Health adaptation
If climate change is the biggest global public health threat faced in the 21st Century1, research faces major challenges of providing adequate evidence for already vulnerable communities to adapt to the health effects of climate change. A growing body of scholarship, particularly since the mid-2000s, suggests that climate change works to further disadvantage groups with already unequal health outcomes1-5. The evidence of major disasters such as Hurricane Katrina6-8 in New Orleans, and the historic 2010-2011 Queensland floods9 in Australia, further suggests the socio-economic basis of climate effects, regardless of the contribution of carbon emissions to such extreme events.
For Australian rural communities, the experience of the Victorian bushfires10 and the Queensland floods9 has underscored the ways in which people in these communities are often isolated from centralised climate management supports, ranging from risk assessment and warning systems to impact and recovery supports. In the wider climate change literature, rural and remote Aboriginal communities have been described as occupying many of the climate change 'hotspots' of the future, by virtue of both their geographic isolation and their socio-economic disadvantage11.
Accordingly, the impacts of climate change are shaped by 'where you live', your resources and your access to infrastructure, and this is why climate change has been seen as a social justice challenge, not simply a challenge to do with managing carbon emissions11.
However, knowledge about adaptation has been relatively slow to develop. In global policy frameworks, adaptation was much less emphasised than mitigation (taking action to reduce carbon emissions) until the 2001 third assessment report of the Intergovernmental Panel on Climate Change (IPCC) which offered a stronger evidence-based understanding of adaptation12. Since then there has been a growing awareness of the importance of adaption, especially in relation to supporting already disadvantaged groups such as rural and Aboriginal communities.
The 4th assessment report of the IPCC defined 'adaptation' as an '[a]djustment in natural or human systems in response to actual or expected climatic stimuli or their effects, which moderates harm or exploits beneficial opportunities'13. The objectives of adaptation have been described in terms of pre-emptive capacity-building, risk reduction, increasing coping and resilience after climate events, and building opportunities presented by climate change14. In health, the adaptation mechanisms are found largely through health service development and can include development of15:
- Health service governance and culture, such as public education programs about heat health.
- The way services are delivered.
- Workforce, through education and training of health professionals.
- Material infrastructure, for example, through risk management for health assets like buildings.
- Finance, for example, development of financial strategies for making adaptation cost effective.
The sorts of activities that might be described as adaptation activities vary and can include, but may not be restricted to, sharing and bearing loss and risk, as well as preventative or risk avoidance actions16.
Current global policy frameworks such as the UN Cancun Agreements17, as well as the relevant WHO resolution WHA61.1918, interpret best practice in adaptation as involving: (i) a strong focus on local community experience and knowledge in developing adaptation; and (ii) research methods that engage with localised health-service development and decision-support needs. The recent watershed 2011 IPCC report on adaptation also emphasises the importance of locally-focussed evidence tailored to the needs of groups already experiencing unequal outcomes because '[i]nequalities influence local coping and adaptive capacity, and pose disaster risk management and adaptation challenges from the local to national levels'19. This emphasis on community-based approaches to adaptation that harness local knowledge is also in emerging research, including research on the health adaptation of Aboriginal people20,21.
The 1994 United Nations Framework Convention on Climate Change ('the UN Convention'), agreed to by 195 Parties to the Convention included an article (Article 4) that required countries to develop and implement mitigation and adaptation plans22. By 2012, a growing number of countries have developed national adaptation plans, including for health23-43. These will hopefully help address the indications that local public health leaders care about climate change but understand less how to make it a priority in health system development44. However, the evidence of applied and scholarly reviews of adaptation over the last few years suggests that little health adaptation is happening in practice, including for vulnerable groups14,44-47. Scrutiny of submitted 'national communications' required under the UN Convention48 also suggests that adaptation, particularly for health, is only emerging in many countries and certainly not occurring to the extent and level of sophistication that the 2011 IPCC report urges19.
One way of exploring the challenge of supporting adaptation to climate change in rural communities is to examine the nature of scholarly evidence available to support that adaptation. Of course, policy and practices relevant to rural communities will not be shaped only by scholarly evidence. The knowledge diffusion literature suggests that research evidence is often used in non-linear and complex ways, if at all, by end users of that evidence49-51. Yet it could reasonably be argued that scholarly climate change and health research ought to help develop best practice, and this is how serving the needs of rural communities is defined in this article. If research alone cannot change practices, it can certainly provide a foundation from which 'best practices' can develop. From January 1995 to the end of July 2012 there were at least 19 164 papers published in the health sciences and social sciences on climate change that could potentially offer an evidence base for adaptation to climate change. The extent to which the content of this body of literature serves best practice health adaptation in rural communities has not yet been systematically examined.
Aim
The aim of the study was to examine indicative evidence about how consistent is the content of scholarly literature - that could potentially offer an evidence base for health adaptation to climate change - with what is known about best practice for meeting the adaptation needs of rural communities. In so doing, the study aimed to offer a basis for rural community stakeholders to better participate in the development of climate change and health research, by way of contributing to better understandings about what research has been done and is needed.
Research questions
The two research questions were: 'What kinds of content define climate change research in disciplines that could potentially contribute to adaptation for health? and 'How is content about rural and Aboriginal communities and best practice in adaptation related to this content?'
Sample
In this study, abstracts were treated as indicative evidence of the content of journal papers.
The study sample comprised all abstracts for research and review papers in the database SCOPUS for the health sciences and social sciences, from 1 January 1995 to the 31 July 2012, obtained using the search term 'climate change' in the title, abstract, or keywords. This provided a total of 19 164 abstracts which were included in the study. At three abstracts per page, this equates approximately to 6388 pages of language data or the equivalent of 21 books each of 300 pages.
