Introduction
Christmas Island and the Cocos (Keeling) Islands are Australian Commonwealth Territories managed by the Australain Department of Transport and Regional Services (DOTARS). The islands are possibly the most remote and isolated of all Australian communities, being over 2500 km from Perth, Western Australia (WA), and accessible by commercial aircraft only twice a week.
The provision of health services in rural WA is unique in Australia due to the distances involved and the isolation of many areas. The provision of obstetric services in these areas is becoming a rarity, even though rural and remote women have the highest fertility rates in Australia1.
Maternity care (ie antenatal, labour and post-natal) within the home or local area is generally a priority for women, particularly multiparous women and women of certain cultures (eg Muslim and Indigenous)2. At present in the Indian Ocean Territories (IOT), however, women are routinely flown to Perth mid-pregnancy for ultrasound scanning, and then again at 36 weeks gestation for delivery3. This is due to a lack of suitably-qualified staff, rather than a lack of facilities.
To offer obstetric services, hospitals must fulfil the recommendations and requirements for the provision of safe obstetric services outlined in the 2003 Western Australian State-wide Obstetric Services Review (Cowen Report), including the provision of appropriately-trained anaesthetists or GP-anaesthetists4.
Additionally, The Guidelines for Rural Obstetric and Midwifery Services in Western Australia outlines four designated levels of service provision in obstetrics, and the equipment and resources (including suitably-qualified obstetricians and anaesthetist) required to meet those levels5.
A number of other reports support these guidelines, including the provision that 30 min is the maximum time allowable for the recall of medical specialists in obstetric care and of anaesthetists in obstetric procedures4.
Christmas Island has a well-equipped, eight-bed hospital with modern facilities, including a birthing suite and operating theatre6, and radiology and pathology7. Visiting medical specialists provide theatre services (including anaesthetics) for booked admissions, but the hospital currently does not have the capability for emergency anaesthetics, due to the lack of a resident GP with suitable procedural skills. Despite the hospital's facilities, it is therefore classified to provide antenatal and post-partum care but not to cater for planned births.
Attracting and maintaining skilled staff, including obstetric and anaesthetic-trained doctors, is crucial in remote areas. The Cohen Report called for urgent review of the incentives for attracting and supporting obstetricians and anaesthetists, including procedural GPs4.
Other very remote parts of Australia employ a variety of models of obstetric service provision, including fly-in services; however, none have the geographical isolation combined with lack of accessible travel options and unique cultural differences that are present in the IOT.
There is a paucity of specific examples in the international literature providing good comparative value to the IOT, and in terms of sheer distance from definitive tertiary health care, their isolation probably makes the islands unique among first world countries. Examples with reasonable similarities do exist in Canada and Alaska where obstetrics services are provided locally in a safe manner. For such isolated populations, respective policy guidelines acknowledge locally-provided obstetrics is possible and beneficial but is dependant on the capability for caesarean section.
The total populations (predominantly Malay and Chinese) are approximately 1500 for Christmas Island and 650 for the Cocos Islands. Two full-time GPs work on Christmas Island and one on the Cocos Islands. Obstetric or anaesthetic procedural GPs are no longer actively recruited for the islands. Experienced midwives have been employed by the Indian Ocean Territories Health Service (IOTHS) in the past, but reduction in obstetric services has meant the loss of skills and personnel. Up-skilling and attraction of midwives would be required if on-island birthing was resumed. Currently the IOTHS is almost exclusively employs agency nursing staff while awaiting a reform of healthcare provision. Experienced midwives are included in this agency supply.
The current obstetric service for the IOTHS has been in effect since March 1998. Prior to this, women delivered their babies vaginally and by caesarean on both Cocos and Christmas Island. Predicted obstetric problems were evacuated off-island to Perth prior to delivery. Some of the women chose to have their babies in Malaysia or Indonesia to be with family. In 1994 on-island birthing ceased on the Cocos Islands and in 1998 on Christmas Island. Between 1994 and 1998, women from Cocos Islands were sometimes delivered on Christmas Island. In the current situation, families are provided with two adult return airfares to Perth and some assistance with accommodation.
Women and their partners regularly question medical staff on the islands about the current obstetric service, in particular why they have to leave their islands to give birth when they previously had a full obstetric service on the islands. It was these concerns that prompted a request to DOTARS for practical support and permission to conduct the study. DOTARS also provided a small grant to one of the authors (SD) to assist her in undertaking the study.
