full article:
To address the challenge of producing and retaining an adequate medical workforce in rural and remote Australia, government and universities have invested in efforts to recruit medical students from rural and remote areas1,2. Strategies shown to improve rural career intentions of medical graduates involve establishing regionally based medical schools and rural clinical schools, the targeted selection of students with a rural background, and providing significant, positive rural experiences during undergraduate training3-6.
James Cook University (JCU) was the first of Australia's 'new' medical schools to be established in a growth phase of medical education that has seen both the number of medical students and the number of medical schools doubling nationally over the past 10 years. The JCU medical school enrolled its first cohort in 2000 with a mission to address the health needs of the North Queensland region7.
JCU's 6-year undergraduate program has built a staffing profile and introduced curricular experiences and student placements to align with the school's mission to produce medical practitioners able to meet the needs of rural and remote communities. For example, students undertake a minimum of 20 weeks of clinical placements in rural and remote towns spread across the second (4-week placement), fourth (8-week placement) and sixth year (8-week placement) of the course. The program has also been decentralised, with the majority of the curriculum being delivered in Townsville for the first 3 years; while in years 4-6 approximately 60% of students are attached to clinical school sites in Cairns, Mackay and Darwin, with the remainder staying in Townsville.
A major component of the school's rural and remote mission has been the establishment of a selection process that is orientated towards attracting and preferentially selecting applicants from rural, remote and Indigenous backgrounds, often targeting secondary school students, as suggested by a sizeable body of rural literature8-11. For example, 73% of the student intake from 2000 to 2008 is from northern Australia, with 61% from locations classified as outer regional, remote or very remote on the Australian Standard Geographical Classification Remoteness Area (ASGC-RA) index (based on population size and distance from the nearest urban centre in relation to access to goods and services)12. Admission decisions are based on a selection policy that combines rurally adjusted academic achievement13, a written personal statement demonstrating attributes relevant to rural medical education and panel interview scores.
This study seeks to determine the impact of JCU medical school's policy of preferentially selecting rural and remote background students on undergraduate performance across the 6 years of the course and on graduate practice location.
Design
The JCU Bachelor of Medicine, Bachelor of Surgery (MBBS) program has produced nine graduate cohorts from 2005 to 2013. This analysis is part of an ongoing longitudinal cohort study that provides information about JCU MBBS graduate outcomes around practice location and specialty training. Previous papers have described career intent and early patterns of practice of the initial graduating cohorts from JCU's medical program14-16. Consent for graduate participation was obtained from an annual exit survey of final year JCU medical students, which has been conducted for all graduating cohorts since 2005.
Participants and data sources
A total of 835 students finished at least year 1 at the JCU medical school between the years 2000 and 2008, with a total of 768 students graduating across the first nine cohorts between 2005 and 2013 (two posthumously). Medical school application and undergraduate data were retrieved from administrative databases held by the JCU medical school and the former Faculty of Medicine, Health and Molecular Sciences.
Variables in the analysis include hometown at application to medical school, if granted advanced standing (lateral entry - entered course in year 2 or later based on previous study and experience), medical school interview score, tertiary entrance/overall position (OP) score (an Australian rank-ordered, school-leaving score; in the state of Queensland called an OP score, which ranges from 1 (highest) to 25), being conferred an Honours degree (completed an overload research project over the final 2 years of course), and if awarded a scholarship (includes 58 Medical Rural Bonded Scholarships17, 45 Rural Australian Medical Undergraduate Scholarships (RAMUS)18 and 84 Queensland Health Rural State Scholarships). The RAMUS does not require a return of service, and while return of service is required for Queensland Health Scholarship holders, this scholarship was only offered to students in the third year of the medical degree, and ceased to be offered after 2013.
Postgraduate practice location
Practice location data were obtained from several sources. Initial contact was made via a JCU School of Medicine Facebook page, which was initiated on student advice in 2005 and has been continued since for all graduating cohorts, maintaining an accurate, current contact list of alumni. Consent for subsequent contact via Facebook, email and telephone was obtained from an annual exit survey of graduating medical students, which has been conducted since 2005 as part of the JCU longitudinal tracking project on graduate outcomes. Further contact was made by email and telephone communication.
