Introduction
It is widely accepted that women experience drug dependency in different ways from men. Compared with male drug users, drug dependent women: experience greater social stigma, because of their roles as mothers1; suffer higher levels of shame and self-blame concerning their drug use2,3; are more likely to be poly-drug users4; and have higher rates of psychological co-morbidity5. The substance abuse treatment field has been criticised for failing to recognise and address women's complex needs and the broader social and economic factors that affect their vulnerability to initiating drug use, and to accessing and remaining in treatment6,7. Consistent with international findings, Australian women are relatively under-represented in illicit drug treatment services, attending treatment services less1, and leaving at an earlier stage, than men8.
Limited evidence suggests that women's experience of substance dependence and attempts to access treatment may also be negatively affected by living in a rural area. In Australia, rural infrastructure problems (poor public transport, inadequate accommodation), insufficient resources (health and treatment services, trained staff) and geographical isolation limit women's access to appropriate care and support9,10. In the Northern Rivers Area (NRA) of New South Wales (NSW) where the study was conducted, both substance dependent women and service providers identified a limited availability of alcohol and other drug (AOD) services that cater for women with children, including counselling, detoxification and rehabilitation facilities and post-detoxification and rehabilitation support11. Service providers struggle to meet the demand for treatment and support services in an area well known for its drug culture.
Case management has been widely used in the USA substance abuse treatment field as a means to reduce barriers to accessing and continuing treatment, with varying degrees of success12. A small number of studies focusing on women provide evidence that case management results in: reduced substance use during pregnancy for women in community-based prevention, education and treatment projects13; retention in substance abuse treatment during pregnancy14; and a decrease in unmet service needs for high-risk clients not in treatment15.
Recognising the complex needs of rural Australian women dependent on illicit drugs, the 1999 NSW Drug Summit recommended an integrated care trial (known locally as WRAP - Women's Referral and Access Project) to investigate new service delivery models in rural areas with the aim of improving the quality of life of women, including their health and social circumstances, through improved access to services16. Four groups of drug dependent women were targeted: (i) women in methadone maintenance treatment (MMT); (ii) pregnant women and/or women with dependent children; (iii) women residing in Nimbin (a small town known for its illicit drug culture since the 1970s); and (iv) Aboriginal and Torres Strait Islander women (Aboriginal). All target groups were women dependent on illicit drugs, with the exception that Aboriginal women dependent on alcohol but no illicit drugs, could also be included. A preliminary needs assessment identified local women's need for improved access to: social support; a full range of AOD services; GPs who bulk-bill; allied health services; support for pregnant women and mothers; and education/training courses11. Case management was one of multiple strategies developed as part of the integrated care trial.
This article presents the findings from a 12 month study to determine whether community-based case management that was not reliant on either the availability of treatment facilities or specialist AOD services was effective in meeting the broader support needs of women and improving their access to existing services. Specifically the model was assessed as to whether it was effective in achieving the aims which had been set by NSW Health: to improve the quality of life, health and social circumstances of participants. Health was conceived of in broad terms that covered both physical and psychological health, including self-esteem. Social circumstances included issues such as living arrangements, safety, housing, employment and access to required services.
The setting
The WRAP case management was implemented by the Northern Rivers Area Health Service (NRAHS; now known as the North Coast Area Health Service), on the far north coast of NSW. The NRA covers 24 555 km2 with a population of 255 647, of whom 50.9% are women and 3.2% are Aboriginal. The largest regional centre, Lismore, has a population of 44 50017. The NRA is an area of low socio-economic status and has a significant illicit drug use problem compared with the rest of NSW18. It is estimated that approximately 1.5% of the population have a substance use disorder19.
The WRAP case management model
The WRAP model adopts a holistic approach, focusing on improving women's quality of life rather than on reducing drug use per se and/or trying to move women into drug treatment. In contrast with the majority of reported studies on case management, WRAP case management was delivered primarily outside formal AOD treatment services, and women were not required to be in treatment or abstinent from illicit drug use. It is a hybrid model, with its primary function to coordinate and facilitate client access to required services, but with direct service provision by case managers (CMs) where necessary. The WRAP protocols include:
- client self-assessment of key needs using a tool developed by the project team
- development of a case plan with the client
- frequent contact with the client as needed
- three monthly review of case plan
- referrals to required services.
Case managers had a limited pool of funds to broker services directly related to client goals (eg relationship counselling, training courses, optometry or newborn baby needs). This did not include the purchase of drug treatment places, as in the 'brokerage' model of case management20. In two locations, women in case management had free access to a female GP, counselling and natural therapies (massage, naturopathy), through a women's health centre.
