The literature devoted to issues concerning the rural health workforce is prevalent and robust throughout the world. The common concern across this literature is one of providing adequate and equitable health care to people who live in rural and remote locations1. While geography is the ubiquitous factor underlying the difficulties of providing this health care, cultural and socioeconomic factors are also contributing concerns to recruiting and retaining a health workforce who can cope with the professional and personal requirements of working in challenging environments.
Australia has attempted to reverse this inequity on many levels, most prominently through education, both undergraduate and postgraduate. The Rural Incentives Program of 1992 was the catalyst for rural workforce initiatives at the undergraduate level followed closely by the development of a national network of rural clinical schools across the major Australian medical schools during 2000-20012,3. In 1997, Flinders University in South Australia took a truly innovative step and began the first longitudinal integrated clerkship4,5, which was modelled on successful programs already established in North America6-13. Since 2000, Australian medical schools have embarked on a variety of rurally focused clinical programs employing a mixture of rural clinical placements from several weeks to a year14-21.
The growing consensus from more than 20 years of research is that the best predictors of medical students intending to and taking up a rural medical career are rural background22,23 and positive rural experiences during medical school11,15,24,25. A recent study by Jones et al26 using a large Australia-wide student sample provided confirmatory data on the positive association between medical students' intention to become a rural doctor and exposure to rural practice during clinical placements. However, they found that the best predictors were having a rural background and an intention to go rural early in their medical studies26.
Likewise at the postgraduate vocational training level, in particular for general practice, there have been various initiatives such as rural training places and incentive payments for general practice registrars to train on a rural general practice pathway. The system that has been in place for the last decade is Commonwealth Government led, to train and support early-career general practitioners (GPs) to practise in rural Australia27. The Commonwealth Government funds General Practice Education and Training to deliver Australian general practice training through 17 regional training providers (RTPs)28. The RTPs are accredited to provide both a general training pathway (3 years), leading to the Fellowship of Royal Australian College of General Practice (ACRRM), and a rural pathway (4 years) resulting in Fellowship of ACRRM. Additionally, the ACRRM delivers unique rural training, the Independent Pathway, which comprises 4 years of distance supported education and allows registrars to train while working in their own rural or remote practice.
Parallel to these strategies has been an underlying notion that it takes a certain type of person to live and work in rural clinical practice. The stuff of folklore perhaps but there continue to be similarities between today's long-serving rural doctors and those of decades ago - living and working in professional isolation with enormous responsibility and few resources. In support of this notion there is a substantial literature around the influence of personality traits on individual career decisions with several studies identifying personality characteristics and their association with speciality choices in most medical disciplines29-34.
Several studies have focused on how personality profiles portray individuals choosing or with the intention of choosing certain medical disciplines30,33,35,36, and how traits might further differentiate between rural and non-rural doctors and medical students37-39, nurses and nursing students40,41, and allied health professionals42. Personality can never be a lone predictor of an individual's career choice and the same can be said about choice of rural or non-rural context. Nevertheless it is not unreasonable to presume that certain people are attracted to specific attributes of a job or lifestyle, and studies show that personality attributes can differ significantly between rural and urban doctors working in obviously different life and work contexts37,39.
Alongside this concept is a vital attribute for rural living: resilience. Resilient individuals tend to recover quickly from setbacks or trauma, learn from their experience, and are better able to cope with challenges in life43. Doctors and medical students benefit from a high degree of resilience to manage the challenges of the profession such as high workload, emotional and physical demands and patient expectations44. It may be argued that even higher levels of resilience may be required of doctors working or training in a rural environment. Therefore this study aimed to take a step further toward understanding if personality traits influence a rural or non-rural practice choice by describing the predominant personalities of existing registrars on either a rural or general GP training pathway.
This study strives to obtain more information about which individuals choose rural medicine and with this information how recruitment, training and retention of a future workforce may be enhanced. While this rationale has been explored with medical students using intention as the dependent variable, registrars are that much closer to their final career choice, and therefore may provide more reliable indicators of the notion of 'who attracts whom' to work in rural medicine.
Participants
From 2011 to 2013, a cross-sectional design sampled GP registrars across all states in Australia. Three distinct Australian vocational training pathways for general practice were studied. The study sample comprised four groups. Three came from RTPs - one each in the states of Queensland (Qld), South Australia (SA) and Western Australia (WA) - and one from ACRRM's Independent Pathway, representing trainees across Australia.
