Paramedics perform a wide range of complex, invasive, and often high-risk emergency medical procedures1,2. The performance of these procedures, however, is not a sufficiently unique occupational characteristic to distinguish paramedics from other healthcare professionals. What truly distinguish paramedics are the settings in which they practice, where they must continually adapt procedures to suit their work environment3. In sectors such as mining, oil, gas, and construction, it is common for employees to work in remote locations in both developed and developing countries4. With the exception of a combat zone, there is arguably not a more hazardous and complex workplace for a paramedic than a remote industrial site, an environment often characterised as isolated5, dangerous6, and clinically unpredictable7. This is evidenced by reports of high mortality rates despite a well-established regulatory environment and significant investment in occupational safety8. The death rate in mining is among the highest of all sectors in Australia8 with Safe Work Australia reporting the number of mining fatalities in 2011-2012 to be 3.84 per 100 000 workers, exceeding the national rate by 70%9. The construction industry fares even worse with a death rate of 4.34 per 100 000, accounting for 11% of all serious workers' compensation claims10. These compelling statistics underscore the especially challenging nature of the environment wherein remote paramedicine is practised.
Due in part to a shift to tertiary education, an expanding scope of clinical practice, and the relative over-supply of qualified graduates11, paramedics are increasingly being hired to provide emergency care, chronic care, and primary health services to employees working in these extreme industrial environments11. In addition to the challenges of practising in remote locations such as mines or offshore oil and gas platforms, paramedics are responsible for managing complex patients who are exposed to a wide range of health risks12. Specific occupational risks include tropical and infectious diseases13, hyperbaric diving injuries14,15, altitude-related illness16, chemical exposures16, as well as minor to severe traumatic injuries17. Compounded by the effects of isolation and high stress levels, patients can also experience worsening mental health and chronic disease states18,19. A key difference between paramedic practice in remote locations and that of traditional paramedicine, which usually takes place in an ambulance in a metropolitan, regional or even combat setting, is that the remote paramedic may be alone with the patient for several hours or days before assistance arrives or medical evacuation can occur7,20. The purpose of this article is to present a review of Australian and international published literature in search of a definition for industrial paramedicine.
The word paramedicine can have a variety of meanings. For the purpose of this investigation, paramedicine is defined as an emerging profession21,22 representing the intersection of health care, public health, and public safety23. In Australia, private-sector paramedicine is quite heterogeneous with practitioner skill and experience levels ranging from novice basic first-aid providers to highly experienced intensive-care practitioners24. The practice of appointing paramedics with limited skills or experience may be having an impact on the safety and quality of the care being provided in remote locations25. As previously mentioned, often these paramedics are the only medical providers on site and the combination of inexperience, limited education, and absence of immediate assistance could potentially expose employees and companies to risk.
This risk may be greater in Australia than in Canada or the UK given that in Australia the title of paramedic can be claimed by anyone24 and some individuals calling themselves paramedics may undertake clinical roles that they are not trained to perform or are beyond their level of expertise26. The absence of title protection for paramedics results from a lack of cohesion in paramedic education, registration, legislation, and employment standards between the states and territories25. Two states are aiming to deal with this ambiguity by introducing or amending legislation to protect the title of paramedic. A Tasmanian law that came into effect in 2014 restricts the use of the title to only those paramedics employed by Ambulance Tasmania27. Subsequent to this change, staff employed by private companies in Tasmania cannot call themselves paramedics unless approved by the Commissioner. South Australia has amended legislation to protect the title of paramedic for only those who hold qualifications prescribed by regulations (yet-to-be-defined)28. It is conceivable that the regulations will identify holders of a university degree in paramedic practice or a similar qualification as the minimum requirement to use the title of paramedic.
Towards an overarching goal of defining the paramedic profession in general, Paramedics Australasia, the peak body for paramedicine in the region, released a document in 2013 proposing a set of paramedic role descriptions29. Each description includes a definition, a summary of the prerequisite education, and a description of other requirements for each role. Also outlined is the operational environment each role works within and the clinical scope of practice for the respective roles. While the document is quite comprehensive, identifying several professional streams and levels of practice, unfortunately, it does not specifically include a definition of an industrial paramedic. Given the specialised nature of the role, the omission of a specific description for industrial paramedics is a major limitation of the Paramedics Australasia document, leaving a key gap in the paramedic profession.
It is both imperative and timely to address the existing gap in role definition, professional regulation, and scope of practice of industrial paramedics30. As mentioned, industrial health and safety is an important and high-risk facet of key natural resource and construction sectors31. In addition to staffing mass public events, the Council of Ambulance Authorities (CAA) notably estimates that 1-2% of the total paramedic workforce in Australia provides private services to industrial or mining operations32. In their 2012 submission to the Health Ministers' Advisory Council, the CAA recommended the development of appropriate regulation to reduce the risk to the public by paramedics practising in this domain32. It is anticipated that the pending resolution of the Australian debate around registration will make a significant contribution to ensuring the provision of safe, quality patient care on remote sites21,33. It will be essential to have the full range of paramedic titles and specialisations defined, including for those working in remote industrial settings. Once a validated definition and practice description exists for industrial paramedics, employers will be better positioned to hire those with the required knowledge, skills, attitudes, and behaviours to function safely in these roles. The key objectives of paramedic registration are to protect public safety, ensure quality service and enhance public confidence33. For this to occur, the personnel calling themselves paramedics must be trained to a minimum standard and provide care in an ethical and responsible manner. All members of the public, including those who live and work in remote areas, need to be confident that paramedics have the required skills, experience, and qualifications to care for them safely and effectively. Likewise, industrial paramedics must be held to the same education and practice standards as their colleagues working traditional emergency response ambulances.
