The prevalence of patients with dementia or other cognitive impairment in Australian hospitals is increasing as a direct consequence of the ageing population1, and this is set to continue2. In the rural Australian coastal location of this study, retirement migration has led to an exponentially increased ageing demographic, with dementia prevalence greater than the average for the Australian state of New South Wales (NSW)2,3. This has implications for current and future health service demand and models of care4.
The impact of the hospital environment on a person with dementia can be profound. Reasons include removal from familiar surroundings, the impact of the busy and noisy environment, staff who are often rushed, the effect of the medical and surgical conditions for which they are admitted to hospital, and an acute medical model that has minimal resources for the individualised care needed by these patients5. The resulting psychological effects on the person with dementia can be fear, anxiety, increased confusion and onset or increase in the behavioural and psychological symptoms of dementia (BPSD)6-8.
The emotional experience for people with delirium can be equally profound. Delirium is an acute onset of confusion which in most cases is attributable to a medical cause. It is common in hospitals, with prevalence rates of 20-52% depending on ward setting and patient demographics9. Delirium occurs more commonly in people with pre-existing dementia10. People with a hyperactive form of delirium can experience delusions and hallucinations leading them to feel fearful of or threatened by those caring for them. They may resist care, become agitated and combative, or try to climb out of bed and abscond. People with hypoactive delirium, who are sleepy and lethargic, may forget to drink, be unable to feed themselves, and can easily become dehydrated or malnourished11.
The consequences for these patients with delirium is greater risk for falls, functional decline, increased length of stay, challenging behaviours, increased use of antipsychotic medication, premature nursing home placement and death12,13. The care and safety of individuals who are cognitively impaired due to dementia, delirium or delirium overlaid on dementia is therefore a major clinical governance challenge for hospital care14. For nursing staff, stress and care burden is increased in care of patients with cognitive impairment, particularly those with agitated, aggressive or wandering behaviours15,16. Studies looking at staff experience when providing health care to this population cite competing demands, lack of time, and the inapplicability of the medical model of care to meet the complex and idiosyncratic needs of patients, resulting in poor job satisfaction as well as increased stress15-17.
The emotional care and security of patients with cognitive impairment using person-centred care advocated by Kitwood18 has consistently been recognised as best practice5,19,20. There have been recommendations for more research supporting care of patients with dementia in hospitals based on this need5, but available studies provide limited evidence about sustainable ways in which this can be achieved21. Caring for these patients clearly takes time, and time is a commodity that many nurses lack.
Accordingly, the use of trained 'sitters' has been recommended as an important adjunct to care for people with dementia and/or delirium in acute hospitals, particularly where family members are not available14,22,23. Evidence on the effectiveness of the use of volunteers for patients with dementia, however, is limited22. Volunteers have been used in a structured multicomponent delirium prevention program developed by Sharon Inouye and colleagues24, called the Healthy Elder Life Program (HELP). HELP has repeatedly demonstrated reductions in incidence of delirium25-27. Even so, the copyright cost of the program and the dedicated interdisciplinary staff resources required for implementation limit transferability, especially in poorly resourced rural settings.
The present study therefore aimed to address this well-established clinical need. The study comprised training a group of volunteers in person-centred care to enhance the emotional care, safety and wellbeing of individuals with dementia and/or delirium in hospital; establish acceptability and feasibility of the program; and examine the effects on patients, staff and volunteers.
A quasi-experimental pre-post design was employed between May and December 2009, in a 63-bed rural acute hospital located on the far south coast of NSW. This location has an ageing population, and dementia prevalence is greater than the NSW average.
Recruitment
Patients: The primary researcher (CB) identified potential patients by reviewing new admissions on the ward list in consultation with a senior staff throughout the project. Eligibility criteria included presence of cognitive impairment (dementia or delirium) and known risk factors for delirium (Table 1). Patients were prioritised for volunteer support based on the clinical judgement of the researcher. For example, a patient with dementia who was wandering, or an agitated or a drowsy delirious patient, were identified as a first priority; patients with delirium risk factors who were relatively independent were a lower priority.
