full article:
Health workforce planning is an important response to the growing challenges of providing consistent high-quality health services at acceptable costs to society1. Shortages of well-trained allied health and medical professionals in underserved areas negatively impact on population health outcomes in those areas. Maintaining an adequate medical workforce in rural and remote Australia has been specifically challenging for many years2. Educational strategies used by the Australian Government to address this issue include encouraging the admission of rural background students and supporting the growth of academic health faculties and Rural Clinical Schools (RCSs)3. To receive RCS support, a medical school must ensure 25% of their students spend a minimum of 12 months in a rural location where they are provided with positive, high-quality clinical education and training experiences as well as the opportunity to gain a real understanding of, and enthusiasm for, rural life.
However, as regional and rural health professional student numbers increase, it is imperative to assess the effectiveness of these educational innovations so strategies can be evaluated, refined and disseminated. This is only achievable if regional academic health faculties and clinical schools can successfully locate and follow up their students after graduation.
The geographical distribution of health professionals is of particular relevance in Australia due to the shortage of medical practitioners in regional and rural areas4. Short- and long-term tracking of the destination of health professional graduates from regional health faculties and clinical schools is necessary to highlight the proportion of graduates from each cohort that choose to remain in rural areas or relocate to metropolitan centres. In addition, information on whether these new graduates work in the private or public sectors, what specialty training or further education they have undertaken, whether they become involved in research or teaching activities, or whether they leave the profession altogether is invaluable for aiding workforce planning.
However, contact details and professional information quickly become obsolete in university databases, particularly for health professions in which postgraduate training requires mobility across states. Hence, it is necessary to develop effective mechanisms to maintain an accurate record of 'contactable' alumni.
The James Cook University (JCU) College of Medicine and Dentistry has been established in north Queensland since 2000 with a mission to address local workforce needs by recruiting northern and rural background students and a curriculum that covers rural, remote, Indigenous and tropical health themes. There has always been strong interest in seeing what JCU medical graduates choose to do with respect to practice location and career choice, so, in 2005, the College began developing processes to enable the longitudinal tracking of its graduates. Longitudinal tracking will evaluate the main outcome of interest - the communities JCU medical graduates serve and their career choice.
This paper describes the experiences of the JCU medical school over the last decade in developing processes and a database to longitudinally track and monitor graduates' training choices and practice location, and ensuring access to follow-up studies for workforce planning.
Approach
The overall graduate tracking approach begins with administering an exit survey to each cohort immediately prior to graduation, which collects their contact details and consent for follow-up contact. Practice location data are recorded yearly in a database via personal contact, plus a JCU medical school FacebookTM page to search for hard-to-trace graduates and by accessing the Australian Health Practitioner Regulation Authority (AHPRA) website (www.ahpra.gov.au). Postgraduate data are coded numerically and entered into the software package used to support the longitudinal tracking database Statistical Package for Social Sciences (SPSS) for Windows v20 (SPSS Inc; www.spps.com).
Exit survey design
The annual, in-house exit survey is administered to each medical cohort immediately prior to graduation, either face-to-face or online. Students provide informed consent to participate. As well as several questions about course quality improvement, this survey collects information on preferred geographical location of future medical practice, location of internship (state or territory, city or town, name of the institution), preferred medical career specialty (and whether they had changed this intention during the course), intention to work in a rural area upon course commencement (and if they had changed this intention), and interest in involvement in medical teaching and medical research.
Graduate tracking processes
On the final page of the exit survey, students were asked to provide their name and contact details (mobile phone number and email address) for tracking. However, this information has not always been completed accurately by the graduating students, so, in 2008, the JCU medical school also created a Facebook page to assist with maintaining contact with graduates and to better connect with medical students. While the JCU medical school adopted Facebook rather late as a communication and engagement strategy, it is not uncommon for higher education institutions to be slow in embracing new technologies5. Facebook and other social network communities provide a less formal method of interacting with people5, which has so far been true for the JCU medical school's Facebook page. JCU students and graduates are under no obligation to 'friend' or 'like' the Facebook page, but most do so and many engage in discussion with the page creator or share items of their own.
The JCU medical school Facebook page was set up as an 'individual' rather than a 'group', 'business' or 'organisation' account, enabling it to have the same abilities of individual Facebook accounts: to add or delete friends; to send private messages to one or multiple accounts including the option to create friend 'groups'; and to 'like' or comment on friends' pages. When a friend request was received for the page, the account moderator checked the name against JCU records to verify if the person was a medical graduate. Occasionally, friend requests were received from prospective students. These requests were declined, with the moderator citing that the purpose of the group was to keep in contact with JCU medical graduates. As the page evolved, students in Year 6 of the medical program were invited to 'friend' the page in an effort to pre-empt their departure from the social groups they were linked to while at the university and maintain contact through the transition from student to intern.
Searching for hard-to-trace graduates on the JCU medical school's Facebook site has been found to be more efficient and effective than using traditional methods such as phone books, calling an intern's last known place of employment, or sending an email to a potentially abandoned or infrequently used email address, as it is likely that nearly all university students now have a Facebook account. The Facebook page has also proved useful for disseminating school newsletters, posting useful or interesting articles, and promoting upcoming events for students, interns and junior doctors. The Facebook page has been accessed extensively over the last six years and currently (2014) has a 'friend list' of 378 graduates from the first nine cohorts (Table 1) and 663 current undergraduate students (total 1041 'friends').
