Introduction
Indigenous Australians experience poor health compared with their non-Indigenous counterparts, as evidenced by a life expectancy 17 years less than that of non-Indigenous Australians1. Moreover, 97% of Indigenous people over the age of 55 years are reported to have at least one chronic health condition2. Asthma, diabetes, and heart and circulatory problems are the three most common diseases reported, with the prevalence of diabetes in the Indigenous population four times that of the non-Indigenous population2.
Inequalities in the health of Indigenous Australians are related to a complex interplay of historic, socioeconomic, cultural and access issues. These ultimately have led to ineffective health services and reduced access to health resources such as essential medicines3-10.
Despite the complexity of reasons contributing to the poor health status of the Australian Indigenous population, a number of significant advances towards improved health care have been made recently. Three significant and successful strategies have been the development of Aboriginal controlled community health organizations and Aboriginal medical services (AMS)11, the expansion of the role of Aboriginal health workers (AHWs)11 and the implementation of Section 100 (S100) of the Australian Pharmaceutical Benefits Scheme (PBS) medicines scheme12.
Under the current S100 scheme, AMS in remote areas can order bulk supplies of PBS medications through a selected pharmacy, and distribute them to patients without charge12. The introduction of this scheme has helped many in remote areas who otherwise may not have had access to medications. However, in 2001 only 27% of our 458 500 strong Indigenous population lived in remote areas of Australia, with 30% living in major cities and the remaining 43% in rural or regional centers13,14. It has been estimated that S100 benefits 36% of the Australian Indigenous population. However, of the 153 S100 approved Aboriginal and Torres Strait Islander health services only four are located in New South Wales (NSW)12, the state with the largest Indigenous population (29%)1,2. This suggests that the program currently may not serve a large proportion of the NSW Indigenous population and that a shortfall still exists in Indigenous access to and use of medication. Spending on pharmaceuticals under the PBS in 2001-2002 per capita in the Indigenous population still remained significantly lower, at one-third that of the non-Indigenous population2.
The 76% of the Indigenous population who do not live in remote areas must obtain their medications through standard delivery systems, for example by visiting a GP for a prescription, and then visiting a pharmacy to have the prescription filled. Where distance explains the lack of access to mainstream health services and pharmacies by Indigenous Australians in remote areas, it does not explain the lack of uptake in urban and rural areas, and indicates that other factors come into play in these circumstances. Unlike the S100 supply scheme, standard delivery systems are not tailored to Indigenous people and may not be appropriate for them to access, and yet the health problems that burden Indigenous Australians are not limited to remote populations15. As a consequence, it has been suggested that the S100 scheme should be made available throughout Australia, allowing Aboriginal people in all areas to access their medications for no charge via their AMS15.
Although the S100 scheme has been a necessary step to address a chronic and serious problem in remote areas, it has made it more difficult for pharmacists to ensure the quality use of medicines since stock control and patient counselling is carried out by the clinic staff, rather than the pharmacist15. Moreover, the introduction of S100 has done little to change the responsiveness of mainstream pharmacy services to the needs of Indigenous Australians. The proposed expansion of S100 raises concerns of a separation of pharmacy services for Indigenous Australians from mainstream services and would require almost no adjustment by pharmacies and pharmacists to meet the needs of Indigenous people.
Our previous study, Hamrosi et al.5 in 2004, which explored the views of AHWs in the then Mid Western Area Health Service, suggested that problems relating to quality use of medicines (QUM) in the community were common. Poor compliance with instructions due to poor understanding, lack of money and low literacy were cited as some of the issues. The AHWs interviewed made suggestions that could be implemented in pharmacies in the future to make them more accessible to Aboriginal people. These suggestions included provision of resources for people with lower literacy levels; increased collaboration between pharmacists and AHWs (Fig 1; such as training of AHW by pharmacists about QUM) and cultural safety training for pharmacists and pharmacy staff5.

Figure 1: Aboriginal health workers' suggestions for improvement from previous study5. AHW, Aboriginal health workers; CMI, consumer medicines information.
