In this article the concept of the rural academic general practice in Australia is explored. Recent Australian general practice history is described with a particular focus on education and research activity. There is a strong demand for an increase in training capacity in rural general practice to accommodate recent increases in learner numbers and to address the current rural general practice workforce shortage. There is also a need to address the dearth of general practice research. The aim of this study was to develop a rural academic general practice framework to assist practices in developing both comprehensive educational activity and a strong research focus.
General practices in Australia
General practices in Australia have traditionally arisen from small businesses focused primarily on health service delivery by general medical practitioners. Since the early 1990s, Australia has seen a steady change in the range of clinical services educational activity undertaken by general practices. This has in part been driven by the Australian Government General Practice Strategy1 and been supported by financial incentives2. There has been a move towards larger practices with an increasing range of allied health services. Practice accreditation against formal standards and compulsory vocational training for general practice has been introduced. Vocational training for general practice in Australia is an apprenticeship model largely based in private general practices. Australian General Practice Training funds vocational training of general practitioners (GPs) through a network of 17 regional training providers (RTPs) that work to the standards of the Royal Australian College of General Practice and the Australian College of Rural and Remote Medicine. As well as the opportunity to host registrars in general practice vocational training, practices can host medical students in community-based placements and interns on rotation.
While many practices in Australia now engage in teaching3, there remains a dearth of active involvement in research4. Publication rates for general practitioners in Australia are low, sitting at 2-5% of the rates achieved by their physician and surgical colleagues5. The Australian Government has endeavoured to support primary care research through the Primary Health Care Research, Evaluation Development (PHCRED) strategy established in 20006. This has largely been a top-down approach by funding universities to undertake primary health research and has not been reflected by an increase in rural primary health publication rates6.
An important but limited initiative supported by PHCRED has been the formation of practice-based networks to facilitate research activity at the level of the general practice and other primary care services7. These networks are supported by university research expertise and organisational structures8. After initially taking a top-down approach, a Victoria-based network (VicReN) has recently adopted a more bottom-up approach by undertaking a member-directed research project with community-based general practitioners as members of the research team8,9. This project has resulted in the publication of two peer-reviewed research papers with community-based general practitioners included in the authorship10,11. Elsewhere, international trends in primary care research identify significant success with practice-based research networks12-14.
In Australia, general practices tend to engage in education delivery in response to opportunities offered by universities and/or general practice training providers. Similarly, active research programs in general practice are most likely associated with university-based research initiatives14. Engagement in education and research by general practice tends to be piecemeal with disjointed funding streams and uncoordinated support. Practices are left to create their own solutions for the required structures for managing educational and research activity.
Pressure for increased training capacity by rural general practices
Currently in Australia demand is increasing for medical student, intern and registrar training placements in rural general practices. This demand is being driven by two imperatives. The first is a need for training placements for the growing number of medical students, interns and registrars. Medical student numbers have increased by 81% between 2005 and 201215 with the majority of these students undertaking their placements in rural clinical schools. Following this increase in medical student numbers is a steep increase in the number of medical interns, many of whom are being accommodated in general practice placements. General practice training program entrants doubled, from 600 to 1200 nationally, between 2010 and 201416,17.
The second imperative seeks to address shortages in the rural medical workforce by placing higher numbers of learners in rural settings both to provide an immediate workforce and to build a rural medical workforce. The 'rural pipeline' is considered to be a means of graduating doctors who are likely to practice rurally: preferentially selecting students from rural backgrounds into medical school and providing them with undergraduate, postgraduate, vocational and post-vocational training in the rural context18-21. Education in rural general practices is core to the 'rural pipeline'22. It has been well established that medical students who are exposed to rural settings during their training are more likely to engage in rural practice after graduating20. Also, placing GP registrars in rural practices provides a rural workforce and is a way of attracting more experienced practitioners to rural communities23. The 'rural pipeline' also supports practising rural doctors by enriching their experience, addressing isolation and helping to develop skills18.
While increasing the number of learners in rural general practice may be a way of attracting and retaining rural GPs, the capacity for rural practices to host more learners is limited. Laurence and Black's 2007 survey of urban and rural training practices found that although GPs were usually willing to increase teaching loads, the ability to do so depended on adequate additional resources and support, particularly in areas such as funding for teaching, practice subsidies and consulting space3.
