full article:
Health statistics demonstrate that people living in rural and remote areas have poorer health outcomes than their counterparts living in major cities. Their lives are shorter and they are more likely to exhibit unhealthy behaviours1. At the same time medical practitioners are unevenly dispersed across Australia, resulting in more limited services in some rural areas2. Effective medical practitioner attraction and retention strategies for rural areas have been sought to improve the availability of services. A recent review of factors making health professionals more likely to work in rural areas has again shown that a 'selection' of rural background students and rural 'education' of undergraduate students are the strongest predictors of future rural practice3. In 2001 the Australian Government Department of Health began what is now the Rural Clinical Training and Support (RCTS) program, which funds rural background 'selection' and rural clinical 'education'. The RCTS program operates in 16 rural clinical training schools from as many universities and exposes 25% of medical students to rural clinical and community 'education' for an extended period4.
At the University of Adelaide, students of the 6-year undergraduate medical program (MBBS; Bachelor Medicine Bachelor of Surgery) have the opportunity to complete the whole of their fifth year of clinical studies at a rural location under the direction of the Discipline of Rural Health. These 'rural cohort' students are taught a parallel curriculum and are examined in the same manner as their city-based counterparts. There are eight widely dispersed learning sites available which range from inner regional to very remote locations.
The University of Adelaide RCTS program is now in its 11th year, having commenced in 2003. This was considered enough time to measure the impact of the graduates of the program on the rural workforce, with the 2003 cohort being postgraduate for 8 years. These cohorts have not been formally tracked until this point. This study is additional to the data collected for the Medical Schools Outcomes Database, which will track Australian medical graduate movement in the long term5.
In late 2012 a retrospective study of the rural cohort students of the University of Adelaide MBBS students who completed their fifth year of clinical studies at a rural location in years 2003 to 2010 was conducted. Only domestic students were included in the study. Recruitment involved obtaining email details of the 127 past students of interest using tools such as alumni records, a rural cohort Facebook page and previously known contact details. Details of 124 past students were found. SurveyMonkey was judged to be an appropriate online instrument for this type of study6. Each past student was sent an email directing them to a 28-question self-complete online survey. Respondents were required to confirm informed consent in order to begin the survey.
The survey was developed to include open and close-ended questions about rural background, placement details, the program's influence, past career decisions and future career intent, including corresponding locations (Appendix 1). A record of career movements since graduation was the only compulsory question. Quantitative data were analysed using descriptive statistics in the Statistical Package for the Social Sciences v20 (SPSS Inc; www.spss.com) and qualitative data underwent thematic analysis in NVIVO v9 (QSR International; http://www.qsrinternational.com/products_nvivo.aspx). A very small number of respondents indicated they took part of some years out of their medical career for parental leave or were travelling overseas. Both of these groups' locations were included in the analysis.
Several systems are used to classify remoteness in Australia, with two outlined in Table 1. The system used in the analysis of this study is the Australian Standard Geographical Classification - Remoteness Area (ASGC-RA) system as defined by the Department of Health's Rural and Regional Health Australia, and is used by the RCTS7.
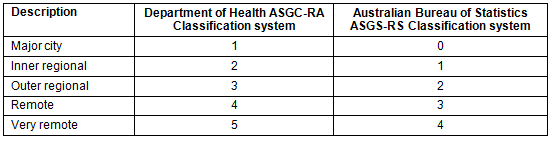
ASGC-RA2-RA5 are regarded as 'rural' areas by the Department of Health for the purpose of this medical education program.
Ethics approval
Ethics approval for the study was gained from the University of Adelaide Human Research Ethics Committee; ethics approval number H2012124.
Seventy-five survey responses were received but one respondent discontinued after only a few questions, leaving 74 useful responses, with a response rate of 58.2%. This is in line with similar single-university surveys that track RCTS program participants, such as those conducted by the University of Queensland and Flinders University in South Australia9-12. Some participants did not answer all questions and therefore totals were adjusted accordingly. There were higher numbers of responses from later cohort years, which is reflective of the program's expansion in recent years. The response rate varied across cohort years, ranging from 40.0% to 73.0%.