Additional data on practice location data were sourced from the Australian Health Practitioner Regulation Authority (AHPRA) website, the validity of which was checked by a comparison of twenty practice locations obtained via direct contact, showing agreement for 18/20 (90%) of cases; a similar percentage to a more in-depth study comparing the accuracy of AHPRA to personal contact19. These four strategies provided practice location data for 744 out of a total of 766 graduates (97%) from 2005 to 2013.
Defining location rurality
The ASGC-RA index (referred to as RA) was used to categorise location data - both for hometown and practice since graduation - into 'metropolitan' (RA 1), 'inner regional' (RA 2), 'outer regional' (RA 3), 'remote' (RA 4) or 'very remote' (RA 5)12. Graduates who did not spend an entire calendar year in one location were classified according to the self-defined location they provided when asked where they had spent the majority of the year. The term 'rural' is used for RA 3, and the term 'remote' for RA 4 and 5.
Bonded medical places and Commonwealth-supported places
From 2000 to 2008, 140 students - 18% of the total - were offered a place in the JCU medical program under the Bonded Medical Place (BMP) scheme. In Australia, 25% of all first-year Commonwealth-supported places (CSP) in medical schools are allocated to applicants as a BMP on the understanding that they will spend the equivalent number of course years working in an area of workforce need20.
Statistics
All data were coded numerically and entered into the computerised Statistical Package for Social Sciences v20 (SPSS, http://www.spss.com). Students accepted into the JCU medical program were assessed for bivariate relationships over a range of undergraduate variables with both their home town at time of application to medical school (coded into ASGC-RA categories; Table 1) and type of place (BMP vs CSP; Table 2) using χ2 test for trend, one-way ANOVA tests or unpaired t-tests, as appropriate.
Graduates of the JCU medical program were assessed for bivariate relationships between quartile scores for overall academic achievement in each year (overall percentage on all scored assessment items categorised into 4=highest academic quartile, 3=second highest academic quartile, 2=second lowest academic quartile or 1=lowest academic quartile) with both their home town at time of application to medical school (coded into ASGC-RA categories; Table 3) and type of place (BMP vs CSP; Table 4) using one-way ANOVA tests or unpaired t-tests, as appropriate. Statistical tests were considered significant when p<0.05. Tables 2 and 3 also include an extra column describing the p value that has been adjusted (using linear logistic regression) for the potential confounding effect of students 'being accepted under a BMP'.
Binary logistic regression analysis was used to assess how a JCU graduate's rural or remote practice location at postgraduate year 1 (PGY 1) and PGY 9 was predicted by home town at application to medical school; categorized into either a metropolitan or inner regional (RA 1 or 2), rural (RA 3) or remote (RA 4 or 5) home town. Results of the logistic regression analysis for PGY 1 and PGY 9 are presented as prevalence odds ratios (POR) together with 95% confidence intervals (95%CI).