There is capacity for rural general practices to increase engagement in education. For example, practices that do not host learners could be recruited as teaching practices, while practices that host one learner may have capacity to host several learners at different levels of training. To achieve this, educational and funding models that are attractive and sustainable for both practices and learners must be developed. For education to be considered as a core activity, the approach to funding, educational support and learner placement must be an integrated one22. Further, issues such as effective teacher orientation and professional development, physical space, infrastructure and internal organisational structures need to be considered22,24.
Elsewhere the authors have reported the advantages and challenges for rural general practices to host several learners at varying levels25. In that report, the perspective of the practice, the learners and the practice patient community was examined. This article addresses the research question, 'What considerations contribute to the development of a rural academic general practice?'
The rural academic general practice
To inform the development of a rural academic general practice, the model of the academic health sciences centre (AHSC) was explored for use in the context of a rural academic general practice. AHSCs are well established in the USA and the UK and are beginning to be acknowledged in Australia26. The AHCS model describes three complementary pillars of service, education and research. A principle of the AHCS model is fostering the 'discovery-care' continuum by bringing clinical services, education and research together in the one institution. AHSCs are characterised by their large scale, resulting in improved patient outcomes and cost efficiencies26. Dzau et al. describe the value of extending this structure into primary care as an AHSC system where the emphasis is not so much a tertiary institution as a vertically integrated system spanning from community-based care through to tertiary hospitals and universities27. Dzau's model of extending the AHSC model to primary care may facilitate progression within the proposed rural academic practice framework, especially in enabling research activity. If rural general practices are enabled to develop internal research capacity, they will have the means to drive research agendas from the bottom up and in this way meaningfully engage local general practitioners to 'address questions relevant to local health needs'8.
The research question is best answered using a qualitative paradigm. An experienced researcher (TM) conducted semi-structured interviews. Six rural general practices in Victoria were recruited: three practices with multi-level learners, two practices with one learner group, and one practice without learners. This sample was selected to explore the diversity of rural general practice engagement in education. Within the practices purposive sampling of staff (GP supervisors, practice managers, senior administration staff, nurses), learners (registrars, interns, medical students) and patients was undertaken (Table 1). A topic guide was developed after reviewing relevant literature around general practice education and training to guide interviewing. Each respondent group had parallel questions and was designed to address the research question (Table 2 contains an example). Audio recordings of interviews were transcribed and checked against the original recording to ensure transcripts were accurate. Transcripts were not offered for respondent validation.
The data were analysed in several stages. Using an inductive thematic analysis28,29, all four members of the research team (TM, JB, MB, DN) independently coded transcripts. Key themes and subthemes were negotiated and all transcripts were analysed again using this thematic template30 with the unit of analysis by general practice. A deductive thematic approach was used to create the framework, revisiting the data for confirmation and for negative case analysis. The creation of the framework was informed further by the literature and the expertise of the research team.
Table 1: Interviewees categorised by role
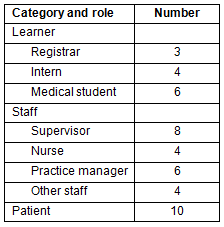
Table 2: Interview topic guide for practice staff

Ethics approval
Human research ethics approval was obtained from Monash University Human Research Ethics Committee, project number CF11/3006 - 2011001694.
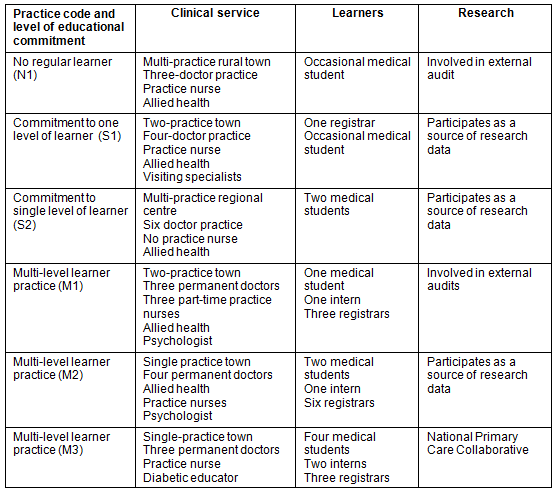
Data were collected from 44 participants using a topic guide developed for each respondent group. Table 2 contains an example. Interviews ranged from 20 to 60 minutes and were audio-taped and transcribed verbatim. Table 3 summarises the characteristics of each general practice unit of analysis.