Twenty-one respondents (28.4%) had spent more than 5 years in a rural area from the beginning of primary school to the beginning of university and 11 (14.9%) had spent some time but less than 5 years. Forty-two respondents (56.8%) had spent no time in a rural area.
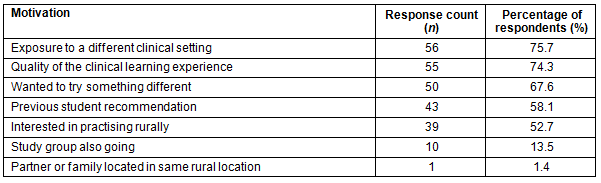
Respondents indicated they entered into the RCTS program for a variety of reasons (Table 2). The most prevalent reasons were 'exposure to a different clinical setting' and 'quality of the clinical learning experience'.
The survey made ample provision for respondent comments. These sections were well used and the information gathered provides more depth to quantitative data. Some comments provided by respondents follow.
Love the country lifestyle, being able to know everyone within the hospital/practice rather than being faceless in the city hospitals, felt very supported by colleagues.
... (I enjoyed the) workplace dynamics - (there is a) much flatter hierarchy than in the hospital system.
The need to do bulk of postgrad training for non-GPs in city is major risk for losing people from rural health.
If my speciality allows - at the moment it looks like I will not be able to do more than 3 months of my basic training and none of my advanced training in a rural area. It is difficult to practice medical specialities in rural areas and I do not have any interest in being a GP.
Table 2: Motivations for entering the Rural Clinical Training and Support program
Program outcomes
Respondents were asked to record the career choices they had made since graduation, including the stage of their training, the speciality they had chosen and the location of each corresponding year.
There were several medical areas in which respondents had chosen to specialise (Table 3). The specialty chosen most was general practice (12 respondents; Royal Australian College of General Practitioners (RACGP) and Australian College of Rural and Remote Medicine (ACRRM)). Twenty-six respondents selected that entering a postgraduate training program was not applicable in 2012. Many of these respondents may have been completing an internship or generalist postgraduate year in 2012. Five respondents had completed postgraduate training by 2012, four of whom were Fellows of RACGP or ACRRM (Table 3). When asked about future career intentions, 85.1% of respondents indicated that they intended to work in a rural area.
The location choices of respondents can be presented in two ways: by 'years since graduation' (showing career progression) and by 'calendar year' (showing effect on rural workforce). This enables evaluation of the complexities of work location decisions over the period since graduation.
Table 4 shows the location of medical practice analysed by 'years since graduation'. It shows that respondents chose to work in a rural location at many points in their postgraduate career and training. During the first year post-graduation from university, a pre-registration or intern year, 13 respondents (18%) were located outside of a major city. The year for which the greatest number of respondents (16 out of 58 respondents (27.6%)) were located outside of a major city was the second year after graduation. Tables 4 and 5 show that respondents travel to both developing and developed overseas countries in various years post-graduation.
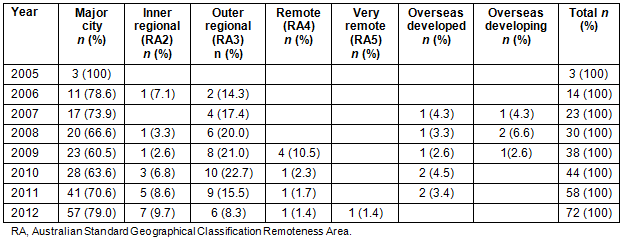
In any given year, between 17.4% and 34.1% of the respondents were located in ASCG-RA2-RA5 areas, an average of 21.8% across the eight possible years (Table 5). Outer regional areas (ASGC-RA3) were the most prevalent rural areas that respondents had chosen to locate themselves in while only one respondent was located in a very remote area (ASGC-RA5) in 2012. However, many of those located in outer regional (ASCG-RA3) and and remote (ASGC-RA4) areas indicated in comments that they visited very remote areas to run clinics as part of their position. In 2012, 15 respondents (20.8%) were located in a rural area (ASGC-RA2-RA5; Table 5). The 2012 data were used for cross-analysis with subsequent questions.
