full article:
Vision impairment is a worldwide health concern affecting 285 million people1. The effect is most felt in countries and communities with limited resource availability where people face poor access to services.
Papua New Guinea (PNG) is the largest and most populous country in the South Pacific, with high levels of vision impairment and blindness2. It is a geographically diverse country of 19 provinces with a population of seven million3, and more than 800 distinctive, mutually unintelligible languages, each representing a distinct culture4. An estimated 87% of the population lives in rural areas and is partially or substantially living a subsistence lifestyle5. Despite a rapid shift towards economic development and modernisation, traditional beliefs around sorcery and witchery are still deeply ingrained6. Deaths and mysterious illnesses can be blamed on suspected sorcerers, and every year many alleged sorcerers, many of whom are women, are injured or killed7. Beliefs in the power of sorcery remain 'culturally embedded' despite national policies and a Sorcery Act (1971) which explicitly forbids the use of sorcery for evil8,9. The country's rugged, mountainous terrain and far-flung island provinces account for the uneven distribution of resources and services such as transport and health. The remoteness and isolation of even major population centres adds to the difficulties of conducting programs in PNG, including those relating to eye health.
PNG's high rates of vision impairment (29%) and blindness (3.9-8.9%) in older adults are primarily due to uncorrected refractive error and cataract2, which can be simply treated with either a pair of spectacles or corrective surgery. Human resources for eye care are extremely limited in PNG. There are currently six ophthalmologists and five optometrists to provide eye care for the entire population10, and most eyecare facilities are located in urban areas (the majority in the capital Port Moresby), leaving rural people with limited access to eye care. Development of eye health infrastructure and service delivery in PNG has been hindered by a lack of medical supplies (surgical supplies and spectacles), poorly maintained medical equipment and a general lack of quality facilities.
While structural determinants such as gender, social class, socioeconomic and political factors impact access to health services, intermediary determinants such as psychosocial factors, behaviours, perceptions, beliefs, experiences and lifestyle choices also shape an individual's capability to access services and achieve good health11,12. Although there have been some examinations of awareness and utilisation of eyecare services in nearby countries13-15, and recent studies investigating vision-specific quality of life16, and perceptions of eye health and eye health services17, these studies have not considered the emotional aspects or social context of vision impairment or the intermediary determinants of health that shape access to service.
The purpose of this article is to examine the experiences, beliefs, perceptions and feelings related to vision impairment in adults in PNG. For health providers, understanding these influences and an individual's behaviour may assist in improving access to services, making programs more appropriate and effective in this challenging environment.
This study used in-depth interviews and both purposive and convenience sampling to explore beliefs and experiences of vision impairment in five provinces representing culturally and geographically diverse regions of PNG. Eastern Highlands and Enga provinces are two densely population provinces in the Highlands region with rugged mountainous terrain; Oro (Northern) Province is a coastal province with scattered villages and very few roads; Central Province is located on the Southern coast and is relatively well serviced by roads; and the National Capital District encompasses Port Moresby, the capital and largest city in PNG. Community leaders helped identify and recruit participants aged more than 18 years who had either vision impairment or a family member with vision impairment or were eye health service providers. Interviews were conducted over a 10-month period in 2010, by a local anthropologist (YH) fluent in Tok Pisin, Hiri Motu and English. Interviews took place in the participant's home, a nearby clinic, an outreach service or the outpatient's eye clinic at Port Moresby General Hospital.
The interview guide comprised open-ended questions exploring how vision impairment affects daily life. Participants with vision impairment were asked about their own experiences of vision impairment, and those without vision impairment were asked about their family members. Eye health service providers were similarly asked about the main causes of vision impairment in PNG, how they believe vision impairment impacts people's daily life and the challenges of providing eye care in PNG. Interviews were conducted in Tok Pisin, Hiri Motu or English according to the participant's preference and hand-recorded. Quotes used in this article are in the language or words used directly by the participants.
