Introduction
The Northern Territory (NT) is situated in northern Australia. It is large - over 1.3 million km2 - and is sparsely populated. It has a total population of approximately 200 000, 59% of whom live in either the capital, Darwin, or in Alice Springs. Twenty-nine percent of the population is Aboriginal1.
Health workforce shortages have long plagued the NT, and the Australian Department of Health and Ageing has designated the NT a 'district of workforce shortage' annually since 1996, when the classification system was first implemented. This problem has been exacerbated by the geographic remoteness of its population, the high prevalence of both infective and chronic diseases, and the complex challenges of Indigenous health. Numerous programs in Australia and abroad have demonstrated the effectiveness of local training as one strategy to address health workforce shortages2-6. In 1994, the Australian Government commenced a 'Rural Health Initiative' to address regional health workforce deficits, leading to the development of over a dozen rural- and community-based clinical training programs across Australia7. The James Cook University School of Medicine (Townsville, Queensland) recently reported a retention rate of over 60% of its first graduating class to internships in northern and/or non-metropolitan Queensland8. Longitudinal studies addressing long-term graduate retention in these regions are underway.
Similar tactics have been applied in the NT. The Flinders University School of Medicine (Adelaide, South Australia) and the NT Government collaboratively established the Northern Territory Clinical School (NTCS) in Darwin in 1997 as a teaching site for students of Flinders University School of Medicine. To reinforce the mission of local recruitment, an annual enrolment quota of 10 Northern Territory and five Aboriginal and Torres Strait Islander students was implemented. On average, five of the quota placements have been filled each year (between 1999 and 2005, only two students enrolled under the Aboriginal and Torres Strait Islander quota.), with the remaining 15 placements allotted to other third-year Flinders University students. In addition, medical students from other institutions and final year Flinders University students can elect to undertake one or more short placements (2-6 weeks) in the NT through the NTCS. Since its inception, the NTCS has matriculated over 140 students (including 37 quota placements) and provided nearly 2000 short placements for other Australian and international students.
The strategic goals of the NTCS are to recruit local, and Aboriginal and Torres Strait Islander students to the Flinders University School of Medicine program, to facilitate a positive and meaningful clinical learning experience, to impart an appreciation for the unique health issues of the NT, and to cultivate a supportive professional network for students and faculty. In principle, these aims enable the NTCS to act as a conduit for medical graduates to join the NT workforce.
This article presents an assessment of the outcomes of six academic years (Flinders School of Medicine graduates: 1999-2005) with respect to the impact of the NTCS on the NT medical workforce. Ongoing studies are in place to evaluate the role of the NTCS in clinical staff and graduate retention, and to identify specific factors associated with living and working as a clinician in the NT.
Methods
Our retrospective analysis included 452 Flinders School of Medicine graduates from 1999 to 2005; students with incomplete records were excluded from the study. Data regarding students' year of enrolment at NTCS, sex, Aboriginal or Torres Strait Islander classification, NT quota status, and total weeks spent in NT placements were collected from the internal (NTCS) administrative database. Internship site was ascertained from the Royal Darwin Hospital intern records and the Flinders Department of Medical Education. The NT Health Professions Licensing Authority medical register was referenced to determine current or elapsed NT registration and registration category.
For the purposes of this study, students who completed their third year of Flinders University Medical program through NTCS are classified as 'NTCS students', and this was further divided into NT quota and non-quota categories. The remaining Flinders University School of Medicine graduates (who in some cases may have undertaken short elective or 'selective' placements in the NT during their final year) are identified as 'non-NTCS'.
Records were de-identified using random number assignment to replace identifying data. SPSS software (SPSS Inc; Chicago, IL, USA) was employed for statistical analysis. De-identified data was evaluated by student's t-test, analysis of variance (post hoc pairwise comparisons were made using protected least significant difference test), cross-tabulation, and/or the χ-square distribution test as appropriate. Differences were considered significant where p<0.05.
Ethical approval for this study was obtained through the Human Research Ethics Committee of the NT Department of Health and Community and Menzies School of Health Research (06/32).
Results
Our analysis was undertaken to evaluate the training experience and internship placement decisions of 452 Flinders University graduates from 1999 to 2005. Ninety-six of the students included in the study undertook their third year of training with NTCS, including 27 enrolled through the NT/Aboriginal and Torres Strait Islander quota program (Table 1).