The social sciences were included to enable consideration of wider climate change adaptation content for rural communities and also to act as a comparator in consideration of how well the health sciences is serving adaptation best practice, because the natural sciences or 'hard' climate science generally considers 'hard' science concepts, not community-based concepts known to be important to adaptation.
Abstracts were divided by the following time periods to allow consideration of changes over time: 1995-2004; 2005-2006; 2007-2008; 2009-2010; 2011-2012. The year 1995 was chosen as the start date of the study because it marks the year following the historic UN Convention on Climate Change22, and far fewer scholarly publications can be observed before this date.
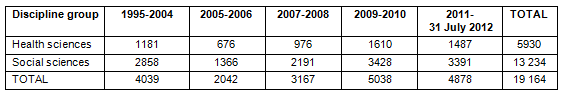
The break-down of numbers of abstracts in the health sciences versus the social sciences, according to each time period, is given (Table 1). The categories 'health sciences' and 'social sciences' in SCOPUS are not entirely mutually exclusive; however, they are sufficiently exclusive to make comparisons meaningful using the chosen method. Most sub-disciplines listed under the health versus social sciences are different. However, there are exceptions; for example, for the 1995-2004 period, 'health sciences' includes a category of papers called 'agricultural and biological sciences' (91 papers) but there are 247 'agricultural and biological sciences' papers listed under the 'social sciences' disciplines for the same period.
Table 1: Numbers of abstracts (reviews and research papers with 'climate change'
in article title, abstract or keywords), in the health sciences
versus the social sciences, according to time period
Analytic procedure
The analysis involved the use of a 'computational linguistics' approach with quantification of the content of the abstracts using Leximancer software v4.0 (www.leximancer.com). The software was employed to map the relative frequency and co-occurrence of concepts about rural communities with common concepts in the abstracts.
The software used is Bayesian-based, and its technical features are given in a detailed validation study52. Leximancer 'learns' from language in the dataset in an iterative fashion and maps the dataset as a network of concepts. It has been applied in a number of qualitative health contexts53-60.
The main output of Leximancer is a concept map that offers a spatial representation of the relative frequency as well as the contextual proximity (overall co-occurrence) of both found and user-selected concepts. The concepts are 'heat mapped' so they appear as coloured spheres (from 'red' or most frequent concepts to 'blue' or least frequent concepts).
For the concept map in this study, concepts about rural and Aboriginal communities and their urban comparator concepts, as well as concepts to do with best practice in the adaptation literature, were manually selected by the researcher. All other concepts were found by the software as common concepts. The nine manually selected concepts were 'rural', 'regional', 'Aboriginal', 'poverty', 'socio-economic', 'economic' (a comparator concept for 'socio economic'),'urban', 'city', 'town'.
The concept map was therefore designed to simultaneously map the relationships between the rural and Aboriginal concepts, their urban comparators, concepts to do with best practice in adaptation, as well as common concepts in the abstracts.
A total of 52 concepts were mapped. Each concept includes like words merged by the software or by the researcher manually (for example, 'Aboriginal' with 'Indigenous'). Blocks of text (usually about a paragraph in length) are the unit of analysis in Leximancer (ie one or more concepts will occur in a single text block). The text blocks grouped by the software under a single concept such as 'rural', will often but not always contain the word 'rural' because the software begins with its own thesaurus and also learns iteratively from the language dataset under consideration. Thus, a text block classified under 'rural' concept might include the word 'farmers' but not the word 'rural' itself.
Common concepts were not mapped where they did not add anything to understanding of the content of the climate change literature. For example, the common words 'author' and 'keyword' were not used as mapping concepts, nor was the word 'abstract' as these are recurring structural linguistic features of abstracts. Names of countries as well as other names were not mapped as concepts but, like the structural linguistic features of the abstracts, they were certainly included in the analysis. For example, rural content about Nigeria was subsumed under the 'rural' concept, and keywords were subsumed under other concepts. This helped ensure that the data output focussed on conceptual content. The possibility of using the word 'remote' as a mapping concept was considered and discarded. 'Remote' is not a viable mapping word because it has multiple meanings in this vast body of literature ('remote sensing technology') and is, in any case, differently defined even in the rural and remote health literature itself61.
Leximancer also has an extensive inbuilt thesaurus of positive and negative sentiment words. A second subsidiary analysis was conducted of sentiment words associated with a select number of nine contrasting concepts: 'health', 'Aboriginal', 'rural', 'urban', 'city', 'town', 'poverty', 'socio-economic', 'economic'. This analysis aimed to find out whether there was a difference between such concepts in the extent to which they were associated with negative or positive sentiment words. It therefore involved finding out and mapping, in a separate quadrant figure, the presence and relative frequency of co-occurrence (with sentiment words) of the subset of nine concepts. A more negative language associated with the 'rural' concept might possibly indicate the presence of a deficit view of rural communities inconsistent with global best practice17,18, which positively emphasises the knowledge and experience these communities bring to climate change adaptation.
The discussion of findings was also informed by manual scanning of all 101 299 distinct text blocks containing all 309 862 instances of the final set of 52 concepts found by Leximancer. This manual scanning was conducted to check whether the building blocks of the Leximancer mapping output (the text blocks) produced findings broadly consistent with what could be observed in manual checks. The layered structure of Leximancer procedures means that the researcher can work iteratively with its analytical procedures, checking and refining the choice of concepts as well as manually checking groupings of all text blocks (in context in the original abstracts), supporting quantitative output. This arguably increases the integrity of the output: the language data are not analysed in an automated 'black box'. Accordingly, while data visualisation of large amounts of language data occurs in the form of the concept map and quadrant, the researcher has access to supporting text blocks, in context, for all software output, for manual checking.
