Worldwide, nursing is facing a significant challenge in recruiting people into the profession and retaining these nurses in the workforce. This is especially true for Australian rural areas, which continue to experience significant nursing shortages over a sustained period1-7. Shortages are spread across all fields of nursing including mental health, emergency, intensive care and general nursing8,9. Simultaneously, the current Australian nursing workforce is ageing with large numbers of nurses due to retire10 and one-third of new graduate nurses leaving within the first 5 years of graduation11. Health Workforce Australia (HWA)10 forecast nursing shortages to continue across Australia with a predicted shortfall of 24 767 registered nurses in 2025 for the state of New South Wales (NSW) alone. Compounding the current rural nursing shortage, many experienced nurses have lost their jobs due to the recent 'slash and burn' health budget cuts across Australian states and territories12. Together, health budget cuts, recruitment, retention and retirement are exacerbating the difficulties of sustaining an adequate rural nursing workforce4,12-15.
According to the Australian Institute of Health and Welfare (AIHW)16 the Australian nursing workforce has 268 018 registered nurses who are registered with the Australian Health Practitioner Regulation Authority and of these 86 497 reside in NSW16. Approximately 13% of the nursing workforce are not employed in nursing which, for NSW, equates to 11 240 registered nurses not working in nursing16. In September 2012 in NSW alone, there were 1520 nursing vacancies in the NSW Health Department17. Theoretically, eight registered nurses are available in NSW for each vacant nursing position with NSW Department of Health, the major employer of nurses in that state.
Australian rural areas have lower retention rates of nurses than their metropolitan counterparts, with more remote communities experiencing an even higher turnover of nursing staff18. In rural communities, nurses make up a greater proportion of the health workforce than in metropolitan settings which makes their role in service provision even more significant19. Rural communities often lack health services, and community members have poorer health outcomes than their metropolitan counterparts20. Rural nursing encompasses unique features, with health service delivery often occurring in isolation from other nurses and support services because of the vast geographical areas nurses work in; this is an everyday part of rural nursing. There is an acknowledgment that rural nursing practice is different from nursing practice in metropolitan areas19. First, by necessity, rural nurses tend to be more generalist practitioners than specialists19,20; in other words, rural nurses often work in small hospitals that provide a wide variety of nursing care, with the scope of practice covering prevention, intervention and rehabilitation across the lifespan19. Second, rural nurses provide multiple services that metropolitan nurses do not provide. For example, in an inner city hospital in Australia, specialised teams deal with all aspects of patient care; however, in a small rural hospital, nurses will deal with all aspects of health care from a cardiac arrest or major car accident through to aged care20.
The role of rural nursing differs from that of metropolitan nursing, and many metropolitan nurses lack an understanding of these differences. This is particularly so in relation to rural isolation as this isolation has an impact on both clinical issues and clinical decisions, therefore making rural nursing unique21. Several issues compound and impact on rural nursing. These are a lack of access to further nurse education and professional development, personal and professional isolation19-21 and a lack of anonymity in small communities, which can compound issues such as mandatory reporting, dealing with disclosures and reporting abuse20,21. In addition are the implications of living and working in the same community6, a concept unique to rural nursing. Rural nurses have to not only understand the culture of the wider rural community, but also understand and manage their local workplace culture. This includes understanding and communicating to others the peculiarities and work patterns of general practitioners and other allied health practitioners with whom they work6. Combined with a lack of mentoring and debriefing6, as well as the difficulties of being managed from a distant geographical location often several hundred kilometres away21, rural nursing is a complex practice. In addition, workplace inflexibility and limited access to acceptable housing contribute to the difficulties of attracting nurses to the rural workforce19.
The purpose of this study was to explore why registered nurses resigned from rural hospitals and to generate a potentially useful substantive (ie beginning or new) theory, a theory that could be used to assist in developing retention strategies for the nursing workforce in NSW rural hospitals. Grounded theory (GT) methods are more commonly used to study areas in which little previous research has been conducted, but GT is also used to gain a new perspective and open up an area that has been frequently studied: the nursing shortage22. This study was informed by Glaserian GT methods23,24.