Table 1: Distribution of students included in the study
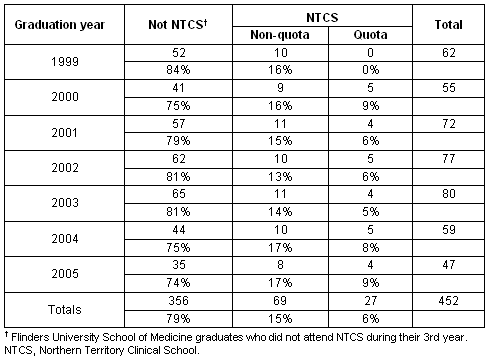
NTCS students spent a significantly greater period of time in the NT during their final (4th) year of the Flinders Medical program than non-NTCS Flinders medical students (16.7 ± 7.9 weeks vs 1.9 ± 3.9 weeks; p<0.01). Placements completed by NTCS quota students were, on average, 25% longer than non-quota students' placements (20.4 ± 8.9 weeks vs 15.3 ± 6.9 weeks; p<0.05).
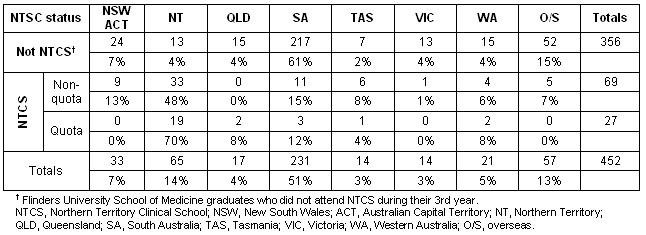
Australia-wide, over 90 intern positions were filled by NTCS students between 1999 and 2006; five students chose internships overseas. NTCS students were more than 10 times as likely to spend their intern year in the NT as non-NTCS Flinders graduates; this probability was even higher for the NTCS quota group. Over 70% of NTCS quota students chose an internship position at NT hospitals (Table 2).
Table 2: Flinders University medical graduates' internship placements (1999-2005). The majority of NTCS students undertook internships in the NT (48% of non-quota students and 70% of quota students), while most (61%) non-NTCS Flinders graduates interned in South Australia.
A relationship between the length of time spent in the NT during the final year and electing an NT internship became apparent in our study (Table 3). Students who spent over half (20 weeks) of their final year in electives/selectives in the NT were nearly 20 times more likely to choose an internship in the NT than those who spent less than 20 weeks. Flinders University graduates who spent less than 20 weeks in the NT during their final year were most likely to internship in South Australia. Of the 65 Flinders University students in the study who interned in the NT, 13 were non-NTCS students, most of whom had spent less than 20 weeks in the NT during year 4.
Interestingly, over 60% of quota students who interned in the NT had elected to spend most of their final year in NT, while non-quota students completed shorter year 4 placements before returning to the NT for internship training (Fig 1).
Table 3: Study sample cross-tabulation: internship state by time spent in the Northern Territory during year 4
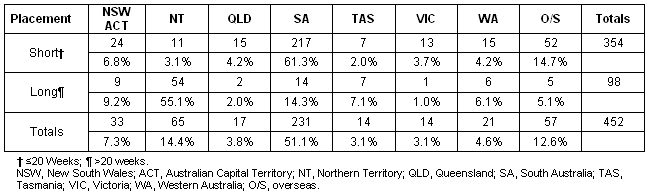
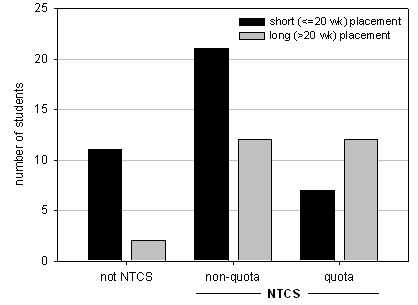
Figure 1: The number of Flinders University-graduated Northern Territory (NT) interns who completed long or short placements in the NT during their final (4th) year of medical school. NTCS, Northern Territory Clinical School.
