full article:
Chronic diseases including such conditions as cardiovascular, respiratory and renal diseases, as well as disability caused by injury such as burns and to the spinal cord, affect many people around the world. These conditions are mostly characterised by complex causality, multiple risk factors, long latency periods, a prolonged course of illness and functional impairment or disability1. As a result of their often intense and prolonged requirement for health care, chronic conditions impose significant costs and challenges to health systems aiming to deliver cost effective, yet effective and appropriate, health care2. Compounding these challenges is the fact that chronic conditions disproportionally affect more Indigenous than non-Indigenous people, who have been shown to have significant challenges accessing health care3,4.
Telehealth, a relatively new modality for healthcare delivery, aims to address some of the challenges facing health systems by increasing healthcare access and quality, enhancing health outcomes and reducing the high costs associated with speciality healthcare services5,6. Telehealth is currently used differently across the world with various levels of effectiveness for healthcare administration, provision and education7. There are no strict definitions for telehealth: in some instances, telehealth is described as a model of care when distance separates those involved4. At other times, it is recommended as a modality used to strengthen the provision of health care7. Broadly speaking, telehealth is the use of information and computer technologies to deliver health care and transmit health information4.
Telehealth lends itself to providing some of the necessary ongoing health care for people suffering chronic conditions8-11 and as a result may have a positive influence on the health and wellbeing of Indigenous peoples experiencing inequitable access to health care. This is particularly the case where people experience geographical isolation and system factors that can inhibit access. The evidence for telehealth is still developing, and the cost effectiveness of telehealth is inconclusive due to lack of quality research data12,13.
Health care provided using telehealth to Indigenous peoples often occurs at the cultural interface between non-Indigenous healthcare professional and Indigenous patient. The cultural interface is where different knowledge systems interact: 'it is a place of tension that requires constant negotiation'14. Telehealth, a subsidiary of technology, cannot be separated from the actual health care itself. Like any healthcare provision for Indigenous peoples, telehealth needs to be culturally appropriate for it to have meaningful health benefits15. A recent report highlighted how the introduction of culturally specific care '... through culturally knowledgeable providers, onsite tribal outreach workers ... as well as building rapport, trust, and engagement with the target patient population'16 may support more culturally safe care. However, there are gaps in the published research regarding how well telehealth can deliver culturally appropriate care to Indigenous peoples17.
Telehealth reviews highlight the need for further exploration around the acceptability of telehealth for use with Indigenous peoples18,19. Where telehealth is received favourably, it is not clear if this is about telehealth per se or about the benefits of receiving any service at all in a remote community20. More consideration of the effectiveness of telehealth in terms of providing culturally appropriate health care to encompass a more holistic concept of health for Indigenous peoples would be helpful in providing a clear understanding. Critical reflection of all telehealth processes and reported outcomes, including from the perspective of the Indigenous peoples who use the service, would be valuable.
Reflection of telehealth in alignment with Indigenous ways of being, doing and knowing to meet the needs of Indigenous peoples is justified. Helen Milroy's contemporary Aboriginal model of holistic health includes cultural, spiritual, social, emotional and physical dimensions21. Influenced by historical, traditional and contemporary layers, Milroy emphasises 'the intersection of both the layers and dimensions which creates the interconnectedness for a whole of life approach to Aboriginal wellbeing'21. As a result, health systems that produce models of care that include telehealth, and the healthcare professionals enacting health care via telehealth, should incorporate and support a holistic view of health such as this. Further still, to be acceptable for recipients, telehealth as a modality for healthcare provision for Indigenous peoples needs to be culturally safe. Culturally safe care is an outcome defined only by the individual receiving care22, and is usually experienced by those who receive care from culturally competent healthcare professionals and systems23.
This review is a systematic meta-synthesis to describe the effectiveness of telehealth for the care of Indigenous peoples with chronic conditions. The focus is to critique the evidence of telehealth for managing chronic conditions in Indigenous populations in three ways: the effectiveness of telehealth in terms of health outcomes (morbidity, mortality and quality of life); the acceptability of telehealth as to how it encompasses a holistic model of health for Indigenous peoples as healthcare consumers and for healthcare professionals; and the feasibility of uptake for health services. Information and communication technologies have the unique capacity to reach underserved populations because of their wide and instant dissemination capability. The evidence for the implementation of telehealth and its ultimate role and effectiveness in providing health care to Indigenous peoples requiring chronic conditions management is yet to be clearly defined. This is especially the case for respecting non-Western biomedical views of health and wellbeing and the lack of evidence for the use of telehealth in respecting the cultural values and health beliefs of Indigenous peoples. It is unclear if actual health outcomes and inequities can be addressed for Indigenous peoples through the uptake and use of telehealth in health services.