Pharmacists, as readily accessible health professionals, play an important role in the healthcare treatment of all Australians. The role of the pharmacist has expanded in recent years to include not only dispensing medications, but also providing health and medicines information, health promotion, medication management reviews (MMR) and disease state management16-19. This research project aimed to ascertain the readiness and willingness of community pharmacists in NSW to take on a greater role in relation to Indigenous health, by exploring their knowledge and opinions about Indigenous health, their current interaction with Indigenous people, and their views as to feasible and achievable ways to help. Pharmacists' views were compared with those of the AHWs elicited in the previous study and any differences in perceptions noted. In addition, pharmacists were asked about their opinion on the proposed extension of the S100 scheme.
Methods
Before its commencement, the project was granted approval from the Human Research Ethics Committee of the University of Sydney, NSW. As there were little existing data in this area, the study design was exploratory and semi-structured, face-to-face, in-depth interviews were carried out. A qualitative research method was used and the concepts explored in the interviews included pharmacists' current knowledge of Indigenous health, their views on the feasibility of proposed new programs and services from the previous study by Hamrosi et al5, and any other ideas they suggested that may improve Indigenous health in the future (Fig 2).

Figure 2: Topic areas for semi-structured questioning. AHW, Aboriginal health workers; CMI, consumer medicines information; QUM, quality use of medicines.
The sampling frame for the study was pharmacists currently employed in community pharmacies in NSW in areas with a significant Indigenous population. To identify these areas the National Aboriginal Community Controlled Health Organisation's (NACCHO) website was used to locate all towns and suburbs in NSW with an Indigenous service, such as AMS or Land Council. A mix of urban, rural and remote locations was sought, though distribution was limited by available time and distance. These towns and suburbs were then assessed for feasibility in travel distance and time, with the most convenient areas being chosen. They included sites in south-east, south-west, central and western NSW. The Guild pharmacy locator was used to identify all pharmacies in these areas. The sample size was determined during the process, when answers reached saturation and no new material was being discovered. The pharmacists were sent a letter outlining the study and inviting them to participate. They were then telephoned one week later to assess their willingness to participate and to arrange a suitable time to meet. The participants were given an information sheet explaining the study objectives and a consent form before commencing.
The interviews were carried out using a semi-structured questionnaire which included questions that were both broad themed and open ended, and some specific yes/no questions to address the study objectives. Interviews were between 15 min and 1 hour in duration, depending on the responses of the pharmacists. The interviews were audio recorded with consent from the pharmacists and were transcribed verbatim, then validated by the interviewer against the original recording. Preliminary data analysis was carried out after each interview with a view to recognizing and exploring any new themes for remaining interviews. The transcripts were thematically content analysed and coded into categories using NVivo (QSR International, Melbourne, VIC, Australia). Sub-themes were not specified in advance, but were obtained from the interviews.
Results
Demographic characteristics
Fifty-one community pharmacists from across NSW were invited to participate in the study. Of these, 27 agreed to participate, and 24 were either deemed unsuitable, due to their lack of Indigenous customers, or declined due to time constraints or dislike of being audiotaped. Demographic information from the participating pharmacists was collected (Table 1) and the distribution of pharmacies participating is displayed (Fig 3). All but one of the pharmacists were working in rural (n = 24) or remote ((n = 2) NSW.
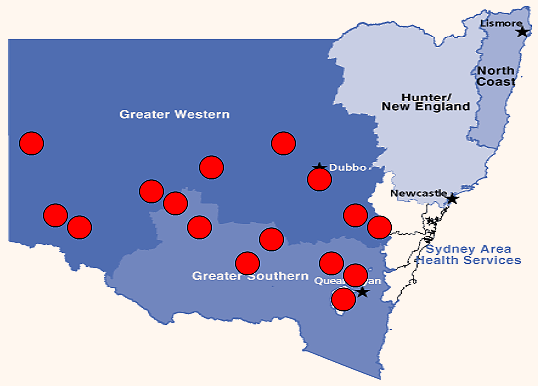
Figure 3: Distribution of the pharmacies where interviews were conducted.
