A sustainable workforce is one which is not person-dependent but at the same time values the individual skills, experiences and ideas a person can bring to a role ... It is one that is able to provide continuous, reliable and safe care to patients ... because staff are appropriately skilled, oriented, supported and rewarded. It is one where staff movement is pre-empted, planned and refilled in a timely and appropriate manner. It is one that doesn't rely on agency and locum staff, but grows a local workforce wherever possible and provides the same incentive packages as those afforded outsiders ... It can be achieved by employing people who are passionate about their job and love a rural/remote lifestyle (questionnaire participant QP172).
In rural and remote regions access to healthcare services is reliant on the availability of a competent workforce. However, attracting and retaining health professionals in rural and remote regions is a global challenge exacerbated by the disparity of distribution between urban, and rural and remote areas1,2. Global workforce shortages intensify challenges associated not only with attraction and retention; they reduce access to health services for vulnerable populations who experience poorer health outcomes than urban populations1-3. These challenges, which resonate with health professionals in remote regions across the world, have led to the realisation that to improve access to health services more sustainable workforces are required. While many researchers have identified factors that influence voluntary turnover and workforce retention4-6, others have focused on the sustainability of health systems and health workforces1,7. Described so eloquently in the opening passage above, the achievement of sustainable remote health workforces is complicated, requiring an appropriate balance of both financial and human resources.
The present study contributes to the research in this field by examining the challenges from the perspectives of health professionals who are currently working in remote regions across various professions (nursing, medical, Indigenous health workers, allied health and dental). This is an area where research gaps have been identified2,5,6. This approach seeks to identify aspects of workforce sustainability beyond the boundaries of a particular health profession. Acknowledging the work of researchers who have examined turnover and retention of particular rural and remote workforces including nurses7-9, doctors10,11 and allied health professionals12,13, this study seeks to build on current knowledge using a complementary approach. This human resource management (HRM) approach examines workforce sustainability through the complementary field of management studies with its evidence-based people and workforce management focus. The characteristics of sustainable remote health workforces emerged through using a management lens to examine how current remote health professionals describe a sustainable remote health workforce.
Wakerman and Humphreys1 caution against focusing on workforce in isolation and this point is well founded. There are always risks in considering aspects of a complex issue in isolation. However, focusing on one aspect enables the researcher to consider the issue at a deeper level and often provides an opportunity to use an alternative lens. For this study, a management lens offers an alternative perspective with a complementary body of evidence through which to examine the issue. Furthermore, this provides the opportunity to use a pragmatic approach more suited to finding solutions than identifying problems, which moves away from the deficit approach1,14.
The aim of this study was to examine how remote health professionals (1) describe a sustainable remote health workforce and (2) propose how it could be achieved. A sustainable remote health workforce that requires further explanation, as follows.
'Sustainability'
Humphreys et al7 propose that for 'the rural and remote health context, the concept of sustainability refers to the ability of a health service to provide ongoing access to appropriate quality care in a cost-efficient and health effective manner' (p. 33). This study considers that efforts to improve workforce sustainability should be compatible with these objectives. Therefore, workforce sustainability refers to the continual supply of competent health professionals to provide health services in a manner appropriate to the remote context. Ultimately, sustainability is built on a strong foundation with appropriate leadership and management practices prepared to meet the challenges and respond to the opportunities, ensuring the needs of all interested parties continue to be realised. Humphreys et al7 conclude that sustainable rural health services must take 'account of the social, economic and environmental dimensions influencing sustainability', suggesting that the key considerations are 'access to services, quality of care and cost of their provision' (p. 35). Furthermore, the contribution of a consistent and competent workforce and access to health services in improving the health of rural and remote populations is frequently emphasised1,15,16.
