full article:
Aboriginal people experience poorer health compared to non-Aboriginal people in Australia. The burden of disease in Australian Indigenous people is two and a half times greater than that of the total Australian population1. In all age groups Aboriginal people experience higher mortality and morbidity1 and for the period of 2005-2007 the gap in life expectancy between Aboriginal and non-Aboriginal males and females was 11.5 and 9.7 years respectively2. The rates of chronic, non-communicable diseases are higher among Aboriginal Australians3, with endocrine, metabolic and nutritional disorders contributing to the mortality of Aboriginal people at six to seven times the rate of that for non-Aboriginal Australians2.
Australian Aboriginal people have experienced significant historical and political marginalisation resulting in intergenerational discriminatory practices (intentional and unintentional), which have a profound effect on health and wellbeing4. Other factors include socioeconomic marginalisation and negative assumptions about Aboriginal peoples that can limit access to appropriate housing, transport, jobs and healthcare services2. These combined factors contribute to the unacceptably large health gap for disease and injury1,5. This is a complex issue that requires action at all levels in government and non-government organisations.
There is an immediate need for health and medical professionals to work with Aboriginal people to close the health gap, and evidence has demonstrated that employment of Indigenous staff and Indigenous leadership within a health service increases the access of the health service to Indigenous people6. However, relatively few Aboriginal professionals are employed in the Australian health system, particularly at an executive management level, and even fewer in specialised fields. As the majority of Indigenous people access health provision through mainstream services, Indigenous people need to feel comfortable accessing these services if Aboriginal health is to improve6. Therefore it is vital that in addition to building the health workforce participation of Aboriginal people, the capability of the non-Aboriginal health workforce is also strengthened, in order to contribute to better prevention and management of chronic health conditions and close the gap in Aboriginal health. It has previously been reported that a well-trained health workforce will help to secure and sustain health improvements for Aboriginal communities7. Therefore, it is imperative to consider how the majority of non-Aboriginal health professionals in Australia can develop confidence and skills to work effectively with Aboriginal people.
There is a body of literature incorporating strategies that non-Aboriginal health professionals can use to work well in Aboriginal health. For example, working in partnership with Aboriginal people has been stressed by multiple authors8-14, and the need for flexibility15. Valuing and incorporating Aboriginal expertise has been previously cited as a beneficial strategy8,13 and relationship building is described as fundamental8,15. Social, cultural and structural factors have also been found to influence care provided to Aboriginal people, with strategies like reciprocity and respect facilitating better care16.
However, health professionals may not have the confidence to use these strategies, are not necessarily at the same stage in their learning about the complexity of Aboriginal health and do not necessarily have the same beliefs and understandings, all of which will influence how they implement the strategies suggested. There is limited literature presenting the positive experiences and attitudes and characteristics of health professionals working in the field of Aboriginal health. Such investigations are important if suitable strategies to support health professionals are to be developed. The purpose of this study was to talk with non-Aboriginal health professionals about their experiences (inclusive of their assumptions beliefs, confidence and fears) working in Aboriginal health. This research arose from the practice dilemmas and challenges encountered by one of the authors (AW) working as a new graduate dietitian with Aboriginal communities in 2007 and 2008.
Terminology
This article uses the term 'Aboriginal', preferred by the Indigenous peoples from the areas where this research was conducted, South Australia. Some of the same issues are likely to apply to Torres Strait Islander people, and this usage is not intended to exclude them. The word 'Indigenous' is used only when part of a direct quote or used by another author.
Researcher standpoint
The primary researcher (AW) identifies as a white person, dietitian and researcher who has worked with Aboriginal communities. In undertaking this research, AW worked alongside Aboriginal people in two communities and the research was strongly guided by her learnings from working in partnership with these communities.
Theoretical framework
The study used a social constructionist epistemology17,18, underpinned by the belief that reality is experienced, or constructed, by the individual19. This approach guides against privileging one type of knowledge over another. A critical theoretical approach was utilised to identify and discuss oppressive structures in health care and society20,21 and critical social research22 and reflexivity23 were the methodological approaches that guided the study. The theoretical framework informed the data collection and analysis; for example, participants' experiences and reflections, rather than a definitive answer, were sought through interview questions.