The concept map
A map is provided (Fig1) of all 52 concepts from the 19 164 abstracts included in this study (ie the 309 862 instances of these concepts in 101 299 distinct text blocks). The concept map is a spatial representation of the frequency and overall co-occurrence of the 52 concepts. It could be conceptualised as an holistic picture of all 52 concepts in this large body of abstracts. Concepts showing in the red spheres are relatively more frequent than concepts showing in the bluer spheres (Fig1). The grey lines suggest typical 'story lines' or pathways made across multiple concepts (they are not simply about relationships between two concepts). The grey lines connecting concepts can be understood as linked chains of concepts. They are designed to capture the main roads or 'highways' of the most direct connection, although they are also influenced by proximity as a weighting in the calculation of the map. This means that concepts that have more direct co-occurrences and are located near each other on the map are most likely to have a grey line connecting them. In contrast, concepts with no co-occurrence or located a long way apart are unlikely to be linked by a grey line. Accordingly, proximity on the map can be understood as being about semantic similarity, for example 'surface' and 'ice'. The grey branching lines are about the typical stories, such as carbon→greenhouse gasses (GHG)→energy. The size of the grey dots shows the extent to which they co-occur with all other concepts.
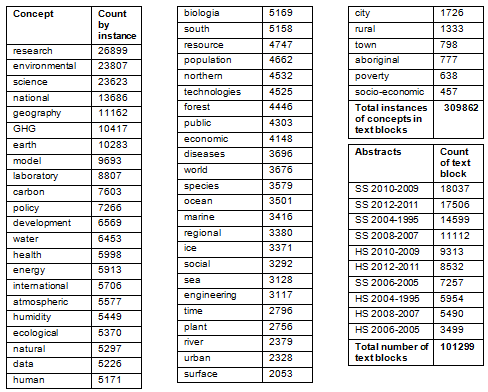
Simple counts of the 52 concepts are provided (in Table 2; their instances in text blocks, as well as total counts of text blocks split by period and whether health services or social sciences abstracts).
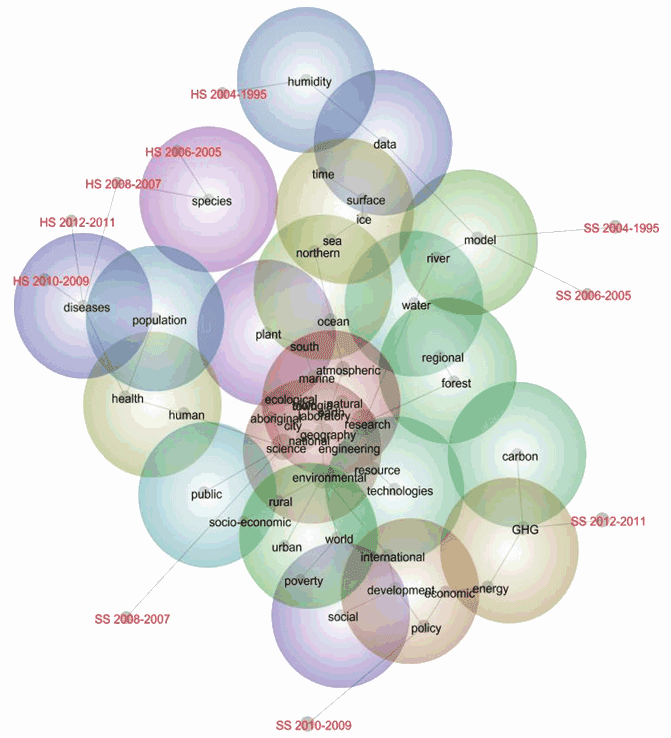 Figure 1: Concept map of social sciences and health science literature on climate change.
Figure 1: Concept map of social sciences and health science literature on climate change.
Note: 'HS 2004-1995' = abstracts for the health sciences
for that period, for example. GHG, greenhouse gas emissions.
Table 2: List of all concepts and counts of their instances in text blocks,
as well as total counts of text blocks split according to period and
whether health services or social sciences abstracts
Accordingly, as Figure 1 suggests, when all abstracts from the health sciences and social sciences are considered (the total set of disciplines that might offer adaptation knowledge) the dominant focus is on GHG emissions and energy issues and this is most true of the social sciences in the period 2012-2011. Economic (but not socio-economic) policy storylines are also dominant in the recent (2010-2009) social sciences literature. Where 'social' concepts occur, they do so relatively infrequently and tend to be connected to storylines about 'development' and 'policy' concepts. 'Rural' concepts (in the green sphere) are relatively less frequent, typically associated with social science research, and tend to be connected to storylines about 'socio economic' and 'environmental' concepts.
When this large body of literature is considered as a whole, rural concepts tend not to be associated with health. The health sciences abstracts, initially more associated with 'humidity' concept storylines, are now much more associated with 'disease' storylines linked to 'species' ,'population' and ultimately 'science' concepts (an example might be tick-borne encephalitis). Considering paired concepts only (the likelihood of two concepts being found in the same text block, another kind of analysis included below), there is a 38% overall likelihood of co-occurrence of the two concepts of 'disease' and 'health' alone.
Unlike the social sciences from 2004-2012, the health sciences abstracts from 2004-2012 do not appear to be well connected to storylines about community such as 'rural' and 'socio economic' and 'Aboriginal' concepts. It is not simply that the health sciences abstracts appear not well connected to rural or Aboriginal community studies. The health sciences abstracts are generally not well connected to other local human systems concepts such as 'city' and 'town'.
