Maldistribution of the primary care workforce remains a key problem characterising geographically large countries like Australia and the USA1-3. As a result, residents of many rural communities continue to experience difficulty accessing primary care doctors (that is, general practitioners (GPs) in Australia, or primary care physicians in the USA) at times of need. Increasingly too, graduates are choosing medical specialities over generalist roles, further compounding the difficulties in recruiting and retaining rural primary care doctors4,5. Nonetheless, professional satisfaction is often high amongst existing rural primary care doctors6, with many rural communities serviced by long-standing doctors7,8.
The supply of primary care doctors in rural communities is dynamic and linked to both the current 'stocks' of doctors and subsequent recruitment and retention levels. Although much research has identified key professional factors relating to recruitment and retention of rural primary care doctors (such as expected or experienced longer work hours, professional isolation, locum relief difficulties and afterhours workload)9-12, less attention has been given to the role of community and place factors on supply13. Doctors' location decisions likely relate to both meeting their professional needs and interests, as well as non-professional satisfaction through, amongst other aspects, various place-related attributes. Conceptually, these latter attributes reflect a community's overall amenity or attractiveness, which arguably influences both rural recruitment and retention relocation decisions14-17.
The amenity of a rural community is a complex and somewhat subjective concept but demographers have demonstrated it to be associated with general population location decisions and migration patterns within and between rural and urban areas17-19. This includes the contribution of a perceived or actual lack of amenity to long-term net out-migration (population loss), for example with households spurning colder climates and more isolated locations20, and places that are poorly endowed with employment opportunities. Given that most doctors work in close proximity to their place of residence, the availability of rural primary care doctors is also likely less problematic in more attractive or 'amenity-rich' regions while low-amenity locations may also be areas where rural doctors prefer not to work.
Several recruitment studies have investigated the role of place characteristics and attractiveness for rural health worker location decisions. One survey of US rural hospital CEOs found that the prime factor associated with staff recruitment was whether their place of residence and employment was a good place to raise their family - notably, that it was safe and had good schools21. Similarly, in Australia doctors considering rural practice want good access to public amenities and spouse employment opportunities22, and a key deterrent to rural practice is the isolation and reduced social interaction opportunities associated with residing in small and inland communities11.
Demographers have demonstrated a significant association between increased community amenity and net in-migration (overall gains in population) to rural areas14,23,24. However, little is known about the extent to which the specific location decisions of doctors are also influenced by amenity, with one Australian study only finding a very weak association between community-level GP shortage and indicators of 'rural amenity'25. The present international study uses Australian and US data to redress this gap in the literature, investigating the extent to which variations in indicators of community amenity are associated with spatial variations in the supply of rural primary care doctors.
Dimensions of community amenity
Measures from two separate dimensions of community amenity: geographic aspects of location, specifically isolation/proximity; and economic and sociodemographic aspects were included in this study, while an indirect (proxy) measure of a third dimension, environmental amenity, was also included. Each community was primarily defined by the respective governing boundaries, combining both town boundaries and other nearby sparsely populated settlements, while a secondary definition used only the town boundaries. Analysis was limited to constructing a set of community amenity measures from readily available small-area national-level datasets, with the different indicators of amenity selected on the basis of the literature.
The first dimension, isolation from professional and non-professional support and services, remains a key element of working and living as a rural doctor. Reduced population density and increased distance to major urban areas have been shown to be dominant reasons for lower rural in-migration in the general population19. Being located near to both a hospital and larger metropolitan areas are important to doctors9. Similarly, good access to schools and water-based recreation are desirable6,11, while isolation through long commuting travel or living in remote areas are less desirable. Practising in small rural communities can bring additional risk to practice viability if insufficient demand occurs26. Isolation is particularly difficult for those communities that have limited natural amenities27 or lack other professional work opportunities, such that young adults move away to seek better employment opportunities for themselves and their spouses26. This contrasts with population growth evident in Australian coastal communities18 or regions with key services and infrastructure such as easy access to air travel28.