This study recruited participants from a broad geographical spread of rural NSW who had resigned from a rural hospital. Participants were required to meet the following inclusion criteria:
- they were a registered nurse
- they had resigned from a rural hospital or area health service after 1 January 2000 (this date was chosen to allow for recruitment from a wider population of nurses)
- the reasons for resignation were not associated with maternity leave, retirement or a family member's geographical relocation.
Participants were recruited by placing advertisements in NSW nursing journals, NSW rural newspapers and a rural electronic newsletter. Participants' previous nursing positions ranged from clinician to senior manager. Other demographic characteristics are presented in Table 1. Data were collected from 12 participants between 2004 and 2009; two participants were re-interviewed in order to elicit further data on key concepts and to enhance category development. All interviews were conducted by a single researcher; the length of each interview varied from 50 minutes to 2 hours and all interviews were audio-recorded. Interviews commenced with two open-ended broad questions ('Tell me your experience of working in a rural hospital' and 'Tell me about what happened when you resigned'). As each interview progressed, the researcher sought to clarify responses and to probe further to expand on responses as the analysis progressed, with questions becoming more focused around the emerging GT. Interviews were then transcribed verbatim and imported into the NVivo v7 software program (QSR International, http://www.qsrinternational.com) for data management.
Consistent with GT methods, data collection and data analysis occurred simultaneously. Participants were interviewed, transcripts analysed and interview questions formulated for the next participant. One researcher coded the data at all times. After the first interview was coded the secondary supervisor validated the coding. Interviews were conducted at either the researcher's or the participant's workplace. Analysis began with creating open codes, a process of analysing interview transcripts line by line. Open codes were then compared with other open codes for similarities and differences. Open codes were subsumed into groups to form preliminary categories. Emergence of the core category occurred after further scrutiny of the data and memo writing (a technique used in GT research to document emerging theoretical insights23,24). After the emergence of the core category, the process of theory building was facilitated by using theoretical coding families (which provide a range of options for theoretical coding as well as a list of theoretical codes to assist the researcher in exploring relationships among the categories23), sorting of theoretical memos and by the integration of theoretical codes. Theoretical codes conceptualise how substantive codes relate to each other and provide the model for theory generation23. Through the relationships of categories and properties the theory becomes 'dense and saturated'23 (p. 93).
Ethics approval
Institutional ethical approval was granted by the human ethics committee at Charles Sturt University; ethics approval number 2004/228. An information sheet explaining the purpose of the research was provided to each participant and all participants provided voluntary consent. The participants were informed that their confidentiality would be maintained and that they could withdraw from the research at any time. As data collection involved participants reflecting on a stressful time of their resignation all participants were offered counselling, but none required it.
Table 1: Participant characteristics

The GT 'degree of value alignment' emerged from the data and conceptually explains why rural nurses resigned - resignation occurred when nurses were unable, or unwilling, to realign their personal values to changed organisational values that have occurred over time in rural hospitals. The GT contained a core category (conflicting values) and a basic social process (degree of value alignment). The theory explains that nurses seek to realign their values in order to create balance (or alignment) with those of the organisation in which they work but when they are no longer able to achieve a balance, a values threshold is reached which in turn eventually leads to resignation. The degree of value alignment may be likened to a set of 'value alignment scales'. Figure 1 provides a visual representation of the GT.
The core category of conflicting values explains the conflict between nurses' personal values (how nurses perceive nursing should occur) and hospital values (how the hospital enables nurses to carry out nursing). Conflicting values also conceptualised a three-stage process, namely sharing values, conceding values and resigning. The transition from one stage to another was contingent on the occurrence of at least one catalyst (ie an event that nurses perceived caused a change in organisational values).