Grounded theory was used to elicit key themes from interview data. Data were open coded and analysed inductively by authors AY and MCA using NVivo v10.0 (QSR International Pty Ltd; http://www.qsrinternational.com/nvivo-product). The primary codes were reviewed to identify emerging themes and reach agreement on a thematic framework (Fig1) before data were analysed again using axial coding. AB and MY reviewed the coded data and original transcripts to revise the thematic framework and confirm that no new themes had emerged. Minor revisions were made to the framework until agreement was reached.

Figure 1: Thematic framework: experiences of vision impairment in Papua New Guinea.
Ethics approval
This study received ethics approval from the Government of PNG, National Department of Health Medical Research Advisory Committee (MRAC ethics approval number 09.07) and the Vision Cooperative Research Centre and Institute for Eye Research Human Ethics Committee, Sydney (VIHEC ethics approval number 09/14). Written informed consent, or verbal informed consent (participants with vision impairment or no formal education) was obtained from participants.
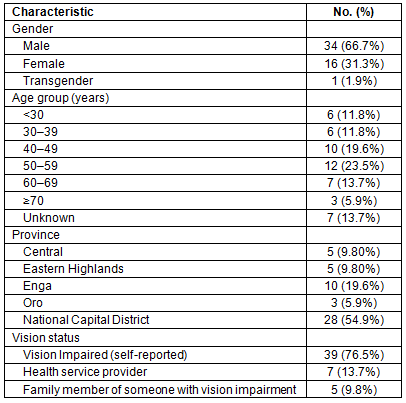
The demographic characteristics of the participants are shown in Table 1. Two-thirds of participants were male (67%), and more than 20% of participants were aged 50-59 years. The majority of participants came from the National Capitol District (55%) and experienced vision impairment (self-reported: 77%).
Table 1: Demographics of participants (n=51)
Beliefs and perceptions about the causes of vision impairment
The most common beliefs and perceptions around the causes of vision impairment were environmental factors, injury and sorcery/witchcraft (Table 2).
More than one-third of all participants identified environmental factors such as the sun, dust, dirt and smoke as contributing factors or the causes of vision impairment. One female participant (participant 22, aged 30-40 years) said that when the sun is really hot, especially in the mornings, her vision gets really dark, 'eye tutak', and tears fall from her eyes. Others complained of blurry vision or watering eyes due to the hot sun and one (participant 51) stated that his eyes 'go blackout' when the sun is really hot and he loses vision completely. Others linked exposure to foreign bodies (dust, ash and smoke) with domestic duties such as cleaning, gardening and burning fires (for cooking, rubbish management and lighting).
Events that involved injury to the eye were reported frequently; intentional violent acts that resulted in eye injury were mentioned exclusively by female participants.
Beliefs in sorcery and witchcraft remain ubiquitous in Papua New Guinean society. Twenty per cent of participants (n=10) believed that vision impairment could be a result of sorcery or witchcraft, believing that a perpetrator is seeking to 'spoil' their eyes in order to seek revenge, or punish them. Participant 24 described how a female relative had 'spoilt' her eyes because (the participant) did not bring any gifts from the city. She stated that the perpetrator's reason was 'eye i mekim olsem na em hamamas na kalap lo balus na raun nabaut' - meaning that because (the participant's) eyes were healthy she was able to travel comfortably in a plane and so if they were 'spoilt' she could no longer travel comfortably and she would be unhappy for the rest of her life. The participant stated that after the event she experienced blurry vision and ocular discomfort. Participant 1 told the story of an elderly couple who were known as exceptional gardeners. A 'jealous' person had stolen their sweat towel to 'spoil them'. The couple both suffered from vision impairment and consequently stopped gardening. The couple visited a traditional healer who was unable to help them, then eventually visited the hospital and were diagnosed with cataracts. They underwent successful surgery; however, despite regaining their vision the couple no longer garden. Other metaphysical occurrences were also described, where falling tears were a prophecy that someone is going to die (participant 5). Prayer and attendance at church was used by two participants to explain vision recovery.