In alignment with the proposed registration and regulation of paramedics, a distinct scope of practice must be defined specifically for this subset of providers who function in remote industrial environments and who have unique responsibilities. Industrial paramedics work in geographic and professional isolation, necessitating largely independent practice12. In many cases, these paramedics have expanded online medical support34 and are able to initiate treatments not routinely performed by traditional paramedics35,36. Acknowledging that additional skills, procedures, medications, and therapies are available to remote paramedics13 necessitates a more comprehensive task analysis to develop a distinct scope of practice. This could inform policy makers and drive the development of accredited curriculum, entry to practice standards, benchmarking against other health professions, and the expansion of discipline-specific continuing professional development (CPD) opportunities37. In keeping with the underlying objectives of registration, these remote paramedics must then be trained to an accredited standard and maintain ongoing professional competence. The aforementioned outstanding issues involving registration, regulation, and scope of practice highlight the importance of defining the industrial paramedic.
The absence of a definition for the industrial paramedicine and a paucity of literature about the qualifications, scope of practice, education, and safety of their practice necessitates this enquiry. Databases were searched using multiple keyword sets. Citations were identified and managed using EndNote (vX6) and an initial screening of the titles and abstracts was carried out. A supplementary search of citations from the reference lists was also conducted. Where relevant, the full publications were obtained and compared to the inclusion and exclusion criteria. The reviewer read the selected articles, documenting them in written short summaries. No hard-copy searching was performed, nor was an Internet search of grey literature conducted for the initial review.
Databases
The search strategy targeted the EBSCOhost (health), MEDLINE, SCOPUS, and CINAHL electronic databases.
Key words
Primary search terms included remote, offshore, mining, and oil. These search terms were combined with the secondary search terms paramedic and emergency medical services using the AND Boolean operator. The combined searches were mapped to the medical subject headings (MeSH 2014) emergency medical services, occupational health, oil and gas fields, mining, and allied health personnel. No date or language limitations were initially applied.
Inclusion/exclusion criteria
Articles were included where:
- a paramedic (or medic, or similar health provider) provided health services of any kind in a remote, oil, gas, mining, or other related environment
- full-text reports published in English or translated to English could be sourced.
Articles were excluded where:
- the report made no mention of the role of paramedic (or similar health provider)
- the role and/or work environment described was that of a traditional or typical ambulance service paramedic
- the citation was returned in a previous search and were therefore a duplicate of those already accepted
- the articles were not available in English
- the full-text article could not be found after extensive searching.
The review process is described in Figure 1. An initial search using the combined two-term sets identified 870 citations. After applying the inclusion and exclusion criteria to a title and abstract review, 69 citations met the criteria, including those discovered by searching the reference lists. Of these, nine citations were excluded because full-text papers could not be found and eight citations were excluded based on review of the full article. The result was 40 articles that discuss the role of paramedics or paramedic-like providers in the remote, industrial or offshore environment (ROP) and 12 articles that discuss the provision of emergency medical services in the mining or oil and gas sectors (MOEMS). The majority of the articles reviewed originated in the UK and the USA and primarily describe paramedic practice in offshore and maritime environments.
Notably, there is a paucity of research published about paramedic practice in non-traditional settings. Additionally, there is no definition or role description in Australia or internationally that adequately reflects all of the characteristics of industrial paramedic practice. Paramedic practice is a relatively young occupation so it is not surprising that formal theories about its practice in a range of work environments are not yet a focus of research3. There are however three common themes drawn from the available literature that can contribute to the creation of a definition for industrial paramedicine: remoteness (where they work), education (how they learn), and practice-based (what they do).
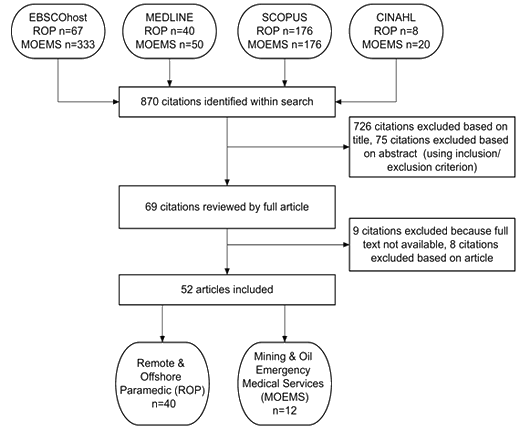 Figure 1: Flow diagram of the review process.
Figure 1: Flow diagram of the review process.
Remoteness of industrial paramedic practice
The literature identifies a number of geographical classifications used to describe traditional paramedic practice in Australia. Paramedics employed by government ambulance services are informally defined as urban, regional, or rural paramedics38-40. Those who work for the Australian Defence Force (ADF) providing out-of-hospital care, primary health care, and casualty evacuation in the military environment are classified as combat paramedics41. In the private sector, paramedics are similarly defined by their environment of practice. The articles reviewed offer a range of terms including industrial paramedic, rig medic, mine paramedic, maritime medic, offshore medic, remote paramedic, and emergency services officer when referring to health personnel working in specific industrial settings19,35,42-44.
The first key differentiating factor between traditional paramedics and industrial paramedics identified in the literature is the remoteness in which industrial paramedics generally practice4,7,20. The offshore oil and gas industry operates within Australian waters and around the globe in some extremely remote and inhospitable locations such as the North Sea, the Caspian Sea, the Gulf of Mexico, the Gulf of Guinea, Sakhalin Island, and the Arctic Circle35. The production of oil and gas has become a key major industry in many countries, including Britain35 where a large workforce is employed to work in the remote environment of the North Sea.
