full article:
Rural background or sustained rural exposure during training are widely accepted to be strongly associated with working in rural practice1-3. Based on this collective evidence a number of initiatives have been introduced in Australia including quarantined places and scholarships in medical schools for rural students, mandatory short-term rural placements for all Australian Commonwealth-supported students and opportunities for longer-term rural placements at rural clinical schools (RCSs)4.
Early data have demonstrated that RCS exposure increased students' intentions to work rurally5 and that RCS graduates are more likely than their peers to work rurally as pre-vocational doctors6. Since the establishment of RCSs a decade ago, research is beginning to report positive longer term outcomes7-9.
In New South Wales (NSW), efforts have been made to foster vertical integration of rural medical training by linking undergraduate training to postgraduate positions in rural areas through the establishment of the Rural Preferential Recruitment (RPR) program10. The pathway, which was developed by the Health Education and Training Institute in 2007, then known as the Postgraduate Medical Council of NSW, is a merit-based process that facilitates recruitment of medical graduates interested in working in a rural setting to pre-vocational training positions in rural hospitals.
This article focuses on an initiative that was introduced prior to both the RPR program and RCSs but often serves as a significant link between the two in encouraging and supporting medical students to choose rural careers.
The NSW Rural Resident Medical Officer Cadetship Program was established in 1988 by the then NSW Department of Health, as a strategy to increase the numbers of junior doctors in rural hospitals. The cadetship offers bonded scholarships, which provide financial support for medical students during their final 2 years of undergraduate study and, in return, cadets are contracted to complete two of their first three postgraduate years in a rural NSW hospital. In addition to the financial support while they are studying, cadets are subsidised to attend education and development events over the 4 years they are involved with the program. They receive a relocation allowance to assist with moving for their rural service and they have access to personalised mentoring, networking and support opportunities.
The aims of the cadetship are to increase the numbers of postgraduate doctors working in rural NSW hospitals as well as the overall recruitment of medical practitioners into rural and remote communities on the basis that positive exposure to rural medicine increases the likelihood of choosing to practise in a rural location. The cadetship is now the only incentive scheme of its kind in Australia and serves as a supportive pathway from undergraduate to postgraduate rural training.
The aim of this study is to report on the results of an evaluation undertaken in 2014 of the cadetship. Specifically, the study will look at where former cadets who entered the program between 1989 and 2010 were working in 2014, what training programs they chose and their attitudes towards the program.
The cadetship
The NSW Rural Doctors Network (RDN) administers the cadetship, which is funded by the NSW Ministry of Health and is now in its 26th year of operation. Applicants must be Australian citizens or permanent residents and enrolled as full-time students at a NSW university with 2 years of their medical degree remaining. Students from medical schools interstate or in New Zealand are also eligible to apply, provided they have completed their final year of secondary school in NSW. Twelve cadetships are offered each year, and since 2011 two cadetship places are reserved for Indigenous applicants annually. Applications are assessed on the basis of a demonstrated interest in rural health and an understanding of the issues affecting rural communities, although applicants are not required to have lived in a rural location.
From 1989 to 2014, 297 medical students accepted a cadetship, an average of 12 cadets per year (Fig1). This included six students who received a cadetship specifically for Indigenous medical students. Four students (1%) did not complete their medical degree. Of the remaining 293 students, 211 have completed their rural service, 23 are currently completing rural service and 27 are undergraduates. Thirty-two (11%) have withdrawn from the program, 19 before commencing rural service and 13 during rural service.
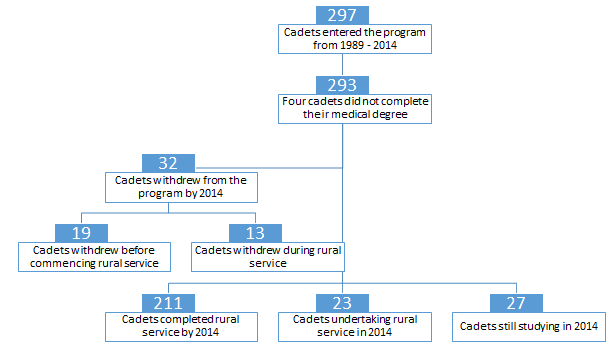
Figure 1: Cadets who entered the cadetship program between 1989 and 2014.
