Australia is one of the most ethnically diverse societies in the world today with nearly 25% of Australian residents being born outside of Australia1. Like all health professionals, doctors have a social responsibility to be equipped to recognise and respect cultures and cultural values different from their own. This is particularly so when working with Aboriginal and Torres Strait Islander Australians who suffer the worst health status in the country on some indicators, in particular preventable diseases such as diabetes, renal disease and cardiovascular disease2.
Traditionally, cultural awareness and diversity education has focussed on elective components in the later stages of a medical education program3. It has also been argued that medical students do not always perceive teaching of cultural diversity to be directly relevant or useful to them4. This therefore poses the challenge of introducing innovative learning and teaching activities into this important area.
In the last decade, several important initiatives were undertaken in Australia to address the educational needs of Australian medical professionals' awareness of Aboriginal and Torres Strait Islander health. The Australian Medical Council developed standards for accreditation of medical schools5. The Committee of Deans of Australian Medical Schools, in association with the Australian Indigenous Doctors Association, developed an Aboriginal and Torres Strait Islander Health Curriculum Framework6, which provides medical schools with a set of guidelines for developing and delivering Aboriginal and Torres Strait Islander health as core medical education content. Various medical colleges have also developed requirements for medical students in Aboriginal and Torres Strait Islander health, such as the Royal Australian College of General Practitioners7.
Like many other Australian universities, Bond found it challenging to implement the recommended Aboriginal and Torres Strait Islander health content across its curriculum and started looking for innovative ways to do so5-7. The Bond Bachelor of Medicine, Bachelor of Surgery (MBBS) program is an accelerated undergraduate medical program of 4.8 years' duration. It has three themes, including the 'Health advocate and professional' theme that covers content pertaining to Indigenous health, anthropology, sociology, social and health psychology, spirituality, medical ethics, health law, medical humanities, and public health.
The review of the Implementation of Aboriginal and Torres Strait Islander Health Curriculum Framework in 2012 clearly identified cultural immersion as one of the most effective implementation initiatives for introducing cultural awareness education to medical students8. As a result, in 2011 Bond reviewed its curriculum and in 2012 piloted immersion as an introductory part of an overall program in Aboriginal and Torres Strait Islander health. This paper reports on the evaluation findings of this compulsory cultural immersion process for all first year students from 2012 to 2014.
Cultural immersion
Cultural immersion is based on the principle that full engagement with another's culture, and their practices and language, is an effective means of learning about oneself9. The term 'culture' refers to the particular way of life of a group of people10, whereas the term 'immersion' means being baptised into, fully submerged, sinking, or a quick dip11. Therefore, for the purposes of this paper 'cultural immersion' is used as a first quick dip into another culture, in a safe, supportive educational environment.
There are some international examples of cultural immersion in a medical context. The John Burns School of Medicine at the University of Hawaii ran a 5 day workshop in which physicians and traditional healers were transported to islands and participated in workshops that comprised historical and cultural aspects of native Hawaiian health12,13. This inclusive approach exposed participants to native concepts of health, knowledge acquisition and care. The written evaluations identified the main strength of the workshop as being the removal of participants from their usual occupational and educational environments. In New Zealand the University of Otago focussed on Pacific Islander health and placed its fourth year medical students with Pacific families in Dunedin, where they were educated about the health of those communities by participation in storytelling and other activities14, and the University of Wellington took 51 of its third year students on a 1 week immersion experience to six small communities in the East Cape region of New Zealand13,15. Participant evaluation reports from all of these universities were positive.
Although there is some literature about cultural immersion in the Australian nursing literature, there is little in the medical literature. Literature that does exist largely refers to placement experiences in developing countries, remote placements, in Indigenous health services, or areas of workforce need16. The University of Notre Dame reports sending its second year students on a 1 week placement into the Kimberleys of Western Australia, essentially as observers of remote life16. They emphasise the importance of good preparation both cognitively and emotionally prior to the immersion experience. The University of Adelaide undertakes a 'rural week' that includes some Indigenous exposure as part of the first and second year curriculum17. While all of these cultural immersion programs were significantly different, they had common curriculum content, including teaching the social determinants of health, the importance of cultural factors in health and illness, and the role of the health professional.
