full article:
The public health nutrition workforce internationally is ill prepared and unsupported to tackle seemingly insurmountable nutrition issues1-4. In Australia the public health nutrition workforce working specifically with remote Indigenous community stores to improve the food supply are challenged by their work role5. Little is known about appropriate workforce development strategies for this workforce. Of what evidence exists to build the capacity of this workforce, support from peers and mentors appears to be a key element2,6,7. A community of practice, or group of people who share a common concern, a set of problems, or interest in a topic, and who come together to fulfil both individual and group goals8, may be an effective workforce development strategy.
Indigenous Australians who live in remote areas experience a disproportionate burden of preventable illness9. Many residents of remote communities have only one store from which to access food, which in most instances is supplemented by little else. The effect of weather, for example the wet season, makes their food supply more vulnerable. The way remote community stores operate and the quality of food they provide are considered critical to the effort to improve the health of Indigenous people living remotely10.
The public health nutrition workforce, employed by remote retail organisations and government and non-government organisations, is expected to support socio-environmental change through the implementation of evidence-based practice to improve the food supply and therefore intake of nutritious food. Work may include improving nutritional quality of the take-away food5, supporting the development of nutrition policies and providing evidence-based information to store management committees and store managers to inform practice. Additional skills are needed to understand work in the retail sector5. Inadequate individual and systemic capacity1,3 bring many challenges in this role, which must be addressed as part of a multitude of strategies to improve the health and nutritional intake of remote Indigenous communities.
It is common for many of these positions to be filled by novice nutritionists (graduated less than 5 years ago)11, who are likely to have the greatest need for professional support and little capacity to implement socio-environmental change2. Support from peers facing similar challenges and collective experience has been shown to be effective in building workforce capacity12. A community of practice, where the focus is on best practice, sharing resources and creating new knowledge to advance a 'domain' or topic of professional practice, may be effective. Communities of practice develop outcomes through three considered elements: work, co-learning and relationships13.
The aim of the study was to evaluate a community of practice designed for public health nutritionists who work with stores in remote Indigenous communities across Australia. Specifically the evaluation aimed to determine the influence of the community of practice on the work of participants and evaluate the elements of the community of practice that influenced its perceived impact.
A qualitative evaluation was employed for this study.
Sampling
All public health nutritionists working for remote store organisations or those employed by government or non-government organisations throughout Australia were the target for the intervention. Although the total size of this workforce across Australia is unknown, in one state/territory at the time of the study there were 19 nutritionists (13 government, 4 non-government and 2 retail store nutritionists) (Annie Villeseche, pers. comm., 8 September 2014). Nationally, this workforce is mostly based in major regional towns and travel up to 500 km by road or non-surfaced road or 1000 km by air to their work in remote communities.
A flyer was distributed via email networks, inviting nutritionists to participate in the community of practice intervention. Participants self-selected to participate and snowball sampling was also used for recruitment, whereby interested participants were asked to identify any other potential participants from their networks14. From the invitation, interested participants contacted the researchers, who explained what involvement in the study would entail, and eligibility was then determined. Selection criteria included current working with remote community stores and a demonstrated need for additional workplace support, by explanation or providing evidence of isolation in a workplace organisational structure.
A total of 24 nutritionists expressed interest. Twelve potential participants were excluded. Of these, six were not given permission from their organisation to participate. Three did not have a role in working with stores and therefore did not meet the inclusion criteria, and three were interested in finding out the success of the community of practice after it was completed rather than being involved. Twelve eligible participants consented to be part of the community of practice and the study. Participant demographics (age, years of experience, qualifications, professional membership) and position descriptions were collected.