Measures
A self-report questionnaire included the Temperament and Character Inventory (TCI-R140) to identify the seven basic dimensions of personality45, and the Resilience Scale, which measures the essential characteristics of resilience46. Basic sociodemographics were also collected (gender, age, marital status, rural background, considering oneself rural, intention to practice rurally, training pathway, intern training location, membership of a rural club during medical school, attended a rural clinical school). Questionnaires were administered by each training group using identical versions either hard copy, administered in a classroom situation, or online (Survey Monkey).
Temperament and character
The TCI is based on Cloninger's psychobiological theory of personality, which distinguishes between the personality domains of moderately stable temperament traits that vary according to individual differences in behavioural conditioning (ie the emotional core of personality), and character traits that develop across the lifespan toward socially approved norms (ie the cognitive domain of personality)47,48. The TCI is validated in adult populations across the world including the USA, Australia, Europe, Israel and Asia, and each scale correlates with other tests of personality, including the five-factor personality model49, performing as well or better than other modern tests in predicting mature coping50,51. The 140-item version, using a five-point Likert scale from 1 ('absolutely false') to 5 ('absolutely true'), was administered. The four temperament traits are novelty seeking, harm avoidance, reward dependence and persistence. The three character traits are self-directedness, cooperativeness and self-transcendence. Each trait is multifaceted. High and low descriptors are summarised in Table 1.
Table 1: High and low descriptors for each temperament and character trait of the Temperament and Character Inventory
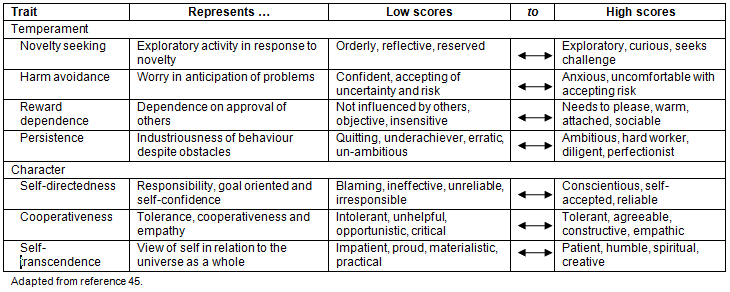
Resilience
The Resilience Scale is a self-reported measure of an individual's ability to respond to adversity. The 26-item version uses a seven-point Likert-scale from 1 ('strongly disagree') to 7 ('strongly agree'). The scale reflects five core characteristics of resilience: perseverance, equanimity, meaningfulness, self-reliance and existential aloneness52. Perseverance indicates a willingness to persist despite adversity. Equanimity refers to balance - the ability to 'take what comes' in life. Meaningfulness is the acknowledgement that life has a purpose and is therefore worth living. Self-reliance reflects an individual's self-belief and their dependence on their own strengths and past success to support their decisions. Existential aloneness is the awareness that every person is unique and this realisation allows a sense of independence and freedom. This study's analysis used the single composite score of resilience as its primary planned criterion of resilience; the study also explored relations with the subscales to clarify understanding.
Analysis
Tests of normality (Kolmogorov-Smirnov statistic) showed the TCI and Resilience Scale scores for the whole sample were normally distributed. The internal consistency (Cronbach alpha) of the Resilience Scale was 0.89, the TCI ranged from 0.84 to 0.88 for character and from 0.76 to 0.89 for the temperament scales. Chi-squared tests examined proportions in the demographic variables. The relationships between demographic characteristics and traits levels were investigated using a series of multivariate analyses of variance (MANOVAs) with Bonferroni post-hoc correction to identify differences between variables and an adjusted α=0.01 to increase sensitivity. ANOVA with post-hoc comparisons examined differences in trait levels between the four registrar groups. These tests used α=0.05 with an accompanying 95% confidence level. All data were analysed using Statistical Package for the Social Sciences v22 (SPSS Inc., http://www.spss.com).
Ethics approval
Ethics approval was obtained through the National Ethics Application Form of the National Health and Medical Research Council of Australia and subsequent approval from the University of Queensland (#2010001618), University of Adelaide (#H-047-2011) and Flinders University (#5134).
Demographics
The questionnaire was completed by 451 out of 785 registrars identified, giving a response rate of 57%.