Despite these very positive reported cultural immersion activities, it was essential for Bond to develop and evaluate its own immersion activity for two main reasons. First, the planned content was significantly different from other reported immersion activities, and second, there were no known examples of cultural immersion activities being undertaken at such an early stage in an undergraduate medical curriculum (ie first year). Therefore, the objective was to establish an early cultural immersion activity as the first building block within the formal, integrated 5 year medical curriculum. An important principle was that it was a normal compulsory part of the curriculum and funded from usual MBBS funds for sustainability.
Initial activity comprised consulting with the right people, so a high level multicultural and multidisciplinary Indigenous Health Group (IHG) was established. The IHG comprised two Aboriginal doctors, an Aboriginal elder and educator, and a doctor who worked in an Aboriginal medical service - all of whom were external to the University and gained fractional academic appointments - as well as five academic staff - two educationalists, a clinical ethicist, an anthropologist and a research psychologist. The role of the group was to develop the Aboriginal and Torres Strait Islander health content across the 5 years of the curriculum and an implementation plan. Research and internal consultation identified that a compulsory cultural immersion process should form the initial part of the Indigenous health curriculum.
During 2012 the IHG met several times to determine the Aboriginal and Torres Strait Islander health learning outcomes of the whole 5 year program, which were based on the standards and guidelines determined by the profession5-7. The group then developed the educational content and objectives of the pilot cultural immersion, as well as the preparatory educational sessions. Significant planning included: identifying a suitable site that could feed and house over 100 people; developing a set of principles to underpin the program and the immersion; finding or developing educational resources; developing a step by step facilitator guide and educational program; identifying Aboriginal or Torres Strait Islander facilitators for various sessions; and developing a comprehensive evaluation process and facilitator briefing and debriefing processes. Significant administrative activities occurred, including the creation and administration of consent forms and the organisation of dietary requirements, lodging arrangements, student groupings, facility maps, travel arrangements, educational resources, first aid equipment, insurance and risk assessment, budget and site visits.
Evaluation of the cultural immersion occurred in two ways. First, a talking circle was an informal place where the students provided verbal feedback about the overall activity and reflections about what they had learned. This feedback was seen as confidential and remained with the group, and is not included in the evaluation findings. The second mode of evaluation was based on level 1 (reaction) and level 2 (learning) of the Kirkpatrick four-level training evaluation model. Students were asked to rate the attainment of the overall learning objectives of the workshop and of each specific educational activity, as well as feedback regarding the organisation, the venue and the workshop facilitators. Ratings were based on a five-point Likert scale ranging from 1=strongly disagree to 5=strongly agree. A section was also provided for written comments regarding the 'best things' about the workshop and those things that could be improved.
The evaluation feedback from the 2012 (n=92), 2013 (n=89) and 2014 (n=90) evaluation forms were entered separately into SPSS (IBM, http://www.ibm.com) and then combined, and statistical analysis was undertaken in 2014. Detailed evaluation reports were written to the Faculty annually for improvements. Findings from the first immersion were also reported to several Faculty-wide staff meetings to ensure everyone understood the importance of this activity. Both the backing and the leadership from the Faculty and MBBS program were critical to its success.
The cultural immersion
Based on the implementation principles, students were introduced to cultural issues from an international perspective first, so that any preconceptions and biases about Aboriginal and Torres Strait Islander Australians were not raised. This was done through two prerequisite lectures: the first introduced culture from an international perspective and then compared an Australian perspective; the second focussed on health status, exploring the social determinants of Aboriginal and Torres Strait Islander health using a storytelling approach. Both lectures were integrated into two 1 week Indigenous-identified cases as part of the overall problem-based learning curriculum.
In November 2012 a pilot of the compulsory cultural immersion was conducted for all first year medical students after approximately 21 weeks of course enrolment. Ninety-two first year medical students attended a 1.5 day overnight cultural immersion to a rainforest retreat, Koonjewarre, at Springbrook in the Gold Coast (Queensland) hinterland. This facility was chosen due to its: ability to provide a 'getaway' feeling; semi-remote location (no mobile phone or Internet); accessibility of buses (60 min drive on safe roads); lodging for 100 people; and kitchen that could accommodate a cohort of which nearly one-third indicated special dietary needs.
Students were divided into four smaller groups of approximately 24 people. They then participated in multiple 50 min cultural education sessions (eight in 2012; nine in 2013). These included a Welcome to Country, historical accounts given by Aboriginal and Torres Strait Islanders, storytelling, and culture and identity sessions, as well as a Cultural Evening Festival under the direction of the students in which they sang and danced their own cultures into the evening. The curriculum included a variety of educational methods such as history maps and the talking circle, as well as the students drawing and discussing their own culture. The immersion concluded with a community survival session, where students had a part of their identified culture removed from their cultural drawing and where they discussed their emotional reactions to this.
