full article:
Dental decay (caries) is the most prevalent health condition in Australia1. Caries can cause oral pain, infection and tooth loss, and pain from dental caries may make everyday activities such as eating and speaking difficult2. In addition, oral diseases, particularly periodontitis, affect not only the mouth, but have also been associated with cardiovascular diseases3, diabetes4, stroke5 and pre-term low-birthweight6.
People living in rural and regional Australian communities have more caries, more severe caries and more untreated caries than those in urban areas7-9. The unique environmental conditions and population groups in these communities may contribute to the higher disease rate. In particular, some towns lack community water fluoridation, and some have a high proportion of Aboriginal people who have significantly worse oral health than their non-Aboriginal counterparts9-11. (The communities and participants in this study comprise both Torres Strait Islander and Aboriginal people; however, the term Aboriginal has been used throughout this article to refer to Aboriginal and Torres Strait Islander people, in recognition that Aboriginal peoples are the original inhabitants of [study setting] New South Wales [NSW]). Because of these and other unique circumstances, mainstream research on caries risk factors may not apply in these settings.
Ninety-four per cent of the population of NSW now drinks fluoridated water. The remaining unfluoridated communities tend to be small and regional or rural. Fluoridation of large towns is a very cost-effective prevention measure, but as the population reduces, so does the cost-effectiveness of fluoridation. It has been suggested that approximately 1000 people may be the cut-off for cost-effectiveness of community water fluoridation, although this may be lower for towns with high numbers of disadvantaged people12.
Aboriginal people are recognised as a high risk group for oral disease. Despite this, scant data exist on the oral health of Aboriginal children in NSW, and few studies have successfully investigated caries risk factors in communities with a high proportion of Aboriginal people.
This study aimed to gather contemporary oral health data from small rural or regional Australian communities, and investigate caries risk factors in these communities.
Setting and participants
Lack of water fluoridation and a large Aboriginal population are key caries risk factors, which are likely to be different in rural and remote communities than in the wider Australian population. Therefore, community selection criteria aimed to recruit adequate numbers of Aboriginal people and unfluoridated communities for meaningful comparisons. Further, selecting communities in similar geographic circumstances was regarded as beneficial for the purposes of comparison. Therefore, all three recognised Aboriginal communities located on the coast south of state capital Sydney were identified. The communities were Wreck Bay, La Perouse and Wallaga Lake. The locations of the three communities are shown (Fig1).
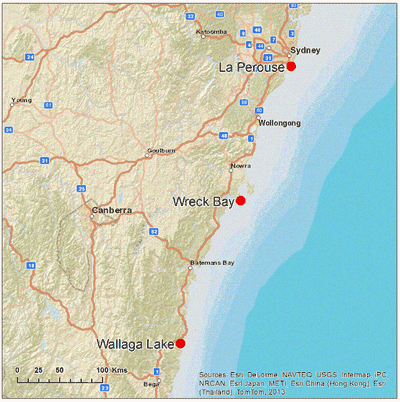
Figure 1: Location of the three study sites in the New South Wales
South Coast Child Dental Health Survey (map used with permission
ArcGIS Resources http://resources.arcgis.com).
While La Perouse is not a rural or regional community, it was included in the study because a fluoridated area with a high proportion of Aboriginal people was needed for comparison with the other two unfluoridated communities, and La Perouse was deemed sufficiently isolated to be comparable for the purposes of the study.
A complete list of schools, preschools and day-care centres near the communities was prepared. The following inclusion criteria were applied to select schools and preschools for the study:
- situated within a 30 km radius of the Aboriginal community of interest or attended by the majority of children in that community
- at least 20% Aboriginal enrolment
- enrols children aged 3-12 years.
On the basis of these criteria, 11 schools and preschools were selected for the study, and all agreed to participate. While it is not possible to know the exact child population within 30 km of the Aboriginal communities of interest, a total of four schools did not meet the selection criteria for level of Aboriginal enrolment and were thus not surveyed. Six of the 11 surveyed schools were in unfluoridated areas and five were in the fluoridated area. All 602 children aged 3-12 years who attended these schools were eligible to participate in the study, and each received informed consent material and a questionnaire to be completed by a parent or carer. Participation in the study required informed parental consent.