The community of practice workforce development intervention
The participants met initially face-to-face in a one-and-a-half day workshop in May 2012 to meet peers and develop a common understanding of how the community of practice would function. Discussions included logistics and group guidelines, including the purpose, so that all participants agreed how to contribute effectively. Selected presentations on planning, implementing and evaluating public health nutrition practice and evidence-based strategies that have been shown to improve remote food supply were delivered. Dedicated time was allocated to identify what the participants hoped to achieve by partaking. Following the workshop, the community of practice met every 6 weeks over 7 months (until December 2012). Sessions ran for approximately 2 hours each and both teleconference and videoconference were used. During these sessions, participants were encouraged to reflect on their work, identify key learning from their practice and raise issues that they wanted support to address. Where time allowed, stories were shared and peers could contribute ideas or examples from their experience of how they had tackled similar situations in their work. A lead facilitator (CEP) used reflective practice target questions to facilitate the participants to think deeply and critically about their work, ensuring participants were not simply reporting on what they were doing at work but exploring the situation and what they had learnt from the experience15. Participants had exclusive access to an online database that included relevant evidence-based resources for the field. Sharing was encouraged through this database, and by email or phone.
Evaluation methods
The 'most significant change' technique16 together with in-depth interviews14 were used for this study to identify the major influence of the community of practice on the work practice of participants and explore their experience of being involved in the group. Triangulation of the two methods of data collection enhanced rigor14,15.
The 'most significant change' technique is used for evaluating complex interventions16. It involves the generation of significant change stories developed by the various participants and a process of prioritising the identified themes through focus group discussion16. The 'most significant change' technique was used to determine the major influence of the community of practice on the work of participants. At the completion of the 7-month community of practice, the participants were invited by the facilitators in an email to share the changes that they had experienced through involvement in the intervention. They were asked, 'Looking back over the last months, what do you think was the most significant change in your work in remote food supply that resulted from involvement in this community of practice, and why was this story significant for you?' Three participants wrote short stories which were de-identified and used for discussion by facilitators in the final group community of practice. The final discussion allowed open discussion, further story sharing by all participants about the most significant change to their practice as a result of participating in the community of practice and prioritisation of most significant change. The discussion lasted for 60 minutes and was recorded and later transcribed.
In-depth interviews were conducted with each participant to further explore participant experiences and impact on work practice. The interviews were designed to complement data collected through the 'most significant change' technique and to further explore participant experience (Table 1). An independent research assistant with knowledge and experience in remote store work and qualitative research skills was employed to conduct the interviews during January and February 2013. This independent interviewer provided participants with the opportunity to be open about their experience. The interviews were recorded and the audio files later transcribed.
Data analysis
Qualitative data were analysed using QSR NVivo v10 (QSR International; http://www.qsrinternational.com). Data from the 'most significant change' technique underwent thematic analysis14 whereby transcribed text was coded without any pre-existing codes or frameworks, codes were categorised and themes developed from categories. In-depth interview data underwent content analysis14 with an existing coding framework due to the plethora of literature already existing on communities of practice, their function and impact, but also allowing for new codes to emerge. The coding framework focused on the function and outcomes of communities of practice and included the following codes: avoids isolation; promotes innovation; increases speed; value creation; tools for alliance; problem solving; knowledge and learning creation; organisational infrastructure; and limitations17.
Initially, the datasets were analysed independently by one author (SH) with another author (CEP) then analysing the most significant change data and a subset of two in-depth interviews to verify categories and themes. The position of SH, who had previously worked as a remote store nutritionist, was managed by using reflexivity techniques and data analysis triangulation14. Data from both methods were then analysed together by comparing themes and categories, and overall themes were then generated through discussion. Narrative quotes were selected to illustrate stories. The themes and descriptors were shared with the participants for further verification.
Table 1: Participant in-depth interview guide and logic

Ethics approval
This study was conducted according to the guidelines laid down in the Declaration of Helsinki, and all procedures involving human participants were approved. Ethics approval was granted by Monash University Human Research Ethics Committee (CF12/0561-2012000230) and Northern Territory Department of Health and Menzies School of Health Research Ethics Committee (12/1747). Written informed consent was obtained from all participants.
Twelve nutritionists were selected to take part in the community of practice and consented to be part of the study. The sample was drawn from across Australia and across a range of organisations of employment and levels of professional experience (Table 2). Eleven of the twelve participants completed the 7-month community of practice. There were on average eight participants in attendance at each session. One participant withdrew after the second session but participated in the in-depth interview. Nine participants were involved in the 'most significant change' discussion. One participant who completed the intervention and contributed to the 'most significant change' discussion passed away before in-depth interview data was collected. The results suggest that the community of practice was perceived to be effective in influencing the practice of participants due to a range of factors, expressed as subthemes (Fig1).