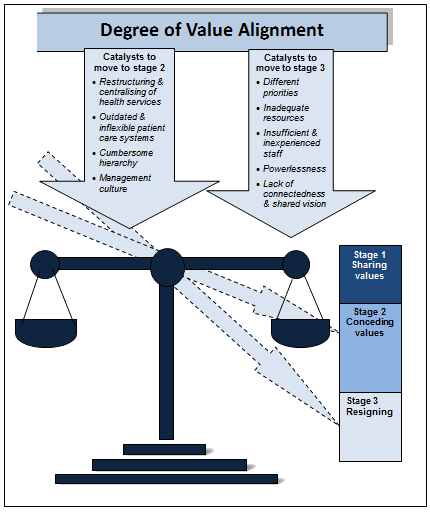
Figure 1: Theory - degree of value alignment
Stage 1: Sharing values
Sharing values explained that for the nurses in this study their personal values were (once) shared with the organisation in which they worked. Providing a high level of patient care was a value that all nurses in this study had in common and underpinned how they practised. The sharing of values was attributed to the fact that these nurses believed that they had the necessary support and resources required to provide a high standard of nursing care; these resources included adequate staffing levels, good communication with nursing hierarchies and budget allocations that were conducive to a high level of care provision. Evidence for sharing of values emerged when nurses spoke of 'the enjoyment of going to work' and 'satisfaction with work', 'being in a supportive environment' and 'having a team to back you'. This stage implied a collaboration, co-existence and co-agreement between the nurse and hospital as to how patient care should be provided.
To be a 'good nurse' was important to all participants and reflected being able to provide a high standard of patient care, being a person of high morals, being seen as a professional, able to treat all patients with respect, able to make people comfortable and always able to do the right thing. In this stage of sharing values, nurses experienced sufficient levels of job satisfaction and this was alluded to during their interviews when they spoke about their experiences in the organisation prior to the events that led to their resignation. Nurses expressed great pride in their work, a sense of satisfaction in being a nurse and an enjoyment of working with colleagues, and our 'workloads were high but [we] were energised and excited by [our] work and had a good network and rapport'. Nurses also felt that the hospital was 'a nice place to work' and they felt 'appreciated and respected'.
While nurses enjoyed a time of sufficient job satisfaction in the sharing values stage, there were specific catalysts (events or triggers) that nurses perceived changed the values of an organisation. These events saw nurses move from stage 1 to stage 2; the catalysts were restructuring and centralising of health services, outdated and inflexible patient care systems, cumbersome hierarchies, negative management culture, bullying, and an attitude (by senior staff in the organisation) that nurses were expendable.
Stage 2: Conceding values
In the second stage nurses began to surrender their values and perform nursing in accordance with the organisation's new values and not their own personal values. As nurses conceded their values, they began to become frustrated and increasingly dissatisfied with their work. The degree of alignment between their values and those of their organisations began to diverge.
As a consequence of the catalysts that moved nurses from stage 1 into stage 2, nurses began to unhappily compromise patient care. This occurred because of different priorities between nurse and organisation, inadequate provision of resources for patient care, and insufficient and inexperienced staffing levels. One participant (pseudonyms are used throughout) described how her priority was to provide a high standard of care while her manager's priority was to come in under budget:
They were being rewarded, all the NUMs [nurse unit managers], by how they undercut the budget and this NUM [name removed] was the only one that ever got an applaud or an award, or congratulations ... he would congratulate her but not anyone else because she comes under budget, all the other wards never ran out of food ... The individual thing in terms of the NUMs for linen and for the food, because we always ran out of linen, we were always ringing up trying to get towels and stuff ... Little things like that were really frustrating that you were always running out of, that you never had any of and you were fighting a constant losing battle. ('Sylvia')
Participants also described that patient care was compromised because of staffing problems and insufficient numbers of nursing staff on the ward to provide patient care. This caused participants to compromise patient care.