Case managers were recruited across the NRA and trained in the WRAP model. During the 12 month trial, 13 individuals (11 females, 2 males) in 14 case management positions actively case managed women as part of WRAP. Eleven of these CMs participated without receiving additional funding from WRAP (non-funded case managers). Nine NRAHS employees (five in existing AOD services) undertook WRAP case management with existing eligible clients, as their workload permitted. Two of the non-funded CMs were from non-government organisations (NGO). Additionally, WRAP funded three part-time CM positions at two NGOs: two were based in Lismore at the Lismore Women's Health Centre (LWHC) and provided outreach to Nimbin (30 km away), and one in Tweed Heads at Tweed Family Centre Community Projects (funded CMs).
The duration of case management was limited by the 12 month trial period and staggered participant recruitment, but most received at least 6 months case management. Funded CMs had caseloads of between nine (working 1 day/week) and 20 clients (working 2 days/week) over a 6 month period; whereas, non-funded CMs typically only had one WRAP client in addition to their existing workloads. The model was not intended to be an outreach service, thus 63% of all client contact was office-based with a further 28% made by phone. Approximately half of all occasions of service (OOS) provided by CMs were classified as case management (case plan reviews, referrals, general check-in with client). Direct service provision was primarily in the area of counselling: 22% of OOS for general counselling; and 11% for AOD counselling. Social and family support accounted for 5% of all OOS. The majority of CMs were qualified counsellors, some working in the AOD field.
Methods
Study design and procedures
To maximise validity, both qualitative and quantitative measures were used in a quasi-experimental longitudinal design with assessments occurring at baseline (recruitment), 3 and 6 months (after recruitment). The qualitative data explored women's experiences and assisted with interpretation of the quantitative data that measured changes. Data were also collected from CMs on their experiences and perceptions, and a range of process measures. However, these data are not included in the current paper, but are provided in the final report21.
After recruitment into case management and provision of written consent, women's contact details were forwarded to the Research Officer (RO) who scheduled the baseline assessment in a location of the woman's choice. Follow-up assessments were scheduled for 3 and 6 months after recruitment and could occur up to one month after this date. At each assessment the RO administered: a structured interview developed by the researchers, the WHO Quality of Life brief version (WHOQoL-BREF)22, and the Rosenberg Self-Esteem Scale (RSES)23.
Case managers were asked to administer the Brief Treatment Outcome Measure (BTOM)24 at baseline and during their 3 month and 6 month case plan reviews. This process was revised during the 3 month data collection phase because some women missed appointments with their CMs, leading to unacceptable rates of missing data. For the remainder of the study, the RO administered the BTOM. Women could withdraw from the study at anytime. The NRAHS Human Research Ethics Committee approved the study.
Instruments
The structured interview assessed women's experiences of case management (positive and negative effects, satisfaction with CM, involvement in case planning, usefulness of case plan, suggested improvements) and outcomes related to specific WRAP objectives (increasing access to health services, education and training and social support) and included open-ended, yes/no and Likert-scale questions. Interviews were audiotaped and professionally transcribed verbatim, with checks for accuracy by the researchers.
The WHOQoL-BREF consists of 26 items from the longer WHOQoL-100 questionnaire of 100 items. It asks about quality of life in the 'last 2 weeks', all items are rated on a five-point scale and it is easily self-administered. The WHOQoL-BREF was developed and field-tested internationally, including in Australia25. The questionnaire includes two items on overall quality of life and general health, while the remaining 24 items measure four domains of quality of life: (i) physical; (ii) psychological; (iii) social relationships; and (iv) environment. The Rosenberg Self-Esteem Scale was selected primarily because of its brevity and because it has been validated and widely used in different populations26. The scale measures self-esteem on a scale from 0 to 30, with higher scores indicating better self-esteem.
The BTOM, developed and validated in Australia, is a brief, multi-dimensional instrument designed for regularly assessing outcomes for clients in AOD treatment. It includes demographics, drugs of concern, the Severity of Dependence Scale (SDS)27, Blood Borne Virus Risk (BBVR) score, quantity and frequency of alcohol and other drug use scores (ODUS), self-reported health status, psychological health (Psychological Wellbeing Scale and number of days bothered by nervous or psychological problems), the Social Functioning Scale, and treatment-specific questions (not relevant for the current study). The majority of items in the BTOM ask about the last 3 months, with the exception of the ODUS score, which covers the last month. The ODUS score is calculated by multiplying the number of days in the last month a substance was used by the average quantity of substance used (that is, number of pills/joints/hits/cigarettes) on those days to give an estimate of monthly use.
