The rate of potentially preventable hospitalisations for Aboriginal and Torres Strait Islander people in Australia is 4.9 times the rate for other Australians, with more than half (55%) of these hospitalisations being for chronic conditions1. Under-use of medicines contributes to poorer control of chronic disease states and higher hospital admissions, morbidity and mortality for Aboriginal and Torres Strait Islander people2,3.
The term 'Aboriginal' in this article is inclusive of all Australian Aboriginal and Torres Strait Islander peoples.
Factors that have an impact on Aboriginal people's engagement with health services and medicines are various. They may include the cost of multiple medicines, the distance to services, poverty, racism, dispossession, lack of control, the stigma associated with a diagnosis of chronic disease, educational disadvantage, shared crowded households, increased patient mobility and inadequate health professional support4,5. Compounding these may be language, health literacy and cultural issues, concurrent use of bush or traditional medicines, lack of continuity of care and the absence of strong relationships with health practitioners6. Failed patient-clinician interactions, poor healthcare delivery systems, complex medicine regimens and struggles with social and emotional wellbeing decrease the likelihood of effective management of medicines7,8.
The Aboriginal Health Service Remote Access (AHSRA) program was established in 1999, providing free Pharmaceutical Benefit Scheme (PBS) medicines, and so improving medication access, for remote Aboriginal people. Two other PBS co-payment schemes, the QUMAX or Quality Use of Medicines Maximised for Aboriginal People9 and the Close the Gap10 programs, commenced in 2008 and 2010 to provide non-remote Aboriginal people with financial assistance with their medicines. These programs, whilst reducing some financial barriers to medicine access, are not sufficient to address all barriers. Without improved understanding of medicines and increased medicine adherence, chronic disease will remain poorly controlled11,12. Engagement of patients in their healthcare goals, communication of medicine information and simplification of complex therapeutic medicine regimens also need to be achieved5.
Clinical pharmacists and the cognitive pharmacy services they deliver - such as patient medicine education, medicine reviews, drug interaction checking, dosage and adverse effect monitoring, medication reconciliation and clinical interventions - can make valuable contributions to improving health outcomes13. Pharmacists need to increase their understanding of Aboriginal culture, Aboriginal Health Services (AHSs) and their Aboriginal Health Worker (AHW) staff, and better understand the needs of their local community, in order to deliver effective primary health care to Aboriginal people and so maximise the therapeutics effects of prescribed medications14.
The Home Medicines Review (HMR) program15 is a cognitive pharmacy service, which was introduced in Australia in 2001 by the Australian Government. This home-based program is designed to assist patients to maximise the benefits of their medication regime and prevent the harmful consequences of medication misuse16. On a referral from a general practitioner (GP), an HMR trained and accredited pharmacist will visit the patient at home, and interview the patient about their medication. The pharmacist explains the medications, their usage and provides appropriate medication information to the patient. The pharmacist then prepares a report of their findings, using information provided by the patient, medical information provided by the GP and the patient's dispensing history from the pharmacy. The accredited pharmacist reports the findings and their recommendations to the referring GP. This report forms the basis of the Medication Management Plan, which the GP may implement with the patient on their next visit. The GP and pharmacist claim payment from Medicare Australia.
Most patients would benefit greatly from an HMR consultation after discharge from hospital, when medication confusion and incidents of medication misadventure increase. There may also be occasions when patients are unable to access primary healthcare services and consult a GP. For these reasons there has been some debate around the need for various health professionals to be permitted to initiate and refer patients for an HMR. To date, program rules still allow only GPs to refer patients for an HMR.
Home Medicine Reviews have been found to raise awareness of medication safety and ultimately reduce adverse events and unnecessary hospital admissions16. Lack of medication information often leads to failure of the patient to take their medicine correctly, which can in turn lead to therapeutic failure or unwanted/dangerous effects from medications5. An HMR creates an opportunity for the patient to receive medication counselling from an accredited pharmacist. The HMR is the perfect platform to improve medication concordance and reduce medication misadventure in those who have complex medication needs17,18. Whilst most HMR studies have found very positive consumer acceptance of the HMR program, some others have reported consumer ambivalence19.