Table 2: Demographics of community of practice participants
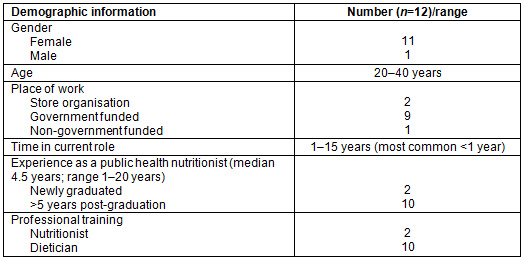
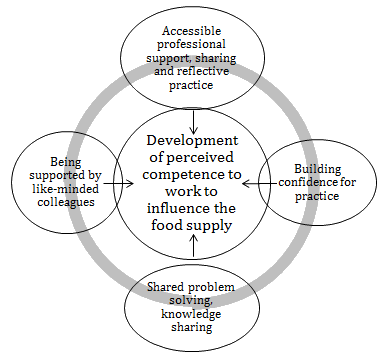
Figure 1: Themes and subthemes identified from 'most significant change' discussion and in-depth interviews.
Development of perceived competence
The majority of participants could not report measurable store change as a result of partaking but felt more effective in their role to change the socio-ecological environment. Participants believed that they were equipped to ask the right questions of the right people with power and influence to make change. They explained that this was a difference in their thinking that could not be found by reading the literature alone. All participants also expressed that food supply change takes time and felt their achievements were relative to this timeframe. Some described their learning in relation to the importance of taking time to scope the capacity of the communities they worked with and for the first time feeling comfortable about not acting immediately, which they felt was an important lesson for working in Indigenous health.
Community engagement and development approaches were reported to be used with greater confidence and ability. The application of specific evidence-based tools and frameworks that were shared in the community of practice was reported to change participants' practice. Participants reported thinking more about evaluation to measure their work. Their role in advocacy at a community level, in raising awareness about the food supply and being a conduit between the store and the community, was said to develop. At an organisational level they were able to advocate spending time in prevention.
I think, without being ... involved in the community of practice, I probably would never have been able to get to where I am now[:] Being able to have a conversation with my colleagues and with my manager about refocusing and restructuring our program to bring about change. (participant 5, 'most significant change' discussion)
The community of practice assisted practice through the following four key functions:
Shared problem solving, knowledge sharing: The group took inspiration from the impact in the field of their combined work. The motivation and generation of enthusiasm was valued. The community of practice did not always have the answer or evidence and this was accepted by participants whereas without the group they explained this would have felt frustrating.
The ability to access resources, including journal articles, and have timely answers to questions, was reported to be a valuable part of being in the community of practice. Having the benefit of peers who had completed similar work and sharing from their experience increased speed in finding solutions. The participants reported that answers also came through exploring their justification of their own approach through reflection in the sessions.
The participants suggested that being able to take part in the community of practice for a longer length of time may have provided them a greater opportunity to meet their learning needs. Seven participants committed to continue participating in the community of practice with the continued support of the facilitators after the initial 7-month period. Flexibility in the arrangement of sessions was required with remote work even though advance notice of sessions was also essential. They suggested that constant evaluation of the group and the technology used may have overcome these limitations of the intervention.
Building confidence for practice: Participants described gaining new skills, tools and approaches to their work as a result of being part of the community of practice. They highlighted that the community of practice helped reinforce the important focus on socio-environmental change rather than a focus on more individually centred nutrition education, which is often expected of their roles. They reported valuing gaining skills in advocacy, which assisted development of competence and being more effective in their work. One participant described having advocated to her work managers for continued work in stores over expanding direct patient care work in regional town settings; others spoke about using the evidence shared in the community of practice to shape their work in remote communities, for example price subsidies and take-away food initiatives.
Most participants described learning about ways to engage with retailers and to work strategically to ensure their nutrition approach also considered business objectives. They shared their learning about the importance of store initiatives leading to mutual benefit, of both the communities' health and the stores' business, and this built their confidence for approaching work in stores.