Eligibility criteria
Women were eligible to participate in WRAP case management if they could be classified into one of the four target groups, and (if not on MMT), had a score of 3 or more out of 15 on the SDS for her main (illicit) drug of concern. The SDS focuses on psychological aspects of dependence, rather than on withdrawal and tolerance, and is considered a reliable assessment of degree of dependence for a range of drugs. A score of 3 is recommended for cannabis dependence28. Aboriginal women dependent only on alcohol were also eligible for inclusion. The CAGE questionnaire (named for its core concepts of Cutdown, Annoyed, Guilty, Eye-opener) was used to assess level of alcohol dependence, with an eligibility cut-off of 2 or more29. It consists of four questions asking if: (i) the person feels they should drink less; (ii) they get angry when others suggest they should drink less; (iii) they feel guilty about their drinking; and (iv) they sometimes need an early morning drink29. Additionally, to be eligible for the outcome study, women had to complete a baseline BTOM. Women who left case management before the outcome assessments were due were excluded from those assessments.
Analysis
Instrument scoring and data entry were conducted by a trained research assistant with reliability checks on a random sample of 20% of the surveys. Scoring and data entry were found to be accurate. Both quantitative and qualitative data were stored in an Access database.
Comparisons were made between baseline and follow-up scores for women with matched data, that is women with the relevant score at both data collection points. The Wilcoxon signed rank test was used to test changes between baseline and 3 months, and baseline and 6 months. The Wilcoxon signed rank test was used because of the small sample sizes and because the differences were not normally distributed. Small sample sizes did not allow for a statistical comparison between the 3 month and 6 month data. All quantitative data analysis was done using SAS v 8 (SAS Institute Inc., Cary, NC, USA).
For the qualitative data analysis, responses were first grouped together by question, followed by thematic analysis for each question. Thematic codes were compared, discussed by two researchers and consensus reached. The analysis was undertaken using Nudist software (QSR International; Melbourne, VIC, Australia). Comparisons were made between 3 month and 6 month responses to identify additional themes or issues arising over time.
Results
Recruitment to and retention in case management
Sixty-three women were recruited into WRAP case management (19 by non-funded CMs and 44 by funded CMs) during the 12 month trial. Of the 36 women not on MMT, scores on the SDS ranged from 4 to 15 with a mean of 9. Only two of the six Aboriginal women recruited were dependent on alcohol. Of the women recruited: 27 were on MMT, 34 were mothers with dependent children, five were pregnant, 21 resided in Nimbin and six were Aboriginal. Some women belonged to more than one group. The majority (45) were recruited in Lismore and Nimbin, reflecting the location of the LWHC.
At 3 months, 50 women remained in case management. At 6 months, 37/60 remained in case management (three women entered the trial late, and were not yet due for 6 month follow up). Fifteen of the exits followed loss of contact with the client despite repeated attempts by the CMs. Five women reported they had achieved their goals or that WRAP was no longer the most appropriate program to meet further needs. Three women left for other reasons: relocation to another city; found the program too overwhelming at the time; and withdrew from the methadone program where the CM was located.
Women in the outcome study
Of the 63 women commencing case management, 55 completed a baseline BTOM and were thus eligible for inclusion in the outcome study, with the remaining eight women only ever attending one appointment with their CM. At 3 months, 49 women were eligible for inclusion in the study (still in case management and completed a baseline BTOM), of whom 34 had follow-up data collected. At 6 months, 21 of the remaining 35 eligible women had data collected. The main reason for non-response at follow-up assessments was difficulty in contacting women for an interview within the specified timeframe.
Characteristics of the women at baseline are shown (Table 1). The majority of women were aged between 30 and 49 years (38/55), with a median age of 32. Most reported a welfare pension (sickness/disability or single parent) as their main source of income. One-third of women had attained post-secondary education qualifications, including 10 at the tertiary level. Eight women lived in some form of temporary, unstable accommodation including caravan parks and refuges. Approximately half the women (n = 28) recruited lived alone or alone with child(ren) and one-third (n = 16) lived with a spouse/partner or spouse/partner and child(ren).