Evaluations of the HMR program provided by consultants employed by the government16,20 identified that Aboriginal and Torres Strait Islander peoples had been 'underserviced' by the HMR program and are the most likely of all Australians to miss out on HMRs, despite having the highest rates of hospitalisation due to medication misadventure16,20. There is no accurate, accessible data documenting the number of HMRs being undertaken with Aboriginal patients; however, anecdotal evidence suggests that the number is still small, despite marginal increases as a result of some pharmacists working with AHSs during the implementation of the QUMAX program from 2008 to 2012. The 2007 Campbell report16 commissioned by Australian Government called for the urgent introduction of a more culturally appropriate model of HMRs and for expanded HMR services to Aboriginal people. To date these recommendations have not been implemented.
The goal of the present study was to explore Aboriginal and Torres Strait Islander perspectives of the HMR program and their suggestions for an 'improved' or more readily accessible model of service. This article reports the analysis of the views of the Aboriginal and Torres Strait Islander people who participated and informs policy and medication initiatives for these Australians.
Very little research has been conducted in the area of medication management and cognitive pharmacy services for Aboriginal and Torres Strait Islander peoples or the role of pharmacists in Aboriginal health. Published research has been reviewed and has been used to situate this study.
This is an exploratory study of Aboriginal and Torres Strait Islander patients' perceptions of the HMR model. An Aboriginal advisory group was established to guide the design and data collection phases of this study. The advisory group members consisted of community elders, an AHS chief executive officer and two health administrators. The group advised on engagement with AHSs, focus group management, language, culture and question design.
As research and researchers have had a poor reputation in many Indigenous settings21, AHSs were chosen as the sites for recruitment of patients and data collection because AHSs provided a culturally safe environment22. Shyness and distrust of the unknown, non-Aboriginal researcher was diminished by holding the focus groups in the familiar surroundings of the AHS.
Aboriginal shyness, poverty, effects of long-term discrimination and powerlessness have been identified as barriers to generating information with Aboriginal participants23. Focus group methodology was chosen because it allows minimally structured 'yarning' that gathers information through conversation and storytelling. Storytelling is the preferred communication method for many Aboriginal people24.
Each AHS was given verbal then written information about the project, and each management and board was asked to approve participation in the study. Aboriginal staff members were asked to assist with patient recruitment and focus group organisation and they acted as cultural brokers, managing the relationship between participants and the researcher. They were vital to establishing trust and cooperation.
Eighteen semi-structured focus groups were conducted with Aboriginal and Torres Strait Islander patients (n=102) at 11 AHSs in five Australian states and territories: Queensland, Northern Territory, South Australia, New South Wales and Victoria. The sites were selected for diversity and included urban (n=2), regional (n=3), rural (n=2) and remote (n=4) settings. They ranged across language groups and they varied in governance, size and service delivery models. The AHSs prescribed and dispensed medicines under different schemes, including AHSRA, QUMAX and Close the Gap, and two sites had in-house pharmacists. Three northern Australian sites were chosen to include Torres Strait Islander people representation. Table 1 indicates the number of participants in each focus group.
The researcher specifically targeted some AHSs where HMRs were being conducted so that she could explore participants' HMR experiences at these sites and thus 20% of focus group participants in this research had received an HMR. The overall percentage of Aboriginal and Torres Strait Islander peoples having had an HMR in Australia is much less than this figure.
Participants of AHSs who were multiple medication users and understood English were recruited to the study by AHS staff. Although no formal demographic data was collected, the researcher recorded in field notes that 75% of participants were female, approximately 90% of participants appeared to be aged over 40 years, and about 70% appeared literate in written English.
Participants were given written material explaining the study by AHS staff, before consent was sought. The researcher confirmed understanding, willingness to participate and permission to record proceedings at the beginning of each focus group before formal consent was obtained.
Two types of focus groups were conducted. Seven focus groups were conducted for people who had already used the HMR program (User, n=23 ) and 11 focus groups were conducted for people who had not had an HMR (Non User, n=79). All focus groups were conducted by the first author. The challenge of conducting high-quality focus groups was not underestimated and analysis of participant interaction as well as content was recorded in field notes after each focus group.