Accessible professional support through sharing and reflective practice: The ability to share within safe grounds allowed debriefing and camaraderie amongst the group. Critical reflection ensured people were not simply sharing what they were doing but how and why. The collective development, commitment, focus and expertise were the points of difference to other professional development opportunities. Participants enjoyed the formality and structure of each session and believed it helped in knowing what to expect every time. Taking time to undertake reflection in the session was said to build skills in reflecting regularly in their work outside of the sessions and build confidence in the process.
Just attending the meetings made me think more about my work, and then I'd reflect even more after the meetings about what we'd discussed. (participant 7, interview)
The majority of participants described themselves as novices in their work and reported often feeling out of their depth and requiring guidance. Participants described feeling isolated and undervalued in their work roles. This was due to working alone on nutrition within the communities in which they worked. They explained that the community of practice reduced this feeling through knowing they were not alone in the work they did and being supported regularly. The six-weekly 'checking in' was said to ease the sense of isolation. They explained that it was worthwhile having the mix of people from across Australia to understand that the challenges faced were similar regardless of geographical or role issues. The range of states represented was said to help participants think more broadly about the different issues and not automatically see them as state- or region-specific.
Just knowing that there was that support was the huge thing for me, and knowing that if I was getting frustrated or felt like things weren't moving, or just wanted to talk out something that I was doing, I knew that I could just call on the group or call on [the facilitators]. (participant 6, interview)
The participants described feeling more valued for the work they do through connecting with others. Some participants identified other mentors and supports that assisted in avoiding isolation in their roles; most were through line managers or internal support, with only two formal mentors mentioned. These types of supports, however, were said to be focused more on the organisation and less on public health nutrition work. The community of practice differed to other supports available because it was reported to increase access to experts in the field who had an understanding of the work.
There was a true sense of support where people looked forward to catching up. Participants reported this helped them mentally within their roles through de-briefing and giving reassurance in a collegial way. Those who utilised the network most identified themselves as always valuing talking to peers and learning through communication.
Support by like-minded colleagues to stay focused: The community of practice allowed time for the participants to reflect, debrief and explore the challenging field they worked in, with peers that understood and were empathetic. It was evident that the type of people who were involved in the community of practice were motivated and passionate about their work and their development for the best outcomes for Indigenous communities. The group facilitated exploration of the challenges in working with remote stores, which they reported kept them motivated to do this work. Working with stores was said to be additionally challenging because they had to navigate their approach with store management, consider the alternative worldview of profit and deal with the frustration that their work took time to produce real outcomes.
I know I get frustrated sometimes with how slow it can be to do this work ... So yes, I think that was one of our discussions one meeting, where others were facing those frustrations as well [and that was reassuring]. (participant 1, interview)
The commonality of positions, people, work experience and age was also acknowledged. The size of the group was reported to be appropriate because there was an ability to get to know all the members, equal time given and a comfortable space for sharing. The majority of members reported sharing on confidential things such as structure and work politics because they felt trust and inspiration by their peers.
... sometimes you felt like you weren't doing a good job and you felt like you weren't being effective and I don't think you can really talk about that in your workplace. It was nice to have a place to go to where they won't - you know, there weren't consequences for being open. (participant 8, interview)
The community of practice facilitator and coordinator were said to be approachable. The facilitator was identified to support equal sharing, deal with conflicting issues within the group and help with career planning. The characteristics identified by members for the facilitator were that they be accessible outside of sessions, provide timely responses, be supportive, a real person, a good listener and provide honest answers in a non-judgemental way.
Two participants with more experience in working with stores felt the professional development focus was basic and did not meet their needs. The nutritionists who were employed by remote store organisations found the community of practice did not promote innovation in their work or objectively change their approach and believed the variance in knowledge and small understanding of business constraints by the group members prevented them from sharing openly in their work and regularly participating. They did not see the benefits from the group nor feel the level of trust required to share with their peers to a level that may then have impacted on their work approach.