This study will include cadets who entered the program from 1989 to 2010, and had completed their rural service by 2014 (n=211).
Data collection
Data was collected using a questionnaire sent to former cadets who entered the program from 1989 until 2010. This included questions relating to background, vocational training, current role, current work location and attitudes towards the cadetship program.
The questionnaire was created using SurveyMonkey and sent to participants by email in February 2014. Two follow-up emails were sent to non-responders 3 and 6 weeks after the initial contact. Email addresses were not available for a small number of cadets and in these cases questionnaires were sent by post or fax. Responses were received from 142 of the 211 cadets in the study group (67%).
Geographical information (where cadets grew up and location of practice in 2014) was categorised using the Australian Standard Geographical Classification - Remoteness Areas (ASGC-RA). ASGC-RA is a geographic classification system that was developed in 2001 by the Australian Bureau of Statistics as a statistical geography structure that allows quantitative comparisons between 'city' and 'country' Australia. Remoteness is calculated using the road distance to the nearest urban centre in each of five classes based on population size. The classification consists of five categories: RA1 - Major Cities, RA2 - Inner Regional, RA3 - Outer Regional, RA4 - Remote and RA5 - Very Remote. In this study, categories RA2-5 are described as rural. Background was defined by the RA classification of the location where cadets spent the majority of their primary schooling.
Data were entered into the Statistical Package for the Social Sciences v22 (IBM; http://www.spss.com) and analysed using standard statistical analysis methods. The analysis explored the factors that contribute to students becoming a cadet and their future career choice and practice location.
Ethics approval
Advice regarding ethics approval was sought from the Hunter New England Human Research and Ethics Governance Unit prior to implementing the survey tool. It was advised that the research did not require approval from a human research ethics committee.
The survey tool used stated that information provided by participants may be published in a de-identified form and no identifiable information would be released to any other organisation.
Demographics of cadets
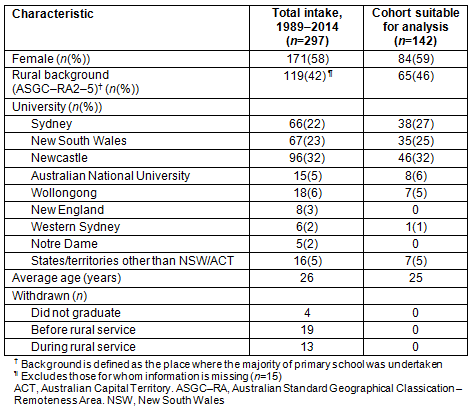
The demographics of cadets in the study group are generally consistent with those of the total cadet intake (Table 1). Over half of cadets in the study group are female (59%), which differs from the current overall medical student population of 50%11. Forty-six percent of cadets in the study group come from rural backgrounds, which is slightly higher than the total cadet intake of 42%. The majority of cadets in both the study group and the overall cadet intake have come from one of three medical schools: the universities of Sydney, NSW and Newcastle. These medical schools have been operating since the beginning of the cadetship program while the other universities have only established their medical programs more recently.
Table 1: Characteristics of all medical students entering the cadetship program and those of cadets in the analysis group
Geographical background in relation to choice of career and practice location
Of the 142 cadets in the study group, 66 (46%) spent the majority of their primary schooling in an urban area (RA1), 65 (46%) came from a rural background (RA2-5) and the remaining 11 grew up overseas (8%) (Table 2).
Based on those who responded to the questionnaire, it would appear that cadets with rural backgrounds were more likely to choose general practice (35 out of 65) than those from urban backgrounds (23 out of 64).