The prioritisation of eye health, including a person's decisiveness or ability to seek appropriate care, was often related to the development or worsening of vision impairment. Four participants stated that work, social obligations and a lack of time were reasons why people did not visit an eye clinic. Three others suggested that 'laziness' or 'attitude problems' were the reason why their family or fellow community members did not seek care when they had a problem, and that it was a person's own fault if they did not seek eye care and their vision worsened.
Some participants (n=8) stated that vision impairment was a natural part of ageing, and they had a fatalistic approach to vision impairment. For instance, participant 31 stated that as he ages he will naturally begin experiencing vision problems because as people age they 'wind down'.
Diet was perceived by some participants (n=6) to both negatively and positively influence both vision impairment and general eye health, with the transition from traditional foods to 'store foods' and fewer vegetables identified as a contributor to vision impairment. However, consumption of carrots was identified as a contributor to good vision.
Some participants (n=4) believed that substance abuse (drinking methanol or homebrew, and smoking) can cause vision impairment, and participant 11 confirmed that his own consumption of methanol had caused him to go blind. Additionally, the traditional practice of chewing betel nut, a mild stimulant popular in PNG, was also perceived to be a contributing factor to vision impairment, as the lime can get into eyes, particularly for babies who are being held by adults.
Table 2: Participant beliefs and perceptions about the causes of vision impairment

Impact of vision impairment on daily life
The impact of vision impairment on daily life was explored (Table 3) according to the thematic framework (Fig1). Restrictions to reading due to vision impairment were common among participants, particularly for women. Participants had the most difficulty with reading the bible and newspapers, followed by reading words or numerals on money, watches, food items, computers, mobile phones and automatic teller machine screens.
Vision impairment impacted the ability of many participants to recognise people's faces, and over 40% of both the women and the men said that they have difficulty recognising faces. In some cases this had resulted in others being upset or angry with them for failing to recognise people; in others it resulted in fear of being unable to recognise an approaching enemy (participant 28).
Most participants with vision impairment provided a variety of stories, describing how vision impairment had made basic daily tasks (eating, gathering food, walking, driving and using the toilet) difficult or unachievable. In some cases participants described how their inability to undertake basic tasks had created a high level of dependency on others. In all of these cases, the participant's family took responsibility for assisting the participant in the undertaking of basic tasks.
Two male participants described how vision impairment had led them to unemployment, while others described how their vision impairment made it very difficult for them to do their job, but that they are unable to leave or retire because they still needed to provide for their dependants.
Routine domestic duties such as repairing traditional wooden stilt houses and growing food are necessary for survival in PNG. The male participants described how vision impairment had affected their own ability to undertake these duties, and the impact it would have for those living in traditional stilted houses that are built over the sea. For women in PNG, sewing is a skill used in paid employment, daily domestic tasks, and in making clothes and handicrafts such as bilums (traditional woven bags) to sell. Nearly half of the female participants (44%) identified sewing as a task they struggled with due to vision impairment.
Table 3: Beliefs and perceptions about impact of vision impairment on daily life

Emotional experiences of vision impairment
Emotional responses were grouped according to the thematic framework (Fig1) in order to further understand the PNG specific social context and emotional implications of vision impairment (Table 4). Worry and/or fear as a result of vision impairment was mentioned by over 50% of both the female and male participants, and was associated with a person's ability to complete basic tasks, identify people, fulfil job requirements and participate in religious/spiritual prayer or rituals. Vision impairment had caused some participants to be fearful and afraid for their safety - from fears about being unable to recognise an approaching enemy, to fears about being bumped by a vehicle while walking on the side of the road.
Several participants (n=7) reported that vision impairment results in feelings of hopelessness. They went on to explain how vision impairment prevented them from participating in an active lifestyle, and undertaking simple domestic duties. In a number of cases people reported that they had just 'given up'.