There wasn't enough staff and ... because of the staff numbers on the floor you couldn't look after them the way you would if you had the time to do it ... you know now some people would be sent to the wards still in bloody sheets and stuff like that because you didn't have time to change them. ('Lee')
It was in this stage that nurses became aware that their priorities were different to those of their hospital. In the sharing values stage, the nurse and hospital shared a priority of providing a high standard of patient care, but in stage 2 nurses became aware that there had been a change in hospital priorities; nurses perceived that their hospital's priority was money and cost savings to the detriment of patient care:
I think that whilst we are stewards of public money and whilst I acknowledge that we need to be good stewards with public money I also think we have lost focus on patients. ('Sally')
Frustration levels became higher for nurses and job satisfaction decreased as patient care was compromised. In this stage, nurses felt they were losing control of nursing decisions that allowed them to provide a high standard of care. Participants found that, due to the lack of these resources, patient care was compromised:
I pride myself in what I do and I just felt like I couldn't do it properly because I didn't have the time and didn't have the resources. ('Jade')
Increasing dissatisfaction was due to compromised values, and over time the gap between personal and organisational values widened. Unable to realign their values to those of the hospitals, nurses moved into the third and final stage, triggered by additional catalysts. These included powerlessness - participating in and witnessing poor patient care, a lack of connectedness and shared vision, and an impact on personal health. As a consequence of compromise of patient care nurses now compromised their personal and professional integrity, which they found deeply distressing.
As nurses believed that their ability to provide patient care became too compromised, they wrestled with their own personal values and felt that they were becoming increasingly powerless. Participants spoke of feeling disengaged and expressed a lack of connectedness with the health system:
I think that I had a feeling that our corporate goals were no longer the goals that I could support morally and ethically. ('Sally')
Stage 3: Resigning
The final stage was resigning. During this stage the nurse resigned, both in the verb meaning to 'give up' and the noun meaning to 'cease employment'. Nurses identified conceding too many of their personal values; this led to an overwhelming sense of compromised integrity and a lack of connectedness with the health system. Nurses entered a phase of 'giving up' as they were unable to resolve the problem of conflicting values and now felt despondent. One study participant summed this up as 'they won; I can't do this anymore'.
Nurses described personal health issues that affected them such as high blood pressure, headaches, emotional stress, episodes of crying, palpitations, chest pains and abdominal problems related to their work. One participant stated that:
When I went to work every evening on night duty I felt sick in the stomach and I felt palpitations. ('Juanita')
After resigning, participants expressed a sense of relief because they had dealt with the conflicting values, but also the sense of failure, anger and, for some, a loss of confidence and self blame about what went wrong.
I was just devastated, absolutely devastated, I've been, my confidence was shattered, my confidence in myself was shattered, its affected my ... son, he's coming home to a mother that's crying all day, his father's stressed because of the financial implications, ... it puts enormous strain on that and it's still, it's still being felt. ('Judy')
Discussion
A three-stage theory, degree of value alignment, emerged from this study. The first stage involved sharing values which seems to concur with Locke's theory of value congruence. Locke's25 theory of value congruence explains that employees are more satisfied with their employer and managers when they share common values. Locke25 refers to this as an entirety relationship because it involves a response to the other person as an end in itself. Value congruence seems to be a widely reported factor that contributes to nurse job satisfaction and nurse retention13,26-29. This study extends what is known about value congruence theory by identifying two further stages that follow sharing values. These additional two stages broadened Locke's25 value congruence theory by identifying the process that occurs when nurses move from a state of value congruence to job resignation. Importantly, the present study identified the catalysts that caused nurses to move from one stage to the next.
Nurses moved from stage 1 (sharing values) to stage 2 (conceding values) as a result of health service restructures that directly affected senior nurse managers. Interestingly, and following several very severe patient incidences in NSW public hospitals, the NSW Government convened a major review of the health system led by senior counsel Peter Garling. Garling comments in his report30 that the greatest criticism of current area health services in NSW is that they are too big, with decision-makers too remote from the people affected by decisions. Not surprisingly, this study, which collected data from some nurses who worked after the 2005 restructure, is consistent with many of Garling's criticisms. The 2005 NSW area health service restructures had a great impact on moving those nurses from a time of sharing values to a time of conceding values. Similarly, a study of remote area nurses across Australia found that the major contributor to job dissatisfaction and reduced levels of nurse retention was the physical distance of health managers from the actual work location31. On 1 January 2011, the original eight large area health services were restructured to form 18 local health networks32. At this stage, it is unclear how these restructures have impacted on nurse job satisfaction and retention.