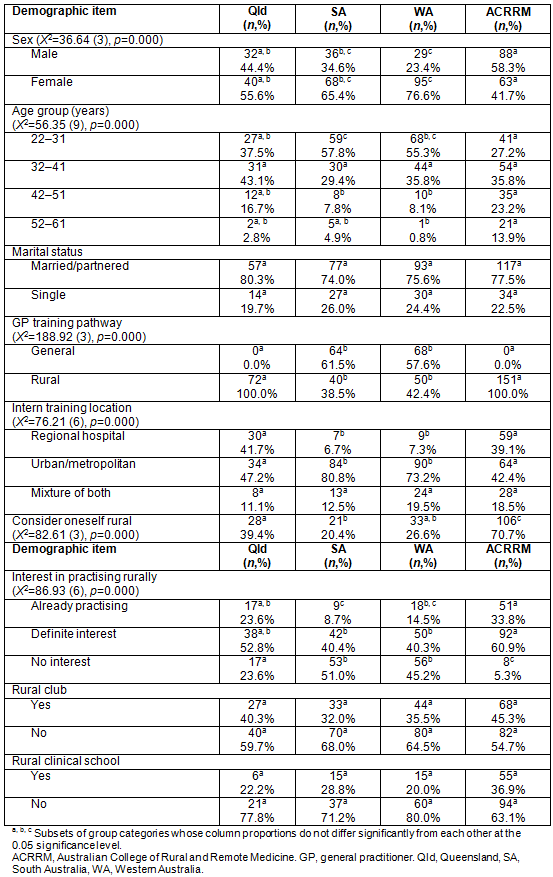
Table 2 shows the demographic variables across and between the four registrar groups. The whole sample was primarily female (59%) and aged 22-31 years (44%), married or partnered (77%) and on the rural training pathway (70%). Looking between groups shows that significantly more ACCRM registrars were male (58%). The SA and WA registrars were mainly female (65% and 77% respectively). Younger registrars (22-31 years) were more prevalent in SA and WA, and older groups (42-51, 52-61 years) more prevalent among ACRRM registrars. Qld and ACRRM registrars were exclusively in the rural training pathway while the majority of registrars in SA and WA were on the general path.
The majority of all registrars did their intern training in an urban or metropolitan hospital. Significantly more Qld (42%) and ACRRM (39%) registrars interned in a regional hospital while SA and WA registrars interned almost exclusively in urban or metropolitan areas (81% and 73% respectively), reflecting the geography of SA and WA (very few regional hospitals can accommodate intern training). Significantly more ACRRM registrars considered themselves to be 'rural' and reported a definite interest in practising rurally or were already training in a rural location.
Table 2: Demographic variables for the four registrar training groups
Comparison of temperament and character trait levels of the registrar sample with population norms
The mean raw scores for each temperament and character trait were ranked against the population norms for the TCI by group and total sample53. Looking at the combined sample and each individual registrar group showed that they all ranked 'average' in the temperament traits of novelty seeking and harm avoidance, 'very high' in reward dependence and persistence, 'very high' in the character traits, self-directedness and cooperativeness and 'very low' in self-transcendence compared to population norms.
Effect of demographic variables on temperament and character trait levels in the combined sample
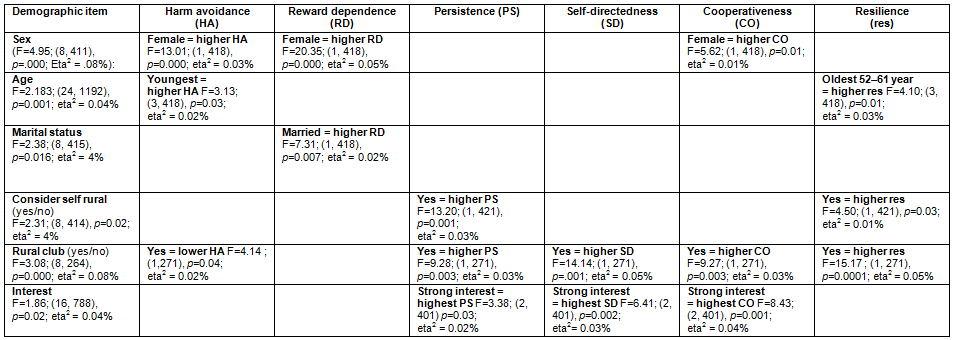
The MANOVA showed that several demographic variables had significant main effects on the levels of traits in the sample, most with medium effect sizes (partial eta2). Table 3 outlines the significant main effects of each independent variable with the univariate follow-up. Where appropriate, post-hoc testing identified where differences occurred. The only interaction detected was between age and gender (F=1.73; (24, 1192), p=0.001; eta2=0.03%) for reward dependence (F=6.12 (3), p=0.000; eta2=0.04%).
Being female, younger and married inclined towards higher levels of harm avoidance, reward dependence and cooperativeness while being older tended towards higher levels of resilience. Considering oneself rural and having a strong interest in rural practice showed higher levels of persistence, self-directedness and resilience. Registrars who belonged to a rural club while at medical school tended toward lower levels of harm avoidance, with higher persistence, self-directedness, cooperativeness and resilience.
