full article:
IntroductionMuch of regional Australia continues to face challenges in recruitment and retention of medical practitioners, despite the apparently successful rural medical education initiatives funded by the Commonwealth Government. These initiatives include rural clinical schools, increased selection and support for rural background students and a 236% increase in domestic medical students since 1999 1. The number of medical graduates in regional communities has increased, and some rural communities have benefited, but those with greater disadvantage, and remote communities, do not appear to have benefited to the same extent 2-4.
International fee-paying (IFP) medical students are a significant component of Australian medical education, contributing additional income and increasing diversity in the cohort. Their contribution to the Australian medical workforce is harder to determine. About 73% remain in Australia for at least some postgraduate training, with their interest in remaining increasing during primary training. Influences include acculturation, positive education and clinical training experience, wanting to secure full registration through completion of their internship year, influence of partner, and concern about availability and quality of training positions in their home countries5. Most of those leaving before internship are on government sponsorships with obligatory return of service in their countries of origin; these were mostly from Malaysia. There are some ethical concerns about the 'brain drain' effect of recruiting international medical graduates from developing nations, where needs may be greater6; this may be less relevant to those who self-fund an Australian education.
Since 1999, the number of IFP graduates in Australia has increased by 242%1. In 2015, a total of 3547 students graduated from Australian medical schools, (13.9%) of them IFP students. Since 2003, Australian immigration policy has allowed IFP graduates to remain in Australia to obtain registration and then apply to remain as skilled migrants. With the substantial increase in domestic medical graduates, there are fewer intern positions than graduates, and domestic graduates usually have first preference. IFP graduates often receive late offers for positions not filled by domestic graduates, often in less popular regional or private hospitals.
The Australian island state of Tasmania, with its small and decentralised population, reflects the national position, although it has some unique features. Distances are smaller and the quality of life is regarded as high, but there are significant shortages of both hospital-based specialists and general practitioners outside of the two major regional cities. The impact is greatest in the north-west region, where health services rely on expensive locums to provide core services7.
The University of Tasmania School of Medicine commenced in 1965. Initially small and Hobart-based, it has progressively increased clinical training capacity in the north and north-west regions. This was expanded further about 10 years ago with the establishment of the rural clinical school in north-west Tasmania and the Launceston clinical school. Since 1985, the Australian Medical Council has accredited all primary medical education against one set of national standards. While most medical schools have transitioned to a mostly graduate-entry master's degree, the Tasmanian medical school retains a school-leaver entry program. Students undertake a 5-year double bachelor degree (MBBS): their first 3 years are based in Hobart, after which they elect to spend their final two program years at the Hobart clinical school (50 per cohort), the Launceston clinical school (40) or the rural clinical school (25). In the early years, a limited number of IFPs were able to study at the rural clinical school. Not all specialist training is offered within Tasmania and only a few training schemes can be completed entirely in Tasmania, eg general practice, anaesthetics, general medicine and emergency medicine.
In 2014, the authors found that 51% of Tasmanian graduates (2002-2013) who elected Hobart or Launceston for their final two training years were working in a major city (Modified Monash 1 category; see Methods) in mainland Australia, compared to 42.7% of students who elected the rural clinical school, and around 37% of graduates overall were working in Tasmania2. Recognising the potential contribution of IFP students to the Tasmanian medical workforce, the authors sought better understanding of their career intentions, work locations and factors that contribute to these choices. This was explored in two ways: a qualitative study exploring graduating students' intentions and factors that contribute to their decisions about work location choices following graduation, and a quantitative study of the locations of all IFP graduates from the Tasmanian medical program.
Methods
Sampling
All IFP student graduates of the Tasmanian medical program between 2000 and 2015 were identified from university records and their 2016 work locations were obtained from the Australian Health Practitioner Registration Authority (AHPRA) website.
Measure of rurality and remoteness
The Modified Monash (MM) categorisation system is the most recent used to assist in administration and funding of national health workforce programs. The population of a community and its distance from the nearest major centre are combined to produce a measure of its 'rurality' or 'remoteness'. Under the MM classification system, locations categorised as MM5-MM7 are considered districts of medical workforce shortage.