The difference between the social sciences and the health sciences, therefore, is not simply that the social sciences focuses more on environmental concepts such as 'river' and mitigation concepts such as 'GHG' or 'energy'. The social sciences appear to focus more on the local and particular issues of community in climate change than do the health sciences.
Accordingly, it is not clear that rural communities as such are being systematically marginalised in this literature: the concepts of 'Aboriginal', 'rural', 'urban', 'city' and 'town' have a 3%, 5%,9%, 6% and 3% likelihood of being found in any one of the 101 299 distinct text blocks in this study containing one of more of the 52 concepts. The concept of 'regional' is more frequent with a 13% likelihood of being found in these text blocks. Arguably, concepts to do with the local and particular needs of communities are generally under-represented.
Relationships between the concept 'rural' and other concepts can also be examined not from the holistic perspective of overall co-occurrences or typical storylines across multiple concepts given above, but by considering co-occurrences of pairs of concepts. When pairs of concepts are considered (the simple likelihood of one concept being found with a second concept) it can be seen that the concept 'rural' occurs most often with the term 'poverty'. It occurs least frequently with the concepts one might associate with mitigation and environmental science; that is, it has a 1% likelihood of co-occurring with 'GHG' and 'carbon' concepts, and a less than 1 in a 100 (0%) chance of co-occurring with concepts such as 'sea' and 'ice'.
Closer inspection of the periods of time suggests that the presence of the 'rural' concept may be improving over time, in both the health sciences and the social sciences. That is, the concept of 'rural' has a 2% likelihood of being found in the abstracts published in the health sciences and the social sciences in 2012-2011 and in abstracts found in the social sciences from 2010-2009. In contrast, the 'rural' concept has a 1% likelihood of being found in abstracts batched by all other earlier years and with the health sciences in 2010-2009.
Similarly, the concept of 'Aboriginal' is found less frequently in older periods in both the health sciences and social sciences, and more frequently in more recent periods, though the percentage changes involved are very small (from 0% to 1%). The 'Aboriginal' concept is found less than 1 in a 100 times in the 1995-2004 periods for both the health sciences and the social sciences, and 1% of the time in all other periods, except for the social sciences in 2006-2005 where it is also found 0% of the time (which in a dataset of 101 299 text blocks does not mean it never occurs).
The sentiment quadrant
Another perspective entirely is provided in Figure 2 by looking at how the rural and Aboriginal concepts are used in the language of sentiment (negative or positive). The relative frequencies or conditional probability of each of nine concepts ('health', 'Aboriginal', 'rural', 'urban', 'city', 'town', 'poverty', 'socio-economic', 'economic') being found with positive versus negative words is represented (Fig2) for each period, comparing the health sciences with the social sciences. The quadrant offers one way of exploring whether the 'rural', 'Aboriginal', 'town', and 'socio economic' concepts are referred to more negatively or positively than the 'urban', 'city', or 'economic' concepts. The 1-20% scale on the X-axis refers to the frequency with which a concept is mentioned in any instance of negative or positive terms in text blocks. The 0-32% scale on the Y-axis refers to the extent of positive rather than negative sentiment associations in each selected concept or the proportion of positive to negative associations in individual selected concepts. That is, concepts in quadrant 1 (the bottom left corner of the quadrant) have a weak frequency of use with sentiment associations generally, and are more likely to co-occur with negative words. Concepts shown in quadrant 4 (top right corner of quadrant) have a higher frequency and are more likely to co-occur with positive words.
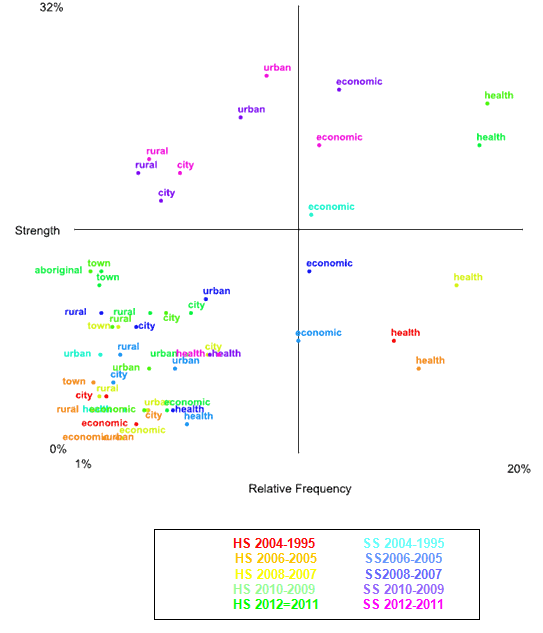 Figure 2: Quadrant map of likelihood of references to selected concepts
Figure 2: Quadrant map of likelihood of references to selected concepts
in association with positive or negative sentiment words.
'Health' is more frequently found in both negative and positive sentiment terms, compared with other concepts (Fig2). It is the most common positive concept of all the nine concepts because of how it is referred to from 2012 to 2009 in the health sciences. The second most common concept in the language of sentiment (both negative and positive) is the 'economic' concept. It is the second most common positive concept because of how it is referred to from 2012 to 2009 in the social sciences. In recent years (2012-2009) the 'rural' concept tends to be more positively represented but it is still behind the 'urban' concept in terms of how positively it is represented.