This study also found that outdated and inflexible patient care systems moved nurses from sharing values to conceding values. The nurses in this study were more up-to-date with models of patient care than people in senior management positions, and the retention of out-dated practices impacted on a nurse's ability to provide a high standard of patient care. This finding raises a question about why nurse managers were not using current evidence to support practice. Alternative models of care have the capacity to accommodate ward circumstances including patients' needs, skill mix and staffing levels33.
The concept of a negative culture within management (termed 'organisational culture' or 'corporate culture' in the literature) emerged in this study as another contributor for moving nurses from sharing values to conceding values. There is a strong link between hospital organisational culture and nurse retention34-37. Organisational culture emerges from the sharing that occurs between colleagues in an organisation, including shared beliefs, attitudes, values and norms of behaviour. Thus, organisational culture is reflected by a common way of making sense of the organisation that allows people to see situations and events in similar and distinctive ways38. Garling30 also identified issues associated with management culture and recommended that a change of culture between clinicians and managers was required to improve health services.
The finding of conceding values was a stage where nurses perceived that the way they were able to provide patient care was starting to be compromised. This study explicitly found that nurses moved from stage 2 (conceding values) into stage 3 (resigning) due to feelings of powerlessness caused by participating (unwillingly) in, and witnessing poor patient care, a lack of connectedness and shared vision with the hospital, and an impact on the nurses' own health. These experiences of the participants in this study resonate with Jameton's descriptions of moral uncertainty, moral dilemmas and moral distress39. Moral uncertainty is a time when nurses are unsure which moral values apply or what the moral problem is; nurses feel dissatisfied with the patients' treatment. Moral dilemma describes a situation where two or more moral principles apply but they support mutually inconsistent courses of action. Moral distress describes a situation when nurses know the right thing to do but institutional constraints make it impossible to pursue the right action39. Moral distress occurred for the participants in this study when there were inadequate resources such as food, linen, dressings, beds and adequate staffing levels to provide a standard of care that aligned with the nurses' values.
The final stage, resigning, occurred because nurses felt a sense of giving up and hopelessness. Webster and Baylis describe this as moral residue and it is 'that which each of us carries with us from those times in our lives when in the face of moral distress we have seriously compromised ourselves or allowed ourselves to be compromised'40(p. 218). Moral residue can be deeply felt and is often very painful and lasting39,41. Moral residue has been reported in the USA and Canada as a contributor to decreased levels of job satisfaction and lower retention rates of nurses42-45. While Jameton39,41, Webster and Baylis40and Hardingham44 established that moral dilemmas, moral distress and moral residue are related to nurse resignation, this study extends this knowledge by identifying the stages within conflicting values in which these occur.
Limitations
There are some limitations to this study. The study collected data from a small sample of nurses who lived in rural and remote locations of one state of Australia, NSW, and the findings reflect the particular time and context in which the study took place; while the findings are not generalisable to a wider population, the findings may resonate with other nurses who have resigned. In addition, although all of the participants had resigned from their rural nursing positions due to a decrease in value alignment, this does not mean that all nurses who experience value misalignment resign. Nevertheless this study deliberately sought to understand, from the perspective of those who had recently resigned, why rural nurses resigned.
