Context
Approximately 3 million people die each year from malaria1, making it a significant public health issue worldwide. Malaria is endemic in Papua New Guinea (PNG) and is the second most prevalent cause of death2,3. As such, it is a major public health issue, recognised by WHO and the PNG Department of Health3,4. In 1994 Felger et al.5 estimated that 47% of the population of two villages in PNG were positive for the plasmodium falciparum parasite. This causes the most dangerous form of malaria which results in death without appropriate treatment. Mueller et al.6 found that, following the 2002 PNG rainy season, 53% of the inhabitants of 11 mountain villages had symptomatic malaria.
In addition to its mortality, malaria affects economic output and contributes to worker absenteeism and non-attendance at school. In remote PNG villages, malaria also inhibits the capacity of communities to manage the burden of every day tasks, such as bringing water to the house for cooking and washing (the source may be more than 2 km distant). Malaria also prevents villagers tending their gardens, which are their main source of food. Records prior to November 2004 at the remote Batri Village Aid Post showed that, among the village population of 1400, there were five deaths from malaria each year and 29 consultations for malaria-related symptoms7.
The use of insecticide impregnated bed nets (supported by an education program explaining the rationale8) are effective in malaria control by preventing contact with mosquitoes (Fig 1). In 2004, the Global Fund to Fight AIDS, Tuberculosis and Malaria (GFATM) http://www.theglobalfund.org/en/files/publicdoc/Framework_uk.pdf agreed to fund a 5 year plan for distributing insecticide impregnated bed nets' in PNG, as a matter of urgency.
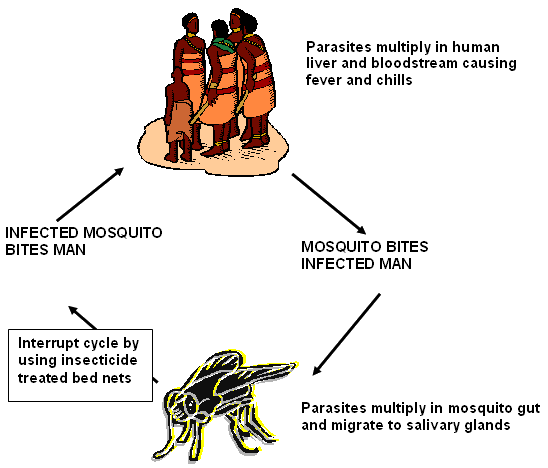
Figure 1: The role of insecticide-treated bed nets in malaria prevention (used with permission9).
The Batri Village was scheduled to receive WHO-approved bed nets in 200910; however, the urban members of the Kewapi language group decided to explore funding opportunities that would enable an earlier intervention. This article explores the experiences of the subsequent 'Batri Village Bed Net Initiative' in negotiating resources and implementing the initiative.
Background
Papua New Guinea is described as a young nation that grapples with major development problems11, including major health disadvantages and a lack of access to basic education and other services. Currently there is a decline in living standards11 and earlier gains in health and education are in danger of being eroded12.
The tropical climate is mediated by a mountainous terrain. These mountains, the dense jungle, vast rivers and poor transport infrastructure make it difficult for remote communities to access even basic services, leading many people from the Highlands region to gravitate to urban Port Moresby. The social isolation due to this difficult terrain has also resulted in a population that speaks over 800 indigenous languages. Each language group has separate traditions and culture, and people identify closely with a tight family grouping even when community members have gravitated to urban settlements.
The people of the Kewapi language group are one of the most disadvantaged peoples of PNG. They reside in a remote rural area which, at the time of writing, was in a state of emergency due to fighting and political turbulence. Members of the community living in Port Moresby also experience extreme poverty, low employment, poor housing and limited access to even basic services13.
Issue
The project
The genesis of the project was the concern of members of the Kewapi language group living in urban Erima, Port Moresby, for those remaining in their home village, Batri, suffering the effects of malaria. The Erima group became part of an 'empowerment research project' in 2004-2005: the Erima Empowerment Research Project (Fig 2). Empowerment research enables members of communities to take ownership of a project agenda and develop relevant initiatives. In this way, disadvantaged communities feel that their concerns are heard, enabling them to engage with political agendas that affect community development14,15 and bring about change.

