Unintentional injuries (injuries for which there is no evidence of a predetermined intent) are one of the leading causes of death worldwide1. WHO estimates unintentional injuries account for more than 3.9 million deaths globally, and over 90% of these deaths are occurring in low- and middle-income countries (LMICs)1. Road traffic crashes (RTCs) and falls are the leading causes of unintentional injuries where RTCs account for 24% of all fatal injuries and falls account for 14%1. Other unintentional injuries include fire-related burns, poisonings and drowning1. Deaths and non-fatal consequences of injuries such as temporary or permanent disabilities, chronic pain and socioeconomic loss can have lasting impacts on the person, families and the communities being affected by the injury1,2. It was predicted the disability-adjusted life-years (DALYs) lost from unintentional injuries was over 94% of the total global DALYs in LMIC2.
Evidence shows that unintentional injuries are preventable as demonstrated by decreased mortality rates from RTC in high-income countries (HICs) such as Australia and some LMICs3-5. Yet unintentional injury prevention is a public health challenge for many LMIC around the world5-7.
Injury prevention is a multi-faceted process: a continuum of factors is associated with the occurrence of an injury5. These factors can be described in terms of the host (the person injured), agent (the force or energy), vector (the mechanism that applies the force) and the environment (both physical and social conditions under which the injury happens)5. Thus when developing injury prevention interventions all these factors should be considered. Interventions could be directed at (1) preventing the occurrence of injury (primary prevention), (2) minimising the severity of injury at the time of injury (secondary prevention) and (3) minimising the severity of injury after the injury has occurred (tertiary prevention)5,8. Primary prevention actions are focused on eliminating the injury from occurring (eg fencing around pools to prevent drowning)9. Secondary prevention focuses on minimising the amount of energy transferred to an individual such as the use of seat belts and air bags to prevent road traffic crashes7. Tertiary prevention aims to manage the impacts of injury on the person after injury occurrence, and this is where the majority of the health sector is involved7.
Injury prevention requires a multisectorial input10. This could include the government, health and private sector. WHO has highlighted this in the guidelines for policy-makers and planners for injury and violence prevention10. However, a multi-sectorial approach can be challenging for many LMIC where economies are usually reliant on foreign aid, there is a vast populace with low socio-economic status', political instability can be a normality, and where health systems are overburdened2,11. Therefore, policy-makers (within the government and health sector) generally direct efforts towards more immediate and observable issues such as managing communicable diseases2. LMIC often have poor data recording systems, distorting the magnitude of the impacts of injury6. Therefore, injury prevention is often overlooked or not a priority in health policy planning2,11. This was one of the issues for the Solomon Islands.
Situating Solomon Islands
Solomon Islands is an archipelago LMIC, located in the Southwest Pacific region, with a population of approximately 561 23112. It consists of more than 900 islands scattered over a total ocean area of 1.3 million km2 (exclusive economic zone)13. Less than 20% of the population lives in urban areas with a large population density distributed in the remote outer islands14. The capital, Honiara, is on the main island (Guadalcanal) and is home to approximately 66 000 people14. Almost all economic growth, services and employment opportunities are concentrated in the capital, Honiara14. Therefore, in terms of social and economic indicators, those living out in the rural areas/islands are more disadvantaged than their urban counterparts14.
Solomon Islands is in the peace-making process after ethnic tensions that occurred in 1998 and then in 200514. Consequently, infrastructure development is stagnant, with most of the country's finances sourced from foreign aid, accounting for over 60% of the gross domestic product in 2006-201114. The economy is subsistence and cash crop agriculture, with less than 25% of the working population involved in paid work14. The majority of those living in the rural areas depend on subsistence farming14.
Health care in the Solomon Islands is free and is regulated by the Ministry of Health and Medical Services (MHMS)14. There is a critical shortage of health personnel in the country with 1.9 health workers (doctors, nurses and midwifes) for every 1000 people14. This is below the minimum standard of 2.3 recommended by WHO14. Equal access to health care remains a challenge for the MHMS due to factors including the archipelago nature of the country and the high rural and remote population density15,16. Thus service delivery to these rural areas is costly and resource intensive to the health system16.
WHO predicted unintentional injuries to account for 5.3% DALYs loss in 2008 and they were identified as the third leading burden of disease in the National Health Strategic Plan 2011-201515,17. However, unintentional injury prevention appeared to be overlooked as a health priority15. Health priorities were focused on prevention and management of communicable and non-communicable diseases15. This is not uncommon for LMICs where health systems are already burdened with communicable and non-communicable diseases; thus, it becomes challenging to consider other issues such as injury6. Lack of adequate injury reporting systems is also a barrier to some of the MHMS health action plans15.
Occupational therapy role in injury prevention
While many professions are involved in injury prevention, occupational therapy is particularly well placed. Occupational therapy is a client-centred profession that is concerned with promoting health and wellbeing through occupations18. Occupations are defined as the everyday activities and tasks that people participate in that give purpose and meaning to their lives18. Occupations can range from a task as simple as preparing a meal (self-care) to participating in paid employment (work) and to being able to enjoy a hobby such as fishing (leisure)18. In injury prevention, occupational therapists are specifically trained to critically analyse the activities of work, leisure and self-care that people are participating in, identify the potential risks and protective factors and then design strategies to reduce the risk of potential injury, in particular in environments such as the home, work or community19.
The majority of the studies that have explored and discussed the occupational therapist roles in unintentional injury prevention have been undertaken in HICs. Here, occupational therapists provided injury prevention interventions such as falls prevention education and environmental modifications in the community/home for the older population20,21, preventing road crash injuries among the older population22,23, prevention of work-related injuries24 and prevention of scarring after burn injuries25.
In LMIC the limited occupational therapy literature focused on a tertiary preventative role in the prevention of unintentional injuries such as in disaster management26,27, spinal cord injury management28,29 and hand injury management30. Although there was a general consensus that awareness of the occupational therapy role in injury prevention within LMICs is limited, it was identified that occupational therapists played a critical role in preventing and minimising the long-term physical and psycho-emotional impacts of the disabilities from injury28-30.