Sample
The research was set within a larger healthy eating and physical activity program (the Eat Well Be Active community programs) delivered in one rural and one metropolitan community in South Australia from 2005 to 2010. Further details about the communities have been reported elsewhere24-27. Non-Aboriginal staff working in the health services where the program was delivered, and who had some experience or an interest working in Aboriginal health, were invited to participate in a semi-structured interview. This invitation included dietitians, occupational therapists, health promotion workers and speech pathologists. Recruitment was face to face where possible and otherwise through email. Dietitians working in various organisations across South Australia were also invited to participate in an interview, to enable a broader representation of dietetics (the professional background of the primary researcher, AW). They were recruited at a state nutrition meeting and through an email flyer. Consistent with the theoretical framework of this study, sampling was by convenience and participants were selected purposively based on their experience or interest in working in Aboriginal health. Purposive sampling ensures participants have relevant experiences to contribute28 and are information rich based on these experiences29. A total of 35 non-Aboriginal health professionals were recruited to the study. Thirty one were female and four were male; 22 were from a rural location.
Data collection
Data was collected through semi-structured interviews, enabling in-depth exploration of the topic and potentially sensitive questions to be explored in a one-to-one discussion. Questions were focused on health professionals' perceptions and experiences of working in Aboriginal health, including their feelings of confidence or unease. Examples of questions from the interview schedule have been included (Fig1). It was developed from the researcher's perspective as a non-Aboriginal health professional working as a dietitian and modified following discussion with individual Aboriginal project mentors and supervisors. The length of interviews varied from 20 to 90 minutes and they were undertaken by the first author (AW), who met participants at locations and times suggested by them. Interviews were recorded using a digital voice recorder, and written, informed consent was obtained before each interview.

Figure 1: Sample questions from interviews with non-Aboriginal health professionals.
Data analysis
Interviews were transcribed and transcripts were de-identified and imported into QSR NVivo v8.0 software (QSR International; http:www.qsrinternational.com). Participants were provided the option to review their transcript and make any changes. Critical social research22 was used to guide emergence and evolution of themes. Data were coded into themes that recurred throughout the interview. Further analysis of themes was guided by the process of deconstruction and reconstruction22. This process enables the researcher to expose the data by breaking it down into its individual elements (that is, attitudes and characteristics of participants) and then put it back together in a different way to expose deeper meaning (for example by grouping individuals with similar attitudes and characteristics) and this process led to development of the groupings. Interview analysis was conducted by one researcher (AW) and guided by supervisors with professional knowledge and experiences in the field. The researcher used a critical reflexive journal to assess and reflect on her own attitudes and potential biases throughout the study23.
Testing at two workshops
The wider relevance of this research was tested soon after development. This was preliminary testing only and further work is required. The groupings were presented at two workshops in South Australia, one of which was a national conference. At these workshops, participants were encouraged to self-reflect and to choose the group they currently most identified with. This was followed by discussions about difficulties in each group, and how participants could move forward to address any challenges.
Ethics approval
Ethics approval was granted by the Flinders University of South Australia Social and Behavioural Research Ethics Committee (4455), the South Australian Aboriginal Health Research Ethics Committee (04-09-285) and the ethics committees of SA Health (293/05/2012) and the Department of Education and Children's Services (CS/06/0116-2.7).
The length of time participants had worked in Aboriginal health varied and included 0-1 year (n=8), 1-5 years (n=13), 5-15 years (n=7) and more than 15 years (n=7).
The experiences of interviewees were classified broadly into four stages along a continuum, with health professionals in the same area of the continuum displaying similar attitudes and characteristics. These groupings are called 'don't know how', 'too scared', 'too hard' and 'barrier breakers' (Fig2). 'Barrier breakers' was further divided into two stages, reflecting the different levels of awareness of cultural identity between these two groups. The experiences of health professionals are presented as a continuum because it was possible for health professionals to show characteristics of more than one group and therefore be between groupings; additionally, it is likely that individuals could move back and forth between groups. Workers who discussed similar experiences and demonstrated similar attitudes and characteristics were grouped based on analysis of quotes from interviews. It was possible for health professionals to show attitudes and characteristics of more than one group, for example if they reflected on a new situation they had been in where they felt less confident, or when they reflected on their past experience working in Aboriginal health, when they may have identified with a different group. This was reiterated by participants at the workshops who said that they might move between the groups if they experience new situations or new locations. The groupings do not appear to be completely distinct, with some groups having similar characteristics (for example discussion of cultural identity). However, what sets each group apart is attitude towards practice in Aboriginal health. The number of non-Aboriginal health professionals displaying attitudes related to each group is presented in Table 1.