In the User focus groups HMR Users were asked to reflect on their experience of having an HMR, and then on their satisfaction or lack of satisfaction with their experience, as well as what they believed might be barriers and facilitators for other Aboriginal and Torres Strait Islander people in accessing the HMR program. Non User focus groups received a description of the HMR program rules and processes. The group then discussed their perceptions of the HMR program, the barriers and facilitators of the HMR model and strategies to increase accessibility of the HMR program for Aboriginal and Torres Strait Islander people.
Focus group questions (Table 2) were modified slightly as a result of early groups and concurrent analysis, to ensure all content raised in early groups was explored.
Focus group recordings were de-identified and transcribed verbatim. Transcripts were coded and analysed for themes. Analysis occurred concurrently. Themes were identified by repetition of words and phrases, and shared meanings, evident across data. Finding were discussed with other researchers to ensure the meanings generated were agreed and mutually shared.
Focus groups continued and concepts were explored until no new findings were being generated and thus saturation of data occurred25. Field notes and summaries written at the end of each focus group were incorporated into the analysis.
Questions about the same issues produced similar findings in different settings despite urban-rural variability. The homogeneity of most findings was surprisingly strong across the varied settings and groups, adding strength to the findings. There was some small variability relating to more general issues of remoteness, such as lack of availability of health professionals and increased usage by patients of local Aboriginal language. There was no significant difference in understanding of medicines or perceptions of the HMR program across the varied geographical settings and thus it has not been necessary to discuss findings according to location.
Table 1: Number of participants at focus groups
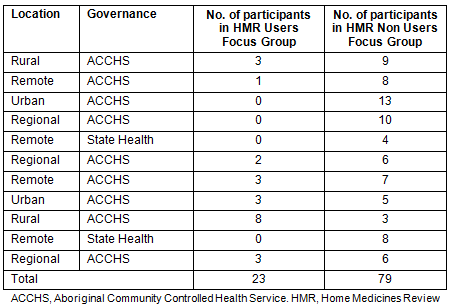
Table 2: Core Home Medicines Review questions to Users and Non Users

Ethics approval
Ethics approval was sought and granted from the University of Sydney Human Research Ethics Committee (11504), the Aboriginal Health and Medical Research Council (New South Wales), the Menzies School of Health Research (Northern Territory, South Australia) and the Aboriginal Health Research & Ethics Committee (Victoria).
Most participants reported difficulties in managing their multiple medicines, and many expressed a desire to better understand their medicines26.
Most of the User participants reported that the HMR interview had been very useful for learning more about their medicines. However, many reported that they found the process confusing and confronting, as no one had explained what was to happen or for what purpose an HMR was being conducted. Most commented they would have liked some follow-up from the pharmacist after the HMR interview, such as a phone call, written report, written medicine information or another meeting.
The majority of the Non User participants believed that HMR could be a useful tool for Aboriginal people, if the process was managed in a culturally appropriate way. Six participants felt the need for an HMR implied 'you are not doing the right thing'.
User and Non User participants suggested ways the HMR program needed to be implemented to increase the uptake of this program by Aboriginal and Torres Strait Islander people as cultural issues and living circumstances are not currently addressed by the rules governing the process.
Findings from the Aboriginal patients about HMR are grouped into two main themes and their subthemes. The main themes are cultural considerations and adapting the HMR process to suit Aboriginal people's needs.
Cultural considerations for Home Medicines Reviews with Aboriginal patients
'It works to be organised by the health service': Most participants, both HMR Users and Non Users, were adamant that they would only agree to having an HMR if it was suggested and organised by their AHS, because 'then you can trust that the pharmacist is appropriate and that it [HMR] is for your benefit'. The AHS was described as a culturally safe service that understood the needs of its Aboriginal patients.
Aboriginal people's shyness was seen as a barrier to some patients having a HMR. 'Some people are shy, some people feel threatened by people they don't know'. The patients often relied on the AHS to assist them organise appointments, navigate the health system and broker relationships with health professionals.
The health service people are people you trust, people that look after you, people you know. If they organise it then it must be okay. Also they know about our family, where to find us and can organise transport and the right time.
'It can't just be anyone': As long as the HMR interview had been organised by the AHS the participants were happy to engage with the pharmacist, even when he/she was a 'stranger'.
