Introduction
The current shortage of 340 full-time equivalent rural GPs (more than 10% of the current rural doctor workforce) in Australia cannot be addressed in the short term by policy and program initiatives aimed at bolstering national self-sufficiency. The major reasons for this relate to the globalization and feminization of the medical workforce, changing work practices of GPs, as well as the rising level of care demanded by an increasingly ageing population1,2. Faced with this situation, key stakeholders, including local, state and federal governments, professional organizations and support agencies developed and implemented a range of educational, funding and regulatory programs aimed at recruiting GPs to rural areas.
Seen from this perspective, the recruitment of international medical graduates (IMGs) to Australia to fill this shortage will continue. They will form an integral and essential part of medical workforce planning with, for example, the number of visas issued to temporary resident doctors, who do not require Australian Medical Council (AMC) accreditation, having increased from 664 in 1993/1994 to 2496 in 200220/033. Currently, IMGs constitute 21% of the Australian medical workforce and over 30% of the remote area medical workforce4,5. The proportion of IMGs practising in Australia is similar to that found in the USA (27%), Canada (23%) and the United Kingdom's National Health Service (24%)5-7. By 2007, the Commonwealth Government aims to add a further 725 full-time equivalent IMGs8.
Increasing numbers of overseas-born medical undergraduates can be expected to undertake part of their training in our region in coming years and greater numbers of IMGs can be expected to commence practice in this region. It is therefore most appropriate to carry out an evaluation of how the education, training and support needs of overseas born medical (under) graduates and IMGs are catered for in our region. As there is a debate as to whether the education, training and support needs of IMGs and other doctors are really different5,9-13, this project aimed to document the current education, training and support needs of IMGs, as well as all other registrars and GPs who currently train and/or practise in our region. For the purposes of discerning differences in these needs, this project also aimed to identify such needs on the basis of gender. This will allow an analysis of relevant responses according to the following three pairs of groups which can be compared:
- IMGs and doctors whose primary medical qualification was obtained from an Australian medical school
- GPs and registrars
- Male and female doctors.
Method
Subsequent to a review of published and relevant literature, two questionnaires were designed; one to be completed by IMGs and the other by GPs whose primary medical qualification was obtained from an Australian medical school. As there is no systematic record that identifies where (in Australia or overseas) a GP's or registrar's primary medical degree was obtained, in August 2004 all GPs and registrars were sent both questionnaires, a cover letter and a reply-paid envelope. A second mail-out, targeting all those GPs who had not returned a completed survey form by the due date, was administered in late 2004. Participants were asked to self-select the appropriate survey form. Both questionnaires contained two main sections: one focusing on demographic and practice issues and the other dealing with information and support programs. The IMG questionnaire incorporated all the 21 questions asked for respondents whose primary medical degree was from an Australian medical school, and also contained additional questions which related to visa and registration matters and ease of commencing medical work in Australia. The draft survey forms were piloted on a sample of GPs who were not included in the study's population.
Names and addresses of the region's practicing GPs were obtained from the three local Divisions of General Practice. The list of the region's registrars, consisting of GP registrars and junior medical officers working in the region's hospitals, was held by the Hunter New England Area Rural Training Unit.
All data were entered and analysed using the SPSS v12.0.1 statistical software package (SPSS Inc, Chicago, IL, USA). Differences between, for example, IMGs and Australian-trained doctors were calculated in respect of selected variables by way of non-parametric χ2 and, in all cases where the expected frequency count in one or more cells was less than five, Fisher's exact tests.
Approval to carry out each project was given by the Hunter New England Health Ethics Committee in 2004.
Results
Eighty-three (56%) of the 149 GPs and 31 (47%) of the 66 registrars surveyed, returned completed questionnaires. The study's full results and some of the project's major findings are published elsewhere14,15.
For purposes of further data analyses, the 114 responses were also grouped into IMGs (20), Australian medical graduates (94), GPs (83), registrars (31), and respondents who were male (69) or female (45).
Participants were asked to indicate whether they would welcome additional information in relation to eight separate issues. The top three issues identified related to the Australian healthcare system, Indigenous health and key rural health issues (Fig 1). Comparing the responses of the relevant target groups, the following statistically significant differences were found in relation to further information requested concerning:
- the Australian health care system:
- proportionately more registrars than GPs would welcome such additional information (χ2 = 21.9, df = 1, p <0.01)
- proportionately more IMGs than Australian-trained doctors requested further information (χ2 = 7.1, df = 1, p <0.01).