Table 3: MANOVA summary: Effects of demographic variables on dependent variables (temperament and character traits and resilience)
Comparison of temperament and character traits levels between registrar groups
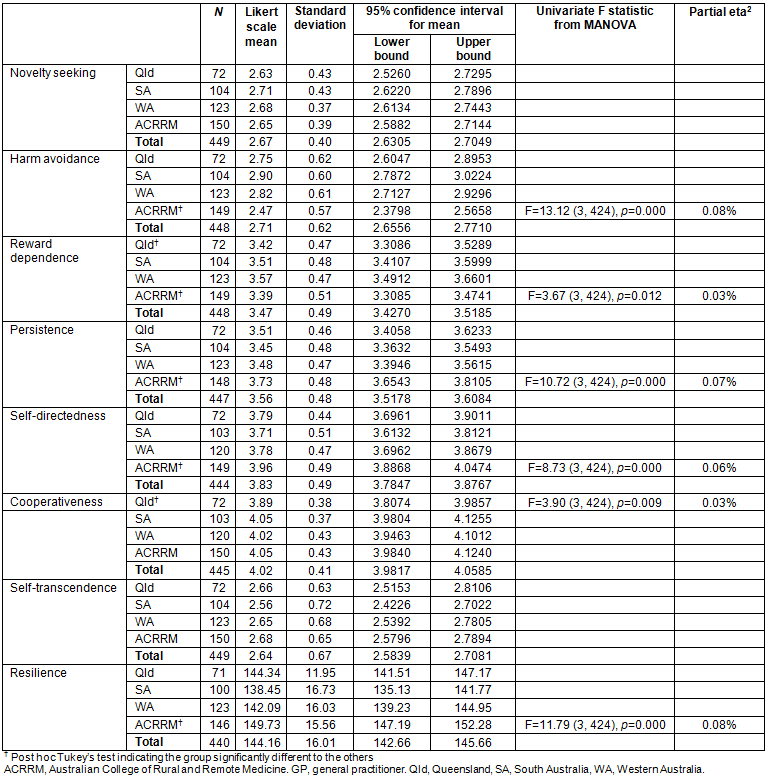
There were significant differences between the four registrar groups in most traits. ACRRM registrars have significantly lower of levels of harm avoidance and higher levels of persistence, self-directedness and resilience compared to all other groups. Table 4 shows the moderate to strong effect sizes associated with these differences. ACRRM registrars were also found to be lower in levels of reward dependence and Qld registrars lower in cooperativeness but with a small effect size.
Because all ACRRM and Qld registrars train in a rural pathway, the authors looked for trait level differences between the rural and general paths and found that all general path registrars had higher levels of reward dependence compared to all rural path registrars (t=3.46, 439; p=0.001). Rural and general path registrars in just the SA and WA RTP groups were compared, but there was no significant differences between them in any trait.
Table 4: ANOVA comparing all four registrar training groups in levels of temperament and character traits and resilience
Discussion
This article builds on previous work that increasingly portrays doctors who work in and students who intend to work in rural and remote locations with a profile of temperament and character traits different to that of their urban counterparts37,38,54 This profile is most notable by levels of harm avoidance that are lower and persistence and self-directedness that are higher than for doctors and students who are not or do not intend on practising rurally. This combination of trait levels has been shown to correlate strongly with high levels of resilience, which the findings of the present study corroborate55.
This sample includes GP registrars training across three distinct Australian vocational training pathways. However, only the registrars in the independent rural pathway of ACRRM portrayed the above profile and differed significantly from the other three groups. It is notable that the Qld registrars, also training with an Australian general practice training provider but offering only a rural training pathway, showed similar but non-significant trends in most trait levels to the ACRRM registrars. Furthermore, when just the pathways were compared, the only difference seen was higher levels of reward dependence amongst the general path registrars compared to rural path registrars. Looking at just the SA and WA RTPs and comparing their rural and the general path registrars, no differences were detected.
These data suggest that individuals training with the SA and WA training providers are attracting similar individuals in regards to levels of certain temperament and character traits, regardless of their chosen training path. This may be explained in part by the differences in training programs: general and rural training paths are offered in both SA and WA, whereas only rural pathways are offered in Qld and by ACRRM. This factor may attract doctors who have similar backgrounds, career interests and, it would seem, trait profiles. Qualitative research associated with this study explored the many personal reasons why registrars might choose a particular training provider or pathway. These will be reported elsewhere. Nevertheless, it is reasonable to assume that registrars with a strong interest and intention to practise rurally would seek out a training provider with a rural focus (ie ACRRM or the Qld RTP), which allows exclusive clinical exposure and lifestyle in a rural setting. In contrast, the SA and WA RTPs offer a more integrated program between the rural and general pathways, which may be attracting doctors who, even though they are training on the rural path, are not as firmly devoted to future rural practice.