The results are presented in two parts: first, the thematic analysis representing the thematic template and, second, the resulting framework for a rural academic general practice. Like many classifications, there is some overlap between themes.
Table 3: General practice characteristics summary
Thematic analysis
The three major themes were organisational, educational and research considerations. Under each major theme, several subthemes were identified. These major and subthemes are detailed in Table 4 with example quotes from the data. In describing and discussing the analysis below, italics are used to highlight subthemes.
For organisational considerations, there were six subthemes. Prominent were the values, vision and culture of each practice. Business and service considerations were not always seen to align with educational considerations, hence the degree to which a practice engaged in education was associated with the value that the practice attached to education in relation to business and service: '[Teaching and its requirements] takes you away from your core business which is basically earning a living and keeping the place on the rails.' (Supervisor S2 - single-learner practice).
The patient population and clinical services was an organisational consideration. Registrars and interns require a clinical load. The patient population of practices with a strong educational focus accepted learners as legitimate practitioners and clinical service delivery was structured to accommodate and utilize learners: 'Well, I don't actually see them as interns, they're doctors to me.' (Patient M3 - multi-level learner practice).
Staffing appeared as an organizational subtheme. For practices with little educational activity, existing staff absorbed education tasks. For practices with significant engagement in education, tasks were more likely to be allocated to staff designated and trained for the role: '[I] have just undertaken an educational coordinator role which is a new role that they have created.' (Staff member M2 - multi-level learner practice).
Physical infrastructure was a fundamental consideration in a practice's capacity to host learners. For example, 'I don't know if we have got the room. If we had the room, we would.' (Practice nurse S1 - single-learner practice). The practices with a strong learner presence had all undertaken infrastructure expansion specifically for hosting learners. Two had received government infrastructure grants for this purpose.
Funding streams for education was an important consideration for all practices: 'It's all to do with time and money; it's as simple as that.' (Supervisor S2 - single-learner practice). The greater the engagement in education the more significant the educational funding as an income stream for the practice. These practices were also more positive about the remuneration afforded by funding for education: 'I think funding's pretty good.' (Supervisor 1 M2 - multi-level learner practice). However, funding was piecemeal and from multiple sources: 'There is a funding stream which comes with them, it's different for all of them.' (Supervisor M3 - multi-level learner practice).
As practices increased their engagement with education, they developed the governance structures to manage the organisational requirements of hosting the learners: 'I have everyone marked on there as all the new learners are coming and leaving. So I really do keep a strict eye on that.' (Practice manager M1 - multi-level learner practice).
For educational considerations there were four subthemes. Educational processes exhibited increasing complexity with greater numbers of learners. Practices with multiple levels of learners used a range of teachers and educational processes, were aware of each learner's curriculum and facilitated formal and informal peer assisted learning. For example:
The teaching sessions always had a plan on, you know, we'll talk up to this level and make sure that we get the student involved to this level and then we go through to the next level. (Practice manager M1 - multi-level learner practice).
Clinical supervision became more structured with greater engagement of learners. Practices with multiple levels of learners had several senior doctors identified as supervisors and there were examples of senior learners being supported to supervise other learners: '..part of me trying to learn exam stuff has been helped by supervising other people.' (Registrar M2 - multi-level learner practice). These practices may have supervisors that have allocated clinical sessions where they supervised without having their own booked patients:
There are times when my role as the supervisor is just supervising ... there'd be some sessions where I won't see any patients booked in for myself. (Supervisor M3 - multi-level learner practice).
Educational networks, facilitated by universities and regional training providers, were important in supporting educational skills and resources:
Well the RTP provided not only payment for us to do the work, but educational material and educational forums for learning ... and the university would be providing educational material ... as well. (Supervisor M1 - multi-level learner practice).