'Remote'
There are many ways to describe geographical remoteness. In Australia, remote regions are often referred to as 'the outback', 'the bush', 'rural' and 'remote'. The geographical context for this study is that of a remote tropical setting in northern Australia, an area with similar climatic and geographical challenges for remote health professionals. This includes areas known as the Kimberley (northern Western Australia), the Top End (Northern Territory), north-western Queensland and far north Queensland. To improve the consistency in reporting, the Australian Bureau of Statistics (ABS) categorised Australia into five geographic regions based on geographical remoteness, which established common terminology for data analysis17. For this study, the two categories, 'remote' (which includes areas that some may refer to as rural) and 'very remote' were combined and are referred to collectively as 'remote'. Therefore, the remote health professionals described in this study worked in areas of northern Australia categorised by the ABS as 'remote' or 'very remote'.
This article analysed the findings from two separate yet complementary data sources: interviews and online questionnaires. First, a purposive sampling method was undertaken to recruit interview participants from different professions and locations currently working or managing health professionals working in remote regions. Participants included managers (health managers and human resource managers) and health professionals with longevity (more than 5 years) in remote regions. Interview participants (IP) were asked the following question: 'This 'project is called A Sustainable Remote Health Workforce; in your own words, what do you think a sustainable remote health workforce would be? What would it look like?' Their descriptions provide evidence for the ways in which these participants view a sustainable remote health workforce. A thematic analysis of the transcripts (n=24) was conducted using NVivo v10 (QSR International; http://www.qsrinternational.com) and the emergent themes formed the first-level coding. These emergent themes were then used to guide data analysis for the responses from the questionnaire in which current remote health professionals were asked the same question.
The online questionnaire was distributed to health professionals working in remote regions of northern Australia. The questionnaire was distributed directly to remote health professionals (n=1317) by eight organisations who agreed to participate in this study. This ensured that the questionnaire was only distributed to health professionals who were currently working in regions identified as remote by this study. A response rate of 21% was achieved with 272 questionnaires returned. This article discusses the findings for the 191 participants (QP) who provided a written response to the same question that was asked of IPs. A thematic analysis of the text responses was conducted using NVivo v10 using the emergent themes from the interview data to guide analysis. The findings from both approaches were compared and contrasted to capture the breadth and depth of the characteristics of a sustainable remote health workforce identified through the study.
Ethics approval
Approval to conduct this research was granted by James Cook University Human Research Ethics Committee (HREC) (H5227), Townsville Hospital Health Service HREC (HREC113/QTHS/225) and the Western Australia Country Health Service HREC (2013:31).
The characteristics of a sustainable remote health workforce, as described by participants, were diverse and varied; however, there were many common characteristics. Analysis of the data from the interviews revealed that there were three extant themes: people, practice and place. Furthermore, analysis of the questionnaire data identified themes consistent with the findings from the interview data. The extant themes and their influence on the attainment of a sustainable remote workforce are examined, with a summary of the key characteristics presented in Tables 1-3.
People
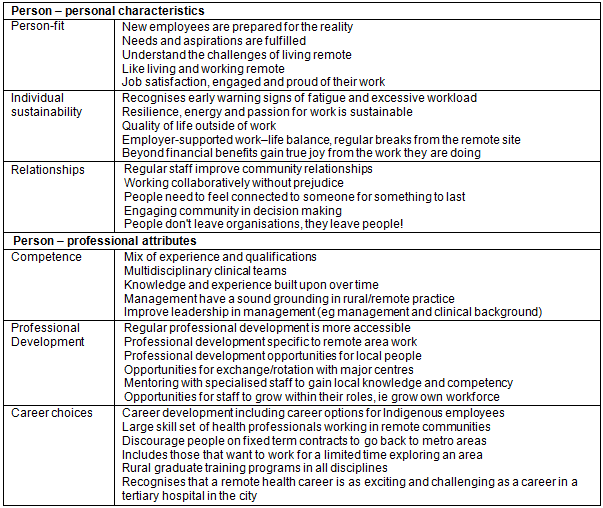
The 'people' theme comprised the aspects that related to the person's characteristics, both personal and professional. Personal characteristics included person-fit, individual sustainability and relationships. These are the characteristics of a person that build resilience and contribute to an individual's compatibility with the community and the organisation. Professional attributes included competence, professional development and career choices. These are the attributes of a person that contribute to their capacity to perform their work competently. The 'person' characteristics described by the questionnaire participants are summarised in Table 1.