In the Solomon Islands, there was limited information regarding occupational therapy services in the country. One study described a placement experience of two occupational therapy students from New Zealand31. This study highlighted the absence of occupational therapists within the allied health team at the hospital31. Likewise, a 2014 health profile report conducted for the country highlighted the absence of occupational therapy services14. This was confirmed by E. Taloafiri (physiotherapist, head of the rehabilitation unit at the National Referral Hospital (NRH)) where the first and only paid occupational therapists in the Solomon Islands left the country to practice in New Zealand (pers. comm., October 2015).
The allied health team at the NRH, which consists of physiotherapists, social workers and community-based rehabilitation workers, provides the required rehabilitative services for the Solomon Islands14. Various organisations such as the Australian Volunteers International and Japanese International Cooperation Agency often employ volunteer occupational therapists in the Solomon Islands; however, this is only on a short-term basis32,33. Occupational therapy services appear to be limited in the Solomon Islands.
Since there is limited information regarding occupational therapy services in the Solomon Islands, this literature review will explore the different roles that occupational therapists are undertaking in unintentional injury prevention in other LMICs to determine the potential of utilising these roles in the Solomon Islands. Likewise, it will explore the types of unintentional injury in the Solomon Islands.
Research objectives
To the authors' current knowledge this is the first integrative review to be conducted for the Solomon Islands regarding injury and the role of occupational therapy in unintentional injury prevention. This integrative review will therefore aim to answer two research objectives:
- to explore and describe the current understanding of the incidence, common types and the burden of unintentional injuries in the Solomon Islands
- to explore the potential role of occupational therapy in unintentional injury prevention in the Solomon Islands based on current occupational therapy activities in other LMICs.
Design
An integrative literature review approach was undertaken to address the two research objectives. Integrative literature reviews allow for the inclusion of diverse methodologies (experimental and non-experimental research)34, an in-depth exploration of this new area of study35, and is proven to be relevant to evidence-based practice34,35.
Search strategy and selection criteria
This integrative review was undertaken with two aims: (1) to explore the incidence, common types and the burden of unintentional injury in the Solomon Islands ('injury') and (2) to explore the role of occupational therapy in unintentional injury prevention in LMICs ('occupational therapy role'). Six databases (Medline, CINAHL, Scopus, PsychInfo, OTDBase and OTSeeker) were searched between 10 and 27 July 2015. A combination of keyword searching, synonyms and subject heading search strategies were used, depending on database functionality (Appendix I). The PRISMA guideline (http:// http://www.prisma-statement.org) was used to provide a systematic approach to this integrative review. Figures 1 and 2 provide a summary for each search process36.
The following inclusion and exclusion criteria were used:
- Articles published in English were included.
- All years (no time limit was applied to all articles) were included.
- Articles specifically discussing/outlined unintentional injuries or an unintentional injury classification (road traffic injuries, falls, burns, drowning, poisoning)1 were included.
- Articles discussing intentional injuries (those that result from purposeful intent and can be self-inflicted and/or interpersonal7) were excluded.
- For the 'injury' section:
- Articles were only included if the injuries were sustained by people in the Solomon Islands.
- For the 'occupational therapy role' section:
- Articles that clearly and specifically identified the involvement of occupational therapists or occupational therapy were included.
- Articles that explored general rehabilitation roles and community-based rehabilitation roles and did not have reference to occupational therapy were excluded.
- Articles for which the study was undertaken in the Solomon Islands or an LMIC were included. (The list of LMICs was taken from the World Bank LMIC listing37.)
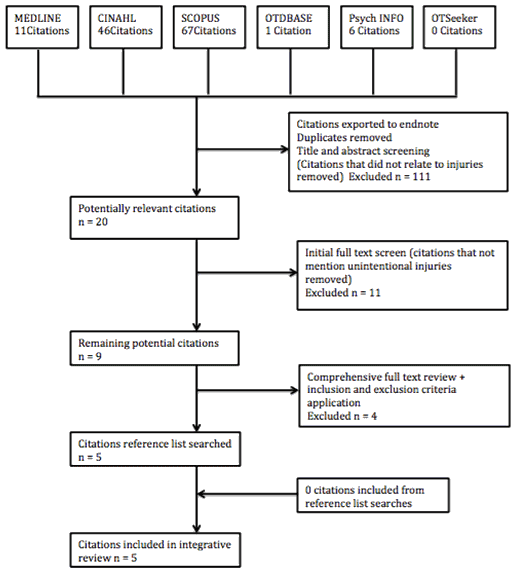 Figure 1: PRISMA flow for 'injury' section of systematic review.
Figure 1: PRISMA flow for 'injury' section of systematic review.
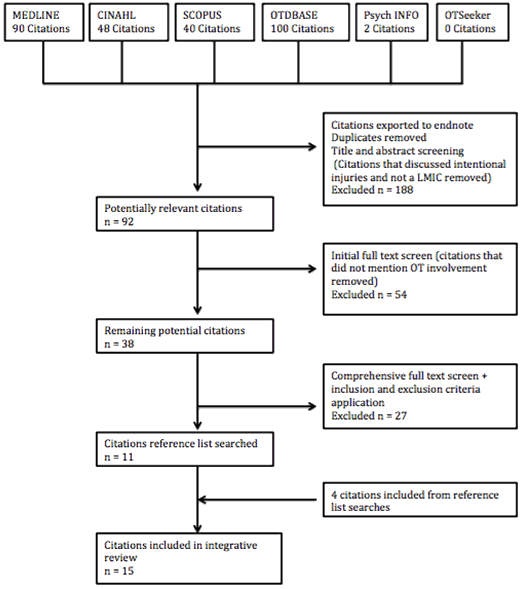 Figure 2: PRISMA flow for 'occupational therapy role' section of systematic review.
Figure 2: PRISMA flow for 'occupational therapy role' section of systematic review.
Data analysis
Analysis was conducted independently for each research objective; however, the same procedure, the principles of the thematic analysis process outlined by Braun and Clarke, was applied38. This process entails an initial reading of the articles, initial category generation, initial code development, category/code reviewing, naming and defining categories/codes and producing the report38.
