full article:
Aboriginal and Torres Strait Islander people have poorer health status than non-Aboriginal Australians1,2. They are significantly under-represented in the health sector generally3, and in medical professions specifically4,5. Medical schools therefore have a social accountability mandate to provide culturally safe contexts in order to enable Aboriginal and Torres Strait Islanders to engage in medical education with confidence6, and to ensure that present and future clinicians provide health services to Indigenous Australians in a respectful and empowering manner7. All medical schools in Australia are reference group members of the Leaders in Indigenous Medical Education (LIME) Network, which seeks to ensure quality and effectiveness of teaching and learning of Indigenous health in medical education.
Cultural safety has been grappled with for many years; however, work done by Maori nurses with the inclusion of cultural safety and training into nurse education has paved the way for many countries to examine culture safety training8. Cultural safety within health professional practice is 'regardful' of people's unique qualities9. Rather than seeing the patient as the 'exotic other', cultural safety requires instead for the health professional to view themselves as 'other' and consider how they can change and adapt their practice to suit their patient's needs, being ever mindful of power differentials8. Whether a service is culturally safe must be determined by the patients, not the providers of the service10.
The Australian Indigenous Doctor's Association views cultural safety on a continuum11. Cultural awareness, which involves understanding difference, is the first step in the learning process. Cultural sensitivity, where self-exploration occurs, is the next step. Cultural safety is the final outcome. Transition between these steps is recognised as a dynamic, multidimensional process where an individual's place in the continuum can change depending on the setting or community.
In recent years cultural safety training programs have become commonplace across the Australian health sector with the aim of increasing knowledge and understanding of Aboriginal history, belief systems, values and concepts of health; and links between the social determinants of health and relationship to health outcomes7. All tertiary-level health professional education curricula have Australian Medical Council accreditation requirements mandating the incorporation of Aboriginal and Torres Strait Islander health into curricula12. Professional colleges have followed this lead with the mandated requirements around Aboriginal health13,14.
Despite all these formal training opportunities, it is well recognised that learners tend to 'internalise and perpetuate the patterns of behaviour that surround them'15. Attitudes towards Aboriginal and Torres Strait Islanders can be resistant to change, because change requires reflection on the premise of our own 'belief, judgement and feeling' to transform our world view16. Mezirow argues that such fundamental changes in frame of reference require a number of key phases including a disorientating dilemma leading to critical assessment of assumptions, recognising that others have negotiated similar change and that the process of transformation is shared, learning new knowledge and exploring options for new roles, and renegotiating established relationships and negotiating new relationships16.
This project aimed to draw on the collectivist approach of Aboriginal people to measure and reflect on the cultural climate of a rural clinical school (RCS) and then, recognising the importance of good company to share the learning journey, design strategies to build on the cultural safety of the organisation16.
Carr's previously validated survey tool was chosen for this study17. The Carr study evaluated medical and dental students' experiences of learning and attainment of university learning outcomes relating to Aboriginal and Torres Strait Islander health. These questions describe four main constructs: social priority, health services provision, preparedness and ability, and future commitment to Aboriginal health. The original survey consisted of 25 questions based on a five-point Likert scale, where 1 was 'strongly disagree' and 5 was 'strongly agree'. In Carr's study, eight questions were excluded because they had not shown test-retest reliability17, In this project two further questions were excluded because they were not considered relevant to all proposed survey participants. Fifteen of the original questions were included in the survey.
Clinician teachers, academics and professional (administrative) staff from a single RCS were invited by email to participate in the online survey. Clinician teachers were defined as clinicians who had a formal affiliation with the RCS such as academic status or a casual appointment.
The power of the study was calculated as >90% for a 0.4 point difference in a five-point Likert scale with standard deviation (SD) of 0.8 and α error 5% if the sample size was 40. Data analysis was conducted using the Statistical Package for the Social Sciences (SPSS; http://www.spss.com). Likert scale means and standard deviations were calculated assuming Likert scores represented a continuous variable between 1 and 5. Data were found to be linear, so one-way between groups ANOVA analysis was conducted to compare the effect of occupational group on Likert scale scores for cultural safety. Post-hoc Fisher's least significant difference (LSD) tests were performed to reduce the risk of type 1 errors.