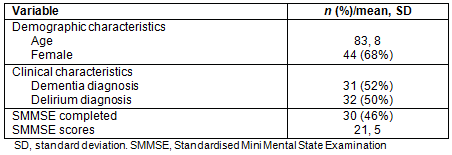
Written consent was sought from 83 potential patients and/or people responsible for them. In gaining consent, the patient/carer consented to being assigned a volunteer, to their medical record being accessed by the researcher to obtain information about their care and treatment, and to publication of this data provided that identifying information was removed. The final sample was 64 because of a lack of consent (n=15), length of stay <48 hours (n=2) or not meeting other criteria (n=2). Whether or not they entered the sample, all patients who needed volunteer support received it. Table 2 presents the patients' characteristics.
Table 1: Criteria for patient inclusion in the study

Table 2: Patient characteristics (n=64)
Nursing staff: All rostered registered nurses, enrolled nurses and nurse unit managers at the hospital (n=50) were invited to provide data. Envelopes containing an information sheet, consent form and the pre-program questionnaire were distributed. Those who returned questionnaires did so in sealed envelopes, which were then forwarded for independent coding and de-identification - they were not seen by the researcher. The same confidentiality process occurred for post-program questionnaires.
Volunteers: Media releases, promotion through existing volunteer groups and word of mouth were used to recruit volunteers. An information pack included details about the study and a volunteer duty statement. Twelve were recruited in April 2009 and a further six subsequently. Volunteers were community members from a range of backgrounds, including past carers, retired nurses, a first-year nursing student, a physiotherapist and other community members who wanted to contribute to and become involved with a hospital volunteer program. All were female. Pre-education questionnaires and consent forms were distributed on the first day of the volunteer training program. The first group of volunteers commenced the intervention phase in early May 2009. Post-program questionnaires were distributed to all volunteers at the end of November 2009. The confidentiality procedure was the same as for nursing staff.
Measures: Patients Those patients able to do so completed the Standardized Mini-Mental State Examination (SMMSE)28. These were either performed by the researcher, another clinical nurse consultant or by other ward staff who had been trained in using the SMMSE. The hospital was already using the SMMSE for cognition screening in the clinical setting, with procedures for the conduct and scoring of the SMMSE in place. Demographic and clinical data collected from medical records included age, sex, diagnosis of dementia or delirium, SMMSE score where completed, length of stay, incidence and number of falls per patient, number of times antipsychotics or other psychotropic medications were administered, and use of analgesics.
Staff and volunteers Staff reported on previous experience with aged or dementia/delirium care; volunteers reported on previous experience caring for someone with dementia. Both staff and volunteers completed some standard measures at baseline and follow-up. The Approaches to Dementia questionnaire29 assesses attitude to people with dementia on a Likert scale and yields two factors: eight attitudinal questions related to hope, where high scores indicate an optimistic view of what can be done, and 11 attitudinal questions related to person-centred care, with a high score indicating understanding of the individual needs of patients. The Approaches to Dementia questionnaire had been tested in three studies29-31. In the present study, Cronbach's alpha ranged from 0.70 to 0.79. Both groups completed a three-item measure based on the Carer Stress Scale32, where respondents report on a five-point scale how stressful they find caring for patients with delirium/dementia, including where there is challenging behaviour. In the present study, Cronbach's alpha for stress ranged from 0.69 to 0.77. Volunteers completed a similarly formatted series of questions about confidence in dealing with people with delirium/dementia, although this is not a validated measure. At both pre- and post-intervention, Cronbach's alpha was 0.90. Both staff and volunteers completed two Likert-scaled questions about the program's acceptability, and an open-ended invitation to express opinions.