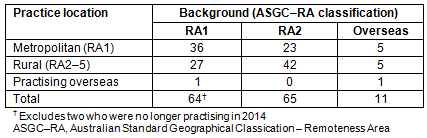
A similar analysis of cadets comparing geographic background and practice location showed cadets who came from a rural background were more likely to be working in a rural location than cadets with urban backgrounds (Table 3) (p<0.032).
Neither gender nor having a spouse from a rural area was a significant factor in practice location.
Table 2: Relationship between background and career choice (n=140)?
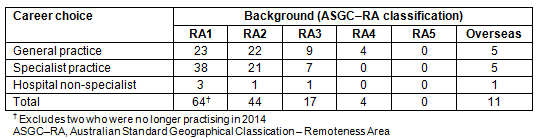
Table 3: Relationship between background and practice location (n=140)?
Career choice and practice location
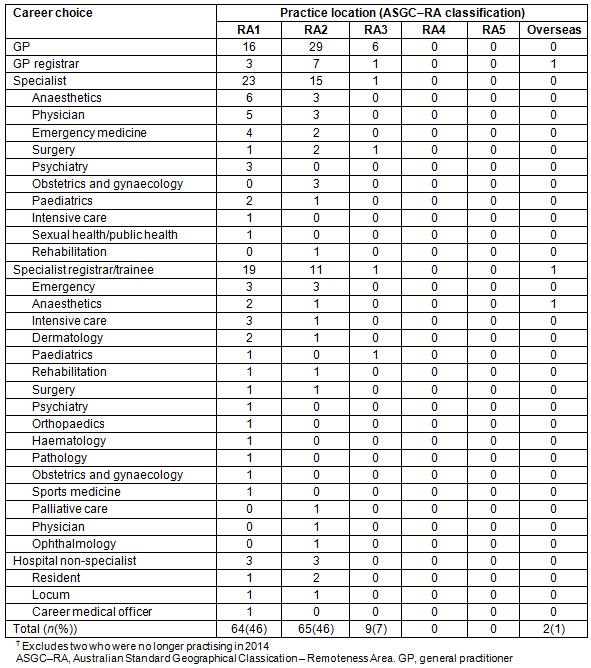
Of the 142 former cadets surveyed, 90 (63%) had completed a vocational training program and were working as fully qualified medical practitioners (51 in general practice and 39 in specialties other than general practice). A further 44 (31%) were trainees (12 in general practice and 32 in other specialties), six were non-specialist hospital doctors and two were no longer practising (Table 4). Overall, the most popular vocational training programs among fully qualified doctors and trainees combined were general practice (n=63, 44%), anaesthetics/intensive care (n=18, 12%) and emergency medicine (n=12, 8%).
Over half of the cadets (n=74, 53%) were working in rural areas (RA2-5) in 2014 (Table 4) and practice location was significantly (p<0.001) influenced by career choice.
While 45% (63) of cadets entered general practice, they made up 58% (81)of those working in rural areas (Table 4). In comparison, those who entered specialties other than general practice constituted 38% (53) of the cohort working in rural areas while hospital non-specialists constituted 4% (5) (Table 4).
Table 4: Relationship between practice location (as defined by Australian Standard Geographical Classification - Remoteness Areas classification) and career choice (n=140)?
The experience of being a cadet
Influence on future career: The questionnaire asked participants how important the cadetship and period of rural service had been in influencing their career path and influencing their decision to practise rurally. Of the 142 cadets in the analysis group, 138 responded to these questions (Table 5). Forty-four percent (n=61) indicated the cadetship and period of rural service were very important in influencing their career path, while a further 40% (n=55) indicated it was somewhat important. Only 16% (n=22) reported the cadetship and period of rural service had no influence on their career path.
Similarly, 15% of cadets reported the cadetship had no influence on their decision to practise rurally (n=21), while 39% (n=54) indicated it was very important, and it was somewhat important for 46% (n=63)(Table 6).