The demographic characteristics of the sample highlight several significant differences between the registrar groups. Compared to the WA and SA registrars, the ACRRM and QLD registrars are mostly male, older, consider themselves to be 'rural', have a definite interest in rural practice and are interned in a regional hospital. These different demographic characteristics are important because the MANOVA highlighted significant main effects of several demographic variables on levels of personality traits, and these fit with the differences seen between the four registrar groups. For example, gender shows a strong effect size on levels of harm avoidance, reward dependence and cooperativeness. The univariate tests showed that women are higher in levels of each of these traits, and this may contribute to the higher levels of these traits among the WA and SA registrars, who were primarily female. Correspondingly, the fewer female ACRRM registrars may have contributed to lower levels of harm avoidance and reward dependence seen in that group.
Age also shows moderate effects on harm avoidance and resilience, with older age groups lower in levels of harm avoidance and higher in resilience, congruent with the levels of each found in the older ACRRM cohort. Similarly, reporting a stronger interest in practising rurally and considering oneself to be 'rural' (ie rural background, experience, lifestyle) were associated with lower harm avoidance and higher persistence, self-directedness and resilience. These were the same trends seen to be significant among ACRRM registrars.
It was unexpected to find that belonging to a rural club showed a low to moderate effect on levels of most traits: harm avoidance, persistence, self-directedness, cooperativeness and resilience. Overall, 40% of the sample reported belonging to a rural club but there were no differences in the proportions between the four registrar groups. The degree of exposure to rural lifestyle and clinical practice varies widely between rural clubs, and membership ranges from students who are devoted to rural medicine to those just wanting to get some experience. It might be supposed that interest in belonging to a rural club is in part a reflection of an individual's attitudes toward rural experiences and supports studies that show exposure to rural practice and life during medical training can dispel preconceptions, good and bad, about its realities56. However, in this respect it is hard to explain why attending a rural clinical school did not show a similar main effect on some traits. A possible explanation might be that rural club membership is completely voluntary whereas some rural clinical schools must ballot students to meet their quota and therefore it is likely that some do not have a strong interest in a rural career. The present study can only speculate that this difference may have some influence on eventual training choice.
It is of note that the sample's average temperament and character trait levels compared to population norms show them as average in novelty seeking and harm avoidance, very high in reward dependence, self-directedness, persistence and cooperativeness, and very low in self-transcendence. This profile has been shown previously as a combination of trait levels common to high-functioning and psychologically mature personalities57. In particular, being high in both self-directedness and cooperativeness is consistently related to a healthy character. Additionally, this sample was also low in levels of self-transcendence which indicates a character that is organised and mature. Persons with organised characters tend to be practical, strong willed and goal oriented, and most often emerge as leaders among their peers58.
There are several limitations of this study to be considered. The design is cross-sectional and therefore excludes any causal conclusions. Furthermore, the self-selected and self-reported nature of data has potential for bias from participants. However, this study's data, although not generalisable, was gathered across several states and the findings support previous research in this area.
Implications for rural doctor training
The implications of the data to the recruitment and training of GP registrars goes further than identifying groups of individuals with similar personality trait patterns. Although the whole sample is portrayed as relatively homogenous in comparison to population norms it is the combination of the levels of individual traits that the literature continues to suggest is different between rural and non-rural doctors37,39,54 and, as this article has shown, between registrars on a rural or general training pathway.
Importantly, the combination of trait levels that tends to differentiate registrars (low harm avoidance, high self-directedness and persistence) correlate strongly with high levels of resilience and corroborate previous research55. It can be argued that resilience is not a trait on its own but is driven by an individual's combination of stable temperament traits, which equip every individual with a certain capacity for resilience, and is further developed by character traits that are influenced by one's environment, life experiences and personal challenges.
Considering first the temperament trait harm avoidance, as pessimistic worry in anticipation of problems, it is a measure of general anxiety. People with low harm avoidance tend to more accepting of uncertainty and a degree of risk, decisive and confident and overall less anxious - all of which are key attributes for a rural doctor. While harm avoidance indicates an emotional drive to avoid harm (i.e. avoid risks and uncertain situations), even as a relatively stable temperament trait, there are ways that high levels of harm avoidance could be moderated through training activities to increase self-awareness. Examples are identifying cues that trigger anxiety, encouraging activities that take a trainee out of their 'comfort zone' (under supervision) and challenging them to deal with uncertainty, or developing activities to gradually increase confidence, and even learning relaxation methods.