Second, the economic and sociodemographic profile of a community influences its attractiveness to providers. On the one hand, although lower house prices and reduced cost of living may enhance attractiveness to some, this may be less important to doctors who typically earn well above average incomes. In contrast, lower house prices and incomes often reflect rural areas that are either in decline or experiencing poor economic growth29, particularly in more isolated rural communities17,18. More prosperous rural regions tend to have more educated populations and increased economic diversity30. The specific demographic composition of a community including the numbers of elderly, unemployed or indigenous people may influence doctors' decision making particularly with respect to locating their practices in socioeconomically deprived communities that may threaten practice economic viability25,31. Hence, when choosing between locations, more affluent rural locations will be preferred by most doctors30,32.
A third dimension, environmental amenity, which predominantly captures aspects of climate, was not explicitly included in this study. Geographers have identified a number of physical characteristics that enhance the attractiveness of specific rural locations as places to live33, including warmer winters, temperate and low-humidity summers, moderate rainfall, varying landscape and ready access to water recreation14,23,34. This dimension was not included for specific locations in the analysis chiefly because climate has strong spatial autocorrelation between adjacent locations, thus fails the requirement for independence within regression models and is not likely to be sensitive to small-area differences of supply. Additionally, climate and topography can't be readily addressed through policy. Instead, environmental amenity is indirectly captured by including jurisdictions (states and territories) in all analyses.
Community amenity indicators
The full list of indicators of community amenity included in this study are summarised in Table 1. Data were collated from the American Community Survey (2011), Robert Wood Johnson Foundation (2014) and the Australian Census of Population and Housing (2011). Proximity measurements were calculated using straight-line distances between locations/communities using ArcGIS v9 software (ESRI; http://www.esri.com/arcgis).
Table 1: Indicators of rural community amenity used in this study
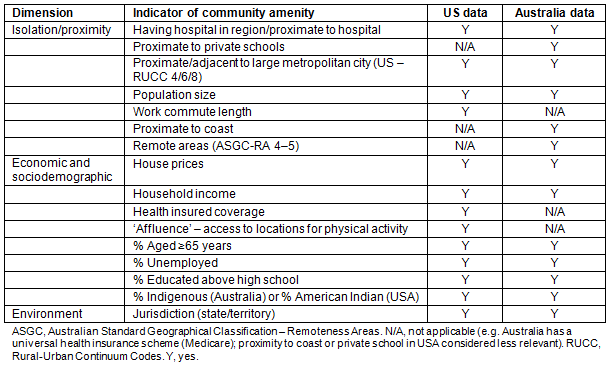
Measures of workforce supply
For this study, provider-to-population ratios (PPRs) were calculated for both the USA and Australia, with PPRs underpinning key policy measures including the US's Medically Underserved Areas and Health Professional Shortage Areas, and Australia's District of Workforce Shortage Areas and Areas of Need35,36. There were 1949 rural counties in the USA (geocoded in 2010, defined by Rural-Urban Continuum Codes 4-9, average county population about 23 000) and 370 rural local government areas (LGAs) in Australia (geocoded in 2011, defined by Australian Standard Geographical Classification - Remoteness Areas 2-5, excluding LGAs that contain cities of >50 000 population and those without an urban area of >500 population, average LGA population about 12 000). US primary care physician head counts (family physicians, general pediatricians and general internists) were drawn from the 2014 American Medical Association Masterfile, while Australian primary care workforce data (full-time equivalence counts) were drawn from the 2012 Australian Government's Medicare Benefits Schedule dataset for all billing GPs.
Despite their wide usage, PPRs are criticised for their use of pre-defined boundaries and assumption that all service utilisation occurs within these impassable boundaries, but the geographical barrier within boundaries is negligible37,38. This has led to the recent development of the two-step floating catchment area (2SFCA) method, which uses catchments that are centred on population and service locations, and accounts for distance decay and relative need39-42. However, the 2SFCA method has not been developed nationally in the USA and was only recently completed at the national level for Australia43. This study uses the latter method as an alternative measure of workforce supply in all 1116 Australian rural towns with populations between 500 and 50 000 residents, using the same GP billing dataset, with a 2011 study finding strong results with this approach when tested in a single state25.
