full article:
A study using participatory action research to explore Indigenous Australians' perspectives of H1N1
This study's multidisciplinary team of researchers set out to influence change in the Australian national pandemic plans. A national study was conducted to explore the views of Aboriginal and Torres Strait Islander people about their experiences with H1N1 using a qualitative participatory action research (PAR) framework1. Aboriginal and Torres Strait Islander community-controlled organisations and health services were involved in the implementation, interpretation and monitoring of the project. The research team designed the study to have PAR framework across multiple sites in Australia. The study used qualitative research methods to collect and analyse information from Aboriginal and Torres Strait Islander participants who had experienced the 2009 H1N1 pandemic (H1N109). Community-based researchers were selected from all participating communities and trained in qualitative research methods. The overarching principles were to develop and maintain strong relationships with communities and organisations, to engage in genuine and open dialogue about the research and to align with national ethical standards. The aims of the study were to:
- identify barriers to the implementation of current containment strategies for H1N109 in rural and remote Aboriginal and Torres Strait Islander communities
- develop culturally appropriate and effective containment strategies for H1N109 and future pandemics in these communities, modified where possible by the experience of the pandemic.
The H1N109 influenza pandemic resulted in higher incidence in New Zealand Maori and Pacific Islanders and greater morbidity in Indigenous populations in the Americas, New Zealand and Australia2. Hospitalisations and deaths from H1N109 were three to six times more common in Indigenous peoples than non-Indigenous peoples living in the same regions3-7. A higher prevalence of diabetes, obesity, asthma, chronic obstructive pulmonary disease and pregnancy in Indigenous communities may have contributed to the higher risks of severe disease. Social disparity, institutionalised racism and differences in access to culturally safe health services also contributed to delayed appropriate treatment3,8. However, a new study has identified a possible biological explanation for greater susceptibility in Australian Aboriginal people to various strains of influenza9.
During the 2009 H1N1 pandemic, the national pandemic influenza plans frequently masked or neglected the lives, needs and interests of disadvantaged groups within the population10,11. The result of this neglect was to further disadvantage the people most likely to require protection from a pandemic12.
Health researchers have long advocated better understanding of important social aspects of the prevention and response to infectious disease outbreaks, including influenza. However, published research and understanding in this field falls significantly behind that of non-communicable diseases13. Social aspects of communities such as cultural values, importance of norms, strong family ties and social networks may impede or facilitate pandemic risk reduction efforts14. Understanding these values and planning from the perspective of the at-risk population is important, but for this to be effective it is essential that the planning is done with respectful engagement of vulnerable communities15.
Choice of methodology
PAR is recognised as a method of research that may be more acceptable to Australian Aboriginal and Torres Strait Islander people, and was supported by the community research partners involved in this project15-17. PAR differs from other research methods in that it seeks to bring about positive change, not simply investigate or describe an issue. In addition, the research process is based on equal and collaborative involvement of the community and participants affected by the issue18-21.
Historically, research on Aboriginal and Torres Strait Islander peoples, and Indigenous people in other countries, has been deemed inappropriate as researchers sought to collect and describe the data without providing benefits to the people or communities researched22. The Aboriginal researchers employed on this project were acutely aware of the practice of researchers taking information from community members without giving anything back19.
PAR offers a way to make the research meaningful for a community18, being based on an action cycle that assists in improving processes for addressing issues from the communities' perspectives23,24. The research team applied a PAR approach that was collaborative, participatory and based on equal partnerships between Aboriginal and Torres Strait Islander community members, organisations, research assistants and researchers. It was driven and owned jointly by the community and the researchers, and involved a two-way respectful conversation that fed into both the process and the outcome of the research. Rather than a linear model of researcher-led data retrieval and analysis, PAR is a cyclical process of planning, acting, observing and reflecting (Fig1). This design enabled each new collection of data in the H1N109 project to be grounded in reflections formed on the previous data.