Volunteers also answered multiple choice questions about delirium adapted from an education resource33. In view of not being able to locate another measure, six multiple choice questions from this resource that were covered by the content of the training were used. Volunteers also completed the Alzheimer's Disease Knowledge Test34, which comprises 20 multiple choice questions about dementia. It is a recognised measure of Alzheimer's disease knowledge and has been used in subsequent papers assessing changes in Alzheimer's disease knowledge in undergraduate students35,36. The delirium and dementia questionnaires were combined to obtain an overall knowledge score.
Project implementation
Consultation with managers and nursing staff occurred throughout the planning phase via an established working group. A resource manual incorporating program procedures for staff and volunteers was written by CB. The resource manual and training materials are now publicly available37. Information sheets were sent electronically to nursing, allied health, medical and domestic staff, and posters were displayed on the wards. Daily information sessions were conducted for staff in the week preceding the implementation. The volunteer training program, underpinned by the principles of person-centred dementia care18, was developed and jointly delivered by CB and a colleague from Alzheimer's Australia NSW. The core training was facilitated over 4 days with an additional half day for mandatory hospital education. Session topics included:
- the volunteer role
- understanding dementia and delirium
- communication and person-centred care with the person with dementia
- understanding and responding to changed behaviour
- safe walking and encouraging gentle exercises with patients
- completion of personal profile and diversional and therapeutic activities
- completing menu selection and food choices
- positioning and assisting patients with eating and drinking
- fitting hearing aids and replacing batteries
- working in the hospital environment
- infection control and use of personal protective equipment
- volunteer documentation
- orientation to the ward and the program procedures.
All volunteers signed a copy of the Greater Southern Area Health Service (GSAHS) Volunteer Roles and Responsibilities and were bound by the GSAHS Code of Practice and Confidentiality for Volunteers. Issues of confidentiality were also covered in the training. If a volunteer did not feel comfortable supporting a patient they knew, they were empowered to inform staff and did not see the patient. Likewise, consent was sought from patients and/or their carers. They were advised that they could withdraw from having a volunteer at any time. However, more often the volunteer's knowledge of the patient and/or their family supported a connectedness and communication between the patients and volunteers.
Although results are reported only for the study sample (n=64), volunteers actually supported 86 patients during the study period. Volunteer duties included:
- sitting with patients individually or in group activity sessions
- making patients comfortable to support their sleep and rest - including adjusting pillows or providing warm drinks or a hand massage or foot massage
- making sure patients were wearing their glasses and hearing aids and checking that these were clean and working properly
- talking to patients about current events and surroundings
- assisting with eating and drinking and, when needed regularly, offering fluids to drink
- assisting with menu selection
- encouraging and accompanying walking as advised by the nurses or physiotherapist
- supporting activities patients enjoy - reading to them, playing cards
- using dementia-friendly communication
- communicating any concerns that may arise to the hospital staff or the dementia/delirium clinical nurse consultant as per volunteer guidelines
- writing down and communicating to staff any changes that are noticed in patient behaviour.
Care was provided over two shifts: 8 am - 12.30 pm and 3-7 pm, excluding weekends and public holidays. They cared for an average of 3.5 patients per shift (range 1-7 patients) with an average patient length of stay of 15 days (range 3-54 days). Regular volunteers worked either one shift per week or per fortnight. A casual pool of volunteers filled in for the volunteers on an ad-hoc basis. Once assigned, volunteers completed a personal profile with the patient or with their family carer. This profile recorded personal preferences and social information to maximise person-centred care7,38. Volunteers had their own documentation system, recording contacts with patients, patient response, therapeutic activities provided and the amount of any food and fluids given. For identification, volunteers were provided with a gold polo t-shirt with 'hospital volunteer' embroidered on the front.
Regular meetings were held with nurse unit managers and volunteers to monitor the program and address issues as they occurred. There was no volunteer coordinator position at the hospital, so CB assumed responsibility for the daily/weekly supervision and support of individual volunteers.
Main data analysis
The Statistical Package for the Social Sciences (SPSS; http://www.spss.com) was used to analyse data. Descriptive statistics were analysed using percentages, the Wilcoxon-Mann-Whitney test and independent t-test. Within-subjects t-test was used for comparing pre- and post-staff questionnaire responses, and repeated measures ANOVA was used to compare the pre-education, post-education and post-program questionnaire responses from volunteers. Planned contrasts were used to compare post-education and post-program scores with baseline scores.