Participants discussed aspects of personal characteristics and professional attributes for individual health professionals. However, there were differences in terms of the priority of aspects; for example, should the priority be person-fit or professional competence? Most participants discussed aspects of 'person-fit', explaining the importance of employing the right people for remote regions, with one saying:
... there needs to be some sort of selection process so that we have people working in remote health for who it's a career, it's a passion, not just a holiday to pay the mortgage. ... part of the sustainability would be recognising that remote and isolated practice is actually a specialty area ... Not just anyone who has a registered nurse qualification can actually be a remote area nurse, nor should they be (IP1).
Several participants commented on career paths with one suggesting that remote nursing be considered a speciality area of nursing, providing a more defined career path. Thus, improving access to professional development may generate an increase in remote career options, contributing to increased remote health workforce sustainability. While there was no consensus about whom the right person was or how to recruit them, there was a strong sense that personal characteristics and professional attributes play an important role.
Table 1: 'Person' characteristics of a sustainable remote health workforce identified by questionnaire participants
Practice
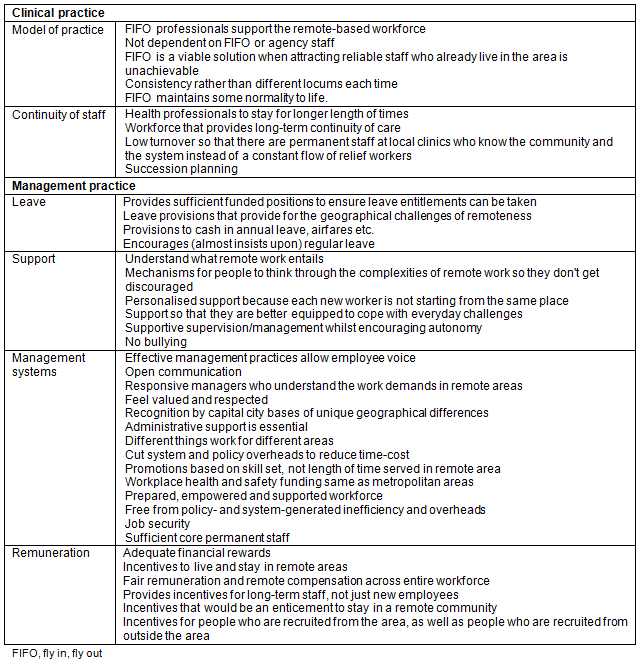
The 'practice' theme comprised the aspects that related to both clinical and management practice. Clinical practice included models of practice and continuity of staff. These are the aspects of clinical practice that influence health service delivery, workforce composition and systems of workforce design. Management practice included leave, support, management systems and remuneration. These management practices influence aspects of organisational and health system policy that contribute to the sustainability of the remote health workforce. The 'practice' characteristics described by the questionnaire participants are summarised in Table 2.
Participants suggested that turnover and vacancies impact on continuous service provision; for example, one respondent said, 'you need to be realistic with sustainable, but I guess it would be something like ensuring that 95% of your positions remained filled' (IP5), while another said sustainability was 'an organisation being able to have a workforce that is capable of delivering a service at 100%' (QP136). Some proposed that continuity of care was closely associated with continuity of health professionals, with one participant saying 'our poor clients, they have such a change of faces, and it takes so long to develop that relationship' (IP5). In contrast, another participant suggested that 'the way forward would be similar to mining and having a FIFO [fly in, fly out] system' (IP6). As one participant explained:
A sustainable workforce does not mean people who work in one position/one site for a long time. It means the positions give individuals the opportunity to grow in their field and are supported during their tenure (QP162).
Management practices contribute to the sustainability of the remote health workforce according to the participants in various ways, including filling vacancies, backfill, attracting health professionals, remuneration and financial incentives, employment patterns and models of practice (eg FIFO). More specifically, some participants suggested that improvements in management practices will influence sustainability, with one participant saying, 'we need managers to actually be skilled in distance management [...] just because they are able to manage a team face to face doesn't mean they have any capability of managing a team from a distance' (IP1). Leadership is a key aspect of effective management practices, as was pointed out by one participant:
... remote services have the opportunity to be more flexible and innovative than large metropolitan services but they need good leadership and the options to do things in ways that work well for their particular areas. Sometimes it just does not work trying to apply models that work well in other parts of the country (QP122).