Table 1: Associations between the hometown of 804? successful applicants to the JCU MBBS program (2000-2008) and their undergraduate characteristics
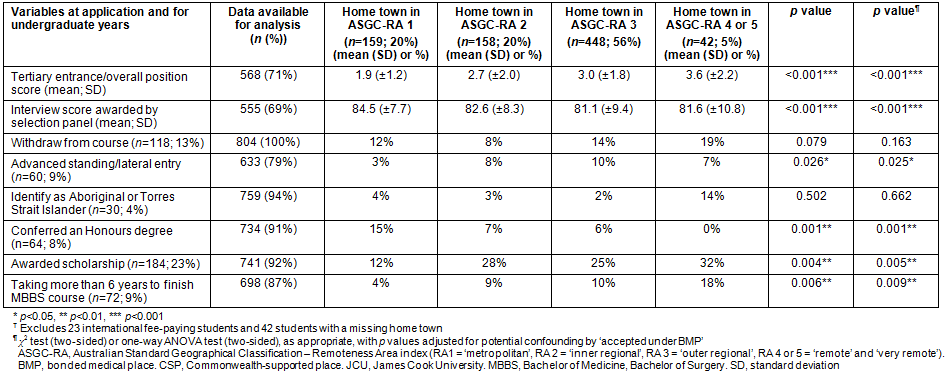
Table 2: Associations between the type of 'place' - Commonwealth-supported place or bonded medical place - given to 774? successful applicants of the JCU MBBS program (2000-2008) and their undergraduate characteristics
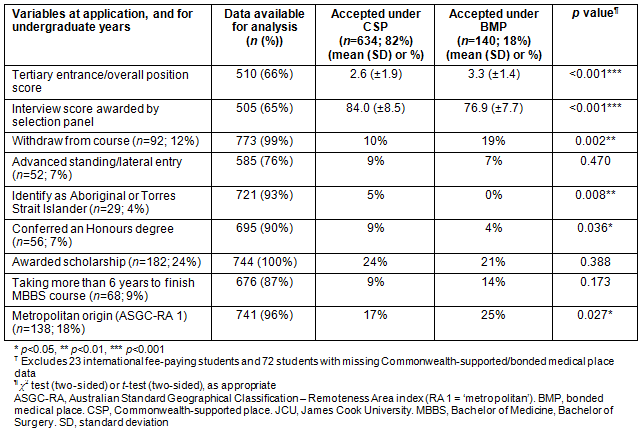
Table 3: Associations between averaged quartile scores for overall academic achievement (4=highest academic quartile, 1=lowest academic quartile) and the home town of 707? graduates from the JCU MBBS program (graduating years 2005-2013)
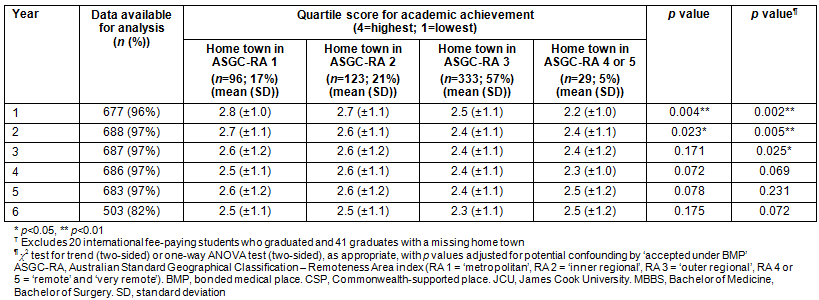
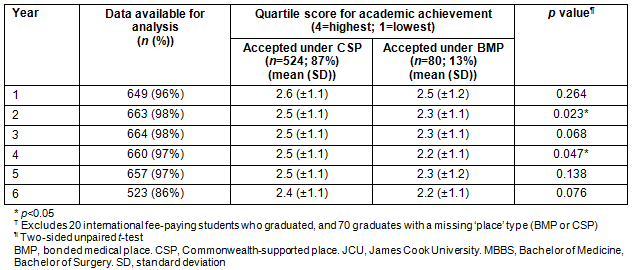
Table 4: Associations between averaged quartile scores for overall academic achievement (4=highest academic quartile, 1=lowest academic quartile) and the type of 'place' - Commonwealth-supported place or bonded medical place - given to 678? students who graduated from the JCU MBBS program (graduating years 2005-2013)
Ethics approval
Ethics approval for the study was obtained from the JCU Human Research Ethics Committee (approval # H1804).
Of the 879 students accepted into the JCU medical program between 2000 and 2008, 4% identified as an Aboriginal person or a Torres Strait Islander, 17% were accepted under the BMP scheme and 9% were advanced standing students. In terms of tertiary entrance/school-leaving score, 29% had an OP of 1 (highest academic achievement), 24% OP 2, 19% OP 3, 12% OP 4, 9% OP5 and 7%≥OP 5. Twenty-three percent received a scholarship at entry to medical school or in the first few years. During the undergraduate years, 8% completed Honours and 13% withdrew from the course.