Figure 2: Erima Empowerment Research Project group at a Port Moresby workshop.
In discussing the prevalence, effects and management of malaria, participants of the initial Erima project began to consider environmental issues that affect the spread of malaria, including the important control strategy of insecticide-impregnated bed nets. There was concern that those in Batri had to wait several years to acquire the GFATM bed nets. A collaborative research approach by members of the initial Erima Empowerment Research Project led to the 'Batri Village Bed Net Initiative'.
In order to be inclusive, projects centred on the needs of vernacular communities must address communication issues16, both in interpretation and capturing meaning (eg in oral histories and visual clues). The demands of this project were facilitated by the assistance of Elders from the language group fluent in English Pidgin and Kewapi. These Elders were also familiar with the cultural norms of the village, including the tribal discussion system, enabling project members to communicate effectively.
Once communication was enabled, those involved used the networks that exist between the community living in Port Moresby and the village to involve 'Wantoks' (members of their extended families) in Batri to recruit members. They used a two-way radio system, passed messages with people trekking to the nearest urban centre and sent letters to the national newspapers about the project. They also enlisted the help of the Mission Aviation Foundation (who have a network of small planes).
A negotiated approach was used to request 400 WHO mosquito nets from the British High Commission in Port Morseby to send to Batri Village. The submission document was researched and prepared by an author [JF] and later affirmed by members of the community as accurately representing their request.
Baseline evidence about the effects of malaria in the village was collected from urban members of the community and by two-way radio from those in Batri. This also provided an opportunity to initiate dialogue about the partnership approach with the people in the village.
Drawing on the skills learned in the initial empowerment research in Erima, members of the Kewapi language group presented the bid to the British High Commission. The bid was approved. Subsequently, members of the community were also involved in:
- ensuring that the nets arrived safely
- identifying who should receive the nets
- ensuring that information about their use was effectively disseminated
- networking with Elders in the Batri village to engage them in:
- targeting women and children as most vulnerable to the effects of malaria
- assisting aid post and health centre staff to monitor effectiveness of the nets in malaria prevention by compiling statistics over the next 5 year period.
- targeting women and children as most vulnerable to the effects of malaria
Messages were sent by two-way radio to alert the villagers to the arrival of the bed nets with their escort, a member of the 'Erima' research team. Members of the village congregated on the air strip where they had built a podium from bush materials to enable everyone to see the speaker and appreciate what was being said during the formal distribution (Fig 3). The bed nets were presented by roll call to the senior female member of each household to take responsibility for their use, care and maintenance. This was unusual in a community where males are most often entrusted with resources, but it reflected the negotiated wishes of the community.
A researcher from the original 'Erima Empowerment Research Project', who is also a member of the language group, travelled with the bed nets and stayed in the village to conduct a series of discussions with the Elders (Fig 4). The focus was to reinforce the efficacy of using bed nets in malaria prevention and to share information about the care and maintenance of the bed nets. In addition, he provided illustrated, laminated leaflets which were distributed to the nearby churches.

Figure 3: Batri people gathered at the airstrip to receive the bed nets.

Figure 4: Author Dr W Ako with Batri Elders in traditional dress.
This model of health promotion emphasised that the relevance, timing, venue content and style of delivery should match the cultural experience of the participants. With this in mind, education sessions about care and maintenance of the bed nets were conducted by an author [WA] on the Batri airstrip. The education sessions also included distribution of material from the WHO Roll Back Malaria Campaign1 which addresses the chronic effects of malaria on maternal and child health, emphasising the efficacy of prevention and treatment strategies. Members of the Kewapi language group talked about the effects of malaria in terms of chronic illness and impact on maternal and child health. These discussions illustrated the profound effect that malaria has on health and social activity such as obtaining water, tending the gardens and childcare in the village. As a result, the villagers agreed to minimise the access of mosquitoes to stagnant water for breeding. They also appreciated the efficacy early treatment to prevent spread of the disease.