Companies engaged in the exploration and development of natural resources are responsible for the health and safety of their workers31. As an example, each offshore oil platform or remote site in the North Sea must have a medical presence on board and clinicians known as offshore paramedics provide the first line of emergency and primary health care12,45. These offshore paramedics also work on seismic exploration ships, cargo ships, and on other maritime vessels20,42,46. The provision of health services in remote locations is neither a new concept nor unique to paramedics. Cox was one of the first (1970) to write about the experiences of St John Ambulance first aid providers, male nurses, and doctors providing medical services on offshore drilling rigs in the North Sea47.
The dangerous work environments at isolated mining sites, oil platforms, maritime vessels, and other remote locations increase the frequency and severity of illnesses and injury18. Remotely based employees have limited access to traditional healthcare resources, including emergency care, primary health, and chronic disease management services11,48. In these health-resource-constrained environments, paramedics are employed by private companies to fill this gap by providing a comprehensive range of healthcare services.
Adding to these challenges, the large distances between major centres in Australia, coupled with a relatively low population density, requires healthcare services to be provided to industry sites and communities located several hundred or thousands of kilometres from a full-service hospital49. The paramedics, doctors, nurses, and allied health professionals who work in these communities have evolved into remote health specialists within their respective fields. Wakerman provides a definition of remote health in Australia50:
Remote Health is an emerging discipline with distinct sociological, historical, and practice characteristics. Its practice in Australia is characterised by geographical, professional and, often social isolation of practitioners; a strong multidisciplinary approach; overlapping and changing roles of team members; a relatively high degree of GP [general practitioner] substitutions; and practitioners requiring public health, emergency and extended care skills.
Like their hospital-based colleagues, paramedics are continually adjusting their professional practice to meet the needs of those who live and work in isolated locations51. A significant difference between remote or offshore paramedic practice and traditional paramedic practice is that the industrial paramedic may be working alone for several hours or days before assistance arrives7,12,20. In addition, the industrial paramedic does not have ready access to other medical professionals or advanced medical facilities that would be available in the urban or regional environments35. Ultimately, the geographical isolation and unique clinical environments where industrial paramedics practice is consistent with Wakerman's definition of remote health and must be considered in a definition for these practitioners.
Education-based description of industrial paramedicine
A second theme identified in the literature relates to the education and training of industrial paramedics. The Australian mining boom of the past decade52 has created a demand for emergency response and health service personnel in remote locations53. None of the articles from the systematic review provided information about industrial paramedic education specific to Australia. Therefore, a subsequent Internet search was performed in April and May 2014 to explore this further. The search revealed that the increasing demand for medical staff by the mining and industrial sectors has given rise to a number of private registered training organisations (RTOs) offering specialised short courses within Australia. Nine companies were identified offering Certificate IV industrial medic courses, ranging in duration from 10 to 16 days. A review of the online job postings during this time period demonstrated that a Certificate IV is the minimum qualification required to secure a job as a paramedic or emergency services officer in the industrial sector, with some of the posted positions requiring an advanced diploma or an undergraduate paramedic degree29.
In Australia, the education and training of traditional paramedics has undergone a significant transformation11,54. In almost all cases, the former in-house vocational training model has been replaced with tertiary, pre-employment education programs11. According to the Council of Ambulance Authorities (CAA), by 2015, the minimum qualification for paramedics to join any of the state or territory ambulance services will be an undergraduate paramedic degree32. The CAA website now lists 13 Australian universities that have full, provisional, or preliminary accreditation for the delivery of paramedic undergraduate degree courses55. Despite the significant growth in the industrial health care sector, it is surprising that none of these undergraduate paramedic courses have an industrial specialisation.
As the scope of practice increases, the role of paramedicine in Australia is becoming indistinct, with a blurring of professional boundaries between that of prehospital care, hospital care, medicine, and nursing39,56. There has been a substantial cultural shift from the 1990s, when paramedics were considered hierarchically inferior to other healthcare providers and even experienced paramedics were often answerable to newly registered nurses57. Paramedicine is evolving beyond emergency response and patient transport towards a discipline shifting towards primary health care within a more integrated medical services approach56,58. Unfortunately, tertiary paramedic education has not kept pace with clinical advancements and career diversification for paramedics in Australia. Paramedic courses maintain their focus on preparing graduates specifically for emergency response within traditional ambulance services59. In many paramedic courses, health promotion, injury prevention, chronic disease management, mental health, social determinants of health, and the extended scope of clinical practice are not taught in sufficient depth11,54,59-61. As a consequence, many graduate paramedics are ill prepared to work in remote industrial settings where these competencies are required; subsequently they are being performed without significant experience or on-the-job training.
Although established courses may remain the status quo, the uniqueness of remote and industrial paramedicine has led to the development of new undergraduate and postgraduate education courses both in Australia and internationally. For example, a Bachelor of Paramedic Practice with a Bachelor of Public Health Promotion double degree course is now being offered by La Trobe University in Victoria. This course is designed to prepare graduates for non-traditional paramedic roles in primary health care in rural and remote locations62. At the postgraduate level, a collaboration between Canberra University and Aspen Medical offers a Graduate Certificate of Remote Industrial Health63 in the Australian Capital Territory (ACT). This two-year, part-time course is offered by distance education to paramedics, nurses, and medical doctors who want to develop knowledge and skills required to provide health services to individuals and organisations located within remote industrial communities63.
Two specialised offshore paramedic courses are available in the UK. A Diploma in Remote and Offshore Medicine is offered by the Royal College of Surgeons of Edinburgh64 and an Offshore Medic course is available through the Nottingham University Hospitals36,65. Both courses are 4 weeks in duration and require students to have experience as a nurse, military medic, medical doctor, or paramedic. The training includes skill sessions, a practicum in the accident and emergency department and a placement with a general practitioner36.