Another temperament trait is reward dependence, which typifies behaviour in response to cues of social reward. This study is congruent with previous work showing women as higher in levels of reward dependence compared to men. People who are lower in reward dependence tend to be more independent, not strongly influenced by others and not as social or socially driven. On the other hand, high reward dependence is indicative of people who are warm and friendly, traits that are desirable for doctors. Yet in certain situations high reward dependence must be carefully 'balanced' in context with the individual's degree of social attachment and dependence. Certain situations could be particularly problematic for doctors in small communities where social attachment to patients as friends may cloud clinical judgement. Role play and scenarios could raise awareness of potential issues and how a trainee might cope in similar situations.
Persistence is the temperament trait that represents behaviour despite frustration, fatigue and reinforcement. People who are high in persistence are industrious, ambitious and hard working. It is common for high-achieving, intelligent individuals to be very high in levels of persistence and this study sample, along with previous work, consistently demonstrates this in medical doctors and students. However, excessively high levels of persistence can lead to a perfectionist attitude. This is a particular dilemma for doctors. Perfectionism promotes harsh judgements by self and others and is a precursor to depression and burnout. Training might address a perfectionist attitude by helping the individual accept their limitations, to learn from failure and to set realistic goals. Low persistence might be increased by working on accomplishment of tasks with intermittent rewards and sticking with a task until it is complete.
The character trait self-directedness represents the self-concept of being responsible and goal oriented. Individuals high in levels of self-directedness are responsible, conscientious and self-accepted. Self-directedness is the most definitive predictor of a mature and resilient personality57. Therefore high self-directedness has many advantages and is a positive moderator of other traits and trait combinations that would otherwise be less desirable. Low levels of self-directedness could be enhanced through training by focusing on goal setting and achievement activities with an increased awareness of responsibilities.
Doctors and medical students benefit from a high level of resilience to cope with and manage the challenges of the profession, arguably more so for rural practice. Along with certain demographic characteristics, the combination and levels of temperament (stable) and character (developmental) traits provide support for the notion of a mixture of personal characteristics that may be indicative of individuals best suited to rural and remote medicine. Further investigation is needed to determine whether individuals with a certain pattern of personal traits are attracted to rural practice training or whether the training itself, in part by exposure to rural life and rural medical practice, selects for those who are most suited to and will eventually choose to practice in a rural location. The former suggests that identifying individuals with a particular trait pattern could be beneficial in recruitment and counselling toward a rural clinical career. The latter suggests that the current initiatives and training programs in place at the undergraduate and postgraduate medical education level are vital in attracting and maintaining the level of interest and continuity of training for those individuals who have intentions toward a rural career. These scenarios are not mutually exclusive, which highlights the importance of providing sustained rural training opportunities to both attract and retain Australia's future rural workforce.
Acknowledgements
The authors acknowledge members of the project team: Janice Bell, Marita Cowie, Taryn Elliot, Jane Harte, Timothy Kelly, Scott Kitchener, Kim Madison, Robyn Synnott, David Wilkinson. This study was supported by an Australian Research Council Grant LP110102082.
References
1. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention. (Online) 2010. Available: http://whqlibdoc.who.int/publications/2010/9789241564014_eng.pdf (Accessed 13 November 2015).
2. Australian Government Department of Health. Review of Australian Government health workforce programs. (Online) 2013. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/review-australian-government-health-workforce-programs (Accessed 13 November 2015).
3. Australian Government Department of Health. Rural clinical training and support (RCTS) 2011-2014 - operational framework. (Online) 2012. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/work-st-rcts-2011-14 (Accessed 13 November 2015).
4. Worley P, Prideaux D, Strasser R. Why we should teach undergraduate medical students in rural communities. Medical Journal of Australia 2000; 172: 615-617.
5. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The parallel rural community curriculum: an integrated clinical curriculum based in rural general practice. Medical Education 2000; 34(7): 558-565.
6. Brazeau NK, Potts MJ, Hickner JM. The Upper Peninsula Program: a successful model for increasing primary care physicians in rural areas. Family Medicine 1990; 22: 350-355.
7. Steams JA, Steams MA, Glasser ML, Londo RA. Illinois RMED - a comprehensive program to improve the supply of rural family physicians. Family Medicine 2000; 32: 17-21.
8. Halaas GW. The rural physician associate program: new directions in education for competency. Rural and Remote Health 5: 359. (Online) 2005. Available: www.rrh.org.au (Accessed 19 December 2014).
9. Schauer R, Schieve D. Performance of medical students in a nontraditional rural clinical program. Academic Medicine 2006; 81: 603-607.