In the most recent period in the health sciences, the 'Aboriginal' concept is still very infrequent in the language of sentiment (positive or negative; Fig2). However, where it does occur it has included a sufficient number of positive associations to appear more positively than many other low-frequency concepts (in sentiment) in the bottom left-hand corner of the quadrant. For example, in health sciences abstracts in 2012-2011, the concept 'Aboriginal' was much lower in frequency in the language of sentiment than the concept 'economic' in, for instance, the social sciences abstracts of 2010-2009. Yet the two concepts in those two bodies of abstracts (HS 2012-2011 vs SS 2010-2009) are level in terms of positive associations.
Summary of findings
In summary, 'rural' and 'Aboriginal' concepts tend to be relatively infrequent (3% and 5% overall likelihood of occurrence, respectively) and are more associated with socio-economic concepts in the social sciences than the health sciences. Multiple concepts in the health sciences literature are typically connected with 'disease' and ultimately 'science' storylines, with a 38% likelihood of paired co-occurrence of 'health' and 'disease' concepts alone. The social sciences appear more focused on the local and particular issues of community in climate change than the health sciences. 'Rural' and 'Aboriginal' concepts have increased by 1% across both discipline areas, since 2011 for the 'rural' concept and since 2004 for the 'Aboriginal' concept. 'Health' concepts in the health sciences and 'economic' concepts in the social sciences, as well as 'urban' concepts, are referred to more positively than either the 'rural' or 'Aboriginal' concepts.
Discussion
This study explored how well climate and health research is serving rural communities using a particular definition of best practice - community-based research with a focus on local knowledge and localised service development. While evidence about adaptation best practice is still emerging, the study has been based on the premise that this definition offers some foundation for exploring whether climate and health research is delivering this best practice.
The study has suggested that rural communities and adaptation best practice are little represented in this literature but has raised complex issues that suggest why this might be so. It is not clear if the under-representation of local community concepts generally in this literature is a function of content or method. Content could be understood as driven by system values about what should be researched. Method could be understood as shaped by dominant ideas of research quality, for example, research guidelines such as those for randomised controlled trials or Cochrane reviews that value globally relevant biomedical research questions. More likely, both system values and institutionalised methodologies have shaped the research available for rural health adaptation. Institutionalised research barriers may also include the complexity of ethics procedures for community engagement projects, including with vulnerable groups, which may also be shaping what adaptation research is being produced. Climate change offers an opportunity to explore whether and how these values and methodologies are compatible with the evidence needed to meet new public health threats.
A strength (and limitation) of this study is that it has examined content rather than quality. A study of content such as this includes all scholarly work that could potentially be useful in some form or another. This may be important in light of the fact that the knowledge translation literature does not provide strong support for the idea that higher quality research (in academic or scholarly definitions) is unproblematically associated with greater evidence take-up. For example, in terms of the health policy-making that shapes local community health systems, a wide range of information, not just research evidence, has been found to be used by decision-makers, and to be shaped by very specific contextual decision-making needs62-65. Alignment with content needs may, therefore, be more important than academic hierarchies of quality in evidence take-up.
However, care must be taken in interpreting the results of this study too negatively for rural and Aboriginal communities. The fact that a relatively small amount of scholarly research is available is not conclusive evidence that not enough research is available. On the other hand, the best practice definition of 'adaptation tailored to localised needs' used in this study carries the implication of needed research volume - there are many distinctive communities all with their own adaptation needs. Yet it may be that applied research by, for example, local government, health agencies and emergency services, is shouldering the weight of best practice adaptation research.
Further, the study did not explore whether and how a disease focus in health might also have benefits for rural communities - such benefits could be demonstrated for much disease-focussed research. It did, however, suggest that a disease focus dominates health sciences literature and that this is typically unconnected to a consideration of the wider socio-economic and systemic determinants of health. In assessing the significance of this finding, it is worth considering the work of many colleagues who have demonstrated that the socio-economic determinants of health are the primary shapers of health66-68, as well as the accumulating evidence in the scholarly literature that socio-economic disadvantage magnifies climate effects1.
The lack of a well developed body of literature on adaptation does not only have a negative opportunity cost (ie lost opportunities to develop health strategies from negative health outcomes of climate change), it also has a positive opportunity cost (ie lost opportunities to develop health strategies engaging with positive health outcomes of climate change). The disease focus of climate and health literature demonstrated in this study may suggest a stronger focus on negative outcomes of climate change than could be developed through engagement with the adaptive potential and capacities of 'real world' local communities that experience both the negative and positive health effects of climate change.
On balance, this study adds some support to the view that a key priority is bringing the learnings of applied community-based researchers, from those in rural health to those in the social sciences, to the science of climate research. This is unlikely to be simply about increasing the amount of funding for climate and health research - a miniscule amount of health research budgets in developed countries such as the USA and Australia69,70. It may be more about valuing kinds of research that are presently poorly valued but more pragmatically useful in the future if research funding is to be consistent with social justice rhetoric in a climate-changing world. For example, the study reflects the fact that Australia is typical of other developed nations such as the USA in spending only 4% of National Health and Medical Research Council funding on health services research70.
While the study is limited to literature about climate change, it reflects the development of interlocking emerging disciplines in public and environmental health. That is, it reflects the fact that understandings of the social determinants of health has a long public policy history in, for example, Britain, but is relatively recent as a field of scholarly enquiry in the public health literature. The study also reflects the emerging nature of an 'environmental determinants of health' approach. It supports a call for applied community-based approaches that draw on these emerging disciplines to help develop a stronger evidence base for engaging with the ways in which human systems mediate the health effects of climate change.