Educational networking was a greater feature of practices with a strong educational engagement.
The impact of learner presence on the practice environment was the fourth educational subtheme. The part that the learners themselves played in the practice environment became much more significant with increasing educational engagement. When one or two learners are present, they tended to be absorbed into the established working community. When there are a number of learners present in a practice at a time, they generated their own social and educational networks. With multiple learners in a practice, learners took on the role of teaching other learners and bringing senior staff up to date:
The registrars taught the interns, the registrars and the interns taught the medical students. In fact that's where most of the teaching happened for the medical students. (Supervisor M1 - multi-level learner practice).
Although not a dominant theme, research considerations had two subthemes. Attitude to research while mixed was on the whole positive across all practices and participants:
... if there is no research everything stagnates and you've absolutely got to have research ... (Patient S1 - single-learner practice).
There were reflections from two supervisors that research processes may be at odds with the way that general practitioners think and operate:
It's time consuming, it's tedious, it's methodologically rigorous. None of those things sit well with most GPs I know. (Supervisor 2 M2 - multi-level learner practice).
There was very little research activity in any of the practices other than clinical audits and being participants in research undertaken by external organisations.
Table 4: Themes and subthemes, with example quotes

Developing a rural academic general practice framework
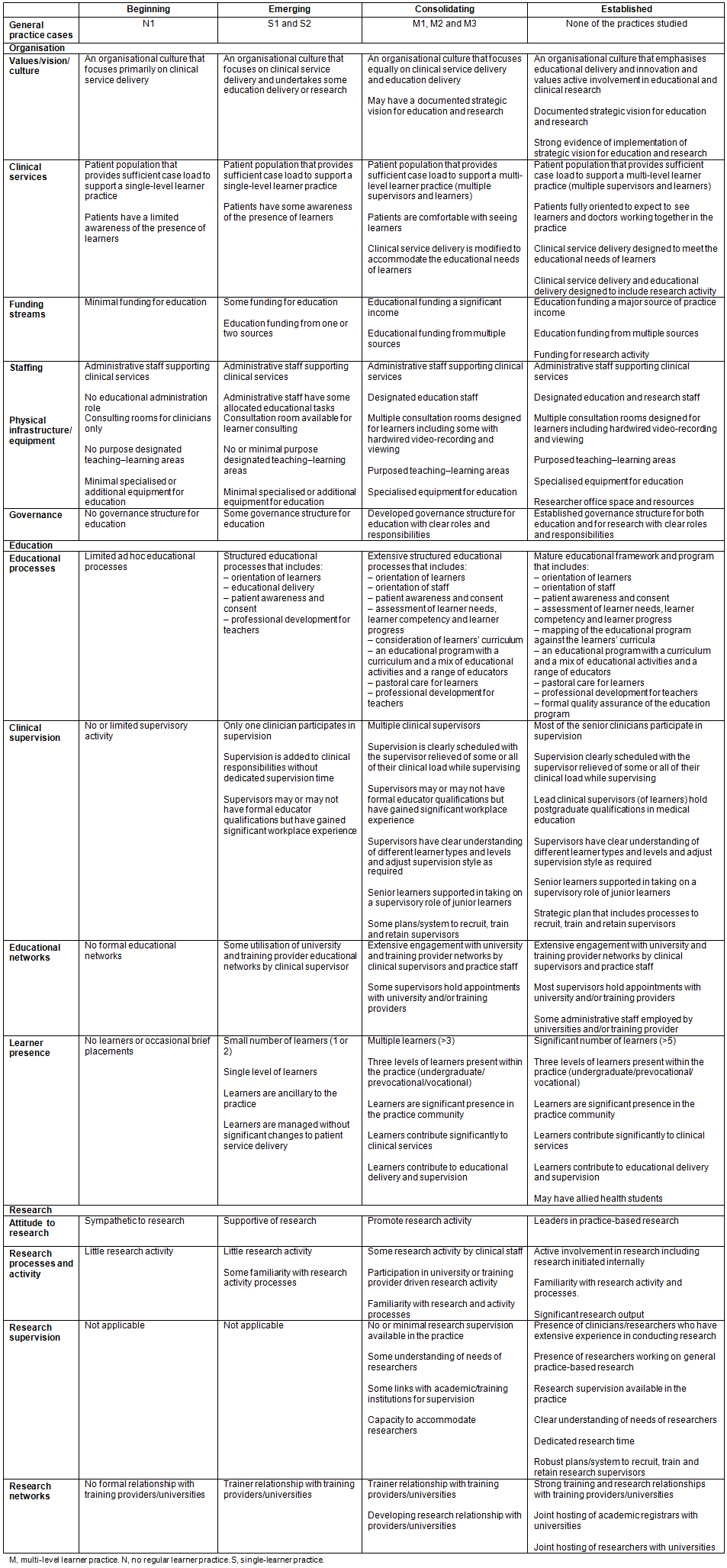
This rural academic general practice framework was based on the thematic analysis above and published literature (Table 5). Four levels of academic engagement by rural general practices are described in the columns beginning, emerging, consolidating and established. All subthemes are reflected in the cells under the broad theme rows. Leveraging the case study research design, the six practices studied were conceived to provide representations of the first three levels of academic engagement: beginning, emerging and consolidating. The features of an established academic rural general practice were supposed from the literature, from extrapolation of the progression of beginning to consolidating rural academic practice, and from the experience of the research team in the rural general practice and academic environments.
Table 5: Framework for rural academic general practices
Discussion
Considerations were identified for progressing on a trajectory from a rural general practice without a training focus to one that has extensive training activity to one that undertakes both training and research and thus could be described as a rural academic general practice. Stages on this pathway have been conceptualised as beginning, emerging, consolidating and established. To effectively foster education and research activity in rural general practices, the considerations identified in the thematic analysis and represented in the framework need to be addressed.