Ethics approval
Ethics approval was obtained from Southern Adelaide Clinical Human Ethics Research Ethics Committee (project number 023.13).
Of the emails that were sent out to potential participants (N=65), a total of 41 participants completed the survey (response rate 63%). Participants comprised 29.3% clinical teachers, 29.3% academic staff and 41.5% professional staff (Table 1).
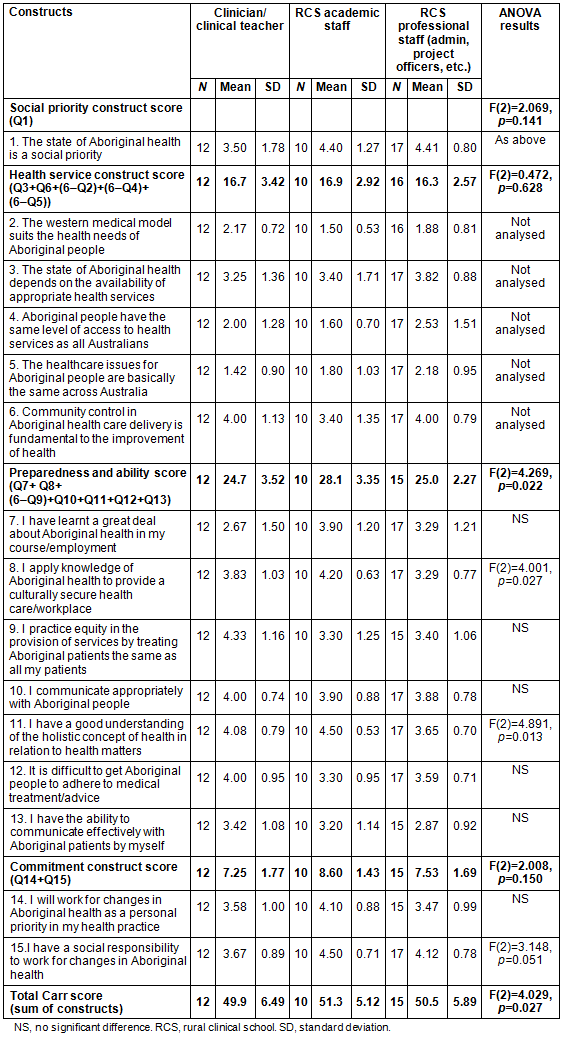
There was a significant effect on overall cultural safety measurement using Carr's tool between the three occupational groups (F(2)=4.029, p=0.027). Posthoc comparisons using Fisher's LSD test indicated that clinical academics demonstrated cultural safety (mean=51.3, SD=5.12) to a greater extent compared with both clinician teachers (mean difference = 6.67, 95% confidence interval (CI)=1.59-11.75, p=0.012) and university professional staff (mean difference=5.53, 95%CI=0.69-10.38, p=0.026). Results are outlined in Table 2 and described in detail below.
Table 1: Participant groups
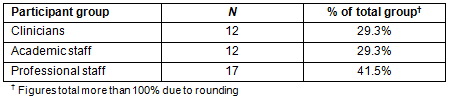
Table 2: Cultural climate findings
Social priority
All three participant groups demonstrated clear agreement that the state of Aboriginal health is a social priority (mean=4.17, SD=1.30) with no statistically significant difference between the groups (F(2)=2.069, p=0.141).
Health service provision
For the health services construct, questions were scored positively or negatively depending on whether they reflected a student learning objective, or the opposite to this. There were no statistically significant differences between the three groups of participants for the construct of health services (F(2)=0.472, p=0.628), with the whole cohort recognising the fundamental role of community control in Aboriginal healthcare delivery and affirming that Aboriginal health depends on the availability of appropriate health services.