10. Zink T, Halaas G, Finstad D, Brooks J. The Rural Physician Associate Program: the value of immersion learning for third year medical students. Journal of Rural Health 2008; 24: 353-359.
11. Rabinowitz HK, Diamond JJ, Markham FW, Wortman M. Medical school programs to increase the rural physician supply: a systematic review and projected impact of widespread replication. Academic Medicine 2008; 83: 235-243.
12. Norris TE, Schaad DC, DeWitt D, Ogur B, Hunt DD, members of the consortium of longitudinal integrated clerkships. Longitudinal integrated clerkships for medical students: an innovation adopted by medical schools in Australia, Canada, South Africa, and the United States. Academic Medicine 2009; 84(7): 902-907.
13. 13. Tesson G, Hudson G, Strasser R, Hunt D. The Making of the Northern Ontario School of Medicine: a case study in the history of medical education. Montreal, ON: McGill-Queen's University Press, 2009.
14. Eley D, Baker P. Does recruitment lead to retention? Rural clinical school training experiences and subsequent intern choices. Rural and Remote Health 6(1): 511. (Online) 2006. Available: www.rrh.org.au (Accessed 19 December 2014).
15. Eley D, Young L, Baker P, Wilkinson D. Developing a rural workforce through medical education: lessons from down under. Teaching and Learning in Medicine 2008; 20(1): 53-61.
16. Eley D, Baker P. The value of a rural medicine rotation on encouraging students toward a rural career: clear benefits from the RUSC program. Teaching and Learning in Medicine 2009; 21(3): 220-224.
17. Critchley J, DeWitt DE, Khan MA, Liaw ST. A required rural health module increases students' interest in rural health careers. Rural and Remote Health 1(7): 688. (Online) 2007. Available: www.rrh.org.au (Accessed 19 December 2014).
18. McDonnel Smedts A, Lowe MP. Clinical training in the top end: impact of the Northern Territory Clinical School, Australia, on the Territory's health workforce. Rural Remote Health 7: 723. (Online) 2007. Available: www.rrh.org.au (Accessed 19 December 2014).
19. Worley P, Martin A, Prideaux D, Woodman R, Worley E, Lowe M. Vocational career paths of graduate entry medical students at Flinders University: a comparison of rural, remote and tertiary tracks. Medical Journal of Australia 2008; 188(3): 177-178.
20. Sen Gupta TK, Hays RB, Kelly G, Buettner PG. Are medical student results affected by allocation to different sites in a dispersed rural medical school? Rural and Remote Health 11: 1511-1515. (Online) 2011. Available: www.rrh.org.au (Accessed 19 December 2014).
21. Playford DE, Cheong E. Rural undergraduate support and coordination, rural clinical school, and rural Australian medical undergraduate scholarship: rural undergraduate initiatives and subsequent rural medical workforce. Australian Health Review 2012; 36(3): 301-307.
22. Laven GA, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11(5): 277-284.
23. Somers GT, Strasser R, Jolly B. What does it take? The influence of rural upbringing and sense of rural background on medical students' intention to work in a rural environment. Rural and Remote Health 7: 706. (Online) 2007. Available: www.rrh.org.au (Accessed 19 December 2014).
24. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: www.rrh.org.au (Accessed 19 December 2014).
25. Wilkinson D, Laven GA, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37(9): 809-814.
26. Jones MP, Bushnell JA, Humphreys JS. Are rural placements positively associated with rural intentions in medical graduates? Medical Education 2014; 48(4): 405-416.
27. Campbell DG, Greacen JH, Giddings PH, Skinner LP. Regionalisation of general practice training - are we meeting the needs of rural Australia? Medical Journal of Australia 2011; 194: S71-S74.
28. Australian Government Department of Health. Commonwealth Government General Practice Education and Training. (Online). Available: http://www.gpet.com.au/Home/Home (Accessed 18 December 2014).
29. McManus IC, Lefford F, Furnham AF, Shahidi S, Pincus T. Career preference and personality differences in medical school applicants. Physiology, Health and Medicine 1996; 1: 235-248.
30. Borges NJ, Osman WR. Personality and medical speciality choice: technique orientation versus people orientation. Journal of Vocational Behaviour 2001; 58: 22-35.
31. Borges NJ, Savickas ML. Personality and medical speciality choice: a literature review and integration. Journal of Career Assessment 2002; 10: 362-380.
32. Lievens F, Coetsier P, De Fruyt F, De Maeseneer J. Medical students' personality characteristics and academic performance: a five factor model perspective. Medical Education 2002; 36: 1050-1058.