Data analysis
Each graduate's 2016 work location postcode was matched to an MM category using the Doctor Connect website. The data were imported into Stata 14 (StataCorp; http://www.stata.com) for descriptive analyses. Students living overseas, or with missing 2016 work location details, were excluded from the analysis of 2016 workplace rurality (MM category). It is likely that most of the students with missing 2016 workplace locations were living overseas, although some may have changed their name since graduation and were therefore not able to be traced through the AHPRA website. Crosstabs were used with χ2 tests to investigate differences in proportions for categorical data, with differences accepted as significant at p<0.05.
Student intentions
All 20 international students in the final year of the Tasmanian medical program in 2015 were invited to participate in semi-structured interviews during their final months of the program. The questions explored their career intentions, both specialty and geographic preferences, and how these may have changed during the program. At the time of the interview, students were asked to assess how well they felt they had assimilated to the local community, on a scale of 1 ('least') to 10 ('most'). A brief follow-up telephone contact was made during their intern year in 2016 to confirm their location. Interviews were transcribed and checked. Thematic analysis was performed using a hybrid approach as described by Boyatzis8: inductive analysis of the raw data to identify themes; and categorising the themes according to a previously identified framework of 'professional', 'social' or 'location' factors affecting the career intentions of rural specialists9.
Ethics approval
Approval for this study was granted by the Tasmanian Higher Research Ethics Committee (H0013913 and H15136).
Results
A total of 261 international students graduated from the Tasmanian medical program from 2000 to the end of 2015, with numbers each year increasing from 9 in 2000 to about 20 as from 2010.
Mean age at graduation was 25.5 (standard deviation 3.2) years, with 142 (54.4%) male and 119 (45.6%) female. Over half (55.2%) were from Malaysia, with the second largest group (16.1%) from Singapore (Table 1). Nineteen (8.3%) students completed their secondary education (year 12) in Tasmania, with 13 students attending schools in Hobart.
Forty-eight (18.4%) graduates were in their first or second postgraduate year (PGY1 or 2) and 213 (81.6%) were PGY3 or greater. Thirty-five graduates had a registered specialist qualification, 28 of them living in Australia. The most common specialty was general practice followed by anaesthesia (Table 2). A substantial number (226, 86.6%) had no specialty recorded, most likely due to incomplete specialist training.
Work location in 2016 was available for 196 (75.1%) graduates. Of these, 189 (72.4 %) were working in Australia, three in Singapore, two in New Zealand, one in the UK and one in Malaysia. The most common locations of IFP graduates in Australia were Victoria (47, 24.9%), Tasmania (42, 22.2%) and New South Wales (27, 14.3%) (Table 3). Eight international graduates, all in PGY1 or PGY2, were working in north-west Tasmania, near the rural clinical school.
In 2016, 126 (67.7%) international graduates in Australia were working in areas categorised as MM1 (Table 4). There was no association between gender and MM location, with 68.8% of women and 67.0% of men working in major cities (MM1 area) (χ2(1)=0.1, p=0.79). A greater proportion of recent graduates (PGY1 or 2) were working in Tasmania compared to those ≥PGY3 (71.4% vs 11.0%, χ2(1)=60.2, p<0.0001), while those ≥PGY3 were more likely to be working in major cities (77.3% vs 25.7%, χ2(1)=34.7, p<0.0001). Only four international graduates ≥PGY10 were working in Tasmania (Fig1).