Table 1: Baseline characteristics of women in the outcome study: all women at baseline, women still in case management at 6 months, women with 6 month BTOM
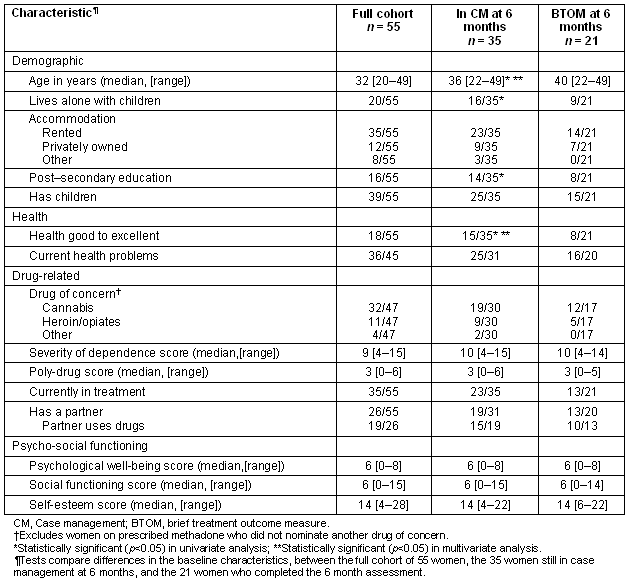
At baseline, median scores on the WHOQol-BREF for the full cohort of 55 women were: overall quality of life (3/5); satisfaction with overall health (2/5); physical and psychological (44/100); social relationships (31/100); and environment (50/100). A comparison of these data with Australian population norms from a community sample28 found highly significant differences on all domains, indicating that the women recruited had significantly lower quality of life than the general Australian community. The full baseline sample had a median score on the RSES of 14/30.
Nearly all women (50/55) reported poly-drug use with a median number of three substances used, including alcohol and tobacco but excluding licit methadone. The most commonly reported illicit drug used in the last month was cannabis (n = 46) followed by opiates (n = 14) and tranquilizers (n = 14). Nearly half the sample (n = 27) was in methadone maintenance treatment. Cannabis was also the most commonly reported 'drug of greatest concern' (n = 32) followed by heroin/opiates (n = 11). The SDS scores for drug of greatest concern showed a median score of 9 out of 15, indicating fairly high levels of dependence. Just under half of the sample (n = 22) reported injecting drug use in the last 3 months, while 18 had never injected. Tobacco was the most commonly reported licit substance used (n = 50), followed by alcohol (n = 34).
At baseline, nearly all women (51/55) reported being bothered by nervous, mental or psychological problems in the last 3 months, with half reporting daily problems. Scores on the Psychological Wellbeing Scale ranged from 0 to 8 (out of 8) with a median score of 6 (higher scores indicate lower levels of wellbeing). Scores for the Social Functioning Scale ranged from 0 to 15 (out of 15) with a median score of 6 (higher scores indicate lower functioning).
Measures of general physical health included: from the WHOQoL-BREF satisfaction with overall health and the physical domain; from the BTOM self-reported health status in the last 3 months; and women's self-reports of health problems in the interview. Baseline data across these different measures indicate a low level of physical health. On recruitment, the majority of women reported multiple and often chronic health problems, and 36 of 55 rated their health status in the last 3 months as poor or fair. Scores on the two WHOQoL-BREF measures were also relatively low.
To identify predictors of retention in case management and assess bias in the 6 month sample, differences in the baseline characteristics were examined between the full cohort of 55 women, the 35 women still in case management at 6 months, and the 21 women who completed the 6 month assessment (Table 1). Age, living alone with children, post-secondary education, and health reported as good to excellent were associated with retention in case management at 6 months on univariate analysis. These variables were entered into a multivariate logistic regression model to identify predictors of retention. Only age (OR 1.18, 95% CI: [1.05, 1.31]) and health (OR 12.00 95%CI: [1.75, 82.57]) were significant in the final model. That is, women who remained in case management were older and reported better health at baseline than those who dropped out. No significant differences were found between the 6 month study sample (n = 21) and all women remaining in case management at 6 months. However, the relatively small sample size limits the ability to detect these differences.
Outcomes of case management
Among the 34 women with matched baseline and 3 month data there were increases in the median score between baseline and 3 months, for all domains of the WHOQoL-BREF, suggesting general improvements in women's quality of life (Table 2), although the increase was statistically significant only for the psychological domain (from 44 to 56, p = 0.02) and the environment domain (from 53 to 63, p = 0.037). However, all the 3 month median scores remained low relative to the Australian population norms. Similar trends in quality of life outcomes were observed in the 6 month sample, including a significant improvement in the psychological domain (from 44 to 63, p = 0.0002; Table 3). Over time, the scores on the psychological domain appeared to increase consistently between baseline (median = 44), 3 months (median = 56) and 6 months (median = 63). There were highly significant improvements in women's self-esteem between baseline and 3 months (14 to 17.5, p<0.0001), and baseline and 6 months (14 to 17, p = 0.0006), among women with matched data, although the median scores were still low.