It is possible to aggregate data that are gathered from questions related to location to make a statement about the time that individual respondents have spent in a rural location since graduation, keeping in mind the varying amount of time that graduates have spent post-graduation. From this it is apparent that 32 people (44%) have spent no time in a rural location since graduation, 20 people (28%) have spent between 3 and 18 months in a rural area since graduation and 20 people (28%) have spent two or more years in a rural area since graduation.
Table 3: Specialisations for which respondents were training or had completed in 2012
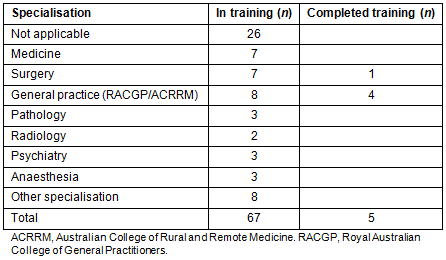
Table 4: Australian Standard Geographical Classification Remoteness Area locations of respondents by year since university graduation
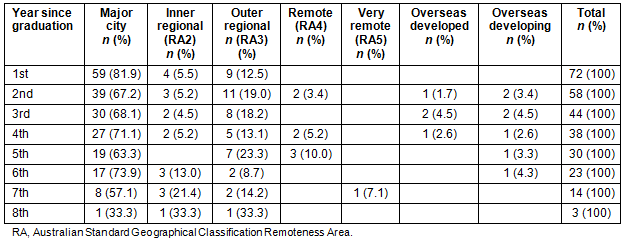
Table 5: Australian Standard Geographical Classification Remoteness Area locations of respondents, by calendar years
Program impact
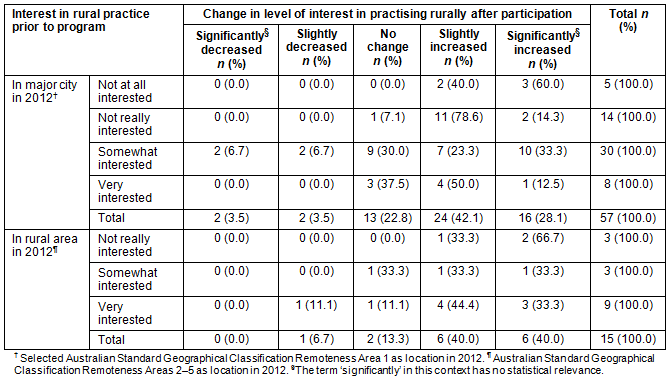
Table 6 shows the interest respondents had prior to completing the RCTS program and the level of change the program brought to their interest in working in a rural area. Results for respondents located in a major city (ASGC-RA1) and rural area (ASGC-RA2-RA5) are shown separately. Observations from this table include the following:
- Five respondents located in a rural area in 2012 and who were initially either 'not really' or 'somewhat interested' in practising in a rural area indicated the RCTs program either 'slightly' or 'significantly increased' their interest.
- Seven respondents located in a rural area in 2012 and who were initially 'very interested' in practising in a rural location indicated the RCTS program 'slightly' or 'significantly increased' their interest.
- Eighteen respondents located in a major city in 2012 and who were initially 'not at all' or 'not really interested' in rural practice indicated the RCTS program 'significantly' or 'slightly increased' their interest.
- Twenty-two respondents located in a major city in 2012 and who were initially 'somewhat' or 'very interested' in rural practice indicated the RCTS program 'slightly' or 'significantly increased' their interest.
- Five people located across both rural areas and a major city in 2012 and who were initially either 'somewhat' or 'very interested' in rural practice indicated the RCTS program either 'slightly' or 'significantly decreased' their interest in rural practice.
Table 6: Location chosen for 2012 and initial and change in interest in practising in a rural area after completing the Rural Clinical Training and Support program
Discussion
Impact on the rural workforce
This study reports on the postgraduate career progress of 74 (58.2%) rural cohort medical students of the University of Adelaide and their contribution to the rural medical workforce. In recent years (2009-2012) between 20.8% and 34.1% of respondents were located in RA2-RA5. More than half of respondents have spent time in a rural area since graduation; additionally, 85.1% of respondents indicated they had intentions to work in a rural area.