Participants felt that it was important for the AHS to form a working relationship with a specific pharmacist, so that this pharmacist could learn to relate to AHS staff and patients: 'I would just like to be given one pharmacist.' It was important that the pharmacist had a good attitude and respected Aboriginal patients. Many felt it would be desirable, and some felt imperative, for this pharmacist to receive cultural awareness training from the AHS: 'It can't just be anyone. They have to be culturally appropriate or they could offend someone.'
'Sometimes you don't want someone in your home': Participants were evenly divided about whether they would be comfortable to have an HMR interview occur in their home or prefer to have it conducted at the health service or clinic. Some discussed the convenience of having it at home for the very elderly and disabled, and others said the benefits included 'you're comfortable in your own home' and that 'in my house I'll open up, I'm the boss kind of thing.' However, half of respondents were adamant that 'sometimes you don't want someone in your home' and stated that 'a lot would rather have it at the clinic' because 'a lot of people don't like strangers in their house' and 'Aboriginal people do get shamed if they haven't cleaned up' and that 'I have a large family coming and going and sometimes it would be noisy and not very private.'
All participants agreed that to give people having an HMR 'a choice (of location) would be a good idea'. Some participants discussed the possibility of having an HMR in the garden, in the park or down by the river. The majority felt that a private space at the AHS was probably a very suitable option for many Aboriginal patients. The majority of study participants agreed that the name 'Home Medicines Review would put some people off having one because they think they have to have it in the home'.
'The health worker is the key': Most participants indicated that they would like to have an AHW present at the HMR interview with the pharmacist. It was felt that an AHW would break down barriers and aid understanding. They 'break the ice' and 'they know about you' and 'diffusing people's fear helps them to understand'. It was also felt that they would aid communication by prompting the right questions, translating and interpreting jargon and explaining concepts. 'The health worker breaks things down for us, so that we can understand'.
The AHW, as the most 'continuous' member of the healthcare team, was seen as a useful resource for follow-up questions and reminders. 'They can help us remember to take our medicines' and 'they can ask the doctor for us' and 'they can explain it later if we don't understand'.
Having an AHW present at a HMR interview was seen as even more imperative when the pharmacist was of differing gender to the patient. A male AHW should attend a male patient and a female AHW attend a female patient to ensure that sensitivities around 'men's business' and 'women's business' are respected. Most stated that the gender of the pharmacist didn't matter as long as they were accompanied by the appropriate AHW. However, a few male participants stated that they would not discuss private health matters with a female pharmacist, even if an appropriate AHW was present.
It was considered important to give patients the choice of a specific AHW to attend the HMR interview. Sometimes the AHW was a community member and the patient stipulated, 'I don't want her to know my business' and 'sometimes because it's not nice in front of that health worker if they're not comfortable with that health worker' or if there is 'family friction'. The choice of which health worker should be present was very important.
Group Home Medicines Reviews: Family members, carers and other community members were often seen as integral to the management of medication and assisting in reminding patients to take their medicines. A number of participants said when having an HMR they would prefer a family member or carer also to be present: 'Sometimes it would be good to have someone else there to help me remember.' It was suggested that family members and carers, as nominated by the patient, should be formally invited to attend the HMR so they feel 'welcome'. A small number of participants also stated they would like to have their HMR or a medication session in a group: 'Being with other people with similar problems helps us to learn. They might ask things we need to know about.' They commented that it would be 'great to get together with other diabetics to see if they have the same issues.'
Adapting Home Medicines Reviews to Aboriginal patients' needs
Explaining the process: Focus group participants who had not had an HMR had little or no awareness of the HMR program. All the participants felt the lack of awareness and promotion of the HMR program were contributing factors to the low uptake of the HMR program by Aboriginal people. 'What is an HMR?' and 'No one knows that it is available' were common sentiments. It was also suggested that the name 'Home Medicines Review' would deter some patients as they would not be comfortable with having a pharmacist visit them at home.
Participants who had had an HMR spoke of some 'nerves' and apprehension before the pharmacist visit and some stated that they were unclear about the purpose of the pharmacist's visit. More communication and fact sheets outlining the process would have been helpful.
A few participants expressed the view that more consultation and communication between government and community around health program design would have been 'helpful'.
