full article:
Dental caries (tooth decay) is the most prevalent, controllable health condition in Australia1. Caries can cause mouth pain, infection and tooth loss. It can make everyday activities such as eating, sleeping and speaking difficult2 and impact on self-esteem, psychological wellbeing and overall quality of life3,4. In addition oral diseases have been associated with some cancers, and chronic diseases like coronary heart disease, stroke and diabetes1,5.
In common with the rural gradient of health in general, the oral health of people living in rural communities in Australia is poor. A national survey of oral health highlighted the disparity in oral disease by remoteness, with people living in Australian cities less likely to suffer from dental caries/loss, more frequently able to visit the dentist, and having access to higher rates of employed dentists when compared to people living in remote areas6. A number of factors can contribute to poor oral health for rural communities including access to and availability of adequate oral health services7,8, retention of the oral health workforce in rural areas9 and reduced access to preventative measures such as fluoridated water10. In addition, the social determinants of ill health - poverty, low levels of education, smoking and poor access to nutritious food at reasonable prices - are all more prevalent in rural and remote areas11-13. This, together with the documented stoicism of rural people14, leads to an acceptance of levels of oral ill health that would be unacceptable to urban populations.
The aim of this article is to compare hospital admissions for controllable dental conditions for residents from three rural towns in Queensland with the whole Queensland population, and to consider the impact of dental coverage provided through the public dental service on utilisation of public dental services in these rural communities in Queensland.
Context
The populations under study were three rural communities in Queensland, identified in this manuscript by the pseudonyms Dusty Plains, Sandy Shores and Rolling Green. These communities were part of a wider study examining rural community engagement in oral health planning: the Rural Engaging Communities in Oral Health (Rural ECOH) project.
The communities purposively selected to participate were agricultural towns with populations varying in size from less than 2000 to between 10 000 and 11 000 residents. The rural communities were selected because of a perceived history of poor oral health from the perspective of the project team and oral health providers. Risk factors such as self-reported obesity and smoking rates were higher than the Queensland average. At the time of the study each community had access to a local hospital with an emergency department and a local general practice. Two of the communities had access to a local public dental service and one community had a visiting dental service. Eligibility requirements for the public dental services were aligned with the rest of Queensland: for adults and their dependents to be eligible for publicly funded dental care they must be a Queensland resident and hold a pension concession card, healthcare card, Commonwealth or Queensland seniors' health card. For children to be eligible to receive publicly funded dental services in Queensland they must be a Queensland resident and between 4 years of age and completing Year 10 of secondary school. Dusty Plains differed from the other communities in that the public dental service was available to all residents because there were no other available dental services during the time of the study. A national partnership agreement (funded by the Commonwealth) to reduce dental waiting lists and treat more public dental patients was introduced in 201315. Table 1 summarises demographic factors, access to oral health services and water fluoridation for each community.
Table 1: Population profile and oral health services in study communities
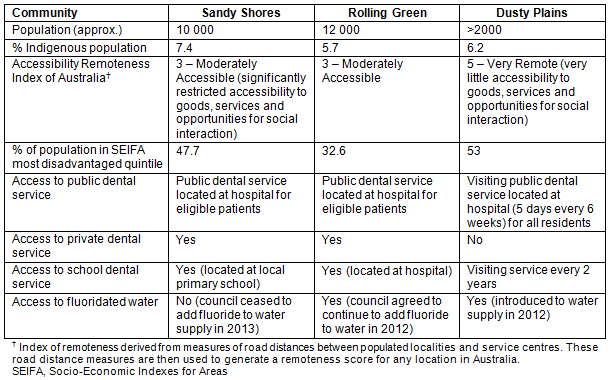
All admitted patient episodes of care in Queensland during calendar year 2013 for dental principal procedures (as defined by International Classification of Disease (ICD10) codes) were collected. Aggregated data for patients with home address postcodes aligning with project communities were included in the study. Due to the small population size of the communities under study, aggregated data were used to minimise the risk of identification, therefore counts for admitted patient episodes of care were combined across all three communities. Public outpatient dental service activity data were also obtained for the selected communities and Queensland for the calendar year 2013 (Medicare Benefits Schedule data from Queensland Public Oral Health 2013). The count of services provided was the unit of measurement and services analysed were Medicare Benefits Schedule category 9: Dental services.