These young doctors frequently move between rural and urban locations, which makes it difficult to express the contribution that graduates who participated in the RCTS program have had on the rural workforce. Many respondents indicated in qualitative comments that they had not chosen one area over the other because they are still completing training. The data produced from this study can account for this movement by showing how long each respondent has spent in a rural area since graduation, perhaps capturing their contribution to the rural workforce more clearly. The 20 graduates (28%) who had spent between 3 and 18 months in a rural area may have been on obligatory rural rotations in their training programs whereas the 20 graduates (28%) who had spent two or more years in a rural area were more likely making an active choice to work in a rural area, some having spent as long as 5 to 7 years rurally. South Australia is a very centralised state with only 27% of the population residing outside the metropolis of Adelaide13. The RCTS program graduate numbers are in similar proportion to the current workforce and the population distribution in South Australia. These data do not suggest that the graduates are redressing the rural medical workforce shortage.
The rural service delivery model that has evolved in South Australia is largely peripatetic: medical specialist services are delivered by day visits and recently some distance technologies. As a result many respondents felt restricted to a major city where specialist training positions are almost exclusively located, some with rural rotations.
Although this analysis hasn't discriminated between states where the graduates now reside, because of the small sample size, subsequent data collection on the enlarging cohort and with longer postgraduate duration will explore an Australia-wide rural workforce impact. These 2012 data, with approximately 20% of University of Adelaide graduates being in rural areas and RACGP/ACRRM fellowships being the most common, suggest that this cohort is contributing to the South Australian rural workforce in proportion to the state's rural-urban population split.
These data support the suggestion that 8 years post-graduation may not be long enough to assess the rural work force outcome14. In addition to the mobile nature of respondents, only five respondents had completed postgraduate training. Of the five who had completed, four were Fellows of RACGP/ACRRM training and one a surgeon (Table 3). All of the RACGP/ACRRM fellows being based in ASGC-RA2 or ASCG-RA3 is a positive indication of the contribution to the rural workforce. Further longitudinal surveying of the enlarging rural cohort will show longer term trends in work location choice.
Influence on career decision-making
It is difficult to show the impact of a voluntary RCTS program; the initial interest many participants have in rural medicine prior to taking part creates a bias10. Somers and Spencer15 have shown that this initial interest increases the likelihood of practising in a rural location. Yet there were respondents who were initially 'very interested' in rural practice whose interest was further increased and were practising in rural areas in 2012. The role of the RCTS program, including the initial decision to take part in it, is important in the progression from medical school to rural practice11,12,16.
Also, the RCTS program exposes students not initially interested in rural medicine to rural practice and inspires an interest in it. The majority of respondents indicated they entered the RCTS program for the 'quality of the clinical learning experience' and for 'exposure to a different clinical setting', often because of advice from past rural cohort students (Table 2). Qualitative comments also confirm this by saying that the RCTS program provides an opportunity to be exposed to rural practice in a supportive, non-hierarchical environment. Just over half of respondents indicated an interest in rural medicine as a motivation for entering the program, so this was not a universal reason. There were respondents working in a rural area in 2012 who were initially only 'not really' or 'somewhat interested' in rural practice that indicated an increased interest.
Study limitations
The initial cohort size and response rate of this study are small with 74 respondents (58.2% response rate). High quality, recent contact details for past graduates of the medical program are difficult to locate. There is a risk of selection bias with people that choose to answer the survey possibly having a greater interest in rural practice and therefore desire to be involved in such a study. These limitations, together with the length of postgraduate training, make it difficult to demonstrate the outcome of the RCTS program as yet. Repeating the survey with a larger sample, as intended, will provide more meaningful insight.
This is the first study of the University of Adelaide RCTS program rural cohort students to report on rural workforce outcomes. The study shows that the program is having a positive impact on the interests of some medical students to transition to rural medicine while providing quality education experiences. Further graduate tracking research, such as the Medical Schools Outcome Database, will document levels of interest at outset and longer term graduate tracking in postgraduate careers.