Conclusion
This study highlights the ways in which evidence available for best practice is shaped by the ways research is conceptualised. Future community-based research in climate change should also be informed by critical examination of the ways in which applied research also contains implicit assumptions that shape what adaptive strategies may be developed. Approaches to gathering evidence for adaptation shaped by 'vulnerability' or 'resilience' or 'opportunity' conceptualisations of adaptation could deliver quite different kinds of evidence in the same communities. This study suggests the importance of better development and use of evidence-based theory about adaptation best practice in climate and health literature generally.
Ultimately, this study suggests there is a need to question the perception that climate change research involves 'hard' climate science or sophisticated quantitative scenarios modelling removed from the traditional applied community-based research contexts of rural health. Changing this perception, including among rural stakeholders and researchers who have arguably been slow to participate in programs of climate change research, is important for rural health. It may ultimately be about building confidence that community-based research does have value in the sciences needed to make a difference in a climate-changing world.
References
1. Costello A, Allen A, Ball S, Bell S, Bellamy R et al. Managing the health effects of climate change. Lancet 2009; 373: 1693-1733.
2. McMichael A, Woodruff R, Hales S. Climate change and human health: present and future risks. Lancet 2006; 367(9513): 859-869.
3. Haines A, Kovats RS, Campbell-Lendrum D, Corvalan C. Climate change and human health: impacts, vulnerability, and mitigation. Lancet 2006; 367(9528): 2101-219.
4. Hanlon P, Carlisle S. Thesis: Do we face a third revolution in human history? If so, how will public health respond? Journal of Public Health (Oxford) 2008; 30(4): 355-361.
5. Patt AG, Tadross M, Nussbaumer P, Asante K, Metzger M et al. Estimating least-developed countries' vulnerability to climate-related extreme events over the next 50 years. Procedings of the National Academy of Science USA 2010; 107(4): 1333-1337.
6. Haney T, Elliott J, Fussell E. Families and hurricane response:evacuation, separation, and the emotional toll of hurricane Katrina. In: D Brunsma, D Overfelt, J Picou (Eds); The sociology of Katrina: perspectives on a modern catastrophe. Lanham, MA: Rowman & Littlefield, 2007; 8.
7. Rudowitz R, Rowland D, Shartzer A. Health care In New Orleans: Before and after Hurricane Katrina. Health Affairs 2006; 25(5): w393-w406.
8. McCallum E, Heming J. Hurricane Katrina: an environmental perspective. Philosophical Transactions. Series A, Mathematical, Physical, and Engineering Sciences 2006; 364(1845): 2099-2115.
9. Holmes C. Queensland Floods Commission of Enquiry: Final Report. Brisbane, QLD: Queensland Government, 2012. Available: http://www.floodcommission.qld.gov.au/__data/assets/pdf_file/0007/11698/QFCI-Final-Report-March-2012.pdf (Accessed 5 June 2012).
10. Teague B, McLeod R, Pascoe S. The 2009 Victorian Bushfires Royal Commission Final Report. Melbourne, VIC: Parliament of Victoria, 2009. Available: http://www.royalcommission.vic.gov.au/Commission-Reports/Final-Report (Accessed 5 June 2012).
11. Patz JA, Kovats RS. Hotspots in climate change and human health. BMJ 2002; 325(7372): 1094-1098.
12. IPCC. IPCC Third Assessment Report - Climate Change 2001: Working Group II: Impacts, Adaptation and Vulnerability. Geneva: United Nations Environment Programme (UNEP) and the UN's World Meteorological Organization (WMO), 2001. Available: http://www.grida.no/publications/other/ipcc_tar/?src=/climate/ipcc_tar/ (Accessed 14 March 2012).
13. Adger W, Agrawala S, Mirza M, Conde C, O'Brien K et al. Assessment of adaptation practices, options, constraints and capacity. In: M Parry, O Canziani, J Palutikof, P van der Linden, C Hanson (Eds). Fourth Assessment Report of the Intergovernmental Panel on Climate Change (Contribution of Working Group II). Cambridge: Cambridge University Press, 2007; 717-743.
14. Massey E, Bergsma E. Assessing adaptation in 29 European countries. Amsterdam: VM Insititute of Environmental Studies, Vrije UniversiteitI, 2008.
15. Bell E. Readying health services for climate change: A policy framework for regional development. American Journal of Public Health 2011; 101(5): 804-813.
16. West C, Gawith M, Eds. Measuring Progress: Preparing for Climate Change through the UK Climate Impacts Programme (Technical Report). Oxford: UK Climate Impacts Programme (UKCIP), 2005.
17. COP. The Cancun agreements: outcome of the Ad Hoc Working group on Long-term Cooperative Action under the Convention. Bonn, Germany: Conference of the Parties, United Nations, 2011. Available: http://unfccc.int/adaptation/cancun_adaptation_framework/items/5852.php (Accessed 31 Jan 2012).
18. WHO. Climate change and health resolution WHA61.19; Agenda item 11.11 Sixty-first World Health Assembly Geneva: World Health Organisation, 2008.
19. IPCC (Eds). Summary for Policymakers. Cambridge: Cambridge University Press, 2011.
20. Ford J. Indigenous health and climate change. American Journal of Public Health 2012; 102(7): 1260-266.
21. Furgal C, Seguin J. Climate Change, Health, and Vulnerability in Canadian Northern Aboriginal Communities. Environ Health Perspectives 2006; 114(12): 1964-1970.
22. COP. United Nations Framework Convention on Climate Change. Bonn, Germany: Conference of the Parties, United Nations, 1994. Available: http://unfccc.int/key_documents/the_convention/items/2853.php (Accessed 31 Jan 2012)
23. EPA. Policy Statement on Climate-Change Adaptation. Washington, DC: US Environmental Protection Agency, 2011. Available: http://www.epa.gov/climatechange/effects/adaptation.html (Accessed 5 June 2012).