Search strategy
A systematic search of the literature was conducted in August 2015 for studies relating to three concept areas: telehealth; Indigenous status; and chronic conditions. Studies were identified from an electronic database search using a combination of subject headings and keywords (Appendix A) in the following databases: MEDLINE and MEDLINE in Process; CINAHL; Web of Science; SCOPUS; Informit; and the Cochrane Library. The search included the following limitations: English language; and last 10 years.
Inclusion and exclusion criteria and quality appraisal
Studies were included in this review if they met each of the following criteria: presented findings from primary research; investigated any aspect of telehealth supporting chronic conditions management; involved Indigenous peoples of any age; and addressed one of the three research questions. Qualitative and quantitative studies were included and all case series and reviews excluded. For each of the three research question (effectiveness, acceptability and feasibility), a range of outcomes were eligible. Outcomes for effectiveness related to Indigenous peoples health outcomes. Evidence of acceptability were by perception of telehealth use by Indigenous peoples as healthcare consumers in terms of cultural acceptability and healthcare professionals in terms of health service delivery. Outcomes related to feasibility were directly regarding health service impact, for example diagnostic capabilities.
The included studies were summarised using a standard data extraction form including a combination of the following items dependent on study type: aim; study design; participants; Indigenous group; country; telehealth intervention; chronic condition management; outcome; and study limitations. Where identified, facilitators and barriers to telehealth as a modality in healthcare delivery were recorded. The strength of evidence for each of the studies included for review was assessed using criteria from the Joanna Briggs Institute24,25. Levels of Evidence for Effectiveness (Table 1)24 and Grades of Recommendation (Table 2)25 were assessed for all included studies.
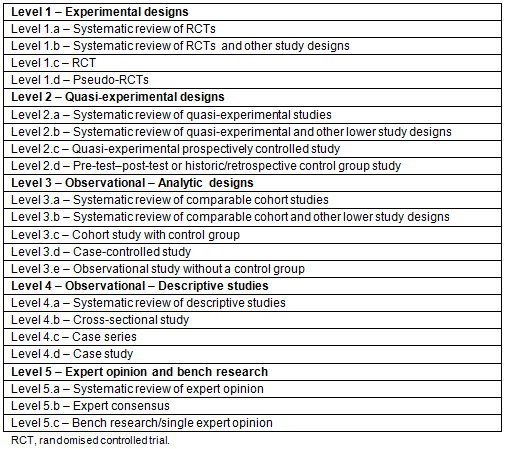
Table 2: Grades of recommendation25

Synthesis
Data selected for inclusion were narratively synthesised and initially presented in terms of quality and design for each research question. The effectiveness of telehealth in terms of health outcomes of consumers was grouped thematically by intervention type, origin of research and health outcome. The acceptability of telehealth data were presented narratively: first, for consumers and second for healthcare professionals. Data relating to feasibility of telehealth were synthesised in terms of health service impact.
The electronic database search returned 2680 studies. Of these studies, 1863 duplicates were removed, leaving 817 studies for screening of title and abstract. A further 713 studies were excluded in this process, resulting in 104 studies being assessed in their entirety for inclusion in this study. From this analysis, 32 met the inclusion criteria for the review. The study selection process is summarised in the PRISMA flow chart (Fig1). Included studies were grouped according to main stated aim. Studies with two or more main aims appear across groups. Of the 32 studies included in this review 11 examine the effectiveness of telehealth in regards to health outcomes for Indigenous people (Supplementary table 1); 10 critique the acceptability of telehealth by Indigenous peoples as healthcare consumers (Supplementary table 2) eight report the acceptability of telehealth from the perspectives of healthcare professionals (Supplementary table 3); and 12 examine the feasibility of telehealth for health services (Supplementary table 4).
The telehealth modalities described in the studies were mostly real-time video-conferencing, internet based applications and portals, and asynchronous technologies. The term telehealth, used collectively throughout this article, was referred to differently in the included studies and synonymous with teleoncology; telemedicine; teleophthalmology; a computerised therapy; web-based therapy; and telemental health. For the included studies, the Indigenous peoples of the countries Australia, North America, New Zealand and the Pacific Islands are referred to as Aboriginal and Torres Strait Islanders; First Nations, American Indian, Alaska Native and Hawaiian; Maori; and Islanders, respectively. The term 'Indigenous peoples' is used throughout where results and discussions are collective. A small number of the studies were not entirely dedicated to Indigenous peoples and had a proportion of non-Indigenous study participants. Chronic conditions described in the included studies were: cancer; congestive heart failure; chronic obstructive pulmonary disease; type II diabetes; mental health conditions; otitis media; heart failure; diabetic retinopathy and injury. The term 'chronic condition' is used throughout where results and discussions are collective. Telehealth was used to manage the chronic conditions of Indigenous peoples through referral, assessment, review, monitoring, support provisions, medication management and self-management.