Initially, studies were read and summarised into tables with the following categories: study design, location of study, injury type and summary of study findings. A process of data reduction was conducted where the summarised data in the initial categories were organised into more specific categories35. For the 'injury' section, categories included crude incidence rate, sustained injuries and body locations, injury location and burden of injury (Table 2). For the 'occupational therapy role' section, categories included injury type and body location, practice setting, occupational therapy role, team and injury prevention stage (Table 3).
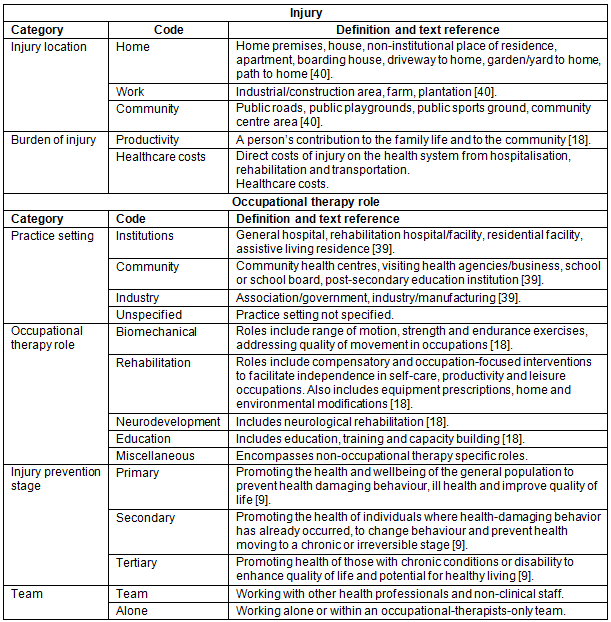
The data within these categories were analysed where commonalities within the data were identified and organised into groups, which were then coded38. Codes were initially defined by the data itself and were refined where possible on existing coding from occupational therapy literature18,39, the International Classification of Diseases injury coding from the Research Center for Injury Studies at Flinders University in South Australia40, and primary healthcare literature8. The code definitions are presented in Table 1. These were then reviewed by the co-authors for consistency, relevance and content validity34. Outlier categories and codes were reviewed and eliminated, adapted or included where appropriate. Tables 2 and 3 display the outcomes of the analysis process.
For the injury section, a crude measure of incidence was calculated to identify injury incidence per annum per 100 000 people in the Solomon Islands. The data used in the analysis were extrapolated from the retrieved articles and the incidence rate was calculated using the following calculation:
Incidence rate = (number of injury cases/population during that period)/(Yx100 000).
where Y = number of years for which the data was collected and used if individual year population not available.
Population figures were derived from the World Bank website for the time period in which the injury counts were identified in the retrieved articles12.
A decision was made to not critically appraise the articles included in this review. The majority of the studies in this review ranked lower in the National Health and Medical Research Council evidence hierarchy due to the dearth of literature in this particular area of study41. The focus of this review was not on the quality of the studies, but on providing a preliminary description of literature that explores unintentional injury and the role of occupational therapy in unintentional injury prevention in LMICs. In light of this, data interpretations are conducted with caution, understanding that these studies are of low-level evidence on the spectrum of critically appraised studies41.
Table 1: Classification of injury and occupational therapy role with codes and definitions
Injury
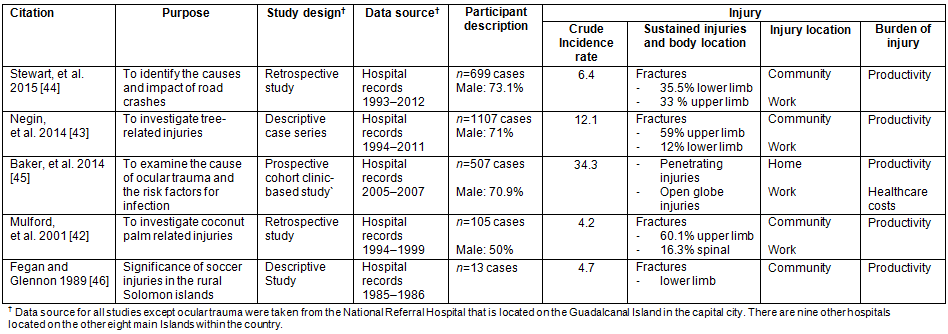
Five articles met the inclusion criteria for information regarding unintentional injury in the Solomon Islands. Study designs included two retrospective studies, two descriptive case series and a prospective cohort clinic-based study. Two studies explored injuries from falls from fruit trees or coconut palms42,43. The remaining three articles explored road traffic crashes44, ocular trauma45 and soccer-related injuries46. Injury incidence per annum per 100 000 population was calculated to be 34.3 for ocular trauma, 12.1 for falls from fruit trees, 6.4 for road traffic crashes, 4.7 for soccer-related injuries and 4.2 for coconut palm-related injuries (Table 2). Common injuries sustained and body locations included fracture of both upper and lower limbs, spinal cord injury and penetrative injuries to the eye (Table 2). The most common places that injuries occurred were in the community and at home (Table 2). Productivity was a common injury burden identified by all five studies, and four of the five studies identified that males sustained most injuries. Only one article discussed the potential healthcare costs associated with injury45.