24. Climate Change and Health Working Group, Tackling the health effects of climate change: A plan to support the health response to the Climate Change Adaptation Action Plan for Wales Cardiff: Welsh Government; 2009. Available: http://wales.gov.uk/topics/health/protection/environmental/publications/climate/?lang=en (Accessed 31 January 2013).
25. Welsh Assembly Government, Climate change strategy for Wales. Cardiff: Welsh Assembly Government, 2010. Available : http://wales.gov.uk/topics/environmentcountryside/climatechange/tacklingchange/strategy/walesstrategy/?lang=en (Accessed 31 January 2013)..
26. Welsh Assembly Government, Climate change strategy for Wales: adaptation delivery plan. Cardiff: Welsh Assembly Government; 2010. Available from: http://wales.gov.uk/topics/environmentcountryside/climatechange/publications/strategy/?lang=en (Accessed 31 January 2013).
27. President of Russia. Climate doctrine of the Russian Federation. Moscow: Government of the Russian Federation, 2009. Available: http://archive.kremlin.ru/eng/text/docs/2009/12/223509.shtml (Accessed 15 February 2012).
28. Scottish Government. Scotland's climate change adaptation framework. Edinburgh: Scottish Government, 2009. Available: http://www.scotland.gov.uk/Topics/Environment/climatechange/scotlands-action/adaptation/AdaptationFramework (Accessed 5 June 2012).
29. Scottish Government. Scotland's Climate Change Adaptation Framework: Health and Wellbeing Sector Action Plan. Edinburgh: Scottish Government, 2010. Available: http://www.scotland.gov.uk/Resource/Doc/175776/0114918.pdf (Accessed 5 June 2012).
30. Finnish Ministry of Agriculture and Forestry. Finland's national strategy for adaptation to climate change. Vammala, 2005. Available: http://www.mmm.fi/attachments/ymparisto/5kghLfz0d/MMMjulkaisu2005_1a.pdf (Accessed 8 March 2012).
31. Department for Environment. Adapting to climate change in England: a framework for action. London, 2008. Available: http://archive.defra.gov.uk/environment/climate/documents/adapting-to-climate-change.pdf (Accessed 6 March 2012).
32. Department of Health. Departmental adaptation plan update. London, 2011. Available: http://archive.defra.gov.uk/environment/climate/documents/dept-adapt-plans/dap-dept-health-110519.pdf (Accessed 6 March 2012).
33. Department for Environment. Defra's climate change plan 2010. London, 2010. Available: http://archive.defra.gov.uk/environment/climate/documents/climate-change-plan-2010.pdf (Accessed 6 March 2012).
34. Department of Health. Climate change plan. London: Department of Health, 2010. Available: http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_114929 (Accessed 5 June 2012).
35. The Federal Government of Germany. German strategy for adaptation to climate change. Berlin, 2008. Available: http://www.bmu.de/english/climate/downloads/doc/42841.php (Accessed 8 March 2012).
36. Spanish Ministry for the Environment. The Spanish national climate change adaptation plan. Madrid, 2008. Available: http://www.magrama.es/es/cambio-climatico/temas/impactos-vulnerabilidad-y-adaptacion/pnacc_ing_tcm7-12473.pdf (Accessed 8 March 2012).
37. National Climate Change Adaptation Research Facility. National climate change adaptation research plan: human health and climate change [draft]. Canberra, ACT: Human Health Adaptation Network Circular, 2011.
38. Council of Australian Governments. National Climate Change Adaptation Framework. Canberra, ACT: Council of Australian Governments, 2007. Available: http://www.climatechange.gov.au/government/initiatives/national-climate-change-adaptation-framework.aspx (Accessed 5 June 2012).
39. Centers for Disease Control. CDC Policy on Climate Change and Public Health. New York: Centers for Disease Control, Department of Human Health Services, 2009. Available: http://www.cdc.gov/climateandhealth/policy.htm (Accessed 5 June 2012)
40. National Climate Commission. Belgian national climate change adaptation strategy. Brussels: National Climate Commission, 2010. Available: http://www.climatechange.be (Accessed 8 March 2012).
41. Danish Government. Danish strategy for adaptation to a changing climate. Copenhagen: The Danish Energy Agency, 2008. Available: http://www.kemin.dk/Documents/Klima-%20og%20Energipolitik/klimatilpasningsstrategi_UK_web.pdf (Accessed 8 March 2012).
42. Netherlands Ministry of Housing Spatial Planning and the Environment, Netherlands Ministry of Transport Public Works and Water Management, Netherlands Ministry of Agriculture Nature and Food Quality, Netherlands Ministry of Economic Affairs, Netherlands Association of Provincial Authorities et al. National programme on climate adaptation and spatial planning: national adaptation strategy - the inter-administrative policy paper. Amsterdam, 2008. Available: http://www.maakruimtevoorklimaat.nl/fileadmin/user_upload/Documenten/PDF/Engelstalige_documenten/inter-admin_policy_paper_ENG.pdf (Accessed 8 March 2012)
43. Netherlands Ministry of Housing Spatial Planning and the Environment, Netherlands Ministry of Transport Public Works and Water Management, Netherlands Ministry of Agriculture Nature and Food Quality, Netherlands Ministry of Economic Affairs, Netherlands Association of provincial Authorities et al. National programme on climate adaptation and spatial planning: national adaptation strategy - policy memorandum. Amsterdam, 2008. Available: http://www.maakruimtevoorklimaat.nl/fileadmin/user_upload/Documenten/PDF/Engelstalige_documenten/policy_memorandum_ENG.pdf (Accessed 8 March 2012).