For analysis, data were grouped by gender, age and Indigenous status and comparisons made between Queensland and the project communities. Hospitalisation rates per 1000 were calculated by dividing the number of dental hospitalisations in a selected group by the population of the selected group and multiplying by 1000. Risk ratios with 95% confidence intervals were calculated to examine the risk of hospitalisation for dental procedures for those living in the project communities compared with the rest of Queensland, and χ2 tests were used to assess the statistical significance of this ratio.
The counts of outpatient service data were converted to percentage of all services delivered to allow comparisons between groups of different sizes. Population data were grouped into five age cohorts (0-14 years, 15-4 years, 25-44 years, 45-64 years and ≥65 years) and compared with the proportion of public oral health services delivered to each age cohort. This allowed for an exploration of the representation of particular groups of the population amongst those receiving public oral health services at each site.
Ethics approval
Ethics approval was granted from James Cook University Ethics Committee (H5540), Queensland Health (HREC/13/QTDD/73) and La Trobe University Faculty of Health Sciences Human Ethics Committee, FHEC reference number (13-052).
Hospitalisation data
Table 2 summarises hospitalisation episodes for dental conditions. In Queensland in 2013 a total of 4196 hospitalisations were attributed to dental health conditions. Of these, 2137 (50.9%) were attributed to children aged 0-14 years and 2059 (49.1%) to persons aged 15 years and older. Aggregated data for the project communities showed that in 2013 there were 43 hospitalisations due to dental conditions, with 30 (69.8%) of the episodes involving children 0-14 years and 13 (30.2%) involving persons aged 15 years and older. Hospitalisation rates per 1000 showed differences between the project communities and the whole of Queensland.
Using the calculated risk ratios (Table 3), persons living in the project communities were twice as likely to be hospitalised for a dental condition compared to the average risk for residents of the whole of Queensland. More concerning, children aged 0-14 years living in the communities were three times more likely to be hospitalised for a dental condition compared to the rest of Queensland. There was little difference in the rates for hospitalisation for dental conditions when comparing persons aged 15 years and older in the communities under study and the whole of Queensland.
Overall, compared with the non-Indigenous population of Queensland, Indigenous persons living in Queensland were more than three times as likely to be hospitalised for a dental condition. In the project communities, non-Indigenous persons were almost twice as likely to be hospitalised compared to the non-Indigenous population of the whole of Queensland. Interestingly there were only small differences in hospitalisation rates between the Indigenous population in the project communities and the whole of Queensland.
Table 2: Summary of hospitalisation episodes, rates for dental conditions in Queensland and rural communities under study in 2013
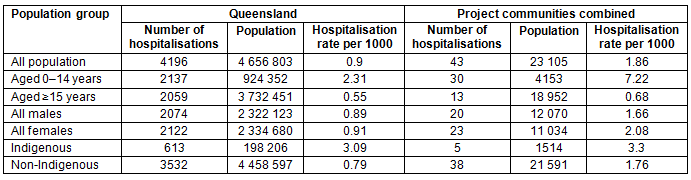
Table 3: Risk of hospitalisation for dental procedures for people living in project communities compared with whole of Queensland
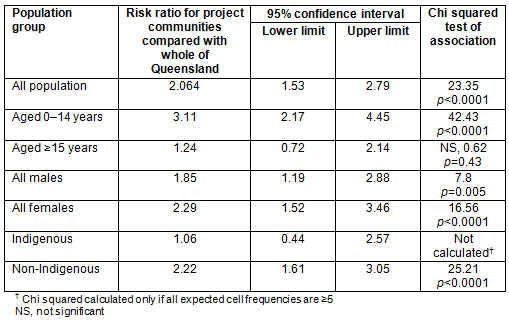
Outpatient service utilisation data
Figures 1-4 show the percentage of public dental services delivered to each age group in the whole of Queensland and project communities. Data for Queensland showed that the majority of services were delivered to children aged up to 14 years of age and adults aged 65 years and older, with gaps in services provided to those of working age. Similar patterns of service distribution were observed for Rolling Green and Sandy Shores. However, in Dusty Plains, where the public dental service was available to all residents, the pattern of distribution of public oral health services at the time of the study was very similar to the distribution of the population.
Examination of services to children for the whole of Queensland showed a large proportion (40%) were delivered to children aged up to 14 years, who represent only 20% of the whole population. The proportions of services delivered to children living in the project communities were less than the whole of Queensland; in Rolling Green 31% of services were delivered to children aged up to 14 years and in Sandy Shores 26% of services were delivered. Public oral health service utilisation data for children aged up to 14 years living in Dusty Plains showed 16% of all public health services were delivered to this population group.