The published studies suggested that telehealth is being used in various ways across the world for chronic condition management with Indigenous populations. The studies also suggested telehealth can be at least as good as face-to-face clinical care assessment, and may improve access to care. Unfortunately, as there were no comparative published studies on health outcomes it is difficult to prove equality or superiority. The studies reported Indigenous peoples tend to be satisfied with the use of telehealth26-28 particularly as it can address the barriers associated with living remotely and away from specialised care29. However some studies reported Indigenous people having reservations about the information and communication technologies including concerns about privacy and confidentiality30 and feeling generally uncomfortable31. For the studies reported by health services, telehealth was feasible in terms of health care and service delivery, and healthcare professionals were somewhat satisfied with using telehealth; however, they found difficulties with information and communication technologies a consistent barrier. The data and heterogeneity of the 32 included studies meant they were not suitable for meta-analysis, and as such a meta-synthesis is used to report in narrative form.
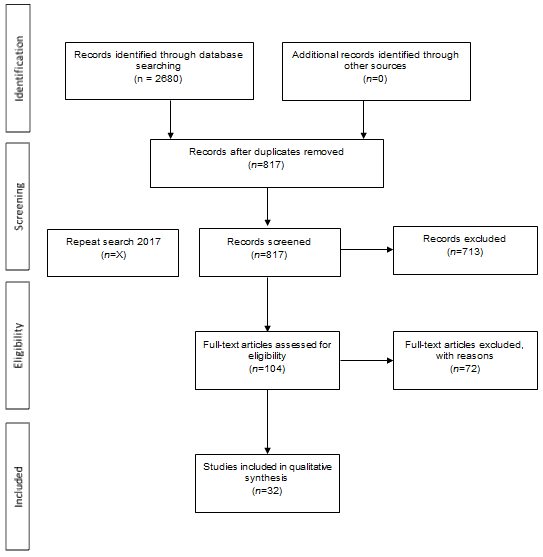
Figure 1: PRISMA flow chart
Effectiveness of telehealth (Supplementary table 1)
Of the 32 studies described in this review, 11 reported the effectiveness of telehealth in terms of health outcomes (morbidity, mortality and quality of life (QOL)) for Indigenous peoples requiring chronic condition management. Study types included four randomised controlled trials (RCTs)32-35, four pre/post29,36-38, two comparative39,40 and one prospective41. Whilst the results indicated that telehealth may improve morbidity and QOL and reduce mortality, studies were limited by factors such as small sample size32,37,40,41, short surveillance periods34, retrospective data29,36,38, lack of controls29,36,38,41 and lack of randomisation36,38-41. The larger RCT with a 5-year follow-up found telemedicine increased the percentage of participants who obtained diabetic retinopathy screening examinations when compared with traditional surveillance. This result may be limited by use of a monetary incentive increasing follow-ups in both groups in the last year of follow-up; however, they should not have affected the proportional difference35.
The most common telehealth intervention, described in six of the studies, was home internet-based monitoring32,33,37,39-41. Other telehealth interventions were three asynchronous image/data transfers for screening, diagnosis and monitoring29,34,35 and two evaluating the use of real-time for assessment and management of chronic conditions36,38. Seven of the studies were based in the USA with American Indian and Alaska Native people, three in Australia with Australian Aboriginal and/or Torres Strait Islander people and one with Maori people from New Zealand. Not all of the participants included in four of the studies were Indigenous peoples34-36,39. Improvements in morbidity were seen by better disease control40,41 and reduced hospitalisation rates and days spent in hospital39. Reductions in rates were not significantly greater when compared with a matched cohort; however, changes to services may have contributed to results evident in the control group for this study39. Improvements in QOL were evident by a reduction of unnecessary transfers36, increased prescription drug use38 and reduced specialist review wait times29. In terms of mortality, a substantial but non-significant trend toward reduced mortality in the intervention group of the 12-month pilot study was evident in one of the RCTs, which was limited by small sample size32.
Acceptability of telehealth by Indigenous peoples (Supplementary table 2)
Of the 32 studies included in this review, 10 reported on the acceptability of telehealth as a modality to healthcare delivery from the perspective of the Indigenous client. Two of these studies30,42 looked at both the Indigenous clients' and the healthcare professionals' perspectives. Differentiation between the two perspectives was clear and enabled separate reporting. All studies reported varying degrees of mostly positive acceptance for a variety of telehealth approaches as the modality for delivery of health care to manage chronic conditions. In particular, Indigenous peoples liked reduced travel costs42. Level of acceptance was obtained predominantly through qualitative interviews27,32,42-45, and measured by self-reported Likert scales in four studies26,28,30,46. All studies, including two pilot trials27,32, reported via descriptive study design, and were limited by small sample sizes and thus have limited capacity to generalise.