In addition to industrial or remote-health-specific training and education, a variety of certifications are considered beneficial for work in the industrial, offshore, and remote health settings (Box 1). Besides their base-level qualification, paramedics can hold a number of training certificates, including Advanced Life Support (ALS) or Advanced Cardiac Life Support (ACLS), International Trauma Life Support (ITLS) or Prehospital Trauma Life Support (PHTLS)36, and alcohol and drug screening. Depending on the location of practice, non-clinical certifications may include Basic Offshore Safety Induction and Emergency Training (BOISET), Helicopter Underwater Egress and Safety Training (HUET), Self Contained Breathing Apparatus (SCBA), firefighting, confined space rescue, road crash rescue, vertical rescue, environmental health, food hygiene, and in some cases a Certificate IV in Occupational Health and Safety (OHS)7,36,46.
Similar to any health profession, education for industrial paramedics extends beyond initial training to include CPD. Continuing professional development is described by Martin as the undertaking of a variety of activities throughout one's career to become a more competent practitioner66. Once employed, paramedics report challenges to maintain their clinical skills in rural and remote settings7,61,67. As unregistered health practitioners in Australia, paramedics are not legally required to participate in ongoing education or skills maintenance68. However, as a condition of employment or to maintain a certificate to practice, government and private ambulance services may require ongoing professional development32,69. Although two published paramedic competency profiles currently exist in Australia, they are only intended to inform curriculum standards and are not enforceable as entry to practice standards or to dictate ongoing CPD requirements55,70,71. Complicating the situation further is that paramedics at industrial sites are often hired and supervised by non-medical managers, who lack understanding and awareness of the need for ongoing specialised clinical education and professional development and therefore do not necessarily consider it a priority7. This deficit of CPD is compounded by widespread skill atrophy in remote paramedics resulting from limited exposure to seriously ill or injured patients13,67. Advanced skills and procedures such as airway management, cardiac resuscitation, major trauma management, and medication infusions are performed infrequently72. These low-frequency, high-risk skills are essential for the rare occasions when the paramedic is required to respond to a major trauma or a cardiac arrest patient requiring acute care and invasive medical procedures43.
It is noted in the literature and by reviewing the job advertisements that while some employers require industrial paramedics to complete training beyond basic paramedic education, there is not yet a minimum standard for entry to practice or CPD for these remote practitioners. Arguably, the uniqueness of the industrial paramedic role requires additional tertiary education with clinical and non-clinical components. In addition, paramedics working independently in remote settings must focus on maintaining their skills and engaging in CPD opportunities. Specialised initial and ongoing education must therefore be carefully considered when developing a definition and role description for industrial paramedicine.
Box 1: Education and training requirements for industrial paramedics

Practice-based description of industrial paramedicine
Beyond discussing the remote and isolated location of industrial paramedic practice and the educational requirements, the literature also provides practice-based narratives of industrial paramedicine by practitioners who have worked in these environments. Unfortunately, these accounts are somewhat dated, ranging from 1991 to 2011, and none originate from Australia46,72,73. The offshore environment in the UK15,35, Canada74, and the USA13,17 provides the best available evidence of the professional background and scope of practice of the paramedics working in this sector. A review of the literature also reveals the importance of telemedicine referral pathways between remote worksites and shore while outlining the non-medical responsibilities of industrial paramedics. It is notable that there has been a significant shift since the 1980s when nurses primarily staffed remote sites30 to today's situation wherein paramedics are increasingly fulfilling these roles4.
Looking first at the professional background of industrial paramedics, interestingly, a 1987 paper from a UK author describes the offshore paramedic as either a registered nurse or the holder of a certificate in first aid and competence in using artificial respiration equipment43. In 1989 the term rig medic was first presented by Duffy, also from the UK45. At the time, all manned oil installations in the UK were required to have a rig medic on board to provide emergency care. This rig medic was typically a nurse with extended training, including an introductory course for working offshore, and who was required to have constant communication with a physician onshore35.
More recently, in 2009, Ponsonby et al. investigated medical emergency response in the offshore oil and gas industry. Looking internationally, they found that policies, regulations, and laws exist requiring manned offshore installations to have medics on board. They describe a medic in the context of the offshore environment7:
The term 'medic' is a loose one within the industry and, in general, refers to an individual with medical or nursing training, who is in charge of medical care at the offshore location. The level of training can vary from advanced first aid training to a medical degree. In many cases, paramedics, emergency medical technicians, or nurses who have had training and experience in emergency medicine are employed.
Turning now to scope of practice, beyond the emergency response role one would expect them to perform, the nature of a remote industrial site requires the paramedic to deal with a variety of medical concerns that are common in a population of predominantly 25 to 50 year-old male employees43. These paramedics must be able to treat minor ailments like dental problems45, ear, eye, nose and throat conditions35, respiratory infections, sexually transmitted diseases, minor soft tissue injuries, as well as provide counselling in the absence of other health professionals43. In 2011, Bisits Bullen studied paramedics working in oil, gas, and mining locations in 44 countries. She found that the medical staffing model for these sites comprised 39% doctors, 29% nurses, and 32% paramedics. Her study also revealed that in addition to providing emergency response, resuscitation, and primary health care, paramedics are very effective at implementing and measuring health promotion strategies that improve health outcomes on remote worksites4. The literature available serves to define a scope of practice for industrial paramedics (Box 2) that spans the professional boundaries of emergency medicine, primary health care, occupational medicine, chronic disease management, and intensive care.
Although industrial paramedics mainly practice independently, some form of telemedicine or online medical assistance is usually available to support them in their expanded scope of practice14,75. The paramedic will work under written instructions, clinical guidelines, or medical protocols established by their employer42,76. In addition, the offshore or remote paramedic will have access to a medical supervisor at another location who is colloquially referred to as the 'topside support'35. Typically, the paramedic also has the ability to consult with a medical doctor using telemedicine via telephone, satellite phone, radio, or internet videoconference34,77.