Given the relatively small sample sizes, responses to the question soliciting views about the program from nursing staff and volunteers were manually coded into categories of 'benefits', 'difficulties' and 'suggestions'. Responses were then analysed for common themes that emerged by CB and, independently, by another researcher. Disputes were settled by consensus.
Ethics approval
This study was approved by the NSW GSAHS Human Research Ethics Committee (approval number 08/GSAHS/38)
Patients
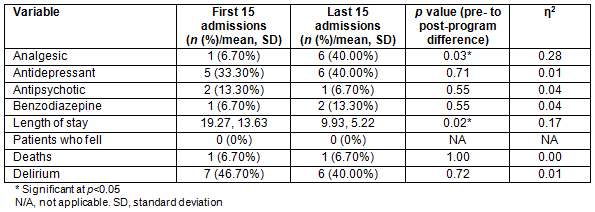
It was impossible to compare outcomes for this sample with data from patients in the period before the program because, pre-project, there was not the same attention to accurate diagnosis and assessment of delirium. Accordingly, to assess improvements over time, the authors looked at length of stay, anti-psychotic and other psychotropic medication use, whether patients were more likely to be on analgesics on discharge, and falls for the first 15 admissions and the last 15 admissions during the data collection period. The beginning of the project was regarded as valid baseline data because the skills and confidence of the volunteers were expected to improve as they gained experience and the project bedded in. No differences were found over time in the number of patients discharged on psychotropic medication. The last 15 patients, however, were significantly more likely to be discharged on analgesic medication, and length of stay was effectively half that of the first 15 patients (Table 3).
There were no falls for the first 15 and the last 15 patients but there were nine other falls during the project, for five patients. Only one fall occurred when a volunteer was on duty; the remainder of the falls occurred on the evening or night shift.
Table 3: Patient outcomes
Nursing staff
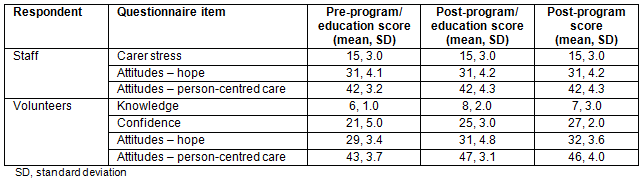
There was a low questionnaire return rate. Of the 50 questionnaires distributed, 29 (58%) were returned pre-program and 31 (62%) post-program. There were only 18 matched pre-post staff responses (36%). No significant changes were found between pre- and post-program staff scores in stress associated with caring for people with dementia (t(14)= -0.76, p=0.46, η2=0.00), hope from the Approaches to Dementia scale (t(15)=0.61, p=0.55, η2=0.00) or person-centred care from the Approaches to Dementia scale (t(17)=0.48, p=0.64, η2=0.00). See Table 4 for outcome means and standard deviations.
Table 4: Staff and volunteer outcomes
Volunteers
The questionnaire return rate for the volunteers was 100% pre-training and 89% post-program. There was no change over time in dementia and delirium knowledge but there was a change in attitude. See Table 4 for outcome means and standard deviations.
For the hope factor of the Approaches to Dementia scale, since Mauchly's test of sphericity indicated that the assumption was violated (χ²(2)=6.18, p=0.05), degrees of freedom were corrected using the Greenhouse-Geisser estimate (ε=0.73). There was significant movement on the hope factor (F(1.45, 20.31)=5.36, p=0.02, η2=0.28). Significant improvements seen after the education (p=0.01) were still evident at follow-up (p=0.00).
Mauchly's test of sphericity indicated a violation of the sphericity assumption for the person-centred care factor of the Approaches to Dementia scale (χ²(2)=8.00, p=0.02). Degrees of freedom were corrected with Greenhouse-Geisser estimate of sphericity (ε=0.70). The volunteers' understanding of the individual needs of patients changed (F(1.39, 20.90)=9.06, p=0.00, η2=0.38), with improvements in person-centred care after the education (p=0.02) being maintained at follow-up (p=0.02).