Facilitators to acceptance of telehealth revolved mostly around healthcare professional cultural competence and information and communication technologies capability. Indigenous clients described preferring face-to-face contact31 because of loss of connection and relationship with the healthcare professional42. An initial face-to-face meeting was thought to facilitate acceptance of telehealth42, especially for mental health assessments43. Client-healthcare professional relationships, linked strongly to trust and rapport, were a recurring theme across these studies. In one study examining the use of real-time video-conferencing for management of type two diabetes mellitus, a downfall of telehealth was described by its inability to enable good relationships42. Furthermore a study that explored acceptability of telehealth for mental health management using real-time video-conferencing highlighted a lack of culturally competent healthcare professionals and systems as key deterrents to the use of telehealth43. Conversely, some participants reported greater continuity and access to mental health services, reduced travel time, and increased comfort in disclosure through telehealth43. Similarly, for a small study based in New Zealand45, young Indigenous people thought favourably of telehealth as the modality to deliver cognitive behavioural therapy for depression.
Acceptability of telehealth by healthcare professionals (Supplementary table 3)
Of the 32 studies included in this review, eight reported on the perspectives of healthcare professionals in terms of their acceptance of using telehealth. Video-conferencing at health services was the telehealth medium described in all but one of the studies47. Five of these studies also reported on Indigenous client acceptance and health service feasibility and therefore appear in other result sections. Studies reported via qualitative design, typically thematically analysed data presented in narrative form, along with survey data from quantitative studies. All studies reported mostly positive views of telehealth as a modality for the delivery of chronic condition management. Acceptance of telehealth appeared to be facilitated by two main themes: knowledge of and access to reliable information and communication technologies, and specific cultural factors including Indigenous healthcare professionals and using traditional practices. Reported acceptance was based upon different aspects of care provision, for example good quality care28, time-saving42 and enhanced collaborative care30. Perceived usefulness of telehealth influenced a healthcare professional's intention to use the modality48 and resistance to information and communication technologies created a barrier for its uptake30. Although reporting overall positive satisfaction, a small study48 based in Canada that surveyed49 healthcare professionals and interviewed five found that real-time video-conferencing was not appropriate for specific mental health conditions and limited the ability of healthcare professionals to intervene. For these eight studies, surveys were primarily used to gauge level of acceptance and were limited by small and non-representative samples28,30,42,47,49,50 and little or absent descriptions of methods28,49.
Health service feasibility (Supplementary table 4)
Of the 32 studies included in this review, 20 evaluated various aspects of the feasibility of telehealth use by health services. For the 12 studies that evaluated feasibility in terms of accuracy and service delivery, a range of telehealth methods, interventions and chronic conditions were covered. Five of these studies also assessed acceptability of telehealth for chronic disease management by Indigenous client and healthcare professionals and are included elsewhere in the results. Feasibility of telehealth for health services was in terms of service delivery and use, healthcare professional outcomes and clinical reliability. Study design, aim and limitations of these 12 studies varied considerably, yet results were relatively consistent. That is, telehealth is feasible for use in the delivery of health care. The studies were a mixture of descriptive, comparative and interventional studies, and included three pilot trials. Whilst not from experimental data, the descriptive studies consistently looked at ways that health services were impacted by the use of telehealth as a modality to healthcare delivery. Results indicated improvements in client involvement with health services47,51-53. Similarly, healthcare professionals showed positive responses in terms of productivity from the use of asynchronous technology47 and healthcare competence following real-time video-conferencing case conferences47,50. Comparative and interventional studies to assess clinical service feasibility of telehealth showed that, for diagnosis reliability, asynchronous images were acceptable for ear, nose and throat54 and cancer screening55, as was face-to-face compared with real-time video-conferencing for mental health diagnosis56. Although a large sample size of 321 participants increased reliability of findings55, the other studies were limited by non-randomisation54, potential screener bias54, and delayed comparison interval56. Therefore, whilst these results are promising in terms of telehealth feasibility for health services, study limitations impact their conclusiveness.