Statistical analysis
The associations between workforce supply and community amenity indicators were initially \ calculating using Pearson's correlations, where increasingly positive scores suggest increased supply. Ordinary least squares multiple linear regression models were then constructed for each of the three supply outcome measures. All statistical models included jurisdiction (state/territory) as a covariate (capturing differences related, for example, to climate and state-level policies not otherwise measured in this study); however, these effect sizes are not reported. Population size weights were applied to all statistical models. All calculations were performed using either StataMP v13.1 for US data or StataSE v12 for Australian data (StataCorp, http://www.stata.com/) and a 5% significance level was used throughout.
Ethics approval
Ethics approval was not required because only publicly accessible existing collections of non-identifiable aggregated data were used in this research.
Table 2 summarises the strength of association between community amenity (as measured by the above indicators), and each of the three supply measures. Increased population size and having a nearby hospital are consistently positively associated with improved medical workforce supply (that is, regions without a local hospital also have poorer primary care supply). Additionally, communities with better educated residents, increased house prices, located near to the coast (Australia) and private schools (Australia), or with higher affluence (USA) were also associated with improved medical workforce supply. In contrast, communities that are most isolated in remote Australia or characterised with long work commutes (USA) and located in 'adjacent rural' areas (USA) had poor supply. The respective medical insurance systems appear to be associated with opposite supply levels, with Australia having higher supply in communities whose populations are older, and characterised by more unemployed residents or with poorer income, while the USA sees poorer supply in communities with similar population characteristics.
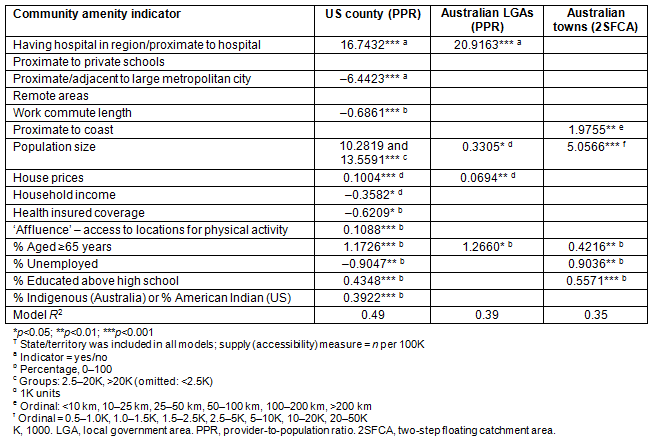
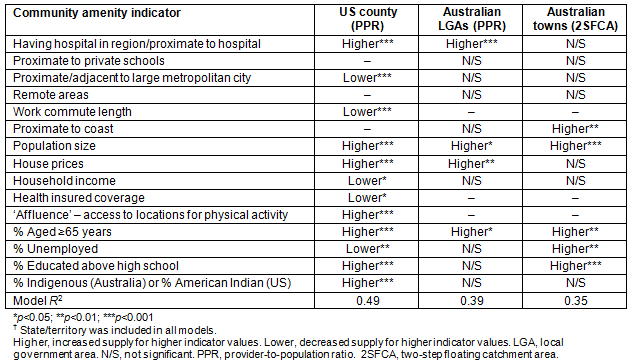
Table 3 summarises the association between indicators of rural community amenity and each supply measure using multiple linear regression models. (Full model details are shown in Appendix A.)
All amenity indicators were significantly associated with supply of the primary care workforce in US counties. Household income has a negative association with supply (a higher income is associated with poorer supply). Population size, having a hospital in the county, house prices and affluence, education level, being American Indian and population age were all strongly positively associated (p<0.001) with improved workforce supply. In contrast, rural counties 'adjacent' to metropolitan cities, those with longer work commutes and regions with increased unemployed populations were all associated (p<0.01) with poorer workforce supply. This US model, in combination with state effects, captures almost half of the observed variation in PPR scores across all rural counties. Both Australian models captured a smaller proportion of the observed variation in supply. Indicators consistently associated with significantly improved supply in both countries include having a hospital in the region, larger population size of the main town in region, more elderly residents, higher education levels and increased housing prices in the region. The proportion of the population unemployed was significantly associated with supply in both Australia and USA; however, their associations were in opposite directions.