Table 2: Published studies exploring injury in the Solomon Islands
Occupational therapy in LMIC
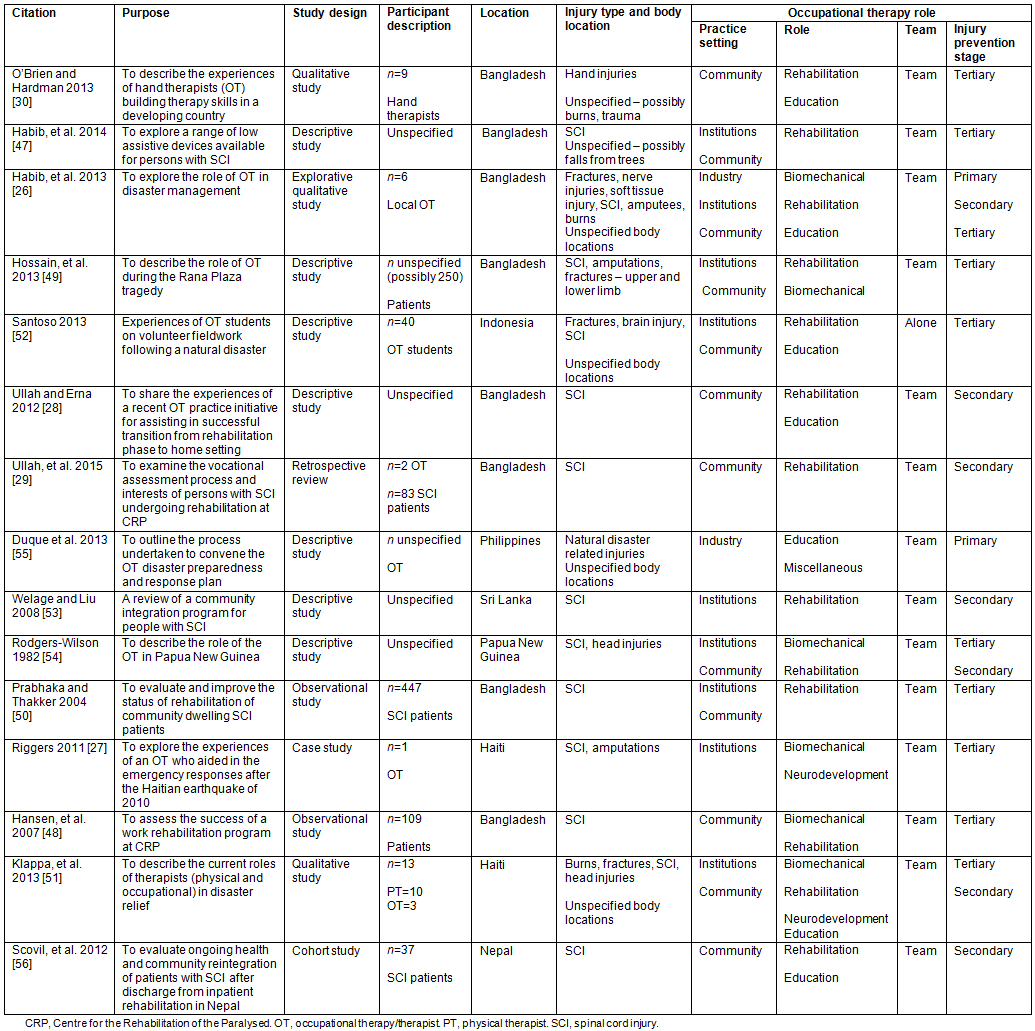
Fifteen articles met the inclusion criteria for this section. There were seven descriptive studies, two qualitative studies, two observational studies and one retrospective review, explorative study, cohort study and case study designs. Eight of these studies were conducted in Bangladesh26,28-30,47-50, two in Haiti27,51 and one each in Indonesia52, Sri Lanka53, Papua New Guinea54, the Philippines55 and Nepal56 (Table 3). Common mechanisms of injury identified in these studies were natural disasters (earthquakes), accidents (road crashes and falling buildings), falls from trees and burns. Common sustained injuries included spinal cord injury, fractures, head injuries, amputations and burn injuries.
Occupational therapists were predominantly practising in the community and institutional (hospital) setting; only one study explored the role of occupational therapy in a government (industry) setting26. Occupational therapy scope of practice was more focused on rehabilitative and biomechanical roles and the occupational therapists were mostly working in a team (explored by all studies but one). Members of the team included a team of occupational therapists or a team with other health professionals including doctors, nurses, physiotherapists, spiritual counsellors, social workers and prosthetists/orthotists. According to this review, occupational therapists were predominantly involved in the tertiary and secondary stage of injury prevention and had very limited contribution in the primary phase of injury prevention (Table 3).
Table 3: Published studies exploring occupational therapy role in low- and middle-income countries
Discussion
There is a dearth of information on injury, its prevention and the role of occupational therapy in injury prevention in the Solomon Islands and LMIC. This review provides a glimpse into the types of unintentional injuries that are occurring in the Solomon Islands and the potential occupational therapy roles in injury prevention that can be translated into the Solomon Islands context from the current activities in LMICs.
Injury in the Solomon Islands
Ocular trauma was identified as the highest occurring injury compared to road traffic crashes and falls from fruit trees in the Solomon Islands (Table 2). It should be noted that the ocular trauma study was the only study to utilise data from more than one hospital. Data from provincial hospitals on the outer islands were used with those from the NRH45. Hence the incidence rates encompassed more presentations and admissions compared to the studies for road traffic crashes and falls from fruit trees, which only used data from the NRH. Thus the crude incidence rates for road traffic crashes and falls does not represent the actual rate for the Solomon Islands, as injuries could be occurring on other islands and not recorded or referred to the NRH. Reports published by WHO have indicated that the rates of road traffic crashes are predicted to rise in the Solomon Islands, due to the current increase in urbanisation14,57. However, most of the figures that WHO utilised were derived from statistical predictions rather than from actual injury data from the Solomon Islands57. This is a depiction of how inadequate information/data can potentially distort the interpretations of the impacts of injury on a population.
Common injuries that people sustained included fractures and spinal cord injury, and these injuries predominantly occurred at home, within the community and to a lesser extent in the workplace (Table 2). Less than 25% of the Solomon Islands population are involved in paid work and the rest are subsistence farmers, thus the prevalence of injury occurrence in home and the community14. Although this information is limited, it provides a glimpse into the types of injury people sustain and where they occur, allowing health professionals, such as occupational therapists, to target injury prevention actions effectively. For example, knowing that children sustain most of the injuries from ocular trauma in the home and within the community45, occupational therapists can target injury prevention strategies to families.
The main burden of injury was the loss of productivity. Injuries were predominantly sustained by the male population within their economically productive ages of 15-44 years42-45. For the purposes of this review, economic productivity was defined within the scope of subsistence farming: to provide food for the family/community and for market produce14. In the Solomon Islands, males are most often the income earners for a family58. However, due to the wantok system, an unwritten social contract that binds extended families via a set of mutual obligations and reciprocal support, a male is often the only provider for a large extended family58. If this person is injured and is unable to work, the entire extended family may become economically vulnerable58. A loss in such productivity means a lack of participation in meaningful occupations, resulting in occupational disruption to the injured person and the family18.