Discussion
Key findings
This review highlights that telehealth is being used across the world to manage a wide variety of chronic conditions experienced disproportionally by Indigenous peoples, but lacks conclusive evidence as to its overall effectiveness, acceptability and feasibility. The existing literature provides some evidence for the effectiveness of telehealth in terms of health outcomes from a western biomedical perspective. This was seen by reductions in hospitalisations, decreased unnecessary transfers and increased health management adherence. However, the acceptability of telehealth appears somewhat mixed for the Indigenous peoples utilising such services, and it is not clear whether or how it can enable health professionals to enact a holistic model of health. Telehealth appears to be feasible for health services in terms of healthcare delivery, and healthcare professionals have mostly positive views of using telehealth. Key gaps reflect a lack of research from a holistic health perspective with a need for more focused research on the cultural competency of healthcare professionals and systems in relation to telehealth, and how cultural safety is experienced.
Health systems: health economics and telehealth with Indigenous peoples
Telehealth is not a health system; however, it is a key component of many systems delivering health care to some of the world's most vulnerable people and therefore needs thoughtful consideration to assess functionality. The World Health Organization57 presents five key components of a well-functioning health system: improving health status; defending populations against what threatens its health; protecting people against consequences of ill health; providing equitable access to people-centred care; and making it possible for people to participate in decisions about their health and health system. This review highlighted that telehealth can improve health status as seen by improvements in diabetic clinical indicators33,41. Public health measures of health promotion, incorporating telehealth, can result in increased involvement with health services49,51-53, thereby potentially defending Indigenous peoples against the threat and risks associated with chronic disease. The review also highlighted that telehealth results in increased screening rates35 and health service utilisation52, potentially protecting people against the consequences of ill health. Similarly, in this review, telehealth enabled more equitable access to specialist services not otherwise available in some geographical locations. Lastly, it was evident that Indigenous peoples were able to participate in decisions regarding the development of telehealth services in their local community, and thus better participate in decisions about the health care they receive58,59.
This review did not evaluate the health economics of telehealth. It is important to note that the decision to incorporate telehealth into the suite of modes of delivery of health care based purely on economic benefits as an argument for use60, or by non-Indigenous people and systems59, fails to consider Indigenous ways of knowing, being and doing and as such cannot be assumed to be generalisable to Indigenous peoples. Further, it is assumed that a reduction in health service cost does not necessarily equate to increasing effective and efficient quality care. If cost is saved to health services, is there a cost to the Indigenous peoples using the service? When people are happy not having to travel, does this come at a cost to their health?
Holistic health: does telehealth address this multidimensional concept?
Indigenous people across the world value a holistic, multi-dimensional concept of health that Helen Milroy21 describes as including physical, psychological, social health and wellbeing, spirituality and cultural integrity. It is important to note that whilst there are some inherent similar characteristics shared between Indigenous peoples across the world, for example their connection to land and holistic health beliefs, significant differences also exist between cultures, like language and rituals. Indigenous peoples are therefore more likely to experience better health outcomes when health care is not compartmentalised, and delivered from a comprehensive model of primary health care to address all aspects of Indigenous health, including social and emotional health and wellbeing. While this review found telehealth is somewhat effective as a modality of healthcare delivery for chronic condition management with Indigenous peoples, the included studies addressed only singular aspects of health and wellbeing and did not encompass a holistic standpoint. For example, physical and psychological health were addressed, albeit singularly, but social health, wellbeing, spirituality and cultural integrity were not addressed. The physical aspects of holistic health could be optimised with telehealth, and whilst psychological health was addressed, it did not translate well with telehealth. It seems the cultural competency of telehealth set up and users in terms of how holistic health care can be provided are yet to be determined.
The cultural interface: barriers and facilitators to telehealth
This review identified where the ability of healthcare professionals and systems to negotiate the cultural interface may increase the acceptability of telehealth from a cultural perspective for Indigenous clients. Mason Durie61 describes the interface as being where Indigenous knowledge intersects with scientific knowledge, in this instance, a Western biomedical standpoint. It is well known that cultural factors influence the way in which Indigenous peoples access and engage with health services and non-Indigenous healthcare professionals62,63. Further, health care is more often than not delivered within cultured space often based on a Western biomedical system of care that does not allow for different concepts of health and healing. Telehealth is no exception.
Culturally competent healthcare professionals30,32,64 and health service delivery27 may facilitate culturally acceptable telehealth. For the non-Indigenous health professional, '... working at the cultural interface requires critical questioning of professional assumptions based on Western knowledge while simultaneously being open to learning about Indigenous knowledges'65. When language barriers42, inability to form trusting relationships43, cultural factors and discomfort with information and communication technologies31 are barriers to delivery and receiving effective health care, other modalities must be implemented.