Cadets were also asked if they would have applied for a postgraduate training position in a rural hospital had they not received a cadetship. Of the 142 cadets surveyed, 140 answered this question. Twenty percent (n=28) of respondents said they would not have applied for a rural postgraduate training position while a further 26% (n=36) said they were unsure. Of these 64 respondents who would not have chosen to work in a rural hospital as a junior doctor without the cadetship, or were not sure if they would have, one-third were working in rural locations in 2014.
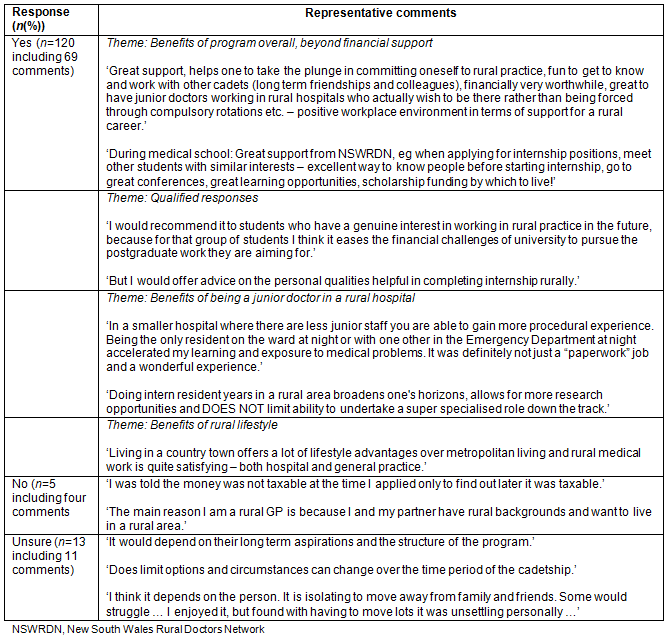
Would former cadets recommend the program to others? The questionnaire also asked if former cadets would recommend the cadetship to other medical students, with 138 of the 142 participants responding (Table 7). Of those, 87% (n=120) said they would recommend the cadetship to other medical students, although 10 of those qualified their responses. The most common qualification was having a real interest in working and living in a rural centre and a willingness and ability to fulfill the 2-year bond (not having commitments keeping them in a metropolitan area). A small group of cadets also expressed concerns around access to training programs other than general practice, with one cadet claiming rural training makes it harder to move back to the city for specialist training.
However, the majority of cadets expressed unreservedly positive sentiments of the benefits of the program, including the financial support, the broad, general experience gained from training in a regional hospital and the lifestyle advantages of living in a rural area. Others noted the benefits of peer support that come from being part of a group, as well as the support and opportunities provided by RDN.
In contrast to the few cadets who stated that postgraduate rural training limited career choice, a larger number of cadets reported their rural service positively influenced their application for specialist training. This view is supported by the finding that 52% of cadets in this analysis have become or are training to become specialists (Tables 2,3).
Five cadets said they would not recommend the cadetship (4%) for reasons including that rural hospitals do not provide enough support, the financial benefit is negated once tax is applied, the requirements are too inflexible, and that it does not result in long-term rural practice.
Similar reasons were given by those who were unsure if they would recommend the cadetship (n=13, 9%). For other cadets in this group, their hesitation was due to not knowing how the program is structured now, while others said it would depend on the type of person.
Table 5: Representative responses to 'How important was the cadetship and period of rural service in influencing your career path?' (n=138)

Table 6: Representative responses to 'How important was the cadetship and period of rural service in influencing your decision to practise rurally?' (n=138)

Table 7: Responses to 'Would you recommend the cadetship to medical students?' (n=138)
Discussion
Consistent with a previous study of the cadetship program undertaken in 200412, data from this study demonstrate that cadets are more likely to have a rural background (46%) compared with the general medical student population of around 27%11. Forty-five percent of cadets in this analysis chose to specialise in general practice, compared with 23.4% of doctors in general practice training programs nationally in 201413.