- indigenous health:
- proportionately more registrars than GPs would welcome additional information on this topic (χ2 = 4.4, df = 1, p = 0.035)
- while not reaching statistical significance (p<0.05), a much larger proportion of IMGs than Australian-trained doctors would welcome such additional information (χ2 = 3.7, df = 1, p = 0.056).

Figure 1: Major information deficits.
All participants were asked whether any of the six programs (advanced business practices, advanced communication skills, clinical skills, consultation skills, cultural training and research skills), offered by a professional organisation, would assist them in furthering their professional career. The most frequently nominated programs were advanced business practices, clinical skills and consultation skills (Fig 2). The percentages listed in Figure 2 reflect the percentage of participants who indicated that such a program would meet one of their professional needs. Statistically significant differences were found between the responses provided by GPs and registrars in relation to:
- clinical skills training with proportionately more registrars requesting such training (χ2 = 4.3, df = 1, p =0.04)
- consultation skills with proportionately more registrars asking for further assistance (χ2 = 6.6, df = 1, p =0.01).
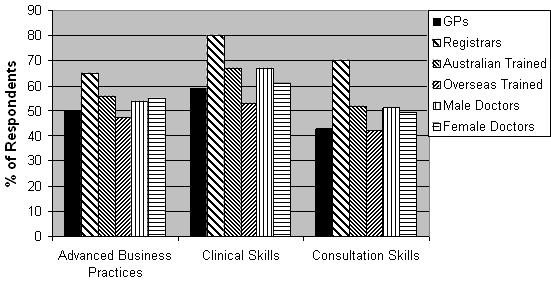
Figure 2: Major programs requested to further professional career.
All participants were asked which issues would need resolving as a matter of priority to better meet their professional needs, ranging from 1 (low priority) to 3 (high priority). The top three priority issues relate to continuing professional development, training opportunities and professional support (Fig 3).
For purposes of data presentation, the four Likert scale categories (1 = very dissatisfied, 2 = dissatisfied, 3 = satisfied, 4 = very satisfied) available to participants in terms of expressing their level of satisfaction with their current medical practice were collapsed into just two categories. The new category 'dissatisfied' combines the total percentage of respondents expressing being either very dissatisfied or dissatisfied. The new category 'satisfied' combines the total percentage of respondents expressing being either satisfied or very satisfied.
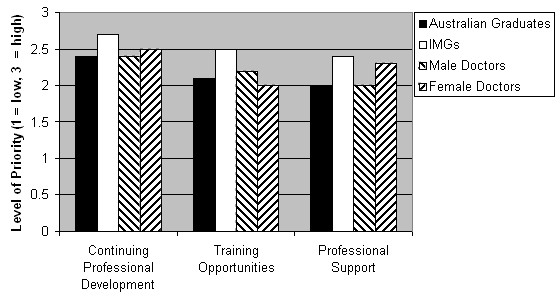
Figure 3: Top professional priority issues.
Figure 4 illustrates the proportion of doctors according to their level of satisfaction with their current medical practice. Overall, the vast majority (86%) of all respondents were either very satisfied/satisfied with their current medical practice. The highest proportion (95%) are IMGs and the lowest proportion (84%) were Australian-trained and male doctors.
There were no statistically significant differences between the following groups of doctors in terms of being either satisfied or dissatisfied:
- GPs and registrars (Fisher's exact, two sided: p = 1)
- Australian trained doctors and IMGs (Fisher's exact, two sided: p = 0.3)
- male and female doctors (χ2 = 0.4, df = 1, p = 0.53).
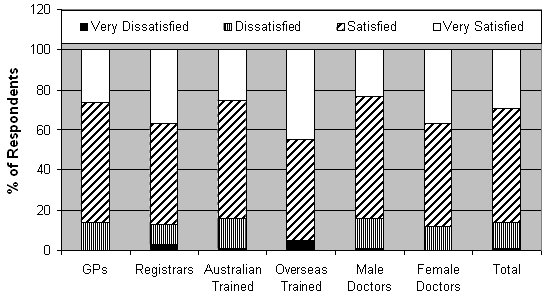
Figure 4: Level of satisfaction with current medical practice.
The average intended length of remaining in rural practice is 40% longer for those doctors who are satisfied with their current medical practice than for doctors who are not satisfied (11.5 years compared to 8.2 years). Figure 5 illustrates that, at every time interval for which comparable data is available, proportionately more doctors who were satisfied with their current medical practice intend to stay in rural areas than doctors who were dissatisfied.