Discussion
This study aimed to determine the influence of the community of practice on the work practice of participants and found that for the majority of participants the community of practice intervention was perceived to be an effective strategy to improve work practice. It provided participants with a mechanism for support to manage the complexity and challenges that they may face in their work roles. The elements that contributed to the success included the joint problem solving, knowledge sharing and regular communication with a group of like-minded colleagues. A community of practice may be an effective and efficient workforce development intervention to improve the food supply in remote Indigenous community stores.
Communities of practice have been previously found to assist the public health workforce in evidence-informed decision making18. The findings from the present study support previous evidence that peer support and facilitated reflective practice can improve perceived competence and ability to improve population nutrition2. The present study also supports evidence on essential elements of communities of practice17. The formalised structure together with productive inquiry through critical questioning and hearing success stories were highly valued by participants.
Trust and feeling safe to share with other participants was perceived to be essential for success. Trust is established through a community of practice through frequent interactions19. Trust allowed participants to divulge problems they were facing and showcase vulnerabilities. The majority of participants felt trust to share; however, the nutritionists who were employed by remote store organisations were reluctant to trust and share and explained that this was due to the greater requirement on confidentiality of business knowledge. The participants who felt less trust prioritised organisational restraints over their own personal development. This may have been a true sense of mistrust or may have been misunderstanding about the discussions that were required to be conducted in order to achieve practice development. Their lack of engagement with the community of practice prevented them from understanding how they could gain from the discussion while at the same time keeping business knowledge confidential. Ensuring all participants in a community of practice feel trust to be able to share to enable reflective practice is essential. Additional emphasis or attention may need to be given to the public health workforce, which has greater organisational constraints.
The results suggest that the community of practice impacted the work practice of participants by strengthening the evidence-based approach to their work and building confidence for changing store infrastructure. Developing knowledge through sharing and creation and development of self-efficacy are reported features of communities of practice20. The important role of the facilitators in bringing the people together and supporting reflective practice and knowledge exchange was part of its success. As has been found in reviews of the evidence of communities of practice20,21, their sustainability as a strategy themselves and of the practice of their participants is unknown. The commitment by the majority of this study's participants to continue with the arrangement provides some evidence of sustainability but also indicates the need for ongoing leadership and facilitation, an attribute of communities of practice that is increasingly being reported in the literature as an important element22.
This intervention provides evidence of a simple strategy to improve the approach of nutritionists to affect the food supply and potentially the impact on the health of remote Indigenous communities. The resources required for administration and participation may be viewed as small compared to other professional development strategies. There is a need to promote the potential impact of communities of practice as a workforce development strategy to managers to increase the support for practitioners to be involved in such endeavours. The practice improvement of the six participants whose organisations did not give them permission to attend is not known and limits the transferability of the findings.
This qualitative research was enhanced through a range of methods. Triangulation of methods was achieved through cross-analysis and comparison of the most significant change and interview data. Although only three written 'most significant change' stories were collected, all participants contributed to the final 'most significant change' outcome. Reflexivity methods including independent researcher conducting interviews, application of existing literature to inform research approaches and analysis also provided rigor. These findings are likely to be transferable to nutritionists working with Australian Indigenous communities but the concept needs to be tested for other practice settings.
Limitations include the inability of the evaluation design to measure actual change to practice due to the limited length of time for which participants were followed. This has been reported as a limitation of other community of practice studies21. Future research is needed to measure the effect of workforce development strategies on the health and nutrition of the communities the workforce supports. Using the 'most significant change' technique16 with other evaluation methods that take into consideration sustainability, and supporting participants to measure the impact of their work on the ground on the nutritional health of Indigenous communities may be a way forward.
This study provides evidence of a community of practice intervention that was evaluated to show improved perceived work practice of nutritionists working in rural and remote Australia. The essential features of this successful community of practice - including reflective practice, peer learning, trust, knowledge sharing and creation and effective organisation - are synonymous with the literature. Extra attention in the establishment of trust to meet the needs of nutritionists who have challenging organisation constraints may be required. Communities of practice can offer an effective workforce development strategy for rural and remote practitioners and should be considered by employers and workforce planners as a way of developing the public health nutrition workforce to more effectively manage population nutrition and health issues into the future.