Method
Enrolled children underwent a clinical dental examination, and parents or carers filled in a questionnaire. The clinical examinations were conducted in October and November 2011, according to a national protocol developed at the Australian Research Centre for Population Oral Health7. Under this protocol, the caries call is taken from enamel cavitation (ie International Caries Detection and Assessment System [ICDAS] classification D2-D3). The system was adopted from the US National Institute of Dental and Craniofacial Research (NIDCR) examination protocol and World Health Organisation 1997 protocol. Three survey teams, each consisting of a dental therapist (examiner) and a dental assistant (recorder), examined children in schoolrooms under standardised conditions using a sterile mirror and dental probe. Dental plaque, decay, trauma and fluorosis were recorded.
Parents were asked to complete a nine-item questionnaire on their child's residential history, use of fluoride supplements, potable water source and tooth-brushing, and their own highest level of education and concession card status (an indicator of socioeconomic status). The questionnaire was deliberately kept short to maximise participation. All questions were validated and standardised by the Australian Research Centre for Population Oral Health or were consistent with Australian Census questions used in the NSW Health Survey Program13.
Examination teams attended a two-day training and calibration workshop run by the Australian Research Centre for Population Oral Health before commencing data collection. At the workshop, the examiners' performance was validated and standardised to that of a 'gold standard' examiner. During the study, diagnostic reliability and validity were monitored by duplicate examinations by the same examiner of 10% of randomly chosen children and a further 10% by the gold standard examiner.
Data preparation and analysis
The results of the examination were recorded by direct computer data entry. Questionnaires were scanned and verified with Cardiff TeleForm (http://www.cardiff-teleform.com/). Data were then exported to Microsoft Excel for cleaning and analysed with SAS v9.2 (www.sas.com).
Examiner validity was measured by comparing all three examiners with the gold standard. The statistical tests used were intra-class correlation and kappa score for agreement. Examiner reliability was measured by comparing each examiner to herself. One examiner conducted too few repeat examinations to allow analysis of her reliability. The remaining data were analysed for reliability by intra-class correlation.
Aboriginal status was ascertained by questionnaire. Identification was maximised by working with an Aboriginal healthcare worker and in partnership with the community.
Children were assigned to fluoridated or unfluoridated groups according to the water supply of their school. This was done to maximise data quality, because the data about the schools was accurate and recorded for all children. This method also allowed for complex living arrangements, because some children lived between two separate homes.
For the descriptive analysis, groups were compared using the χ² test.
Caries experience was determined using two measures: the deciduous and permanent decayed, missing and filled teeth (dmft/DMFT) score, and the proportion of children who were caries-free. The dmft/DMFT was calculated for each child by adding all teeth with one or more carious lesions (either currently carious or filled, implying previous caries).
The dmft/DMFT were analysed in 2 year-age strata to control for the strong effect of age on caries experience. The 5-6 and 11-12 year age groups are reported as index groups, in line with national and state-wide research11,12. The dmft/DMFT results for all children were included in the modelling.
Logistic regression was used to determine independent predictors for caries (Yes/No) as the dependent variable. Potential independent predictors of caries were determined a priori, and included water fluoridation, Aboriginal status, age, gender, concession card status (Y/N), parent education level (completed school/did not complete school) and tooth-brushing frequency (≤ 1/day, ≥ 2/day). Initially logistic regression models tested for associations between individual predictors and caries experience. All predictors with a p-value <0.25 were then entered into a single logistic regression model and the backwards selection method was used to derive the final model. Effect modification was examined in two sets of sensitivity analyses of fluoridation status and tooth-brushing/Aboriginal status. A p-value of less than 0.05 was considered statistically significant.
Ethics approval
Ethics approval for the survey was granted by the NSW Population & Health Services Research Ethics Committee (Reference 2011/07/336), the ACT Health Human Research Ethics Committee (approved on 22 July 2011), the NSW Department of Education and Communities through the State Education Research Approvals Process, the ACT department of Education and Training, the Aboriginal Health and Medical Research Council Human Research Ethics Committee and the University of NSW Human Research Ethics Committee.