Exclusion and shame were often spoken about interdependently, and were characterised by situations where participants felt excluded due to vision impairment.
In other cases shame was attributed to spectacle use, particularly for the female participants. Some women noted that they were concerned about wearing either spectacles or sunglasses as they feared that others would be jealous of them, as sunglasses can be a proxy indicator of wealth or status. One participant defined jealous behaviour as a characteristic of 'highlanders'.
Table 4: Emotional impact on participants of vision impairment

Discussion
This is the first study that has provided an in-depth investigation of the perceptions and emotional reactions to vision impairment in PNG. Asking participants to respond in their own words has revealed beliefs and perceptions of the causes of vision impairment, the emotional impact of vision impairment, and presented information about the social context.
Refractive error and cataract are the two leading causes of vision impairment among adults aged more than 50 years in PNG2. While participants in this study were somewhat aware of the impact of environment, nutrition, ageing and substance abuse, medical causes (eg cataract, refractive error, diabetic retinopathy) were rarely mentioned, if at all.
Subsistence agriculture remains a main source of food and income in PNG, particularly in rural and remote villages. Participants reported how their vision impairment restricts their gardening, farming and income-generating activities. Equally, participants identified environmental stressors as one of the main causes of vision impairment. Currently, eye health services in PNG do not have significant preventative eye health components. Incorporating environmental education programs, such as those used successfully with migrant agricultural workers18,19, may help to improve awareness and result in greater eye protection. Although there are likely to be greater challenges in reaching subsistence farmers in PNG, further research may evaluate the efficacy of routine preventative eyecare safety messages, as well as the acceptability and feasibility of safety eye wear and sun protection. However, any health promotion campaign to increase sun protection via sunglasses would need to carefully evaluate any unintended negative consequences for participants due to the social response to wearing sunglasses, as expressed by some of the female participants in the present study, and similar to a previous investigation into the perceptions of eye health services in PNG17.
Previous studies in PNG have identified physical abuse and foreign bodies as the leading causes of ocular injury20. Widespread and entrenched gender inequity in PNG leaves girls and women particularly vulnerable to abuse, exploitation and violence21, as reflected in female participants' stories of eye injury. Ongoing action at the government and civil society level is needed to address structural factors that support gender-related violence.
Some participants in this study believed that they had been a victim of sorcery or witchcraft and had experienced vision impairment as a result. Persisting beliefs in sorcery and witchcraft influence treatment-seeking behaviour, and acceptance of conventional treatment17,22,23. In the absence of scientific or naturalistic explanations, Papua New Guineans commonly use sorcery and witchcraft as a traditional sociomedical belief system to place meaning around injury, sickness and death. Acquiring wealth can fuel the hostility behind accusations of sorcery24(p.195). The story of the elderly gardening couple exemplifies the depth and complexity of belief in sorcery and the way it can shape an explanatory model for physical impairment and illness. Persisting beliefs in sorcery/witchcraft need to be considered when developing culturally appropriate eye health promotion and education information.
Chewing betel nut is a widespread practice in PNG - one study found up to 94% of pregnant women continued to chew betel nut during pregnancy25, an area of health service delivery that has been identified as needing improvement in PNG26. Participants in this study reported instances where 'lime' (calcium hydroxide used in conjunction with betel nut) has entered babies' eyes, supporting previous studies identifying lime burns as a common cause of ocular injury in infants in PNG20. Further investigation to assess the need for antenatal counselling messages about the dangers of chewing betel nut while holding infants is suggested, as participants have identified here.