Table 1: Demographic information of pharmacists and pharmacies involved in study.


Figure 4: Pharmacists' suggestions for further ways to improve quality use of medicines in the Indigenous population. AMS, Aboriginal medical service; AHW; Aboriginal health worker; HCP, health care professional.
Main health concerns
Pharmacists were asked to identify the main health concerns of their Indigenous customers. Those mentioned included diabetes and cardiovascular disease, such as hypercholesterolemia and hypertension. Pharmacists related these to poor nutrition, non-compliance with treatments and a lack of interest regarding their health. Many pharmacists identified their Indigenous customers as suffering from chronic illnesses at a much higher prevalence, and with the onset at a younger age than their non-Indigenous counterparts.
...their culture is to live clean with all the natural food. When they're integrated into our society with our fatty food and sugary foods, their bodies just can't tolerate it as well, so they're more prone to diabetes and high cholesterol and things like that... diabetes definitely. Every Indigenous customer I've got here is diabetic. (P23)
Asthma, eye problems, skin problems, mental health conditions, kidney disease and substance abuse were also mentioned, along with problems accessing healthcare providers.
Issues with prescribed medicines
The majority of pharmacists felt that compliance was a major problem with their Indigenous customers. Some identified Webster packing as a means to improving compliance, but noted this was not always an easy fix.
Its got to be compliance, yes ...I've got tablets here now, they take one or two out and say they'll come back with the money, so you give them some to go on with, but they never turn up to get the others. They're very poor tablet takers. (P13)
... with the people that are on the Webster packs, I think that there needs to be a bit of explanation there because sometimes they come back and they've punched out just a few days and that's it. The rest of it's still in there. (P21)
It is important to note that not all pharmacists identified compliance as a problem, and a minority stated that many of their Indigenous customers took their medication without difficulty.
A lot of our patients come back regularly and they're quite happy taking their medications on their own. Even some of them have been offered a pack but they're quite happy and compliant, yeah. (P25)
When asked about their views on the possible causes of non-compliance, the majority of pharmacists indicated that lack of money as the main problem. They felt this often resulted from poor money management and/or the low priority given to medication and health expense. A small number of pharmacists were holding debts for Indigenous customers that were yet to be settled.
I had a gentleman in today whose child needed three things on the script. He couldn't afford them so he just got the antibiotics. (P1)
They might have three or four prescriptions to take, but may only take two because of cost. I have given credit in the past, but I won't anymore because they don't come back and pay. (P27)
Difficulty with communication was also thought to contribute to poor compliance. Reasons included a general lack of understanding of the need to take medications but also the negative perception held by some Aboriginal people towards healthcare providers.
Some of them have trouble with their regimen of taking them on a regular basis, perhaps don't understand the requirements and necessity to take them regularly. Even ones with Webster packs, they occasionally have, well some people have enormous trouble comprehending how to take them. (P15)
It would appear to me that the more incidents we have in our shop with communication and attitude type problems are from Aboriginal people than they are from non-Aboriginal people. (P2)
However, some pharmacists had no problem in communicating with their Aboriginal clients and many felt that this problem was seen more in other ethnic groups served by their pharmacy.
A number of pharmacists felt that literacy was a barrier to medication compliance, with some suspecting that a proportion of their Indigenous customers may be lacking the level of literacy required to read directions on a label. Transport was also identified as a causing a barrier to compliance with treatment, but only by several pharmacists.
Issues surrounding Indigenous customers shopping in pharmacies
The majority of pharmacists interviewed felt that Indigenous people were comfortable shopping in the pharmacy and that they were given the same treatment as non-Indigenous patients. Staff were courteous and polite and had no attitude problems and so, in their opinion, the Indigenous community felt the same way as the non-Indigenous community with regard to the pharmacy.
