Introduction
Head lice are one of the oldest companions of humans1. They are host specific, obligate ectoparasites, a globally prevalent parasite of people2. Treatment, management and control of head lice infections (pediculosis) can be complex. Increasingly, worldwide pediculicide resistance, particularly in developed market economies, is adding to the difficulties experienced by many families3,4. Studies have recently suggested that traditional ad hoc mass school-based screening may not the best use of resources when controlling head lice5-7.
Parents and healthcare professionals have difficulty accurately reporting head lice infections8,9. However, health departments generally regard pediculosis as a low priority health problem, typically allocating minimal resources to its control, and encourage the public (parents) and/or non-health bodies to take responsibility for its management and control. But how equipped and willing are parents to manage these infections? How much do they actually know? It appears that there are no studies in the literature that address this. This article presents the results of a parental survey conducted in two sites in Australia that aimed to answer these questions.
Our study investigated the knowledge, attitudes, and practices of parents towards head lice infections, specifically addressing issues such as screening practices, the costs associated with infection, where parents seek advice on the treatment and management, and the number of days of school absenteeism resulting from a head lice infection. The survey was conducted in Victoria (Vic), a temperate region of Australia located in the southeast, and in north Queensland (NQ), a tropical zone located in the northeast. Both of these studies were nested within a wider prevalence study conducted at the same sites, which determined the prevalence of head lice infections in school aged children. It also examined whether commonly held risk factors for an infection, such as long hair and being male or female, held true6.
Methods
Participants and sampling process
In Vic, 16 government primary schools (eight rural and eight metropolitan schools) were randomly selected with probability proportional to weight. Classes within the school were randomly selected until approximately 200 children from the school were invited to participate. In NQ all 23 rural government primary schools, irrespective of size, located between and including Innisfail (17°31'S 146°01'E) in the north and Bowen (19°59'S 148°16'E) in the south and east of the Great Dividing Range, but excluding schools in the conjoined cities of Townsville/Thuringowa, were asked to participate.
In both states, children with parental consent were then screened for head lice by applying hair conditioner to all hairs of the head, combing with a nit comb, wiping the combings onto paper tissue, and checking visually for head lice or their eggs. Viability of eggs was also assessed visually. Following the screening, the parent/guardian of each child was sent an anonymous questionnaire together with their child's results. Vic parents were sent a head lice information pamphlet produced by the health department10, and NQ parents were sent a head lice information sheet11. In both states, the parent/guardian was asked to return the questionnaire in the following week by either returning it directly to the school or using the enclosed free-post addressed envelope. The questionnaires were collected from the school approximately 2 weeks after the screening. In order to optimise the return of surveys, each school was telephoned once a week for two further weeks.
Questionnaire
While a standard anonymous questionnaire was used in both sites, there were some minor differences in the questionnaires used. These changes made the questionnaires applicable in to the local setting and did not affect comparability of the results.
In order to assess parental knowledge, parents were asked 10 'true or false' questions. These questions focussed on some of the common myths associated with head lice transmission, treatment and management. The questions had a response format of 'true', 'false' or 'do not know'. Three questions sought demographic data; one question asked whether the child had participated in the screening program; 15 questions sought information on parental management of and attitude towards head lice.
Statistical analysis
Analysis was conducted using Stata v 9 (StataCorp, College Station, TX, USA). Non-respondents and variables with missing values were excluded from the analysis as indicated in the results. The estimated standard errors were adjusted for cluster sampling. Thematic analysis was used to analyse open-ended questions.
Ethical approval
Approval of the study was granted by ethics committees of the education and health departments (in Vic), and James Cook University (in NQ).
Definitions
Parents who did not answer at least five of the 10 knowledge questions correctly were classified as having a poor knowledge of head lice.
Results
Response rate
The response rate for the questionnaire survey was calculated on the basis of the number of children screened in each school. These children were a subset of those children invited to participate in the wider study6. In Vic, the response rate was 39% (743/1838, cluster-sampling adjusted) ranging from 12.3% to 83.7% at an individual school level. The response rate was higher in the metropolitan than non-metropolitan schools but this difference was not significant after adjustment for cluster sampling (44.5 and 34.9%, respectively p = 0.16) (Table 1).