Table 2: Comparison of baseline and 3-month data for women with matched data
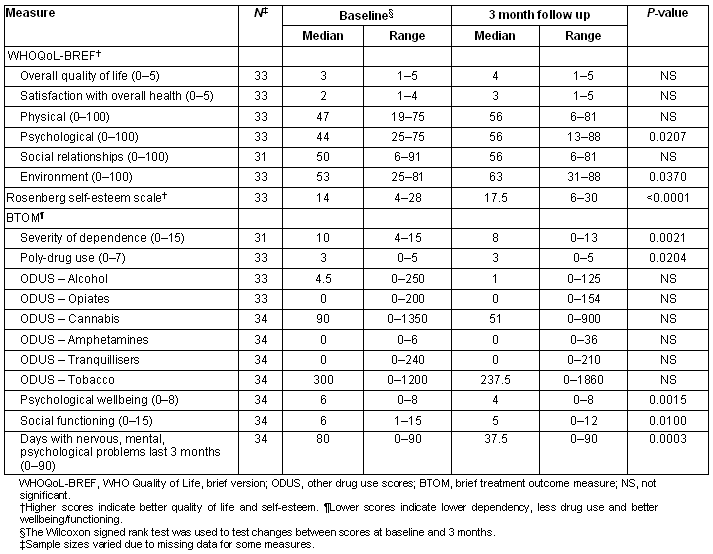
Table 3: Comparison of baseline and 6-month data for women with matched data
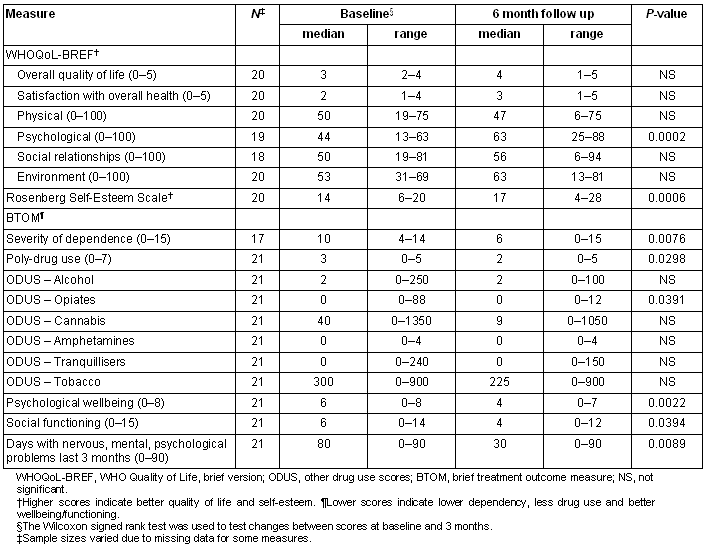
Significant improvements were found on a number of the BTOM median scores between baseline and 3 months: severity of dependence (from 10 to 8, p = 0.0021); poly-drug use (from 3 to 3, p = 0.0204); psychological wellbeing (from 6 to 4, p = 0.0015); social functioning (from 6 to 5, p = 0.0100); and the number of days women reported psychological problems in the last 3 months (from 80 to 37.5, p = 0.0003) (Table 2). Decreases in the use of cannabis and tobacco, the most widely used substances, were found but were not significant. The same significant results were observed between baseline and 6 months (Table 3). The data also suggest a continuous reduction in the severity of dependence and a continuous improvement in social functioning over 6 months; however, the small sample size did not allow for a statistical comparison over time.
Women's experiences of WRAP case management
If it wasn't for WRAP I wouldn't have been able to go on. It's given me support, confidence in myself and strength to keep going. (At 3 months)
Nearly all women reported a range of positive effects resulting from their participation in WRAP case management. The majority of women reported improved physical health in their interviews, which they attributed largely to the free access to medical and complementary health services at LWHC.
It's usually really hard for me to get appointments and afford them so WRAP has been affordable, regular support, both emotional and physical. Knowing that it's regular and ongoing, I've been able to deal with ongoing health issues with the naturopath. (At 6 months)
It's been good having access to a woman doctor. The massage and other programs have been excellent. I'm feeling less isolated. (At 6 months)
The most commonly identified benefits were similar at 3 and 6 months: regular and ongoing support; improved access to health services; reduction in drug use; improved self-esteem and increased motivation.
Being treated like a human being, having my needs considered, having someone to listen to me. (At 3 months)
Case management has enabled me to access services that I've needed. I didn't know some of the services were available before that. It's put me in touch with INTRA and other drug-related services. (At 3 months)
Counselling has been what's gotten me through. I feel capable of doing things I didn't think I could. (At 3 months)
Its given me the push to be honest with myself and get up in the morning. (At 3 months)
Other outcomes reported by some women included, improved parenting and/or relationships, assistance with employment, improved access to other services and a decreased sense of isolation.