Table 2: 'Practice' characteristics of a sustainable remote health workforce identified by questionnaire participants
Place
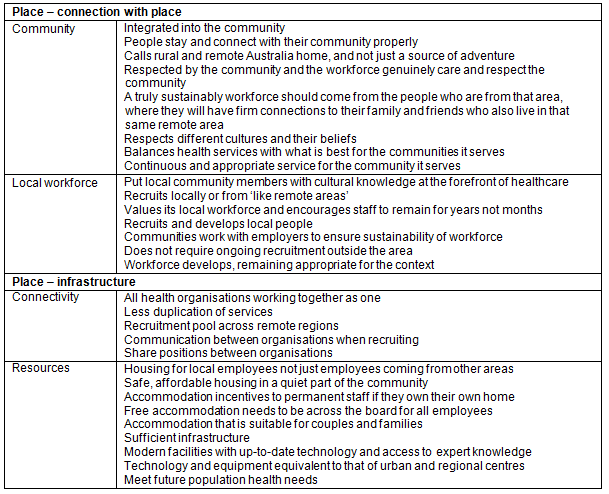
The 'place' theme comprised the aspects that related to the physical work location. They include the person's connection to the place (geographic location/community) and the infrastructure. Connection with place included community and local workforce. These characteristics result from an emotional connection to place. Infrastructure included connectivity and resources. These are the attributes of place that contribute to sustainability through cooperation, collaboration and adequate infrastructure and the resources to work effectively. The 'place' characteristics described by the questionnaire participants are summarised in Table 3.
Sustainability may be achieved through greater connectivity between the different health service providers. One participant emphasised that 'a sustainable remote health workforce is actually having appropriate people delivering [health services] according to the population needs' (IP3). Therefore, connection with the community is vital. Aspects of workforce sustainability that described a connection with place were discussed, suggesting that the physical work environment contributes to sustainability. For example, health professionals suggested that a sustainable remote health workforce 'needs to have people that are living in the community that belong to the community' (IP12). Another explained that it is about community acceptance:
... sustainable remote health workforce is actually a workforce that is developed from the community and it is a workforce that the community accepts as well. I think there's not enough attention paid to the right fit in a community (IP3).
Accommodation in remote regions was frequently mentioned as an infrastructure concern, with participants suggesting that addressing accommodation inadequacies was essential. Some participants described aspects of perceived disadvantaged, saying that 'free accommodation needs to be across the board for all employees, not just the ones who come from outside our area (needs to be fair to locals who want to stay)' (QP58). Many participants described perceived inequities with accommodation as well as other incentives offered to attract health professionals to remote regions. In addition, health professionals described their experiences with poor accommodation. One manager, explained that 'whilst we all want to be intrinsically motivated' accommodation is important because if they had 'dodgy accommodation, if people weren't sure if they were going to be assaulted in the night ... [it] doesn't matter what the manager does, you [are] not going to keep them there' (IP11). This suggests that the influence of infrastructure is such that the absence of basic conditions impacts the ability of management practices to improve retention and, in fact, they are suggesting that management practices are negated in these circumstances.
Table 3: 'Place' characteristics of a sustainable remote health workforce identified by questionnaire participants
Discussion
Management practices were recognised as being critical for developing, implementing and maintaining the sustainability of remote health workforces. Studies investigating turnover and retention in rural and remote regions identified that management practices are interrelated with other aspects of remote health care5,6,18. In addition, the influence of effective management practices on the sustainability of remote workforces continues to be specifically highlighted2,6,19,20. It is believed that management practices build the foundation of sustainable workforces, particularly in remote regions where health services understand the value of having the right person, with the right skills, in the right place, at the right time6,21.