About half of the participants said they would like follow-up, and feedback from the HMR pharmacist after the interview, and a few even said they would like to see a copy of the report sent to the doctor.
Most participants who had had an HMR thought that an HMR was just a 'chat' with a pharmacist about their medicines. Only two participants realised that the pharmacist wrote a report for the doctor and that subsequent medication changes might relate to the pharmacist's recommendations. Mostly they felt that, 'Afterwards nothing happened. I don't think anything changed.'
Referrals: Participants felt that many patients were unlikely to take referral documents from a doctor to the pharmacy and then directly liaise with an accredited pharmacist to make an appointment, as is suggested in the HMR program rules. They felt that, 'If it's too much mucking around for us, it won't happen.'
Many participants, and all those from the more remote areas, suggested that an AHW or AHS nurse should be able to write an HMR referral, as it was the AHWs and nurses who knew them 'best' and were the health professionals with whom they interacted most often. It was the AHWs and nurses who offered continuity of care, whilst many doctors 'come and go'.
Participants felt that it was the AHW that best understood if they needed assistance with medication management, assistance with transport to attend the HMR interview, which family member to invite and when to make an appointment with the GP. Because the AHW was seen as the person who would be mostly likely to follow up after the HMR, it was viewed as important that the AHW was also involved in and aware of the HMR referral.
Medication specialists: AHWs were seen as the most accessible and most approachable of the health professionals at the AHS and a few participants commented, 'we need a health worker that specialises in medicines.'
We need health workers to be trained as experts, to be able to have this knowledge to link between the pharmacy, the doctor and the patient's journey in the community so that all the questions can be answered.
Written resources: None of the participants who had had an HMR had received any written material. Most believed, 'it would have been good if the pharmacist had left some written information, simple to understand, to show to my family and read later'. A number of participants throughout the focus groups commented on the need for simple, jargon-free, culturally appropriate medication resources to assist in the understanding of their medication and health management. Many participants expressed the desire for a comprehensive medicines list that could be kept in their wallet or bag.
Discussion
This study showed that many Aboriginal people were keen to have a pharmacist working within their health service. They felt that a pharmacist working with their AHS would be someone with whom they could develop rapport and trust, and who would be available to deliver medication reviews, medical education and other clinical services to Aboriginal patients.
The current HMR model and associated rules are restrictive and not conducive to utilisation of the program by Aboriginal and Torres Strait Islander people. Issues of referral, organisation, location, reimbursement and follow-up need to be addressed to increase the number of Aboriginal people who can use this program. As in studies with non-Aboriginal patients, barriers to HMR included pride and independence, confidence issues with an unknown pharmacist, concerns regarding the home visit, and lack of information about the program27. There are facilitators identified in this study that may increase the uptake of HMRs with Aboriginal and Torres Strait Islander patients, improve health and have economic benefits.
Home Medicines Review rules dictate that referrals can only be written by a GP15. Previous studies have identified that GPs' lack of understanding of the HMR process and GPs' time constraints have resulted in low HMR initiation rates28,29. In remote areas of Australia, GPs are often scarce or on short-term contracts, resulting in lack of rapport and lack of continuity of patient care. Remote GPs need to prioritise acclimatisation, cultural orientation, medical emergencies and acutely ill patients, as well as manage chronic disease. Referrals for HMRs are very low in such areas. In urban and rural AHSs, the GPs are often overloaded with complex patients with high disease burden. Long and complex patient consultations may result in low prioritisation of HMRs and low numbers of HMR referrals. Participants in the study identified that they more often discussed their medicines with the nurses or AHWs, with whom they more frequently engaged, rather than with their GPs. Aboriginal Health Workers and nurses are best placed to identify patients at risk of medication mismanagement and therefore program rules need to allow AHWs and AHS nurses to write an HMR referral.
The present study confirmed the important role that AHSs play in the primary healthcare for Aboriginal and Torres Strait Islander people30. Aboriginal Health Services were described as comfortable, safe environments that understood and addressed Aboriginal patients' needs, and acted as the broker of services to the community. Study participants identified that it was the AHS who should organise the HMR interview and organise follow-up after the interview. It was through the AHS that culturally appropriate information about the HMR process and written information about medicines should be distributed. It was the AHS, commonly described as the clinic, that was identified as the most culturally safe place for the HMR interview to occur. Studies show that having pharmacists integrated in a clinic or medical practices has strong patient support and results in improved patient outcomes31,32.
