Paramedics are considered experts in pre-hospital emergency care. Paramedic practice has traditionally been concerned with the provision of pre-hospital and out-of-hospital emergency medical services in a community or industrial setting, with the aim of stabilising the patient and transporting them to a hospital or health provider for further treatment1. The paramedic profession, especially in rural areas, has witnessed an extension beyond this emergency care focus.
Paramedics are working more closely with other professions in an extension of care and expanded scope of practice that incorporates primary health care. This collaborative care in rural areas may range from paramedics working and being educated with other professions in the hospital environment, to involvement in healthcare planning in the pre-hospital environment2. The resultant synergy of education and practice among various professions is synonymous with the basic premise of interprofessional learning (IPL) where processes are ultimately directed toward improved patient care outcomes.
Interprofessional learning could be considered an overarching concept incorporating both interprofessional education (IPE) and interprofessional practice (IPP). Interprofessional education occurs when two or more professions learn with, from and about each other, and IPP occurs when two or more professions are committed to working and interacting together. This interaction is more comprehensive than different professions simply working side by side; it involves working together to achieve a common purpose of healthcare delivery, with mutual respect and improved health outcomes3-5. Stone4 offers a comprehensive definition of IPL:
It [IPL] is a philosophical stance, embracing lifelong learning, adult learning principles and an ongoing active learning process, between different cultures and health care disciplines. IPL philosophy supports health professionals working collaboratively in a health care setting, through a purposeful interaction with service users and carers, to produce quality patient centred care. It acknowledges both formal and informal methods of learning which progress to develop service delivery4.
The rural setting offers an ideal environment in which to explore IPL and the relationships between healthcare professionals in the delivery of care. Rural interprofessional teams include a diverse range of professionals such as doctors, nurses, counsellors, physical therapists, dental hygienists and community health workers6. The types of care offered by interprofessional teams in rural areas have ranged from primary health care preventative services such as general health assessments, childhood obesity programs, information on organ donation, pap smears, road safety campaigns and palliative care7,8. In rural Australia, there have been positive reports of community interaction and primary health care service provision using interprofessional teams that include paramedics2,9.
The traditional approach to paramedic practice has centred on pre-hospital and out-of-hospital emergency medical services, generally practised in isolation to other health professionals. However, a number of proposals have been made to extend the role of paramedics to involve greater consultation with other healthcare providers in the ongoing care for patients in their own homes. As early as 2000, the United States National Highway Traffic Safety Administrator envisaged the future role of paramedics as one that would be more integrated with the overall health system by undertaking a community-based management role10. The potential for rural paramedics in this integrated role appeared in a 2004 agenda for the future of rural paramedics in the USA11, and also a 2005 strategic directions article on the future of paramedic services in Canada12. The focus has been on integration with the health system and provision of a mobile primary healthcare service offering activities such as self-care, injury prevention programs and social services12. Most recently in Australia, a nationwide project has offered federal funding for the establishment of extended paramedic care models that will see paramedics working within primary health care and providing services complementary to those offered by general practitioners13. Some of this funding has been directed to rural areas where paramedics will be involved in patient care services such as ongoing wound care, initiation of antibiotic therapy, urinary catheterisation, and in areas such as pathology, chronic and palliative care. These proposals emphasise the critical importance of interprofessional activity.
Given the interprofessional nature of rural practice and proposals for expanded paramedic care, the rural environment offers an ideal opportunity by which to explore paramedic interaction with other professions. This article reviews literature that reports on rural paramedics' engagement with IPL and identifies gaps where future research is required.
A search was conducted across May 2013 of literature related to IPL in rural areas that incorporated paramedic care. This search used a technique based on research by Dimoliatis and Roff14, who identified search terms for the MEDLINE database most likely to retrieve articles relevant to inter/multi-professional education. In developing search algorithms, they argued searching the title/abstract as an effective approach in the search for interprofessional literature. Further to this, using a combination of prefixes 'inter' and 'multi' with adjectives 'professional', 'disciplinary' and 'shared' and the nouns 'education', 'learning' and 'training' retrieves almost all possibly relevant articles. This present study incorporated these search terms in combination with each of the terms 'rural' and 'remote' and also 'paramedic/s' and 'pre-hospital'. Each of these was also combined with the search term 'collaboration'.