Telemedicine is a branch of e-health that uses communications networks for delivery of healthcare services and medical education from one geographical location to another78. This technology serves to improve medical emergency management in remote locations. It brings the patient closer, albeit virtually, to specialists and can allow for earlier appropriate treatment67. Innovations in telemedicine now include the transmission of 12-lead ECGs79,80, radiographs81, scope and camera images34, and ultrasound examinations67,82. The performance of these diagnostic procedures in remote settings demonstrates the expanded role of the remote paramedic. A further advantage of telemedicine consulting is the prevention of unnecessary medical evacuations, which has economic benefits for the employer35. In a 1996 article, Rhodes identified an oil production site in northern Russia where doctors supported paramedics via telemedicine. This clinical collaboration reportedly prevented a number of unnecessary medical evacuations, saving the company between US$50 000 and US$75 000 for each avoided transport18.
In addition to clinical duties within their scope of practice, paramedics are required by some worksites to take on a suite of non-clinical responsibilities. These can include providing first aid training for staff30,72, monitoring safe work practices, issuing personal protective equipment46, monitoring worksite and accommodation sanitation13,83 as well as testing food73 and drinking water for contamination18,43,46.
Despite the good work of previous international authors, a standardised role or practice description is yet to be defined for the industrial paramedic globally. Indeed, no article provides a definition of industrial paramedic specific to Australia. As evidenced in the literature, the expected practice of the industrial paramedic is unique, comprehensive, and specialised to suit their geographical and functional work environment. Taking into consideration the key themes highlighted in the available literature regarding their practice environment, education, and scope of practice, a proposed sample role description (Box 3) for the industrial paramedic includes an amalgamation of clinical and non-clinical responsibilities.
Box 2: Industrial paramedic scope of practice4,14,42,43,45,46
 Box 3: Proposed industrial paramedic role description4,7,12-14,42,46,73,74,84
Box 3: Proposed industrial paramedic role description4,7,12-14,42,46,73,74,84

Discussion
A comprehensive review of available literature reveals some common themes related to industrial paramedicine as well as opportunities for further investigation. Much of what is known about remote paramedic roles is directly or indirectly linked to traditional paramedicine, albeit with unique work locations, education pathways, and practice characteristics.
To provide context to the discussion, it is important to appreciate the current climate for paramedicine in Australia. All paramedics, whether traditional or industrial, are not yet recognised as health professionals and are not part of the Australian Health Practitioner Regulations Agency (AHPRA)85. Without regulation, and in the absence of legislation, the paramedic title is not protected and essentially anyone can identify themselves as a paramedic24. It is noted that protection of title legislation came into effect in South Australia and Tasmania in 201428,86. Until such time as national registration or specific legislation can prevent it, those with any level of training and experience can be employed to provide emergency and primary health care services at industrial sites. This practice may pose a clinical safety risk to patients25,26. Given the inherent hazards already associated with remote industrial work9,10, it is essential to reduce controllable risk factors whenever possible.
It is important to consider that in the absence of formal regulation and registration, paramedics are not obligated to participate in any regular CPD. Additionally, if employers do not appreciate the importance of clinical skills maintenance and do not actively support their paramedics, these practitioners are at risk of 'rusting out'87 and losing their clinical competence, especially in high-risk, low-frequency skills such as endotracheal intubation74. The literature reports that, in the industrial sector, many paramedics are only engaged in patient care 5-10% of the time13,72; the remainder of their work hours are spent performing non-clinical administrative, inspection, and staff training functions30,43,67. As such, a pressing challenge facing industrial paramedic practice is defining the clinical skills required for remote industrial environments and developing education programs for skill acquisition and retention when there is limited opportunity for clinical practice.
The literature clearly illustrates that the sectors in which industrial paramedics work are higher risk workplaces9,10. According to Campeau's space-control theory3, paramedics are concerned with establishing control over their immediate work space in order to reduce risks and create an environment that supports the delivery of emergency patient care. In contrast to other healthcare providers, paramedics do not have predictable and predetermined work areas. Rather, they must accept the location where they find a patient as their working area and adapt themselves and the environment accordingly3. It is conceivable that this adaptability is what makes paramedics uniquely well suited to work in remote industrial settings.
Based on the articles reviewed and analysed in the context of the current climate, a working definition of industrial paramedic is offered:
An industrial paramedic is an advanced clinical practitioner in paramedicine with an expanded scope of practice. The industrial paramedic provides emergency response, primary health care, chronic disease management, injury prevention, health promotion, medical referral, and repatriation coordination at remote mining sites, offshore installations, and other isolated industry settings. The industrial paramedic is resourceful, adaptable, and comfortable working independently. Industrial paramedics practice on site with limited resources, remotely located from tertiary care, and use telemedicine to consult with other health professionals as required. Industrial paramedics are experts at rapidly assessing, prioritising, and establishing control in their unpredictable workspace to reduce risks and create an environment conducive to quality patient care. The industrial paramedic preferably holds a specialised tertiary qualification and is committed to maintaining their clinical competency through continuing professional development.
Subject to scrutiny and further development by practising industrial paramedics and by future in situ research, this proposed definition provides an evidence-based description of contemporary industrial paramedic practice. In the current climate of professionalising paramedicine, it is essential to define the specialisations that exist within the discipline. The acceptance and adoption of a definition for industrial paramedicine will offer recognition to these unique practitioners as well as serve to inform professional bodies, employers, legislators, academics, and researchers going forward.
Campeau tells us that occupational knowledge is not static and it is important for paramedics to establish their theories of practice as their work evolves88. Such work would help differentiate paramedic practice from related professions and assist with the identification of the most appropriate research topics88. Certainly, industrial paramedicine is one emerging role that requires further investigation, beginning with the acceptance of a role definition.