They might feel they might be judged by other customers, but in terms of service personnel there shouldn't be any. In here the girls here are particularly nice. They don't have any sort of attitude. (P10)
Despite this view, most of the pharmacists interviewed could think of possible barriers to Indigenous people shopping in pharmacies. These included: Indigenous customers feeling uncomfortable when pharmacy staff kept a close watch on them, often the result of previous theft; anger with 'the system' and resentment towards non-Indigenous people; and failure to understand of the importance of carrying Medicare and concession details when accessing prescribed medication.
... theft is an issue. They all tend to get followed around a little bit more. (P16)
Where we do have problems with them is it's very hard to get them to carry concession cards, Medicare cards, and they can be almost aggressive when they are asked to produce them, you know. (P8)
A small proportion of pharmacists felt that Indigenous people may not be aware of what services pharmacists and pharmacies provide, hence making them less likely to come in. Some felt that Indigenous customers were less health conscious or may have an issue with privacy and confidentiality. This could be in relation to the pharmacist or concern about other customers listening. The lack of Indigenous pharmacists and pharmacy assistants was also identified by a minority of respondents as a possible issue.
Role and interaction with Aboriginal health workers
Although the majority of pharmacists interviewed were aware that AHWs were in place in the community, their perceptions of the role of an AHW varied greatly. This may simply reflect the wide range of roles that AHWs actually perform in the health system. More than half of the pharmacists interviewed had never had any contact with the AHWs in their area and had never been approached by them. However, many pharmacists expressed a willingness to collaborate with these workers.
Of the small number of pharmacists who had regular contact with AHWs, the majority worked in pharmacies with an AMS nearby, and found that this made communication and collaboration easier. Interaction generally involved liaising on Webster pack issues, providing information on medication and disease states, discussing compliance issues and reasons for non-compliance, dispensing prescriptions for AMS patients and management relating to the financial issues of patients.
Views on feasibility and possible benefit of programs proposed by Aboriginal health workers
When the suggestions made by the AHWs in our previous study (such as provision of resources for people with lower literacy levels, increased collaboration between pharmacists and AHWs; Fig 1), and cultural awareness training for pharmacists and pharmacy staff5) were put to the pharmacists, the following responses were given.
Most of the pharmacists interviewed felt that the current consumer medicines information (CMI) offered were a problem, but that in many cases this was not an issue confined to the Indigenous population. Many felt that anyone with a lower literacy level would find a CMI hard to read and too long, with the possibility of leaving the patient confused and intimidated.
For some people just to give them five pages is more than they can realistically read and comprehend. It goes beyond, it's not totally an Aboriginal problem anyway. It's wider than that. But yes, I can see that people would find that daunting and don't want to read it. (P6)
However, most of the pharmacists strongly agreed that a shorter, more easy to read CMI would be of benefit not only to their Aboriginal customers, but also their other customers, including those from non-English speaking backgrounds for whom similar barriers to medicines information access may exist. A minority of pharmacists disagreed, and felt that these were not needed because the current CMI could be made more appropriate to these customers by simply highlighting the relevant facts.
Pharmacists were then asked to identify any possible barriers to implementation of an easier CMI. Concerns about the process of identifying people appropriate for the shorter CMI emerged because pharmacists did not want to seem as though they were labeling certain people unable to read or understand. People admitting they have trouble reading or feeling embarrassed to ask for the shorter CMI, and identifying Aboriginal people as needing an 'easier' CMI were also identified as issues.
The only problem is people admitting that they can't read. I think that's the big thing because like I said, it's something people find really embarrassing and just wouldn't tell you straight off the bat, sort of thing. (P26)
The suggestion of an Aboriginal-specific CMI was met with conflicting opinions. While the majority of pharmacists felt that it was feasible and may be of benefit to their Indigenous customers, others believed it would not be necessary, or would further segregate and 'label' the Aboriginal population.
Increased Collaboration between Aboriginal health workers and pharmacists
The majority of pharmacists interviewed indicated that they would be willing to host an AHW in the pharmacy for the purpose of health promotion, and felt that it may be of benefit to their Indigenous community. Many of the pharmacists who did not wish to participate in a service such as this felt that it would be of more benefit in a pharmacy with a larger Aboriginal clientele.