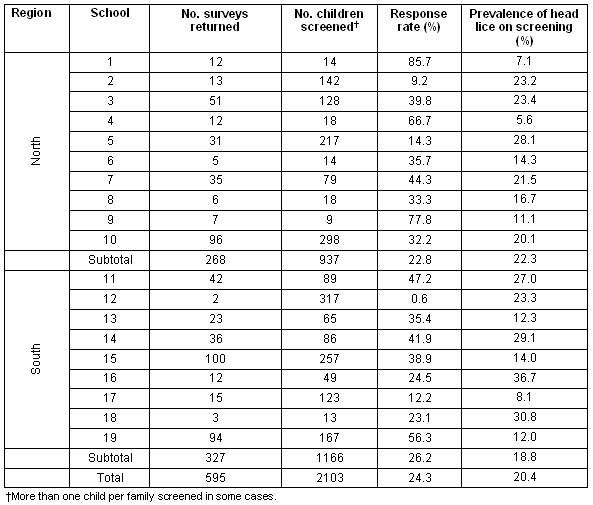
In NQ, 22 schools participated in the study. Three schools did not receive the questionnaires and were excluded from the results. The response rate was 24.3% (595/2103; adjusted for cluster sampling) ranging from 0.6% to 85.7% at individual school level. There were similar proportions of respondents north and south of Townsville (22.8% and 26.2%, respectively p = 0.8012; cluster sampling adjusted) (Table 2).
Because the parental surveys were anonymous it was not possible to assess whether children of non-respondents were more or less likely to have head lice than those of respondents. There was a weak negative correlation detected between the parental response rate and the prevalence of active head lice infections found on screening by school in both sites (Vic [r = -0.08 and NQ [r = -0.52).
Table 1: Response rate and prevalence of active pediculosis by schools in metropolitan and non-metropolitan study areas in Victoria. Results adjusted for cluster sampling.
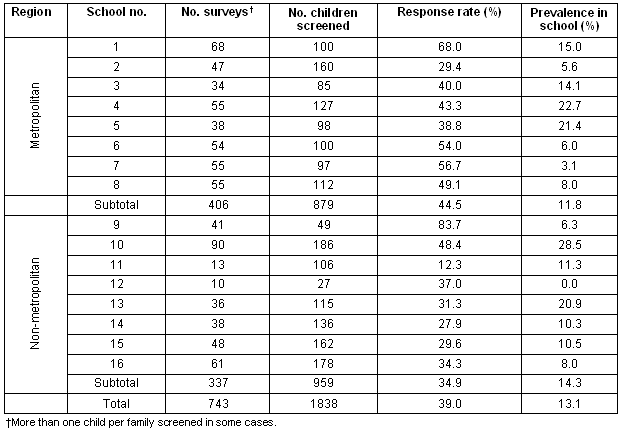
Table 2: Response rate and prevalence of active pediculosis by schools in north Queensland. Results adjusted for cluster sampling.
Parental knowledge
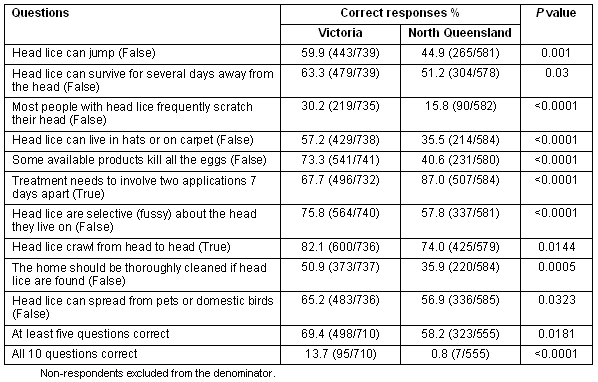
Parental knowledge of head lice was limited in both Vic and NQ with only 7.1% of parents answering all questions correctly (102/1265; cluster-sampling adjusted; 73 missing values). The majority of parents answered at least five out of 10 questions correctly (63.6%, 821/1265; cluster-sampling adjusted). However, many of the common myths about head lice were reflected in the results (Table 3).
Table 3: Results from 'true or false' questions in Victoria and north Queensland. Proportions and p values were adjusted for clustering. Correct answer in parenthesis in first column.
At both study sites there was a negative correlation between parents answering more than half of the true or false questions correctly and the prevalence of active infections found on screening (Vic r = -0.08 and NQ r = -0.52). There was almost no correlation between response rate and knowledge at both study sites (Vic, r = -0.07 and NQ, r = -0.05).
Parental responsibilities and concerns
Parents at both sites stated they should be responsible for checking and treating head lice (99.8% and 98.6% for NQ and Vic, respectively) (Table 4). While the majority felt they would be able to both effectively check and treat their child for head lice, the proportions for both were significantly higher in NQ (Table 4). The proportion of parents who had seen lice was higher in NQ than in Vic (91.4% and 67.5%, respectively), as was the proportion who had seen head lice eggs (90.6% compared with 67.1%) (Table 4).