The role of AHWs was seen as pivotal to the success of an HMR by the study participants, reinforcing previous literature describing the important role of AHWs in brokering communication between health professionals and Aboriginal patients33. Aboriginal Health Workers were described by participants as the health professionals who could best identify the patient need for an HMR, the most trusted organisers, the most effective communicators and the most likely ongoing source of information about medicines. There is currently no reimbursement for AHW involvement in the HMR process. Often, AHWs work across numerous programs within the AHS, including early childhood, sexual health, mental health and healthy lifestyle promotions. They are often overburdened with work commitments, and often attend to community health needs out of work time. To ensure the AHWs' time is allocated to medication issues and involvement in HMRs, the HMR program needs to be able to reimburse the AHS for their involvement in medication management roles. A number of participants suggested the need for some AHWs to specialise in medicines, reinforcing previous studies suggesting more AHW medication training34,35.
Group medical consultations are a new innovation being used to enhance patient engagement and to address issues of GP shortage and overload due to ageing populations and increasing burdens of chronic disease36,37. Patients who have received care in groups reported improvement in health outcomes, improved sense of trust in the physician, and tended to report better coordination of care, better community orientation and more culturally competent care38. A few participants of the present study identified that they would like to receive medication information as a group. They felt an HMR interview could be a more effective education session if conducted with a group of patients with similar medical conditions, and with the pharmacist, AHW and possibly the nurse and doctor also participating.
Study participants strongly supported the HMR program, stating that the HMR program or similar could greatly assist Aboriginal people manage their medicines and improve their health. More funding and significant time and resources need to be invested in medication management programs for Aboriginal patients. The current HMR program has been designed with little or no understanding of Aboriginal culture and little or no input from Aboriginal people. There is a need to design and implement cognitive pharmacy services that can effectively deliver medication assistance in urban, rural and remote settings and to Aboriginal and Torres Strait Islander communities. The funding for this program needs to be uncapped to ensure viability, sustainability and confidence is invested in this program.
The study was limited by English language requirement for participation. The participants were selected by the AHS staff, not randomly drawn or selected. It is suspected that AHS staff approached those with whom they had stronger relationships and those they felt would be effective focus group participants. This may have caused some bias. A wide range of sites were used to try to maximise variability. Despite diversity of settings, there was considerable consonance across responses. The views of Aboriginal people who do not attend AHSs have not been captured and therefore it is difficult to extrapolate findings to all Aboriginal and Torres Strait Islander people. However, the sample size was larger and more diverse than for many studies with Aboriginal participants and therefore has merit.
Increasing HMRs for Aboriginal and Torres Strait Islander people has the potential to increase medication knowledge, medication adherence and therefore improve chronic disease management.
The current HMR program rules impede rather than facilitate HMRs for Aboriginal people. Changes needed to increase the uptake of HMRs by Aboriginal and Torres Strait Islander people include promotion to increase awareness of HMRs; providing leaflets to patients outlining the HMR process; allowing an HMR referral to be written by a nurse or AHW; facilitating the HMR interview by allowing choice of location, AHW and family member; reimbursing AHSs for staff organisation and attendance of HMR interviews; and providing HMR follow-up to patients. It is suggested that the HMR program be remodelled and renamed after consultation with Aboriginal and Torres Strait Islander people.
Solutions that would assist with health workforce shortages, managing the increasing burden of chronic disease and funding shortfalls, include employing pharmacists within AHSs, training AHWs to specialise in medicines and reimbursing pharmacists to conduct individual or group medication education sessions.
If the Australian Government is serious in addressing the health inequities that exist for Aboriginal and Torres Strait Islander people it needs to invest in medication education strategies that will assist Aboriginal people to manage their medicines. The HMR program could be a useful tool but tailoring of this program is needed to increase awareness, accessibility, acceptability and effectiveness for Aboriginal and Torres Strait Islander people. Until the government engages Aboriginal people to assist in health program design it will continue to exclude Aboriginal people from mainstream programs, such as HMR and continue to increase the inequity.