According to Mauchly's test of sphericity, the assumption was satisfied for volunteer confidence (χ²(2)=5.17, p=0.08). Volunteers were more confident in their understanding and care of patients post-program (F(2, 30)=11.79, p=0.00 η2=0.44). This increased confidence was significant post-education (p=0.01) and at follow-up (p=0.00).
Program acceptance
Staff acceptance: Of the 23 nursing staff who answered the qualitative items on the post-project questionnaire, 92% reported enjoyment in the program and 96% either agreed or strongly agreed that it was worthwhile and should continue. An open-ended question about drawbacks/benefits elicited only one outright criticism, from a nurse who otherwise appreciated the program but felt that some volunteers interfered in patient/nurse care. There were some complaints about having to complete the staff questionnaire and two suggestions that there should be volunteers on the night shift - thereby implying endorsement of the program. All the remaining comments (76%) were positive. Consensus between two independent researchers produced five themes. These were improved quality of care for patients because of volunteers' skills, better patient outcomes - in particular being more settled and contented, assistance and support for staff, reduced time-pressure on staff and assistance with nutrition and hydration for patients. Table 5 presents a sample of comments - with the following statement perhaps best encapsulating the majority of comments made:
The program took away a lot of pressure from nursing staff. The patients were more settled because they had one-to-one care. Also patients were accompanied in their meal times which resulted in them having a better dietary intake - nurses don't have enough time to provide this supervision time.
Acceptance of the program by staff was convincingly positive.
Table 5: Examples of staff comments about the program

Volunteer acceptance: All volunteers enjoyed being part of the program and agreed or strongly agreed that the program was worthwhile and should continue. Ninety percent of the comments concerned the benefits for patients, family/carers and/or themselves. The open-ended questions elicited three main themes: enjoyment in their interactions with patients, personal satisfaction in their role and positive patient response. The following volunteer statement is representative:
The benefits I experienced working with the patients is to see the change they go through. Some patients on the program, when first admitted are anxious, insecure, suspicious and lacking of trust. After a period of time with them, one sees the unfolding of trust, love, respect and cooperation. Very rewarding.
The remaining comments related to either finding the paperwork burdensome or the difficulties associated with trying to find stimulating methods to suit all patients.
Post-project outcome
Post-study, management and staff committed to continuing the program, with nurse unit managers and senior staff assuming responsibility for identifying and referring eligible patients. Program procedures were reviewed and change management techniques have successfully sustained the program. At the time of writing, the program continues with a volunteer coordinator 1 day per week, supported by a clinical nurse consultant (CB). A continuing quality improvement process monitors ongoing staff and volunteer satisfaction and perceptions of the program, with positive findings. Replication of the volunteer program has occurred at other rural hospitals, within and beyond the health area.
Discussion
The main finding of the present study is that it is possible, at minimal cost, to introduce and then maintain over time a program to improve quality of care for older people with dementia and/or delirium in an acute rural hospital. The program was inexpensive because the supportive care was undertaken entirely by volunteers, the only salaried position being a part-time coordinator who was employed post-research. The volunteers' main role was engaging with and providing person-centred support for inpatients assessed as having dementia or delirium or being at risk of delirium. This included basic activities such as general conversation, reassurance, encouraging ambulation or helping with feeding (Table 3). While this role required an understanding of and empathy for people with cognitive impairment, the tasks were mainly 'low-tech' and similar to the role of a family carer - activities for which busy nurses often have limited time (see also quote 4, Table 5)17.
Volunteers were educated about dementia and delirium but they seem to have been well informed at the outset because there was no difference pre- and post-program in knowledge scores, probably because many were former carers or had worked pre-retirement in caring professions. However, learning from the education, together with the close contact with the care of multiple patients, does not appear to have changed their attitude to the nature of individualised care and reduced the endorsement of pessimistic statements.
