Introduction
Rural clinicians require expertise spanning not just office-based primary care, but also procedural skills such as emergency medicine, anaesthesia, obstetrics and surgery. As such there is a requirement to remain at the forefront of several different fields. Therein lies a dilemma - how to maintain the necessary knowledge, particularly in the face of rapidly evolving developments across several clinical arenas.
There is a concerted effort by professional bodies to embrace the diversity of rural medicine and define rural generalist pathways, ensuring that rural clinicians have the necessary skills to perform their diversified role. Whilst the focus of training organisations and professional colleges is often focused on training rural generalists, there is less emphasis on maintenance of knowledge and skills. Clinicians should be 'life-long learners' - yet the reality is that the knowledge translation of new concepts may take years to percolate to frontline practice, through the usual means of reading the literature, publication of consensus guidelines and attendance at upskilling events and conferences1. Use of simple tools utilising web 2.0 technology enables rapid sharing of new concepts in practice between clinicians, development of consensus best practice and allowing one to stay abreast of both basic and cutting edge medicine.
Free open access medical education for rural clinicians
Conceived in 2012, free open access medical education (FOAMed) is an evolving paradigm, which was initially enthusiastically adopted by emergency and critical care clinicians.
If you want to know how we practised medicine five years ago, read a textbook.
If you want to know how we practised medicine two years ago, read a journal.
If you want to know how we practise medicine now, go to a (good) conference.
If you want to know how we will practise medicine in the future, listen in the hallways and use FOAM.2
A full report of the development of FOAMed can be read from Nickson and Cadogan, authors of the lifeinthefastlane.com website3,4. Key features of the FOAMed paradigm include:
- Sharing educational resources, such as slide presentations, clinical images, ECGs and case presentations (traditionally held in personal or institutional collections) with colleagues globally, for use or modification without expectation of reward (although attribution is expected).
- Use of web 2.0 connectivity to share articles (blogs), audio (podcast) or video (vodcast) reviews, and collate and curate educational resources.
- Encouragement of asynchronous learning, such as the 'flipped classroom' (disseminating educational content via blogs, podcasts and vodcasts prior to formal face-to-face teaching or conference sessions) or review of material offline when convenient.
- Use of social media platforms to allow clinicians to broaden the reach of usual 'corridor conversations', gathering experience through establishing global discussion networks on evolving clinical concepts or revision of established dogma.
FOAMed has the power to democratise knowledge and to rapidly shorten the 'knowledge translation' gap between inception, publication and bedside application5. Yet the benefits of FOAMed remain confined to those 'in the know'. Concerted efforts are being made to engage grassroots clinicians and educationalists, who may be suspicious of both web-based and social media platforms, to demonstrate the benefits of FOAMed.
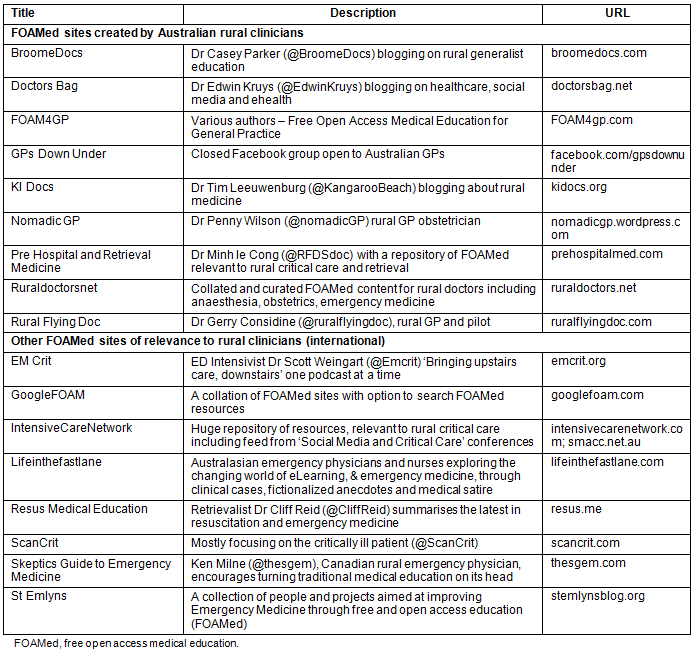
Weingart, one of the leading bloggers for emergency medicine and critical care, has established the paradigm of 'bringing upstairs care, downstairs'6. This is the translation of cutting edge critical care FOAMed into the emergency room. As rural clinicians, we believe in extending the power of FOAMed further- to bring 'quality care, out there' to rural clinicians. One of us (CP) has run an educational blog since 2011, with interactive case studies allowing feedback from clinicians in Australia and overseas. Inspired by this, many other rural clinicians have established blogs that have become a repository for collated and curated FOAMed resources and reflections (Table 1).