Preparedness and ability
Within the preparedness and ability construct there was a difference between the groups (F(2)=4.269, p=0.022). Posthoc comparisons using the Fisher's LSD test indicated that academics have a higher overall score for preparedness (mean=28.1, SD=3.35) than clinicians (mean difference=3.43, 95%CI=0.81-6.06, p=0.012) and university professional staff clinicians (mean difference=3.10, 95%CI=0.61-5.60, p=0.017).
Academic staff were more likely to agree that they apply their knowledge of Aboriginal health to provide culturally secure care/workplaces (mean= 4.20, SD=0.63), (F(2)=4.001, p=0.027) than university professional staff (mean difference=0.906, 95%CI=0.24-1.58, p=0.010). They also agreed more strongly that they have a good understanding of the holistic concept of health (mean=4.50, SD=0.53), (F(2)=4.891, p=0.013) than university professional staff (mean difference =0.853, 95%CI=0.29-1.41, p=0.004).
Future commitment to Aboriginal health
Within the future commitment construct there was no significant difference between the groups (F(2)=2.008, p=0.150). There was a lower level of agreement by clinicians to having a social responsibility to work for changes in Aboriginal health (mean=3.67, SD=0.89). Although ANOVA results did not reach statistical significance (F(2)=3.148, p=0.051), posthoc comparisons using Fisher's LSD test indicated that clinicians had a lower score when compared to academics (mean difference= -0.833, 95%CI= -1.51 to -0.16, p=0.017).
Discussion
Westwood and Westwood proposed that in order to increase awareness of how culture impacts on health service delivery and improves health outcomes for Aboriginal peoples it is important that training be specific to local area and community needs7. Intersectional frameworks recognise the lived experience and assumptions that individuals bring to their life and working environment. These frameworks posit that individuals hold multiple social locations, which interact with one another to uniquely shape the health views, needs and experiences of the individuals from minority groups18. Intersectorial frameworks are heavily influenced by socioeconomic status, political influences, educational outcomes and cultural norms. They provide a way of exploring cultural identity. This theoretical perspective suggests that position within an organisation is an important factor when considering meaning perspectives.
The authors hypothesised that clinicians, academics and professional staff hold different educational, cultural and political status within the RCS organisation and therefore may experience and contribute to the cultural climate of the RCS differently. Exploring collective understandings of the health of Aboriginal people in clinician, academic and professional staff groupings could discover important differences between these groups, and allow tailored educational approaches to be developed. Limitations of this study include that Carr's original tool is validated for an undergraduate medical and dentistry program and is for curriculum evaluation. The authors postulate, however, that it is valid to assess whether the cultural climate of an RCS supports Aboriginal health learning objectives within the medical curriculum, or whether the cultural climate of the organisation represents a hidden curriculum that needs to be addressed.
Implications for clinicians
In comparison to the clinical academics studied, clinicians were less prepared as a group to acknowledge differences between Aboriginal and non-Aboriginal peoples. They did not consistently recognise the influence of autonomy and power differentials on the Aboriginal people's health status or their capacity to adhere to standardised medical advice. This one-dimensional approach to illness may explain why clinicians seemed less confident that they understood the holistic concept of health in relation to Aboriginal patients, and why they did not express being strongly driven by social responsibility to work for changes in Aboriginal health.
One hypothesis for the one-dimensional approach to illness is that the theory and practice of medicine has been dominated by the positivist bioreductionist discourse of medical science and that this professional culture can blind clinicians to how the social determinants of health influence positional power within the health system, and prevent a patient-centred approach to the practice of medicine19. Racial non-concordance has previously been demonstrated to negatively impact on doctors' understanding of their patients20. Challenges to patient-centred care of Aboriginal people may be further accentuated for overseas-trained doctors providing clinical care in this area of rural Australia - some may still be grappling with the gap between the culture of their own country and that of Australia.