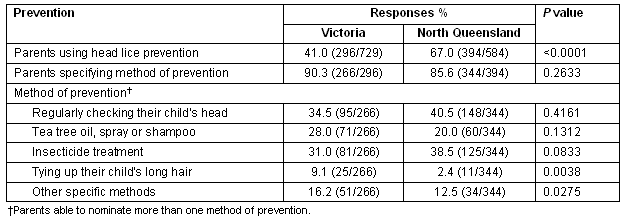
A higher proportion of NQ parents used a method (chemical and/or non-chemical) in order to prevent head lice than in Vic (67.0%, 394/584 in NQ and 41.0%, 295/729 in Vic, p<0.0001, adjusted for clustering, 25 missing values) (Table 5).
Table 4: Parental detection and treatment practices and beliefs by state Victoria and north Queensland. Proportions and p values were adjusted for cluster sampling.
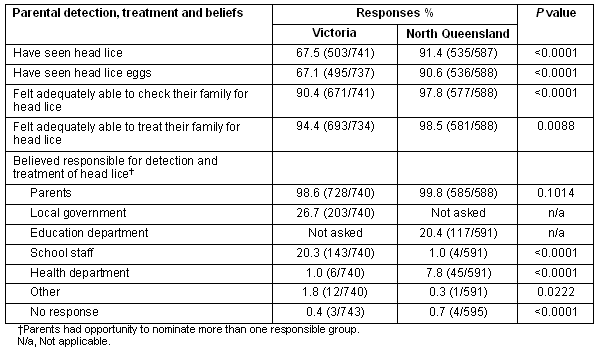
Table 5: Methods of prevention used by parents in Victoria and north Queensland. Proportions and p values were adjusted for cluster sampling.
Most parents saw head lice infections as a health concern (Vic 78.4%, 574/734 and NQ 81.0%, 474/584, p = 0.1; adjusted for clustering; 20 missing values). The majority of parents said they would talk to people outside their home if their child had head lice, most commonly speaking with friends, family, and other parents (Vic 71.4% and NQ 72.0%). Despite most parents indicating they had been given advice about head lice (Vic 82.2% and NQ 78.9%), the majority of parents wanted further information (67.4%, 386/583 in NQ and 50.0%, 361/672, p<0.0001, adjusted for clustering, 27 missing values).
Cost associated with infections
More than three-quarters of parents spent less than $50 per year on head lice infections (NQ 76.2% 453/595 and Vic 76.7% 570/743, p = 0.9, cluster-sampling adjusted, 25 missing values). Less than 5% of parents at both sites spent more than $150 as a result of head lice. There was a weak positive correlation between the prevalence of infections found at the school and the proportion of respondents spending more than $50 per year on head lice (Vic r = 0.40 and NQ r = 0.30).
A high proportion of children had missed school as a result of having head lice (Vic 24.4% and NQ 30.3%). In Vic, 13.9% of parents indicated their child had missed school in the preceding 12 months as a result of head lice (similar data were not available for NQ). In Vic there was a weak positive correlation (r = 0.39) between the proportion of families with a child who had been absent from school as a result of head lice in the preceding 12 months and the prevalence of active head lice infections found by screening (Fig1).

Figure 1: Correlation between the proportion of children missing school as a result of head lice in the preceding 12 months and the prevalence of active head lice infections, by school, Victoria (r = 0.39).
Discussion
The present study appears to be the only study of the knowledge, attitudes and practices of parents with respect to head lice and their control. Despite a small proportion of parents (7.1%) answering all true and false questions correctly, the majority of parents felt they were able to effectively check and treat their children for head lice. Parents in both states used the same methods to prevent infections and were equally concerned about them. Almost all the respondents believed that head lice infections were a health problem and wanted primary responsibility for detection and treatment. They discussed head lice with people outside their home and obtained their advice from similar sources. Similarly, high proportions of children at both sites had missed school as a result of head lice.
The response rate between schools varied in both Vic and NQ. While the definitive reason for this cannot be determined from our study, it may reflect further questionnaire follow up conducted by individual schools. As the surveys were anonymous, we were unable to determine at an individual level if parents who responded to our survey were more or less likely to have children with head lice, or if they were different from those who had not agreed to the screening and, therefore, more or less interested in head lice control. At both sites there was a weak negative correlation detected between the parental response rate and the prevalence of active head lice infections found on screening by school. This suggests schools with a low prevalence of active infections had a higher proportion of parents responding to the survey. Did parental knowledge of head lice influence the response rate? Were parents more or less likely to respond if they were better informed? We detected a very weak negative correlation between parental knowledge and prevalence. However, it is not known whether a high level of knowledge among parents correlates with effective control and, if it does, what level is required in a population to obtain effective control. We were unable to determine if there was a correlation between individual parents' knowledge and the response rate.