33. Vaidya NA, Sierles FS, Raida MD, Fakhoury FJ, Przybeck TR, Cloninger CR. Relationship between specialty choice and medical student temperament and character assessed with Cloninger inventory. Teaching and Learning in Medicine 2004; 16: 150-156.
34. Stillwell NA, Wallick MM, Thal SE, Burleson JA. Myers-Briggs Type and medical specialty choice: a new look at an old question. Teaching and Learning in Medicine 2006; 12: 14-20.
35. Taber BJ, Hartung PJ, Borges NJ. Personality and values as predictors of medical specialty choice. Journal of Vocational Behaviour 2011; 78: 202-209.
36. Hartung PJ, Borges NJ, Jones BJ. Using person matching to predict career specialty choice. Journal of Vocational Behaviour 2005; 67: 102-117.
37. Eley D, Young L, Przybeck TR. Exploring the temperament and character traits of rural and urban doctors. Journal of Rural Health 2009a; 25: 43-49.
38. Eley D, Young L, Przybeck TR. Exploring temperament and character traits in medical students; a new approach to increase the rural workforce. Medical Teacher 2009b; 31: e79-84.
39. Jones MP, Humphreys JS, Nicholson T. Is personality the missing link in understanding recruitment and retention of rural general practitioners? Australian Journal of Rural Health 2012; 20: 74-79.
40. Eley D, Eley R, Young L, Rogers-Clark C. Exploring temperament and character traits in nurses and nursing students in a large regional area of Australia. Journal of Clinical Nursing 2011; 20: 563-570.
41. Eley DS, Eley RM. Personality traits of Australian nurses and doctors: challenging stereotypes? International Journal of Nursing Practice 2011; 17: 380-387.
42. Campbell N, Eley D, McAllister L. What can personality tell us about working in the bush: the temperament and character traits of remote Australian allied health professionals? Australian Journal of Rural Health 2013; 21(5): 240-248.
43. McAllister M. McKinnon J. The importance of teaching and learning resilience in the health disciplines: a critical review of the literature. Nurse Education Today 2009; 29(4): 371-379.
44. Howe A, Smajdor A, Stöckl A. Towards an understanding of resilience and its relevance to medical training. Medical Education 2012; 46(4): 349-356.
45. Cloninger CR, Svrakic DM, Przybeck TR. A psychobiological model of temperament and character. Archives of General Psychiatry 1993; 50(12): 975-990.
46. Wagnild G. The resilience scale user's guide. Worden, MT: The Resilience Centre, 2009.
47. Cloninger CR. Feeling good: the science of well-being. New York: Oxford University Press, 2004.
48. Josefsson K, Cloninger CR, Hintsanen M, Jokela M, Pulkki-Raback L, Keltkangas-Jarvinen L. Parental care-giving and home environment predicting offspring's temperament and character traits after 18 years. Psychiatry Research 2013; 209(3): 643-651.
49. McCrae RR, John OP. An introduction to the five factor model and its applications. Journal of Personality 1992; 60: 175-215.
50. Picardi A, Caroppo E, Toni A, Bitetti D. Stability of attachment-related anxiety and avoidance and their relationships with the five-factor model and the psychobiological model of personality. Psychology and Psychotherapy 2005; 78: 327-345.
51. Grucza RA, Goldberg LR. The comparative validity of 11 modern personality inventories: predictions of behavioural acts, informant reports, and clinical indicators. Journal of Personality Assessment 2007; 89: 167-187.
52. Wagnild GM, Collins JA. Assessing resilience. Journal of Psychosocial Nursing and Mental Health Services 2009; 47(12): 28-33.
53. Cloninger CR, Przybeck TR, Svrakic DM, Wetzel RD. The temperament and character inventory: a guide to its development and use. 1994. St Louis, MS: Center for Psychobiology of Personality, 1994.
54. Eley DS, Young L, Shrapnel M. Rural temperament and character: a new perspective on retention of rural doctors. Australian Journal of Rural Health 2008; 16: 12-20.
55. Eley DS, Cloninger CR, Walters L, Laurence C, Synnott R, Wilkinson D. The relationship between resilience and personality traits in doctors: implications for enhancing well being. PeerJ 2013; 1: e216.
56. Elliot T, Bromley T, Chur-Hansen A, Laurence C. Expectations and experiences associated with rural GP placements. Rural and Remote Health 9: 1264. (Online) 2009. Available: www.rrh.org.au (Accessed 19 December 2014).
57. Cloninger CR, Zohar AH. Personality and the perception of health and happiness. Journal of Affective Disorders 2011; 128(1-2): 131-134.
58. Cloninger CR. What makes people healthy, happy and fulfilled in the fact of current world challenges? Mens Sana Monographs 2013; 11: 16-24.