The air strip sessions were conducted in day light hours and at times that took into account activities such as selling in the market, church going and personal safety. The style of delivery built on the traditional forum of the Southern Highlands. This involves addressing the Elders of the community and respecting norms while challenging traditional beliefs.
Analysis
The Southern Highlands Province is fraught with issues of poor governance and misappropriation of medical supplies, linked to the decline of the service infrastructure and local political disharmony. This lead to scepticism from medical colleagues and officials about the possibility of successful funding, acquisition and distribution of bed nets in such a remote community. Despite these concerns, the Batri Village Bed Net Initiative was completed successfully, demonstrating good governance and acquittal.
This was due to the wide consultation with a range of stakeholders, including Elders and other community members. The form of the later education sessions the Batri air strip was important because community members felt that the 'Erima research team' were engaging with the reality of village life. The deliberate timing meant the sessions were inclusive, allowing a wide participation. The project commitment to translation and authentication of meaning also contributed to the sense of respect and acknowledgement of the cultural context of the villagers. In the 2005 evaluation phase of the project, members of the community reported that they felt that their issues and concerns had been heard and respected. This led to participator planning and community ownership, demonstrated by the participation of both villagers and Port Moresby members of the language group in such activities as publicising the project, setting criteria for who should receive the nets, and ensuring the safe arrival and distribution of the nets.
Since the deployment of the nets in November 2004 there have been no deaths from cerebral malaria in the community, an improvement in the previous 5 deaths per year. Members of the community also report that villagers are more able to perform everyday activities, such as tending their gardens, because they are enjoying better health. In September 2006 the Batri village radio operator's wife sent a radio message saying in Kewapi: Wena ali maa ralalua me yanda paia. The translation is: 'You (Dr Ako and Dr Jane) introduced the nets and increased the population of men and women'. She explained that this was because no one is dying and babies are born living. This statement illustrates the profound effect that a relatively simple malaria prevention strategy can have if adopted effectively - even in a remote rural community.
Both the chair of Rotary Against Malaria and the grants coordinator for the British High Commission in Port Moresby commented on the exceptional commitment of the members of the community in taking ownership of the project, and the effectiveness of this process. Members of the research team have since worked with the High Commission in using this empowerment approach to introduce bed nets in other areas in PNG.
Discussion of the Batri Village Bed Net Initiative has paved the way to widen the debate about community development. Members of the community are currently working with the research team in developing a proposal to explore how empowerment strategies can enhance capacity building, affect health experiences and thus help alleviate poverty within remote PNG rural communities.
Lessons learned
This project explored whether an empowerment approach to community development can affect the lived experience of health for people in a rural village in PNG. The project design accommodated the logistics of using a partnership approach to work across diverse cultures. What emerged was that a genuine interest in, and affirmation of, the local culture is the crucial factor in a positive outcome. This is consistent with the literature on empowerment research and peer learning17.
Strengths of the project were in capitalising on the traditional discussion forum of the community, and relating to community concerns. This led to a supportive culture that enabled mutual sharing and exploration of issues, a crucial aspect of collaborative projects18,19. This approach also allowed power dynamics within the project to be acknowledged and addressed, within the constraints of time and commitment20.
Commitment to this enhancement approach to community development requires collaborative work with a 'critical reference group'14 in problem solving. Following this approach, the project showed that members of language groups in PNG can and will actively engage in collaborative discussion about a health issue. Further, they were also able to influence change within their social context. A significant project development was the Wantoks' networking between the urban and rural strands of the Kewapi language group. This suggests further potential for focused health promotion projects.
Projects like this effective health intervention, owned and implemented by members of a networked language group, can empower people living in remote areas of low resources to adopt effective health promotion strategies.
References
1. WHO. Roll Back Malaria Campaign. (Online) 2004. Available: http://www.rbm.who.int/cgi-bin/rbm/rbmportal/custom/rbm/home.do (Accessed 20 November 2006).