Methods
This article presents the qualitative findings of a larger study conducted from February to December 2005, that included retrospective documentation of pregnancies, deliveries and obstetric outcomes for women cared for under the IOTHS from 1995 to 2004 inclusively.
The qualitative aspect of the study sought to add context and depth to the broader study. The aims of the qualitative study were to:
- Determine perceptions of IOT residents about their experiences of on-island and off-island birthing.
- Gain an understanding of the social, economic and cultural impacts of the obstetric service on IOT residents.
- Identify possible areas for improvement in the current service and explore potential solutions.
One of the authors (SD) has provided a locum and outreach service to the islands over 8 years. The researcher sought volunteers for the study though flyers and at women's health forums. Individual interviews were conducted with 28 of the islands' women, some of whom attended with their partner. Interviews were conducted during May 2005 and utilised interpreters where required or requested. A purposive sample was sought and demographics of interviewees (Tables 1, 2) were deemed to approximate the cross-section of women living on the islands. Residents from all three islands were represented in the interviews, and the participants had had between one and six babies. Their babies had been born off- and on-island in various ratios (Table 3, 4).
Table 1: Age of interviewees
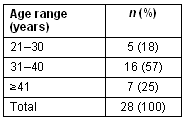
Table 2: Ethnicity of interviewees
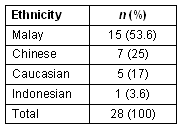
Table 3: Number of off-island births of interviewees
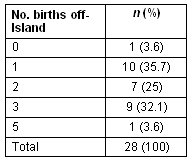
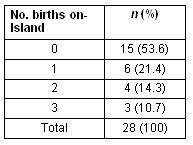
Table 4: Number of on-island births of interviewees
Interviews took an average of 30 min each and were semi-structured with the researcher using a series of broad prompts. Information about the study and informed consent forms were translated into Bahasa Malay and Chinese dialects, as appropriate. All interviewees gave informed consent; interviews were audio-recorded and transcribed verbatim. Text files were then imported into QSR NVivo software (QSR International Pty Ltd; Melbourne, Victoria, Australia) which was used to manage analysis of the data. The constant comparative method of analyse was used so that data were analysed as they were collected, and findings could direct further lines of enquiry.
The majority of data analysis was undertaken by SD while SR independently coded parts of a selection of interviews and both researchers compared and discussed coding until consensus was reached.
A number of levels of coding were employed; initially segments of the transcriptions were coded for thematic content. Themes were then examined as to their relationship to each other. A further stage developed scenarios ranging across a number of continuums. These scenarios were then checked back against the raw data and initial coding for verification. Themes and findings were discussed and presented to current and past medical staff from the IOT to corroborate coding categories and obtain peer input.
The financial, social and psychological costs for IOT women and their families were estimated, and the financial costs for DOTARS were also examined.
Approval for the study was obtained from The University of Western Australia, Human Research Ethics Committee.
Results
This article presents only one aspect of the study, being the qualitative findings; however, some of the quantitative data is presented to provide context to the study.
Quantitative findings
All quantitative data presented were collected by the researchers in the larger study using various methods of data collection and verification. From 1995 to 2004, IOT women experienced 323 confinements resulting in 326 babies (including three sets of twins) (Tables 5, 6)
Table 5: Place of birth by year of babies born to Indian Ocean Territories residents 1995-2004
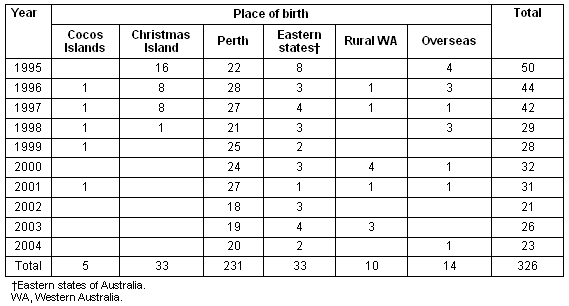
Table 6: Delivery age range by year of Indian Ocean Territories women 1995-2004
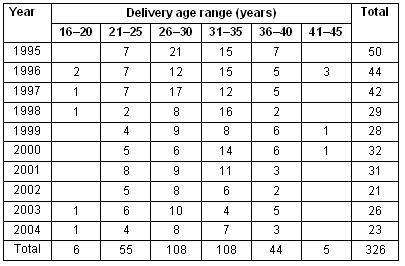
The annual number of births fell by over 50%, from 50 in 1995 to 24 in 2005, and a drop of 31% (from 42 to 29) was recorded from 1997 to 1998, the year in which on-island deliveries ceased. The average number of deliveries fell from 45.3 for 1995-1997 to 26.7 for 1998-2005.