Although healthcare cost was identified as a burden, the study that highlighted this burden acknowledged that there was limited information available to quantify this burden45. The issue of late presentation to hospitals resulting in complications that required expensive and intensive hospitalisation was discussed in relation to the burden of healthcare costs45. Factors including reliance on traditional medicine, lack of healthcare education, geographical isolation and cost of travel contributes to late presentations in the Solomon Islands14,16,45. Likewise, these can impact on health service delivery to the outer rural and remote islands16. This highlights the importance of injury prevention in the rural and remote areas in the Solomon Islands, where access to healthcare facilities are limited.
Role of occupational therapy in injury prevention
The few studies identified provide an overview of the range of roles that occupational therapists are undertaking in LMICs. Almost all the studies described the occupational therapist's role in injury prevention at the tertiary prevention stage. Occupational therapists were predominantly focused on enhancing quality of life after injury to ensure that people have as much independence as possible within their daily lives26-30,47-56. These roles encompass remediation (range of motion exercises, upper limb exercises, splinting), compensatory actions (assistive equipment prescription, home modifications) and return-to-work programs (vocational trainings)26-30,47-56. Occupational therapists also undertook educational roles including capacity-building training26,27,30,52. Although there were some differences in the mechanisms/causes of injury between the LMICs and Solomon Islands, the resulting sustained injuries were similar (fractures and spinal cord injuries). Thus the identified occupational therapy roles in these LMICs have the potential to be applied in the Solomon Islands.
Occupational therapists primarily worked as part of a team. The importance and benefits of working as part of a multidisciplinary or an interdisciplinary team to both the health professionals and patients were highlighted by many studies in HICs and LMICs59,60. These studies emphasised that team care approaches can lead to a better quality of care to the patients and often result in more patient satisfaction in regards to rehabilitation59,60. Therapists working in rural and remote settings or in under-resourced contexts often are the sole practitioners in their specialised fields, thus are recommended to collaborate with other health professionals61. It is recommended that occupational therapists practising in the Solomon Islands work in collaboration with the rehabilitation and medical teams at the hospital in order to provide effective injury prevention measures.
Within this review occupational therapists were predominantly providing interventions at the secondary and tertiary phases of prevention. Only two studies discussed an occupational therapy role in the primary prevention stage26,55. Bourke-Taylor and Hudson discussed that, despite the current push towards prevention in LMICs, occupational therapists working in these settings find themselves practising within the secondary and tertiary stages of prevention, undertaking the traditional rehabilitation roles62. Occupational therapists can be seen to have a narrow scope of practice in rural and remote settings where there is lack of awareness of the occupational therapy role among other health professionals and clients30,60. This limits occupational therapist roles to 'hand therapists' or 'rehabilitation of physical function [therapists]'30,63. As stated, occupational therapists practising in rural and remote settings are often the only therapists61. Consequently, they are faced with challenges including undertaking diverse duties, and managing complex and large caseloads, and they often have little or no time for prevention and can only focus on providing immediate health care61,64,65. Yet it is recommended that occupational therapists setting up in LMICs should initiate participation in primary prevention where possible62.
This literature review did not find information on training, recruitment and retention of occupational therapists in injury prevention in LMICs. However, training, recruitment and retention of occupational therapists in LMICs with rural and remote settings has been identified as a challenge by some studies65,66. Common barriers to service provision experienced by occupational therapists practising in rural and remote areas include geographical location, transport costs, travel times, limited health professionals, lack of professional supports and opportunities for professional growth65,66. This is also likely to be true in the Solomon Islands where large population densities are distributed among the remote outer islands.
Economic incentives are one of the largest contributors to attrition of skilled staff such as occupational therapists from LMICs to HICs30. In the Solomon Islands the lack of professional support such as the presence of an occupational therapy association or an advocate group and low economic incentives could be the barrier to retention of occupational therapists14,65. Thus strategies such as financial incentives, provision of professional supports and opportunities for professional growth should be considered when establishing occupational therapy services in the Solomon Islands to maintain continuous training, recruitment and retention.
Recommendations for future studies
Despite limited literature it could be argued that occupational therapists have the potential to play a significant role in injury prevention within LMICs as prevention is an important part of their training19. Thus it is recommended that steps be undertaken to establish occupational therapy in the Solomon Islands. Krefting outlined four strategies that could aid the development of occupational therapy services in LMICs: (1) documenting the extent of disability (injury), (2) development of a comprehensive rehabilitation plan, (3) prioritising needs and (4) developing educational models67. The principles within these strategies were utilised by occupational therapists setting up services in Bangladesh and the Dominican Republic and were shown to be a success30,62.
Utilising these studies as examples, future studies can explore how occupational therapists can apply these strategies to assist in the establishment of occupational therapy in the Solomon Islands. However, there is also a need to understand the country's economic, social and political context and the rural and remote nature of the Solomon Islands when considering developing occupational therapy services62,63.
Due to limited data regarding unintentional injuries in the Solomon Islands, it is recommended that an in-depth study of injuries in the Solomon Islands be undertaken. Likewise, future studies should consider an audit of the current reporting system in order to provide a better understanding of the burden of injuries in the Solomon Islands.
Limitations
While this present review focuses on unintentional injuries, it is acknowledged that a number of studies relating to intentional injuries such as domestic violence in the Solomon Islands were excluded. Intentional injuries could be explored in future research when a comprehensive injury reporting system has been established, as this will provide a more complete representation of the burden of injury in the Solomon Islands.
The potential of not finding all relevant articles relating to this research is a limitation. An attempt has been made to ensure that all LMICs were included within the search terms/strategies by incorporating all the LMICs listed by the World Bank; however, there is still the likelihood of potentially overlooking some countries due to the broad nature of LMICs.
This review only included peer-reviewed articles. An initial search of government websites such as WHO and the Solomon Islands statistical website presented reports with either incomplete injury-related data or the reports were unsuitable for analysis in this review. A systematic research of reports published by government websites such as WHO, United Nations and World Bank could potentially provide more information regarding the incidence of unintentional injury in the Solomon Islands.
