full article:
Background
It is well established that rural-origin medical students are more likely to enter rural work than their urban peers. It has been further suggested that these rural graduates have a predisposition to return to their own home towns or regions1. To date there is no published data to uphold the second assertion.
If there is a link between place of origin and place of work, this may have implications for further development of rural recruitment targets for medical schools, so as to better match areas of workforce need. This would allow more sophisticated workforce planning in Australia. We therefore aimed to demonstrate where, relative to their town of origin, rural-origin students work after graduation.
Methods
All students entering Medicine at the University of Western Australia through the rural recruitment program (RRP) from 1993 to 2006 - so that all graduates were at least postgraduate year (PGY)3 at the time of this study - and for whom town of origin information was available were included under Human Research Ethics Committee approval RA/4/1/6491. A prior study showed that from 2002 to 2006, with the implementation of a specific rural recruitment program, the percentage of rural entrants in the medical program increased from a baseline of 12% to 23%2.
Rural students were classified into their towns and regions of origin. The principal place of practice for each rural-origin graduate was then obtained from the Australian Health Practitioner Regulation Agency website from March to July 2014. This town was compared with their rural-origin town to establish whether their workplace was the same town, same region, or simply rural with no other match. ArcGIS mapping software was used to map participant origin, current principal place of practice, and the trajectory between the two.
Results
There were 233 RRP students from 1993 to 2006, of whom four did not have home location identified. Proportionately more medical students were recruited from populous rural centres in the south of the state (32.93 medical students per 10 000 population) than from small remote towns in the north (4.37 medical students per 10 000 population). Of the 229 eligible participants, 49 could not be identified through the Australian Health Practitioner Regulation Agency. Although 25% of the identified graduates returned to rural work (45/180), they did not tend to return either to their home region (9/229, 4%) or their home town (6/229, 3% returning to three locations: Broome, Bunbury, Collie). Instead, the majority moved considerable distances away to other states and regions (Fig1).
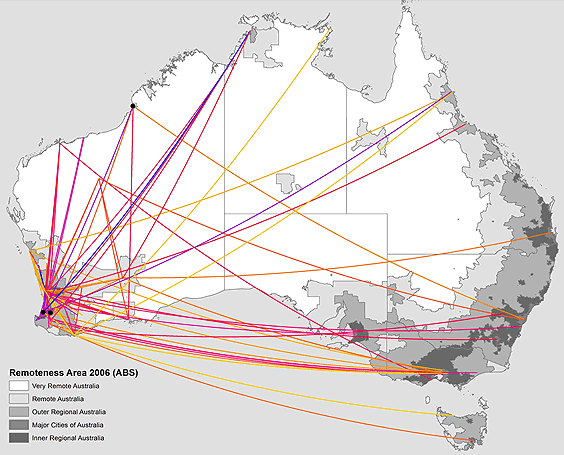
Figure 1: Rural-origin graduates' migration pathways from town of origin in Western Australia to town of principal practice location in 2014. Each origin location has been given a colour to allow to show flow direction.
Discussion
We confirm that one in four rural origin students return to work rurally3. However, we provide the first evidence that rural origin students do not 'return home'. This finding runs counter to the North American suggestion that recruiting students from rural towns could make good these towns' local medical shortfall. To the contrary, since Australian rural students tended to disperse widely, these data suggest there is no benefit in preferential recruitment from any particular rural area. Rather, the benefit is in recruiting more rural students.
Since rural graduates scatter to towns remote to their own, those towns most in need of workforce may well benefit from initiatives to expose students to their practices. There is early evidence that medical students placed for an undergraduate year in rural and remote locations go on to return to more remote locations than those not so placed4,5. Those placed remotely for postgraduate training appear also to remain more remote6. This is an important consideration for federal funding, since the cost of remote medical student placements is greater than for peri-urban settings, but may lead to better long term workforce distribution. This possibility is yet to be explored.
The almost complete lack of return to the same town or region was striking. It would appear that rural-origin students up to PGY16 postgraduation specifically go elsewhere than 'home'. This might reflect Cutchin's7 discussion about 'experiential place integration', with dimensions of security, identity, freedom and integration, which include not being constrained by the expectations of one's own home town, along with a strong connectedness to rural life in general.
Conclusion
Although rural-origin students return in relatively high rates to rural communities, they principally do so for communities other than their place of origin. This qualification of 'rural return' confirms the effectiveness of current rural student recruitment, and also confirms that rural recruits in any given state are an important constituent of the rural workforce at large in Australia.
Robert Buttner, Nathan Blakely, Sam Curtin, Ben Wall, Sue Poughnault, Tessa Burkitt and Denese Playford
The Rural Clinical School of Western Australia, University of Western Australia
References
1. Rabinowitz H, Diamond J, Markham F, Wortman J. Medical school programs to increase the rural physician supply: a systematic review and projected impact of widespread replication. Academic Medicine 2008; 83: 235-243. https://doi.org/10.1097/ACM.0b013e318163789b
2. Emery J, Hurley S, Williams J, Poughnault S, Mercer A, Tennant M. A seven-year retrospective analysis of students entering medicine via a Rural Student Recruitment program in Western Australia. Australian Journal of Rural Health 2009; 17: 316-320. https://doi.org/10.1111/j.1440-1584.2009.01105.x
3. Playford D, Evans S, Atkinson D, Auret K, Riley G. Impact of the Rural Clinical School of Western Australia on work location of medical graduates. Medical Journal of Australia 2014; 200: 104-107. https://doi.org/10.5694/mja13.11082
4. Playford D, Nicholson A, Riley GJ, Puddey IB. Longitudinal rural clerkships: increased likelihood of more remote rural medical practice following graduation. BMC Medical Education 2015; 15: 55. https://doi.org/10.1186/s12909-015-0332-3
5. Kondalsamy-Chennakesavan S, Eley DS, Ranmuthugala G, Chater AB, Toombs M, Darshan D, et al. Determinants of rural practice: positive interaction between rural background and rural undergraduate training. Medical Journal of Australia 2015; 202(1): 41-45. https://doi.org/10.5694/mja14.00236
6. Jamieson JL, Kernahan J, Calam B, Sivertz KS. One program, multiple training sites: does site of family medicine training influence professional practice location? Rural and Remote Health (Internet) 2013; 13: 2496. Available: www.rrh.org.au (Accessed 6 February 2017).
7. Cutchin MP. Physician retention in rural communities: the perspective of experiential place integration. Health & Place 1997; 3(1): 25-41. https://doi.org/10.1016/S1353-8292(96)00033-0