In addition, there was significant improvements on both the hope and person-centred care factors on the Approaches to Dementia questionnaire. These changes were evident following the education and, interestingly, were maintained to the end of the program. There is also evidence of greater confidence after the education and at the end of the program in working with patients.
All volunteers stayed in the program for the entire 6 months and expressed great satisfaction with the work. This may have been helped by mature age and the nature of rural communities, which meant the volunteers often already knew the patient or family. Nevertheless, such knowledge supported connectedness and communication, as well as continuity.
There were no changes in staff measures. This may be related to the low return of questionnaires but is perhaps not surprising given the exposure of staff in this hospital to many cognitively impaired elderly patients over time. In addition, nursing staff were not required to change practice other than be systematic in screening for dementia/delirium at admission. The main finding with staff was that they accepted the volunteer program and have continued to do so. Although there were occasional boundary disputes, nurses not only tolerated volunteers on the wards but also felt they complemented and supported the nursing role. They 'took the heat off', met the need for 'increased care', led to 'smoother recovery' and produced more 'content and settled patients', for example (Table 7). A number of studies have shown the frustrations and difficulties nurses experience when they do not have the time to provide for these patients39.
Acceptance of changes by staff in the care delivered to older people is by no means a given40 and, beyond the program requiring minimal change and the pragmatic fact that nurses found it helpful, there are other factors likely to have reduced resistance. Two common themes in the compliance literature and in the present study are that nursing staff were active participants throughout the planning stage, and that the program was introduced in systematic stages. Other factors are more site-specific - in the present study the hospital was relatively small, there was a relatively stable workforce, and the nurse introducing the program (CB) had been a long-term colleague within the hospital.
For patients, the most striking finding was that, as the project bedded in, length of stay was almost halved, the last 15 admissions staying for a mean duration of less than 10 days. If replicated, this would be a significant cost saving. There was no significant increase in the number of patients discharged on more psychotropic medications; it is possible that this is a positive result given that the default strategy for patients with serious behavioural disturbance had previously been PRN (as-needed) anti-psychotic medications. There was, however, a small increase in those taking analgesics, suggesting that close proximity to patients had given volunteers a better awareness of the significant issue of unrecognised and therefore untreated pain in dementia41.
The value of volunteers in falls prevention cannot be determined by findings of this project, but it is suggestive that only one fall occurred when volunteers were on duty. Given that most falls occurred in the evening or night, the request from two nurses for volunteer shifts at night, while not practical, is understandable. Future evaluations need to examine whether volunteers can minimise falls at least during the day, given the multiple negative consequences and costs of falls in older people42.
The main limitation of the present study is that this was a pilot project, not a controlled trial, with a relatively small sample - partly because of a low response rate with staff questionnaires. Low response rates likely reflect the reality of conducting research in these types of setting. These hospital wards are extremely busy places, where staff must prioritise the many and varied clinical needs of the patients over completing questionnaires. The volunteer confidence measure was not a validated instrument. Clinically, the program has been a success the findings cannot necessarily be generalised to other hospitals because the authors worked in a rural Australian setting with known staff and minimal turnover, and the project was introduced by a familiar senior nurse. While the program is being rolled out to other rural hospitals, the authors cannot conclude its utility in urban centres.
Nevertheless, the authors have shown that it is possible to introduce and sustain a program like this at minimal cost in a rural hospital, with nursing staff accepting and appreciating that it is making a difference to them and the patients in their care. There is further evidence that having trained and well-supervised volunteers reduces patients' length of stay, increases awareness of untreated pain and possibly helps reduce falls. Finally, for the volunteers themselves, the program has provided fulfilment and an experience of positive contribution to the wellbeing of patients.
Acknowledgements
Sincere appreciation is extended to the wonderful volunteers for their person-centred care, commitment and contributions to ongoing program improvements, the participating patients and family carers and the managers and staff of Bega Hospital. Particular acknowledgement and appreciation is extended to Barbra Williams from Alzheimer's NSW for her partnership and support in establishing and implementing the volunteer program.