Its [WRAP] helped me get direction, especially when I started. Helped me get out of a DV situation. It helped to have someone objective to talk to and offer advice. Helped keep my focus on life. (At 3 months)
I think I've provided better care for my son. I think I could've got postnatal depression but they've really helped me get through the initial stages of motherhood. They were life saving. (At 3 months)
When asked how WRAP case management had contributed to these outcomes, women at both 3 and 6 months highlighted the importance of the regular and ongoing support provided by, and the availability of, their CM in enabling them to confront and deal with their problems.
It's like having someone who is your contact with the world. She's the person you can ask all the silly questions and not be judged. She takes me seriously. She's always so positive, available when I need her and happy to hear from me. (At 3 months)
Because I've had just one person she knows what I'm doing. There's someone who's interested in my life. She sent me to have a massage and then asked how it went. (At 3 months)
It was like a counselling role but I felt more relaxed. Case management was different from counselling I have had. I was really comfortable with her [CM]. I really trusted her. (At 3 months)
At 6 months, women being case managed at the LWHC emphasised the support from a team, not just their CM. Many of these women also commented on the importance of access to bulk-billing GPs and free complementary health care (massage, naturopathy) in enabling them to move forward in their lives.
It's a great support network, the team at Women's Health Centre. It's a really positive time in my fortnight to have a massage and see the counsellor and doctor. I haven't had a drink or cigarette for 3 months. (At 6 months)
It's given me someone to talk to so I'm not feeling so alienated. Provides a great team support system. The team approach has been important. (At 6 months)
Case plans and their regular review also contributed to the positive perceptions of case management. Women found that the case planning process helped to: clarify goals; provide perspective, focus and direction; and prioritise issues, while the case plan reviews acted as positive reinforcement.
At the 3 month interview, two women did not report any positive effects of their participation because they felt very little or nothing had happened for them. At 6 months, two women reported negative effects in addition to benefits, one stating she had experienced people in her community calling her a drug addict.
Discussion
This article described a case management model for drug dependent women, and presented outcomes from a trial in a rural area. Women who entered the program had moderate needs but significant drug use issues, both of illicit and licit substances. After 6 months, 62% of women recruited remained in case management, with older women and those with better self-reported health status at recruitment more likely to do so. The positive impact of WRAP case management on women's lives was consistently identified over time and by different data collection methods: in women's comments about their experiences in case management and the outcome measures. These findings were confirmed by observations made by CMs21. The results indicate that the model, linking women with services and some direct service provision, was generally well accepted by women, and achieved significant improvements in quality of life, and health and social circumstances, consistent with the trial aims. Improvements were most marked in terms of psychological wellbeing, self-esteem, and social functioning, with significant reductions in drug dependency and drug use.
Data from the psychosocial outcome measures are consistent with women's subjective reports of the positive impact of case management. Self-esteem has been shown to be an important predictor of substance use and psychological wellbeing30, and of retention in treatment31. The improvements in self-esteem and other psycho-social domains may have contributed to the changes observed in relation to drug use: a significant reduction in severity of dependence and in the number of different classes of drugs used by women; and a trend towards less heavy use of all drugs in the last month, with a significant decrease in opiate use.
For women, the most valuable aspect of case management was the regular support provided by their CM. Their comments highlighted the importance of having access to one trusted, non-judgemental individual who both listens and provides practical assistance. These findings are consistent with previous work identifying the relationship between the client and CM as critical12,32, and the importance of combining practical support and advice with emotional support33. Case managers also identified this as one of the key factors contributing to successful case management21. Women also highlighted the positive role of the case planning process in enabling them to identify unmet needs, and set and achieve goals. Case plans also provided a formal mechanism to review progress, providing positive reinforcement for women. Brun and Rapp34 report similar findings from case management clients in a substance abuse aftercare program who noted the value of goal planning. This would suggest that development of a case plan and regular review of client progress is an integral component of successful case management for drug dependent women.
The funding for the trial was for a limited period. However, the services involved have attempted to sustain implementation of the model. Those services which were undertaking case management within existing resources have continued to use the model. The two NGOs that were funded to employ a CM have also continued to use the model and approach within available resources. However, to date they have not been successful in obtaining funding to employ a CM.
Limitations
This study used a quasi-experimental longitudinal design with assessment at baseline, 3 month and 6 months, and did not have a control group. Changes in outcomes were assessed by comparison of women's 3 month and 6 month data with their baseline data. It is possible that some of the observed changes in outcomes were an artefact of participation in the research and/or that changes were unrelated to case management. To maximise validity, and to contextualise the quantitative data, different data collection methods were used. Although not reported here, CMs were also interviewed21. In most cases there was concordance between these different methods.