Historically, research has not been a positive experience for Indigenous communities25. Researchers have a responsibility to cause no harm, but traditional forms of research have been a source of distress for Indigenous peoples due to inappropriate methods and practices23,26. PAR offers a way to make the research meaningful for the community and enables an action research cycle that assists in improving processes for addressing issues, such as pandemic influenza, from the communities' perspectives.
PAR is increasingly recognised as useful for health research in marginalised groups like Indigenous populations27. It has potential to reduce the negative effects that conventional research has had on Indigenous peoples28,29 by recognising the community knowledge power base.
The recognition that power is directly related to knowledge lies at the very heart of the collaborative participatory research project. For public health researchers who are committed to reducing the health inequalities that are associated with social disadvantage, this approach offers a strategy that embraces self-determination, encourages and even demands ongoing consultation and negotiation, and provides opportunities for capacity-building and empowerment in the communities involved in the research30.
Importantly, when communities seek control of the research agenda, and actively engage in the research, they are establishing themselves as more powerful agents27. With the increasing use of PAR approaches to address public health issues, there is potential for bridging the gap between research and practice in addressing social issues and creating conditions that facilitate people's control over the determinants of their health31. A key strength of PAR is the partnership between participants' real world knowledge and researchers' methodological expertise31. Partnerships that are formed with marginalised and vulnerable populations need to ensure that concepts of cultural humility and cultural safety are integrated, and maintain mutual respect and trust31. PAR stages included engagement with community groups, organisations, individual and group interviews, yarning (talking) circles and community reports. Strong community engagement at different sites meant that the engagement processes, although based on standard principles of research, was adapted to the differing local contexts and stakeholders.
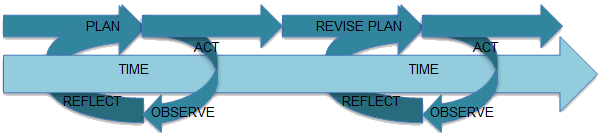
Figure 1: Participatory action research23.
During this study, the research team identified important and novel aspects of the methods.
Multidisciplinary team and Aboriginal and Torres Strait Islander researchers
The research team comprised senior and early-career researchers, Aboriginal and Torres Strait Islander and non-Aboriginal and Torres Strait Islander people. Members came from a wide variety of disciplines including medicine, veterinary science, epidemiology, public health, anthropology, health promotion, nursing and education. In common was a commitment to, and a long history of working on, applied research prioritised with Aboriginal and Torres Strait Islander communities. Members also shared a value of social justice for Aboriginal and Torres Strait Islander people. All researchers had established relationships with at least one other person on the team and some had long histories of working together. There was an assumed complementarity of knowledge and skills in the team, an assumption that was tested and confirmed as the research progressed.
Aboriginal and Torres Strait Islander researchers were recruited from their local communities across Australia: three were employed in community-controlled health services; two were government health employees, and four were community members with diverse employment histories. Researchers of both genders were employed at each research site and included senior community members and young people. These researchers had different knowledge and skill sets and different educational backgrounds17. Training workshops were held in various locations to train Aboriginal and Torres Strait Islander researchers in qualitative research methods. These workshops were led by very experienced qualitative researchers who had worked in remote Aboriginal communities for many years. The Aboriginal and Torres Strait Islander researchers collected qualitative data, advised on cultural and community protocols, and the research team collectively analysed this data.
Ethics
Human Research Ethics Committee (HREC) approvals were granted from universities and state authorities. HRECs included James Cook University (H3546) in Queensland, the Aboriginal Health and Medical Research Council (746/10) and the Hunter New England HREC (09/09/16/4.01) in New South Wales, and the Western Australian Aboriginal Health Ethics Committee (291 06/10). Under ethical research principles involving Aboriginal and Torres Strait Islander participants the additional ethics criteria required can be methodologically challenging in a number of ways. Gaining documented approvals and support from community-controlled organisations, local government and other agencies was required for this study. Additional ethical challenges included ensuring that local community protocols for consultations were followed and that data had local ownership32. This meant that in 2009 multisite approval processes across jurisdictions and universities were necessary. Additionally, all ethics applications had to document how the project adhered to specific ethical principles centered on spirit and integrity and included responsibility, respect, reciprocity, equality and survival and protection32.