Acknowledgements
The authors would like to thank the editor and reviewers for providing outstanding feedback, advice, and recommendations. Your support and wisdom are greatly appreciated.
References
1. Bigham BL, Buick JE, Brooks SC, Morrison M, Shojania K, Morrison LJ. Patient safety in emergency medical services: A systematic review of the literature. Prehospital Emergency Care 2012; 16(1): 20-35.
2. Jensen J, Croskerry P, Travers A. Paramedic clinical decision making during high acuity emergency calls: design and methodology of a Delphi study. BMC Emergency Medicine 2009; 9: 17-20.
3. Campeau AG. The space-control theory of paramedic scene-management. Symbolic Interaction 2008; 31(3): 285-302.
4. Bisits Bullen PA. Medics as a channel for worksite health promotion in remote global locations. American Journal of Health Promotion 2012; 26(6): 352-355.
5. Torkington AM, Larkins S, Gupta TS. The psychosocial impacts of fly-in fly-out and drive-in drive-out mining on mining employees: a qualitative study. Australian Journal of Rural Health 2011; 19(3): 135-141.
6. Lenné MG, Salmon PM, Liu CC, Trotter M. A systems approach to accident causation in mining: an application of the HFACS method. Accident Analysis & Prevention 2012; 48(0): 111-117.
7. Ponsonby W, Mika F, Irons G. Offshore industry: medical emergency response in the offshore oil and gas industry. Occupational Medicine 2009; 59(5): 298-303.
8. Ehsani JP, McNeilly B, Ibrahim JE, Ozanne-Smith J. Work-related fatal injury among young persons in Australia, July 2000-June 2007. Safety Science 2013; 57: 14-18.
9. Safe Work Australia. Mining Fact Sheet, 2013. Available: http://www.safeworkaustralia.gov.au/sites/swa/about/publications/pages/fs2010mininginformationsheet (Accessed 24 April 2014).
10. Safe Work Australia. Construction fact sheet. (Online) 2013. Available: http://www.safeworkaustralia.gov.au/sites/swa/about/publications/pages/fs2010constructioninformationsheet (Accessed 24 April 2014).
11. Joyce CM, Wainer J, Piterman L, Wyatt A, Archer F. Trends in the paramedic workforce: a profession in transition. Australian Health Review 2009; 33(4): 533-540.
12. Donnelly R. The offshore industry: overview. Occupational Medicine 2009; 59(5): 296-297.
13. Aalund LR. Remote paramedics have high level of training. The Oil and Gas Journal 1996; 94(18): 42.
14. Proctor JC. Distant oceanic paramedical practice: an example of environmental health nursing in remote hazardous locations. Life Support & Biosphere Science: International Journal of Earth Space 1998; 5(4): 437-442.
15. Harries MG. Medical aspects of the North Sea oil industry. Journal of the Royal Society of Medicine 1983; 76(9): 793-795.
16. Vearrier D, Greenberg MI. Occupational health of miners at altitude: adverse health effects, toxic exposures, pre-placement screening, acclimatization, and worker surveillance. Clinical Toxicology 2011; 49(7): 629-640.
17. Taylor DH, Casta R, Walker V, Collier F, Fromm RE, Jr. Air medical transport of patients from offshore oil and gas facilities. Historical accident data and initial experience. Air Medical Journal 1993; 1(1-2): 21-28.
18. Rhodes A. Oil companies focus on health care for remote operations. The Oil and Gas Journal 1996; 94(34): 76-80.
19. Gardner R. Overview and characteristics of some occupational exposures and health risks on offshore oil and gas installations. Annals of Occupational Hygiene 2003; 47(3): 201-210.
20. Putnam J. Maritime health care. British Journal of Sports Medicine 2005; 39(10): 693-694.
21. O'Meara P. Paramedics marching toward professionalism. Journal of Emergency Primary Health Care 7(1). (Online) 2009. Available: http://ro.ecu.edu.au/jephc (Accessed 30 April 2013).
22. Williams B, Onsman A, Brown T. Is the Australian paramedic discipline a full profession? Journal of Emergency Primary Health Care 8(1). (Online) 2010. Available: http://ro.ecu.edu.au/jephc (Accessed 30 April 2014).
23. United States Department of Transportation National Highway Traffic Safety Administration. Emergency medical services: agenda for the future. (Online) 1999. Available: http://www.ems.gov/pdf/2010/EMSAgendaWeb_7-06-10.pdf (Accessed 5 May 2014).
24. Eburn M, Bendall JC. The provision of ambulance services in Australia: a legal argument for the national registration of paramedics. Journal of Emergency Primary Health Care 8(4). (Online) 2010. Available: http://ro.ecu.edu.au/jephc (Accessed 5 May 2014).
25. Paramedics Australasia. Public risk and paramedic regulation: response to the Australian Health Ministers' Advisory Council consultation paper: options for regulations of paramedics. (Online). 2012. Available: http://nrha.org.au/hcrra/sites/default/files/papers-submissions/Paramedics Australasia Submission on Paramedic Registration.pdf (Accessed 30 April 2014).
26. Australasian College for Emergency Medicine. Submission to the Australian Health Ministers' Advisory Council: September 2012. Consultation paper - options for regulation of paramedics. (Online) 2012. Available: http://www.acem.org.au/getattachment/c808f6cb-12c9-415a-8604-aed91cb730c4/Submission-on-options-for-regulation-of-paramedics.aspx (Accessed 30 April 2014).
27. Eburn M. Ambulance Service Amendment Act 2013 (Tas). (Australian Emergency Law blog). (Online) 2014. Available: http://emergencylaw.wordpress.com/2014/01/24/ambulance-service-amendment-act-2013-tas (Accessed 24 April 2014).