Table 2: Correlations between supply and indicators of community amenity
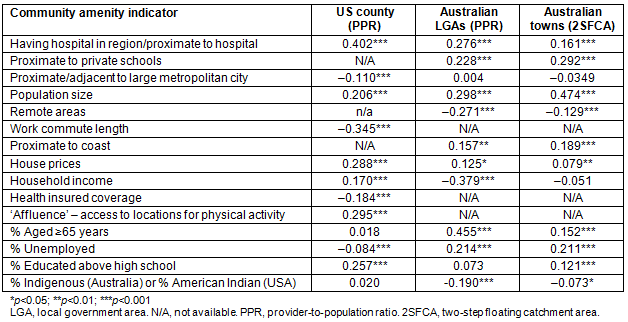
Table 3: Summary of multivariate linear regression models? of rural supply
Discussion
This study provides key empirical evidence of the extent to which community amenity contributes to differences in the supply of rural primary care doctors in both Australia and the US. Overall, these data support the idea that the distribution of the rural medical workforce is skewed towards more affluent and educated areas, and away from smaller, poorer and more isolated rural towns which struggle to attract adequate primary care services. Rural communities are often idealised as offering high local amenity, including good recreational opportunities, a wealth of natural environmental attributes, improved lifestyle and close-knit supportive communities44-46. However, these community characteristics often go hand-in-hand with characteristics that are less attractive to doctors, such as relative isolation, poorer access to other desirable services and professional opportunities, and the lack of anonymity in small communities46.
This study revealed clear and statistically significant positive associations between workforce supply and having a hospital nearby. This finding highlights the challenges in retaining doctors in communities where the infrastructure of a local hospital is absent or where a strong peer support network is not readily available47. Working in such places can limit opportunities for professional support and collegiality, limit sharing of workload (especially on-call/after-hours work) and increase the difficulty of taking time-off. The absence of a local hospital additionally limits the scope of practice, for example by reducing opportunities to participate in procedural work like obstetrics or emergency medicine.
A strong positive association between workforce supply and the population size of rural communities was also revealed by this study. This finding tends to broadly support the Australian government's shift towards considering community size in addition to geographic remoteness in recent rural medical workforce policy changes. This is exemplified through the government's move to adopt the Modified Monash Model to guide the allocation of GP rural retention incentives rather than the Australian Standard Geographical Classification - Remoteness Areas48,49.
Increased supply of rural doctors was also found to be associated with better serviced/more affluent regions. Economists argue that house prices are a strong indicator of a location's attraction50, consistent with the finding that doctors were also more likely to work in rural areas with higher housing prices across both countries. Doctors are among the top income-earners in both countries and, as such, their preference for more attractive locations for residence and tendency to pay the higher housing premium is not surprising. The US measure of county affluence was also significantly associated with increased doctor supply. While access to other services such as shopping, employment, cultural and other recreational opportunities was not directly measured, it is known that these services are all strongly related to population size51 . Additionally, while poorer access to schools was not significant within the Australian models, this measure is strongly correlated with population size and shown to be a major reason for dissatisfaction of doctors living in smaller rural areas or not taking up rural practice in the first instance6,9,26 .
Australia and the USA share geographical similarities, being large in size (7.8 and 9.8 million km2 respectively), and both with vast areas characterised by very low population densities. Notably, Australia's population hierarchy is largely centred on a few coastal metropolitan cities (63% of Australia's population live in six coastal capital cities, with some capitals containing more than two-thirds of its state's population), while other 'regional centres' are mostly only 5-10% of the population size of the largest metropolitan city in that state. The attraction of a coastal location is also well recognised within Australian rural migration literature14 , and this too was reflected in the increased doctor supply observed in coastal towns. In contrast, the US settlement hierarchy exhibits significantly less urban primacy, with most states having multiple regional/urban cities that constitute 25-80% of the population size of the largest metropolitan city in that state, while on a national scale the coast provides only minor amenity. Rural US counties that fall between, or are adjacent to, the larger service centres are those where commuting distances are longer, so it follows that supply of doctors is poorer in these outlying locations. While remote areas of Australia are associated with poorer medical workforce availability, this was not reflected in the multiple regression models, largely due to collinearity with coastal proximity, population size, education levels and the proportion of elderly in the population.