No differences were observed between male and female participants or those from a rural or metropolitan location. Participants who had worked in Aboriginal health for longer were more likely to be 'barrier breakers'. For example, all 'barrier breakers' in stage 2 had 15 years or more experience. Ten of eleven 'barrier breakers' in stage 1 had 5-15 years or more than 15 years experience. The other stages did not appear to be related to length of time worked, but rather to exposure and experience to Aboriginal health. For example, two dietitians in the 'don't know how' group had between 5 and 15 years practice experience but had very rarely worked with Aboriginal people in their jobs.
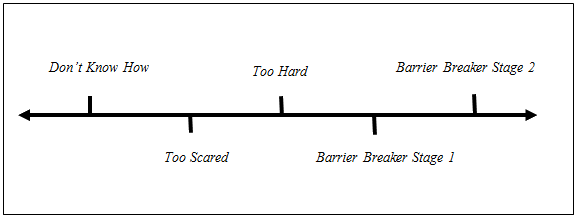
Figure 2: Continuum of practice of non-Aboriginal health professionals working in Aboriginal health.
Table 1: Number of non-Aboriginal health professionals in the four groups:
'don't know how', 'too scared', 'too hard' and 'barrier breaker' (stages 1 and 2) (n=35)

Four attitudes of non-Aboriginal workers
'Don't know how': Health professionals in this group discussed not knowing how to work in Aboriginal health and lacking strategies to do so. One dietitian said that, previously, she hadn't known where to start:
... before I started work with Aboriginal Communities I was kind of like 'geez how am I going to do this? Like, I know nothing basically'... I went in feeling like I [knew] nothing ... (health professional 4)
The effect of not knowing how was a sense of paralysis and an uncertainty about how to proceed:
I just don't see Aboriginal people within the township of [town] ... I just don't know where they are ... I am at a loss to know what could improve or help because I can't see the group and I'm not sure whether I need someone to come along and say 'okay, [name], let's go and meet the Aboriginal Community', I just don't know what could help. (health professional 31)
One worker reflected on being in the 'don't know how' group and how they were able to move along the continuum through informal mentoring:
I have been quite open that I didn't have as much experience, I have been quite open that I haven't known a lot, I was quite vocal about that with management at [organisation] and that's why I was able to sort of be sort of informally mentored. (health professional 12)
'Too scared': Those in this group were fearful about working in Aboriginal health. This fear was in two main areas - fear of being racist and fear of getting things wrong, including doing or saying the wrong thing or making assumptions. This fear was a barrier to practice; for example:
I come into it with this background fear, you know I'm in a place now where I really want to engage and I really want to be involved and start doing things and it has been a little bit like two steps forward and one step back and you know, you do something and then all of a sudden you think 'oh, I did that wrong, I don't know what it was, I feel like we can't discuss it, I'll go away for a while until the next window of opportunity comes up and then I'll have another go'. So I think with me personally there's this underlying fear of I'm gonna do something wrong. (health professional 17)
Some of the things that led to this apprehension included past experience, described here by one participant:
I grew up, and can tell a personal story, in Darwin [Northern Territory], and in walking to school I would walk past members of the Aboriginal community who were inebriated and would ask me for money and harass me if I didn't have it and I was fearful. As an adult, more recently I experienced a group of Aboriginal people in Coober Pedy [remote community in South Australia] and I was fearful again. Even all the thinking that I've done, I can still flip into feeling frightened and then the kind of shame that went along with that, how easy it is to feel unsafe in relationships and how vulnerable we are as people. (health professional 29)
'Too hard': Non-Aboriginal health professionals in this group had worked in Aboriginal health for longer than the 'don't know how' or 'too scared' groups and their awareness of barriers to practice increased over this time. External barriers and challenges discussed were identification of Aboriginal people to work with and wider determinants having an impact on health behaviours (eg healthy eating) that health professionals did not feel they could address (eg low income). Health professionals described in detail their understanding of the barriers many Aboriginal families experience in terms of prioritising healthy eating and said it was the presence of these barriers, rather than their practice as health professionals, that made it hard for Aboriginal people to be healthy. For example:
A lot of Aboriginal populations are living in quite low socio-economic and quite bad conditions ... it could be quite difficult when people have got all these other things that seem like much higher priorities, so more immediate concerns like 'we don't have enough money to pay the bills' and those types of things mean that nutrition can sort of seem like something that can go on a back burner. (health professional 5)
Whether because of not knowing how, fear of being racist or getting things wrong or the presence of external barriers, health professionals in the 'don't know how', 'too scared' and 'too hard' groups were not able to work very much in Aboriginal health, without uncertainty and discomfort. An example of the effect of this was given:
I think that people mightn't necessarily initiate work in this area. If there is a program that is pre-existing they will do it but they might not initiate or lead into that area even though there are major needs there. (health professional 23)
'Barrier breaker' (stages 1 and 2): In contrast, 'barrier breakers' were aware of the many challenges of working in Aboriginal health but continued to work in the area regardless. One worker said:
If something doesn't work then you find another way to make it happen. If something wasn't going to work or isn't working then you wouldn't just walk away. (health professional 6)
Health professionals in this group were aware of not only external barriers, for example the socioeconomic barriers described by those in the 'too hard' group, but also personal factors that may influence their practice, for example their attitudes and beliefs about Aboriginal people. 'Barrier breakers' in stage 2 understood the importance of making clients feel comfortable in their presence (particularly Aboriginal people) by stating upfront who they are, where they come from and providing some information about their families to develop a connection as a place to begin conversation. One participant described how she did this:
I have changed some things in my own practice. When I introduce myself to Aboriginal families and Community I introduce myself as a woman who comes from the [region] and who is the mother of two children so I kind of talk about the things that I do really value about myself rather than going into the Speech Pathologist der-da-der. (health professional 29)
Characteristics of workers in the four groups: Participants across the four groups consistently discussed particular issues related to their work in Aboriginal health. These included participants' willingness to work in Aboriginal health, practice and experience in Aboriginal health, awareness of Aboriginal history and awareness of cultural identity. The depth in which participants discussed these issues varied and contributed to their placement in the different groups (Fig3).
Figure 3 demonstrates that workers in all of the groups were willing to begin working in Aboriginal health; one participant (health professional 10) stated 'most dietitians go in, or they start work with the understanding that the Indigenous population is a high priority area and they all want to work there'. The focus on external barriers they felt they could not control made working in this area less appealing for those in the 'too hard' stage. Hence they were slightly less willing to work in Aboriginal health.
Of workers in all of the groups, 'barrier breakers' were most likely to share their practice experiences of working in Aboriginal health during their interview (Fig3). They had the most practice experiences, had generally worked in Aboriginal health for the longest, did not perceive a 'right' or 'wrong' way to work in Aboriginal health and were at a stage where they were able to work with Aboriginal people more freely, without fear or feeling constrained by barriers.
Awareness of the impact and importance of Aboriginal history and colonisation of Australia increased across the groups (Fig3). Those in the 'don't know how' and 'too scared' groups did not know enough about Aboriginal history for it to affect their work.
In contrast, those in the 'too hard' and 'barrier breaker' groups had a reasonable understanding of past and current discriminatory practices and social inequalities facing Aboriginal Australians. Unlike 'barrier breakers', those in the 'too hard' group had not yet developed strategies to deal with knowledge of this history and the guilt associated with awareness of atrocities to Aboriginal peoples was immobilising, for example:
... because you're sorry. There's nothing I personally can do about it and then it is heaps difficult because [you think] 'well what can I do about this'? .... it is hard not to feel bad, it really is. (health professional 4)
An awareness of one's own cultural identity and the impact of it on the healthcare encounter was only discussed by 'barrier breakers' in stage 2. For example, one participant described her cultural identity, and how an awareness of this guided her around actions that were and were not appropriate:
I see myself as of the dominant culture, I'm English, I'm a migrant and have been a migrant twice to this country and I'm White ... there are things that [Aboriginal Health Worker] can do that I simply couldn't do. I'm not Aboriginal and it is not appropriate for me to try and do some of those things. (health professional 22)
The capacity to recognise the importance of one's identity in working relationships, and hence reach the phase of 'barrier breaker' stage 2, came from a realisation that one's identity impacts on the care that is provided. To do so, the individual had to engage in high levels of self-reflection about themselves. This was a skill uniquely observed in the barrier breakers stage 2. For example:
I suppose I've also learnt a lot about what it means to be White and a comfortable middle class White girl and have explored more what I bring. (health professional 29)
For this participant, realisation also came through working with Aboriginal people, and seeing the daily struggles faced:
... probably for me the understanding of my own Whiteness has been part of that journey as well, so that thing about being a Whitefella and being part of a dominant culture and what that means because I think most White people would never have to think about who they are in their own community because they just are, so they never have to struggle with the same sort of issues that Aboriginal people have to, such as whether I'll be accepted here or whether I'll be judged or looked down on there. (health professional 9)