A beginning practice may be reluctant to host learners because of uncertainty about the impact of learners on the patient population and on the doctor-patient relationship. They may be concerned about the additional workload that learners might bring and how to manage this. They may be unsure of the financial consequences of hosting learners, may not have the physical space and may be uncertain of their knowledge and capacity for teaching. To encourage these practices to take on learners, training providers and universities need to be able to clearly articulate how these concerns might be addressed.
Emerging practices in the framework have had some involvement in education while health service delivery remains the primary focus. Usually only one level of learner and a single supervisor are present in the practice. A culture of teaching is appreciated but is not significant. Patients may or may not be aware that the practice hosts a learner. The supervisor's interest in teaching is often the motivator for the practice's involvement in education. The practice receives a small amount of educational income. Resources required to support several learners and a strong culture of education (more than one supervisor, physical space for learners and administrative support) are often the barriers for these practices moving towards the consolidating and established academic status. There may be the concern that hosting more learners will erode the financial viability of the practice. To encourage an emerging practice to take the next step in increasing their engagement in education, support for infrastructure and training supervisors is critical. Also there needs to be clear financial value in making education a stronger focus. This value needs to be well articulated.
Consolidating practices are likely to have been involved in education for some time and to hold learning to be a significant priority within the practice culture. Patients within these practices are well aware of the presence of learners and generally expect and accept learner involvement in consultations. Consolidating practices have multiple supervisors who are involved in teaching and who value the presence of students, interns and registrars. As teaching is a developed activity in these practices, educational payments form an important component of the practice's business revenue. Dedicated administrative support for education is present. While research is appreciated, there is minimal engagement. For advancement of research activity, a clear route needs to be articulated for developing research skills with mentoring and role models. Research networks are essential to supporting research activity development in the practice. There also needs to be a good business case for practices to engage in research.
In an established practice, service, education and research are viewed as equal priorities. Strong relationships with educational and research institutions (universities and regional training providers) are present. As with the consolidated practices, resources (patient population, physical infrastructure, supervision and educational administration) are sufficient to host multiple learners at varying stages of their training. Also, processes for curriculum development, orientation and teaching are well established. Supervisors are likely to hold formal educational qualifications. There is administrative support for both the educational and the research activities. These practices conduct research either independently or in close partnership with academics from outside institutions. Personnel within the practice are familiar with research paradigms and processes, ethics approval and scholarly writing. Research grants together with education payments and grants are significant funding streams for the practice.