Therapeutic relationships: trust and rapport
Relationship development was key for both Indigenous clients and healthcare professionals in many of the studies. This was highlighted by constant reference to its importance - for better health outcomes, cultural appropriateness and facilitating telehealth uptake. Essentially, the acceptability of telehealth and its ability in having the potential to improve healthcare is dependent on its ability to facilitate and enhance these vital relationships42. Two studies focused on different aspects and perspectives of telehealth32,43 suggested that initial consults must be face-to-face in order for relationship development. Telehealth may be an acceptable modality to healthcare delivery because it enables Indigenous peoples to receive treatment in their home community. However, when actually given a choice over how their health care is delivered, does this suggest that Indigenous peoples would prefer a face-to-face approach? In contrast, when discussing the use of telehealth for cancer management, the healthcare professionals in one study assumed and agreed that telehealth 'is an appropriate model that is well received by Indigenous patients'30. How this assumption was made is unclear. For this study, relationship importance was regarding the benefits of telehealth for healthcare professionals. It was reported that telehealth enabled professional relationships and therefore enhanced collaborative care. When clients want face-to-face contact, time, trust and ultimately relationships42, it is difficult to decide on which is the most appropriate model of healthcare delivery for Indigenous peoples. Does the potential of telehealth to bridge a physical divide make it a culturally appropriate and acceptable healthcare model? Further still, can telehealth bridge a cultural health divide?
Strengths and limitations
To our knowledge, this is the first systematic review of studies focused on the use of telehealth for chronic condition management with Indigenous people from around the world. Ambiguity exists regarding a precise definition of both culturally competent care and the holistic management of chronic conditions. The identification of specific aspects of telehealth that are both effective and acceptable for use with Indigenous peoples will assist in guiding health policy and planning. Although every effort was made through our comprehensive systematic search approach to identify all relevant research available, some studies may not have been identified. Furthermore, the studies in this review had methodological limitations. Whilst addressing health economics by assessing the efficacy of telehealth is very important, it was beyond the scope of this study. Recent reviews12,13 suggest inconclusive evidence due to a lack of RCTs, small sample sizes and the absence of quality data and appropriate measures.
Future research
The present evidence highlights gaps in current research regarding the use of telehealth as a modality for health care for chronic condition management with Indigenous peoples. The review provides guidance on the areas to which future research is mostly likely to be useful. The effectiveness of health care for Indigenous peoples has proved to be greatest when aimed at addressing holistic health needs66. This may be addressed by a shift in focus whereby health systems and healthcare professionals value and incorporate the knowledge of communities and individuals with lived experience via community consultation and through embedding Indigenous knowledges into healthcare training. Respectful consultation will highlight the perspective of those who are most affected by telehealth, and in essence will inform more appropriate and acceptable telehealth initiatives43. A better understanding of telehealth approaches and resultant health outcomes is needed42, and similar to other reviews67 we suggest that more rigorous and larger studies of a wider range of Indigenous peoples is needed to produce more conclusive evidence for the effectiveness of telehealth for beneficial health outcomes with Indigenous peoples. It appears that telehealth is promising, but that more work needs to be done to ensure cultural safety and the cultural competence of health professionals and services with research considering the contexts in which telehealth is being used, in a hope that it is conceptualised to uphold culturally safe practices.
Telehealth is a multifaceted concept involving all aspects of the health system. Its implementation and use as a modality to health care is complex and it is experienced differently on all accounts by services, healthcare professionals and end users. In addition, the use of telehealth with Indigenous peoples raises important consideration of cultural appropriateness and acceptability. This review illustrates issues of cultural differences in healthcare delivery. It highlights differing levels of relationship importance as well as the need for community involvement and culturally competent care when incorporating telehealth in service delivery for Indigenous peoples. Recognition and consideration of cultural competencies will support telehealth in progressing beyond simply bridging a physical divide to having a more positive influence on health outcomes for Indigenous peoples. Indigenous peoples have a right to receive health care from culturally competent healthcare professionals and systems. Further still, Indigenous people have the right to experience culturally safe care. This can be facilitated through respectful listening to and meaningful engagement with Indigenous peoples and communities and by the delivery of care by Indigenous people. All stakeholders share in the responsibility for implementing and maintaining effective and acceptable telehealth for Indigenous people requiring chronic condition management.
References
1 Risk factors contributing to chronic disease. Cat No. PHE 157. Canberra: AIHW, 2010.
2 Global status report on noncommunicable diseases 2014. Geneva: WHO, 2014.
3 Inequalities in non-communicable diseases and effective responses. Lancet 2013; 381(9866): 585-597.
4 Australia's health 2014. Australia's health series no. 14. Cat. no. AUS 178. Canberra: AIHW, 2014.
5 Introduction to the practice of telemedicine. Journal of Telemedicine and Telecare 2005; 11(1): 3-9.
6 Telemedicine in the future. Journal of Telemedicine and Telecare 2005; 11(8): 384-390.
7 Telemedicine: opportunities and developments in Member States: report on the second global survey on eHealth. Geneva: WHO, 2010.