Locations with a high percentage of elderly residents were consistently associated with significantly higher workforce supply. This age cohort is by far the largest user of primary care, so it should not be surprising that primary care workforce supply is higher in such communities. What can't be measured by this study, however, is the greater health needs (demands) of this cohort, so it is difficult to tell whether the higher workforce supply scales with their increased needs, and whether this is an attraction for rural doctors. Similarly, Australia's Indigenous populations and US's American Indian populations are concentrated more in smaller communities located throughout rural and remote regions, and have significantly higher health needs than the general Australian or American population. However, indigeneity has a non-significant (Australian) or negative (US) association with supply despite the increased health needs of these indigenous populations.
Not having a universal access medical insurance system places particular importance on the ability of patients to pay within US primary care doctor's location decisions. It is not surprising that supply levels were significantly lower in rural areas with more uninsured residents. However, associations between other socioeconomic and sociodemographic amenity indicators and supply are less consistent, with household income and unemployment having contrasting associations with supply when comparing the two countries. Supply was higher in locations with more residents educated above high school in both countries, although this study cannot determine how this makes a location more attractive to doctors.
In addition to PPRs for both countries, this study tested the 2SFCA method in Australia (it was not available for the USA). While this method is becoming increasingly popular to measure spatial accessibility in preference to PPRs, the set of attractiveness measures were the least predictive with this model (R2=0.35). The 2SFCA method places a larger emphasis on proximity and is thus sensitive to small-area (community-level) differences of supply accessibility; however, place attractiveness may be more homogeneous at the regional level, thus minimising the benefit of a community-level approach. Uptake of the 2SFCA method continues to grow worldwide, although the present study's results suggest that its additional small-area sensitivity may not always be advantageous.
A key limitation of this study is that professional factors have not been directly considered as predictors of workforce supply. While population size and having a nearby hospital may indirectly reflect professional factors, there were no direct measures included in the study such as a lack of procedural work, onerous on-call arrangements, difficulties in getting locum relief, inadequate workforce mix and poor infrastructure. This is relevant for future research, as little is known about whether various indicators of community amenity outweigh professional factors in location decision making of doctors. It is also acknowledge that many of the included indicators of community amenity are more complex than what this study captured. For example, all schools and hospitals were assumed to be homogeneous, but in reality often vary greatly in size, composition and quality. Other limitations include an assumption throughout this article that higher supply is always better, although it is possible for some rural communities to be oversupplied, while the use of head count (USA) and full-time equivalence (Australia) data may have contributed to small differences between countries. In addition, supply is only one measure of workforce distribution, with turnover, retention and continuity of care being important alternative measures, especially for remote areas and marginalised groups47 . Finally, while some spatial autocorrelation is present, an assessment of model residuals using Moran's I was not statistically significant.
Continued maldistribution of the rural primary care workforce suggests that current policies and solutions are not entirely effective in the quest to overcome workforce shortages and inequitable access to primary care. This study highlights that rural medical workforce distribution is skewed towards more affluent and educated areas, whereas smaller and more isolated rural towns continue to struggle to attract adequate supply of primary care services. 'Rural' is frequently assumed to be homogeneous in much rural health workforce research and policy, but this can overlook major differences of place. In addition, most rural medical workforce policies continue to only target professional issues (such as improved after-hours support or locum relief), whereas improved community amenity for doctors likely depends upon broader regional development initiatives including local community infrastructure (such as housing, schools, health facilities and transport). Improved evidence-based planning should differentiate between locations better in order to better target workforce incentives and interventions to the most problematic locations. Future primary care workforce policies need to place a greater focus on rural communities that, for a variety of reasons, may be less attractive to doctors.
Acknowledgements
The research reported in this article is a project of the Centre of Research Excellence in accessible and equitable primary health service provision in rural and remote Australia funded by the Australian Primary Health Care Research Institute, which is supported by a grant from the Commonwealth of Australia as represented by the Department of Health. The information and opinions contained in it do not necessarily reflect the views or policy of the Australian Primary Health Care Research Institute or the Department of Health. This research was conducted in collaboration with the Robert Graham Center for Policy Studies in Family Medicine and Primary Care, Washington, DC.