This study examined the factors that influence the achievement of a sustainable remote health workforce, through three extant themes: people, practice and place. However, it is acknowledged that sustainability is influenced by factors outside the scope of this study, such as political, economical, social and environmental factors (Fig1). While these factors contribute to the holistic approach needed to achieve sustainability, it is beyond the scope of this study to specifically comment on their influence other than to agree with the current evidence that improvements to healthcare funding, socioeconomic and environmental conditions that benefit the health outcomes for rural and remote populations are a critical component of sustainability7,18,21.
Focusing on the three extant themes, the influence of management practices on workforce sustainability is apparent. The 'person' factors that emerged in this study were not remarkable; they exist in any healthy employment relationship5,6,21. They include a workforce where competent, resilient and passionate health professionals who like the environment in which they work have access to adequate, regular leave and professional development opportunities that allow them to gain new skills for advancement4,5. Additionally, healthy relationships with colleagues and managers enhance collaboration, and engagement with the local community5,22. While management practices cannot ensure the community's acceptance of individual health professionals, managers can work with community members to ensure appropriate person-fit and then support their adjustment into the remote community. Hence, new employees who are well prepared for the remote workplace are welcomed and orientated in localised practices5,23. Improved collaboration between health service providers can reduce duplication of services, provide opportunities for professional development, career pathways and develop opportunities to share 'talent' in remote regions. This may benefit the health professional, the community and health service providers6.
Models of service delivery are improved where management practices support the workforce through clear communication and genuine understanding of the challenges of remote work environments. Competent, engaged health professionals, with high levels of job satisfaction, may be located in the remote region or be regular FIFO health professionals who frequently visit the remote location15,24,25. These regular FIFO health professionals can provide relief and additional clinical knowledge improving health outcomes for the community whilst providing continuity of care where these clinical services are not available locally15,25. Hence, effective management practices including adequate health and safety, maintaining reasonable levels of core staff, backfill and expediently filling vacancies can enhance the benefits of flexible models of service delivery12,16,22,26.
Interestingly, the health professionals who participated in this study provided a realistic and pragmatic contribution to the narrative. They described a sustainable remote health workforce in terms of the people that comprise it, the people that have a stake in it and the people who manage it, yet remain focused on the overall purpose - providing appropriate health services for remote populations. While several suggest improving current resources, such as housing and clinic equipment, many suggested areas where sustainability arises from equity2,6,21. In particular, they suggest that the inequity in incentive payments between clinical disciplines influences retention where health professionals work in teams of equivalent contribution27. Similarly, they highlight the difference in incentives and benefits offered to attract new health professionals compared to those received by community residents or long-term health professionals. This disparity appears to make the local and long-term health professionals feel less valued. Management practices influence this sense of inequity in remuneration and incentives. In addition, the perceived inequity between the infrastructure and resources further contributes to the sense of injustice. Thus, to improve workforce sustainability, managers could focus on reducing perceived inequities and embracing opportunities to develop the local workforce2,6,25.
In remote regions where chronic workforce shortages are reported, to attain workforce sustainability attention to both attraction and retention is critical25. Health professionals make decisions about remaining with their employer from within the remote practice setting20,28. This suggests that an increased focus on retaining those less transient health professionals, such as those with community ties or long-term community-based histories, should be areas in which retention rewards are focused. This approach would avoid feelings of inequity and disadvantage, as described by some remote health professionals. Drawing on psychological contract theory, which describes the unwritten contracts that exist between an employer and an employee29, it appears that these perceived inequities may be factors that fuel dissatisfaction. Campbell et al4 cite Herzberg's motivation-hygiene theory, explaining that employees need sufficient extrinsic rewards to not feel dissatisfied, before the intrinsic motivators that are present in the work itself will lead to job satisfaction. Accordingly, management practices that minimise dissatisfaction are paramount in areas where turnover is high. Management practices that are perceived as fair make all employees feel valued and reinforce the balance of reciprocity29,30, and are less likely to breach an employee's perception of the psychological contract. Such fair practices traditionally influence retention through management concepts such as organisational commitment, occupational citizenship behaviour and job satisfaction29,31.