However, of the 74 cadets in this cohort who were working in rural locations, 27 were of urban background (36%). This reinforces the finding from the 2004 cadetship evaluation that the program serves as an effective link between medical school and rural practice, particularly rural general practice, for students from both a rural and urban background.
Significantly, more than half of cadets in this analysis were working in rural locations (RA2-5) in 2014 compared with 21% of all medical practitioners nationally14.
Career choice is a significant determinant of practice location. Those in general practice were much more likely to work in rural areas, which is consistent with previous studies including one looking at specialty choice and career location of RCS graduates from the University of Queensland8 and another from Western Australia15. Practice location is influenced by a variety of factors including population size and demographics in relation to specialty type, and teaching and supervision capacity of hospitals for registrars and training places.
When the cadetship program began in 1989 there was little encouragement for medical graduates to work in rural areas. However, the past two decades have seen the introduction of RCSs and university departments/centres of rural health as well as rural hospitals gaining accreditation to provide pre-vocational training. One quarter of Commonwealth-supported medical students are expected to spend at least 1 year of their clinical training in a rural setting while a 4-week structured rural placement must be provided for the remaining Commonwealth-supported students4. Similarly, positive changes have occurred in postgraduate training with the percentage of postgraduate year 1 places in non-metropolitan areas accounting for 13.6% of total positions in 2014 compared to 5.3% in 2004. Both of these developments have meant that many more students and junior doctors have had the opportunity to experience rural practice, resulting in a gradual shift in common perceptions around rural training16. This was demonstrated by an evaluation of the rural programs at the Australian National University, which found that students were motivated to spend a year in a rural location because it was thought that training in a rural setting would provide them with superior clinical exposure17.
Qualitative results from this study indicate that attitudes towards rural training have indeed shifted among cadets over time. Previous evaluations of the cadetship program, some unpublished, indicate significant numbers of cadets felt that postgraduate rural training was a barrier to many vocational training programs and would only recommend the program to students interested in pursuing general practice. Some cadets who were interested in training in specialties other than general practice reported feeling isolated and vulnerable when it came time to apply for a vocational training program12. In contrast, 87% of cadets in this study reported they would recommend the program to others, a proportion that remained the same among cadets who have pursued general practice training and those who chose other specialties. Some cadets commented that their rural service positively influenced their application for specialist training.
The cadetship program is one of the few initiatives to support junior doctors between graduation and entry onto vocational training programs - particularly general practice - which has historically been where a gap occurs in the rural training pipeline18,19. Even fewer incentive-based initiatives target the postgraduate training years.
Internationally, three systematic reviews have been published evaluating the effectiveness of incentive programs worldwide as a means of addressing health worker shortages20-22. The first of these reviews, by Sempowski, found that return of service programs were successful in achieving short-term recruitment, but less effective in encouraging long-term retention20. Sempowski's review included 10 publications, most of which were from the USA, and focused on programs targeting medical practitioners. Bärnighausen and Bloom's review included 43 studies, 34 of which were from the USA, and encompassed incentive schemes for all types of health workers. This second review found that participants of incentive programs were actually more likely than non-participants to work in underserved areas long-term, although they are less likely to remain in the same location as the original placement21. Similarly, although the majority of the cadets in this cohort were working in a rural area when surveyed, they were not necessarily working in the same region as their rural service.
The third review, by Wilson et al, which looked at eight programs in USA, South Africa and Australia, found that the success of scholarship and bursaries with return of service agreements was highly variable and required further long-term investigation22. However, an assessment of one of the scholarship incentive schemes in South Africa found that mentoring and ongoing support to students while at university and ensuring smooth integration into the hospital workforce was essential to the success of the program22. Similarly, it is apparent from the responses from cadets in this analysis that the mentoring, networking and support components of the cadetship program are integral to the success of the program and one of the main reasons it is so highly regarded by former cadetship recipients.