The Medical Board of the NT grants conditional registration to medical graduates undertaking internships in NT hospitals - full registration may be applied for with satisfactory completion of the intern year. Forty-nine students included in this study had been granted full registration in the NT; of the 39 graduates with current/active registration (as of August, 2006), 29 (74%) were NTCS alumni.
Discussion
The NT capital, Darwin, is not usually considered part of rural Australia, but due to its small size and remote location, it bears many similarities to rural areas - including a medical workforce shortage. The results of our study demonstrate that the establishment of a clinical training program with an emphasis on local recruitment is an effective method of augmenting the local health workforce. A substantial fraction of NTCS alumni have elected to compete their intern year in the NT, a preference that strongly associates with the length of time spent in the NT during the final year/s of their degree. In addition, it has been shown that many of our graduates are or have been registered by the Medical Board of the NT - although the long-term retention rate of these junior doctors is as yet undetermined. And while retention is recognised as a key challenge to the NT health workforce, addressing this issue falls in many ways beyond the scope of the NTCS. Future studies are planned to evaluate whether and how preceptorship impacts job satisfaction and retention (ie for consultants engaged in teaching the NTCS medical students). Our other current research endeavours include exploring the motivations and expectations of incoming students, identifying the variables that influence student training and career decisions, and gaining a clearer understanding of the impact of the NTCS on the urban and rural medical workforce in the NT.
The factors that influence medical student recruitment and retention, especially in regard to the rural workforce, remain a topic of considerable interest and research. Such factors were identified in a recent report5, which reviewed and compiled key outcomes of 21 multivariate cohort studies undertaken in US medical schools between 1990 and 2000. In this analysis, individual factors were characterised as deriving by 'nature' (pre-medical school - inherent to the student or resulting from their upbringing) or 'nurture', that is factors influenced by the medical training experience (Fig 2). This differentiation is useful in terms of identifying issues relevant to recruitment tactics and for developing approaches to 'nurturing' future practitioners through the curriculum and training experience.

Figure 2: Factors associated with the recruitment of physicians to rural areas. From key issues described in Brooks et al5.
Two pre-medical school factors found to have significant association with rural recruitment were: (I) having had a rural upbringing; and (ii) expressing a career intention of rural or family practice. The presumed relevance of these factors to the NT was a driving force behind the implementation of the NTCS quota program - the 'train locals locally' approach. Indeed, a condition of application to the NTCS quota is residential status in the NT, and the great majority of applicants report an intention to live and work in the NT at the completion of their training (as reported in anonymous, voluntary surveys conducted for an internal audit of the NTCS, 2006, data not shown). Reasons behind the low number of students applying under the Aboriginal and Torres Strait Islander quota remain unknown, but addressing this issue is a priority in the recruitment and strategic planning endeavours of the NTCS.
A significant proportion of non-NT students who come to study in the NT also stay for internship training; therefore, it is valuable to understand what drives their career decisions. A widely held perception is that the allure of the NT lies in its promise of adventure and opportunities to contribute meaningfully to Indigenous health; however, little research has been done to substantiate these ideas. Results of our preliminary studies on the motivation and intentions of our students suggest that a tropical/outback lifestyle and challenging clinical environment are enticing factors (authors' pers. data, 2006). And, as anticipated, an interest in Indigenous health was commonly cited as a reason for choosing to study in the NT.
Aspects of the medical school and/or the training experience also relate to career choice; in particular, location in a rural state, public ownership, and community-based curricula were associated with higher rates of recruitment to rural areas5,9. Although the NTCS utilises a primarily hospital-based teaching framework, students undertake placements in both a rural and urban general practice, and the integration of NT health issues across the curriculum is a core strategic aim of the program.
The NTCS is keenly aware of the current issues in medical education and the health workforce, and is committed to reflecting these matters in its administrative and academic strategies. Research addressing the effectiveness of the clinical school in achieving its aims will guide future directions and shed light on important questions in clinical training. Longitudinal studies are necessary to evaluate the long-term impact of the NTCS; in the meanwhile, efforts will continue toward understanding the factors involved in producing highly-skilled, dedicated, and compassionate clinicians.