The World Health Organization2 suggests there is a need for further evaluation of the varied attraction and retention strategies that have been implemented globally. It reports that 'policy-makers should be aware of the potential sensitivities surrounding giving health workers specific financial incentives'(p. 29)2, going on to describe the problems that this may cause with others not covered under the incentive schemes. Buykx et al6 report on a systematic literature review that found that despite increased financial incentives for medical professionals, 'there is little evidence that these incentives have made any significant difference to the medical workforce supply in underserved areas' (p. 102). While incentives have been the focus for improving retention, WHO2 suggests that personal and professional support for isolated health professionals is a complementary intervention and that they are more 'likely to augment each other's impact but are ineffective in isolation'(p. 30)2. In fact, WHO2 suggests that a core requirement for all of the retention incentives and interventions 'to be effective will come from developing, deploying and motivating effective local service managers and strengthening human resources management systems' (p. 30).
Hence, effective management practices and leadership appear to be the way to achieve and maintain sustainability of remote health workforces6,20,21. The WHO2 findings are conveying a similar message to that of the managers and health professionals who participated in this study when proposing that incentives and rewards in isolation are not effective in improving long-term workforce retention21. Furthermore, a supportive work environment and management practices that are congruent with the remote context, when combined with equitable incentives and rewards, are more likely to influence workforce sustainability in the long term16,20.
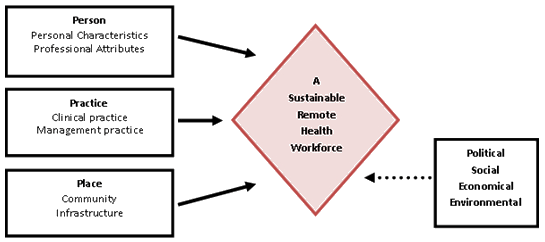
Figure 1: Characteristics of a sustainable remote health workforce.
Limitations
Low participation rates are a disadvantage of online questionnaires32. The response rate of 21% was low, which means that the findings may not be representative of all remote health professionals. The low response rate is consistent with this type of research tool, particularly with participants from rural and remote regions with the Australian Medical Association reporting a response rate of 13%, and Rural Doctors Association of Australia reporting 13.5% for online questionnaires in rural Australia33,34. In addition, there may be a self-selection bias, with health professionals interested in the topic more likely to participate32,35,36, or a non-response bias, which 'refers to the bias that exists when respondents to a survey are different from those who did not respond in terms of demographic or attitudinal variables'(p. 411)36. In studies with a low response rate, the potential self-selection bias and non-response bias mean that the findings are not generalisable. However, the findings were consistent with the literature, suggesting that the sample was adequate to provide a good indication of the current remote health professional's perspective.
This study made it clear that it sought the view of current remote health professionals about the sustainability of remote health workforces; however, it did not define 'remote' in the questionnaire. While it is not believed to have negatively impacted the findings it is acknowledged as a limitation given the different interpretations of 'remote', particularly the differentiation between 'remote' and 'rural'17.
The sustainable remote health workforce described in the opening passage of this article is not idealistic, nor is it unrealistic. It is an insightful narrative from a health professional with experience and expertise in remote health - someone who knows the landscape. Furthermore, it is indicative of the way in which current remote health professionals describe a sustainable remote health workforce. The solutions-focused approach of this study revealed possibilities for policies that could have a positive influence on the sustainability of remote health workforces. The findings reinforced the importance of ensuring that health professionals with current remote work experience and expertise are contributing to the planning and strategy development for the achievement of sustainable future remote health workforces. As seen in the opening passage, remote health professionals have much to offer this discussion.
A sustainable remote health workforce is about an appropriate mix of health professionals with suitable personal characteristics and professional attributes to meet remote populations' needs. Beyond person-fit, a sustainable remote health workforce requires an appropriate model of service delivery that provides continuity of health care through improved retention of competent health professionals. This study found that management practices influence the outcomes of policy choices that provide for the achievement of sustainable remote health workforces. Hence, realising a sustainable remote health workforce requires management practices focused on aspects of people, practice and place.