The search extended beyond the MEDLINE database and incorporated the same search terms across SCOPUS, CINAHL and the University of Tasmania (UTAS) electronic library search. Specific journal searches conducted in the same manner include the Journal of Emergency Pre-Hospital Care (JEPHC) and the Journal of Interprofessional Care. The SCOPUS search only allowed examination of abstract rather than title and abstract. The UTAS search and CINAHL searches were conducted across all fields. On completion of the initial search process, relevant articles were examined for references also appropriate to IPL and rural paramedic care.
Journal articles, conference proceedings, reports and proceedings were all considered. All levels of evidence were also included. Journal articles were in English and no restrictions were placed on year of publication. To maintain relevance to interprofessional activity across paramedic care, certain literature was excluded. This included literature that was not healthcare related, did not refer to paramedic care, involved only a single profession, and did not have a clear statement of interprofessional intervention.
The content of each article was examined for relevance to definitions of IPE, IPP and IPL and grouped accordingly. Articles concerned with both IPE and IPP were considered to be examples of IPL. Articles that did not fit the concept 'interprofessional' were regarded as examples of multi-disciplinary teamwork - where health professionals work closely alongside each other but not necessarily in an interactive, collaborative or communicative way15.
The initial search methods used for this review yielded 24 articles with interprofessional themes that included paramedic care in rural and remote areas. Articles were published between 1997 and 2012. A review of all reference lists produced a further eight articles. None of the articles sourced represented level 1 (systematic review) or level 2 (randomised control trial) evidence16. The concepts of interest that emerged from a full content review of each of these articles were IPE, multidisciplinary teamwork and IPL.
Interprofessional education
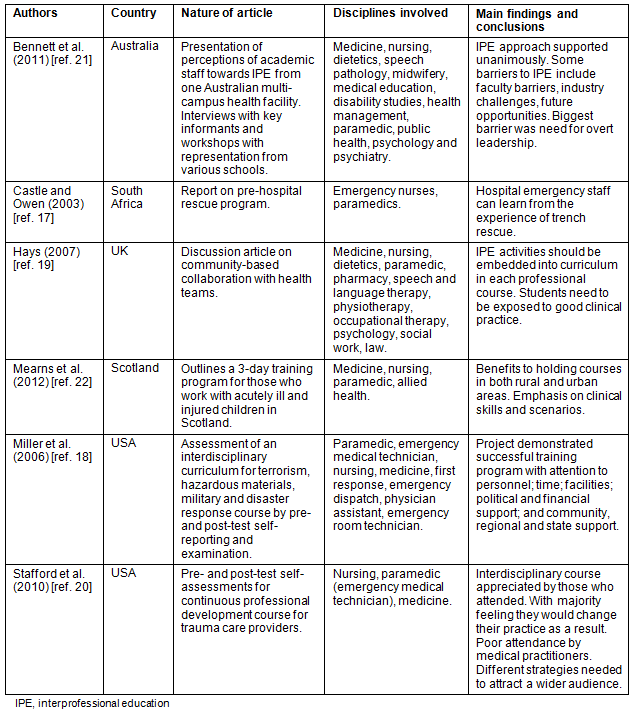
Interprofessional education incorporating paramedics is one of the concepts highlighted in this literature search. The relevant articles are listed in Table 1. Early reports of IPE, involving paramedics in rural areas focused on the 'high end' disaster medicine aspect of pre-hospital care. Castle and Owen17 reported on paramedics undergoing trench rescue training in South Africa, and how hospital emergency staff gained patient care experience and awareness of 'in field' practice from participation in such training programs. Similar benefits have appeared in training among various pre-hospital and emergency department professionals in the USA, with courses designed around terrorism, hazardous materials, military and disaster response18.
More conventional paramedic response when incorporated with an IPE environment was focused on the traditional accident and emergency role of paramedics. Hays19 discussed the advantages of different educational activities that various professions may be involved in, but incorporation of paramedics was limited to accident scene scenarios, or first aid knowledge, rather than participation in chronic disease cases or home-based assessments. Stafford et al20 mentioned attendance of pre-hospital providers at an IPE initiative that incorporated development of rural trauma teams. Although the study was primarily concerned with attendance of surgeons, it was reported that pre-hospital (paramedic) provider attendance numbers at these courses was second only to nursing staff.