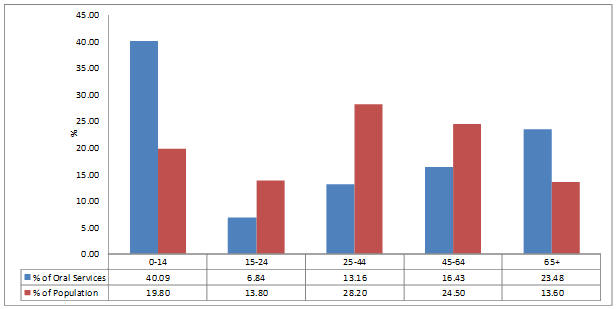
Figure 1: Percentage of public outpatient dental services by age group in Queensland.
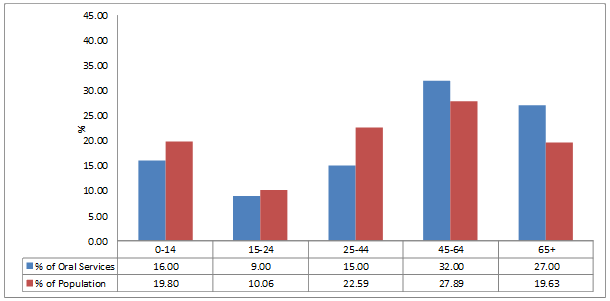
Figure 2: Percentage of public outpatient dental services by age group in Dusty Plains.
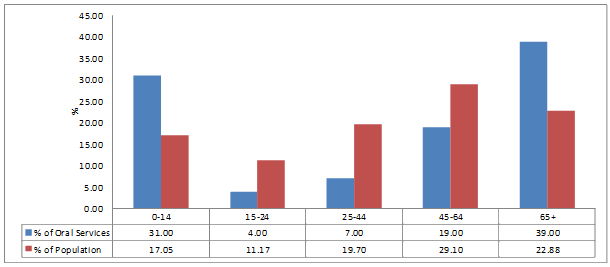
Figure 3: Percentage of public outpatient dental services by age group in Rolling Green.
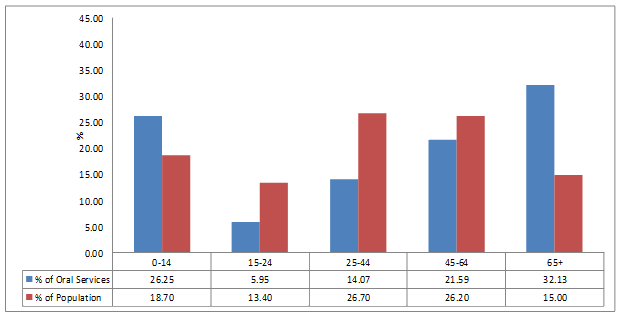
Figure 4: Percentage of public outpatient dental services by age group in Sandy Shores.
Discussion
This article aimed to explore hospital admissions for controllable dental conditions and utilisation of public oral health services in three rural towns in Queensland compared to that of the overall Queensland population. Analysis of hospitalisation data highlighted the increased risk of hospitalisation for dental conditions for people living in rural areas, specifically children aged up to 14 years and Indigenous people.
Eligibility requirements of Queensland public dental services dictate that a large proportion of services would be delivered to children under 14 years and adults older than 65 years. However, data on utilisation of public dental services in the communities under study compared with the whole of Queensland showed that children aged up to 14 years may not be accessing public oral health services proportional to need. In the case of one rural community, after the cost and eligibility barrier was removed the provision of oral health services more closely matched the population distribution, thus changing the profile of oral services provided in the town.
Studies have shown that parents/caregivers play a crucial role in influencing children's oral health16,17. Parental oral health status, knowledge and behaviours18,19, in addition to structural barriers such as cost, eligibility and ability to attend appointments20, can impact on oral health status and dental visiting patterns. Indigenous Australians are more likely to live in rural and remote areas21, have poorer oral health and are less likely to receive treatment to address or prevent poor oral health compared with non-Indigenous Australians22,23. The present analysis of hospitalisation data clearly shows that the disparity in oral health of Indigenous and non-Indigenous Australians living in Queensland persists and that further preventive and oral health promotion interventions targeting Indigenous populations in Queensland are required. Limitations of the study include the limited sample size and small populations of the communities selected, therefore broader conclusions are not possible. In addition the authors acknowledge that public dental services account for a small proportion of dental services in Australia, with the largest source of dental expenditure borne by individuals through the private system1. However, the results allow some commentary about oral health admissions and oral health services within rural communities and their impact in areas where private dental practice is non-viable and public services are often the only oral health services available.