The head lice information provided to parents with the questionnaires contained all the answers to the 'true or false' questions, yet the results reflect that parents either did not read the information provided or that it did not meet their needs. Parents in our study most commonly obtained their management information from school staff, pharmacies and friends. While these may be trusted sources, they do not necessarily provide accurate information or information free from commercial bias.
A higher proportion of NQ than Vic parents had seen both lice and eggs. This difference may be explained by the prevalence of head lice in the two states. In Vic the prevalence of active pediculosis detected among primary school students (13.0%)6 was lower than that reported in both temperate (21.0%) and tropical (20.9%) NQ12,13, and in this study (20.4%) (Table 2).
Parents showed a poor understanding of the signs and symptoms of infections. Detection by parents has a low sensitivity and specificity8. Treatment and prevention practices may also be potentially dangerous, with a minority of parents routinely using insecticidal products as a prevention strategy. The majority incorrectly believed it is necessary to undertake environmental cleaning measures, and also said they wanted more information. We believe health authorities, school staff and parents frequently underestimate the complexity and perseverance that may be needed to control this highly adapted parasite. Parental desire to be responsible for head lice control should not be seen as the cue for health authorities to cease involvement. Instead, it should be seen as an opportunity for better allocation of government resources by ensuring policy and guidelines reflect evidence and support parents' willingness to be responsible for detection and treatment.
Informing other parents about a child's head lice is an important component of contact tracing and this should be encouraged in management policies, as should the need to regularly screen children at home. There does, however, need to be an understanding that the screening itself will not prevent head lice. In Australia, there is no clinically proven method of prevention available, yet parents reported using dangerous and costly methods to 'prevent' head lice. These reports included more than 10% of respondents using insecticidal products on a regular basis, presumably regardless of whether or not the child had an infection. Frequent screening would enable parents to detect an infection earlier and, consequently, make management easier.
A high proportion of primary school children have missed school due to head lice. In Vic specific legislation enabling children with head lice to be excluded from school has been widely enforced. In NQ, however, the specific legislation has not been as widely utilised. Our results found that in spite of specific legislation, or the lack of it, similar proportions of children have missed school. In Vic the higher the proportion of children with head lice at a school, the higher the proportion of children reported as missing school in the preceding 12 months. While this correlation demonstrates that principals are exercising their 'right' to exclude children under the legislation, it does not demonstrate that exclusion has an influence on the prevalence of head lice within the school. We believe it is unacceptable for children to miss educational opportunities as a result of head lice, and policies should not continue to recommend excluding children with head lice from school.
While our results indicated almost half the respondents had not spent any money on head lice control in the preceding 12 months, our questions of cost did not take into consideration indirect costs, such as the amount of time parents spent treating head lice infections or even lost work hours involved in collecting children sent home from school. In the absence of an understanding of how head lice treatments work, or an understanding of the need to focus treatment on the lifecycle of the louse and the head of the child, a great deal of the time and money parents spend treating head lice is wasted. There are no short cuts available; however, working collaboratively with other parents and concentrating efforts on the use of sensitive detection methods and synchronised detection practices, effective treatment strategies, and contact tracing will improve treatment outcomes.
Limitations
One of the major limitations of the study was the low response rate. The denominator for the response rate was calculated based on the number of children participating in the head lice screening (ie each child who was provided with a questionnaire along with their results). However, some of the children screened were siblings, and families with more than one participating child were instructed to complete only one per survey per household, rather than one per child. If a high proportion of siblings had been screened, then the true response rate would have been higher. How much higher is difficult to determine, as the surveys were anonymous. The Australian Bureau of Statistics suggests the average number of children, aged 0-17 years per family is 1.914. Making a conservative assumption that the number of primary school aged children (5-12 years) per family is less, perhaps 1.5 children per family, then the response rate improves. In Vic it would be in the order of 59.2% (743/1225) and in NQ 38.6% (595/1404).
Conclusions
This appears to be the most comprehensive study of parental knowledge, beliefs, and practices regarding head lice infections. Although parents wanted responsibility for the management of pediculosis, deficiencies in their knowledge indicate they may be inadequately equipped to do so. Given the high proportion of children in both states who have missed school as a result of head lice, it is recommended that health departments in Australia should work to ensure that consistent and accurate messages about pediculosis are disseminated, and that relevant legislation is amended to prevent children being excluded from school.