References
1. Australian Institute of Health and Welfare. Dementia care in hospitals: costs and strategies. Canberra: AIHW, 2013.
2. Access Economics. Caring places: planning for aged care and dementia 2010-2050. Canberra: Access Economics, 2010.
3. Australian Bureau of Statistics. 4106.1 - Population Ageing in New South Wales, 2008, Dec. 2008 (Internet) 2010. Available: http://www.abs.gov.au/ausstats/abs@.nsf/mf/4106.1?OpenDocument (Accessed 30 June 2010).
4. Richard Gilbert Consulting. Bega Valley Health Service clinical service plan final draft: 8 November 2011. Sydney: Richard Gilbert Consulting, 2011.
5. Moyle W, Olorenshaw R, Wallis M, Borbasi S. Best practice for the management of older people with dementia in the acute care setting: a review of the literature. International Journal of Older People Nursing 2008; 3(2): 121-130.
6. Cunningham C. Understanding challenging behaviour in patients with dementia. Nursing Standard 2006; 20(47): 42-45.
7. Cunningham C, Archibald C. Supporting people with dementia in acute hospital settings ... first in a series of five. Nursing Standard 2006; 20(43): 51-55.
8. McCloskey RM. Caring for patients with dementia in an acute care environment. Geriatric Nursing 2004; 25(3): 139-144.
9. Australian Health Ministers Advisory Council. Clinical practice guidelines for the management of delirium in older people. Melbourne: Victorian Department of Human Services, 2006.
10. Fick DM, Hodo DM, Lawrence F, Inouye SK. Recognizing delirium superimposed on dementia. Journal of Gerontological Nursing 2007; 33(2): 40-47.
11. Fong TG, Tulebaev SR, Inouye SK. Delirium in elderly adults: diagnosis, prevention and treatment. Nature Reviews Neurology 2009; 5(4): 210-220.
12. Härlein J, Halfens RJ, Dassen T, Lahmann NA. Falls in older hospital inpatients and the effect of cognitive impairment: a secondary analysis of prevalence studies. Journal of Clinical Nursing 2011; 20(1-2): 175-183.
13. Hill KD, Vu M, Walsh W. Falls in the acute hospital setting - impact on resource utilisation. Australian Health Review 2007; 31(3): 471-477.
14. Schofield I. Delirium: challenges for clinical governance. Journal of Nursing Management 2008; 16(2): 127-133.
15. Borbasi S, Jones J, Lockwood C, Emden C. Health professionals' perspectives of providing care to people with dementia in the acute setting: toward better practice. Geriatric Nursing 2006; 27(5): 300-307.
16. Byers DC, France NEM. The lived experience of registered nurses providing care to patients with dementia in the acute care setting: a phenomenological study. International Journal for Human Caring 2008; 12(4): 44-49.
17. Nolan L. Caring for people with dementia in the acute setting: a study of nurses' views. British Journal of Nursing 2007; 16(7): 419-422.
18. Kitwood T. Dementia reconsidered: the person comes first. Buckingham, UK: Open University Press, 1997.
19. Moyle W, Borbasi S, Wallis M, Olorenshaw R, Gracia N. Acute care management of older people with dementia: a qualitative perspective. Journal of Clinical Nursing 2011; 20(3-4): 420-428.
20. McCormack B, Karlsson B, Dewing J, Lerdal A. Exploring person-centredness: a qualitative meta-synthesis of four studies. Scandinavian Journal of Caring Sciences 2010; 24(3): 620-634.
21. National Research Ageing Institute. What is person centred health care? A literature review. Melbourne: Victorian Government Department of Human Services, 2006, p. 105.
22. Jones J, Borbasi S, Nankivell A, Jockwood C. Dementia related aggression in the acute sector: is Code Black really the answer? Contemporary Nurse 2006; 21(1): 103-115.