Thackrah and Thompson state that 'Attention of cultural complexity, structural determinants of inequality and power differentials within health care settings ... provides a more expansive notion of cultural competence and a nuanced understanding of the role of culture in the clinic'21. Intersectional frameworks seek to provide a model to explore how people's capacity for self-determination is multi-dimensional and includes education, political and cultural factors18. The authors have interpreted the clinician findings as demonstrating the need to build on the culture of medicine by focusing cultural safety training for clinicians on locally specific social determinants of health, and the collaborative partnership between patients and clinicians in achieving health outcomes. A clinical focus such as using simulation scenarios involving local community members as standardised patients is proposed. This could provide clinicians with opportunities to examine their own intersectionality, and learn interviewing skills that will uncover patient intersectionality specific to local Aboriginal peoples7. Using Mezirow's Transformative Learning theory, the theoretical foundation for this tailored approach to cross-cultural training aims to facilitate participants to undergo a disorientating dilemma so clinicians become more critically reflective of their own assumptions22.
Implications for academic staff
When compared to clinicians the academic staff in the RCS central to this study demonstrated a more detailed understanding of the complexities of culture and the impact that this has on health outcomes. It is unclear if these perspectives attracted clinicians to academic positions within the RCS or whether the RCS organisational focus was responsible for nurturing these views; however, higher education institutions have traditionally engaged in critical discourse around power. Academic clinicians recognised their social responsibility to work toward 'closing the gap'. Academic staff still had a strong affiliation to their professional norms, and have leadership roles within the clinical setting with students and often more broadly within the profession. They have a responsibility to hold the profession to account for the health outcomes of Aboriginal people, and need to be supported to facilitate critical reflection in those they lead. The authors propose that academic clinicians seek to develop dual roles of leadership within the medical profession and followership23 within the Aboriginal communities with which they work. Followership is a complex skill perhaps best conceptualized as a dance partner in a waltz: too strong and the partner takes the lead; too weak and the leader is not supported in the dance. Using Mezirow's Transformative Learning theory, the authors recognise that formal partnerships with local Aboriginal community leaders or Aboriginal health workers would provide good company, where these cultural experts could coach and mentor clinical academics.
Implications for professional staff
Compared with the academic staff, professional staff in the RCS were more neutral about preparedness and ability questions such as 'good understanding of holistic concept of health' and 'applying knowledge to promote secure workplace'. This may be because RCS professional roles are not directly clinical and there are a range of staff levels, with fewer survey participants involved in leadership roles. This survey did not capture professional staff activities including local Aboriginal community engagement and actively supporting Aboriginal medical students. The authors propose that professional staff can be supported to participate in supported cultural immersion with local Aboriginal groups, for example through participating annually in the annual National Aboriginal and Islander Day Observance Committee (NAIDOC) Week activities and regularly hosting the local Aboriginal women's group at the RCS. Mezirow's Transformative Learning theory offers the theoretical perspective for this strategy by recognising the importance of 'trying on different selves' and renegotiating relationships16.
This study recognises the importance of fostering an organisational climate that has cultural safety as a core value. Mezirow's Transformative Learning theory has a preference for learning where students and professional groups can question, challenge and rejuvenate their personal values24.
Despite formal curriculum measures, medical students are most likely to adopt the cultural attitudes of the people in the environment around them. This study sought to measure the cultural climate of clinicians, academics and professional staff in a single RCS and develop tailored strategies to improve the cultural safety of the organisation based on Mezirow's Transformative Learning theory. Only through tailored approaches to cross-cultural training opportunities is it likely that participants will be able to engage with the material and reflect upon how cultural climate impacts on the health and wellbeing outcomes of Aboriginal people.
References
1. Bramley D, Hebert P, Jackson R, Chassin M. Indigenous disparities in disease-specific mortality, a cross-country comparison: New Zealand, Australia, Canada, and the United States. New Zealand Medical Journal 2004; 117(1207): 1-16.
2. Hill K, Barker B, Vos T. Excess Indigenous mortality: are Indigenous Australians more severely disadvantaged than other Indigenous populations? International Journal of Epidemiology 2007; 36(3): 580-589.