2. Save the Children. Papua New Guinea: Training volunteers to improve community health. (Online) 2003. Available: http://www.savethechildren.net/new_zealand/what_we_do/our_projects/papua_new_guinea.html (Accessed 10 January 2006).
3. Naraqi S, Feling B, Leeder SR. Disease and death in Papua New Guinea. Medical Journal of Australia 2003; 178: 7-8.
4. World Health Organisation. Papua New Guinea Health Situation, WHO Regional Office of the Pacific Region. (Online) 2006. Available: http://www.wpro.who.int/countries/04png/health_situation.htm (Accessed 10 November 2006).
5. Felger I, Tavul L, Kabintik S, Marshall V, Genton B, Alpers M. Plasmodium falciparum: extensive polymorphism in merozoite surface antigen 2 alleles in an area with endemic malaria in Papua New Guinea. Experimental Parasitology 1994; 79: 106-116.
6. Mueller I, Namuigi P, Kundi J, Ivivi R, Tandrapah T, Bjorge S, Epidemic malaria in the Highlands of Papua New Guinea. American Journal of Tropical Medicine 2005; 72: 554-560.
7. Fitzpatrick J. An exploration of empowerment in the developing world context of Papua New Guinea. Bristol: University of the West of England, 2006; 1-79.
8. Dawson AJ, Joof BM. Seeing, thinking and acting against malaria: a new approach to health worker training for community empowerment in rural Gambia. Rural and Remote Health 5: 353. (Online) 2005. Available: http://www.rrh.org.au/ (Accessed 10 November 2006).
9. Fitzpatrick J. Malaria: promoting awareness and prevention of a critical crisis in a remote area of Papua New Guinea through community involvement. CONNECT: Global Connections 2006; 5: 19-22. Available: http://www.connectpublishing.com/articles/foundarts.asp (Accessed 13 June 2007).
10. Global Fund. Community based malaria and HIV/AIDS prevention and control in Papua New Guinea. (Online) 2003. Available: http://www.theglobalfund.org/programs/grantdetails.aspx?compid=702&grantid=252&lang=en&CountryId=PNG (Accessed 13 June 2007).
11. Executive Board of the United Nations Development Programme and the United Nations Populations Fund. Country Co-operations Frameworks and Related Matters: Country Programme Outline for Papua New Guinea (2003-2007). (Online) 2002. Available: http://www.undp.org.pg/documents/undppngcp.pdf (Accessed 13 June 2007).
12. AusAID. Country programs: Papua New Guinea. (Online) 2007. Available: http://www.ausaid.gov.au/country/papua.cfm (Accessed 13 June 2007).
13. Simms PA. Papua New Guinea needs law and order above all. BMJ 2003; 326(7381): 165.
14. Riedy C, Watson E, Cheney H, Tario K. Community Empowerment Final Research Report. Sydney: Institute of Sustainable Futures and Moreland Energy Foundation at Teh, University of Technology Sydney, 2004; 1-40.
15. Wadsworth Y. Everyday evaluation on the run. Sydney, NSW: Allen and Unwin, 1997.
16. Lim R. Outside the classroom: oral and visual research methods applied in vernacular settlements. Proceedings, International Conference on Integrating Teaching with Research and Practice in the Built Environment. 8-10 September 2003; Wadham College, Oxford; 2003.
17. Peersman G, Flores S, Zee A, Elke A. Systematic review of interventions for preventing HIV in young people in low income countries. (Online) 2001. Available: http://www.cochrane.org/colloquia/abstracts/capetown/capetownPD11.html (Accessed 20 November 2006).
18. Kreugar RA. Focus groups a practical guide to applied research. London: Sage, 1994.
19. Morgan JA. The focus group guide book. London: Sage, 1998.
20. Schulz R, Scroeder D, Brody C. Collaborative narrative inquiry: fidelity and the ethics of caring in teacher research. International Journal of Qualitative Studies in Education 1997; 10: 473.

