical students do in the healthcare facilities during early clinical placements, or the specific roles that the organisations or their health professionals play in student learning. No data on resource allocation to them is available, although there are funding schemes available to support some rural placements. However, it is unlikely that early clinical placements are cost-neutral for host organisations or that junior medical students can contribute to service delivery to even the limited extent possible with senior students, particularly in longer primary care placements19. The total of almost 100 000 days of engagement with more junior students is therefore likely to be at substantial cost to the health and social care system, and may represent a significant, currently understated, contribution to the cost of basic medical education.
The benefits of early clinical placements need to be weighed against their resource and opportunity costs. Although goodwill remains a strong and essential feature of basic medical education, these data raise important questions about how medical education should prioritise utilisation of the healthcare system for both undergraduate and postgraduate education. Clinical experience is an essential part of medical training, although the duration appears to vary substantially among programs that range from 4 to 6 years in total duration, and so far there is little evidence on which to determine the 'ideal' timing and duration of clinical experience. Further research is needed on the educational benefits of AEE, particularly the potential to link theory to practise and facilitate earlier competence20. Until this is clearer, the imposition on healthcare facilities of a heavy and increasing clinical supervision load raises questions about prioritisation and the possible dilution of experience of more senior medical students who need experience to prepare for early postgraduate roles and responsibilities. Would it be more sensible to focus that effort (and resource cost) on those who would benefit most from experience in 'frontline' health care? This may mean reducing the use of major hospitals and general practice for early clinical placements. In particular, shorter placements, which are more likely to be observational than participatory, could be relocated to less acute health and social care settings, where an emphasis on understanding the broader healthcare context and practising interpersonal and diagnostic skills may be achievable. One outcome should be less impact on patient care pathways and supervisory capacity in more acute care settings, where students requiring immersion in practice - those in longitudinal and senior placements - can be given increased experience.
Limitations
This study provides only high level data that describes the national utilisation of the healthcare system. It is possible that utilisation may vary from region to region, and for unused capacity to be available in regions more distant from medical school locations.
At a time when the capacity for teaching of the Australian healthcare system appears to be reaching its limits, more efficient utilisation of the healthcare system may be facilitated by the development of much clearer expectations of, and support for, early clinical placements. This may allow for priority to be given for more senior clinical placements in more acute clinical settings, and the expansion of early clinical placements into less acute health and social care settings, where learning outcomes can be achieved with less impact on service providers and patient care pathways.
Acknowledgement
The research on which this article is based used data provided by the Medical Schools Outcomes Database (MSOD) Project, Medical Deans Australia and New Zealand. The author is grateful to the Australian Government Department of Health and Ageing for funding the project from 2004 to 2011, to Health Workforce Australia for funding from 2011 onwards and to the medical students, graduates and doctors who participated.
References
1. D'Amore A, Mitchell EK, Robinson CA, Chesters JE. Compulsory medical rural placements: senior student opinions of early-year experiential learning. Australian Journal of Rural Health 2011; 19(5): 259-266.
2. Howe A, Dagley V, Hopayian K, Lillicrap M. Patient contact in the first year of basic medical training - feasible, educational, acceptable? Medical Teacher 2007; 29: 237-245.
3. Bokken L, Rethans JJ, van Heurn L, Duvivier R, Scherpbier A, van der Vleuten C. Students' views on the use of real patients and simulated patients in undergraduate medical education. Academic Medicine 2009; 84: 958-963.
4. Haffling AC, Håkansson A, Hagander B. Early patient contact in primary care: a new challenge. Medical Education 2001; 35: 901-908.
5. Brennan N, Corrigan O, Allard J, Archer J, Barnes R, Bleakley A, Collett T, de Bere SR. The transition from medical student to junior doctor: today's experiences of tomorrow's doctors. Medical Education 2010; 44: 449-458.
6. Bleakley A, Brennan N. Does undergraduate curriculum design make a difference to readiness to practice as a junior doctor? Medical Teacher 2011; 33: 459-467.
7. Dornan T, Littlewood S, Margolis SA, Scherpbier A, Spencer J, Ypinazar V. How can experience in clinical and community settings contribute to early medical education? A BEME systematic review. Medical Teacher 2006; 28: 3-18.
8. Colquhoun C, Hafeez MR, Heath K, Hays RB. Aligning clinical resources to curriculum needs: the utility of a group of teaching hospitals. Medical Teacher 2009; 31: 1084-1088.
9. Smithson S, Hart J, Wass V. Students' hopes and fears about early patient contact: lessons to be learned about preparing and supporting students during the first year. Medical Teacher 2010; 32: e24-30.
10. Yardley S, Brosnan C, Richardson J, Hays R. Authentic early experience in medical education: a socio-cultural analysis identifying important variables in learning interactions within workplaces. Advances in Health Sciences Education: Theory and Practice (Online) 2012. DOI 10.1007/s10459-012-9428-2.
11. Kelly E, Nisker J. Medical students' first clinical experiences of death. Medical Education 2010; 44: 421-428.
12. Seabrook MA. Clinical students' initial reports of the educational climate in a single medical school. Medical Education 2004; 38: 659-669.
13. Yardley S, Teunissen PW, Dornan T. Experiential learning: AMEE Guide No. 63. Medical Teacher 2012; 34: e102-15.
14. Health Workforce Australia. Health Workforce 2025 - Doctors, nurses and midwives, Volume 1. Adelaide: Health Workforce Australia, 2012.
15. Sen Gupta TK, Woolley T, Hays RB, Seidl I, Johnson A. Challenges with maintaining clinical teaching capacity in regional hospitals. Medical Journal of Australia 2011; 195: 584-585.
16. Hays RB, Oldfield K. Challenges to GP teaching capacity. Australian Family Physician, 2006; 35: 935.
17. Humphreys JS, Prideaux D, Beilby J, Glasgow NJ. From medical school to medical practice: a national tracking system to underpin planning for a sustainable medical workforce in Australasia. Medical Journal of Australia 2009; 191: 244-245.
18. Olson LG, Hill SR, Newby DA. Barriers to access to patients in a group of teaching hospitals. Medical Journal of Australia 2005; 183: 461-463.
19. Hudson JN, Weston KM, Farmer EA. Medical students on long-term regional and rural placements: what is the financial cost to supervisors? Rural and Remote Health, 12: 1951. (Online) 2012. Available: www.rrh.org.au (Accessed 18 March 2013).
20. O'Neill PA, Willis SC, Jones A. A model of how students link problem-based learning with clinical experience through 'elaboration'. Academic Medicine 2002; 77: 552-561.