In contrast, health professionals in the 'too scared' and 'too hard' groups reflected less on cultural identity issues within the client-health provider relationship and more on the role of racism generally. For example, those in the 'too scared' group were aware of racism in society and were fearful of unknowingly perpetuating this:
I didn't care if I spent all my time talking to my clients about the weather ... of course I feel differently now but [before] I wasn't so outcomes and relationship focussed. I hoped people thought I wasn't being racist, (whispered) that was what I was so scared of. (health professional 4)
Being aware of their cultural identity and the importance of this in the healthcare encounter enabled 'barrier breakers' to be content in not always knowing the personal details of a client's situation. For example:
... there are often a lot of things happening that are not appropriate for me to know about ... (health professional 22)
This was in contrast to health professionals in other groups, who displayed distress during interviews when they did not understand why Aboriginal people chose not to engage with them:
I tried to get to the Elders as well and made contact with [name] who was involved with it at that time and I had to put a proposal of what I wanted to chat to them about to her and I had to keep chasing and chasing her and eventually she said oh, they're not interested. (health professional 1)
Similarly, 'barrier breakers' were more likely to recognise the importance of understanding and responding to cultural differences regarding the goal of equity as a significant means towards implementing the principle of equal treatment within the healthcare encounter:
I heard someone say recently how tiring it is not to have your difference known and that really stuck in my mind as part of what respect is. It is actually knowing that you're different, we are all different, each one of us is different, but not to have your difference known and recognised and respected is a difficult thing. So, to actually acknowledge where someone is, somebody's identity and actually acknowledging that, and respecting that and being mindful of that ... so it is not when you are working with people, it is not always about seeing only that facet of it, but it is also about respecting who they are. (health professional 22)
Therefore 'barrier breakers' in stage 2 identified the importance of having a useful reaction to difference; that is, 'acknowledging that difference but not prefacing everything you do and say by acknowledging that difference' (health professional 22).
This is in contrast to workers in the 'don't know how' group who consistently commented how they treated everyone the same, in order to address concerns that Aboriginal people are offered 'special treatment', for example:
... you can't treat anyone differently, you've just got to treat them as you would anyone else. (health professional 15)
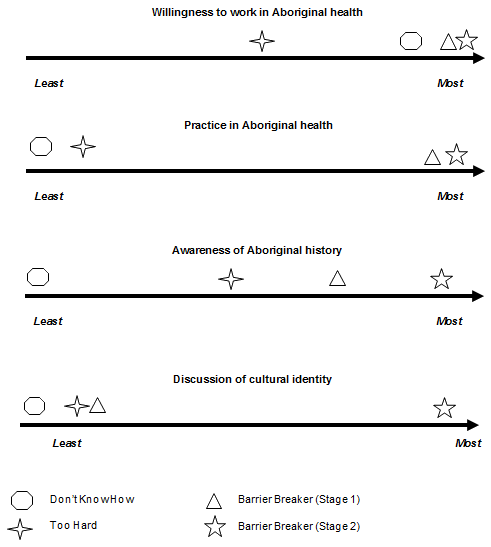
Figure 3: Characteristics of workers across the continuum of practice
('don't know how', 'too scared', 'too hard' and 'barrier breakers' stage 1 and 2).
Discussion
This article reports on attitudes and experiences of some non-Aboriginal health professionals working in Aboriginal health in South Australia. Four groupings of health professionals working in Aboriginal health have been presented. It is envisaged that these groupings can be used by non-Aboriginal health professionals to think about where they might fit in terms of their own attitudes and characteristics related to working in Aboriginal health and ultimately reflect critically on and adjust their practice.
The attitudes and characteristics of workers in the four groups have been discussed in the literature. For example, it was found that while there is a mandate for occupational therapists to work in Aboriginal health, there is little guidance about how to do this15. Similarly, fear about working in Aboriginal health has been identified in non-Aboriginal people working in other professions, such as social work8, mirroring the concerns of the 'too scared' group. The role of guilt in the responses of non-Aboriginal people to Aboriginal people has been explored elsewhere, with an acknowledgement that attitudes towards Indigenous people can be influenced by feelings of guilt30, and the potential for guilt to be a stimulus for non-Aboriginal people to find out more about Aboriginal people31. The quote from health professional 15 about treating everyone the same demonstrates difference blindness, which means that health professionals 'treat all patients the same, regardless of age, gender, ethnicity or religious belief'16. Difference blindness has been identified in other non-Aboriginal health professionals when speaking about their experiences working in Aboriginal health16. The focus on external barriers exhibited by those in the 'too hard' group has also been reported elsewhere; participants in a workshop about race and culture were more likely to attribute Indigenous ill health to structural factors than to consider the agency of Indigenous people32. This is the first study to identify these characteristics consistently across a group of health professionals and present a conceptual model summarising their experiences.