Overall in the IOT, the number of women aged 15-44 years fell from 602 in 1996 to 411 in 2004, a drop of 32%. The birth rate, meanwhile, fell by 38%, from 8.8% in 1996, to 5.4% in 2004 (calculated using Australian Bureau of Statistics8 census data for 1996 and 2001, and Australian Bureau of Statistics population estimates for 2004).
On Christmas Island, the birth rate for the equivalent population and time period remained relatively stable at 6% in 1996, 7.5% in 2001 and 5.8% in 2004. On the Cocos Islands, however, the birth rate more than halved, falling from 11.6% in 1996, to 9.6% in 2001 and 5% in 2004. A combination of the reduction in the number of fertile female residents and the reduced birth rate are jointly responsible for the overall reduction in births for the IOT during the period investigated.
Qualitative findings
Initial coding of interview transcripts revealed five major categories:
- Choice and safety
- Economic difficulties
- Social issues
- Accommodation problems
- Cultural, religious and spiritual issues
Relationships between these categories were then examined and are depicted (Fig 1). Women and their partners considered both positives and negatives of birthing on- and off-island, and then weighed this against safety issues. Perceptions of safety were strongly influenced by past experiences of place of birthing.
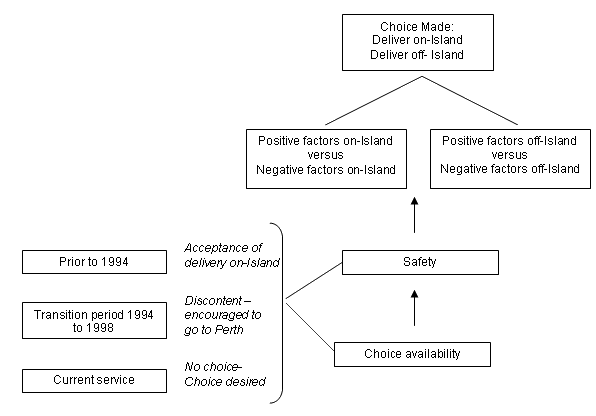
Figure 1: Schematic representation of qualitative data coding.
Choice and safety
Having choice about where the baby was born, was the most significant or core category, but exercising that choice was affected by a number of factors, particularly safety. The women's response to safety issues was largely based on their previous experiences and their understanding of the IOT obstetric service. Past experience of birthing in the IOT also determined their attitudes to the possible choices.
All I want to know is about the safety of my baby, that's it. But because I find that I have normal deliveries, I wanted to do it again on-island but I still cannot do it. The doctor is not experienced with delivery. Even if I have a normal pregnancy, they still want me to deliver in Perth (X1)
Newer mothers appeared not to have gained confidence in GP obstetricians:
I would rather go to Perth to deliver because they have specialists there. (X13, aged 28)
Economic difficulties
Financial issues arose from two sources: the cost of relocation for five or more weeks and loss of earnings.
Until 2002, only the mother was provided with a free air ticket, although DOTARS now provide the family with two airline tickets. The expectant parents may, however, need or choose to take additional family members, such as existing children or their own parents. Additional travel and accommodation expenses must be met by the families themselves. The family may also need to hire a car on the mainland, pay for child care and buy warm clothes for the trip.
Its not just enough to fly her to Perth for free and say 'OK, we've done our job, she can go.' It's the cost of me going there, cost of flying my parents in, the costs of staying with someone. Where will I get all that from? (X2)
As well as economic considerations, there are also logistical difficulties. The heavily pregnant woman must pack for herself and her family for a trip of up to 7 weeks, as well as prepare the house for departure. The return journey will take between 7 and 12 hours from door-to-door, on a small plane that is not equipped for a baby.
Social
Coding under social issues encompassed the father of the child, the siblings, the extended family and also friends.