Pharmacists were asked to identify any facilitators that may increase participation, or improve outcomes if such a program were to take place. Availability of sufficient advertising was felt to be important because pharmacists were concerned with lack of attendance from the Indigenous community if they were not informed.
You'd have to advertise that there was an Aboriginal liaison officer here to discuss their medicines issues. Otherwise they could stand here for 4 hours, 5 hours and not see an Aboriginal patient. (P24)
Pharmacists felt that to facilitate such a session, an AHW would be needed who was comfortable with the local Indigenous community, had sufficient health and medicines knowledge, and was available on a set day. Pharmacists also suggested setting up a table in the corner of the pharmacy for the AHW, having appointments with the AHW, and having the session coordinated with the local clinic day. To attract Indigenous customers to the program a minority of pharmacists suggested providing an extra incentive, such as a morning tea, or displaying artwork by local Indigenous children for the local Indigenous adults to view or judge.
Lack of Indigenous customers and possible lack of interest from local Indigenous community were seen as barriers to such a service. In addition, pharmacists suggested that Aboriginal people may feel self-conscious in presenting themselves, or may not like to be treated differently from the general population.
I don't think the community, the Aboriginal community here in town would support such a thing because they don't like to see themselves any different to the rest of the community. They don't like to be treated differently and the Aboriginal community here is sort of fairly well integrated in the town. (P2)
A minority of pharmacists were also concerned as to whether the service would be received well by the non-Indigenous community.
It's hard to say because from the viewpoint of the white community, if that's how you want to put it, Aboriginal people seem to be given heaps of stuff and there are people, very needy people in the white community also, and that's something I think needs to be taken into consideration. I just think it should be on a needs basis, not on a whether you're Aboriginal, or whether you're not Aboriginal. And, I don't know, it would very largely depend on whether it could create antagonism. But there's discrimination both ways, and that's the reality. I mean you live in a community like this, it's just, when there's need in both areas... sometimes it seems very unfair. (P25)
The time to organize such an event, available space in the pharmacy, and disruption to general patronage were identified as potential barriers.
Medicines Education - Support by pharmacists for AHWs
Nearly all respondents felt that pharmacists had a role in AHW education on medicines issues and were willing to participate in seminars with their local AHWs.
... we're more accessible than the doctors and it's a relationship built up and in rural areas. Doctor numbers are declining or if they are remaining stable, the population is stripping what you do need. (P14)
We definitely have a role there... but we definitely don't have enough pharmacists to do it. (P18)
Coordination, the availability of support material, involving other healthcare professionals, such as GPs or diabetes educators, and the provision of funding, or a locum provided were identified as factors that may increase participation in these seminars. There was no consensus on the most appropriate time to schedule the seminars, because some pharmacists preferred daytime, while others preferred evening times.
When asked about barriers to such a service, nearly half the pharmacists complained of a lack of available time to participate in such extra curricular activities. Many pharmacists expressed a feeling of being over-worked and had difficulty finding other pharmacists to relieve them for planned time off. A smaller, yet substantial number of pharmacists were concerned with public speaking, and felt they would be more comfortable educating on a one-to-one basis.
Possible further ways to improve quality use of medicines among the Indigenous population
Many pharmacists were currently running health and medicines awareness programs in their pharmacies, such as smoking cessation, weight loss and diabetes education. None of the respondents had been involved in, or currently ran, any health and medicines awareness programs tailored to the Indigenous community. When asked about possible ways pharmacists could benefit the health of Indigenous people and improve QUM in the Indigenous population, many pharmacists offered suggestions (Fig 4). Financial assistance and further subsidies emerged as a major theme, with many pharmacists believing that if medicines and/or Webster packing was subsidised their Indigenous customers would have the opportunity to be more compliant with their therapy.