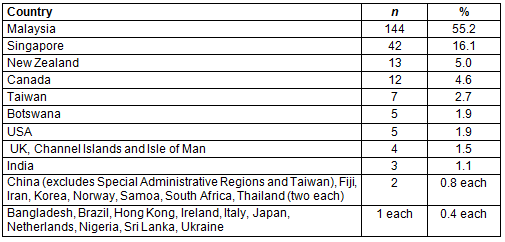
Table 2: Graduate specialty, as recorded by Australian Health Practitioner Registration Authority, of international medical students graduating from University of Tasmania School of Medicine, 2000-2015
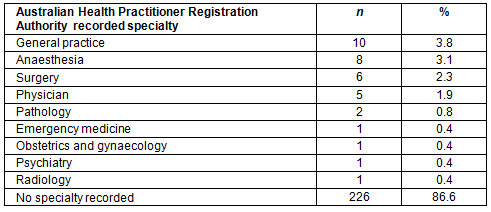
Table 3: State/territory of residence/work for international medical students graduating from University of Tasmania School of Medicine, 2000-2015, living in Australia in 2016 (n=189)
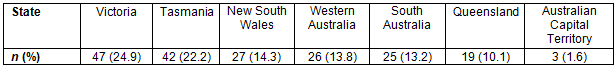
Table 4: Rurality of 2016 workplace location (using Modified Monash) for international medical students graduating from University of Tasmania School of Medicine, 2000-2015, living in Australia in 2016 (n=189)

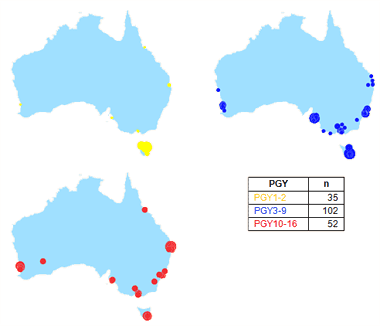
Figure 1: 2016 work location (postcode) of international students graduating from University of Tasmania School of Medicine, 2000-2015.
Student intentions
In 2015, 15 (8 females and 7 males) of the 20 final year international students agreed to participate, 14 face to face and 1 by telephone. In 2016, 12 (6 female and 6 male) participants were able to be contacted for follow-up.
On applying to medical school, six of the participants intended to remain in Australia following graduation, but by their final year all 15 participants intended to remain for at least their intern year. Two students who intended to remain in Australia on entry to medical school attended one or more years of secondary schooling in Australia. All students scored their assimilation at 5-10 (mean 7.27), with students who had spent time at secondary school in Australia scoring highest (10). The biggest barrier to assimilation was the lack of time for extracurricular activity due to their heavy academic workload.
The factors influencing choice of postgraduate work location identified by students could be grouped under three themes: 'professional', 'social' and 'location'9.
Professional factors: The professional factor most influencing decisions to remain was workplace culture. Participants felt that they would 'fit' and be treated better in the Australian system than in their home country.
I think that things are changing in third and fourth years, we actually had clinical experience so it wasn't actually just lectures and you know, lectures I can get anywhere. The experience of the actual clinical environment and seeing the work ethics and the communication between the doctors, I think has helped influence my decision quite a bit. Because I've also had electives and selective placements back home so I've seen how the culture is and I have to say it's quite a bit different. Sometimes a bit questionable I'd say. You hear stories about how some people teach by humiliation and that's not actually uncommon back home. (participant 14, female)Most students were happy to stay for their intern year in the community where they completed the program, due to familiarity with the local hospital. As they were eligible for an intern position offer in Tasmania only after domestic student preferences were filled, some students strategically chose rural locations because they were less popular.
I did my fourth and fifth year in [this place] and I really enjoyed it. I had a couple of consultants in the hospital who actually became my role models. I think that's one of the main factors why I'm staying - why I'm choosing to stay to learn from them and I think it's a good hospital, internship wise. (participant 2, male)
Availability of specialist training opportunities were important. Most participants were intending to pursue specialties for which training was not available in Tasmania, and would have to pursue a metropolitan training program on the mainland.
... I'm trying to proceed my advanced training. Then I would obviously need a bigger hospital, with better facilities, where I can get more exposure with more patients and more advanced technologies available. (participant 7, male)Social factors: Social factors influenced both staying and leaving. Being near family or a partner, or having the opportunity of meeting a potential partner, was the main influencing social factor. Seven students (all female) intended to return to their home country at some stage to be near family.
My parents are getting older and at some point I will need to take care of them - either bringing them here or - it just depends. (participant 15, female)Obligations to family or their country were factors for some students:
Yes, I mean there'll be reasons why I'd go back. It would be mostly family. In terms of job-wise, environment-wise I still prefer to stay. (participant 12, female)
I think the main thing is tuition fees, because as an international student, our tuition fees are quite high. It's very expensive. So, I thought that - because I'm on the Father-Mother Scholarship [parents paying for tuition fees] and I'd like to pay back them after I graduate, it's not quite possible to earn back the same amount in a short period of time if I go back because of our currency exchange rate. So, it's more ideal to stay back in Australia to earn back the tuition fee. (participant 8, F)Students who had a positive rural experience during their training entertained the possibility of choosing a rural location after graduation but perceived working in a rural location would reduce their chance of meeting a potential partner.