References
1. Hughes R. Competency development needs of the Australian public health nutrition workforce. Public Health Nutrition 2003; 6(8): 839-847.
2. Palermo C, Hughes R, McCall L. A qualitative evaluation of an Australian public health nutrition workforce development intervention involving mentoring circles. Public Health Nutrition 2011; 14(8): 1458-1465.
3. Steyn N, Mbhenyane X. Workforce development in South Africa with a focus on public health nutrition. Public Health Nutrition 2008; 11(8): 792-800.
4. Shuftan C, Jonsonn U. Competence: for what, and so what? [correspondence]. World Nutrition 2012; 3(3): 4.
5. Gregoriou A, Leonard D. RIST evaluation of the remote Indigenous stores and takeaways resources in Queensland and the Anangu Pitjantjatjara Yankunytjatjara lands of South Australia. Brisbane: Queensland Health, 2010.
6. Hughes R. Competency development in public health nutrition: reflections of advanced level practitioners in Australia. Nutrition and Dietetics 2003; 60(3): 205-211.
7. Palermo C, McCall L. The role of mentoring in public health nutrition workforce development. Perspectives of advanced-level practioners. Public Health Nutrition 2008; 11(8): 801-806.
8. Wenger E. Communities of practice: learning, meaning, and identity. New York: Cambridge University Press, 1998.
9. Vos T, Barker B, Begg S, Stanley L, Lopez A et al. Burden of disease and injury in Aboriginal and Torres Strait Islander peoples: the Indigenous health gap. International Journal of Epidemiology 2009; 38(2): 470-477.
10. House of Representatives Aboriginal and Torres Strait Islander Affairs Committee. Everybody's business: remote Aboriginal and Torres Strait community stores. Canberra: Commonwealth of Australia, 2009.
11. Colles S, Belton S, Brimblecombe J. Insights into nutritionists' practices and experiences in remote Australian Aboriginal communities. Australian and New Zealand Journal of Public Health 2015, 22 April; doi: 10.1111/1753-6405.12351 (epub ahead of print).
12. Palermo C, Hughes R, McCall L. An evaluation of a public health nutrition workforce development intervention for the nutrition and dietetics workforce. Journal of Human Nutrition and Dietetics 2010; 23(3): 244-253.
13. Wenger E, McDermott R, Snyder W. Cultivating communities of practice: a guide to managing knowledge. Boston: Harvard Business School Press, 2002.
14. Liamputtong P. Qualitative research methods, 3rd ed. South Melbourne: Oxford University Press, 2009.
15. Mann K, Gordon J, MacLeod A. Reflection and reflective practice in health professions education: a systematic review. Advances in Health Sciences Education 14(4): 595-621.
16. Davis R, Dart J. The 'most significant change' (MSC) technique. London: CARE International, 2005.
17. Saint-Onge H, Wallace D. Leveraging communities of practice for strategic advantage. Burlington, MA: Elsevier, 2003.
18. Meagher-Stewart D, Solberg S, Warner G, MacDonald JA, McPherson C, Seaman P et al. Understanding the role of communities of practice in evidence-informed decision making in public health. Qualitative Health Research 2012; 22(6): 723-739.
19. Ranmuthugala G, Cunningham F, Plumb J, Long J, Georgiou A, Westbrook J, et al. A realist evaluation of the role of communities of practice in changing healthcare practice. Implementation Science 2011; 6: 49.
20. Li L, Grimshaw JM, Nielsen C, Judd M, Coyte PC, Graham ID. Use of communities of practice in business and health care sectors: a systematic review. Implementation Science 2009; 4: 27.
21. Ranmuthugala G, Plumb J, Cunningham F, Georgiou A, Westbrook J, Braithwaite J, et al. How and why are communities of practice established in the healthcare sector? A systematic review of the literature. BMC Health Services Research 2011; 11: 273.
22. Jennings Mabery M, Gibbs-Scharf L, Bara D. Communities of practice foster collaboration across public health. Journal of Knowledge Management 2013; 17(2): 226-236.