This review focused on the role of occupational therapists and used LMIC data to explore this role in more detail. The authors were unable to find any articles that describe who is providing current unintentional injury prevention services in the Solomon Islands and acknowledge that occupational therapists are only one group who are trained to provide this service.
This is the first time to the authors' knowledge that an attempt has been made to explore unintentional injuries and the occupational therapy role in unintentional injury prevention for the Solomon Islands. This review identified ocular trauma, road traffic crashes and falls from fruit trees as injuries in the Solomon Islands; however, it is likely that this is an underrepresentation of the types of injury occurring. Occupational therapists were identified as having the potential to significantly contribute towards injury prevention, particularly in facilitating independence and quality of life after injury (tertiary prevention). Only a few studies highlighted occupational therapists' involvement in primary prevention of injury, although occupational therapists were encouraged to increase their participation in primary prevention interventions.
There was limited literature regarding occupational therapy in the Solomon Islands, therefore it is recommended that future studies should consider the potential of initiating the establishment of occupational therapy in the Solomon Islands. Likewise, recommendations are made for future research to consider an audit of the current injury reporting system and an in-depth exploration of all injuries in the Solomon Islands to assist in the development of effective injury prevention interventions.
References
1. World Health Organization. Injury and violence: the facts. (Internet) 2014. Available: http://apps.who.int/iris/bitstream/10665/149798/1/9789241508018_eng.pdf?ua=1&ua=1 (Accessed 1 November 2015).
2. Chandran A, Hyder AA, Peek-Asa C. The global burden of unintentional injuries and an agenda for progress. Epidemiologic Reviews 2010; 32(1): 110-120. http://dx.doi.org/10.1093/epirev/mxq009
3. Jiang H, Livingston M, Manton E. The effects of random breath testing and lowering the minimum legal drinking age on traffic fatalities in Australian states. Injury Prevention 2014; 21(2): 77-83. http://dx.doi.org/10.1136/injuryprev-2014-041303
4. Kingham S, Pearce J, Dorling D, Faulk M. The impact of the graduated driver licence scheme on road traffic accident youth mortality in New Zealand. Journal of Transport Geography 2008; 16(2): 134-141. http://dx.doi.org/10.1016/j.jtrangeo.2007.04.002
5. Norton R, Hyder AA, Bishai D, Peden M. Unintentional injuries. In: DT Jamison, P Musgrove, A Meachem (Eds). Disease control priorities in developing countries. Washington, DC: World Bank, 2006; 737-753.
6. Gosselin, RA. The increasing burden of injuries in developing countries: direct and indirect consequences. Techniques in Orthopaedics 2009; 24(4): 230-232. http://dx.doi.org/10.1097/BTO.0b013e3181bfd56c
7. de Ramirez SS, Hyder AA, Herbert HK, Stevens K. Unintentional injuries: magnitude, prevention, and control. Annual Review of Public Health 2012; 33: 175-191. http://dx.doi.org/10.1146/annurev-publhealth-031811-124558
8. Scriven A. Promoting health: policies, principles and perspectives. In: A Scriven (Ed). Health promoting practice: the contribution of nurses and allied health professions. Basingstoke, Palgrave, 2005; 1-16.
9. Bugeja L, Richard CF. An analysis of stratagems to reduce drowning deaths of young children in private swimming pools and spas in Victoria, Australia. International Journal of Injury Control and Safety Promotion 2013; 20(3): 282-294. http://dx.doi.org/10.1080/17457300.2012.717086
10. World Health Organization. Developing policies to prevent injuries and violence: guidelines for policy-makers and planners. (Internet) 2006. Available: http://www.who.int/violence_injury_prevention/publications/39919_oms_br_2.pdf (Accessed 12 September 2015).
11. Sethi D, Aljunid S, Sulong SB, Zwi AB. Injury care in low- and middle-income countries: identifying potential for change. Injury Control and Safety Promotion 2000; 7(3): 153-164. http://dx.doi.org/10.1076/1566-0974(200009)7:3;1-N;FT153
12. World Bank. Population total. (Internet) 2015. Available: http://data.worldbank.org/indicator/SP.POP.TOTL (Accessed 19 September 2015).
13. World Health Organization. Solomon Islands. (Internet) 2015. Available: http://www.wpro.who.int/countries/slb/31SOLpro2011_finaldraft.pdf?ua=1 (Accessed 21 November 2015).
14. World Health Organization. Human resources for health country profiles: Solomon Islands. (Internet) 2014. Available: http://www.wpro.who.int/hrh/documents/publications/wpr_hrh_country_profiles_solomon_islands_upload.pdf (Accessed 1 November 2015).
15. World Health Organization. National health strategic plan: The Ministry of Health and Medical Services Solomon Islands Government 2011-2015. (Internet) 2011. Available: http://www.wpro.who.int/health_services/solomon_islands_nationalhealthplan.pdf?ua=1 (Accessed 1 November 2015).
16. Negin J, Martiniuk ALC, Farrell P, Dalipanda T. Frequency, cost and impact of inter-island referrals in the Solomon Islands. Rural and Remote Health (Internet) 2012; 12(3): 2096. Available: www.rrh.org.au (Accessed 19 May 2015).
17. World Health Organization. Solomon Islands: WHO statistical profile. (Internet) 2015. Available: http://www.who.int/gho/countries/slb.pdf?ua=1 (Accessed 1 November 2015).
18. Curtin M, Molineux M, Supyk-Mellson J (Eds). Occupational therapy and physical dysfunction: enabling occupation. 6th edn. London: Elsevier, 2010.
19. Scaffa ME, Chromiak SB, Reitz SM, Blair-Newton A, Murphy L, Wallis CB. Unintentional injury and violence prevention. In: ME Scaffa, SM Reitz, MA Pizzi (Eds). Occupational therapy in promotion of health and wellbeing. Philadelphia: FA Davis, 2010; 350-375.