References
1. Dussault G, Franceschini MC. Not enough there, too many here: understanding geographical imbalances in the distribution of the health workforce. Human Resources for Health 2006; 4: 12. https://doi.org/10.1186/1478-4491-4-12
2. Petterson SM, Liaw WR, Phillips RL, Rabin DL, Meyers DS, Bazemore AW. Projecting US primary care physician workforce needs: 2010-2025. Annals of Family Medicine 2012; 10(6): 503-509. https://doi.org/10.1370/afm.1431
3. Wakerman J, Humphreys JS. Sustainable workforce and sustainable health systems for rural and remote Australia. Medical Journal of Australia 2013; 199(Supp 5): 14-17. https://doi.org/10.5694/mja11.11639
4. Sivey P, Scott A, Witt J, Joyce C, Humphreys J. Junior doctors' preferences for specialty choice. Journal of Health Economics 2013; 31(6): 813-823. https://doi.org/10.1016/j.jhealeco.2012.07.001
5. Chen C, Petterson S, Phillips RL, Mullan F, Bazemore AW, O'Donnell SD. Toward graduate medical education (GME) accountability: measuring the outcomes of GME institutions. Academic Medicine 2013; 88(9): 1267-1280. https://doi.org/10.1097/ACM.0b013e31829a3ce9
6. McGrail MR, Humphreys JS, Scott A, Joyce C, Kalb G. Professional satisfaction in general practice: does it vary by community size? Medical Journal of Australia 2010; 193(2): 94-98.
7. McGrail MR, Humphreys JS. Geographical mobility of general practitioners in rural Australia. Medical Journal of Australia 2015; 203(2): 92-97. https://doi.org/10.5694/mja14.01375
8. Ricketts TC. The migration of physicians and the local supply of practitioners: a five-year comparison. Academic Medicine 2013; 88(12): 1913-1918. https://doi.org/10.1097/ACM.0000000000000012
9. Humphreys JS, Jones J, Jones M, Hugo G, Bamford E, Taylor D. A critical review of rural medical workforce retention in Australia. Australian Health Review 2001; 24(4): 91-102. https://doi.org/10.1071/AH010091a
10. Pathman D, Konrad T, Dann R, Koch G. Retention of primary care physicians in rural health professional shortage areas. American Journal of Public Health 2004; 94(10): 1723-1729. https://doi.org/10.2105/AJPH.94.10.1723
11. Scott A, Witt J, Humphreys JS, Joyce C, Kalb G, Jeon S-H, et al. Getting doctors into the bush: General Practitioners' preferences for rural location. Social Science and Medicine 2013; 96(1): 33-44. https://doi.org/10.1016/j.socscimed.2013.07.002
12. Wilson N, Couper I, De Vries E, Reid S, Fish T, Marais B. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health (Internet) 2009; 9: 1060. Available: www.rrh.org.au (Accessed 2 February 2016).
13. Schmitz DF, Baker E, Nukui A, Epperly T. Idaho rural family physician workforce study: the community apgar questionnaire. Rural and Remote Health (Internet) 2011; 11: 1769. Available: www.rrh.org.au (Accessed 2 February 2016).
14. Argent N, Tonts M, Jones R, Holmes J. The amenity principle, internal migration, and rural development in Australia. Annals of the Association of American Geographers 2014; 104(2): 305-318. https://doi.org/10.1080/00045608.2013.873320
15. Gosnell H, Abrams J. Amenity migration: diverse conceptualizations of drivers, socioeconomic dimensions, and emerging challenges. GeoJournal 2011; 76(4): 303-322. https://doi.org/10.1007/s10708-009-9295-4
16. Niedomysl T, Clark WAV. What matters for internal migration, jobs or amenities? Migration Letters 2014; 11(3): 377-386.