Of all the vocational training programs, general practice training is still the most versatile for those doctors wishing to become part of the rural workforce. General practice registrars can complete all their training through regional training providers without the need to return to an urban setting. A major development in rural medical training has been the establishment of state-based rural generalist training pathways. These programs aim to produce general practitioners who can provide primary care in a rural community as well as advanced procedural services such as anaesthetics or obstetrics through the local health service. In 2016 there will be 34 positions offered under the Rural Generalist Training program in NSW.
In this cohort of cadets, six out of nine general practice trainees were working in rural areas including two who were part of the Rural Generalist Training program. By comparison, 13 out of 33 (39%) specialist trainees were working in rural areas. This supports other research demonstrating the importance of developing more rural training positions for specialties beyond general practice to encourage junior doctors who are already working in rural areas to remain23,24.
There has however been a move in recent years to increase opportunities for specialty training in rural areas with the establishment of the Specialist Training Program by the Australian Government Department of Health25. Through the nationally supported program, 12 specialist medical colleges are funded to extend vocational training for registrars beyond traditional metropolitan teaching hospitals including regional and rural hospitals and community health settings. In 2015, 900 STP positions were funded nationally25.
The move towards vertical integration has enabled a rural stream to be developed within some areas of medicine so that appropriate experience and training can occur. This is most advanced in general practice and emergency medicine but other specialties are slowly moving in this direction. The cadetship program provides an important link in the pathway between rural undergraduate and vocational training.
The cadetship program, which ensures doctors complete two of their first 3 years of postgraduate training in a rural, non-coastal hospital, is an effective link between medical school and rural practice, particularly general practice. The success of the program relies in part on the mentoring, networking and other educational opportunities available to cadets, which serves to encourage and maintain cadets' enthusiasm for rural medicine throughout the 4-year program. The limitations of this study are the small sample size and the potential response bias. It would be beneficial for future evaluators to have a control group.
This study has demonstrated that targeted incentive based scholarship schemes with a return-of-service component can be beneficial, particularly where they include ongoing support and reinforcement throughout the transition from undergraduate to postgraduate training. Also apparent is the importance of developing more vocational training pathways in rural areas to retain those who want to remain in a rural location.
References
1. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health (Internet) 2003; 3: 212. Available: www.rrh.org.au (Accessed 25 November 2015).
2. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11(6): 277-284. http://dx.doi.org/10.1111/j.1440-1584.2003.00534.x
3. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health (Internet) 2009; 9: 1083. Available: www.rrh.org.au (Accessed 25 November 2015).
4. Department of Health. Rural Clinical Training and Support (RCTS) 2011-2014 - operational framework. Canberra: Australian Government.
5. Eley DS, Baker PG. Will Australian rural clinical schools be an effective workforce strategy? Early indications of their positive effect on intern choice and rural career interest. Medical Journal of Australia 2007; 187(3): 166-167.
6. McDonald Smedts A, Lowe MP. Efficiency of clinical training at the Northern Territory clinical school: placement length and rate of return for internship. Medical Journal of Australia 2008; 189(3): 166-168.
7. Worley P, Martin A, Prideaux D, Woodman R, Worley E, Lowe M. Vocational career paths of graduate entry medical students at Flinders University: a comparison of rural, remote and tertiary tracks. Medical Journal of Australia 2008; 188(3): 177-178.
8. Eley DS, Synnott R, Baker PG, Chater AB. A decade of Australian rural clinical school graduates - where are they and why? Rural and Remote Health (Internet) 2012; 12: 1937. Available: www.rrh.org.au (Accessed 24 November 2015).