During the trial, 23 women left case management but for most, the reasons are unknown. It is likely that case management was less successful at meeting their needs than it was for those who remained. This is a concern because the women who left were younger and had poorer health status. Many of these women were thought to be itinerant because they only had one contact with their CM, after which they were untraceable. Thus, positive outcomes and comments cannot be generalized to all women recruited. Additionally, the 6 month matched sample was relatively small due to difficulties following women up for assessments at this stage. Although there was no evidence that the final sample differed from all women remaining in case management, the small sample size limits the ability to detect differences and the women may differ on factors not measured. Thus, the findings may not be generalizable to all women remaining in case management. Finally, the small number of women with matched results limits the ability to detect meaningful changes and, thus, it is possible that the study has underestimated or overestimated the benefits. Despite these limitations, it is clear that for the women for whom both baseline and 6 month data were available, the program resulted in significant important benefits.
Conclusions
The WRAP case management model, one of adopting a holistic approach with a focus on improving women's quality of life rather than focusing on reducing drug use per se and/or trying to move women into drug treatment, appears to be successful. There is strong evidence for improvement in many areas of women's lives over the period of case management. For women, the success of case management was a result of the consistency and continuity provided by having one person who provided much needed support and assistance.
Given that most studies of case management have focused on treatment access and retention, these findings make an important contribution to currently limited evidence on the impact of case management on treatment outcomes for substance using women. Overall, these findings add weight to existing claims that addressing women's specific needs and broader issues in their lives can lead to improved outcomes, including a reduction in drug use6,35,36.
Acknowledgements
The authors wish to acknowledge that the rural Integrated Care Trial for Drug Dependent Women was funded by the Drugs Program Bureau (now known as the Centre for Drug and Alcohol), New South Wales Health, and managed by Area Mental Health Services, North Coast Area Health Service. The authors would like to thank Richard Buss, Manager Area Mental Health Services, and the project Steering Committee for their support and advice. Thanks also to Kris Keevers, WRAP Project Officer, for her contribution to the project development and implementation. The authors especially thank the women and service providers who participated in this study.
References
1. Swift W, Copeland J, Hall W. Characteristics of women with alcohol and other drug problems: findings of an Australian national survey. Addiction 1996; 91: 1141-1150.
2. Hunter GM, Judd A. Women injecting drug users in London: the extent and nature of their contact with drug and health services. Drug and Alcohol Review1998; 17: 267-276.
3. O'Connor LE, Berry JW, Inaba D, Weiss J, Morrison A. Shame, guilt, and depression in men and women in recovery from addiction. Journal of Substance Abuse Treatment 1994; 11: 503-510.
4. Fiorentine R, Anglin MD, Gil-Rivas V, Taylor E. Drug treatment: explaining the gender paradox. Substance Use and Misuse 1997; 32: 653-678.
5. Brown VB, Melchior LA, Panter AT, Slaughter R, Huba GJ. Women's steps of change and entry into drug abuse treatment a multidimensional stages of change model. Journal of Substance Abuse Treatment 2000; 18: 231-140.
6. Ashley OS, Marsden ME, Brady TM. Effectiveness of substance abuse treatment programming for women: a review. American Journal of Drug and Alcohol Abuse 2003; 29: 19-35.
7. Hagan TA, Finnegan LP, Nelson-Zlupko L. Impediments to comprehensive treatment models for substance-dependent women: treatment and research questions. Journal of Psychoactive Drugs 1994; 26: 163-171.
8. Copeland J, Hall W, Didcott P, Biggs V. A comparison of a specialist women's alcohol and other drug treatment service with two traditional mixed-sex services: client characteristics and treatment outcome. Drug and Alcohol Dependence 1993; 32: 81-92.
9. Dunn P. Introduction. Rural health and drug and alcohol dependence: doublejeopardy. In: S Griffith, P Dunn et al. (Eds). Drug and alcohol services in rural and remote Australia. Issues paper. Wagga Wagga: Charles Sturt University, 1998; 1-6.
10. New South Wales Government. New South Wales Ministerial Committee on Health Service in Smaller Towns. Report to the NSW Minister for Health. A framework for change. Sydney: NSW Government, 2000.
11. Sheldrake M, Leitch K, Keevers K, Gilmore V, Passey M. A wrap up of the needs assessment November 2001 - February 2002. An integrated care trial for drug (illicit) dependent women and their families. Lismore, NSW: Northern Rivers Area, Health Service, 2003.