Table 1: Recommended FOAMed resources for rural clinicians
Amongst FOAMed users, cases and concepts are reviewed then disseminated as educational podcasts, vodcasts or blog posts in efforts to shorten the knowledge translation gap that typically occurs in rural medical education. Unfortunately many traditional routes to continuing professional development (upskilling events, courses required for credentialing in rural hospitals, educational events) do not cover the cutting edge, contemporary concepts in care that are the essence of FOAMed. This is disappointing given the potential benefits of such knowledge to rural clinicians and their patients.
Examples of practical FOAMed: airway management and cutting edge critical care
Airway management, particularly emergency intubation, can be one of the most stressful activities for the rural clinician - he or she may have only infrequent exposure to this high-risk, tightly coupled procedure. Moreover, these patients are usually critically unwell, and the procedure must take place with limitations of available personnel, equipment to manage the difficult airway and without specialist backup. New developments in airway management have been developed and disseminated via FOAMed prior to traditional journal publication. Perhaps most discussed is the technique of apnoeic diffusion oxygenation7. Recognising the utility of such a technique, this concept was shared as FOAMed, enabling refinement and rapid adoption within the emergency medicine and critical care community prior to formal publication8.
FOAMed also allows 'dogmalysis' - the rapid dispelling of inaccurate or superseded medical knowledge - rather than the slow trickle of revised medical knowledge through the traditional routes of conference abstracts, journal publication, write up in textbook or incorporation into course material. Other examples abound where the usual pathway from publication to practice has been rapidly shortened through use of FOAMed8. Pertinent to rural clinicians are discussions around management of emergencies such as cardiac arrest9, use of bedside ultrasound for decision making10, subtleties in trauma and airway management and use of agents such as ketamine for psychiatric sedation and transfer11. It is true that the emergency and critical care communities are early adopters of FOAMed into clinical practice, with FOAMed resources recently incorporated into curriculum and the journal of the Australasian College of Emergency Medicine8. The Royal Australian College of General Practitioners now recognises use of social media FOAMed resources such as the 'GPs Down Under' Facebook group discussions and other FOAMed resources as being recognised for continuing professional development points12 (K. Price, pers. comm. 2015).
Using social media and web 2.0 technology
Social media has many connotations. Anyone who has read a web article and clicked on the 'comment' section, used a smartphone to text or posted to Facebook is already using social media. Connectivity is expected in our modern world, yet social media is often associated by clinicians with inane chit-chat about celebrities, rather than as a professional tool for education. Moreover, there are fears that use of social media risks breaching professional standards13. Organisations are developing standards for the use of social media, but the following rule of thumb from the Mayo Clinic blog serves well, 'Don't Lie, Don't Pry - Don't Cheat, Can't Delete - Don't Steal, Don't Reveal'14.
Twitter is a microblogging platform (limited to 140 characters) allowing rapid signposting of information and real-time discussion among colleagues worldwide. Many medical conferences now have moderated twitter streams to allow real-time feedback on speakers and promote instantaneous dissemination outside of the conference room into the global community. The use of a hashtag allows collection of information on specific topics (eg #FOAMed, #smaccGOLD, #GoRural) and collation of educational material (eg the moderated #GasClass anaesthetic stream or Twitter-based journal clubs such as #twitJC). The Royal Australian College of General Practitioners now encourages moderated Twitter educational discussions via the hashtag #RACGPed, with continuing professional development points awarded for such interactivity (K. Price, pers. comm. 2015).
For those sceptical of dipping their toes into the public arena of Twitter, the use of online discussion fora such as Google+ and comments sections on websites that collate FOAMed information may be more familiar. Some useful blog resources are included in Table 1; this list is ever-growing. Concomitantly, the availability of audio (podcasts) and video (vodcasts) allows content rich resources to be created, downloaded and used for asynchronous education offline. Technology such as smartphones or tablets means that content is always available, whether it be for morning commute, at the gym or at the bedside15. Social media use is gaining acceptance within medical education circles; FOAMed merely extends the paradigm to disseminate free information and encourage content creation, collation, curation and communication16.