Capacity building
An important foundation for the research strategy was the capacity building of all team members involved in PAR. A series of training workshops that focused on qualitative research methods, data collection and data analysis were conducted in three of the research sites in Australia. These workshops were conducted at key points of the research journey, just in time for it to be relevant and meaningful to the researchers33. The training workshops were attended by chief and associate investigators, and research assistants, at various locations. This collaborative process highlighted another two-way learning approach to the research which placed equal value on respecting the values of Indigenous and non-Indigenous members' cultures, knowledge, processes and worldviews34.
The multidisciplinary nature of the research team and the various stages of their research careers necessitated different levels of support, mentoring and capacity development. The research team members benefited from their learning from the Aboriginal and Torres Strait Islander researchers by challenging their own assumptions and approaches to research. At the same time, community researchers gained a better understanding of the formal research process and the opportunities available from the higher education system. Support, guidance and mentoring provided the community researchers with opportunities to help them plan their future careers and education pathways.
Sampling
As is appropriate for this type of qualitative research, the Aboriginal and Torres Strait Islander researchers operated within existing social and work networks to identify study participants. This approach enabled participants from across the communities to be involved. A purposive sampling technique was used in the selection of participants, which included Aboriginal community-controlled health services staff and Aboriginal and Torres Strait Islander community members of mixed ages and genders.
Collective research process
The PAR cycles included engagement with community groups, organisations, individual and group interviews, yarning circles and feedback presentations for community reports. The sampling framework and data collection questions were developed by the research team as part of the training workshops. A collective and collaborative process was used involving all researchers at all stages of data collection, data coding, data analysis and reporting. Using a thematic analysis process at each site the data were coded inductively with a thematic coding scheme. Then a collective and collaborative process was used where the researchers identified and defined themes across all the data. As the combined themes and concepts emerged, further data reduction and interpretation occurred. This culminated in a novel, systematic and innovative group analysis and writing process. The PAR framework allowed Aboriginal and Torres Strait Islander researchers to become equal and valued members of the research team. Despite numeracy and literacy levels, the Aboriginal and Torres Strait Islander researchers were well supported in their capacity development. Two major challenges occurred, one during data collection and the other during analysis. During interviews, community-based researchers initially did not probe participants for further information on areas of common understanding. During analysis the other challenge was deciding on how to document community-based strategies that were deemed ineffective (on the basis of evidence) in reducing transmission of influenza but were perceived effective by the community.
Research action and feedback
The participants spoke of the need to enter into a respectful dialogue with Aboriginal and Torres Strait Islander communities, to discover what communities wanted to know before authorities told them their views. It was considered important that researchers, government agencies and health services listen deeply to what is really meant, and then share the information that is needed by the communities.
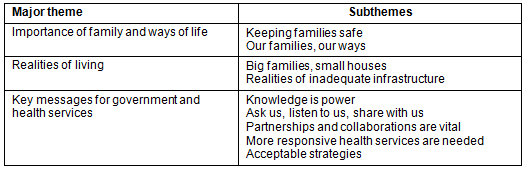
An interim report was developed and presented to participants and organisations involved in the study to closely consider and comment on what was found as an essential activity of the PAR framework34. The data gathering process and the dissemination of the interim report provided many opportunities for the PAR process to flow from the research. New or modified ways to reduce risk from H1N109 were adopted by families, health services, community groups and government departments involved in the research. Examples included families increasing hand washing and reducing direct social contact when sick, a childcare centre ensuring that sick children did not attend the centre, health services planning for outreach services and a state health department engaging more closely with the Aboriginal community-controlled health sector. Self-determination and empowerment are key values that the research action and feedback was able to support. These values are integral in the development of Indigenous health. The major themes and subthemes from the study (Table 1) were confirmed throughout the PAR framework.