The four Likert scale categories (1 = very discontented, 2 = discontented, 3 = contented, 4 = very contented) available to participants in terms of expressing their level of contentment with life as a rural doctor were collapsed into two categories. The new category 'discontented' combined the total percentage of respondents who expressed being either very discontented or discontented. The new category 'contented' combined the total percentage of respondents who expressed being either contented or very contented.
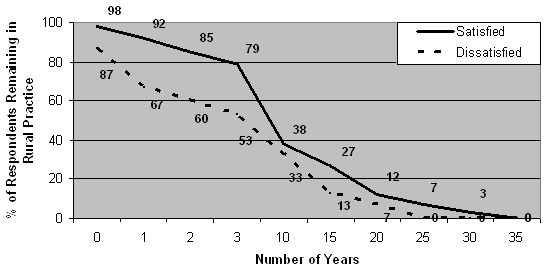
Figure 5: Number of years intending to stay in rural practice by satisfaction with current medical practice.
Figure 6 illustrates the proportion of doctors who were either contented or discontented with life as a rural doctor. Overall, the vast majority (83%) of all respondents were satisfied with their current medical practice. The highest proportion (89%) were IMGs and the lowest proportion (81%) were registrars.
There were no statistically significant differences between the following groups of GPs in terms of being either contented or discontented:
- GPs and registrars (χ2 = 0.17, df = 1, p = 0.68)
- Australian-trained doctors and IMGs (Fisher's exact, two sided: p = 0.52)
- male and female doctors (χ2 = 0.06, df = 1, p = 0.81).
The average intended length of remaining in rural practice was 51% longer for doctors contented with their life as a rural doctor than for those doctors who were discontented (11.8 years compared with 7.8 years). Figure 7 illustrates that, at each time period for which comparable data was available, proportionately more doctors who were contented, intended to remain in rural practice.
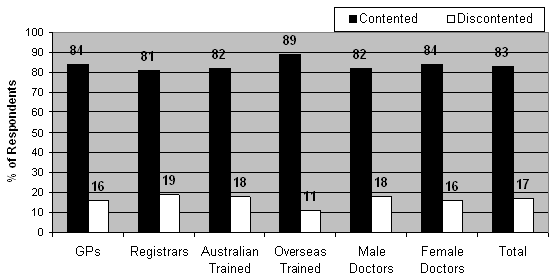
Figure 6: Level of contentment with life as a rural doctor.
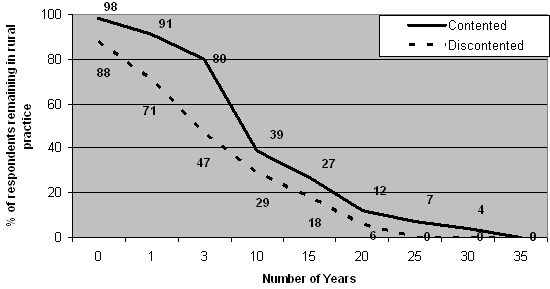
Figure 7: Number of years intending to stay in rural practice by contentment with life as a rural GP.
Discussion
Retaining rural doctors in rural practice depends on satisfactorily addressing a range of professional and non-professional items16,17. In a recent article, systematic and organized professional support mechanisms, as well as good educational facilities for their children and work opportunities for their partners, were identified as significant factors contributing to IMGs remaining in rural practice18.
Our results highlight that the most important education, training and support needs identified by all the participants relate to:
- more detailed information in the areas of Indigenous health and key rural health issues being made available
- programs in respect of advanced business practices, clinical skills and consultation skills being provided by appropriate professional organizations
- continuing professional development, training opportunities and professional support being offered.
These results do not concur with other research findings which suggest that, 'interventions not affecting on-call and related professional issues will not solve the key problem'19. An explanation for this may be found in the fact that a very high proportion of the doctors responding to our survey indicated that they were either satisfied/very satisfied (86%) with their current medical practice or contented/very contented (83%) with their life as a rural doctor. These high proportions hold true for male and female doctors as well as registrars, and are well in excess of the 75% of GPs and 65% of registrars expressing being either satisfied/very satisfied and the 77% of GPs and 60% of registrars indicating being contented/very contented in a recent survey of rural doctors20. Furthermore, our respondents also expressed a very high level of satisfaction (rating of 3 or higher on a four-point Likert scale) with professional support organizations, especially the Australian College for Rural and Remote Medicine, the NSW Rural Doctors' Network, the local Divisions of General Practice and the regional Training Consortium9.