In 2013 another session was added - Join the Dots - where postcards of Aboriginal art were explored by students who told stories about what was represented18. In 2013, as a result of student feedback, an additional post-immersion lecture was added. Specifically, the session applied the links between Aboriginal and Torres Strait Islander history and health outcomes - an appropriate clinical end-cap to the event. Also in 2013, a compulsory in-semester assessment was added to the MBBS program, requiring students to draw a concept map that linked the history of Aboriginal and Torres Strait Islander Australians with health outcomes and to write a 500 word explanatory statement and reflection. This proved to be a very useful process as it enabled students to personally link their own thoughts and feelings about the history of Aboriginal Australia with their own cultural experiences, and helped staff measure the attitudinal shift and potential changes in behaviour19.
It should be noted that the students, whilst all are required to be Australian citizens, were from a large variety of cultural groups (eg India, Pakistan, Iran, Asia, South Africa and New Zealand) and many were first generation Australians. Additionally, the facilitators were of various nationalities (eg Indigenous Australia, USA and UK). Hence this cultural diversity added richness to the overall experience, as many students could identify with some of the patterns of cultural oppression discussed and the many different perspectives.
Ethics approval
Ethics approval RO1543 was attained for this study through Bond University Research Ethics Committee.
What did the students think?
Based on descriptive statistics, the evaluation feedback about the 2012 cultural immersion was extremely positive. As a result it was decided that the immersion, with some refinements, would be continued as an ongoing, compulsory and assessable component of the first year MBBS program.
The greatest strength of the immersion was identified as the facilitators, who consisted of the initial development team of nine, as well as three Torres Strait Islanders, three Aboriginal dancers and a Bond Indigenous Support Officer who told her own personal story, which proved to be the highest rated activity. Students overwhelmingly reported a very positive experience. They generally expressed their overall satisfaction with the cultural immersion activity and agreed that it was a well organised process in which the facilitators contributed positively to their experience.
Students generally agreed that the preparatory materials provided them with sufficient information about the workshop and stated that as a result of attending they could describe the influence of culture on perspectives, attitudes, assumptions, beliefs and behaviours. Furthermore, they indicated that they were able to identify their own cultural values and reflect on their implications for health care, and could identify their own emotional reactions to Aboriginal and Torres Strait Islander history. The descriptive statistics indicated that students felt more confident communicating with Aboriginal and Torres Strait Islander peoples and could explain the connection between their history and health outcomes. Fig1 displays the individual mean ranks (range 1-5) of the achievement of the overall objectives.
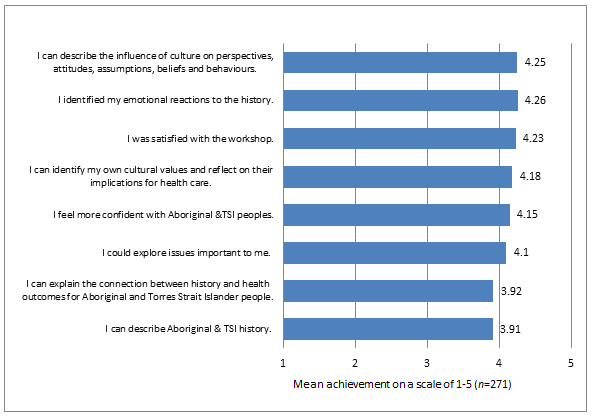
Figure 1: Achievement of learning outcomes
In the evaluation of the individual sessions the students strongly agreed that the Storytelling session enabled them to understand first-hand the impact that the history of Aboriginal Australia has on health outcomes.
It (the storytelling session) opened my eyes that Indigenous history is not something just in the past but affects individuals even today.
Students also strongly agreed that the Welcome to Country session enabled them to understand the importance and roles of elders, traditions, ceremony and significance of the land to Aboriginal peoples. Students indicated that the Torres Strait Islander History and History Maps sessions met their objectives and noted the importance of Aboriginal and Torres Strait Islander facilitators. One comment exemplified this:
Having Aboriginal and Torres Strait Islander people able to personally tell us what's important to them and what has shaped their lives - we can learn history and health care in lectures, but it's invaluable for them to share their culture with us.