References
1. Wakerman J, Humphreys J. Sustainable workforce and sustainable health systems for rural and remote Australia. Medical Journal of Australia Open 2012; Supplement 3: 14-17.
2. WHO. Increasing access to health workers in remote and rural areas through improved retention. France: WHO Press, 2010.
3. Perkins D, Larsen K, Lyle D, Burns P. Securing and retaining a mental health workforce in Far Western New South Wales. Australian Journal of Rural Health 2007; 15: 94-98.
4. Campbell N, McAllister L, Eley D. The influence of motivation in recruitment and retention of rural and remote allied health professionals: a literature review. Rural and Remote Health (Internet) 2012; 12(3): 1900. Available: www.rrh.org.au (Accessed 29 October 2015).
5. Onnis L, Pryce J. Health professionals working in remote Australia: a review of the literature. Asia Pacific Journal of Human Resources 2016; 54: 32-56. http://dx.doi.org/10.1111/1744-7941.12067.
6. Buykx P, Humphreys J, Wakerman J, Pashen D. Systematic review of effective retention incentives for health workers in rural and remote areas: towards evidence-based policy. Australian Journal of Rural Health 2010; 18: 102-109.
7. Humphreys JS, Wakerman J, Wells R. What do we mean by sustainable rural health services? Implications for rural health research. Australian Journal of Rural Health 2006; 14(1): 33-35. http://dx.doi.org/10.1111/j.1440-1584.2006.00750.x.
8. Garnett S, Coe K, Golebiowska K, Walsh H, Zander K, Guthridge S, Li S, Malyon R. Attracting and keeping nursing professionals in an environment of chronic labour shortage: a study of mobility among nurses and midwives in the Northern Territory of Australia. Darwin: Charles Darwin University Press, 2008.
9. Hegney D, McCarthy A, Rogers-Clark C, Gorman D. Retaining rural and remote area nurses. The Queensland, Australia experience. The Journal of Nursing Administration 2002; 32(3): 128-135. http://dx.doi.org/10.1097/00005110-200203000-00005.
10. Hays R, Wynd S, Veitch C, Crossland L. Getting the balance right? GPs who chose to stay in rural practice. The Australian Journal of Rural Health 2003; 11(4): 193-198. http://dx.doi.org/10.1111/j.1440-1584.2003.tb00535.x.
11. Humphreys JS, Jones MP, Jones JA, Mara P. Workforce retention in rural and remote Australia: determining the factors that influence length of practice. Medical Journal of Australia 2002; 176(10): 472-476.
12. Kruger E, Tennant M. Oral health workforce in rural and remote Western Australia: practice perceptions. Australian Journal of Rural Health 2005; 13(5): 321-326.
13. O'Toole K, Schoo AM. Retention policies for allied health professionals in rural areas: a survey of private practitioners. Rural and Remote Health 10(2): 1331. (Online) 2010. Available: www.rrh.org.au (Accessed 29 October 2015).
14. Gorton S. Who paints the picture? Images of health professions in rural and remote student resources. Rural and Remote Health (Internet) 2015; 15(3): 3423. (Online) 2015. Available: www.rrh.org.au (Accessed 29 October 2015).
15. Hunter E, Onnis L, Santhanam-Martin R, Skalicky J, Gynther B, Dyer G. Beasts of burden or organised cooperation: the story of a mental health team in remote, Indigenous Australia. Australasian Psychiatry 2013; 21(6): 572-577.
16. Fisher KR, Fraser JD. Rural health career pathways: research themes in recruitment and retention. Australian Health Review 2010; 34: 292-296.
17. Australian Bureau of Statistics. ASGC remoteness classification: purpose and use. Census paper no. 03/01. Available: http://www.abs.gov.au/websitedbs/D3110122.nsf/0/f9c96fb635cce780ca256d420005dc02/$FILE/Remoteness_Paper_text_final.pdf (Accessed 22 March 2016).
18. Humphreys JS, Wakerman J, Wells R, Kuipers P, Jones, JA, Entwistle P. 'Beyond workforce': a systemic solution for health service provision in small rural and remote communities. Medical Journal of Australia 2008; 188(8 Suppl): S77-S80.