Acknowledgements
Sincere thanks to the members of the Aboriginal advisory panel, the AHS staff and focus group participants who gave their time so generously to assist this research.
Travel for this project, 'Strategies to Increase Home Medicines Review for Aboriginal and Torres Strait Islander People', was partially funded by a Small Projects Grant from the Department of Health and Ageing as part of the Research and Development Fund managed by the Pharmacy Guild of Australian under the Fourth Community Pharmacy Agreement 2010.
References
1. Australian Institute of Health and Welfare. Access to health services for Aboriginal and Torres Strait Islander people. (Online) 2011. Available: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=10737418951&libID=10737418 (Accessed 1 December 2013).
2. Australian Institute of Health and Welfare. Expenditure on health for Aboriginal and Torres Strait Islander people 2008-9. Health and welfare expenditure series no. 44, cat. no. HWE 53. (Online). Available: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=10737419253&libID=10737419252 (Accessed 1 December 2013).
3. Kelaher M, Dunt D, Taylor-Thomson D, Harrison N, O'Donoghue L, Barnes T, et al. Improving access to medicines among clients of remote area Aboriginal and Torres Strait Islander Health Services. Australian & New Zealand Journal of Public Health 2006; 30: 177-183.
4. Murray R. Prescribing issues for Aboriginal people. Australian Prescriber 2003; 26: 106-109.
5. Davidson PM, Abbott P, Davison J, Digiacomo M. Improving medication uptake in Aboriginal and Torres Strait Islander peoples. Heart, Lung & Circulation 2010; 19: 372-377.
6. Commonwealth of Australia. The effectiveness of special arrangements for the supply of Pharmaceutical Benefits Scheme (PBS) medicines to remote area Aboriginal Health Services. (Online) 2011. Available: http://www.aph.gov.au/Parliamentary_Business/Committees/Senate/Community_Affairs/Completed_inquiries/2010-13/pbsmedicines/report/index (Accessed 1 December 2013).
7. Larkin C, Murray R. Assisting Aboriginal patients with medication management. Australian Prescriber 2005; 28: 123-125.
8. Emden C, Kowanko I, De Crespigny C, Murray H. Better medication management for Indigenous Australian: findings from the field. Australian Journal of Primary Health 2005; 11: 80-90.
9. National Aboriginal Community Controlled Health Organisation. QUMAX - Quality Use of Medicines Maximised for Aboriginal and Torres Strait Islander Peoples Program. (Online). Available: http://www.naccho.org.au/promote-health/qumax/ (Accessed 1 December 2013).
10. Department of Human Services. Closing the Gap - PBS co-payment measure. (Online) 2012. Available: http://www.medicareaustralia.gov.au/provider/pbs/pharmacists/closing-the-gap.jsp (Accessed 1 December 2013).
11. Price Waterhouse Coopers for Medibank Private. Health literacy, implications for Australia. (Online) 2011. Available: http://www.medibank.com.au/Client/Documents/Pdfs/Health_literacy_-_implications_for_Australians.pdf (Accessed 1 December 2013).
12. World Health Organization. Adherence to long term therapies: evidence for action. (Online) 2003. Available: http://www.who.int/chp/knowledge/publications/adherence_report/en/ (Accessed 1 December 2013).
13. Tan ECK, Stewart K, Elliott RA, George J. Pharmacist services provided in general practice clinics: a systematic review and meta-analysis. Research in Social & Administrative Pharmacy 2014; 10(4): 608-622.
14. Stoneman J, Taylor SJ. Pharmacists' views on Indigenous health: is there more that can be done? Rural & Remote Health; 7(3): 743 (Online) 2007. Available: www.rrh.org.au (Accessed 1 December 2013).
15. Medicare Australia. Home Medicines Review (HMR). (Online) 2013. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/medication_management_reviews.htm (Accessed 30 October 2013).
16. Campbell Research & Consulting. Home Medicines Review Program. Qualitative research project. Final report. (Onine) 2008. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/hmr-qualitative-research-final-report (Accessed 3 January 2014).
17. Ponniah A, Shakib S, Doecke CJ, Boyce M, Angley M. Post-discharge medication reviews for patients with heart failure: a pilot study. Pharmacy World & Science 2008; 30: 810-815.