In this study, participants have recounted how vision impairment affects their lives and the lives of their family members. Restrictions range from everyday activities such as sewing, mending houses and reading the bible, through to restrictions of fundamental social interactions such as recognising faces. Additionally, the emotional perspectives of people with vision impairment have been investigated in order to explore quality of life, the person's needs, and provide some understanding into the relationship between people with vision impairment and their caregivers. Although no participants spoke directly of depression, 'worry', 'sadness' and 'exclusion' were all commonly reported. The link between vision impairment and depression or other emotional disturbances (for instance lower well-being) is well documented27,28 ; however, social supports can provide a buffer against depression.
An overwhelming majority of the population in PNG is rural, people tend to live in villages with close relatives21 (p.225). and these close kinship systems have been identified as a strength in terms of health, especially for women26. For people with vision impairment, the support provided by these kinships systems can be vital for meeting everyday needs. Yet vision impairment can create social exclusion and jeopardise these social supports.
Participants' stories also connected social exclusion to the perceived effects of spectacle use. To lessen the negative social and emotional impacts of vision impairment, eye health services providers must cultivate linkages with other emotional wellbeing, counselling and support services. Additionally, further explorations of the negative social implications of spectacle use in PNG are warranted.
As this study obtained the views of participants using convenience sampling from five areas, caution must be exercised about using the concepts gathered here to inform eye health services in other areas of PNG as the responses cannot be assumed to be representative of the population. There was also an over-representation of men (67%) - the lack of female voices meant that gender-specific views on vision impairment were unable to be explored.
The accuracy of the note-taking process and translations may have been improved by using audio- or video-recording and professional translators. However, it is anticipated that the impact of this will be minimal since the trilingual interviewer was well practiced in taking detailed notes and working in a diverse language environment.
In the PNG context there are a multitude of structural determinants that challenge the development of effective health services. Despite these challenges, eye health service providers in PNG must also consider behaviours, perceptions, beliefs and experiences, which impact a person's capability to access services and achieve good eye health.
By providing information on the beliefs, perceptions and emotional reactions to vision impairment in five provinces in PNG, this study has provided knowledge that health services can use to make programs more appropriate and effective in this challenging environment. The findings will allow planning and adaptation of eye health services to better inform the population, promote eye health awareness and reveal how eye health services in PNG could better provide appropriate care, all with the goal of reducing avoidable vision impairment in PNG.
Acknowledgements
The authors acknowledge PNG Eye Care for providing on-ground logistic support. This study was supported by an Avoidable Blindness Initiative research grant through the Department of Foreign Affairs and Trade, Australian Government.
References
1. Pascolini D, Mariotti S. Global estimates of visual impairment: 2010. British Journal of Ophthalmology 2012; 96(5): 614-618.
2. Garap JN, Sheeladevi S, Shamanna BR, Nirmalan PK, Brian G, Williams C. Blindness and vision impairment in the elderly of Papua New Guinea. Clinical & Experimental Ophthalmology 2006; 34(4): 335-341.
3. National Statistical Office of Papua New Guinea. 2011 National Population and Housing Census of Papua New Guinea. Port Moresby: National Statistical Office, 2011.
4. World Health Organization. Western Pacific country health information profiles 2011 revision. Philippines: World Health Organization, Western Pacific Region, 2011.
5. National Statistical Office of Papua New Guinea and ORC Macro. Demographic and health survey 2006. Port Moresby and Calverton, Maryland, USA: National Statistical Office and ORC Macro, 2009.
6. Kuman G. Sorcery, witchcraft and development in Papua New Guinea. Catalyst 2011; 41(1): 19-37.
7. Manjoo R. Report of the Special Rapporteur on violence against women, its causes and consequences. United Nations General Assembly, Human Rights Council. Geneva: Human Rights Council, 2012.
8. World Health Organization, National Department of Health Papua New Guinea. Health service delivery profile: Papua New Guinea. Philippines: World Health Organization, 2012.
9. Robinson N. Statement on sorcery-related killings and impunity in Papua New Guinea. Sorcery and Witchcraft-related Killings in Melanesia: Culture, Law and Human Rights Perspectives Conference. Canberra: Office of the United Nations High Commissioner for Human Rights, 2013.