17. Partridge MD. The duelling models: NEG vs amenity migration in explaining US engines of growth. Papers in Regional Science 2010; 89(3): 513-536. https://doi.org/10.1111/j.1435-5957.2010.00315.x
18. Argent N, Tonts M, Jones R, Holmes J. Amenity-led migration in rural Australia: a new driver of local demographic and environmental change? In: GW Luck, D Race, R Black (Eds). Demographic change in Australia's rural landscapes:implications for society and the environment. Australia: Springer Science and Business Media and CSIRO Publishing, 2011.
19. Rupasingha A, Liu Y, Partridge M. Rural bound: determinants of metro to non-metro migration in the United States. American Journal of Agricultural Economics 2015; 97(3): 680-700. https://doi.org/10.1093/ajae/aau113
20. Chen Y, Rosenthal SS. Local amenities and life-cycle migration: do people move for jobs or fun? Journal of Urban Economics 2008; 64(3): 519-537. https://doi.org/10.1016/j.jue.2008.05.005
21. MacDowell M, Glasser M, Fitts M, Fratzke M, Peters K. Perspectives on rural health workforce issues: Illinois-Arkansas comparison. Journal of Rural Health 2009; 25(2): 135-140. https://doi.org/10.1111/j.1748-0361.2009.00209.x
22. Laurence CO, Williamson V, Sumner KE, J F. 'Latte rural': the tangible and intangible factors important in the choice of a rural practice by recent GP graduates. Rural and Remote Health (Internet) 2010; 10: 1316. Available: www.rrh.org.au (Accessed 2 February 2016).
23. Deller SC, Tsai T-H, Marcouiller DW, English DBK. The role of amenities and quality of life in rural economic growth. American Journal of Agricultural Economics 2001; 83(2): 352-365. https://doi.org/10.1111/0002-9092.00161
24. Hunter LM, Boardman JD, Onge JMS. The association between natural amenities, rural population growth, and long-term residents' economic well-being. Rural Sociology 2005; 70(4): 452-469. https://doi.org/10.1526/003601105775012714
25. McGrail MR, Humphreys JS, Joyce C, Scott A, Kalb G. Rural amenity and medical workforce shortage: is there a relationship? Geographical Research 2011; 49(2): 192-202. https://doi.org/10.1111/j.1745-5871.2011.00690.x
26. Weinhold I, Gurtner S. Understanding shortages of sufficient health care in rural areas. Health Policy 2014; 118(2): 201-214. https://doi.org/10.1016/j.healthpol.2014.07.018
27. von Reichert C, Cromartie JB, Arthun RO. Reasons for returning and not returning to rural U.S. communities. The Professional Geographer 2014; 66(1): 58-72. https://doi.org/10.1080/00330124.2012.725373
28. Rasker R, Gude PH, Gude JA, van den Noort J. The economic importance of air travel in high-amenity rural areas. Journal of Rural Studies 2009; 25(3): 343-353. https://doi.org/10.1016/j.jrurstud.2009.03.004
29. Wu J, Gopinath M. What causes spatial variations in economic development in the United States? American Journal of Agricultural Economics 2008; 90(2): 392-408. https://doi.org/10.1111/j.1467-8276.2007.01126.x
30. Isserman AM, Feser E, Warren DE. Why some rural places prosper and others do not. International Regional Science Review 2009; 32(3): 300-342. https://doi.org/10.1177/0160017609336090
31. Jones JA, Humphreys JS, Adena MA. Doctors' perspectives on the viability of rural practice. Rural and Remote Health (Internet) 2004; 4: 305. Available: www.rrh.org.au (Accessed 2 February 2016).
32. Irwin EG, Isserman AM, Kilkenny M, Partridge MD. A century of research on rural development and regional issues. American Journal of Agricultural Economics 2010; 92(2): 522-553. https://doi.org/10.1093/ajae/aaq008
33. Green GP, Deller SC, Marcouiller DW (Eds). Amenities and rural development: theory, methods and public policy. Northhampton, MA: Edward Elgar Publishing, 2005.
34. McGranahan D. Natural amenities drive rural population change. (Internet) 1999. Agricultural Economic Report No. 781. Available: https://www.ers.usda.gov/webdocs/publications/aer781/13201_aer781.pdf (Accessed 2 February 2016)
35. Mason J. Review of Australian Government health workforce programs. (Internet) 2013. Available: http://www.health.gov.au/internet/main/publishing.nsf/content/review-australian-government-health-workforce-programs (Accessed 2 February 2016).