Students were accepted from across Australia - 159 (19%) from metropolitan centres (RA 1), 158 (19%) from inner regional centres (RA 2), 448 (54%) from outer regional centres (RA 3), and 42 (5%) from remote or very remote centres (RA 4 and 5), while 23 (3%) were international fee-paying students.
Having a rural or remote home town (RA 3-5) at application was significantly associated with a poorer tertiary entrance score expressed as OP (p<0.001), a lower interview score for medical school selection (p<0.001), being less likely to be admitted into the Honours program (p=0.001), being an advanced standing/lateral entry student (p=0.025), being awarded a rurally associated scholarship (p=0.005), and taking longer to complete the 6-year course (p=0.009), than their metropolitan or inner regional peers.
Being accepted under the BMP scheme rather than a CSP was significantly associated with students having a poorer tertiary entrance score expressed as OP (p<0.001), a lower interview score for medical school selection (p<0.001), withdrawing from the course (p=0.002), being less likely to identify as Aboriginal or Torres Strait Islander (p=0.008), being less likely to be admitted into the Honours program (p=0.036), and reporting a metropolitan home town at application to medical school (p=0.027).
Having a rural or remote home town at application was significantly associated with graduates having lower quartile scores for overall academic achievement (4=highest academic quartile, 1=lowest academic quartile) than metropolitan or inner regional peers across years 1-3 (p=0.002, p=0.005 and p=0.025, respectively; Table 3). Post-hoc comparisons using the Tukey honest significant difference test indicated that the mean score for the RA 1 graduates was significantly different from that of the RA 3 graduates across all continuous variables; however, the RA 3 graduates did not differ significantly from either the RA 2 or RA 4 or 5 graduates, thus showing a gradient effect rather than a difference in the extremes between RA 1 and RA 4 or 5.
Being accepted under the BMP scheme rather than a CSP was significantly associated with graduates having a lower quartile score for overall academic achievement in year 2 (p=0.023) and year 4 (p=0.047; Table 4).
Across all postgraduate years, graduates having a rural or remote hometown at application were more likely to practise in rural or remote locations than graduates coming from metropolitan or inner regional centres. This percentage steadily increased from PGY 1 to PGY 9 for remote origin graduates, while the percentage of metropolitan or inner regional origin graduates working in rural or remote locations slowly dropped off from PGY 1 to PGY 9 (Fig1).
PORs in PGY 1 for rural origin graduates and remote origin graduates choosing to practise in rural areas in comparison to metropolitan/inner regional origin graduates were 2.6 (p<0.001; 95%CI 1.9-3.6) and 1.8 (p=0.139, 95%CI 0.9-3.6), respectively, while in PGY 9 the PORs for rural origin graduates and remote origin graduates choosing to practise in rural areas in comparison to metropolitan/inner regional origin graduates were 4.2 (p=0.017, 95%CI 1.3-13.8) and 9.5 (p=0.071, 95%CI 0.8-109.2), respectively.
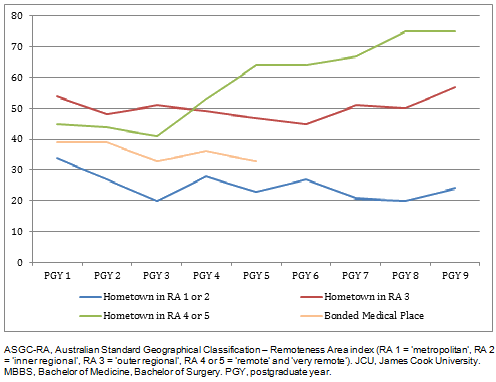
Figure 1: Association between the percentage of 700 graduates from the JCU MBBS program practising in a rural location (ASGC-RA 3-5) during their postgraduate years 1-9, with both their home town at application to medical school, and if accepted under a bonded medical place.
Discussion
This study shows that rural and remote background students admitted to the JCU medical program demonstrated some different characteristics compared to non-rural students in a range of personal, undergraduate and postgraduate factors. Students having a rural or remote hometown (RA 3-5) were significantly less likely to be admitted into the Honours program, but significantly more likely to be awarded a scholarship, be admitted as an advanced standing entry, to take longer in completing the course and to have poorer tertiary entrance score expressed as OP and lower interview scores than metropolitan or inner regional origin (RA 1 or 2) students.