Paramedic participation in IPE has not been limited to emergency or first aid care. Bennett et al21, when reporting on the perceptions of university academic staff toward IPE initiatives, recognised the contribution of university paramedic schools and included informants from these schools to advise on faculty perceptions of IPE. Mearns et al22 noted the attendance of paramedics, nurses, doctors and other health professionals at three-day paediatric training courses in rural and urban Scotland. Although some of the course content included general first aid or paediatric life support, other content included communication, understanding the rights of paediatric patients and child protection issues.
Table 1: Interprofessional education
Multidisciplinary teamwork
The concept of 'multidisciplinary' is considered to have a different meaning to 'interprofessional': health professionals may work alongside each other collaboratively, but not necessarily with a shared purpose that includes reciprocal learning.
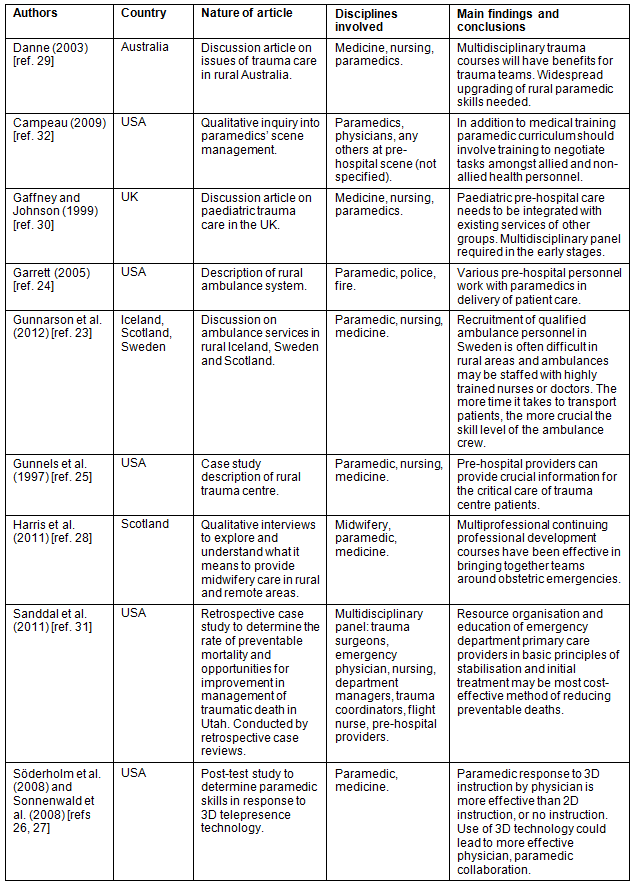
Several articles described multidisciplinary teamwork (Table 2). In some cases, paramedics worked on ambulances alongside other professions such as nursing or medicine in the provision of pre-hospital care23. Traditionally, however, paramedics responded to patients without initial assistance and incorporated other professions as care progressed. Importantly, this involved not only medical personnel but also professionals such as police and fire services24. Pre-hospital care also included a multidisciplinary approach even when other disciplines were not present at an incident. Here, paramedics notified a trauma centre of patient condition and sought advice from other medical personnel at the trauma centre about care of a patient25-27.
Several authors acknowledged the importance of the paramedic on the multidisciplinary team. Harris et al28 reported on midwives and obstetric care in rural Scotland. They recognised the expertise of paramedics in pre-hospital care when associated with the management of obstetric emergencies by midwives in rural areas. Danne29 suggested multidisciplinary trauma courses and the need for more widespread upgrading of paramedic skills in rural areas to deal effectively with trauma patients. Two articles illustrated multidisciplinary teamwork that did not involve direct patient care. Gaffney and Johnson30 and Sanddal et al31 recognised the expertise of pre-hospital providers in trauma care, with their inclusion of paramedics on multidisciplinary panels of review to determine appropriate trauma management.