Contact is thus made with graduates by email, telephone or the Facebook page every 2-3 years. The last major attempt in gaining individual contact with graduates was in 2012, where use of email, telephone and Facebook provided self-reported postgraduate training data and yearly practice location for 456 of 536 (85%) of all graduates from 2005 to 2011. For those graduates for whom the JCU medical school does not have contact details, and during the years when personal contact is not undertaken, data on practice location are sourced annually from the AHPRA website. Using AHPRA, along with personal contact strategies, has allowed practice locations to be identified each year for 98% of graduates.
The validity of using the AHPRA site for obtaining practice location data has also been checked internally using a comparison of 20 practice locations obtained via direct personal contact, which showed agreement in 18 out of 20 (90%) cases; this is a similar percentage to a more in-depth study reported by Playford and colleagues comparing the accuracy of AHPRA with personal contact6.
Table 1: Number of graduates from the first nine cohorts who have completed the exit survey and/or are FacebookTM friends with the James Cook University College of Medicine and Dentistry
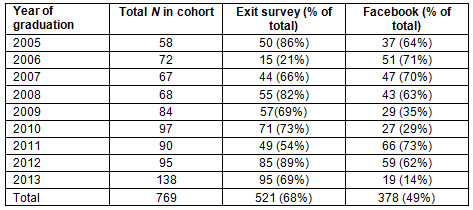
Longitudinal tracking database
Postgraduate data are linked to the graduates' admission and undergraduate data retrieved from administrative databases held by the university and the medical school. Admission data include student identification number, hometown at application to medical school, date of birth, gender, ethnicity, interview score, and Tertiary Entrance Score (an Australian rank - ordered, school-leaving score). Undergraduate data included if awarded Honours; rural placement location in Years 2, 4 and 6; if awarded a rurally orientated scholarship; if granted advanced standing (entered course in Year 2 or later); if entered on a Bonded Medical Place; and Clinical School location in Years 5 and 6 of the course (Townsville, Cairns, Darwin or Mackay).
The database is set up alphabetically for each commencing student. Additional variables are created to record whether or not the student drops out and what year they graduate. Postgraduate practice location (eg Townsville, Brisbane) is entered each year as the graduate progresses from postgraduate Year 1 to beyond. The graduate's admission into and/or completion of any specialty training programs is determined from personal contact every 2-3 years. A list of tips for using the database for analysis and some practical applications are also provided in Figure 1.
While it is intended that the tracking database will be maintained for the foreseeable future to allow regular follow-up of graduates well into their established careers, graduate numbers are increasing at the JCU medical school, going from 58 in 2005 to over 160 in 2014, and it is intended that from 2015 onwards, personal contact will be made with graduates on a less frequent basis. While patterns of practice will continue to be monitored for each cohort using the AHPRA website, monitoring via personal contact will only be undertaken on a periodic basis rather than bi-annually, which is likely to be every fifth year; that is, postgraduate year 5, postgraduate year 10 etc. Thus, in the future, the graduate tracking approach will be a series of cohort studies, with cohorts identified by year of graduation.

Figure 1: Practical pointers for running a longitudinal tracking database.
Ethics approval
Ethical approval for the study was obtained from the JCU Human Research Ethics Committee (No. H1804).
Using the AHPRA website along with the personal contact strategies has allowed practice locations to be identified each year for 98% of all JCU medical graduates. The longitudinal tracking database has provided a comprehensive and complete picture of the location of practice of JCU medical graduates from 2006 to 2014, with the tracking system combined with the AHPRA website enabling exploration of the patterns of practice to be conducted with considerable confidence. This successful graduate tracking system may be of value to other health institutions in Australia or around the world. In addition, successful mapping of graduates' geographical location of employment and subsequent career pathways will determine whether current and past government funding and financial support for regional medical programs like regional medical schools and RCSs successfully increase the medical workforce in underserved areas of Australia.
Acknowledgements
The authors gratefully acknowledge the co-operation of all JCU medical graduates who consented to be contacted for the school's longitudinal tracking project.
References
1. Kaur B, Carberry A, Hogan N, Roberton D, Beilby J. The medical schools outcomes database project: Australian medical student characteristics. BMC Medical Education, 2014; 14: 180.
2. Ricketts TC. The changing nature of rural health care. Annual Reviews of Public Health 2000; 21: 639-657.
3. Australian Government Department of Health and Ageing. Rural Clinical Training and Support (RCTS) 2011-2014. Canberra, ACT: Department of Health and Ageing. (Online) 2014. Available: www.health.gov.au/clinicalschools (Accessed 17 June 2015).
4. Ricketts TC. The changing nature of rural health care. Annual Reviews of Public Health 2000; 21: 639-657.
5. Fagerstrom A, Ghinea G. Co-creation of value in higher education: using social network marketing in the recruitment of students. Journal of Higher Education Policy and Management 2013; 35(1): 45-53.
6. Playford D, Power P, Boothroyd A, Manickavasagar U, Ng WQ, Riley G. Is the National Registration website (Australian Health Practitioner Regulation Agency) effective in tracking Australian medical graduates' rural work? Australian Journal of Rural Health 2013; 21(5): 249-253.