Students strongly agreed that the Draw your Culture session allowed them to explore cultural groupings, to see that culture is a driving force and that it contributes to the establishment of individual and collective identity. They agreed that this session enabled them to examine how their beliefs and practices can affect their health beliefs. The Self and Community Survival session also enabled students to understand the effects of being deprived of certain cultural dimensions and it assisted them to specifically categorise and rank-order culture at an individual and collective level. Another student observation documents the impact of first-hand experience:
The Self and Community Survival session really effectively gave me more a personal perspective on a loss of culture by using Indigenous cultures as a vehicle to also learn about the cultures of other members of the cohort; identifying what's important about my culture and reflecting about what would happen if something is taken away ... it was really powerful.
Students agreed that the Cultural Evening Festival enabled them to have fun and become motivated about cultural issues and the Joining the Dots session enabled them to understand the importance of a holistic view of health and the factors that influence health and wellbeing.
Students strongly agreed that the facilitators contributed positively to their learning, particularly the facilitators in the Storytelling, Draw your Culture and Self and Community Survival sessions. Fig2 displays the mean ranks (range 1-5) of the evaluation items pertaining to individual sessions and facilitator contributions.
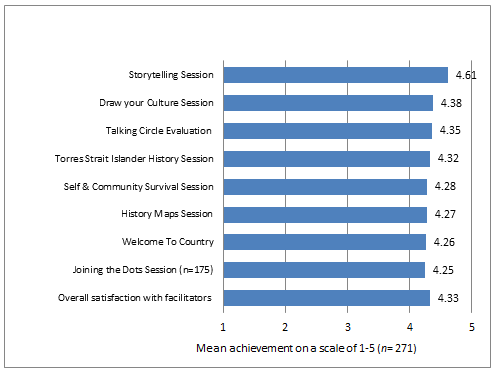
Figure 2: Level of student satisfaction with facilitation of sessions
Elsewhere in the evaluation students were asked an open ended question regarding the 'best things' about the immersion activity and what could be improved. The Storytelling session was overwhelmingly identified as the 'best thing' about the cultural immersion by 57.5% of students, followed by bonding with the cohort, the Torres Strait Islander session, and learning more about culture. Overall there was clear evidence that students valued the novelty and difference of the cultural immersion as a teaching activity, with some finding it a life changing experience and others expressing their gratitude:
Before I came here I thought I could find all this information in a book or on the web, but having experienced what I have the past 2 days is something that will stay with me for the rest of my life.
Thank you so much - the cohort is grateful as a whole for this rare opportunity.
A worthwhile activity that I'm privileged to be a part of.
Being away from campus helped me to fully appreciate the importance of culture and its connection with health care.
Thank you - it was a great experience and really gave me more perspective about life and about myself.
Meals were identified by students (n=77) as the item most in need of improvement, followed by the accommodation (n=55). Other identified suggestions were to make better use of the surrounding rainforest environment and the camp facilities (eg canoes, obstacle course, more stories and opportunities to spend more time on Aboriginal history).
Cultural immersion has been proven to be a very useful process to orientate students early in the medical education program about Aboriginal and Torres Strait Islander history, culture and health outcomes. Immersion has also provided students with an opportunity to learn about their own constructions of culture, and the cultures of those around them. Students greatly appreciated the learning opportunity and it has given them a hunger for more in successive years. The facilitators also learned a lot about teaching in this important area. The Indigenous health team have recently been awarded the Faculty Teaching Award as well as the Vice Chancellor's Teaching Excellence Award for their work.
The future
The overall Aboriginal and Torres Strait Islander content is now well-integrated into the renewed MBBS curriculum at Bond University. The first year program focuses on 'building awareness'. The second year program focuses on 'respecting difference', where students undertake three 1 week Aboriginal or Torres Strait Islander cases. Third year focuses on 'building resilience'. It includes a video of three cases about identity and social and emotional wellbeing, responding to racism, and the role of Aboriginal Community Controlled Health Services, so that students can understand different models of care and services offered prior to their clinical years.
Additionally, although there is a lot of cross-cultural education going on in the health arena, there is little in the literature regarding the effect that these activities are having. Therefore, the Indigenous Health Group is undertaking a 5 year longitudinal study to measure the impact of these activities. The team will report on the initial findings of the study in future conference presentations and publications. However, initial findings indicate significant differences in attitudes and improved cognitive links between the immersion activity and the students' comprehension of the social determinants of health, which is very pleasing. More research of this nature is required to ensure that the teaching of Aboriginal and Torres Strait Islander health is having an impact on the cultural safety of health professionals in their future practice.