One article, in adopting a theoretical perspective of paramedic work, offered a link from multidisciplinary teamwork to IPE. Campeau32, in adopting a grounded theory approach to examine paramedic scene management, suggested that in addition to more technical or procedural medical components, paramedic curriculum should involve training in how to negotiate working with allied and non-allied personnel at the scene of patient care. The article by Campeau32 offers insight into the synergy that can exist between multidisciplinary teamwork and interprofessional education. Although the study was around scene management that incorporated varied personnel in practice, the author suggested such training would also benefit other healthcare personnel in their understanding of the patient/paramedic environment.
Table 2: Multidisciplinary teamwork
Interprofessional learning
Some of the literature described the concepts of IPE or of multidisciplinary teamwork and also addressed the processes involved with professional interaction, a key component of IPL (Table 3).
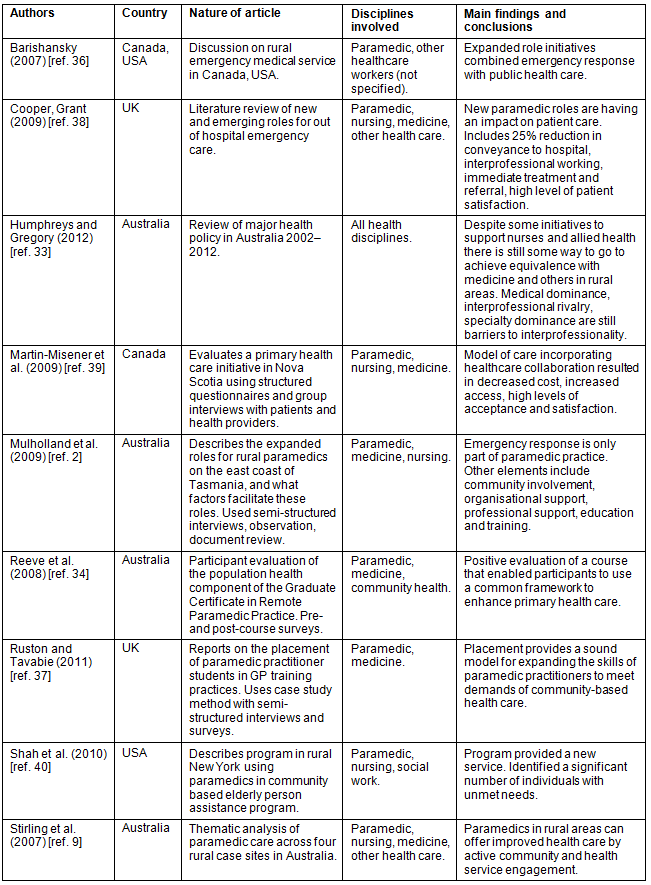
Some articles contained cursory acknowledgement of the role of paramedics, and others offered more comprehensive descriptions of interprofessional activities. Humphreys and Gregory33, in their review of major health policy in Australia, referred to the possibility of an expanded scope of practice for paramedics to work more closely with other health professionals in rural areas. More specific to IPL, in Australia paramedics have been able to undertake a Graduate Certificate in Remote Paramedic Practice through the Mount Isa Centre for Rural and Remote Health of James Cook University in Queensland. This course involved paramedics learning from medical practitioners and other health professionals to become part of a rural primary healthcare team. Following a review of the program, Reeve et al34 reported increased participation in patient education and health promotion, increased partnership with other community healthcare providers, engagement in service provision and changes to patient care such as greater interaction, with more time spent in the patient's home environment.
Paramedic work has been shown to involve more than traditional emergency care, and has included a move into primary health care with community involvement, organisational support, professional support, and education and training. Paramedics in rural areas have participated in education sessions with other health professionals, worked informally in assistance roles in emergency departments, and have consulted with other health practitioners in patient care planning2,9,35,36. These enhanced roles for paramedics have been further described by Ruston and Tavabie37, who reported on a program in the UK where paramedics were specifically trained to work in community-based health care. These paramedic 'practitioners' undertook placements in general medical practices, both learning from and working with GPs and other health professionals. In an earlier review of these new roles for paramedics in the UK, Cooper and Grant38 found a 25% reduction in conveyance to hospital, in addition to interprofessional working, the ability for immediate treatment and referral, and high degrees of patient satisfaction.