8 Home telehealth for diabetes management: a systematic review and meta‐analysis. Diabetes, Obesity and Metabolism 2009; 11(10): 913-930.
9 Home telehealth for chronic obstructive pulmonary disease: a systematic review and meta-analysis. Journal of Telemedicine and Telecare 2010; 16(3): 120-127.
10 The successes and challenges of providing a paediatric burns service by telehealth in Western Australia. Journal of Telemedicine and Telecare 2007; 13(Suppl 3): 63-64.
11 A review of three years experience using email and videoconferencing for the delivery of post-acute burns care to children in Queensland. Burns 2004; 30(3): 248-252.
12 Cost-utility and cost-effectiveness studies of telemedicine, electronic, and mobile health systems in the literature: a systematic review. Telemedicine and e-Health 2015; 21(2): 81-85.
13 Systematic review of studies of the cost-effectiveness of telemedicine and telecare. Changes in the economic evidence over twenty years. Journal of Telemedicine and Telecare 2012; 18(1): 1-6.
14 Indigenous knowledge and the cultural interface. Disrupting preconceptions: Postcolonialism and education. Flaxton, Qld: Post Pressed, 2002; 19.
15 Aboriginal health in Canada: historical, cultural, and epidemiological perspectives. 2nd edn. Toronto: University of Toronto, 2006.
16 Review of American Indian veteran telemental health. Telemedicine Journal and e-Health 2012; 18(2): 87-94.
17 Reaching agreement for an Aboriginal e-health research agenda: the Aboriginal Telehealth Knowledge Circle consensus method. Rural and Remote Health 2010; 10(1). Available: www.rrh.org.au (Accessed 1 August 2015).
18 Eye health programs within Remote Aboriginal Communities in Australia: A review of the literature. Australian Health Review 2008; 32(4): 664-676.
19 Inclusion of underserved racial and ethnic groups in cancer intervention research using new media: A systematic literature review. Journal of the National Cancer Institute - Monographs 2013; (47): 216-223.
20 Current Directions in Videoconferencing Tele-Mental Health Research. Clinical Psychology - Science and Practice 2009; 16(3): 323-338.
21 Health impact assessment of the Northern Territory emergency response. Sydney: Australian Indigenous Doctors' Association, 2010.
22 Cultural safety in nursing: The New Zealand experience. International Journal for Quality in Health Care 1996; 8(5): 491-497.
23 Cultural Competence and Medical Practice in New Zealand. Presented at the Australian and New Zealand Boards and Council Conference, Wellington, New Zealand. 2001.
24 New JBI levels of evidence. Adelaide, SA: Joanna Briggs Institute, 2001.
25 New JBI grades of recommendation. Adelaide, SA: Joanna Briggs Institute, 2013.
26 Satisfaction with telehealth for cancer support groups in rural American Indian and Alaska Native communities. Clinical Journal of Oncology Nursing 2010; 14(6): 765-70.
27 The Internet Diabetes Self-Management Workshop for American Indians and Alaska Natives. Health Promotion Practice 2011; 12(2): 261-270.
28 Successful implementation of a telemedicine-based counseling program for high-risk patients with breast cancer. Mayo Clinic Proceedings 2013; 88(1): 68-73.
29 Evaluation of an ear health pathway in remote communities: improvements in ear health access. Australian Journal of Rural Health 2014; 22(3): 127-132.
30 Teleoncology for Indigenous patients: The responses of patients and health workers. Australian Journal of Rural Health 2012; 20(5): 265-269.
31 Acceptability of telepsychiatry in American Indians. Telemedicine and e-Health 2008; 14(, 5): 461-466.
32 Results of a telehealth-enabled chronic care management service to support people with long-term conditions at home. Journal of Telemedicine and Telecare 2012; 18(3): 172-175.
33 Online diabetes self-management program: A randomized study. Diabetes Care 2010; 33(6): , 1275-1281.
34 Comparing the effectiveness of telemedicine , and traditi, onal surveillance in providing diabetic retinopathy screening examinations: A randomized controlled tria. Telemedicine and e-Health 2013; 19(12): 942-948.
35 Long-term comparative effectiveness of telemedicine in providing diabetic retinopathy screening examinations: A randomized clinical trial. JAMA Ophthalmology 2015; 133: 518-525.
36 Videoconferencing could reduce the number of mental health patients transferred from outlying facilities to a regional mental health unit. Australian and New Zealand Journal of Public Health 2012; 36(5): 478-482.
37 Using participatory action research to assist heart failure self-care amongst indigenous Australians: A pilot study. Action Learning and Action Research 2013; 19(2): 40-60.