I think it would increase compliance if it was free. And from my experience they manage their money very poorly, so if there was some way of funding their medication I would be all for it. I feel that it's cheaper to pay for medication than to pay for a hospital visit. The Webster patients I've had who have dropped off, have done so because of cost. I had a lady who we started on the Webster pack in January and she had problems paying so she dropped off in February. I've only recently seen her and she was in a really bad way. She's gained weight, her blood pressure is through the roof and she told me that she was very sorry to have stopped the Webster pack because it really worked for her. (P25)
Many suggested ways in which medicines information and counseling could be made more readily available to Indigenous patients, such as education programs in the pharmacy and at the AMS, a newsletter with medicines and health information tailored to Indigenous people, dosage cards for medications to put on the fridge, summary medication charts, MMR and having the AHW available to help counsel or reinforce what the pharmacist has explained. A number of pharmacists were keen on inter-professional collaboration and education and felt that that would have multiple benefits.
I think that idea of the Aboriginal health workers liaising with us is by far the best idea. I mean if we could develop a relationship, once I had a suspicion that someone wasn't using their preventer say, I could then contact the health worker and they could follow it up. (P8)
Cultural safety programs for pharmacists and staff: The concept of cultural safety and cultural awareness training was explained to pharmacists and they were asked if they thought it would be worth undertaking for their pharmacy. Most of the respondents agreed that such a program would be of benefit to themselves and pharmacy staff, and indicated they would endeavor to participate if it were offered to them.
I think it would be a good idea, for us to understand. If we've got a better understanding of them, we'll know how to better communicate with them. (P1)
A minority of pharmacists felt that this was not necessary, due to lack of Indigenous customers, or lack of perceived cultural barriers with their Indigenous customers.
When asked about facilitators to increase participation in cultural safety training, the main suggestion was to have the sessions at night time, over one or a period of weeks with a meal or refreshments provided. In addition, pharmacists suggested that the training should be easy to understand and run by the AHWs. The provision of training via workbooks, the internet or DVD, were identified as possible solutions to time and distance issues. When asked about barriers to cultural safety training, lack of time, staff not wanting to attend and a low percentage of Indigenous customers were mentioned. A small proportion of pharmacists were concerned with the cost of a locum to cover them if the training were held during the day.
It's a commitment outside of work that people have to do. If you have it at night time then you are expecting the people who work full time to come in at night time, then you've got students who are the majority of my casual staff who've got other commitments plus they have to study and school and all the other stuff. (P19)
Views on proposed changes to S100 supply to Aboriginal patients
Approximately half of the pharmacists interviewed had previously heard about S100 supply to remote Aboriginal communities, and one pharmacist was currently working in a pharmacy that participated in the program. Pharmacists who were unaware were given an outline of the program, and the proposed extension of S100 was explained to all pharmacists, who were then asked to give their views. This question uncovered extreme differences of opinion between the pharmacists. The majority of pharmacists could see the possible benefits of the program, such as increased compliance, less hospitalisations, improved health outcomes and more consistency in health services, but many felt this type of program would cause increased segregation and thought it was unnecessary in areas where pharmacies were readily accessible to the population.
Yes. I believe it would improve health outcomes in this community, yes I do. (P18)
The main concern raised by respondents was the quality of information given and level of checking that would be carried out by the AHW. Pharmacists had different opinions on the level of training AHWs would need to carry out this task and the possible benefit of increased compliance versus possible risk of missing a serious interaction or an important counseling point.
So the Aboriginal health worker would have to be well qualified with the dispensing of the medicines. I don't know how that works, they'd have to be qualified. I don't know how that would work either, if they're not pharmacists. (P11)
Moreover, pharmacists were unsure about the role they would play if S100 were extended. Their concern was that if their role was reduced this may have a negative impact on QUM, such as possible abuse or overuse of medications. A minority expressed apprehension at the idea of the extension for fear of reduced customer traffic in the pharmacy and, hence, loss of trade.
Because many pharmacists agreed that cost and financial management is the issue behind low compliance and poor health outcomes, the suggestion was raised that medicines should be available to Indigenous patients at no charge in the pharmacy. Many felt this would overcome the main barrier of cost, while still allowing the pharmacist to perform their role in medication management, and preventing the further segregation of Indigenous people.