Father of the child: For most expectant fathers, paid leave for the duration is not an option, so if they are able to get the time away from work they must take it as leave without pay. If this is not a viable financial option for a family, the expectant mother must travel alone. Partners then attempt to time their flights with the anticipated time of labour, causing further anxiety for all concerned.
The end result is often that fathers are prohibited from being present at delivery, which has cultural and religious implications as well as the obvious social and emotional consequences:
As a Muslim, the husband has to be there for the delivery. He has to pray for the child. I couldn't do that for my last child, as I wasn't there. And of course a woman wants her partner to be there to give her moral support, to give her strength... (X2, Malay man)
Siblings: Existing children are another issue for IOT women. Women who deliver near their homes usually have friends, family or neighbours who can help with the care of existing children. Some IOT women have to take their children with them to the mainland, however, and may not have such social supports. As a consequence, they have to take the children with them to appointments and even to the delivery.
Caring for the siblings can also prevent partners, who accompany the woman to the mainland, from attending the birth, and teachers have expressed concern about children being absent from school for many weeks while they are with their mothers on the mainland.
We have to think about the children's education. We are leaving the two eldest children with my family and we will take the two youngest ones. We have to give them some money to care for our kids. (X4)
Leaving older children on the island raises issues of finding someone to care for them and the cost of that care, but it also means separation from their mother at an important family life event.
My three children stayed on the island with my parents and sisters. I missed them. I was away for six weeks. (C11)
Extended family and friends: It is customary in Muslim families for the grandmothers to be present at the birth to help with important religious rituals at the time of birth, and in the following days. Many pay the $AU1800 air fare themselves so that they can do this.
For those IOT families with extended family and friends on the mainland, the birth of a new baby was a chance to visit and spend time with them. For these families this was seen as a positive, along with the chance to shop and extend the horizons of older children.
The good thing is because you have to go at 36 weeks, it's a bit of a holiday and a bit of a shopping trip, but I still think it's too long. (C6)
Accommodation
Families are offered some financial support to assist with accommodation, however short term accommodation is difficult to source and not always close to the hospital. Women who stay with family members reported a strain on family relationships, as they felt the presence of themselves and their children was an added burden.
Especially we don't have anywhere to stay and the vehicle is expensive for hiring a car, and the people we stayed with, I mean they're OK but its OK to stay for a little while but not any longer than two or three weeks. (C5)
Cultural, religious and spiritual
IOT women delivering on the mainland may also be unable to observe childbirth rituals, such as having the mother and mother-in-law present, or the new mother staying in the house for 30 to 40 days after the birth.
Because we are Chinese we are supposed to wait after our labour. We need to sit at the house for a long time and you're not supposed to come out... We are not allowed to shower, not allowed to drink water, we need to drink just a milk drink or whatever. Yellow ginger and hot drinks to prevent the wind getting in. (X10, Chinese woman)
On discharge from hospital, IOT women are required to take the next available flight home from Perth. This prevents them from being able to observe the required period of seclusion.
Families also reported finding it difficult to source halal food, mosques and temples on the mainland.
Discussion
Data from this study support the assertion that a fall in the annual number of deliveries to IOT women coincided with the cessation of on-island birthing, and may reflect a deliberate reduction in birth rate because of having to leave the Islands for confinement.
Overall, the financial and socio-cultural burdens for families to accommodate off-island confinements are extensive, and warrant genuine recognition and proposal of solutions.
IOT families can suffer financial hardship through lost income, and large additional expenses such as airline tickets for family members as a result of having to go off-island to give birth. Their cultural, religious and spiritual requirements are also often compromised as they are unable to perform required practices and/or rituals.
Interviewees, across all cultures, including Caucasian, continuously expressed disappointment about the loss of choice. If choice were available, some women would definitely opt to have their babies on-island. Others, however, might still wish to go to the mainland if, for them, it is a chance to shop and visit family.
Whatever their preference, the desire for full obstetric services to be reinstated on the islands for low-risk pregnancies was a recurring theme in the data. Another indication from women interviewed was that, if on-island birthing were available, they would have more children.
While other places in rural Australia have long distances and poor access, the IOT are unique in that they can only be reached by plane at significant cost and only twice a week. The average time that women spend off-island is 5 weeks, but it can be more than 6 weeks, which is a long time to be away from home. The cultural difficulties these families face on the mainland are different to those normally seen in Perth and it is the combination of these factors which makes this situation unique.