Two articles are particularly useful in describing the potential of IPL for rural paramedics. A comprehensive three-year evaluation of a primary healthcare project on Long and Brier Islands in Nova Scotia involved paramedics, nurses and physicians39. The study reported not only positive collaboration between health team members, but also increased access to healthcare services and the cost-effectiveness of this model of patient care in rural communities with low emergency call volumes. Shah et al40 reported similar success with a program in rural New York state. Here, paramedics were trained in geriatric care in order to provide collaborative home-based assessment and care for elderly adults who accessed emergency medical services. Health screening by paramedics resulted in home visits from a nurse or social worker with further evaluation in the fields of vaccinations, advanced directives, formal and informal support services, nutrition, activities of daily living, depression, alcohol and drug abuse, falls, cognition, medication and home safety. This interprofessional activity also identified an otherwise unknown number of individuals with unmet needs.
Hauswald et al41 described an 'advanced care' project with paramedics working cooperatively with nursing and medical staff to provide primary healthcare services in rural USA. In a continuation of the paramedic practitioners initiative reported by Ruston and Tavabie37 similar schemes have been in operation in the UK since the early 2000s. Emergency care practitioners (ECPs) are described as paramedics trained to work from general practitioner surgeries, support primary healthcare teams, attend unscheduled home visits and arrange hospital admissions, with time divided between local minor injury units and ambulance stations. Other paramedic practitioners have undertaken training in wound care and suturing, joint examination, social needs assessment, antibiotic administration and radiological referral to provide care in referral with other health professionals38,42-46. Emergency care practitioners and paramedic practitioners have appeared in both rural and urban areas of the UK. Evidence from Australia has shown that rural paramedics in particular have been involved in IPE and practice that has evolved through informal networks. In a major study of case sites across four Australian states, O'Meara et al47 highlighted the involvement of rural paramedics with other health professionals in the treatment of minor injuries and the provision of primary health care.
Table 3: Interprofessional learning
Discussion
This literature review is an investigation of IPL specifically incorporating paramedic practice and care in rural communities. The choice of a rural setting was made because of the unique perspective the rural environment has on IPL, with teams of various health professionals collaborating to improve patient care outcomes. The literature was grouped into three categories: IPE, multidisciplinary teamwork and IPL. Each incorporated professional interaction but in different ways. Interprofessional education involved professions learning with, from and about each other. Multiprofessional teamwork represented collaboration between health professionals in practice. Interprofessional learning included the interactive processes that occurred as well as education and collaborative practice components. Arguably, all were orientated to the end goal of providing quality, patient-centred care.
Paramedics have been involved in education programs with other healthcare professions. In some instances, this education process has been about specific aspects of pre-hospital intervention, such as the disaster response program18 trauma team development20 or paediatric care22. The aim of such education has been to inform practice with, for example, more efficient trauma teams, or a greater understanding of paediatric care.
Traditional paramedic practice has not necessarily been interprofessional in nature. It has generally been more multidisciplinary, where professionals collaborate to achieve patient care whilst protective of their own professional identity and activity spaces. Non-medical personnel such as police and fire crews have assisted at accident scenes24, paramedics have been part of obstetric emergency teams28, trauma teams29 or even clinical review panels30, but their membership has often been determined by their specific disciplinary expertise. Campeau's32 work on the theory of paramedic scene management acknowledged the collaboration of allied and non-allied personnel in provision of paramedic care; however, rather than multidisciplinary working, the paramedic scene of care had become one in which individual professions were involved in complex collaborative processes.
It is this awareness of the processes of collaborative practice, and the interprofessional nature of education, that suggests that paramedics in rural areas may be involved in a process of interactive, IPL. Frequently, the literature indicated a move in rural paramedic practice toward roles incorporating interprofessional interaction not previously seen with traditional emergency care. Reeve et al34, and Ruston and Tavabie37 both mentioned paramedics training and working with medical and other healthcare practitioners in pursuit of a primary healthcare model of practice. Mulholland et al2 suggested that informal primary healthcare practices existed alongside an emergency care model in rural areas. This extended scope of practice for paramedics continued as a prominent theme in the literature around IPL incorporating paramedic care. Articles referred to processes where training and practice are undertaken with other health professionals to provide clinical care beyond that of emergency care, incorporating interventions such as wound care, antibiotic administration, radiological referral, and even social needs assessment38,42-46. The Long and Brier Islands project39 and the New York initiative40 saw paramedics and other health professionals learning about, from and with each other, with commitment to working together and achieving common healthcare delivery. These are all principles of interprofessional education, practice and learning4,48.