28. South Australia Government. South Australian Bills: Health Practitioner Regulation National Law (South Australia) (Protection of Title - Paramedics) Amendment Bill 2013. (Online) 2013. Available: http://www.austlii.edu.au/au/legis/sa/bill/hprnlaotpab2013973/ (Accessed 24 April 2014).
29. Paramedics Australasia. Paramedic role descriptions. (Online) 2013. Available: http://www.paramedics.org/content/2009/07/PRD_211212_WEBONLY.pdf (Accessed 5 May 2014).
30. Bonnar A. Offshore medic or offshore OHN? Occupational Health 1994; 46(1): 24-25.
31. Mearns K, Hope L, Ford MT, Tetrick LE. Investment in workforce health: exploring , the implications for workforce safety climate and commitment. Accident Analysis & Prevention 2010; 42(5): 1445-1454.
32. , ,, , Council of Ambulance Authorities. Regulation of paramedics. (Online) 2012. Available: http://www.caa.net.au/attachments/article/127/2012_Regulation_of_Paramedics_CAA_Submission_Final.pdf (Accessed 2 May 2014).
33. FitzGerald G, Bange R. Defining a regulatory framework for paramedics: a discussion paper. Journal of Emergency Primary Health Care 5(2). (Online) 2007. Available: http://ro.ecu.edu.au/jephc/ (Accessed 5 May 2014).
34. Berger E. Telemedicine: has its time come? Annals of Emergency Medicine 2010; 56(5): A15-A17.
35. Norman JN, Ballantine BN, Brebner JA, Brown B, Gauld SJ, Mawdsley J, et al. Medical evacuations from offshore structures. British Journal of Industrial Medicine 1988; 45(9): 619-623.
36. Aslop P. Provision of the training of offshore medics. Journal of Paramedic Practice 2011; 3(1): 48-49.
37. Safriet BJ. Closing the gap between can and may in health-care providers'scopes of practice: a primer for policymakers. Yale Journal on Regulation 2002; 19(2): 301-334.
38. Mulholland P. A comparison of the practice of rural and urban paramedics: bridging the gap between education, training, and practice. Master of Medical Science thesis. Hobart, Tas: University of Tasmania, 2010.
39. Mulholland P, O'Meara P, Walker J, Stirling C, Tourle V. Multidisciplinary practice in action: the rural paramedic - it's not only lights and sirens. Journal of Emergency Primary Health Care 7(2). (Online) 2009. Available: http://ro.ecu.edu.au/jephc/ (Accessed 5 May 2014).
40. Australian Institute of Health and Welfare. Older Australia at a glance. (Online) 2007. Available: http://www.aihw.gov.au/publication-detail/?id=6442468045&libID=6442468043 (Accessed 5 May 2014).
41. Australian Defence Force. Defence jobs: Combat paramedic. (Online) n.d. Available: http://www.defencejobs.gov.au/army/jobs/CombatParamedic (Accessed 7 May 2014).
42. Scott J, Lucas R, Snoots R. Maritime medicine. Emergency Medicine Clinics of North America 1997; 15(1): 241-249.
43. Phillips JC. Medical support by a team of doctors to offshore paramedics. Journal of the Royal College of General Practitioners 1987; 37(297): 168-169.
44. Aalund LR. Other facets of remote medicine. The Oil and Gas Journal 1996; 94(18): 47-48.
45. Duffy B. Dental problems in the offshore oil and gas industry: a review. Occupational Medicine 1996; 46(1): 79-83.
46. Mills D. A year in the life of a remote medic. Journal of Paramedic Practice 2011; 3(5): 260-262.
47. Cox RAF. Medical services to offshore drilling. Injury 1970; 1(3): 217-225.
48. Aalund LR. Oil companies focus on emergency care for expats in Russia. The Oil and Gas Journal 1996; 94(18): 33-36.
49. Bourke L, Humphreys JS, Wakerman J, Taylor J. Understanding rural and remote health: a framework for analysis in Australia. Health & Place 2012; 18(3): 496-503.
50. Wakerman J. Defining remote health. Australian Journal of Rural Health 2004; 12(5): 210-214.
51. Reeve C, Pashen D, Mumme H, De La Rue S, Cheffins T. Expanding the role of paramedics in northern Queensland: an evaluation of population health training. Australian Journal of Rural Health 2008; 16(6): 370-375.
52. Measham TG, McKenzie FH, Moffat K, Franks DM. An expanded role for the mining sector in Australian society? Rural Society 2013; 22(2): 184-194.
53. Wakerman J, Humphreys JS. Sustainable workforce and sustainable health systems for rural and remote Australia. The Medical Journal of Australia 2012; 1(3): S14-S17.
54. Hou X-Y, Rego J, Service M. Review article: paramedic education opportunities and challenges in Australia. Emergency Medicine Australasia 2013; 25(2): 114-119.
55. Council of Ambulance Authorities. Accredited courses. (Online) 2013. Available: http://www.caa.net.au/education/accredited-courses (Accessed 5 May 2014).
56. Reynolds L. Contextualising paramedic culture. In: P O'Meara, C Grbich (Eds). Paramedics in Australia: contemporary challenges of practice. Frenchs Forest, NSW: Pearson Education Australia, 2009; 28-43.
57. Hawks SR, Hammond RL. Tackling stress management from all sides. Journal of Emergency Medical Services 1990; 15(9): 50-57.
58. Mulholland P, O'Meara P, Walker J, Stirling C, Tourle V. Multidisciplinary practice in action: the rural paramedic - it's not only lights and sirens. Journal of Emergency Primary Health Care 2009; 7(2).
59. Thompson J, Drummond C. Exploring paramedic patient assessments. Journal of Paramedic Practice 2013; 5(6): 342-347.
60. O'Meara P, Ruest M, Stirling C. Community paramedicine: higher education as an enabling factor. Australasian Journal of Paramedicine 2014; 11(2).