36. United States Department of Health and Human Services. National Health Service Corps. (Internet) 2015. Available: http://www.nhsc.hrsa.gov/ (Accessed 18 May 2015).
37. McGrail MR, Humphreys JS. Measuring spatial accessibility to primary care in rural areas: improving the effectiveness of the two-step floating catchment area method. Applied Geography 2009; 29(4): 533-541. https://doi.org/10.1016/j.apgeog.2008.12.003
38. Guagliardo MF. Spatial accessibility of primary care: concepts, methods and challenges. International Journal of Health Geographics 2004; 3: 3. https://doi.org/10.1186/1476-072X-3-3
39. Luo W, Qi Y. An enhanced two-step floating catchment area (E2SFCA) method for measuring spatial accessibility to primary care physicians. Health & Place 2009; 15(4): 1100-1107. https://doi.org/10.1016/j.healthplace.2009.06.002
40. Luo W, Wang F. Measures of spatial accessibility to health care in a GIS environment: synthesis and a case study in the Chicago region. Environment and Planning B 2003; 30(6): 865-884. https://doi.org/10.1068/b29120
41. McGrail MR. Spatial accessibility of primary health care utilising the two step floating catchment area method: an assessment of recent improvements. International Journal of Health Geographics 2012; 11: 50. https://doi.org/10.1186/1476-072X-11-50
42. Wan N, Zou B, Sternberg T. A 3-step floating catchment area method for analyzing spatial access to health services. International Journal of Geographical Information Science 2012; 26(6): 1073-1089. https://doi.org/10.1080/13658816.2011.624987
43. McGrail MR, Humphreys JS. Spatial access disparities to primary health care in rural and remote Australia. Geospatial Health 2015; 10(2): 138-143. https://doi.org/10.4081/gh.2015.358
44. Lichter DT, Brown DL. Rural America in an urban society: changing spatial and social boundaries. Annual Review of Sociology 2011; 37(1): 565-592. https://doi.org/10.1146/annurev-soc-081309-150208
45. Ulrich-Schad JD, Henly M, Safford TG. The role of community assessments, place, and the great recession in the migration intentions of rural Americans. Rural Sociology 2013; 78(3): 371-398. https://doi.org/10.1111/ruso.12016
46. Hancock C, Steinbach A, Nesbitt T, Adler S, Auerswald C. Why doctors choose small towns: a developmental model of rural physician recruitment and retention. Social Science and Medicine 2009; 69(9): 1368-1376. https://doi.org/10.1016/j.socscimed.2009.08.002
47. Russell D, Humphreys JS, McGrail MR, Cameron I, Williams PJ. The value of survival analyses for evidence-based rural medical workforce planning. Human Resources for Health 2013; 11: 65. https://doi.org/10.1186/1478-4491-11-65
48. Australian Government Department of Health. Rural classification reform - frequently asked questions. (Internet) 2015 Available: http://www.doctorconnect.gov.au/internet/otd/publishing.nsf/content/classification-changes (Accessed 19 August 2015).
49. Humphreys JS, McGrail MR, Joyce CM, Scott A, Kalb G. Who should receive recruitment and retention incentives? Improved targeting of rural doctors using medical workforce data. Australian Journal of Rural Health 2012; 20(1): 3-10. https://doi.org/10.1111/j.1440-1584.2011.01252.x
50. Schlapfer F, Waltert F, Segura L, Kienast F. Valuation of landscape amenities: a hedonic pricing analysis of housing rents in urban, suburban and periurban Switzerland. Landscape and Urban Planning 2015; 141(1): 24-40. https://doi.org/10.1016/j.landurbplan.2015.04.007
51. Menec VH, Hutton L, Newall N, Nowicki S, Spina J, Veselyuk D. How 'age-friendly' are rural communities and what community characteristics are related to age-friendliness? The case of rural Manitoba, Canada. Ageing & Society 2015; 35(1): 203-223. https://doi.org/10.1017/S0144686X13000627
_____________________________
Appendix A: Full details of multivariate linear regression models? of rural supply