Compared with their Australian-trained colleagues, an even higher proportion of the region's IMGs were satisfied/very satisfied (95% compared with 84%) and contented/very contented (89% compared with 82%). Our region's IMGs were also well satisfied with the support available from relevant support organizations. The fact that responses from the participating IMGs were, in general, similar to those provided by doctors whose primary medical degree was obtained from an Australian medical school may also be due to the following:
- unlike the situation in Australia as a whole, where most IMGs hold temporary visas21, 88% of this region's IMGs were permanent residents and 76% of IMGs held a general registration
- a much higher AMC exam pass rate than their counterparts practising in Australia (about 85% for this region's IMGs compared with approximately 56% for IMGs working in Australia)22.
Our results lend support to an approach which endeavours to meet the education, training and professional support needs of the region's medical workforce by focusing on identified priority needs of the region's medical workforce as a whole, rather on the variations between the various target groups, be they GPs, registrars, male, female, Australian or overseas trained doctors. Such a strategic approach to retaining our region's doctors is most appropriate due the following major reasons:
- high demand for specific, advanced professional courses across all target groups
- high levels of satisfaction with current medical practice across all target groups
- high levels of contentment with life as a rural doctor across all target groups.
Such a focus does not detract from benefits arising from the development of more comprehensive strategies aimed at specific target groups, such as, for example, IMGs or female doctors. Rather, it contends that such specifically targeted strategic interventions be made available to all our region's doctors who wish to benefit from them, be it on the basis of the doctor's situated learning and living environments and/or modality, format, timing and location of strategies being offered23,24. The following two examples may serve as illustrations of this point.
A workshop, held in 2003, focused on the education and training needs of IMGs and debated many issues which would assist IMGs in their early years of training and support them in unsupervised practice. Nevertheless, the participants concluded that many of these major problems facing IMGs '...are also issues for local graduates. Wherever possible, initiatives to aid overseas trained doctors should be integrated into the broader system to support all doctors'13.
A 2004 report demonstrating the value of a systematic gender analysis in respect of pertinent issues relating to sustainable rural practice, concluded that:
The future trend will be for an increasing proportion of female rural doctors and they will require flexible professional and practice structures that allow them to be women as well as doctors'20.
While facilitating and effectively implementing these two strategies are deemed to significantly increase the level of professional satisfaction and contentment for female rural, GPs, the report's data also demonstrated that these same two strategies are assessed by male rural GPs as being of equal statistical significance in increasing their professional satisfaction and contentment20.
Limitation of study
The response rate (56%) concerning GPs was adversely affected by the policy decision of one of the three Divisions of General Practice not to provide names and addresses of its GPs to any outside organization. This resulted in this Division administering the distribution of the survey forms pertaining to their GPs. This Division's GPs' response rate (38%) was well below the response rate of GPs working in the other two participating Divisions (60% and 69%, respectively).
While the overall GPs' response rate (56%) is acceptable, no assessment as to any response bias (eg age, gender, number of sessions working per week and years of practice in this region) can be made. This is due to the fact there is no accessible data available which lists whether a GP's first medical qualification has been obtained overseas or not. While generalisability to the region is not given, the sheer number of responses received from IMGs (20) and Australian medical graduates (94) means that any programs developed on the basis of these responses will find a receptive target audience, as well as stretch resources available for effective program delivery.
While meeting this region's doctors' professional needs is crucial in retaining rural GPs, there are a range of non-professional needs, including work opportunities for partners, access to good educational facilities for their children, availability of good housing, social and cultural facilities, which will also have a bearing on whether currently practising doctors will remain in our rural area16-19. While this project did not attempt to address these matters, a previous project carried out in this region, documented the importance of such non-professional factors in a doctor's decision to remain in rural practice25. A recent qualitative study focusing on factors impacting on IMGs' ability to integrate into their rural communities demonstrated, in part, the importance of a supportive community environment which caters for the social, cultural, education and employment needs of these doctors and their families18. Until such a project is carried out in our region focusing on such community, family and personal issues impacting on a doctor's decision to remain or leave rural practice, no conclusion can be drawn as to whether this region's IMGs' assessment in respect of such non-professional needs differs sufficiently from their colleagues who have obtained their first medical degree in Australia to warrant special consideration.