Table 1: Major study themes and subthemes
Vulnerable or neglected groups and populations often become more disadvantaged during epidemics and other emergencies35. Typically their special needs are ignored because health system responses are designed to maximise efficiency and produce the best outcomes for the majority of the population36. The research framework that was adopted allowed the voices of vulnerable groups to be heard, listened to and appropriate action taken in respectful, collaborative partnerships. The most effective responses in this study were seen in relationships that had been established over decades between Aboriginal medical services and investigators, while research relationships established specifically for the purposes of the project were less successful because of changes in personnel.
A number of strengths of the research framework used became clear throughout the project. The perspectives of Aboriginal and Torres Strait Islander people were paramount to the research process. Respect of and for Aboriginal and Torres Strait Islander cultures underpinned the project. PAR is an approach that may work towards de-colonising research27,28,37 and bringing about sustainable change. Further strengths of PAR included having people working together with different capabilities and skills but complementary experiences and directions, research training, mentoring and capacity building of the whole team, and actions to reduce the risk of H1N109 being implemented as the research progressed.
In this study, the PAR framework enabled a collaborative partnership between Aboriginal and Torres Strait Islander community members, organisations, and novice and experienced researchers. The collection and analysis of this data formed an interim report that captured the main findings so that health services and organisations could use this to improve their responses to pandemic influenza. Throughout the entire project, Aboriginal and Torres Strait Islander community research assistants were actively involved in research capacity training, data collection, group analysis of the data, and writing up of the research findings. The important role they played in the research project has been described previously17. The findings from this research were used as an advocacy tool with government to include Aboriginal and Torres Strait Islander peoples in the National Pandemic Plan. This is a good example of how knowledge translation could look in practice.
Making the implicit explicit was both a strength and a challenge for the research team. At times, the Aboriginal and Torres Strait Islander researchers were placed at some risk when they explored issues that most often go unsaid in communities. As a result, when working with the data, the community researchers were able to provide a more complete translation of the concepts raised by the research.
If the project was to be repeated, the research team would be expanded to include a person allocated to coordinate community engagement at each site. Further, to enable deeper understandings to emerge and acceptance of new measures developed, all participants and groups would need to be fully engaged in the research process. Community organisations operate in dynamic and changing environments, therefore flexible engagement strategies are necessary. Developing strong mutually agreed frameworks for engagement may assist in this challenging process.
The initial results of this research have been published elsewhere and include a number of recommendations and strategies for government, health services and families1. An important focus of this article is the translational research framework38. Translational research contributes to informing practice and policy in Indigenous health38. Translational research is associated with the concept of knowledge translation developed in Canada and mandated by the Canadian Institutes of Health Research (CIHR)38,39. Within CIHR's 'knowledge to action process' model, a representation of knowledge translation, this article can be defined as the 'identify problem/identify, review and select knowledge' step39,40.
Actions to reduce the risk of pandemic influenza transmission in the community need to be driven by the understandings emerging from this research. The importance of family and community ways was a strong and recurring message for governments. The reality of life in Aboriginal and Torres Strait Islander communities differs from that of many non-Indigenous communities, and pandemic influenza strategies need to take account of these differences. The key messages to government and health services stemming from the research were that community engagement and partnership is vital, and health services need to be more responsive. In 2013, this study's research team was given the opportunity to provide feedback on the revised Australian Health Management Plan for Pandemic Influenza. The results of this research are being incorporated into the latest revisions of this plan.
The social aspects of communities, such as cultural values, importance of norms, strong family ties, and social networks, need to be integral in research methods for addressing issues in vulnerable populations. The model of research described here could provide a useful starting point for researchers who are working in these environments and with these populations, and argues for respectful engagement with communities as a cornerstone for this type of research.
Acknowledgements
The authors would like to thank the National Health and Medical Research Council, Hunter New England Aboriginal Health Partnership, Kimberley Aboriginal Medical Service Council, Mamu Health Service, Tamworth Aboriginal Medical Service, Armajun Aboriginal Medical Service, Palm Island Aboriginal Shire Council, Torres Shire Council and Torres Strait Island Regional Council.
References
1. Massey PD, Miller A, Saggers S, Durrheim DN, Speare R, Taylor K, et al. Australian Aboriginal and Torres Strait Islander communities and the development of pandemic influenza containment strategies: community voices and community control. Health Policy 2011; 103: 184-190.