61. O'Meara P, Tourle V, Stirling C, Walker J, Pedler D. Extending the paramedic role in rural Australia: a story of flexibility and innovation. Rural and Remote Health 12(2): 1978. (Online) 2012. Available: www.rrh.org.au (Accessed 5 May 2014).
62. La Trobe University. University handbook 2014: Bachelor of Paramedic Practice/Bachelor of Public Health Promotion. (Online) 2014. Available: http://www.latrobe.edu.au/handbook/2014/undergraduate/health-sciences/single-degrees/bparpracpubhlthprom.htm.htm (Accessed 7 May 2014).
63. University of Canberra. Graduate Certificate in Remote Industrial Health. Course description. (Online) 2012. Available: http://www.canberra.edu.au/coursesandunits/course?course_cd=178JA (Accessed 5 May 2014).
64. Royal College of Surgeons of Edinburgh. Remote and offshore medicine. Programme overview. (Online) 2013. Available: http://www.rcsed.ac.uk/education/academic-programmes/remote-and-offshore-medicine.aspx (Accessed 5 May 2014).
65. Nottingham University Hospitals. Offshore medic. Course description. (Online) 2013. Available: http://www.nuh.nhs.uk/our-services/services/clinical-skills-and-competency-centre/training/external/offshore-medic/ (Accessed 5 May 2014).
66. Martin J. The challenge of introducing continuous professional development for paramedics. Journal of Emergency Primary Health Care 4(2). (Online) 2006. Available: http://ro.ecu.edu.au/jephc (Accessed 5 May 2014).
67. Mair F, Fraser S, Ferguson J, Webster K. Telemedicine via satellite to support offshore oil platforms. Journal of Telemedicine & Telecare 2008; 14(3): 129-131.
68. Australian Health Ministers' Advisory Council. Final report: options for regulation of unregistered health practitioners. (Online) 2013. Available: http://www.aasw.asn.au/document/item/4692 (Accessed 2 May 2014).
69. Ambulance Service of New South Wales. Paramedics. (Online). Available: http://www.ambulance.nsw.gov.au/about-us/Paramedics.html (Accessed 1 June 2014).
70. Paramedics Australasia. Australasian competency standards for paramedics. (Online) 2011. Available: http://www.paramedics.org.au/content/2011/10/PA_Australasian-Competency-Standards-for-paramedics_July-20111.pdf (Accessed 2 May 2014).
71. Council of Ambulance Authorities. Paramedic professional competency standards v.2. (Online) 2010. Available: http://caa.net.au/downloads/ppcs.pdf (Accessed 2 May 2014).
72. Mallard AS. EMS offshore. A new horizon for paramedics. Journal of Emergency Medical Services 1991; 16(10): 50-52, 54.
73. Baker D. Offshore medicine. Emergency Medical Services 2001; 30(3): 57-58.
74. Moulton Barrett D. Health care. Oil rig medicine: Is 40 hours' training enough? Canadian Medical Association Journal 1983; 128(12): 1438-1441.
75. Anscombe DL. Healthcare delivery for oil rig workers: telemedicine plays a vital role. Telemedicine and e-Health 2010; 16(6): 659-663.
76. Polsky S, Krohmer J, Maningas P, McDowell R, Benson N, Pons P. Guidelines for medical direction of prehospital EMS. Annals of Emergency Medicine 1993; 22(4): 742-744.
77. Dittrick P. Offshore care on line. The Oil and Gas Journal 2009; 107(39): 16.
78. Sood S, Mbarika V, Jugoo S, Dookhy R, Doarn CR, Prakash N, et al. What is telemedicine? A collection of 104 peer-reviewed perspectives and theoretical underpinnings. Telemedicine and e-Health 2007; 13(5): 573-590.
79. Webster K, Fraser S, Mair F, Ferguson J. A low-cost decision support network for electrocardiograph transmission from oil rigs in the North Sea. Journal of Telemedicine & Telecare 2008; 14(3): 162-164.
80. Väisänen O, Mäkijärvi M, Silfvast T. Prehospital thrombolysis perfomed by a ship's nurse with on-line physician consultation. Resuscitation 2005; 64(2): 233-236.
81. Brebner JA, Norman JN, Page JG, Ruddick-Bracken H. Research based training for the nurse practitioner. Accident & Emergency Nursing 1995; 3(2): 92-94.
82. Boniface KS, Shokoohi H, Smith ER, Scantlebury K. Tele-ultrasound and paramedics: real-time remote physician guidance of the Focused Assessment With Sonography for Trauma examination. The American Journal of Emergency Medicine 2011; 29(5): 477-481.
83. MacNeil M. Offshore medic training: a university initiative. Occupational Health 1987; 39(10): 306-307.
84. Davidson RG. Paramedics at work. Emergency offshore. Nursing Times 1982; 78: 98-100.
85. Australian Health Practitioner Regulation Agency. The National Boards. (Online) 2013. Available: http://www.ahpra.gov.au/Health-Professions.aspx (Accessed 5 May 2014).
86. Eburn M. New law for ambulance services in Tasmania - update. (Australian Emergency Law blog). (Online) 2013. Available: http://emergencylaw.wordpress.com/2013/09/07/new-law-for-ambulance-services-in-tasmania-update/ (Accessed 24 April 2014).
87. Sheather R. Professionalisation. In: P O'Meara, C Grbich (Eds). Paramedics in Australia: contemporary challenges of practice. Frenchs Forest, NSW: Pearson Education Australia, 2009; 62-83.
88. Campeau AG. Why paramedics require 'theories-of-practice'. Journal of Emergency Primary Health Care 6(2). (Online) 2008. Available: http://ro.ecu.edu.au/jephc/ (Accessed 5 May 2014).