20. Tolley L, Atwal A. Determining the effectiveness of a falls prevention programme to enhance quality of life: an occupational therapy perspective. British Journal of Occupational Therapy 2003; 66(6): 269-276. http://dx.doi.org/10.1177/030802260306600606
21. Tse T. The environment and falls prevention: do environmental modifications make a difference? Australian Occupational Therapy Journal 2005; 52(4): 271-281. http://dx.doi.org/10.1111/j.1440-1630.2005.00525.x
22. Classen S, Shechtman O, Awadzi KD, Joo Y, Lanford DN. Traffic violations versus driving errors of older adults: informing clinical practice. American Journal of Occupational Therapy. 2010; 64(2):233-241. http://dx.doi.org/10.5014/ajot.64.2.233
23. Stutts JC, Wilkins JW. On-road driving evaluations: a potential tool for helping older adults drive safely longer. Journal of Safety Research 2003; 34(4):431-439. http://dx.doi.org/10.1016/j.jsr.2003.09.014
24. McCluskey A, Lovarini M, Bennett S, McKenna K, Tooth L, Hoffmann T. What evidence exists for work-related injury prevention and management? Analysis of an occupational therapy evidence database. British Journal of Occupational Therapy 2005; 68(10): 447-456. http://dx.doi.org/10.1177/030802260506801003
25. Anzarut A, Olson J, Singh P, Rowe BH, Tredget EE. The effectiveness of pressure garment therapy for the prevention of abnormal scarring after burn injury: a meta-analysis. Journal of Plastic, Reconstructive & Aesthetic Surgery 2009; 62(1): 77-84. http://dx.doi.org/10.1016/j.bjps.2007.10.052
26. Habib MM, Uddin MJ, Rahman SU, Jahan N, Akter S. Occupational therapy role in disaster management in Bangladesh. World Federation of Occupational Therapists Bulletin 2013; 68(1): 33-7. http://dx.doi.org/10.1179/otb.2013.68.1.010
27. Riggers L. Healing Haiti: the experience of an occupational therapist in disaster response. (Masters thesis). Washington, United States: University of Puget Sound, 2011.
28. Mosayed Ullah M, Jahan Ema A. 'Good start' for spinal cord injury management: an occupational therapy initiative of Bangladesh. World Federation of Occupational Therapists Bulletin 2012; 66(1): 33-34. http://dx.doi.org/10.1179/otb.2012.66.1.012
29. Ullah MM, Sarker A, Chowdhury SK. Assessment for returning to work after spinal cord injuries and patient's vocational preferences. Work 2015; 50(3): 387-393. http://dx.doi.org/10.3233/WOR-151995
30. O'Brien L, Hardman A. Developing hand therapy skills in Bangladesh: experiences of Australian volunteers. Journal of Hand Therapy 2013; 27(1): 30-37. http://dx.doi.org/10.1016/j.jht.2013.09.006
31. Burggraaf A, Bourke-Taylor H. Occupational therapy student's fieldwork placement: institutional and community based rehabilitation models in the Solomon Islands. New Zealand Journal of Occupational Therapy 2008; 55(2): 25-31.
32. Australian Volunteers International. Occupational therapist and mentor. (Internet) 2015. Available: http://www.australianvolunteers.com/jobs/10533571-occupational-therapist-and-mentor/ (Accessed 8 October 2015).
33. Japan International Cooperation Agency. JICA volunteers in Solomon Islands (Internet) 2015. Available: http://www.jica.go.jp/solomon/office/activities/volunteer/ku57pq00001zbq8s-att/volunteer_map.pdf (Accessed 8 October 2015).
34. Whittemore R, Knafl K. The integrative review: updated methodology. Journal of Advanced Nursing 2005; 52(5): 546-553. http://dx.doi.org/10.1111/j.1365-2648.2005.03621.x
35. Torraco RJ. Writing integrative literature reviews: guidelines and examples. Human Resource Development Review 2005; 4(3): 356-367. http://dx.doi.org/10.1177/1534484305278283
36. Moher D, Liberati A, Tetzlaff J, Altman DG. The PRISMA Group. Preferred reporting items for systematic reviews and meta-analysis: the PRISMA statement. PLoS Medicine (Internet) 2009; 6(7). http://dx.doi.org/10.1371/journal.pmed.1000097
37. World Bank. Country and lending groups. (Internet) 2015. Available: http://data.worldbank.org/about/country-and-lending-groups (Accessed 9 November 2015).
38. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006; 3: 77-101. http://dx.doi.org/10.1191/1478088706qp063oa
39. Canadian Occupational Therapists. Profile of occupational therapy practice in Canada. (Internet) 2012. Available: https://www.caot.ca/pdfs/2012otprofile.pdf (Accessed 13 October 2015).
40. Australian Institute of Health and Welfare National Injury Surveillance Unit. ICD-9-CM, ICD-10. NDS-IS level 1, item 3 Place of injury occurrence type. National Data Standards for Injury Surveillance (NDS-IS) version 2.1. (Internet) 1998. Available: https://web.archive.org/web/20130423234305/http://www.nisu.flinders.edu.au/pubs/manuals/ndsis/ndsisman-Summary.html (Accessed 13 October 2016).
41. Coleman K, Norris S, Weston A, Grimmer-Somers K, Hillier S, Merlin T, et al. NHMRC additional levels of evidence and grades for recommendations for developers of guidelines. (Internet) 2009. Available: https://www.nhmrc.gov.au/_files_nhmrc/file/guidelines/stage_2_consultation_levels_and_grades.pdf? (Accessed 29 October 2015).
42. Mulford JS, Oberli H, Tovosia S. Coconut palm-related injuries in the Pacific Islands. ANZ Journal of Surgery 2001; 71(1): 32-34. http://dx.doi.org/10.1046/j.1440-1622.20, 01.02021.x
43. Negin J, Vizintin P, Houasia P, Martiniuk ALC. Barking up the wrong tree: injuries due to falls from trees in Solomon Islands. The Medical Journal of Australia 2014; 201(11): 698-700. http://dx.doi.org/10.5694/mja14.01083
44. Stewart JM, Negin J, Farrell P, Houasia P, Munamua AB, Martiniuk A. Extent, causes and impact of road traffic crashes in the Solomon Islands 1993-2012: data from the orthopaedic department at the National Referral Hospital, Honiara. Rural and Remote Health (Internet) 2015; 15 (3): 2945. Available: www.rrh.org.au (Accessed 9 October 2015).