9. Kondalsamy-Chennakesavan S, Eley DS, Ranmuthugala G, Chater AB, Toombs MR, Darshan D, et al. Determinants of rural practice: positive interaction between rural background and rural undergraduate training. Medical Journal of Australia 2015; 202(1): 41-45. http://dx.doi.org/10.5694/mja14.00236
10. Health Education and Training Institute (Medical Portfolio) PSD - procedure - rural preferential recruitment. Document number 12/3456. Available: http://www.heti.nsw.gov.au (Accessed 24 November 2015).
11. Medical Deans Australia and New Zealand. Workforce data report 2014. (Internet) 2014. Available: http://www.medicaldeans.org.au/wp-content/uploads/MedicalDeans_2014WorkforceDataReport_05092014.pdf (Accessed 1 November 2015).
12. Dunbabin JS, McEwin K, Cameron I. Postgraduate medical placements in rural areas: their impact on the rural medical workforce. Rural and Remote Health (Internet) 2006; 6: 481. Available: www.rrh.org.au (Accessed 1 November 2015).
13. The Australian Government Department of Health. Medical Training Review Panel: Eighteenth Report. (Internet) 2015. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/work-pubs-mtrp-18 (Accessed 1 November 2015).
14. Australian Institute of Health and Welfare Medical workforce 2012. (Internet) 2014. National Health Workforce series no. 8. Cat. no. HWL 54. Available: http://www.aihw.gov.au/publication-detail/?id=60129546100 (Accessed 1 November 2015).
15. Playford DE, Evans SF, Atkinson DN, Auret KA, Riley GK. Impact of the Rural Clinical School of Western Australia on work location of medical graduates. Medical Journal of Australia 2014; 200(2): 104-107. http://dx.doi.org/10.5694/mja13.11082
16. Rogers ME, Creed PA, Searle J. Junior doctors' and medical students' commitment to working in areas of workforce shortage. Rural and Remote Health (Internet) 2011; 11: 1775. Available: www.rrh.org.au (Accessed 1 November 2015).
17. Lee YH, Barnard A, Owen C. Initial evaluation of rural programs at the Australian National University: understanding the effects of rural programs on intentions for rural and remote medical practice. Rural and Remote Health (Internet) 2011; 11(2): 1602. Available: www.rrh.org.au (Accessed 1 November 2015).
18. Smith DM. Barriers facing junior doctors in rural practice. Rural and Remote Health (Internet) 2005; 5(4): 348. Available: www.rrh.org.au (Accessed 1 November 2015)
19. Nichols A, Worley PS, Toms LM, Johnston-Smith PR. Change of place, change of pace, change of status: rural community training for junior doctors, does it influence choices of training and career? Rural and Remote Health (Internet) 2004; 4: 259. Available: www.rrh.org.au (Accessed 24 November 2015).
20. Sempowski IP. Effectiveness of financial incentives in exchange for rural and underserviced area return?of?service commitments: a systematic review of the literature. Canadian Journal of Rural Medicine 2004; 9(2): 82?88.
21. Bärnighausen T, Bloom DE. Financial incentives for return of service in underserved areas: a systematic review. BMC Health Services Research 2009; 9: 86. http://dx.doi.org/10.1186/1472-6963-9-86
22. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health (Internet) 2009; 9: 1060. Available: www.rrh.org.au (Accessed 24 November 2015).
23. Playford DE, Cheong E. Rural Undergraduate Support and Coordination, Rural Clinical School and Rural Australian Medical Undergraduate Scholarship: rural undergraduate initiatives and subsequent rural medical workforce. Australian Health Review 2012; 36(3): 301-307. http://dx.doi.org/10.1071/AH11072
24. Schauer A, Woolley T, Sen Gupta T. Factors driving James Cook University Bachelor of Medicine, Bachelor of Surgery graduates' choice of internship location and beyond. Australian Journal of Rural Health 2014; 22(2): 56-62. http://dx.doi.org/10.1111/ajr.12080
25. Department of Health. Specialist Training Program (STP) operational framework. (Internet). Available: http://www.health.gov.au (Accessed 24 November 2015).