The process of generating a theory of rural nurse resignations, grounded in the data, has led to useful insights and knowledge relevant to the nursing profession. From this study, several findings arose that are significant. Rural nurses need to understand the importance of the degree of value alignment between themselves and the hospital in which they work. It is pertinent that rural nurses (in fact, all nurses) reflect and consider what values they hold, to what point they are willing to concede their values and how they can assist hospitals in helping nurses to sustain these values. Active self-reflection by rural nurses of their values and how they align with those of their organisations may assist rural nurses to identify the source of their job dissatisfaction. For those in senior management positions it is crucial that they have the skills to articulate and imbue the organisations' values, to be explicit in how these values accommodate nurses' values and to ensure that the values of their hospitals values (both explicit and implicit) are incorporated into the culture of the ward.
References
1. Health Workforce Australia. Health workforce 2025 - doctors, nurses and midwives. Volume 1. Health Workforce Australia, Adelaide, 2012.
2. Australian Nursing Federation. Submission to the Australian Government audit of the shortage of health professionals in rural and remote Australia. Australian Nursing Federation, Canberra, 2008.
3. Hegney D, McCarthy A, Rogers-Clark C, Gorman D. Why nurses are attracted to rural and remote practice. Australian Journal of Rural Health 2002; 10: 178-186.
4. Kenny A. Nursing shortages will cripple rural health care. (Online) 2009. Available: http://www.abc.net.au/news/stories/2009/02/02/2479976.htm (Accessed 4 Mary 2009).
5. Kenny A, Duckett S. Educating for rural nursing practice. Journal of Advanced Nursing 2003; 44(6): 613-622.
6. Mills J, Francis K, Bonner A. The problem of workforce for the social world of Australian rural nurses: a collective action frame analysis. Journal of Nursing Management 2007; 15(7): 721-730.
7. Pearson A. Claims, contradictions and country life in Australia: the evidence on rural nursing and midwifery. International Journal of Nursing Practice 2008; 14(6): 409-410.
8. Australian Institute of Health and Welfare. Nursing and midwife labour force 2005. National Health Labour Force Series no. 39 (Online) 2008. Available: http://www.aihw.gov.au/publications/hwl/nmlf05/nmlf05.pdf (Accessed November 2008).
9. Australian Institute of Health and Welfare. Nursing and midwifery labour force 2008. Bulletin no. 81., cat. no. AUS 130. AIHW, Canberra, 2010.
10. Health Workforce Australia. Health workforce 2025 - doctors, nurses and midwives. Volume 2. Health Workforce Australia, Adelaide, 2012.
11. Levett-Jones T, Fitzgerald M. A review of graduate nurse transition programs in Australia. Australian Journal of Advanced Nursing 2005; 23(2): 40-45.
12. Australian Nursing Federation. Make health an election priority. (Online) 2013. Available: http://www.nswnurses.asn.au/news/45875.html (Accessed 22 April 2013).
13. Duffield C, Roche M, O'Brien-Pallas L, Diers D, Aisbett C, King M, et al. Glueing it together: nurses, their work environment and patient safety. University of Technology, Sydney, 2007.
14. Graham E, Duffield C. An ageing nursing workforce. Australian Health Review 2010; 34: 44-48.
15. NSW Nurses' Association. Industrial relations policy and the NSW nurse shortage. A report by the NSW Nurses' Association. NSW Nurses' Association, 2007.
16. Australian Institute of Health and Welfare. Nursing and midwifery workforce 2011. AIHW, Canberra, 2012.
17. NSW Health. Local health districts - nursing positions being actively recruited. (Online) 2012. Available: http://www0.health.nsw.gov.au/nursing/employment/dohrs.asp (Accessed 11 April 2013).
18. Hegney D, Plank A, Buikstra E, Parker V, Eley R. Nurses worth listening to. Project report. University of Southern Queensland, Toowoomba, 2005.
19. Francis K, Mills J. Sustaining and growing the rural nursing and midwifery workforce: understanding the issues and isolating directions for the future. Collegian 2011; 18(2): 55-60.
20. Daly J, Speedy S, Jackson D (eds). Contexts of nursing in Australia, 3rd edn. Churchill Livingstone, Sydney, 2010.
21. Drury V, Francis K, Dulhunty G. The lived experience of rural mental health nurses. Online Journal of Rural Nursing and Health Care 2005; 5(1), 1-14.