10. International Agency for the Prevention of Blindness Western Pacific Region. Western Pacific regional update and country profiles. Philippines: International Agency for the Prevention of Blindness, 2013.
11. Sen A. Why health equity? Health Economics 2002; 11(8): 659-666.
12. Solar O, Irwin A. A conceptual frameword for action on the social determinants of health. Social determinants of health discussion paper 2 (policy and practice). Geneva: World Health Organization, 20010.
13. Brian G, Maher L, Ramke J, Palagyi A. Eye care in fiji: a population-based study of use and barriers. Ophthalmic Epidemiology 2012; 19(2): 43-51.
14. Palagyi A, Ramke J, du Toit R, Brian G. Eye care in Timor-Leste: a population-based study of utilization and barriers. Clinical & Experimental Ophthalmology 2008; 36(1): 47-53.
15. du Toit R, Ramke J, Naduvilath T, Brian G. Awareness and use of eye care services in Fiji. Ophthalmic Epidemiology 2006; 13(5): 309-320.
16. Paudel P, Khadka J, Burnett A, Hani Y, Naduvilath T, Fricke TR. Papua New Guinea vision-specific quality of life questionnaire: a new patient-reported outcome instrument to assess the impact of impaired vision. Clinical & Experimental Ophthalmology 2015; 43(3): 202-213.
17. Burnett A, Yu M, Paudel P, Naduvilath T, Fricke T, Hani Y, et al. Perceptions of eye health and eye health services among adults attending outreach eye care clinics in Papua New Guinea. Ophthalmic Epidemiology 2015; 22(6): 361-369.
18. Forst L, Lacey S, Chen HY, Jimenez R, Bauer S, Skinner S, et al. Effectiveness of community health workers for promoting use of safety eyewear by Latino farm workers. American Journal of Industrial Medicine 2004; 46(6): 607-613.
19. Luque JS, Monaghan P, Contreras RB, August E, Baldwin JA, Bryant CA, et al. Implementation evaluation of a culturally competent eye injury prevention program for citrus workers in a Florida migrant community. Progress in Community Health Partnerships: Research, Education, and Action. 2007;1(4):359-369.
20. Verma N, Verma A, Jacob G, Demok S. Profile of ocular trauma in Papua New Guinea. Australian and New Zealand Journal of Ophthalmology 1997; 25(2): 151-155.
21. Hinton R, Earnest J. Stressors, coping, and social support among women in Papua New Guinea. Qualitative Health Research 2010; 20(2): 224-238.
22. Macfarlane JE, Alpers MP. Treatment-seeking behaviour among the Nasioi people of Bougainville: choosing between traditional and western medicine. Ethnicity and Health 2009; 14(2): 147-168.
23. Byford J, Veenstra N. The importance of cultural factors in the planning of rehabilitation services in a remote area of Papua New Guinea. Disability and Rehabilitation 2004; 26(3): 166-175.
24. Zocca F. Gender and accusations of malevolent sorcery and witchcraft in Papua New Guinea. Catalyst 2010; 40(2): 192.
25. Senn M, Baiwog F, Winmai J, Mueller I, Rogerson S, Senn N. Betel nut chewing during pregnancy, Madang province, Papua New Guinea. Drug and Alcohol Dependence 2009; 105(1): 126-131.
26. Larsen GL, Lupiwa S, Kave HP, Gillieatt S, Alpers MP. Antenatal care in Goroka: issues and perceptions. Papua New Guinea Medical Journal 2004; 47(3/4): 202.
27. Thurston M. An inquiry into the emotional impact of sight loss and the counselling experiences and needs of blind and partially sighted people. Counselling and Psychotherapy Research 2010; 10(1): 3-12.
28. De Leo D, Hickey PA, Meneghel G, Cantor CH. Blindness, fear of sight loss, and suicide. Psychosomatics 1999; 40(4): 339-344.