This model has two particular strengths. First, this is a holistic model that places service, education and research together as integrated activities for the mature academic rural general practice. In this way, each activity supports the other activities. Second, this is a bottom-up model putting the individual general practice at the centre rather than on the periphery. Putting the individual general practice at the centre gives a capacity for genuine ownership of academic activity by general practices. This focus is likely to engender research agenda setting and ownership by general practices14 and integration of research into clinical services31 and educational activity in the community setting.
It is acknowledged that the model suggests that engagement in education precedes engagement in research. This is consistent with the historical reality of the recent steep increase in the engagement of general practices in education while engagement in research has remained low5. The present study's sample of general practices and subsequent model was based on engagement in education. It would be valuable to test the framework on a sample based on engagement in research.
Strengths and limitations
The study strengths include the sampling of the diverse types of practices and the interviews with multiple stakeholders. The method of analysis was robust, with several rounds of data interrogation. The case study method enabled interpretation of results at the level of the practice, reflecting a realistic unit of analysis for propelling significant change.
The study was set in rural Victoria, which may not reflect the broader landscape of general practices, training providers and higher education in other locations. The multidisciplinary research team (general practitioner, allied health academic/practitioner, organisational behaviour academic and education academic) enabled several perspectives to be offered during each phase of the study. This strengthens the study, reducing biases associated with a singular perspective. However, it may also mean that nuances were overlooked in data that are evident to those immersed in practice. Throughout the project, the research team met regularly and shared their perspectives and analyses. As in all interview-based studies, the quality of data may have been influenced by the context of the interview itself. Although the interviewer is experienced, it is possible that interviewees offered views that they thought socially desirable. However, early interview transcripts were reviewed by at least one other research member and interview technique examined. The interviewer approach was considered 'neutral' and 'encouraging'. The interviewer made notes on each interview and although some interviewees were noted as more forthcoming than others, with rapport established the flow of conversation in all interviews became easy.
Future research may investigate the transferability of the findings, especially using negative case analysis. It would be valuable to test the framework in other settings.
There is already sturdy evidence that learners are essential to addressing long-term workforce issues in Australian rural general practices. An established culture of learning is a fertile environment for developing research activity. This study documents that the pathway to becoming an academic rural general practice is a complex process, which requires many years of deliberate development. This development is best driven by a strategic vision of the practice shared by the key stakeholders such as practice owners, the permanent practitioners and the senior practice management staff. It is considered that the proposed framework will provide guidance to practices exploring one or more steps in the transition towards a full rural academic practice. It will also provide guidance for educational institutions and funding bodies wishing to support educational and research activity in rural general practices.
Acknowledgements
The authors acknowledge General Practice Education and Training for funding for this project and the five rural general practices that participated. The authors thank Associate Professor Elmer Villanueva for his contribution to the conception of the project.
References
1. General Practice Consultative Committee, Department of Human Services and Health. The future of general practice: a strategy for the nineties and beyond. Canberra, ACT: National Health Strategy, 1992.
2. Coote W. General practice reforms, 1989-2009. Medical Journal of Australia 2009; 191(2): 58-61.
3. Laurence C, Black L. Teaching capacity in general practice: results from a survey of practices and supervisors in South Australia. Medical Journal of Australia 2009; 191: 102-104.
4. Magin P, Pirotta M, Farrell E, Van Driel M. General practice research - training and capacity building. Australian Family Physician 2010; 39(5): 265-266.
5. Askew D, Schluter P, Gunn J. Research productivity in Australian general practice: what has changed since the 1990s? Medical Journal of Australia 2008; 189(2): 103-104.
6. Brown L, McIntyre E. The contribution of primary health care research, evaluation and development-supported research to primary health care policy and practice. Australian Journal of Primary Health 2012; 20(1): 47-55.
7. Oceania Health Consulting. Evaluation of the Primary Health Care Research, Evaluation and Development Strategy. (Online) 2005. Available: http://www.phcris.org.au/phcred/reports/PHCRED%20Evaluation%20-%20Full%20Report.pdf (Accessed 24 March 2014).