23. Day J, Higgins I, Koch T. Delirium and older people: what are the constraints to best practice in acute care? International Journal of Older People Nursing 2008; 3(3): 170-177.
24. Inouye SK, Bogardus STJ, Charpentier PA, Leo-Summers L, Acampora D, Holford TR, et al. A multicomponent intervention to prevent delirium in hospitalized older patients. New England Journal of Medicine 1999; 340(9): 669-676.
25. Caplan G, Harper E. Recruitment of volunteers to improve vitality in the elderly: the ReViVe study. Internal Medicine Journal 2007; 37: 95-100.
26. Palmisano-Mills C. Common problems in hospitalized older adults: four programs to improve care. Journal of Gerontological Nursing 2007; 33(1): 48-54.
27. Sandhaus S, Zalon ML, Valenti D, Dzielak E, Smego RA, Arzamasova U. A volunteer-based Hospital Elder Life Program to reduce delirium. Health Care Management (Frederick) 2010; 29(2): 150-156.
28. Molloy DW, Alemayehu E, Roberts R. Reliability of a Standardized Mini-Mental State Examination compared with the traditional Mini-Mental State Examination. American Journal of Psychiatry 1991; 148(1): 102-105.
29. Macdonald AJ, Woods RT. Attitudes to dementia and dementia care held by nursing staff in U.K. 'Non-EMI' care homes: what difference do they make? International Psychogeriatrics 2005; 17(3): 383-391.
30. Lintern T, Woods B, Phair L. Training is not enough to change care practice. Journal of Dementia Care 2000; 8(2): 15-17.
31. Zimmerman S, Williams CS, Reed PS, Boustani M, Preisser JS, Heck E, et al. Attitudes, stress, and satisfaction of staff who care for residents with dementia. Gerontologist 2005; 45(suppl 1): 96-105.
32. Bird M, Llewellyn-Jones R, Korten A, Smithers H. A controlled trial of a predominantly psychosocial approach to BPSD: treating causality. International Psychogeriatrics 2007; 19(5): 874-91.
33. Vancouver Island Health Authority. Delirium in the older person: a medical emergency: pre-post test. (Internet) 2006. Available: http://www.viha.ca/mhas/resources/delirium/tools.htm (Accessed 8 November 2008).
34. Dieckmann L, Zarit S, Zarit J, Gatz M. The Alzheimer's disease knowledge test. Gerontologist 1988; 28(3): 402-407.
35. Karlin NJ, Dalley M. Alzheimer's disease knowledge: a comparison study. Journal of Clinical Geropsychology 1998; 4(3): 211-217.
36. Sullivan K, Finch S, O'Conor F. A confidence interval analysis of three studies using the Alzheimer's disease knowledge test. Aging and Mental Health 2003; 7(3): 176-181.
37. NSW Agency for Clinical Innovation. Volunteer dementia & delirium care implementation and training resource. Chatswood, Sydney: Agency for Clinical Innovation, 2014.
38. Edvardsson D, Nay R. Acute care and older people: challenges and ways forward. Australian Journal of Advanced Nursing 2009; 27(2): 63-69.
39. Edberg A-K, Bird M, Richards DA, Woods R, Keeley P, Davis-Quarrell V. Strain in nursing care of people with dementia: nurses' experience in Australia, Sweden and United Kingdom. Aging and Mental Health 2008; 12(2): 236-243.
40. Cameron I, Kurrle S, Quine S, Sambrook P, March L, Chan D, et al. Improving adherence with the use of hip protectors among older people living in nursing care facilities: a cluster randomized trial. Journal of the American Medical Directors Association 2011; 12(1): 50-157.
41. Cohen-Mansfield J, Lipson S. The utility of pain assessment for analgesic use in persons with dementia. Pain 2008; 134(1-2): 16-23.
42. Chen JS, Simpson J, March L, Cameron I, Cumming R, Lord S, et al. Risk factors for fracture following a fall amongst older people in residential care facilities in Australia. Journal of the American Geriatrics Society 2008; 56(11): 2020-2026.