45. Baker ML, Painter G, Hewitt AW, Islam FM, Szetu J, Qalo M, Keeffe J. Profile of ocular trauma in the Solomon Islands. Clinical & Experimental Ophthalmology 2014; 42(5):440-446.
46. Fegan D, Glennon M. Significance of soccer injuries in the rural Solomon Islands. Tropical Doctor 1989; 19(4): 183-184.
47. Habib MM, Jahan N, Nahar L. Low assistive technologies for persons with spinal cord injury (SCI) in Bangladesh. World Federation of Occupational Therapists Bulletin 2014; 69: 37-41. http://dx.doi.org/10.1179/otb.2014.69.1.011
48. Hansen CH, Mahmud I, Bhuiyan AJ. Vocational reintegration of people with spinal cord lesions in Bangladesh - an observational study based on vocational training project at CRP. Asia Pacific Disability Rehabilitation Journal 2007; 18(1): 63-75.
49. Hossain MI, Nahar N, Nayan MJ, Jahan Ema A, Arafat Alve MY. Experience of Bangladeshi occupational therapists with 'Rana Plaza Tragedy' survivors: recovery and rehabilitation phases of disaster management. World Federation of Occupational Therapists Bulletin 2013; 68(1): 14-19. http://dx.doi.org/10.1179/otb.2013.68.1.006
50. Prabhaka MM, Thakker TH. A follow-up program in India for patients with spinal cord injury: paraplegia safari. Journal of Spinal Cord Medicine 2004; 27(3): 260-262. http://dx.doi.org/10.1080/10790268.2004.11753758
51. Klappa S, Audette J, Do S. The roles, barriers, and experiences of physical and occupational therapists in disaster relief: post-earthquake Haiti 2010. Disability and Rehabilitation 2014; 36(4): 1-9.
52. Santoso TB. Occupational therapy fieldwork experience in disaster response and recovery. World Federation of Occupational Therapists Bulletin 2013; 68(1):31-43. http://dx.doi.org/10.1179/otb.2013.68.1.009
53. Welage N, Liu KP. Review of a home and community integration programme for people with spinal cord injuries: Hong Kong and its relevance to Sri Lanka. Hong Kong Journal of Occupational Therapy 2008; 18(1): 34-39. http://dx.doi.org/10.1016/S1569-1861(08)70011-1
54. Rodgers-Wilson M. The occupational therapist in Papua New Guinea. Papua New Guinea Medical Journal 1982; 25(2): 123-126.
55. Duque RL, Grecia A, Ching PE. Development of a national occupational therapy disaster preparedness and response plan: the Philippine experience. World Federation of Occupational Therapists Bulletin 2013; 68(Nov): 26-30. http://dx.doi.org/10.1179/otb.2013.68.1.008
56. Scovil CY, Ranabhat MK, Craighead IB, Wee J. Follow-up study of spinal cord injured patients after discharge from inpatient rehabilitation in Nepal in 2007. Spinal Cord 2012; 50(3):232-237. http://dx.doi.org/10.1038/sc.2011.119
57. Health Data. Global burden of disease: Solomon Islands. (Internet) 2010. Available: http://www.healthdata.org/sites/default/files/files/country_profiles/GBD/ihme_gbd_country_report_solomon_islands.pdf (Accessed 16 March 2015).
58. Nanau GL. The Wantok system as a socio-economic and political network in Melanesia. The Journal of Multicultural Society 2011; 2(1): 31-35. http://dx.doi.org/10.15685/omnes.2011.06.2.1.31
59. Körner M. Interprofessional teamwork in medical rehabilitation: a comparison of multidisciplinary and interdisciplinary team approach. Clinical Rehabilitation 2010; 24(8): 745-755. http://dx.doi.org/10.1177/0269215510367538
60. Wade DT, Gage H, Owen C, Trend P, Grossmith C, Kaye J. Multidisciplinary rehabilitation for people with Parkinson's disease: a randomised controlled study. Journal of Neurology, Neurosurgery & Psychiatry 2003; 74(2): 158-162. http://dx.doi.org/10.1136/jnnp.74.2.158
61. Boshoff K, Hartshorne S. Profile of occupational therapy practice in rural and remote South Australia. Australian Journal of Rural Health 2008; 16(5): 255-261. http://dx.doi.org/10.1111/j.1440-1584.2008.00988.x
62. Bourke-Taylor H, Hudson D. Cultural differences: the experience of establishing an occupational therapy service in a developing community. Australian Occupational Therapy Journal 2005; 52(3): 188-198. http://dx.doi.org/10.1111/j.1440-1630.2005.00493.x
63. Scheidegger G, Torrance-Foggin ME. Occupational therapy and cultural understanding - cross-cultural experiences in a newly established occupational therapy service in Qinghai Province, China. World Federation of Occupational Therapists Bulletin 2015; 71(2): 88-95. http://dx.doi.org/10.1179/2056607715Y.0000000001
64. Kingston GA, Williams G, Judd J, Gray MA. Hand therapy services for rural and remote residents: results of a survey of Australian occupational therapists and physiotherapists. Australian Journal of Rural Health 2015; 23(2): 112-121. http://dx.doi.org/10.1111/ajr.12141
65. Mills A, Millsteed J. Retention: an unresolved workforce issue affecting rural occupational therapy services. Australian Occupational Therapy Journal 2002; 49(4): 170-181. http://dx.doi.org/10.1046/j.1440-1630.2002.00293.x
66. Roots RK, Li LC. Recruitment and retention of occupational therapists and physiotherapists in rural regions: a meta-synthesis. BMC Health Services Research 2013; 13(1): 1-13. http://dx.doi.org/10.1186/1472-6963-13-59
67. Krefting L. Strategies for the development of occupational therapy in the Third World. American Journal of Occupational Therapy 1992; 46(8): 758-761. http://dx.doi.org/10.5014/ajot.46.8.758
___________________________________
Appendix I. Search strategies