The importance of understanding one's own cultural background and its impact on health care has also been found in other studies33 and is consistent with a cultural safety approach. Health care is culturally safe if perceived by the recipient of the care to be so34. Cultural safety is underpinned by the process of identity formation and principles including self-reflection and patient-centred care34. It recognises the power imbalance inherent in the healthcare interaction34. Consequently this approach requires health professionals to reflect on their own identity, culture, position, values, attitudes, experiences and practices that inform the way that they exist in the world, rather than learn about the 'other'8,35-38. Cultural safety acknowledges that improving equitable access to health care is 'not just a matter of what members of the dominant culture do with 'others' but what they should do with 'themselves''39. Learning about the 'other' needs to be 'preceded and continuously accompanied by ongoing critical reflection undertaken by students and professionals on their own cultures and own practices'39. By considering their own cultural identity, and its impact on the healthcare encounter, 'barrier breakers' in stage 2 demonstrated a culturally safe approach. Hence an important question is how can more health professionals be supported to reach the same point as 'barrier breakers' (stage 2)? An awareness of cultural identity and its impact on the healthcare encounter defined 'barrier breakers' in stage 2, suggesting that it is pertinent that all health professionals are trained in and operate from a cultural safety approach is pertinent. A more culturally safe workforce will have better engagement with Aboriginal individuals, communities and families which will contribute to better approaches to management and prevention of chronic health conditions for Aboriginal people and hence is relevant to health service delivery. Despite this, there is currently a lack of programs in the published literature underpinned by a cultural safety approach40. Hence a tool such as the one presented in this article is useful to facilitate health professionals to start shifting the lens back upon themselves, consistent with a cultural safety approach.
The research identified characteristics that assist non-Aboriginal health professionals to practise in Aboriginal health and these include an awareness of cultural identity, reflection on one's own position and an awareness of Aboriginal history. Therefore health professionals looking to develop skills in Aboriginal health could focus on development of these characteristics as a form of professional development. They could also be a focus of training and education at university level. This is also relevant to health service delivery; for example, individual reflection on values and beliefs and how they inform practice can enable health professionals to think about whether their own beliefs and practices promote or compromise the health of Aboriginal people41. Furthermore, the fact that some of the stages were related to exposure and experience to Aboriginal health, rather than to length of time worked, suggests that exposure to Aboriginal health - including working with Aboriginal people - is important for all health professionals. Exposure to Aboriginal health issues at university level could assist in preparation for this.
It is of interest to consider why health professionals displayed the attitudes and characteristics discussed. The characteristics of the 'too scared' and 'too hard' groups suggest that teaching health professionals and students a little bit about Aboriginal health, history and colonisation, without follow-up support or discussion about strategies to deal with an awareness of these issues, can in itself be immobilising. The fact that most health professionals were willing to work in Aboriginal health suggests that non-Aboriginal health professionals may not require a lot of encouragement to work in Aboriginal health; however, the challenges faced when exposed to the area suggest that health professionals require encouragement and support once they get there. This is supported by other literature; for example, support networks have been identified as one factor that contributes to dietitians' decisions to begin and continue working in rural and remote locations42, and it is recognised that one of the challenges that health professionals face when working in rural and remote areas is a higher proportion of Indigenous clients43. Additionally, training health professionals in cultural safety would provide them with greater skills in critical reflection, which could help them to work through issues related to colonisation, history and determinants of health for Aboriginal people and identification of their own attitudes and values. Another option is mentoring in the workplace, as a form of professional development and/or education and training, in particular mentoring from people in 'barrier breaker' stages, which could assist those in earlier groups with strategies but also assist 'barrier breakers' to keep progressing and continue reflecting on their own work.
The groupings were well received when used at the workshops, suggesting the model is likely to be relevant to dietitians and other health professionals beyond the study sample. It may also be used by individual health professionals as a basis for self-reflection, in the context of building relationships with Aboriginal people to improve their practice or in workshops to facilitate group discussions as previously demonstrated. The groupings also have the potential to be used by Aboriginal people who work with non-Aboriginal people. For example, an Aboriginal mentor for this research reflected that the model could assist her to initially place a non-Aboriginal person's reaction or comment in the context of these groupings, rather than attribute comments immediately to racism (K. O'Donnell 2011, pers. comm., 11 November).