These disparities may be attributed to a number of causes. Living in rural and remote locations may have limited the educational opportunities available at school and from work experience for these students21. They are also more likely to be first in family at university, often lacking the family help, support and insight into learning at tertiary level, thus resulting in lower academic performance in the early years22,23.
In the earlier, more theory-based years of the course, graduates with a rural or remote hometown had, as a group, a significantly lower quartile score for overall academic achievement across years 1-3. However, by year 4, while rural and remote origin graduates had somewhat lower averaged quartile scores as a group, this trend was no longer statistically significant, and by years 5 and 6 - which have a much greater clinical focus - the averaged quartile scores showed little difference between the groups. Thus, while these findings show graduates from more metropolitan centres have better early academic indicators than graduates from rural and remote centres, this difference appears to disappear during the clinical years, resulting in graduates of comparable academic performance regardless of location of origin.
In addition, graduates having a rural or remote hometown practise predominantly in rural and remote towns over the first nine postgraduate years - fulfilling the mission of the JCU medical school to produce medical graduates for rural and northern Australia14. This is in contrast to graduates from RA 1 or 2 towns who increasingly tend to return to urban areas over their postgraduate years. Thus, while a higher percentage of rural and remote origin JCU medical students are more likely to take an extra year to finish than the RA 1 or 2 students through failing and repeating a year, they do most often graduate and have similar academic abilities at graduation as the RA 1 or 2 students, suggesting that academic disadvantage evident at the beginning of the course is ameliorated through the support and learning opportunities available through the combination of the academic and the clinical environments.
In terms of the length of practice, rural and remote origin students are much more likely to practise in rural and remote areas, even more so as they progress into mid-career15. This is especially so for remote origin students, who are predominantly practising in rural and remote areas (which traditionally have experienced significant, ongoing medical workforce shortage) into PGY 5-9. Interestingly, quite significant numbers of students from metropolitan and inner regional centres also end up practising rurally, perhaps demonstrating a previous rural intention and/or impact of the JCU medical program.
The reality that RA 1 or 2 student applicants have better tertiary entrance scores than RA 3-5 students and are rated higher in the interviews is likely a direct impact of the JCU medical program's selection policy. The JCU medical school selects a relatively small number of outstanding candidates (based on academic history and interview performance) from a large pool of applicants from RA 1 or 2 towns. The reasons why many RA 1 or 2 students apply to JCU are unclear. However, medicine is a sought-after course, so some applicants may be looking for a place in any location, while others may be interested in the rural/remote or tropical focus, or the prospect of direct entry from high school.
The study also shows, unsurprisingly, that scholarships are more likely to be held by rural and remote origin students, reflecting the reality that most scholarships available in the JCU medical school are rurally linked, requiring a rural background or commitment to work in a rural area after graduation. In addition, the withdrawal rate is somewhat higher in rural and remote origin students than metropolitan students, though not significantly. In a systematic review of medical school dropouts, the only common factor was lower entry qualifications24. However, it is likely that students from smaller rural or remote towns may face additional challenges beyond any differences in academic ability, study skills and the norms and expectations of higher learning, for example lack of support mechanisms and social networks, as well as difficulty adjusting to life in a larger regional location25.
Interestingly, RA 1 students were far more likely to be admitted into the Honours program than students from other areas. Offers of a place in the Honours program are made to students with higher levels of academic achievement in years 1-4, predominantly before the gap narrows between rural and non-rural students. Additionally, RA 1 students often have more confidence in their ability to pursue Honours associated with previous attendance at non-government schools and having parents who are professionals26. Alternatively, the higher rates of RA 1 students undertaking Honours could be driven by concern over the availability of intern places, as recent media discourse quoting the Australian Medical Students Association may be inducing non-bonded students to complete an integrated Honours program to increase their options for intern places27,28.