Conclusion
The current obstetric service in the IOT is not meeting the needs of the population. The number of births to IOT women has fallen, and qualitative data supports the view that this is due to the considerable financial, logistical, social, cultural and spiritual difficulties faced by women having to leave the islands to deliver their babies.
State-of-the-art birthing facilities already exist on Christmas Island; however, for a full obstetric service to be reinstated, experienced GP-anaesthetists, GP-obstetricians and midwives would need to be employed. Due to the current Australian rural medical workforce shortage, competitive remuneration and rostering packages would probably be needed to assist in attracting suitably skilled doctors. Nonetheless, as the estimated total annual cost of transferring women off-island for birthing is currently in excess of $215,000, it is likely that on-island birthing could still be cost-effective.
Three models of service delivery offer possible solutions to the problems in the current IOT obstetric service. As a proportion of the women will always need to be evacuated to the mainland and some will always want to do so, the third proposal should be implemented as soon as possible irrespective of what other changes are adopted.
- GP Anaesthetists and GP Obstetricians be employed on Christmas Island to provide a full obstetric service.
- Low-risk pregnancies and women electing to have a caesarean section, be permitted to deliver on-island. This could utilise a fly-in obstetric team.
- Greater assistance be provided on the mainland, especially with regard to accommodation and child care.
The uniqueness of the IOT means that the results of this qualitative study cannot be generalised to other areas. However, in any situation where an obstetric service is provided at a vast distance from the women's home and in a predominantly different cultural context, one would expect similar issues would need to be addressed. Policy makers need to look beyond the guidelines when determining health service provision to very remote areas and consider the critical financial, social and cultural costs that accompany such policies.
It has been recommended that the IOTHS undertake a feasibility study to investigate the implementation of the models of service delivery as determined by this study. The preferred option for IOT residents is to have the choice of having their babies close to their own homes so all their cultural, social and spiritual needs can be met.
Should a safe obstetric service continue to be unavailable on Christmas Island, it is imperative that assistance for IOT families while on the mainland is improved without delay. These improvements should encompass funding, transport, accommodation close to the hospital, child care and attention to cultural safety issues.
Without change, many families of the IOT will continue to be denied the opportunity of celebrating the birth of their children in the joyful the way they should be able to expect. Instead, they are forced into a situation which is so stressful spiritually, culturally, financially and logistically that some say they are finding it preferable to simply forgo having further children. Potential solutions are available and should be implemented and trialled.
Acknowledgements
The authors would like to acknowledge the contribution of Ms Viven Gee, from the Midwives Notification System, for provision of statistical data; Professor Jon Emery, from the Discipline of General Practice at The University of Western Australia, for advice on data analysis; and Ms Tansy England for editing assistance. The authors would also like to thank the following Island residents for their assistance with data collection: Nameli Yaderie, Pamela Jones, Carol Gaffney, Wendy Grinter RN, Kathy Millsteed RM and Celine Cheah. Finally, very special acknowledgement must be made of all the interviewees who gave so freely of their time and so generously of their knowledge and experiences.
References
1. Commonwealth of Australia. Australian Institute of Health and Welfare report. Canberra, ACT: Commonwealth of Australia, 1998.
2. WA Branch of the Maternity Coalition. Implementing the National Maternity Action Plan in WA. Perth, WA: WA Branch of the Maternity Coalition, 2004.
3. Commonwealth of Australia. Indian Ocean Territories situation report. Armidale, NSW: Department of Transport and Regional Services, 2000.
4. Cohen H. Western Australian statewide obstetric services review. Perth: Department of Health Western Australia, 2003.
5. Department of Health Western Australia. Rural obstetrics and midwifery guidelines. Perth: DoHWA, 2000.
6. Bath R. Indian Ocean Territories Health Services Development Project - report to the Commonwealth Department of Transport and Regional Services, Department of Health Western Australia. Perth: DoHWA, 2002.
7. Australian Government. Department of Transport and Regional Services. (Online) 2005. Available: www.dotars.gov.au (Accessed 27 March 2007).
8. Australian Bureau of Statistics, Census of Population and Housing. 1996 and 2001. B01 Selected Characteristics: All persons; and B03 Age by Sex, in ABS Population Estimates by Age and Sex 2004. Canberra: Commonwealth of Australia, 2004.