Limitations of the research must also be considered. The majority of health professionals interviewed were White Australians (meaning they 'participate in the racialised societal structure that positions them as 'White' and accordingly grants them the privileges associated with the dominant Australian culture'44); an avenue for future research would be to explore whether the characteristics, experiences and confidence level of non-Aboriginal and non-White health professionals working in Aboriginal health is similar or different. Most of the groups are focused on what is difficult about working in Aboriginal health, therefore some further investigation into what is positive in each group would also be warranted. The data were collected by one person only and demographic details about participants were not collected (other than gender and length of time working in Aboriginal health).
The findings of this study suggest that the attitudes and characteristics of non-Aboriginal health professionals working in Aboriginal health vary and can be considered across a range of groups. By encouraging self-reflection about where a health professional's experiences, characteristics and confidence lie, the groups can be used to encourage non-Aboriginal health professionals, rather than Aboriginal clients or workers, to be the focus for change. This complements a cultural safety approach to cultural training where health professionals are required to assess their own identity and values. It provides a non-confronting way through which all health professionals can begin discussions about working together in Aboriginal health.
Acknowledgements
Annabelle Wilson would like to acknowledge Luita Casey, Mark Thompson and Kim O'Donnell for their mentorship during the PhD research that informed this paper. The researchers would also like to acknowledge all of the research participants, in particular the Aboriginal people in the project communities who contributed.
Annabelle Wilson was supported by a scholarship from SA Health in 2008 and an Australian Postgraduate Award and 'top-up' scholarship from SA Health from 2009 to 2011. The Eat Well Be Active Community Programs were funded by the Government of South Australia, SA Health and implemented by Southern Primary Health, of Southern Adelaide Health Service, and Murray Mallee Community Health, of Country Health SA.
References
1. Vos T, Barker B, Stanley L, Lopez A. The burden of disease and injury in Aboriginal and Torres Strait Islander peoples: summary report. Brisbane, Qld: School of Population Health, The University of Queensland, 2007.
2. Australian Institute of Health and Welfare. The health and welfare of Australia's Aboriginal and Torres Strait Islander people: an overview. Canberra, ACT: Australian Government, 2011.
3. Australian Bureau of Statistics. The health and welfare of Australia's Aboriginal and Torres Strait Islander peoples. Canberra, ACT: ABS, 2010.
4. Eckermann A, Dowd T, Chong E, Nixon L, Gray R, Johnson S. Binan Goonj: bridging cultures in Aboriginal health. Sydney, NSW: Churchill Livingstone, 2006.
5. Helps Y, Moller J, Kowanko I, Harrison JE, O'Donnell K, de Crespigny C. Aboriginal people travelling well: issues of safety, transport and health. Canberra, ACT: Department of Infrastructure, Transport, Regional Development and Local Government, 2008.
6. Hayman N, White NE, Spurling GK. Improving Indigenous patients' access to mainstream health services: the Inala experience. Medical Journal of Australia 2009; 190(10): 604-606.
7. Anderson C. Indigenous footprints on health curriculum. The Australian Journal of Indigenous Education 2009; 38(Supplement ): 40-45.
8. Bennett B, Zubrzycki J, Bacon V. What do we know? the experiences of social workers working alongside Aboriginal people. Australian Social Work 2009; 64(1): 20-37.
9. Blackman R. Knowledge for practice: challenges in culturally safe nursing practice. Contemporary Nurse 2009; 32(1-2): 211-214.
10. Macaulay AC. Improving Aboriginal health. Canadian Family Physician 2009; 55(4): 334-336.
11. Stedman A, Thomas Y. Reflecting on our effectiveness: Occupational therapy interventions with Indigenous clients. Australian Occupational Therapy Journal 2011; 58(1): 43-49.
12. Watts E, Carlson G. Practical strategies for working with Indigenous people living in Queensland, Australia. Occupational Therapy International 2002; 9(4): 277-293.
13. Smith D. Rethinking nursing best practices with Aboriginal communities: Informing dialogue and action. Nursing Leadership 2010; 22(4): 24-39.
14. Read C. Working with an Aboriginal Community Liaison Worker. Rural and Remote Health 6: 1-9. (Online). 2006. Available: www.rrh.org.au (Accessed 25 March 2015).
15. Thomas Y, Gray M, McGinty S. Occupational therapy at the 'cultural interface': lessons from research with Aboriginal and Torres Strait Islander Australians. Australian Occupational Therapy Journal 2011; 58(1): 11-16.
16. McBain-Rigg K, Veitch C. Cultural barriers to health care for Aboriginal and Torres Strait Islanders in Mt Isa. Australian Journal of Rural Health 2011; 19: 70-74.
17. Berger P, Luckmann T. The social construction of reality - a treatise in the sociology of knowledge. London: Penguin Books, 1966.