Despite some evidence of IPL incorporating paramedic care, the ways in which different rural groups involved in paramedic care interact and construct meaning about an interprofessional approach to patient care are largely underexplored. The sourced literature to date is largely descriptive of certain procedures and programs; there is sparse knowledge around interactions of various professions involved; little is known of the influence of this activity on aspects such as professional identity or culture. Leadership is an area recognised as important in new paramedic interventions41,44,45; however, the effect(s) of group interaction and implications for leadership within paramedic care and IPL is underexplored. Importantly, the aim of IPL is for quality patient-centred care, yet few articles reported on the impact of IPL on patient outcomes.
Interprofessional learning involves complex processes between people from different disciplines. Further investigation of paramedics' involvement with other professionals may add to the understanding of IPL. Rural and remote areas, where there are often strong imperatives for healthcare providers to work together to achieve the best possible patient outcomes, can be an ideal setting for such investigations.
Limitations
The scope of this review was limited to discussion on IPL and rural paramedic care, and the terms used, specific search engines and journals limited the literature selected. Although journal articles, conference proceedings, reports and proceedings that were able to be located were all considered, other relevant literature may exist among 'grey literature'. A search of all fields rather than title/abstract alone may capture greater data. For paramedic literature, a search on 'expanded scope' or 'extended care/practice' may reveal further articles where interprofessional learning or activity is taking place but not referred to as such.
Rural paramedics are involved with other healthcare professionals, often in new or expanded roles. Within these roles, paramedics collaborate in IPE, learning with, from and about other healthcare professionals, and are involved in multidisciplinary practice. Published journal articles that report on this interaction are largely descriptive in nature and few describe the dynamics of this interaction or the conditions under which interprofessional activity could yield potential benefit to health service delivery or patient outcomes. Interprofessional learning brings together education and practice in a process whereby individual professions interact together with a common aim of enhanced patient care. Interprofessional learning embraces adult learning principles and ongoing active learning processes in a philosophical stance supporting collaborative, purposeful, informal and formal interaction in the healthcare setting. As an overarching construct, IPL may be used to frame further investigation of this interaction and may help shape the emerging role of paramedics in rural settings where population size and other factors limit the availability of health professionals.
References
1. Department of Health. Consultation paper: options for regulation of paramedics. Perth: Australian Health Ministers' Advisory Council, July 2012.
2. Mulholland P, O'Meara P, Walker J, Stirling C, Tourle V. Multidisciplinary practice in action: the rural paramedic - it's not only lights and sirens. Journal of Emergency Primary Health Care (Online) 2009. Available: http://ro.ecu.edu.au/jephc/vol7/iss2/6/ (Accessed 27 June 2014).
3. Freeth D, Hammick M, Reeves S, Koppel I, Barr H. Effective interprofessional education: development, delivery and evaluation. Oxford: Blackwell Publishing, 2005.
4. Stone J. What is IPE/IPL/IPP?: Australian Interprofessional Practice & Education Network (AIPPEN). (Online). Available: http://www.aippen.net/what-is-ipe-ipl-ipp (Accessed 5 July 2011).
5. Centre for the Advancement of Interprofessional Education. Defining IPE. (Online) Available: http://www.caipe.org.uk/about-us/defining-ipe (Accessed 25 April 2011).
6. Connelly T, Assell R, Peck P. Interdisciplinary education for health science students in the rural home health agency. Kentucky January. Public Health Reports. 1975; 90(4): 325-330.
7. Florence JA, Goodrow B, Wachs J, Grover S, Olive KE. Rural health professions education at East Tennessee State University: survey of graduates from the first decade of the Community Partnership Program. Journal of Rural Health 2007; 23(1): 77-83.
8. Kelley ML, Habjan S, Aegard J. Building capacity to provide palliative care in rural and remote communities: does education make a difference? Journal of Palliative Care 2004; 20(4): 308-315.