44. Balbus J, Ebi K, Finzer L, Malina C, Chadwick A et al. Are we ready?: Preparing for the public health challenges of climate change. New York: Environmental Defence Fund, 2008. Available: http://www.edf.org/health/reports/are-we-ready (Accessed 5 June 2012).
45. EEA. Adapting to climate change - SOER 2010 thematic assessment Copenhagen, Denmark: European Environment Agency, 2010. Available: http://www.eea.europa.eu/soer/europe/adapting-to-climate-change (Accessed 5 June 2012).
46. Swart R, Biesbroek R, Binnerup S, Carter T, Cowan C et al. Europe Adapts to Climate Change Comparing National Adaptation Strategies. Helsinki, Finland, 2009. Available: http://www.peer.eu/fileadmin/user_upload/publications/PEER_Report1.pdf (Accessed 5 June 2012).
47. Ford J, Berrang-Ford L, Paterson J. A systematic review of observed climate change adaptation in developed nations. Climatic Change 2011; 106: 327-336.
48. UN. United Nations Framework Convention on Climate Change. Submitted National Communications. Geneva: United Nations, 2012. Available: http://unfccc.int/national_reports/annex_i_natcom/submitted_natcom/items/4903.php (Accessed 31 January 2012).
49. Rogers E. Diffusion of Innovations. New York: The Free Press, 1995.
50. Dearing JW. Evolution of diffusion and dissemination theory. Journal of Public Health Management and Practice 2008; 14(2): 99-108.
51. Nutley S, Walter I, Davies H. Using Evidence: How Research Can Inform Public Services Bristol: The Policy Press, 2007.
52. Smith AE, Humphreys MS. Evaluation of unsupervised semantic mapping of natural language with Leximancer concept mapping. Behavior Research Methods 2006; 38(2): 262-279.
53. Baker SC, Gallois C, Driedger SM, Santesso N. Communication accommodation and managing musculoskeletal disorders: doctors' and patients' perspectives. Health Communication 2011; 26(4): 379-388.
54. Cretchley J, Gallois C, Chenery H, Smith A. Conversations between carers and people with schizophrenia: a qualitative analysis using Leximancer. Qualitative Health Research 2010; 20(12): 1611-1628.
55. Hepworth N, Paxton SJ. Pathways to help-seeking in bulimia nervosa and binge eating problems: a concept mapping approach. The International Journal of Eating Disorders 2007; 40(6): 493-504.
56. Hewett DG, Watson BM, Gallois C, Ward M, Leggett BA. Intergroup communication between hospital doctors: implications for quality of patient care. Social Science & Medicine 2009; 69(12): 1732-1740.
57. Kuyini AB, Alhassan A-RK, Mahama FK. The Ghana community-based rehabilitation program for people with disabilities: what happened at the end of donor support? Journal of Social Work in Disability & Rehabilitation 2011; 10(4): 247-267.
58. Kyle GJ, Nissen L, Tett S. Perception of prescription medicine sample packs among Australian professional, government, industry, and consumer organizations, based on automated textual analysis of one-on-one interviews. Clinical therapeutics 2008; 30(12): 2461-2473.
59. Pakenham KI, Tilling J, Cretchley J. Parenting difficulties and resources: the perspectives of parents with multiple sclerosis and their partners. Rehabilitation Psychology 2012; 57(1): 52-60.
60. Travaglia JF, Westbrook MT, Braithwaite J. Implementation of a patient safety incident management system as viewed by doctors, nurses and allied health professionals. Health 2009; 13(3): 277-296.
61. Wakerman J. Defining remote health. Austra, lian Journal of Rural Health 2004; 12(5): 210-214.
62. Dobbins M, Jack S, Thomas H, Kothari A. Public health decision-makers' informational needs and preferences for receiving research evidence. Worldviews Evidenced Based Nursing 2007; 4(3): 156-163.
63. Mays N, Pope C, Popay J. Systematically reviewing qualitative and quantitative evidence to inform management and policy-making in the health field. Journal of Health Services Research and Policy 2005; 10(Suppl1): 6-20.
64. Sorian R, Baugh T. The power of information: closing the gap between research and policy. Health Affairs: The Policy Journal of the Health Sphere 2002; 21(2): 264-273.
65. Dobbins M, Rosenbaum P, Plews N, Law M, Fysh A. Information Transfer: What do decision-makers want and need from researchers? Implementation Science 2007; 2(1): 20.
66. Commission on the Social Determinants of Health. Final report: closing the gap in a generation: health equity through action on the social determinants of health. Geneva: World Health Organisation, 2008.
67. Rainham D. Do differences in health make a difference? A review for health policymakers. Health Policy 2007; 84(2-3): 123-132.
68. Marmot M, Friel F, Bell R, Houweling T, Taylor S. Closing the Gap in a Generation: Health Equity through Action on the Social Determinants of Health Geneva: World Health Organisation, 2008. Available: http://www.who.int/social_determinants/thecommission/finalreport/en/index.html , (Acc, esse, , , , d 6, , February 2013).<, /p>
69. Ebi K, Balbus J, Kinney P, Lipp E, Mills D et al. U.S. Funding Is Insufficient to Address the Human Health Impacts of and Public Health Responses to Climate Variability and Change. Environmental Health Perspectives 2009; 117(6): 857-862.
70. NHMRC. NHMRC research funding datasets 1990-2010. Canberra, ACT: NHMRC, 2012. Available: http://www.nhmrc.gov.au/grants/research-funding-statistics-and-data/funding-datasets (Accessed 5 June 2012).