3. West R, Usher K, Foster K. Increased numbers of Australian Indigenous nurses would make a significant contribution to 'closing the gap' in Indigenous health: What is getting in the way? Contemporary Nurse 2010; 36(1-2): 121-130.
4. Lawson KA, Armstrong R, Van Der Weyden MB. Training Indigenous doctors for Australia: shooting for goal. Medical Journal of Australia 2007; 186(10): 547.
5. Schwenke TM. Training Aboriginal doctors. Medical Journal of Australia 1990; 153(6): 309-310.
6. Garvey G, Rolfe IE, Pearson SA, Treloar C. Indigenous Australian medical students' perceptions of their medical school training. Medical Education 2009; 43(11): 1047-1055.
7. Westwood B, Westwood G. Aboriginal cultural awareness training: policy v. accountability - failure in reality. Australian Health Review 2010; 34: 423-429.
8. Ramsden I. Cultural safety and nursing education in Aotearoa and Te Waipounamu. Doctoral dissertation, Victoria University of Wellington.
9. Papps E, Ramsden I. Cultural safety in nursing: the New Zealand experience. International Journal for Quality in Health Care 1996; 8(5): 491-497.
10. Rigby W, Duffy E, Manners J, Latham H, Lyons L, Crawford L, et al. Closing the Gap: cultural safety in Indigenous health education. Contemporary Nurse 2010; 37(1): 21-30.
11. Australian Indigenous Doctor's Association. Cultural safety for Aboriginal and Torres Strait Islander doctors, medical students and patients: position paper. (Online). Available: http://www.aida.org.au/wp-content/uploads/2015/03/Cultural_Safety.pdf (Accessed 7 March 2014).
12. Australian Medical Council. Standards for assessment and accreditation of primary medical programs by the Australian Medical Council. (Online) 2012. Available: http://www.amc.org.au/joomla-files/images/Accreditation/FINAL-Standards-and-Graduate-Outcome-Statements-20-December-2012.pdf (Accessed 7 March 2014).
13. Australian College of Rural and Remote Medicine. ACRRM Primary Curriculum 2013. Available: https://www.acrrm.org.au/misc/curriculum/Default.htm (Accessed 7 March 2014).
14. Royal Australian College of General Practice. RACGP Curriculum Statements 2011. (Online) 2011. Available: http://curriculum.racgp.org.au/statements/aboriginal-and-torres-strait-islander-health/ (Accessed 7 March 2014).
15. Suchman AL, Williamson PR, Litzelman DK, Frankel RM, Mossbarger DL, Inui TS. Toward an informal curriculum that teaches professionalism. Journal of General Internal Medicine 2004; 19[5p2]: 501-504.
16. Mezirow J. Understanding transformation theory. Adult Education Quarterly 1994; 44(4): 222.
17. Carr S, Paul D, Bazen J. Integrated undergraduate Aboriginal health curricula: validating a program evaluation survey tool. Focus on Health Professional Education 2011; 12(3): 34-40.
18. Powell Sears K. Improving cultural competence education: the utility of an intersectional framework. Medical Education 2012; 46(6): 545-551.
19. Malterud K. The art and science of clinical knowledge: evidence behind measures and numbers. Lancet 2001; 358(9279): 397-400.
20. Street RL, Haidet P. How well do doctors know their patients? Factors affecting physician understanding of patients' health beliefs. Journal of General Internal Medicine 2011; 26(1): 21-27.
21. Thackrah R, Thompson S. Refining the concept of cultural competence: building on decades of progress. Medical Journal of Australia 2013; 199(1): 35-38.
22. Berger J. Dancing on the treshold of meaning: recognizing and understanding the growing edge. Journal of Transformative Education 2004; 2: 336-351.
23. Collinson D. Rethinking followership: a post-structuralist analysis of follower identities. Leadership Quarterly 2006; 17(2): 179-189.
24. Greenhill J, Poncelet A. Transformative learning through longitudinal integrated clerkships. Medical Education 2013; 47: 333-341.