BMP students show many similar trends to rural students in pre-medical school and undergraduate performance indicators - poorer tertiary entrance/OP scores, lower interview scores, less likely to be admitted into the Honours program than their peers - even though these students are much more likely to come from metropolitan areas. BMP students were also significantly more likely to withdraw from the course than their peers. However, BMP students who went on to graduate had, on average, only slightly worse (non-significant except for years 2 and 4) quartile scores for academic achievement than their CSP peers. Thus, while 19% of BMP students drop out of the course, they do most often graduate and have similar capabilities at graduation as their CSP peers. However, graduates accepted under the BMP scheme had lower engagement in rural practice than their rural origin peers in the 5 years of data available, although higher than their metropolitan/inner regional-origin peers.
Limitations
While the database is mostly complete, for example postgraduate practice location has only 3% of data missing, missing data may be a limitation for a number of variables, including tertiary entrance/OP score and interview score (about a third of data missing), whether the student was accepted into the medical program as advanced standing (25% missing), and if the student was accepted under a BMP or CSP (9% missing).
Another significant limitation of this study is that the findings are specific to JCU medical graduates. The nature of the JCU MBBS program - an undergraduate course that preferentially selects students with a rural background - is not representative of all medical students or graduates across Australia. In addition, student home town was self-defined as 'your hometown at application to medical school', which may not always reflect where they had spent the majority of their life before medical school.
Additionally, while care has been taken to ensure the accuracy of graduate destination data of the JCU medical school's first nine cohorts, it has been collected from a variety of sources, with 87% of student practice location data being self-reported and the additional 10% obtained from the AHPRA website, which, based on correlations between data from this website and data from personal contact, is estimated to be only 90% accurate19.
This study demonstrates significant associations between selecting students from rural and remote backgrounds, their academic performance in the early undergraduate years and their postgraduate practice location. However, as students progressed into the later clinical years of the course, these early differences in academic performance associated with rurality of hometown were no longer statistically significant.
Using outcome indicators such as students' selection data, yearly academic achievement and other pre- and post-graduation variables has provided useful evaluative measures of the mission of the JCU medical program. It may be concluded that JCU's policy of preferentially selecting students with rural and remote home towns contributes in producing the necessary medical workforce in rural and remote Australia without compromising academic standards. However, further research is required into the support needs of rural and remote students in the preclinical years, and into the reasons why a higher proportion of remote origin students withdraw from the course.
This data also adds to an understanding of the 'outcome of interest'. While many studies use conventional academic measures such as examination results and progression rates, the authors suggest that when academic standards are met, then the outcome of interest is what a graduate does with his/her degree, in this case location of practice and the communities they serve.
References
1. Ricketts TC. The changing nature of rural health care. Annual Review of Public Health 2000; 21: 639-657.
2. Productivity Commission. Australia's health workforce. Canberra: Australian Government, 2005.
3. Walker JH, DeWitt DE, Pallant JF, Cunningham CE. Rural origin plus a rural clinical school placement is a significant predictor of medical students' intentions to practice rurally: a multi-university study. Rural and Remote Health 12: 1908. (Online) 2012. Available: www.rrh.org.au (Accessed 22 September 2015).
4. Playford DE, Evans SF, Atkinson DN, Auret KA, Riley GJ. Impact of the Rural Clinical School of Western Australia on work location of medical graduates. Medical Journal of Australia 2014; 200(2): 104-107.
5. Rabinowitz H, Paynter N. The role of the medical school in rural graduate medical education: pipeline or control valve. Journal of Rural Health 2000; 16(3): 249-253.
6. Barrett F, Lipsky M, Lutifyya M. The impact of rural training experiences on medical students: a critical review. Academic Medicine 2011; 86(2): 259-263.
7. Hays R, Stokes J, Veitch J. A new socially responsible medical school for regional Australia. Education for Health 2003; 16(1): 14-21.
8. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 2009; 9: 1083.
9. Eley R, Hindmarsh N, Buikstra E. Informing rural and remote students about careers in health: the effect of health careers workshops on course selection. Australian Journal of Rural Health 2007; 15(1): 59-64.