8. Soos M, Temple-Smith M, Gunn J, Johnston-Ata'Ata K, Pirotta M. Establishing the Victorian Primary Care Practice Based Research Network. Australian Family Physician 2010; 39(11): 857-862.
9. Temple-Smith M, Clark M, Pirotta M. Making a difference - are you game? Australian Family Physician 2011; 40(1-2): 49.
10. Garth B, Temple-Smith M, Clark M, Hutton C, Deveny E, Biezen R, et al. Managing same day appointments - a qualitative study in Australian general practice. Australian Family Physician 2013; 42(4): 238-243.
11. Garth B, Temple-Smith M, Clark M, Hutton C, Deveny E, Biezen R, et al. 'Your lack of organisation doesn't constitute our emergency' - repeat prescription management in general practice. Australian Family Physician 2014; 43(6): 404-408.
12. Gunn J, Temple-Smith M, Pirotta M, Sanci L, Deveny E. 2011 Strategic roadmap for Australian research infrastructure. Submission to the Department of Innovation, Industry, Science and Research General Practice and Primary Health Care Academic Centre. Melbourne, VIC: University of Melbourne, 2011.
13. Cooke J. A framework to evaluate research capacity building in health care. BMC Family Practice 2005; 6: 44.
14. Del Mar C, Askew D. Building family/general practice research capacity. Annals of Family Medicine 2004;2:535-540.
15. Joyce C, Stoelwinder J, McNeil J, Piterman L. Riding the wave: current and emerging trends in graduates from Australian university medical schools. Medical Journal of Australia 2007; 186(6): 309-312.
16. Willcock S, Coote W. The Australian General Practice Training program - reflections on the past decade. Medical Journal of Australia 2011; 194(11): S55-S58.
17. Department of Health and Ageing. Building a national health and hospitals network - training record numbers of GPs. Media release. Department of Health and Ageing, 2010.
18. Tesson G, Curran V, Pong R, Strasser R. Advances in rural medical education in three countries: Canada, the United States and Australia. Education for Health 2005; 18(3): 405-415.
19. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health. 9(2):1060. (Online) 2009. Available: www.rrh.org.au (Accessed 7 July 2014).
20. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9(1): 1083. (Online) 2009. Available: www.rrh.org.au (Accessed 6 July 2014).
21. Campbell DG, Greacen JH, Giddings PH, Skinner LP. Regionalisation of general practice training - are we meeting the needs of rural Australia? Medical Journal of Australia 2011; 194(11): S71-S74.
22. Walters L, Worley P. Training in rural practice: time for integration? Australian Journal of Rural Health 2006; 14(5): 171-172.
23. Rosenthal D, Worley P, Mugford B, Stagg P. Vertical integration of medical education: Riverland experience, South Australia. Rural and Remote Health 4(1): 228. (Online) 2004. Available: www.rrh.org.au (Accessed 25 May 2013).
24. Larsen K, Perkins D. Training doctors in general practices: a review of the literature. Australian Journal of Rural Health 2006; 14(5): 173-177.
25. Morrison T, Brown J, Bryant M, Nestel D. Benefits and challenges of multi-level learner rural general practices - an interview study with learners, staff and patients. BMC Medical Education 2014; 14: 234.
26. Fisk N, Wesselingh S, Beilby J, Glasgow N, Puddey I, Robinson B, et al. Academic health science centres in Australia: let's get competitive. Medical Journal of Australia 2011; 194(2): 59-60.
27. Dzau V, Ackerly D, Sutton-Wallace P, Merson M, Williams R, Krishnan K, et al. The role of academic health science systems in the transformation of medicine. Lancet 2009; 375: 949-953.
28. Fereday J, Muir-Cochrane W. Demonstrating rigor using thematic analysis: a hybrid approach of inductive and deductive coding and theme development. International Journal of Qualitative Methods 2006; 5(1): 80-92.
29. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006; 3: 77-101.
30. Miles M, Huberman A. Qualitative data analysis: an expanded sourcebook, 2nd edn. Thousand Oaks, CA: SAGE Publications, 1994.
31. Mant D, Del Mar C, Glasziou P, Knottnerus A, Wallace P, van Weel C. The state of primary-care research. Lancet 2004; 364(9438): 1004-1006.