18. Gergen K. The social constructionist movement in modern psychology. American Psychologist 1985; 40(3): 266-275.
19. Schwandt TA. Constructivist, interpretivist approaches to human inquiry. In N Denzin, Y Lincoln (Eds). Handbook of qualitative research. Thousand Oaks: Sage Publications, 1994; 118-137.
20. Haralambos M, Holborn M, Health R. Sociology themes and perspectives. London: Collins, 2004.
21. Neuman WL. Social research methods qualitative and quantitative approaches. Needham Heights: Allyn & Bacon, 2000.
22. Harvey L. Critical social research. Sydney: Unwin Hyman Ltd, 1990.
23. Etherington K. Becoming a reflexive researcher: using our selves in research. London: Jessica Kingsley Publishers, 2004.
24. Magarey A, Pettman T, Wilson A, Mastersson N. Changes in primary school student's behaviour, knowledge, attitudes and environments related to nutrition and physical activity. ISRN Obesity 19 March 2013, 752081.
25. Pettman T, Magarey A, Mastersson N, Wilson A, Dollman J. Improving weight status in childhood: results from the eat well be active community programs. International Journal of Public Health 2014; 59(1): 43-50.
26. Wilson A, Jones M, Kelly J, Magarey A. Community-based obesity prevention initiatives in Aboriginal communities: the experience of the eat well be active community programs in South Australia. Health 2012; 4: 1500-1508.
27. Wilson A, Magarey A, Dollman J, Jones M, Mastersson N. The challenges of quantitative evaluation of a multi-setting, multi-strategy community based childhood obesity prevention program: lessons learnt from the eat well be active community programs in South Australia. Public Health Nutrition 2009; 13(8): 1262-1270.
28. Popay J, Rogers A, Williams G. Rationale and standards for the systematic review of qualitative literature in health services research. Qualitative Health Research 1998; 8: 341-351.
29. Patton M. Qualitative research and evaluation methods. Thousand Oaks: Sage Publications, 2002.
30. Pedersen A, Beven J, Walker I, Griffiths B. Attitudes towards Indigenous Australians: the role of empathy and guilt. Journal of Community and Applied Social Psychology 2004; 14: 233-249.
31. Selby J. Working divides between indigenous and non-indigenous: disruptions of identity. International Journal of Qualitative Studies in Education 2004; 17(1): 143-156.
32. Kowal E, Paradies Y. Ambivalent helpers and unhealthy choices: public health practitioners' narratives of Indigenous ill-health. Social Science and Medicine 2005; 60: 1347-1357.
33. Cunningham J, Wollin J. The importance of clinical experience in Aboriginal communities. Contemporary Nurse 1997; 7: 152-155.
34. Taylor K, Guerin P. Health care and Indigenous Australians: cultural safety in practice. South Yarra: Palgrave Macmillan, 2010.
35. Foster CH. What nurses should know when working in Aboriginal communities. The Canadian Nurse 2006; 102: 28.
36. Nguyen HT. Patient centred care: cultural safety in Indigenous health. Australian Family Physician 2008; 37: 990-994.
37. Pyett P, Waples-Crowe P, van der Sterren A. Challenging our own practices in Indigenous health promotion and research. Health Promotion Journal of Australia 2008; 19: 179-183.
38. Williams R. Cultural safety - what does it mean for our work practice? Australian and New Zealand Journal of Public Health 1999; 23: 213.
39. Ryder C, Yarnold C, Prideaux D. Learning and unlearning: is communication with minority patients about self or others? Medical Teacher 2011; 33: 781-782.
40. Downing R, Kowal E, Paradies Y. Indigenous cultural training for health workers in Australia. International Journal for Quality in Health Care 2011; 23(3): 247-257.
41. Durey A, Wynaden D, Thompson SC, Davidson PM, Bessareb D, Katzenellenbogen JM. Owning solutions: a collaborative model to improve quality in hospital care for Aboriginal Australians. Nursing Inquiry 2012; 19(2): 144-152.
42. Heaney SE, Tolhurat H, Baines SK. Choosing to practice in rural dietetics: what factors influence that decision? Australian Journal of Rural Health 2004; 12: 192-196.
43. Brown L, Capra S, Williams L. Profile of the Australian dietetic workforce: 1991-2005. Nutrition and Dietetics 2006; 63: 166-178.
44. Kowal E. The politics of the gap: Indigenous Australians, liberal multiculturalism, and the end of the self-determination era. American Anthropologist 2008; 110(3): 338-348.