Implications
Our results illustrate that being able to successfully meet the identified education, training and professional support needs will contribute significantly to all our region's GPs, and not just IMGs, being retained in rural practice. Our findings support the notion that, wherever possible, a fully integrated strategic approach, focusing on meeting the doctors' professional needs should guide the development and implementation of relevant, comprehensive retention strategies for the region's rural doctors.
References
1. Australian Institute of Health and Welfare 2005. Medical labour force. AIHW cat no HWL 32. Canberra: AIHW, 2003.
2. Brooks PM, Lapsley HM, Butt DB. Medical workforce issues in Australia: 'tomorrows doctors - too few, too far'. Medical Journal of Australia 2003; 179: 206-208.
3. Birrell B, Hawthorne L. Medicare Plus and overseas trained doctors. People and Place 2004; 12: 83-99.
4. Australian Department of Health and Ageing. Productivity Commission Health Workforce Study. (Online) 2005. Available: http://www.pc.gov.au/study/healthworkforce/subs/sub009.rtf (Accessed 1 January 2006).
5. Confederation of Postgraduate Medical Education Councils. Information and resources relating to education and training available to overseas trained doctors in Australia. Melbourne: CPMEC Administration, 2004.
6. McMahon GT. Becoming a physician: coming to America - international medical graduates in the United States. New England Journal of Medicine 2004; 350: 2435-2437.
7. Buske L. Canada's cosmopolitan medical profession. Canadian Medical Association Journal 2002; 166: 1320.
8. Australian Department of Health and Ageing. Drawing on qualified health professionals from overseas. (Online) 0000. Available: http://www.health.gov.au/ (Accessed 12 June 2007).
9. McGrath BP. Integration of overseas-trained doctors into the Australian medical workforce. Medical Journal of Australia 2004; 181: 640-642.
10. Sullivan EA, Willcock S, Ardzejewska K, Slaytor EK. A pre-employment programme for overseas-trained doctors entering the Australian workforce, 1997-99. Medical Education 2002; 36: 614-621.
11. Hawthorne L, Birrell B. Doctor shortages and their impact on the quality of medical care in Australia. People and Place 2002; 10: 55-67.
12. Kidd MR, Zulman A. Educational support for overseas trained doctors. Medical Journal of Australia 1994; 160: 73-75.
13. Confederation of Postgraduate Medical Education Councils. In: Workshop on Education and Training for Permanently Resident Overseas Trained Doctors. 6-8 August 2003; Wellington, NZ; 2003.
14. Alexander C, Fraser J. Information, training and support needs for GPs and registrars working in northern New South Wales. Tamworth: Hunter New England Area Rural Training Unit, 2005.
15. Alexander C, Fraser J. Professional career needs of GPs and registrars working in northwestern NSW. Australian Family Physician 2005; 34(Suppl): 7-9.
16. Hoyal FMD. Retention of rural doctors. Australian Journal of Rural Health 1995; 3: 2-9.
17. Hays RB, Veitch PC, Cheers B, Crossland L. Why doctors leave rural practice. Australian Journal of Rural Health 1997; 5: 198-203.
18. Han G-S, Humphreys JS. Overseas-trained doctors in Australia: community integration and their intention to stay in a rural community. Australian Journal of Rural Health 2005; 13: 236-241.
19. Humphries JS, Jones MP, Jones JA, Mara PR. Workforce retention in rural and remote Australia: determining the factors that influence length of practice. Medical Journal of Australia 2002; 176: 472-476.
20. Wainer J, Strasser R, Bryant L. Sustainable rural practice: successful strategies from male and female rural doctors Traralgon, VIC: Monash University School of Rural Health, 2004.
21. Birrell RJ. Australian policy on overseas-trained doctors. Medical Journal of Australia 2004; 181: 635-639.
22. Frank I. Australia: what's working, what's not working? What needs stopping, what needs starting? In: Confederation of Postgraduate Medical Education Councils. Workshop on Education and Training for Permanently Resident Overseas Trained Doctors. 6-8 August 2003; Wellington, NZ; 2003; Appendix VI.
23. Grant J. Learning needs assessment: assessing the need. BMJ 2002; 324: 156-159.
24. Booth B, Lawrence R. Quality assurance and continuing education needs of rural and remote general practitioners: how are they changing. Australian Journal of Rural Health 2001; 9: 265-274.
25. Alexander C. General practitioner numbers in the New England Health Area and factors which influence these GPs to move to and to stay in this region. Tamworth, NSW: New England Area Rural Training Unit, 1997.