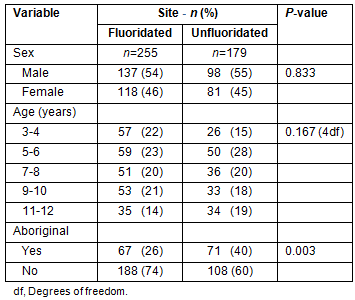
A dental examination was performed for 434 children (response rate 72%). Of the unexamined children, six had informed parental consent but refused an examination, 13 were absent from school, and the remainder did not obtain informed parental consent. Participants ranged in age from 3 to 12 years (mean age 7.7 years) and more participants were male than female (235 & 199, respectively). More participants identified as non-Aboriginal (68%) than Aboriginal (32%) and slightly more attended school in fluoridated sites (59%) than unfluoridated sites (41%). Most children used fluoridated toothpaste (99%), and most had never taken fluoride tablets (95%). Exactly half of all parents reported having a healthcare or concession card and more than two-thirds of parents (73%) had completed school. Finally, only half of all children (49%) brushed their teeth more than once a day, and just over half (56%) had visited the dentist in the previous 12 months. Table 1 shows the number and proportion of children at fluoridated and unfluoridated sites by sex, age and Aboriginal status.
No statistically significant differences were found between Aboriginal and non-Aboriginal children in baseline characteristics such as age, use of fluoride tablets, use of fluoride toothpaste or timing of the most recent dental visit; however, Aboriginal children were significantly more likely to attend school in an unfluoridated area (p=0.003) (Table 1), brush less often (p<0.001) and have parents who held a concession card (p<0.001) and had not completed school (p<0.001).
A mixed fluoride history was recorded for 53% of children; that is, these children had lived in both a fluoridated and an unfluoridated area in their lifetimes.
The intra-class correlation coefficient for the validity of the examiners was 0.96 for the decayed, missing or filled surfaces per child, and the kappa value indicating agreement between examiners and the gold standard was 0.91 for the decayed, missing or filled category of individual teeth. The intra-class correlation coefficient indicating the reliability of the examiners averaged 0.97 for decayed, missing or filled surfaces per child.
Table 1: Descriptive statistics of children in the NSW South Coast Child Dental Health Survey at fluoridated and unfluoridated sites by sex, age and Aboriginal status
Oral health
The 5-6 year-old children had an average dmft of 1.5, and 11-12 year-old children had an average DMFT of 1.0. For Aboriginal children, the 5-6 year-old dmft was 2.3 and 11-12 year-old DMFT was 2.1. In unfluoridated areas, the 5-6 year-old dmft was 2.1 and 11-12 year-old DMFT was 1.3. A total of 51% of 5-6 year olds in the sample had no caries experience (dmft/DMFT=0), and 38% of 11-12 year olds had no caries experience.
Predictors of caries
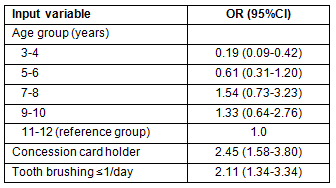
In the final model, the only factors significantly associated with having caries (Y/N) were age group, concession card status and tooth-brushing frequency. Children of parents with a concession card were approximately 2.5 times more likely to experience caries, and children who brushed their teeth less than twice/day were approximately twice as likely to experience caries. Gender, water fluoridation, Aboriginal status and parental education were not significant predictors of caries experience (Table 2).
Table 2: Significant predictors of caries experience in children aged 3-12 years in three small rural/regional NSW communities, 2011
Sensitivity analysis
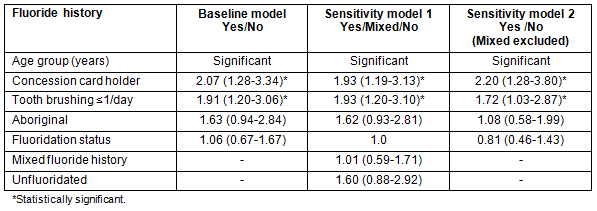
The finding that water fluoridation was not significantly associated with caries was unexpected, so the authors investigated whether there may have been some dilution bias in the way children were categorised into fluoridated or unfluoridated groups. Primary sensitivity analyses were therefore performed for the group of children with a mixed fluoride history (ie children who have lived or attended school in both a fluoridated area and unfluroidated area in their lifetime). In sensitivity model 1, data were analysed for three fluoride histories; fully fluoridated, fully unfluoridated and mixed. In sensitivity model 2, children with a mixed fluoride history were excluded from the analysis, leaving 'pure' fluoridated and unfluoridated groups. While these models resulted in slightly altered odds ratios, concession card status and tooth-brushing frequency remained significantly associated with caries in both models, and gender, water fluoridation, Aboriginal status and parental education remained non-significantly associated (Table 3).