38 Characteristics of telemental health service use by American Indian Veterans. Psychiatric Services 2012; 63(2): 179-181.
39 Program evaluation of remote heart failure monitoring: Healthcare utilization analysis in a rural regional medical center. Telemedicine and e-Health 2015; 21(3): 157-162.
40 Control of type 2 diabetes mellitus using interactive internet-based support on a Northern Plains Indian reservation: A pilot study. Topics in Clinical Nutrition 2007; 22(2): 185-193.
41 The association between e-mail messages and health outcomes in diabetes patients. Human Communication Research 2013; 39(2): 252-268.
42 Patient and provider perspectives on using telemedicine for chronic disease management among native Hawaiian and Alaska native people. International Journal of Circumpolar Health 2013; 72(Suppl. 1): 930-936.
43 Conversations on telemental health: Listening to remote and rural first nations communities. Rural and Remote Health 2011; 11(2): 1-19. Available: http://www.rrh.org.au (Accessed 1 August 2015).
44 Dismantling sociocultural barriers to eye care with tele-ophthalmology: Lessons from an Alberta Cree community. Clinical and Investigative Medicine 2013; 36(2): E57-E63.
45 'It's mean!' the views of young people alienated from mainstream education on depression, help seeking and computerised therapy. Advances in Mental Health 2012; 10(2): 195-203.
46 Telepsychiatry with rural American Indians: Issues in civil commitments. Behavioral Sciences & the Law 2008; 26(3): 287-300.
47 Teleophthalmology for first nations clients at risk of diabetic retinopathy: a mixed methods evaluation. JMIR Medical Informatics 2015; 3(1): e10.
48 Factors influencing mental health providers' intention to use telepsychotherapy in First Nations communities. Transcultural Psychiatry 2013; 50(2): 323-343.
49 The diffusion of telehealth in rural American Indian communities: a retrospective survey of key stakeholders. Telemedicine Journal and E-health 2012; 18(1): 60-66.
50 Role of telehealth/videoconferencing in managing cancer pain in rural American Indian communities. Psycho-Oncology 2012; 21(2): 219-223.
51 Communication plays a critical role in web-based monitoring. Journal of Diabetes Science and Technology 2009; 3(3): 461-467.
52 The feasibility of a community-based mobile telehealth screening service for Aboriginal and Torres Strait Islander children in Australia. Telemedicine Journal & E-Health 2010; 16(9): 950-956.
53 Expanding the walls of the health care encounter: Support and outcomes for patients online. Health Communication 2011; 26(2): 125-134.
54 Accuracy of pre-recorded video images for the assessment of rural indigenous children with ear, nose and throat conditions. Journal of Telemedicine and Telecare 2006; 12(Suppl. 3): 76-80.
55 Feasibility of remote CT colonography at two rural Native American medical centers. American Journal of Roentgenology 2010; 195(5): 1110-1117.
56 Diagnostic reliability of telepsychiatry in American Indian veterans. American Journal of Psychiatry 2007; 164(1): 115-118.
57 Key components of a well functioning health system. 2010. Available: http://www.who.int/healthsystems/EN_HSSkeycomponents.pdf (Accessed 11 November 2015).
58 Developing the Native People for Cancer Control Telehealth Network3. Telemedicine Journal & E-Health 2011; 17(1): 30-4.
59 The University of Hawai'i Rural Health Collaboration: partnerships to provide adult telepsychiatry services. Psychiatric Services 2010; 61(10): 961-963.
60 A modeled economic analysis of a digital tele-ophthalmology system as used by three federal health care agencies for detecting proliferative diabetic retinopathy. Telemedicine Journal & E-Health 2005; 11(6): 641-651.
61 Understanding health and illness: research at the interface between science and indigenous knowledge. International Journal of Epidemiology 2004; 33(5): 1138-1143.
62 Health care access for Aboriginal and Torres Strait Islander People living in urban areas, and related research issues: a review of the literature. Darwin: Cooperative Research Centre for Aboriginal Health, 2008.
63 Confronting institutionalized racism. Phylon (1960-) 2002; 7-22.
64 Mental health professionals' perspectives of telemental health with remote and rural First Nations communities. Journal of Telemedicine & Telecare 2011; 17(5): 263-267.
65 Occupational therapy at the 'cultural interface': Lessons from research with Aboriginal and Torres Strait Islander Australians. Australian Occupational Therapy Journal 2011; 58(1): 11-16.
66 National Aboriginal and Torres Strait Islander Health Plan 2013-2023. Canberra: Commonwealth of Australia, 2013.
67 Methodologies for assessing telemedicine: a systematic review of reviews. International Journal of Medical Informatics 2012; 81(1): 1-11.