9. Stirling CM, O'Meara P, Pedler D, Tourle V, Walker J. Engaging rural communities in health care through a paramedic expanded scope of practice. Rural and Remote Health 7: 839. (Online) 2007. Available: www.rrh.org.au (Accessed 20 December 2008).
10. National Highway Traffic Safety Administrator. Emergency medical services agenda for the future. (Online) 2000. Available: http://www.ems.gov/pdf/2010/EMSAgendaWeb_7-06-10.pdf (Accessed 27 June 2014).
11. Department of Health and Human Services USA. Rural and frontier emergency medical services agenda for the future: a service chief's guide to create community support of excellence in EMS. Rockville, MD: US Department of Health and Human Services, Health Resources and Services Administration, Office of Rural Policy, 2004.
12. Emergency Medical Services Chiefs of Canada. The future of EMS in Canada: defining the new road ahead. (Online) 2006. Available: http://www.emscc.ca/docs/EMS-Strategy-Document.pdf (Accessed 17 July 2011).
13. Health Workforce Australia. Extending the role of paramedics. (Online) 2012. Available: http://www.hwa.gov.au/work-programs/workforce-innovation-and-reform/extended-scopes-of-practice-project/extending-role-of-paramedics (Accessed 7 April 2012).
14. Dimoliatis IDK, Roff S. Interprofessional/multiprofessional health professions education: designing an efficient search to scope the literature of this exploding field. Health Information & Libraries Journal 2007; 24(4): 274-282.
15. Atwal A, Caldwell K. Nurses' perceptions of multidisciplinary team work in acute health-care. International Journal of Nursing Practice 2006; 12(6): 359-360.
16. Cochrane Consumer Network. Levels of evidence. (Online) 2013. Available: http://consumers.cochrane.org/levels-evidence (Accessed 16 July 2013).
17. Castle N, Owen R. Rescue paramedic style: A training scenario. Emergency Nurse 2003; 11(2): 29-32.
18. Miller GT, Scott JA, Issenberg SB, Petrusa ER, Brotons AA, Gordon DL, et al. Development, implementation and outcomes of a training program for responders to acts of terrorism. Prehospital Emergency Care 2006; 10(2): 239-246.
19. Hays R. Interprofessional education in the community: where to begin. The Clinical Teacher 2007; 4(3): 141-145.
20. Stafford RE, Dreesen EB, Charles A, Marshall H, Rudisill M, Estes E. Free and local continuing medical education does not guarantee surgeon participation in maintenance of certification learning activities. The American Surgeon 2010; 76(7): 692-696.
21. Bennett PN, Gum L, Lindeman I, Lawn S, McAllister S, Richards J, et al. Faculty perceptions of interprofessional education. Nurse Education Today 2011; 31(6): 571-576.
22. Mearns C, Wilson J, Buchanan M. Multiprofessional education: improving care for acutely ill children. Nursing Children & Young People 2012; 24(4): 14-7.
23. Gunnarson B, Svavarsdottir H, Duason S, Sim A, Munro A. Ambulance transport and services in the rural areas of Iceland, Scotland and Sweden. Journal of Emergency Primary Health Care 5(1). (Online) 2012. Available: http://ro.ecu.edu.au/jephc/vol5/iss1/3 (Accessed 31 June 2013).
24. Garrett R. Reaping rewards in rural EMS. Emergency Medical Product News 2005; 13(5): 16-23.
25. Gunnels MD, Wood R. Level I and level III trauma center collaboration: a case study. Journal of Emergency Nursing 1997; 23(4): 382-383.
26. Söderholm HM, Sonnenwald DH, Manning JE, Cairns B, Welch G, Fuchs H. Exploring the potential of video technologies for collaboration in emergency medical care: Part II. Task performance. Journal of the American Society for Information Science and Technology 2008; 59(14): 2335-2349.
27. Sonnenwald DH, Söderholm HM, Manning JE, Cairns B, Welch G, Fuchs H. Exploring the potential of video technologies for collaboration in emergency medical care: Part I. Information sharing. Journal of the American Society for Information Science and Technology 2008; 59(14): 2320-2334.