As the tooth-brushing and Aboriginal status variables were strongly associated, secondary sensitivity analyses were performed to determine which was the driving factor in caries experience. In sensitivity model 1, tooth-brushing was excluded, and Aboriginal status became significantly associated with caries experience (OR=1.9, 95% CI 1.12-3.24). In sensitivity model 2, Aboriginal status was forced into the final model, with age group, concession card status and tooth-brushing frequency. In this model, Aboriginal status still conferred a higher risk for caries experience, but was not significant (OR=1.64, 95% CI 0.94-2.85), and the odds ratios for the other variables decreased but remained significant.
Table 3: Primary sensitivity analyses, NSW South Coast Child Dental Health Survey
Discussion
Concession card status, age and brushing frequency were highly significant predictors of caries experience in these communities. Aboriginal status also became a significant variable in sensitivity analyses.
While the small number of children living in unfluoridated areas in NSW necessarily limited the sample size, the regression modelling had sufficient power to detect three independent factors significantly associated with caries experience. It is possible that with a larger sample size, other variables, namely Aboriginal status and water fluoridation may have become significant. Nevertheless, this study has shown that water fluoridation and Aboriginal status are less significantly associated with caries in these communities than socio-economic status, age and tooth-brushing.
Data were primarily analysed according to children's current school fluoride status. This was done deliberately to improve accuracy; however, it may have introduced some dilution bias into the results; for example, a child who attended school in an unfluoridated area but lived in a fluoridated area (either currently or in the past) would have been assigned to the unfluoridated group, but would have the benefit of water fluoridation in their home. This dilution bias may be significant, because it is known that approximately half of the children had a mixed fluoride history; however, in sensitivity analyses these results persisted even when the mixed fluoride group was removed, leaving 'pure' fluoridated and unfluoridated groups, showing that the dilution bias does not significantly affect the results.
The remaining findings of this study are consistent with the bulk of Australian literature about risk factors for dental caries. The present study sample had worse oral health than either state or national average in both the 5-6 year old and 11-12 year age group8,14. This finding is consistent with other studies, which show that child oral health is worse in rural or remote Australian communities8,9. Concession card status was used in this study as one indicator of a family's socioeconomic status. The strong association between poor oral health and low socioeconomic status is also well established11,15-17, and is consistent with the present results. Finally, Aboriginal children have consistently been shown to have poorer oral health than non-Aboriginal children9-11. This difference between Indigenous and non-Indigenous children's oral health also exists in many other countries, including New Zealand, Canada and the USA10,18. The present study found that being Aboriginal was associated with brushing less frequently, a finding that is also consistent with other Australian literature9,19.
In the broader context of closing the substantial gap in health outcomes between rural and metropolitan residents, Aboriginal and non-Aboriginal people and those from high and low socioeconomic backgrounds, a combination of water fluoridation and targeted approaches to improving oral health will be needed. It is acknowledged that there is a strong body of evidence showing that water fluoridation is effective in reducing caries, and is particularly useful for reaching the most disadvantaged any community; however, this study indicates that approaches targeting other risk factors may also have good impact. Given the low tooth-brushing frequency this study found among Aboriginal children and the well-established preventive effect of daily brushing with fluoride toothpaste20,21, a school-based program to increase tooth brushing for Aboriginal children may be an initial step for improving oral health outcomes; however, it must be remembered that these programs have historically been relatively resource-intensive and difficult to implement, and only able to reach children who attend school and are compliant.
The rural/remote children in this study had worse oral health than either state or national average in both the 5-6 year old and 11-12 year age groups. Socioeconomic status, tooth-brushing and Aboriginal status were significantly associated with caries in these communities. To close the substantial gap in oral health outcomes between rural and metropolitan residents, approaches that target rural areas, Aboriginal people and those from low socioeconomic backgrounds are needed.
Acknowledgements
This work was completed while Dr Zander was an employee of the NSW Public Health Officer Training Program, funded by the NSW Ministry of Health. She undertook this work while based at the NSW Centre for Oral Health Strategy. The Program is offered in partnership with the University of New South Wales.
References
1. Armfield J, Roberts-Thomson K, Spencer A. Australia's Health 2000: the seventh biennial health report of the Australian Institute of Health and Welfare. Canberra, ACT: Australian Institute of Health and Welfare, 2000; 19.