22. Glaser B. Basics of grounded theory analysis. Sociology Press, Mill Valley, California, 1992.
23. Glaser B. Theoretical sensitivity. Sociology Press, California, 1978.
24. Glaser B. Naturalist inquiry and grounded theory. Forum: Qualitative Social Research 2004; 5(1).
25. Locke E. The nature and causes of job satisfaction. In M Dunnette (ed.) Handbook of Industrial and Organizational Psychology. Rand McNally, Chicago, 1976; 1297-1349.
26. Gullate M, Jirasakhiren E. Retention and recruitment: reversing the order. Clinical Journal of Oncology Nursing 2005; 9(5): 597-604.
27. Horton K, Tschudin V, Forget A. The value of nursing: a literature review. Nursing Ethics 2007; 14(6): 716-740.
28. Leiter M, Jackson N, Shaugnessy K. Contrasting burnout, turnover intention, control, value congruence and knowledge sharing between Baby Boomers and Generation X. Journal of Nursing Management 2009; 17: 100-109.
29. Tourangeau A, Cranley L. Nurse intention to remain employed: understanding and strengthening determinants. Journal of Advanced Nursing 2006; 55(4): 497-509.
30. Garling P. Acute care services in NSW public hospitals. Final report of the Special Commission of Inquiry. Sydney, 2008.
31. Weymouth S, Davey C, Wright J, Nieuwoudt L, Barclay L, Belton S, et al. What are the effects of distance management of the retention of remote nurses in Australia? Rural and Remote Health 7: 652 (Online) 2007. Available: www.rrh.org.au (Accessed March 2008).
32. NSW Health. National health reform. (Online) 2010 Available: http://www.health.nsw.gov.au/initiatives/healthreform/index.asp (Accessed 29 September 2010).
33. Duffield C, Roche M, Diers D, Catling-Paul C, Blay N. Staff, skill mix and the model of care. Journal of Clinical Nursing 2010; 19(15-16): 2242-2251.
34. Brown P, Fraser K, Wong C, Muise M, Cummings G. Factors influencing intentions to stay and retention of nurse managers: a systematic review. Journal of Nursing Management 2012; 21(3), 459-472.
35. Buffington A, Zwink J, Fink R, DeVine D, Sanders C. Factors affecting nurse retention at an academic magnet hospital. The Journal of Nursing Administration 2012; 42(5), 273-281.
36. Park S, Kim T. Do types of organizational culture matter in nurse job satisfaction and turnover intention? Leadership in Health Services 2009; 22(1): 20-38.
37. Shermont H, Krepcio D. The impact of culture change on nurse retention. The Journal of Nursing Administration 2006; 36(9): 407-415.
38. Davies H, Nutley S, Mannion R. Organisational culture and quality of health care. Qualitative Health Care 2000; 9: 111-119.
39. Jameton A. Nursing practice and ethical issues. Prentice-Hall, New Jersey, 1984.
40. Webster G, Baylis F. Moral residue. In: S Rubin, L Zoloth (eds). Margin of error: the ethics of mistakes in the practice of medicine. University Publishing Group, Hagerstown, MD, 2000.
41. Jameton A. Dilemmas of moral distress: moral responsibility and nursing practice. Perinatal Women's Health Nurse 1993; 4: 542-551.
42. Erlen J. Wanted-nurses: ethical issues and the nursing shortage. Orthopaedic Nursing 2004; 23(4): 289-292.
43. Elpern E, Covert B, Kleinpell R. Moral distress of staff nurses in a medical intensive care unit. American Journal of Critical Care 2005; 14(6): 523-530.
44. Hardingham L. Integrity and moral residue: nurses as participants in a moral community. Nursing Philosophy 2004;5.
45. Pendry P. Moral distress: recognizing it to retain nurses. Nursing Economics 2007; 25(4): 217-221.