Acknowledgements
The authors wish to thank Drs Graham Byrnes and Petra Buttner for their assistance with the study design; Chris Cahill and Sheryl Thomas for their assistance with questionnaire distribution in NQ and the parents, schools, and children both in NQ and Vic who participated in the study and provided their opinions on pediculosis.
References
1. Maunder B. Attitude to head lice: a more powerful force than insecticides. Journal of the Royal Society of Health 1985; 105: 61-64.
2. Gratz NG. Human lice their prevalence, control and resistance to insecticides. A review 1985-1995. Geneva: World Health Organization, 1997.
3. Roberts RJ, Burgess IF. New head-lice treatments: hope or hype? Lancet 2005; 365(9453): 8-10.
4. Hunter JA, Barker SC. Susceptibility of head lice (Pediculus humanus capitis) to pediculicides in Australia. Parasitology Research 2003; 90: 476-478.
5. Vander Stichele RH, Gyssels L, Bracke C et al. Wet combing for head lice: feasibility in mass screening, treatment preference and outcome. Journal of the Royal Society of Medicine 2002; 95: 348-352.
6. Counahan M, Andrews R, Büttner P, Byrne G, Speare R. Head lice prevalence in primary schools in Victoria, Australia. Journal of Paediatrics and Child Health 2004; 40: 616-619.
7. Aston R, Duggal H, Simpson J, Burgess I, Dawes M. Head lice: evidence-based guidelines based on the Stafford Report. Journal of Family Health Care 2002; 12(5Suppl): 1-21.
8. Counahan M, Andrews R, Speare R. Reliability of parental reports of head lice in their children. Medical Journal of Australia 2005; 182: 137-138.
9. Pollack R, Kiszewski A, Spielman A. Overdiagnosis and consequent mismanagement of head louse infestation in North America. Pediatric Infectious Diseases Journal 2000; 19: 689-693.
10. Department of Human Services. Scratching for Answers? Melbourne, VIC: Department of Human Services, 2001.
11. Speare R. Head lice information sheet. Townsville, QLD: James Cook University, 1999.
12. Speare R, Büttner PG. Head lice in pupils of a primary school in Australia and implications for control. International Journal of Dermatology 1999; 38 285-290.
13. Speare R, Thomas G, Cahill C. Head lice are not found on floors in primary school classrooms. Australian and New Zealand Journal of Public Health 2002; 26: 208-211.
14. Australian Bureau of Statistics. Population by age and sex, Australian states and territories. Canberra: Australian Bureau of Statistics, 2000.
Abstract
Introduction: Although parents in developed market economies regard head lice infections (pediculosis) as a significant problem, health departments generally rate pediculosis as a low priority health issue, encouraging parents to manage and control it. But how well equipped and willing are parents to manage the infections? There do not appear to be any studies in the literature addressing these issues. This article presents the results of a survey conducted in Australia that aimed to answer these questions.
Methods: A cross-sectional survey of parents of primary school aged children in Victoria (Vic) and north Queensland (NQ) was conducted using a self-administered questionnaire. The study investigated the knowledge, attitudes and practices of parents regarding head lice infections.
Results: Only 7.1% of 1338 who completed the questionnaire answered all 10 knowledge questions correctly and more than one-third failed to answer half correctly. There was a weak negative correlation between parents' knowledge and the prevalence of active pediculosis in the school. Almost all parents wanted the responsibility for treating pediculosis and more than three-quarters saw it as a health concern. A higher proportion of parents in NQ used preventative strategies (67% vs 41%). Most parents spent less than AU$50 per year on treatments. Alarmingly, however, the proportion of children missing school as a result of pediculosis was 24.4% and 30.3% in Vic and NQ, respectively. In Vic there was a positive correlation (r = 0.39) between missing school in the previous 12 months and prevalence of pediculosis in the school.
Conclusions: This appears to be the most comprehensive study of parental knowledge, beliefs, and practices regarding head lice infections. Although parents wanted responsibility for the management of pediculosis, deficiencies in their knowledge indicate they may be inadequately equipped to do so. Given the high proportion of children in both states who have missed school as a result of head lice, it is recommended that health departments in Australia should work to ensure that consistent and accurate messages about pediculosis are disseminated, and that relevant legislation is amended to prevent children being excluded from school.
Key words: Australia, pediculosis, school absenteeism, treatment.
You might also be interested in:
2010 - Building capacity for acute care in developing countries
2010 - Prevalence, awareness, treatment and control of hypertension in an elderly population in Greece