Acknowledgment
This study was funded as an evaluative requirement of the Department of Health Rural Clinical Training and Support scheme for the Discipline of Rural Health, University of Adelaide.
References
1. Australian Institute of Health and Welfare (AIHW). Australia's health 2012. Canberra, ACT: AIHW, 2012.
2. Walker J, DeWitt DE, Pallant J, Cunningham C. Rural origin plus a rural clinical school placement is a significant predictor of medical students' intentions to practice rurally: a multi-university study. Rural Remote Health 12: 1908. (Online) 2012. Available: www.rrh.org.au (Accessed 20 December 2013).
3. Wilson N, Couper I, De Vries E, Reid S, Fish T, Marais B. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural Remote Health 9(2): 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 20 December 2013).
4. Commonwealth Department of Health and Ageing (DoHA). Rural Clinical Training and Support 2011 - 2014 - Program guidelines. Canberra, ACT: DoHA, 2012.
5. Medical Deans Australia and New Zealand. Medical Schools Outcome Database. (Online) 2010. Available: http://www.medicaldeans.org.au/msod (Accessed 8 January 2014).
6. Van Gelder MM, Bretveld RW, Roeleveld N. Web-based questionnaires: the future in epidemiology? American Journal of Epidemiology 2010; 172(11): 1292-1298.
7. Australian Government Department of Health, Rural and Regional Health Australia. Map layer information. (Online) 2013. Available: http://www.ruralhealthaustralia.gov.au/internet/rha/publishing.nsf/Content/LayerInformation (Accessed 13 January 2014).
8. Australian Bureau of Statistics, Australian Statistical Geography Standard (ASGS): Volume 5- Remoteness Structure. Report No. 1270.0.55.005. (Online) 2001. Available: http://www.ausstats.abs.gov.au/Ausstats/subscriber.nsf/0/A277D01B6AF25F64CA257B03000D7EED/$File/1270055005_july%202011.pdf (Accessed 13 January 2014).
9. Eley D, Baker P, Chater A. The Rural Clinical School Tracking Project: More IS better - Confirming factors that influence early career entry into the rural medical workforce. Medical Teacher 2009; 31(10): e454-459.
10. Worley P, Martin A, Prideaux D, Woodman R, Worley E, Lowe M. Vocational career paths of graduate entry medical students at Flinders University: a comparison of rural, remote and tertiary tracks. Medical Journal of Australia 2008; 188(3): 177-178.
11. Stagg P, Greenhill J, Worley P. A new model to understand the career choice and practice location decisions of medical graduates. Rural and Remote Health 9(4): 1245. (Online) 2009. Available: www.rrh.org.au (Accessed 20 December 2013).
12. Eley D, Baker P. Does recruitment lead to retention? Rural Clinical School training experiences and subsequent intern choices. Rural Remote Health 6(1): 511. (Online) 2006. Available: www.rrh.org.au (Accessed 20 December 2013).
13. Australian Bureau of Statistics (ABS). Regional population growth, Australia, 2012. Report No. 3218.0. (Online) 2012. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/3218.02012?OpenDocument (Accessed 18 February 2013).
14. Eley D, Synnott R, Baker P, Chater A. A decade of Australian Rural Clinical School graduates - where are they and why? Rural Remote Health 12: 937. (Online) 2012. Available: www.rrh.org.au (Accessed 20 December 2013).
15. Somers GT, Spencer RJ. Nature or nurture: The effect of undergraduate rural clinical rotations on pre-existent rural career choice likelihood as measured by the SOMERS Index. Australian Journal of Rural Health 2012; 20(2): 80-87.
16. Playford DE, Cheong E. Rural Undergraduate Support and Coordination, Rural Clinical School, and Rural Australian Medical Undergraduate Scholarship: rural undergraduate initiatives and subsequent rural medical workforce. Australian Health Review 2012; 36(3): 301-307.
_____________________________
Appendix I: Online survey regarding career choices since graduation and experiences during the Rural Clinical Training and Support program