10. Bly J. What is medicine? Recruiting high-school students into family medicine. Canadian Family Physician 2006; 52: 329-334.
11. Fraser J, Alexander C, Simpkins B, Temperley J. Health career promotion in the New England area of New South Wales: a program to support high school career advisers. Australian Journal of Rural Health 2003; 11(4): 199-204.
12. Australian Bureau of Statistics. ASGC Remoteness Classification: purpose and use. Census paper # 03/01. Canberra: Commonwealth of Australia, 2003.
13. Hays RB, Bower AJ. Modifying academic ranking of rural and remote medical school applicants. Medical Journal of Australia 2001; 174(7): 371-372.
14. Veitch C, Underhill A, Hays R. The career aspirations and location intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation Rural and Remote Health 6: 537 (Online) 2006. Available: www.rrh.org.au (Accessed 22 September 2015).
15. Sen Gupta T, Murray R, Hays R, Woolley T. James Cook University MBBS graduate intentions and intern destinations: a comparative study with other Queensland and Australian medical schools. Rural and Remote Health 13: 2313 (Online) 2013. Available: www.rrh.org.au (Accessed 22 September 2015).
16. Sen Gupta T, Woolley T, Murray R, Hays R, McCloskey T. Positive impacts on rural and regional workforce from the first seven cohorts of James Cook University medical graduates. Rural and Remote Health 14: 2657. (Online) 2014. Available: www.rrh.org.au (Accessed 22 September 2015).
17. Department of Health. Medical Rural Bonded Scholarship (MRBS) Scheme 2014. (Online) 2014. Available: http://health.gov.au/mrbscholarships (Accessed 20 November 2014).
18. National Rural Health Alliance. Rural Australia Medical Undergraduate Scholarship (RAMUS) Scheme. (Online) 2014. Available: http://ramus.ruralhealth.org.au (Accessed 20 November 2014).
19. Playford D, Power P, Boothroyd A, Manickavasagar U, Ng WQ, Riley G. Is the National Registration website (Australian Health Practitioner Regulation Agency) effective in tracking Australian medical graduates' rural work? Australian Journal of Rural Health 2013; 21(5): 249-253.
20. Department of Health. Bonded Medical Places (BMP) Scheme. (Online) 2014. Available: http://www.health.gov.au/bmpscheme (Accessed 20 November 2014).
21. Perry L, McConney A. School socio-economic composition and student outcomes in Australia: implications for educational policy. Australian Journal of Education 2010; 54(1): 72-85.
22. Bail C, Naylor R, Arkoudis S. The first year experience in Australian universities: findings from two decades 1994-2014. Melbourne: The University of Melbourne, 2015.
23. Southgate E, Kelly BJ, Symonds IM. Disadvantage and the 'capacity to aspire' to medical school. Medical Education 2015; 49(1): 73-83.
24. O'Neill LD, Wallstedt B, Eika B, Hartvigsen J. Factors associated with dropout in medical education: a literature review. Medical Education 2011; 45: 440-454.
25. Devlin M, McKay J. Reframing 'the problem': students from low socio-economic status backgrounds transitioning to university. In H Brooke, D Fergie, M Maeorg, D Michell (Eds). Universities in transition: foregrounding contexts of knowledge in the first year experience. Adelaide: University of Adelaide Press, 2014; 97-126.
26. Laurence CM, Zajac IT, Turnbull DA, Sumner KE, Fleming J. Applicants to the University of Adelaide medical school: influences, motivation and alternative career choices. Focus on Health Professional Education 2013; 14(2): 81-90.
27. Colbin M. Medical students worried about a shortage of internships. ABC News PM. (Online) 2012. Available: http://www.abc.net.au/pm/content/2012/s3516456.htm Accessed 24 April 2014).
28. Preiss B, Medew J. Medical students fear intern glut. (Online) 2013. Available: http://www.smh.com.au/national/medical-students-fear-interns-glut-20130205-2dwfe.html (Accessed 22 September 2015).