The findings of this study are consistent with published research1,24-26 and provide evidence that some rural communities and at-risk groups (ie Indigenous Australians and children) continue to experience poor oral health. To reduce the disparities in oral health outcomes between people living in urban areas and rural communities, planning of oral health services must be mindful of the rural context. It has been well documented that there is a limited oral health workforce in rural areas, requiring creative solutions and partnerships across oral health, health and allied health professionals. One solution is the integration of oral health into general health interventions within primary care; health professionals who regularly engage with families and children have an important role in providing preventive oral health care and encouraging good oral health behaviours, such as regular dental visits. This sentiment is echoed in the 2015-2024 national oral health plan2, which states that the 'broader health workforce can play an important role in oral health promotion, dietary advice and simple non-invasive disease prevention ... [as they] will have more contact with the consumer'. The data also provide further evidence for a flexible approach to funding oral health services via private/public/non-government organisation partnerships for at-risk communities, particularly those who have difficulties in access to oral health services, so they are able to avail themselves of basic oral health services to avoid more costly treatment or hospitalisation.
Preventable hospitalisation rates for dental conditions and distribution of public oral health services provide some insight into the adequacy of oral health services within rural communities and the disproportionate burden of poor oral health amongst rural Australians. Furthermore, the findings highlight the vital importance of a collaborative approach to planning and service delivery to improve oral health for rural communities. Further work is required to design, implement and evaluate oral health promotion and health service interventions to address these disparities in oral health status and care provision, with a particular focus on children and Indigenous Australians.
References
1. Australian Institute of Health and Welfare. Oral health and dental care in Australia: key facts and figures trends. Canberra, ACT: Australian Institute of Health and Welfare, 2014.
2. Oral Health Monitoring Group. Healthy mouths healthy lives: Australia's national oral health plan 2015-2024. (Internet) 2015 Available: http://www.coaghealthcouncil.gov.au/Portals/0/Australia%27s%20National%20Oral%20Health%20Plan%202015-2024_uploaded%20170216.pdf (Accessed 13 September 2016).
3. Gerritsen AE, Allen PF, Witter DJ, Bronkhorst EM, Creugers NHJ. Tooth loss and oral health-related quality of life: a systematic review and meta-analysis. Health Quality Life Outcomes 2010; 8: 126.
4. Kramer PF, Feldens CA, Ferreira SH, Bervian J, Rodrigues PH, Peres MA. Exploring the impact of oral diseases and disorders on quality of life of preschool children. Community Dentistry and Oral Epidemiology 2013; 41(4): 327-335. https://doi.org/10.1111/cdoe.12035
5. Victoria Dental Health Services. Links between oral health and general health: the case for action. Carlton, Vic.: Dental Health Services Victoria, 2011.
6. Australian Institute of Health and Welfare, Hardford J, Islam S. Adult oral health and dental visiting in Australia: results from the National Dental Telephone Interview Survey 2010. Dental Statistics and Research Series no. 65. Cat. no. 227. Canberra, ACT: Australian Institute of Health and Welfare, 2013.
7. Steele L, Pacza T, Tennant M. Rural and remote oral health, problems and models for improvement: a Western Australian perspective. Australian Journal of Rural Health 2000; 8(1): 22-28. https://doi.org/10.1046/j.1440-1584.2000.81224.x
8. Tennant M, Kruger E. Turning Australia into a 'flat-land': what are the implications for workforce supply of addressing the disparity in rural-city dentist distribution? International Dental Journal 2014; 64(1): 29-33. https://doi.org/10.1111/idj.12059
9. Godwin DM, Hoang H, Crocombe LA, Bell E. Dental practitioner rural work movements: a systematic review. Rural and Remote Health (Internet) 2014; 14(3): 2825. Available: www.rrh.org.au (Accessed 13 September 2016).