New developments such as GoogleGlass (an internet-enabled camera and visual display worn as glasses) may allow the rural clinician and specialist colleagues to share visual information about a patient. Similarly, information (such as infrequently used drug protocols or explanation of how to perform a procedure) can be pushed to the rural clinician via the GoogleGlass display. Such wearable technology is rapidly becoming available and early adopters among the FOAMed community hope to shape such content for future clinical benefit.
Drinking from the fire hose
With the explosion of information available, the rural clinician may feel overwhelmed with information - a process alluded to as 'drinking from the fire hose'. Having effective filters to allow streaming of only relevant content is essential. Fig 1 summarises strategies to effectively use online resources.

Figure 1: Strategies to effectively use online FOAMed
Concerns are commonly raised about sorting information from resources that may be of variable quality. Yet the same argument can be applied to papers published in peer reviewed journals, many of which may suffer from the same problems of quality, quantity and, most importantly, delay in translation to the bedside17,18. Peer review is a cornerstone of the FOAMed community, with the connectivity and implicit willingness to share ideas freely amongst global FOAMed users offering immediate peer review and quality control. Moreover, a social media index for FOAMed sites has been developed, akin to the impact factor used in traditional journal publications19. An international consensus has been developed for assessing the quality of FOAMed sites in emergency medicine and these criteria are easily transposed to FOAMed resources for other specialties, including primary care20.
It should be emphasised that FOAMed is predominantly a tool to share rapidly emerging concepts and narrow the knowledge translation gap; it is no substitute for formal medical education and postgraduate training. The origins of FOAMed are firmly ensconced in testing new ideas and disseminating them; it has potential to further the continuing medical education of established clinicians, rather than to teach novices from scratch. Indeed there is a danger in novice clinicians embarking on a course of action that they have 'read about on a blog'. But the information genie is out of the bottle - students and registrars are using the tools of the internet and social media to gather information, and experienced rural clinicians need to be familiar with these information streams and help to moderate knowledge.
For those exploring FOAMed, visiting a few well-organised and curated sites or podcasts is a sensible way to start. Subscribing to a few well-trusted blogs or podcasts allows highly relevant, peer reviewed and current content to be delivered to your inbox or iTunes library via RSS feeds for browsing at your leisure. An excellent review can be found in a short 400 s 'pecha kucha' talk entitled Dr INFOLove or 'How I learned to stop worrying and love the FOAMed'21. Using effective filters prevents the problem of 'information overload' yet allows the rural clinician to remain up-to-the-minute in knowledge.
Summary
FOAMed is a powerful tool for rural clinicians and educators. Using the internet and various social media platforms, new clinical information and discussion can be shared with colleagues worldwide. Underpinning FOAMed is a sense of community, a willingness to share information freely, with the cornerstone being improved patient care through more rapid application of useful clinical concepts.
It is said that only a fool learns from his own mistakes, a wise man from the mistakes of others (source unknown).
Rural clinicians, traditionally isolated through distance and with the added challenge of being a 'jack of all trades, master of none', can tap into the collective experience of experts and peers in the global medical community using FOAMed resources to improve patient care and clinical skills (Fig2). We are all comfortable with sharing our ideas and skills with patients, colleagues and students on a daily basis in the clinic or at conferences, FOAMed extends the sharing of such knowledge to a global stage.
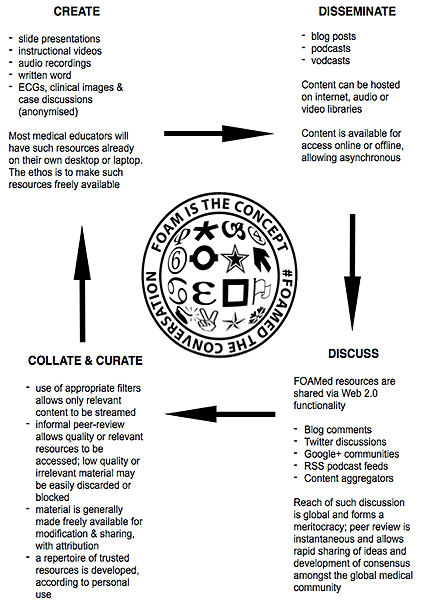
Figure 2: Overview of FOAMed content creation, collation and curation, with communication and collaboration
References
1. Davis D, Evans M, Jadad A, Perrier L, Rath D, Ryan D, et al. The case for knowledge translation: shortening the journey from evidence to effect. British Medical Journal 2003; 327: 33-35.