2. Mason J, Pearce MS, Walls AW, Parker L, Steele JG. How do factors at different stages of the lifecourse contribute to oral-health-related quality of life in middle age for men and women? Journal of Dental Research 2006; 85(3): 257-261.
3. Ylostalo PV, Järvelin MR, Laitinen J, Knuuttila ML. Gingivitis, dental caries and tooth loss: risk factors for cardiovascular diseases or indicators of elevated health risks. Journal of Clinical Periodontology 2006; 33(2): 92-101.
4. Taylor GW, Borgnakke WS. Periodontal disease: associations with diabetes, glycemic control and complications. Oral Disease 2008; 14(3): 191-203.
5. Joshipura KJ, Hung HC, Rimm EB, Willett WC, Ascherio A. Periodontal disease, tooth loss, and incidence of ischemic stroke. Stroke 2003; 34(1): 47-52.
6. Xiong X, Buekens P, Fraser WD, Beck J, Offenbacher S. Periodontal disease and adverse pregnancy outcomes: a systematic review. British Journal of Gynaecology 2006; 113(2): 135-143.
7. Australian Institute of Health and Welfare. Australia's dental generations: the National Survey of Adult Oral Health 2004-06. Dental Statistics and Research Series no 34. Canberra, ACT: Australian Institute of Health and Welfare, 2007.
8. Armfield JM, Spencer AJ, Brennan DS. Dental health of Australia's teenagers and pre-teen children: the Child Dental Health Survey, Australia 2003-04. Canberra, ACT: Australian Institute of Health and Welfare, 2010.
9. Kruger E, Dyson K, Tennant M. Pre?school child oral health in rural Western Australia. Australian Dental Journal 2008; 50(4): 258-262.
10. Harford J, Spencer J, Roberts Thomson K. The Health of Indigenous Australians. Oral Health. Oxford: Oxford University Press, 2003.
11. Hallett K, O'Rourke P. Dental caries experience of preschool children from the north Brisbane region. Australian Dental Journal 2002; 47(4): 331-338.
12. Wright JC, Bates MN, Cutress T, Lee M. The cost-effectiveness of fluoridating water supplies in New Zealand. Australian and New Zealand Journal of Public Health 2001; 25(2): 170-178.
13. Computer Assisted Telephone Interviewing Technical Reference Group. Population Health Monitoring and Surveillance: Question Development Field Testing, Field Test 1 Report. Asthma. Canberra, ACT: Demographic Characteristics & Diabetes PHDIS Unit and Australian Institute of Health and Welfare, 2003.
14. Phelan C, Byun R, Skinner JC, Blinkhorn AS. Child Dental Health Survey 2007: a snapshot of the oral health status of primary school-aged children in NSW. New South Wales Public Health Bulletin 2009; 20(4): 40-45.
15. Sanders A. Social Determinants of Oral Health: conditions linked to socioeconomic inequalities in oral health and in the Australian population. AIHW Population Oral Health Series no 7. Canberra, ACT: Australian Institute of Health and Welfare, 2007.
16. Slade GD, Sanders AE, Bill CJ, Do LG. Risk factors for dental caries in the five-year-old South Australian population. Australian Dental Journal 2006; 51(2): 130-139.
17. Vargas CM, Crall JJ, Schneider DA. Sociodemographic distribution of pediatric dental caries: NHANES III, 1988-1994. Journal of the American Dental Association1998; 129(9): 1229-1238.
18. Williams S, Jamieson L, MacRae A, Gray C. Review of Indigenous oral health, 2011. Australian Indigenous HealthInfoNet. (Online) 2011. Available: http://www.healthinfonet.ecu.edu.au/other-health-conditions/oral/reviews/our-review (Accessed 27 June 2013).
19. Jamieson LM, Bailie RS, Beneforti M, Koster CR, Spencer AJ. Dental self-care and dietary characteristics of remote-living Indigenous children. Rural and Remote Health 6(2): 503. (Online) 2006. Available: www.rrh.org.au (Accessed 20 June 2013).
20. Marinho VC, Higgins JP, Sheiham A, Logan S. Fluoride toothpastes for preventing dental caries in children and adolescents. Cochrane Database of Systemic Reviews 2003(1): CD002278.
21. Centers for Disease Control and Prevention. Recommendations for Using Fluoride to Prevent and Control Dental Caries in the United States. Morbidity and Mortality Weekly Report 2001. Available: http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5014a1.htm (Accessed 27 June 2013).