12. Siegal HA, Rapp RC, Li L, Saha P. Case management in substance abuse treatment: perspectives, impact, and use. In: FM Tims, CG Leukefeld et al. (Eds). Relapse and recovery in addictions. New Haven: Yale University Press, 2001; 253-274
13. Eisen M, Keyser-Smith J, Dampeer J, Sambrano S. Evaluation of substance use outcomes in demonstration projects for pregnant and postpartum women and their infants: findings from a quasi-experiment. Addictive Behavior 2000; 25: 123-129.
14. Laken MP, Ager JW. Effects of case management on retention in prenatal substance abuse treatment. American Journal of Drug and Alcohol Abuse 1996; 22: 439-448.
15. Thompson AS, Blankenship KM, Selwyn PA, Khoshnood K, Lopez M, Balacos K et al. Evaluation of an innovative program to address the health and social service needs of drug-using women with or at risk for HIV infection. Journal of Community Health 1998; 23: 419-440.
16. New South Wales Government. NSW Drug Summit 1999 Government Plan of Action. Sydney: New South Wales Government, 1999.
17. Northern Rivers Health Equity Working Group. Northern Rivers equity profile - phase 1. Lismore, NSW: Northern Rivers Area Health Service, 2003.
18. Parke J. Drugs and community action strategy situation analysis North Coast. Coffs Harbour, NSW: Premier's Department New South Wales, 2000.
19. Northern Rivers Area Health Service. NRAHS strategic directions for drug and alcohol services. Lismore: Northern Rivers Area Health Service, 2001.
20. Bedell JR, Cohen NL, Sullivan A. Case management: the current best practices and the next generation of innovation. Community Mental Health Journal 2000; 36: 179-194.
21. Sheldrake M, Passey M, Leitch K, Keevers K, Gilmore V, Bardon V. Evaluation of Women's Referral and Access Project (WRAP). A rural integrated care trial for women dependent on illicit drugs. Final Report. Lismore, NSW: Northern Rivers Area Health Service, 2003.
22. World Health Organization. WHOQOL-BREF introduction, administration, scoring and generic version of the assessment. Field trial version. Programme on mental health. Geneva: World Health Organization, 1996.
23. University of Maryland. The Rosenberg Self-Esteem Scale. College Park, MD: Sociology Department University of Maryland, 2002.
24. New South Wales Health. Brief treatment outcome measure administration and procedures manual. Sydney: NSW Health, 2002.
25. Australian Centre for Posttraumatic Mental Health. The Australian WHOQol-BREF. Description of the Australian WHOQoL-BREF. Melbourne, VIC: Australian Centre for Posttraumatic Mental Health, 2003.
26. Blascovich J, Tomaka J. Measures of self esteem. In: JP Robinson, PR Shaver, LS Wrightman (Eds). Measures of personality and social psychological attitudes: volume 1 in measures of social psychological attitudes series. San Diego, CA: Academic Press, 1991
27. Gossop M, Darke S, Griffiths P, Hando J, Powis B, Hall W, Strang J. The Severity of Dependence Scale (SDS): psychometric properties of the SDS in English and Australian samples of heroin, cocaine and amphetamine users. Addiction 1995; 90: 607-614.
28. Swift W, Copeland J, Hall W. Choosing a diagnostic cut-off for cannabis dependence. Additction 1998; 93: 1681-1692.
29. Ewing JA. Detecting alcoholism: The CAGE Questionnaire. JAMA 1984; 252: 1905-1907.
30. Stein JA, Leslie MB, Nyamathi A. Relative contributions of parent substance use and childhood maltreatment to chronic homelessness, depression, and substance abuse problems among homeless women: mediating roles of self-esteem and abuse in adulthood. Child Abuse and Neglect 2002; 26: 1011-1027.
31. Bartholomew NG, Rowan-Szal GA, Chatham LR, Simpson DD. Effectiveness of a specialized intervention for women in a methadone program. Journal of Psychoactive Drugs 1994; 26: 249-255.
32. Meier PS, Barrowclough C, Donmall MC. The role of the therapeutic alliance in the treatment of substance misuse: a critical review of the literature. Addiction 2005; 100: 304-316.
33. Finkelstein N. Treatment programming for alcohol and drug-dependent pregnant women. International Journal of Addiction 1993; 28: 1275-1309.
34. Brun C, Rapp RC. Strengths-based case management: individuals' perspectives on strengths and the case manager relationship. Social Work 2001; 46: 278-288.
35. Salmon MM, Joseph BM, Saylor C, Mann RJ. Women's perception of provider, social, and program support in an outpatient drug treatment program. Journal of Substance Abuse Treatment 2000; 19: 239-246.
36. Hser Y, Polinsky ML, Maglione M, Anglin MD. Matching clients' needs with drug treatment services. Journal of Substance Abuse Treatment 1999; 16: 299-305.