2. Institute of Environmental Science and Research Limited (ESR). Seroprevalence of the 2009 influenza A (H1N1) pandemic in New Zealand. Client report FW10057, for New Zealand Ministry of Health. ESR: Wellington, 2010.
3. La Ruche G, Tarantola A, Barboza P, Vaillant L, Gueguen J, Gastellu-Etchegorry M. The 2009 pandemic H1N1 influenza and indigenous populations of the Americas and the Pacific. Eurosurveillance 2009; 14: 1-6.
4. Rudge S, Massey PD. Responding to pandemic (H1N1) 2009 influenza in Aboriginal communities in NSW through collaboration between NSW Health and the Aboriginal community-controlled health sector. New South Wales Public Health Bulletin 2010; 21: 26-29.
5. Flint SM, Davis JS, Su JY, Oliver-Landry EP, Rogers BA, Goldstein A, et al. Disproportionate impact of pandemic (H1N1) 2009 influenza on Indigenous people in the Top End of Australia's Northern Territory. Medical Journal of Australia 2010; 192: 617-622.
6. Kelly H, Mercer G, Cheng A. Quantifying the risk of pandemic influenza in pregnancy and Indigenous people in Australia in 2009. Eurosurveillance 2009; 14(50): 1-3.
7. Boggild A, Yuan L, Low D, McGeer A. The impact of influenza on Canadian First Nations. Canadian Journal of Public Health 2011; 102: 345-348.
8. Aldrich R, Zwi AB, Short S. Advance Australia Fair: social democratic and conservative politicians' discourses concerning Aboriginal and Torres Strait Islander peoples and their health 1972-2001. Social Science & Medicine 2007; 64: 125-137.
9. Qui Quiñones-Parra S, Grant EJ, Loh L, Nguyen THO, Campbell K, Tong S, et al. Pre-existing CD8+ T cell immunity to the novel H7N9 influenza A virus varies across ethnicities. Proceedings of the National Academy of Sciences 2014; 111(3): 1049-1054.
10. Garoon JP, Duggan PS. Discourses of disease, discourses of disadvantage: a critical analysis of National Pandemic Influenza Preparedness Plans. Social Science Medicine. 2008; 67(7): 1133-1142.
11. Miller A, Durrheim D. Aboriginal and Torres Strait Islander communities forgotten in new Australian Pandemic Action Plan: 'Ask us, listen to us, share with us'. eMJA 2010; 193(6): 316-317.
12. Connal L, Rogers WA, Braunack-Mayer A. Social justice and pandemic influenza planning: the role of communication strategies. Public Health Ethics 2008; 1: 223-234.
13. Cohen JM, Wilson ML, Aiello AE. Analysis of social epidemiology research on infectious diseases: historical patterns and future opportunities. Journal Epidemiology Community Health 2007; 61: 1021-1027.
14. Vaughan E, Tinker T. Effective health risk communication about pandemic influenza for vulnerable populations. American Journal of Public Health 2009; 99(2): 324-332.
15. Massey PD, Pearce G, Taylor KA, Orcher L, Saggers S, Durrheim DN. Reducing the risk of pandemic influenza in Aboriginal communities. Rural and Remote Health 9: 1290. (Online) 2009. Available: www.rrh.org.au (Accessed 10 October 2014).
16. Yunupingu B. 'A plan for gamma research' in Aboriginal pedagogy: Aboriginal teachers speak out. Geelong: Deakin University Press, 1991.
17. Kelly JM, Saggers S, Taylor K, Pearce G, Massey PD, Bull J, et al. 'Makes you proud to be black eh?': reflections on meaningful Indigenous research participation. International Journal for Equity in Health 2012; 11(40): 1-15.
18. Kemmis S, McTaggart R. Participatory action research: communicative action and the public sphere. In: NK Denzin, YS Lincoln (eds). The Sage handbook of qualitative research. 3rd ed. Thousand Oaks, CA: Sage Publications, 2005.