Conclusions
The NTCS has trained over 100 medical students, many of which have joined the NT health workforce as interns and junior doctors. Through a quota program, we have engaged local students who express an interest in living and studying in the NT; studies are underway to assess the impact of this recruitment strategy on the regional workforce shortage. Alhough preliminary, this study supports the concept that 'training locals locally' is an effective mechanism to enlist and retain clinicians to the NT.
Acknowledgements
The authors extend their appreciation to the Flinders Department of Medical Education and Dr Vino Sathianathan (Deputy Medical Superintendent, Royal Darwin Hospital) for the provision of data; and Joseph McDonnell (Menzies School of Health Research) for statistical advice.
References
1. Northern Territory Government. Northern Territory submission to the Productivity Commission Health Workforce Study - Department of Health and Community Services. (Online) 2005. Available: http://www.pc.gov.au/study/healthworkforce/subs/subpp182.pdf Accessed 26 April 2007.
2. Mathews M, Rourke JTB, Park A. National and provincial retention of medical graduates of Memorial University of Newfoundland. Canada Medical Association Journal 2006; 357-360.
3. Dunbabin JS, McEwin K, Cameron I. Postgraduate medical placements in rural areas: their impact on the rural medical workforce. Rural Remote Health 6: 481. (Online) 2006. Available: www.rrh.org.au (Accessed 26 April 2007).
4. Peach HG, Trembath M, Fensling B. A case for more year-long internships outside metropolitan areas? Medical Journal of Australia 2004; 180: 106-108.
5. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77: 790-798.
6. Kamien M, Buttfield IH. Some solutions to the shortage of general practitioners in rural Australia. Part 4. Professional, social and economic satisfaction. Medical Journal of Australia 1990; 153: 168-171.
7. Australian Government. National Rural Health Strategy. In: Australian Health Ministers' Conference. Canberra: Australian Government Publishing Service, 1994.
8. Veitch C, Underhill A, Hays RB. The career aspirations and location intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation. Rural Remote Health 6: 537. (Online) 2006. Available: www.rrh.org.au (Accessed 26 April 2007).
9. Rabinowitz HK, Diamond JJ, Markham FW, Hazelwood CE. A program to increase the number of family physicians in rural and underserved areas: impact after 22 years. JAMA 1999; 281: 255-260.
Abstract
Introduction: The Northern Territory Clinical School (NTCS), a teaching site of the Flinders University School of Medicine, was established in Darwin, Northern Territory (NT; 1997) in response to a need for regional clinical training. An enrolment quota of NT resident, Aboriginal and Torres Strait Islander students was implemented to encourage the recruitment of local applicants to the medical program. The objective of this study was to assess the impact of the NTCS and the quota program on the NT health workforce at the intern and junior doctor levels.
Methods: A database was constructed to compile the training location, quota participation, place of internship, and NT medical registration of 452 Flinders School of Medicine graduates (1999-2005). Statistical analysis of de-identified data yielded outcomes regarding length of placement in the NT, internship state, and registration by the NT medical board.
Results: Students enrolled with the NTCS elected to spend significantly more time in the NT during their final year of medical school than non-NTCS Flinders University students (16.7 ± 7.9 weeks vs 1.9 ± 3.9 weeks; p<0.01). Quota students undertook longer NT placements than their non-quota NTCS peers (20.4 ± 8.9 weeks vs 15.3 ± 6.9 weeks; p<0.05). A significant proportion (54%) of NTCS alumni completed their internship training in the NT, and NTCS students were more than 10 times more likely to spend their intern year in the NT than non-NTCS Flinders graduates. Of the quota cohort, 70% chose an internship position at NT hospitals. Likewise, NTCS students were more than 10 times as likely to have current or expired registration on the NT medical register as other Flinders School of Medicine graduates.
Conclusions: The NTCS has trained over 140 medical students, many of which have joined the NT health workforce as interns and junior doctors. The quota program has been an effective method of enlisting local students who express an interest in living and studying in the NT. Current studies are underway to assess the impact of NTCS recruitment and training strategies on the regional workforce shortage. This preliminary data supports the concept that 'training locals locally' has had positive outcomes for the NT health workforce.
Key words: clinical school, medical workforce, Northern Territory.
You might also be interested in:
2019 - We Have to Drive Everywhere: Rural Nurses and Their Precepted Students
2007 - GP perceptions of workforce shortage in a rural setting