2. Lex J. International EM education efforts and e-learning. Free Emergency Medicine Talks. (Online) 2012. Available: http://freeemergencytalks.net/2012/08/joe-lex-international-em-education-efforts-e-learning/ (Accessed 21 June 2014).
3. Nickson CP, Cadogan MD. Free open access medical education (FOAMed) for the emergency physician. Emergency Medicine Australasia 2014; 26: 76-83.
4. Foam. Life In The Fast Lane. (Online) 2014. Available: http://lifeinthefastlane.com/foam/ (Accessed 21 June 2014).
5. Diner BM, Carpenter CR, O'Connell T, Pang P, Brown MD, Seupaul RA, et al. Graduate medical education and knowledge translation: role models, information pipelines, and practice change thresholds. Academic Emergency Medicine 2007; 14(11): 1008-1014.
6. Weingart S. Bringing upstairs care, downstairs one podcast at a time. (Online). Available: http://emcrit.org/about-me/ (Accessed 21 June 2014).
7. Weingart SD, Levitan RM. Preoxygenation and prevention of desaturation during emergency airway management. Annals of Emergency Medicine 2013; 59(3): 165-175.
8. Cadogan M, Thoma B, Chan TM, Lin M. Free open access meducation (FOAM): the rise of emergency medicine and critical care blogs and podcasts (2002-2013). Emergency Medicine Journal 2014; 31: e76-77.
9. Cadogan M. All in a lather over targetted temperature management. Life in the fastlane. (Online) 2013. Available: http://lifeinthefastlane.com/all-in-a-lather-over-ttm/ (Accessed 29 March 2015).
10. Parker C. Bedside ultrasound evidence echoes. Broome Docs. (Online) 2014. Available: http://broomedocs.com/2014/02/bedside-ultrasound-evidence-echoes/ (Accessed 29 March 2015).
11. Le Cong M, Finn E, Parsch CS. Management of the acutely agitated patient in a remote setting. Medical Journal of Australia 2015; 202(4): 182-183.
12. GPs Down Under. (Online) 2015. Available: http://gpsdownunder.com (Accessed online 29 March 2015).
13. DeCamp M, Cunningham AM. Social media: the way forward or a waste of time for physicians? The Journal of the Royal College of Physicians of Edinburgh 2013; 43: 318-322.
14. Timimi F. A 12-word social media policy. Mayo Clinic Center for Social Media, 2012. Available: http://network.socialmedia.mayoclinic.org/2012/04/05/a-twelve-word-social-media-policy/ (Accessed 21 June 2014).
15. Australian College of Rural and Remote Medicine. JAMIT (just a minute instant tutorials) competition entries. YouTube. (Online) 2013. Available: https://www.youtube.com/playlist?list=PL0OijzDDBQuYt9GJIF0EzravTSzGBWwAE (Accessed 21 June 2014).
16. Cheston CC, Flickinger TE, Chisolm MS. Social media use in medical education: a systematic review. Academic Medicine 2013; 88(6): 893.
17. Smith R. Medical journals 'a colossal problem of quality'. BMJ Blogs. (Online) 2013. Available: http://blogs.bmj.com/bmj/2013/09/24/richard-smith-medical-journals-a-colossal-problem-of-quality/ (Accessed 21 June 2014).
18. Radecki R. How are we accelerating knowledge translation? BMJ Blogs. (Online) 2014. Available: http://blogs.bmj.com/emj/2014/04/21/how-are-we-accelerating-knowledge-translation/ (Accessed online 21 June 2014).
19. Thoma B, Sanders JL, Lin M, Paterson QS, Steeg J, Chan TM. The social media index: measuring the impact of emergency medicine and critical care websites. Western Journal of Emergency Medicine. (Online) 2015. Available: http://escholarship.org/uc/item/7t7777m7 (Accessed 16 August 2015).
20. Thoma B, ChanTM, Paterson QS, Milne WK, Sanders JL, Lin M. Emergency medicine and critical care blogs and podcasts: establishing an international consensus on quality. Annals of Emergency Medicine 2015: in press.
21. Nickson C. Dr INFOlove: or 'How I learned to stop worrying and love the FOAM'. Social Media and Critical Care, (Online) 2013. Available: https://vimeo.com/57826734 (Accessed 21 June 2014).

