full article:
The Tasmanian medical program, with undergraduate entry and a 5-year duration, is the main source of the medical workforce in Tasmania, providing about 36% of the whole workforce1. There is a significant workforce maldistribution across the state, particularly in the north-western region, where medical services are reliant on international medical graduates and short-term locum appointments. It appears that relatively few Tasmanian medical graduates work outside of the two main cities1.
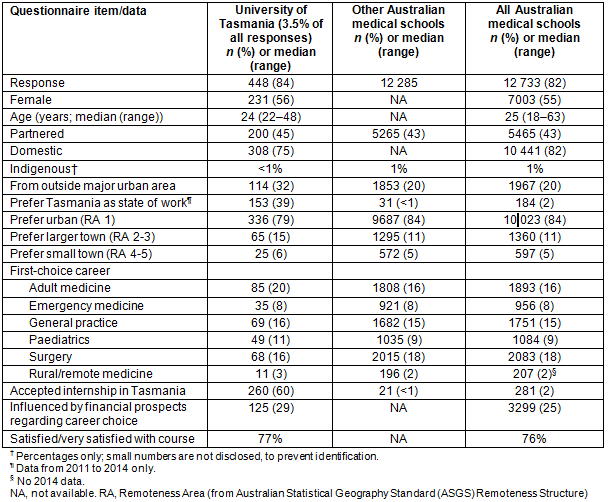
The early career contribution to the local workforce of the medical program was explored through analysis of data from exit questionnaires administered to five consecutive cohorts of graduates, from 2010 to 2014, as part of the Medical Schools Outcomes Database project2. The data included demographic information, geographic and specialty career preferences, and interest in working in Tasmania. These data are presented in Table 1, comparing graduates from the University of Tasmania with those from both other Australian medical schools and all Australian medical schools combined, including Tasmania.
The results show that University of Tasmania medical graduates have little impact on the national data and are similar to those of other Australian medical schools with respect to demographic data, career preferences, student satisfaction ratings and financial considerations in career choice. However, there were some key differences. The first is that a substantially higher proportions of students come from communities outside of major urban centres (30% vs 20%), although this may be explained by the categorisation of the whole of Tasmania as 'rural' because it is separated from the mainland. The second difference is that a higher proportion stated a preference to work in Tasmania in the future (39% vs <1%). The third is that a higher proportion accepted intern positions in Tasmania (60% vs 2%). This may reflect the state government guarantee of positions for local graduates, because 33% of Tasmanian graduates in Tasmanian intern positions accepted positions interstate for specialist training, which in Australia commences after a generalist internship.
These data raise three interesting points. First, it is clear that the Tasmanian medical program, while constituting a small part of the national medical education context, is the major contributor to the state's local medical workforce. Staffing the state's hospitals with junior doctors might be difficult without the local program. Second, a substantial proportion (61%) of graduates expressed a preference to work outside of Tasmania. Tasmania's population demography demonstrates features of both regional and rural communities and 'island' states or nations, such as Newfoundland and Iceland, with a 'normalisation' of youth emigration to seek opportunities not available locally, combined with a desire to return 'home' at some stage3,4. It is possible that this phenomenon may impact negatively on medical workforce recruitment and retention. Third, unlike those of other regional medical schools5, Tasmanian program graduates have a lower preference for rural medicine careers, more akin to the average for all Australian medical graduates. It is therefore possible that the state's workforce maldistribution could be addressed through implementing rural medical education initiatives proven useful elsewhere. With this in mind, we at the University of Tasmania School of Medicine have introduced evidence-based strategies such as a rural admissions pathway and a strengthened rural clinical school program, which has shown early success at recruiting their graduates to local positions6. We have also lobbied the state government to introduce a rural medical generalist model in the north-western region, with training programs and career pathways that support this model7.
Table 1: Data from Australian medical school exit (graduation) questionnaires, 2010-2014
Richard Hays, Allison Turnock and Emma Warnecke, School of Medicine, University of Tasmania
References
1. Australian Health Practitioner Regulation Agency. 2014 Tasmanian report. Annual report summary 2014/15. P19-20. (Internet) 2015. Available: http://www.ahpra.gov.au/annualreport (Accessed 28 November 2016).
2. Humphreys JS, Prideaux D, Beilby J, Glasgow N. From medical school to medical practice - a national tracking system to underpin planning for a sustainable medical workforce in Australia. Medical Journal of Australia 2009; 191: 244-245.
3. Bjarnason T, Thorlindsson T. Should I stay or should I go? Migration expectations among youth in Icelandic fishing and farming communities. Journal of Rural Studies 2006; 22: 290-300. https://doi.org/10.1016/j.jrurstud.2005.09.004
4. Gabriel M. Australia's regional youth exodus. Journal of Rural Studies 2002; 18: 209-212. https://doi.org/10.1016/S0743-0167(01)00039-0
5. Sen Gupta TK, Murray R, Hays RB, Woolley T. James Cook University MBBS graduate intentions and intern destinations: a comparative study with other Queensland and Australian medical schools. Rural and Remote Health (Internet) 2013; 13: 2313. Available: www.rrh.org.au (Accessed 8 February 2017).
6. Shires L, Allen P, Cheek C, Wilson D. Regional universities and rural clinical schools contribute to rural medical workforce, a cohort study of 2002-2013 graduates. Rural and Remote Health (Internet) 2015; 15: 3219. Available: www.rrh.org.au (Accessed 8 February 2017).
7. Sen Gupta TK, Manahan DL, Lennox DR, Taylor NL. The Queensland Health Rural medical generalist pathway: providing a medical workforce for the bush. Rural and Remote Health (Internet) 2012; 13: 2319. Available: www.rrh.org.au (Accessed 8 February 2017).