28. Harris FM, van Teijlingen E, Hundley V, Farmer J, Bryers H, Caldow J, et al. The buck stops here: midwives and maternity care in rural Scotland. Midwifery 2011; 27(3): 301-307.
29. Danne PD. Trauma management in Australia and the tyranny of distance. World Journal of Surgery 2003; 27(4): 385-389.
30. Gaffney P, Johnson G. Paediatric prehospital trauma care. Trauma 1999; 1(4): 279-284.
31. Sanddal TL, Esposito TJ, Whitney JR, Hartford D, Taillac PP, Mann NC, et al. Analysis of preventable trauma deaths and opportunities for trauma care improvement in Utah. Journal of Trauma 2011; 70(4): 970-977.
32. Campeau A. Introduction to the 'space-control theory of paramedic scene management'. Emergency Medical Journal 2009; 26: 213-216.
33. Humphreys JS, Gregory G. Celebrating another decade of progress in rural health: what is the current state of play? Australian Journal of Rural Health 2012; 20(3): 156-163.
34. Reeve C, Pashen D, Mumme H, De La Rue S, Cheffins T. Expanding the role of paramedics in northern Queensland: an evaluation of population health training. Australian Journal of Rural Health 2008; 16: 370-375.
35. Mulholland P, Stirling C, Walker J. Roles of the rural paramedic - much more than clinical expertise. (Online) 2009. Available: http://ruralhealth.org.au/10thNRHC/10thnrhc.ruralhealth.org.au/papers/docs/Mulholland_Peter_B4.pdf (Accessed 27 June 2014).
36. Barishansky RM. The rural EMS crisis. EMS: Emergency Medical Services Magazine 2007; 36(10): 70-71.
37. Ruston A, Tavabie A. An evaluation of a training placement in general practice for paramedic practitioner students: improving patient-centred care through greater interprofessional understanding and supporting the development of autonomous practitioners. Quality in Primary Care 2011; 19(3): 167-173.
38. Cooper SJR, Grant J. New and emerging roles in out of hospital emergency care: a review of the international literature. International Emergency Nursing 2009; 17: 90-98.
39. Martin-Misener R, Downe-Wamboldt B, Cain E, Girouard M. Cost effectiveness and outcomes of a nurse practitioner-paramedic-family physician model of care: the Long and Brier Islands study. Primary Health Care research & Development 2009; 10: 14-25.
40. Shah MN, Caprio TV, Swanson P, Rajasekaran K, Ellison JH, Smith K, et al. A novel emergency medical services-based program to identify and assist older adults in a rural community. Journal of the American Geriatrics Society 2010; 58(11): 2205-2211.
41. Hauswald M, Raynovich W, Brainard AH. Expanded emergency medical services: the failure of an experimental community. Prehospital Emergency Care 2005; 9(2): 250-253.
42. Woollard M. The role of the paramedic practitioner in the UK. Journal of Emergency Primary Health Care 4(1). (Online) 2006. Available: http://ro.ecu.edu.au/jephc/vol4/iss1/11/ (Accessed 7 July 2008).
43. Cooke M. Emergency care practitioners: a new safe effective role? Quality and Safety in Health Care 2006; 15(6): 387.
44. Cooper S, O'Carroll J, Jenkin A, Badger B. Collaborative practices in unscheduled emergency care: role and impact of the emergency care practitioner - qualitative and summative findings. Emergency Medicine Journal 2007; 24(9): 625-629.
45. Mason S, Coleman P, O'Keeffe C, Ratcliffe J, Nicholl J. The evolution of the emergency care practitioner role in England: experiences and impact. Emergency Medicine Journal 2006; 23: 435-439.
46. Cooper S, Barrett B, Black S, Evans C, Real C, Williams S, et al. The emerging role of the emergency care practitioner. Emergency Medicine Journal 2004; 21(5): 614-618.
47. O'Meara P, Walker J, Stirling C, Pedler D, Tourle V, Davis K, et al. The rural and regional ambulance paramedic: moving beyond emergency response. Report to The Council of Ambulance Authorities Inc. Bathurst, NSW: School of Public Health, Charles Sturt University, 2006.
48. World Health Organization. Framework for action on interprofessional education and collaborative practice. Geneva: Department of Human Resources for Health, 2010.