19. Onnis L. Managers are the key to workforce stability: an HRM approach towards improving retention of health professionals in remote northern Australia. In: Proceedings, 28th Australia and New Zealand Academy of Management (ANZAM) Conference, 3-5 December 2014, UTS Sydney. Sydney: University of Technology Sydney, 2014.
20. Onnis L, Dyer G. Maintaining hope: the intrinsic role of professional support. Journal of Mental Health Training, Education and Practice (in press).
21. Rural Health Standing Committee. National Strategic Framework for Rural and Remote Health. (Internet). Available: http://www.ruralhealthaustralia.gov.au/internet/rha/publishing.nsf/Content/EBD8D28B517296A3CA2579FF000350C6/$File/NationalStrategicFramework.pdf (Accessed 26 March 2016).
22. Devine S. Perceptions of occupational therapists practising in rural Australia: a graduate perspective. Australian Occupational Therapy Journal 2006; 53(3): 205-210. http://dx.doi.org/10.1111/j.1440-1630.2006.00561.x.
23. Kent-Wilkinson A, Starr L, Dumanski S, Fleck J, LeFebvre A, Child A. International nursing student exchange: rural and remote clinical experiences in Australia. Journal of Agromedicine 2010; 15(1): 58-65. http://dx.doi.org/10.1080/10599240903389672.
24. Margolis S. Is Fly in/Fly out (FIFO) a viable interim solution to address remote medical workforce shortages? Rural and Remote Health (Internet) 2012; 12(4): 2261. Available: www.rrh.org.au (Accessed 29 October 2015).
25. Hussain R, Maple M, Hunter SV, Mapedzahama V, Reddy P. The Fly-in Fly-out and Drive-in Drive-out model of health care service provision for rural and remote Australia: benefits and disadvantages. Rural and Remote Health (Internet) 2015; 15(3): 3068. Available: www.rrh.org.au (Accessed 29 October 2015).
26. Bent A. Allied health in Central Australia: challenges and rewards in remote area practice. Australian Journal of Physiotherapy 1999; 45(3): 203-212.
27. Santhanam R, Hunter E, Wilkinson Y, Whiteford H, McEwan A. Care, community, capacity: rethinking mental health services in remote Indigenous settings. Australian Journal of Primary Health 2006; 12(2): 51-56.
28. Cutchin MP. Community and self: concepts for rural physician integration and retention. Social Science and Medicine 1997; 44(11): 1661-1674. http://dx.doi.org/10.1016/S0277-9536(96)00275-4.
29. Knights JA, Kennedy BJ. Psychological contract violation: impacts on job satisfaction and organizational commitment among Australian senior public servants. Applied HRM Research 2005; 10(2): 57-72.
30. Ko J, Hur S. the impacts of employee benefits, procedural justice, and managerial trustworthiness on work attitudes: integrated understanding based on social exchange theory. Public Administration Review 2014; 74(2): 176-187. http://dx.doi.org/10.1111/puar.12160.
31. Coyle-Shapiro L, Kessler I. consequences of the psychological contract for the employment relationship: a large scale survey. Journal of Management Studies 2000; 37(7): 903-930. http://dx.doi.org/10.1111/1467-6486.00210.
32. Evans J, Mathur A. The value of online surveys. Internet Research 2005; 15(2): 195-219.
33. Australian Medical Association. Rural health issues survey. 2007.
34. Rural Doctors Association of Australia. Rural, regional and remote medical specialists survey. Final report. (Internet) 2012. Available: http://www.rdaa.com.au (Accessed 29 October 2015).
35. Wright KB. researching internet-based populations: advantages and disadvantages of online survey research, online questionnaire authoring software packages, and web survey services. Journal of Computer-Mediated Communication 2005; 10(3). http://dx.doi.org/10.1111/j.1083-6101.2005.tb00259.x
36. Sax LJ, Gilmartin SK, Bryant AN. Assessing response rates and nonresponse bias in web and paper surveys. Research in Higher Education 2003; 44(4); 409-432.