18. Kairuz T, Bye L, Birdsall R, Deng T, Man L, Ross A, et al. Identifying compliance issues with prescription medicines among older people: a pilot study. Drugs & Aging 2008; 25: 153-162.
19. Carter SR, Moles R, White L, Chen TF. Patients' willingness to use a pharmacist-provided medication management service: the influence of outcome expectancies and communication efficacy. Research in Social and Administrative Pharmacy 2012; 8(6): 487-498.
20. Urbis Keys Young. Evaluation of the Home Medicines Review Program - pharmacy component. (Online) 2005. Available: http://beta.guild.org.au/uploadedfiles/Medication_Management_Reviews/Overview/Urbis%20Keys%20Young%20evaluation.pdf (Accessed 3 January 2014).
21. Smith LT. Decolonising methodologies. Research and Indigenous peoples. 2nd ed. London and New York: Zed Books Ltd, 2012.
22. Belfrage M. Why "culturally safe" health care? Medical Journal of Australia 2007; 186: 537-538.
23. Leipoldt E. Aboriginal people with disability and their use of advocacy: a phenomenological approach (Bachelor of Social Science Honours thesis). Perth, WA: Edith Cowan University, 1998.
24. Gorman D, Toombs M. Matching research methodology with Australian indigenous culture. Aboriginal and Islander Health Worker Journal 2009; 33(3): 4-7.
25. Walker JL. The use of saturation in qualitative research. Canadian Journal of Cardiovascular Nursing 2012; (22): 37-46.
26. Swain L, Barclay L. They've given me that many tablets, I'm bushed. I don't know where I'm going. Australian Journal of Rural Health 2013; 21: 216-219.
27. White L, Klinner C, Carter S. Consumer perspectives of the Australian Home Medicines Review Program: Benefits and barriers. Research in Social & Administrative Pharmacy 2012; 8: 4-16.
28. Emblem G, Miller E. Home Medicines Review - the how and why for GPs. Australian Family Physician 2004; 33: 49.
29. Roughead E, Pratt N, Peck R, Gilbert A. Improving medication safety: influence of a patient specific prescriber feedback program on rate of medication reviews performed by Australian general practitioners. Pharmacoepidemiology and Drug Safety 2007; 16: 797-803.
30. Baeza JI, Lewis JM. Indigenous health organizations in Australia: connections and capacity. International Journal of Health Services : Planning, Administration, Evaluation 2010; 40: 719-742.
31. Rigby D. Collaboration between doctors and pharmacists in the community. Australian Prescriber 2010; 33: 191-193.
32. Freeman C, Cottrell W, Kyle G, Williams I, Nissen L. Integrating a pharmacist into the general practice environment: opinions of pharmacist's, general practitioner's, health care consumer's, and practice manager's. BMC Health Services Research 2012; 12: 229.
33. Abbott P, Gordon E, Davison J. Expanding roles of Aboriginal health workers in the primary care setting: seeking recognition. Contemporary Nurse 2007; 26: 66-73.
34. Hamrosi K, Taylor SJ, Aslani P. Issues with prescribed medications in Aboriginal communities: Aboriginal health workers' perspectives. Rural & Remote Health; 6: 557 (Online) 2006. Available: www.rrh.org.au ( Accessed 1 December 2013).
35. McRae M, Taylor SJ, Swain L, Sheldrake C. Evaluation of a pharmacist-led, medicines education program for Aboriginal Health Workers. Rural & Remote Health; 8: 946. (Online) 2008. Available: www.rrh.org.au (Accessed 1 December 2013).
36. Bronson DL, Maxwell RA. Shared medical appointments: increasing patient access without increasing physician hours. Cleveland Clinic Journal of Medicine 2004; 71: 369-370.
37. Yehle KS, Sands LP, Rhynders PA, Newton GD. The effect of shared medical visits on knowledge and self-care in patients with heart failure: a pilot study. Heart & Lung 2009; 38: 25-33.
38. Clancy DE, Brown SB, Magruder KM, Huang P. Group visits in medically and economically disadvantaged patients with type 2 diabetes and their relationships to clinical outcomes. Topics in Health Information Management 2003; 24: 8-14.