Acknowledgements
The authors thank Narelle Jackson for her administrative activities supporting the three cultural immersions, and Professor Richard Hays for his leadership and support.
References
1. Australian Government. Our people. Canberra: Australian Government, 2014. Available: http://australia.gov.au/about-australia/our-country/our-people (Accessed 12 March 2015).
2. MacRae A, Anomie TN, Burns J, Catto M, Gray C, Levitan L, McLoughlin N, Potter C, Ride K, Stumpers S, Trzesinski A, Urquhart B, eds. Overview of Australian Indigenous health status, 2012. 2013. Available: http://www.healthinfonet.ecu.edu.au/health-facts/overviews (Accessed 12 March 2015).
3. Mutchnick IS, Moyer CA, Stern DT. Expanding the boundaries of medical education: evidence for cross-cultural exchanges. Academic Medicine 2003; 78(10): S1-S5.
4. Dogra N, Karnik N. Teaching cultural diversity to medical students. Medical Teacher 2004; 26(8): 677-680.
5. Australian Medical Council. Standards for assessment and accreditation of primary medical programs by the Australian Medical Council 2012. Kingston, ACT: Australian Medical Council, 2013.
6. The Project Steering Committee. CDAMS Indigenous health curriculum framework. Melbourne: Committee of Deans of Australian Medical Schools, 2004.
7. RACGP. Aboriginal and Torres Strait Islander health. In: RACGP curriculum for Australian general practice 2011. Melbourne: Royal Australian College of General Practitioners, 2011. Available: http://curriculum.racgp.org.au/statements/aboriginal-and-torres-strait-islander-health/ (Accessed 19 July 2015).
8. Australian Indigenous Doctors Association. A review of the implementation of the Indigenous Health Curriculum Framework and the Healthy Futures Report within Australian medical schools. Parkes, ACT: Medical Deans Australia and New Zealand and the Australian Indigenous Doctors Association, 2012.
9. Carpenter DA, Kamaka ML, Kaulukukui CM. An innovative approach to developing a cultural competency curriculum: efforts at the John A. Burns School of Medicine, Department of Native Hawaiian Health. Hawai'i Medical Journal 2011; 70(11 Suppl 2): 15-19.
10. Smith JD. Australia's rural and remote health: a social justice perspective, 2nd edn. Melbourne: Tertiary Press, 2007.
11. The Free Dictionary. Cultural immersion. 2014. Available: http://www.thefreedictionary.com/immersion (Accessed 17 February 2014).
12. Kamaka M. Cultural immersion in a cultural competency curriculum. Academic Medicine 2001; 76(5): 512.
13. Crampton P, Dowell A, Parkin C, Thompson C. Combating effects of racism through a cultural immersion medical education program. Academic Medicine 2003; 78(6): 595-598.
14. Sopoaga F, Connor JL, Dockerty JD, Adams J, Anderson L. Training medical students in Pacific health through an immersion programme in New Zealand. New Zealand Medical Journal 2012. 125(1349): 37-45.
15. Dowell A, Crampton P, Parkin C. The first sunrise: an experience of cultural immersion and community health needs assessment by undergraduate medical students in New Zealand. Medical Education 2001; 35(3): 242-249.
16. Mak DB, Watson R, Hadden J. Preparing medical students to undertake a cultural immersion experience: introductory frameworks for preparatory and post-immersion activities. International Journal for the Scholarship of Teaching and Learning 2011; 5(1): 18.
17. Newbury JW, Shannon S, Ryan V, Whitrow M. Development of 'rural week' for medical students: impact and quality report. Rural and Remote Health 5(3): 432. (Online) 2005. Available: www.rrh.org.au (Accessed 12 May 2015).
18. Gold Coast Aboriginal and Torres Strait Islander Partnership Advisory Council, Karulbo. All together strong and deadly community partnerships. Resource guidebook, making it easier to work respectfully with Aboriginal and Torres Strait Islander communities. Coolangatta, QLD: Krurungal - Aboriginal and Torres Strait Islander Corporation for Welfare, 2012.
19. Kirkpatrick D. Kirkpatrick's four level training evaluation model. 2014. Available: http://www.mindtools.com/pages/article/kirkpatrick.htm (Accessed 8 December 2014).