I think I would like to work in [a rural area] if I have a family, because I think I'm currently not attached so maybe it's a bit harder to meet someone. (participant 10, F)Location: Students from Singapore were used to city living, and favoured a shift back to a large city. Only two of the fifteen students, both from Malaysia, had a firm preference for working in a regional or rural location, but their partner's preference or work commitments meant this needed to be negotiated. Access to infrastructure, particularly international airports for faster access to travel for family visits, was one of the main drivers for most of choice of location.
... probably if I need to travel back to Malaysia for emergency reasons I'll have longer transit time and have to travel for longer time to get there. (participant 5, female)Discussion
I'd really like to work in a metro hospital, Melbourne, Sydney hopefully. If not, Perth or Brissy [Brisbane, in Queensland] would be all right, or even Adelaide [in South Australia] I guess. (participant 6, male)
International medical students make an important contribution to Australian medical education and the Australian medical workforce. A substantial proportion of IFP graduates from the Tasmanian medical program remain in Australia following graduation even though this was, for many, a change in intention since commencing the program. After internship, most move to mainland metropolitan centres.
The profile of international students in the Tasmanian medical program is similar to the national profile, with Malaysia and Singapore being the top two sources of students5. However, the movement pattern is different to that reported for Tasmanian graduates as a whole. Only 22% of those traced were working in Tasmania, compared with about 36% of all Tasmanian graduates over a 42-year follow-up period10. This indicates that IFP graduates play a less substantive role in the state's medical workforce. Further, very few were working outside of MM1 and MM2 communities, indicating that IFP graduates play an almost insignificant role in developing a medical workforce for rural and remote communities.
The reasons for this pattern are related to access to social and family support, and to opportunities for postgraduate specialty training, which are restricted in a small health economy such as Tasmania's. Social and professional factors are similar to those found by Hawthorne and To5; however, location factors play a greater role in IFP graduates leaving Tasmania because they seek locations with more direct travel access to their home countries. Because a majority of graduates had not yet completed specialty training, this pattern may change as they find positions, although low numbers in general practice and rural medical practice may change less because those training programs are available in Tasmania.
For medical programs with a strong rural focus, this study highlights an emerging tension between internationalisation and the medical school's obligation to supply local and rural workforces. The fixed factors that influence IFP graduate' place of work such as proximity to major international airports cannot be changed to promote working in rural areas. Increasing specialist training opportunities in rural areas may encourage both IFPs and domestic graduates to stay rurally. Where rural training places are limited, expanding the rural health workforce will be best served by prioritising students most likely to stay rurally. The strongest predictor appears to be a rural background, fostered through positive rural training experiences10-12. However, the exclusion of international students from many of the rural medical education initiatives, such that these students may not be prepared or encouraged to consider rural careers, may also represent a lost opportunity.
Limitations
The authors could not trace the location of 25% of graduates, and the 2016 workplace location was reliant on AHPRA registration data, so graduates who have left Australia, changed their names or ceased practice could not be included. Had they been included, the contribution of international graduates to the Tasmanian workforce may be proportionately lower - as low as 16% compared to 22% reported. The IFP students available for interview were restricted to final-year medical students in a single year, and it is possible that their career preferences and influences may be different to those of students trained in the early 2000s.
Conclusions
International student graduates from the Tasmanian medical school make an important contribution to both local medical education and the Australian medical workforce. However, the contribution to the Tasmanian and rural Australian medical workforces is small, because most move after early postgraduate experience to mainland metropolitan locations, which are more accessible to their home country and specialist training opportunities. Rurally focused medical programs may need to reconsider how they manage IFP students. Offering rural postgraduate training opportunities that target those graduates most likely to stay in the rural workforce seems to be the most likely strategy to enhance rural retention in Tasmania.
Acknowledgements
The authors acknowledge the IFP graduating students who took part in the qualitative interviews with candour.
References