10. Ehsani JP, Bailie R. Feasibility and costs of water fluoridation in remote Australian Aboriginal communities. BMC Public Health (Internet) 2007; 7: 100. Available: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1906759/ (Accessed 13 September 2016).
11. Dixon J, Welch N. Researching the rural-metropolitan health differential using the 'social determinants of health'. Australian Journal of Rural Health 2000; 8(5): 254-260.
12. Australian Institute of Health and Welfare. Rural, regional and remote health status and determinants of health. Canberra, ACT: Australian Institute of Health and Welfare, 2008.
13. Marmot M, Bell R. Social determinants and dental health. Advances in Dental Research 2011; 23(2): 201-206. https://doi.org/10.1177/0022034511402079
14. Chater AB. Looking after health care in the bush. Australian Health Review 2008; 32(2): 313-318. https://doi.org/10.1071/AH080313
15. Council of Australian Governments. National partnership agreement on adult public dental services. (Internet) 2016. Available: http://www.federalfinancialrelations.gov.au/content/npa/health/national-partnership/Adult_Public_Dental_Services_NP.pdf (Accessed 13 September 2016).
16. Arrow P, Raheb J, Miller M. Brief oral health promotion intervention among parents of young children to reduce early childhood dental decay. BMC Public Health 2013; 13: 245. Available: http://bmcpublichealth.biomedcentral.com/articles/10.1186/1471-2458-13-245 (Accessed 13 September 2016). https://doi.org/10.1186/1471-2458-13-245
17. Duijster D, de Jong-Lenters M, Verrips E, van Loveren C. Establishing oral health promoting behaviours in children - parents' views on barriers, facilitators and professional support: a qualitative study. BMC Oral Health (Internet) 2015; 5: 157. Available: http://bmcoralhealth.biomedcentral.com/articles/10.1186/s12903-015-0145-0 (Accessed 13 September 2016).
18. Virgo-Milton M, Boak R, Hoare A, Gold L, Waters E, Gussy M, et al. An exploration of the views of Australian mothers on promoting child oral health. Australian Dental Journal (Internet) 2016; 61: 84-92. Available: http://onlinelibrary.wiley.com/doi/10.1111/adj.12332/full (Accessed 13 September 2016).
19. Hooley M, Skouteris H, Boganin C, Satur J, Kilpatrick N. Parental influence and the development of dental caries in children aged 0-6 years: a systematic review of the literature. Journal of Dentistry 2012; 40: 873-885. https://doi.org/10.1016/j.jdent.2012.07.013
20. Kelly SE, Binkley CJ, Neace WP, Gale BS. Barriers to care-seeking for children's oral health among low-income care-givers. American Journal of Public Health 2005; 95: 1345-1351. https://doi.org/10.2105/AJPH.2004.045286
21. Australian Bureau of Statistics. Estimates of Aboriginal and Torres Strait Islander Australians, June 2011. (Internet) 2011. Available: http://www.abs.gov.au/ausstats/abs@.nsf/mf/3238.0.55.001 (Accessed 13 September 2016).
22. Slade G, Spencer A, Roberts-Thomson K. Australia's dental generations - The National Survey of Adult Oral Health 2004-6. Dental Statistics and Research Series 34. Cat. no. DEN165. Canberra, ACT: Australian Institute of Health and Welfare, 2007.
23. Brennan DS, Roberts-Thomson KF, Spencer AJ. Oral health of Indigenous adult public dental patients in Australia. Australian Dental Journal 2007; 52(4): 322-328. https://doi.org/10.1111/j.1834-7819.2007.tb00509.x
24. Crocombe L, Stewart J, Brennan D, Slade G, Spencer A. Is poor access to dental care why people outside capital cities have poor oral health? Australian Dental Journal 2012; 57: 477-485. https://doi.org/10.1111/adj.12000
25. Smith K, Kruger E, Dyson K, Tennant M. Oral health in rural and remote Western Australian Indigenous communities: a two-year retrospective analysis of 999 people. International Dental Journal 2007; 57: 93-99. https://doi.org/10.1111/j.1875-595X.2007.tb00444.x
26. Caffery L, Bradford N, Meurer M, Smith A. Association between patient age, geographical location, Indigenous status and hospitalisation for oral and dental conditions in Queensland, Australia. Australian Journal of Primary Health (Internet) 2016. Available: http://www.publish.csiro.au/paper/PY15105.htm (Accessed 13 September 2016).