19. Stringer E, Genat W. Action research in health. Upper Saddle River, NJ: Pearson Merrill Prentice Hall, 2004.
20. Stringer E. Action research. A handbook for practitioners. Thousand Oaks, CA: Sage Publications, 1996.
21. Evans M, Miller A, Hutchinson P, Dingwall C. 'De-colonizing research practice: Indigenous methodologies, Aboriginal methods, and knowledge/knowing'. In: P Leavy (ed.) Oxford handbook of qualitative research. New York: Oxford University Press, 2014; 179-191.
22. Cochran PAL, Marshall CA, Garcia-Downing C, Kendall E, Cook D, McCubbin L, et al. Indigenous ways of knowing: implications for participatory research and community. American Journal of Public Health 2008; 98(1): 22-27.
23. Wadsworth Y. What is participatory action research? Action Research International, paper 2, 1998.
24. Whyte, WF. Participatory action research. Newbury Park: Sage, 1991.
25. Smith Tuhiwia L. Decolonizing methodologies: research and Indigenous peoples. London: Zed Books, 1999.
26. National Health and Medical Research Council. National statement on ethical conduct in human research. (Online) 2007. Available: http://www.nhmrc.gov.au/book/national-statement-ethical-conduct-human-research (Accessed 30 September 2013).
27. Baum F, MacDougall C, Smith D. Participatory action research. Journal of Epidemiology Community Health 2004; 60: 854-857.
28. Hecker R. Participatory Action Research as a strategy for empowering Aboriginal health workers. Australian and New Zealand Journal of Public Health 1997; 21: 7.
29. Matsuda JR, Creighton G, Nixon S, Frankish J. Building capacity for community based participatory research for health disparities in Canada: the case of partnerships in community health research. Health Promotion Practice 2011; 12(2): 280-292.
30. Pyett P. working together to reduce health inequalities: reflections on a collaborative participatory approach to health research. Australian and New Zealand Journal of Public Health 2007; 26: 332-335.
31. Cargo M, Mercer S. The value and challenges of participatory research: strengthening its practice. Annual Review of Public Health 2008; 29: 325-350.
32. National Health and Medical Research Council. Keeping research on track: a guide for Aboriginal and Torres Strait Islander peoples about health research ethics. (Online) 2006. Available: http://www.nhmrc.gov.au/guidelines/publications/e65 (Accessed 30 September 2013).
33. Leach A, Haun DE. Deliver the lesson now: just in time training. Medical Laboratory Observer 2003; 35(7): 42-47.
34. Miller A, Clough A, Durrheim DN, Pearce G, Broome J, Judd J, et al. Influenza studies with Aboriginal and Torres Strait Islander communities - keeping families safe. Project report on feasible containment strategies for swine influenza H1N1 in rural and remote Aboriginal and Torres Strait Islander communities. NHMRC grant number 601034. Unpublished community research report, James Cook University, 2010.
35. Hutton D. Putting the puzzle together: reducing vulnerability through people-focused planning. Radiation Protection Dosimetry 2009; 134(3-4): 193-196.
36. Jaspars S, Shoham J. Targeting the vulnerable: a review of the necessity and feasibility of targeting vulnerable households. Disasters 1999; 23(4): 359-372.
37. Israel B, Shulltz AJ, Parker EA, Becker AB. Review of community based research: assessing partnership approaches to improve public health. Annual Review of Public Health 1998; 19: 173-202.
38. Thomson N. Translational research and the Australian Indigenous. HealthInfoNet - working paper. (Online) 2012. Available: http://www.healthinfonet.ecu.edu.au/translational_research (Accessed 6 February 2015).
39. Tugwell P, Robinson V, Grimshaw J, Santesso N. Systematic reviews and knowledge translation. Bulletin of the World Health Organization 2006; 84(8): 643-651.
40. Graham ID, Logan J, Harrison MB, Straus SE, Tetroe J, Caswell W, et al. Lost in translation: time for a map? Journal of Continuing Education in the Health Professions 2006; 26(1): 13-24.