That is a problem because pharmacists are counsellors... I think that they could just get it for free from the pharmacy... like diabetics with Diabetes Australia. Have a similar thing with the Aboriginals... like if you were a pharmacy that can give medication for free to Aboriginal people you could have a flag sticker on your window that they could recognise. (P27)
A smaller number of pharmacists raised the idea of having subsidised Webster packs supplied by the pharmacy to the AMS, where Aboriginal people could pick them up. This allows the pharmacist to assess the medication regimen, perform the final check and assess what information needs to be relayed to the patient. The pharmacist could then collaborate with the AHWs on a regular basis to discuss medication and compliance issues.
That would be brilliant. That would really work. And I think things like dose changes will be picked up very quickly because the pharmacy liaises with the doctor and I think compliance, the Aboriginal health worker would see straight away. (P25)
Discussion
The majority of pharmacists in this study had a good knowledge of Indigenous health. The issues they cited, for example health concerns and management, compliance, and lifestyle of Indigenous people are all consistent with current literature1,2,7 and the views of the AHWs5.
The current involvement of pharmacists with their Indigenous population varied with the community. This possibly reflects the non-homogenous nature of Indigenous culture.
A small number of pharmacists stated that the concerns of their Indigenous community were no different to the non-Indigenous community in relation to health status and medicines compliance and did not seem to be aware of the major health differentials which exist. Some clearly did not acknowledge the impact that history and politics have had on the health of Indigenous Australians. Instead, their language at times implied blame. However, it is important to note that very few of the pharmacists interviewed had attended any form of cultural awareness training, nor had they been offered it, and this may explain some of the negative stereotypical comments made by some participants. On a positive note, however, the majority of interviewees agreed that having a greater understanding of Indigenous culture would be beneficial, and that they were prepared to undertake any training that would help their Indigenous patients achieve greater compliance with their medications.
There were several limitations to this study. First, it was not possible to conduct interviews in all areas of NSW, and the north-east section was omitted completely owing to time constraints. This may have resulted in a non-representative sample. In addition, the pharmacists invited who did not participate could potentially have raised themes not encountered by this sample. However, the distribution of pharmacies reached provided access to pharmacists with a range of experience with Indigenous patients, as was intended and as can be seen from their comments. A further limitation was that a single data source was used and therefore no triangulation was possible.
The future path of Indigenous people and pharmacy services
There was no clear consensus by pharmacists on the best way to improve access to medicines for Indigenous people. All respondents raised concern with the possible QUM issues if the proposed extension of the S100 scheme goes ahead, because pharmacists play an important role in checking medication suitability and providing counselling20-22. These concerns have previously been identified by the groups proposing the extension as something that has to be addressed if the proposal is acted upon15.
The S100 supply has been described as one of the most significant improvements in health service delivery for many years, and has already shown improvements in health outcomes in areas where it is implemented12. Some pharmacists did agree that this may be the only way to improve compliance in their Indigenous community. Many, though, did not see a need and felt the Indigenous population in non-remote areas would be better served by further subsidisations of medicines and Webster packing, available from the pharmacy. The new proposal has taken this point into account and included the possibility of prescriptions being dispensed in the pharmacy without a co-payment being charged15.
However, even if such subsidisation takes place it may still not completely solve the issue of underutilisation of medicines by Indigenous Australians. One of the most interesting findings in this study was the identification of a major gap in perceptions between pharmacists and AHWs when respondents were asked about Indigenous people's access to pharmacy. While AHWs in the previous study stated that many Indigenous people found pharmacies to be impersonal, confusing and uncomfortable5, pharmacists seemed to be unaware of this, with only one pharmacist out of the 27 identifying it as an issue. This barrier to medicines access was also highlighted in a previous review6, which found that Indigenous people across remote, rural and urban sites experience similar difficulties with accessing medicines.
Conclusion
Clearly if pharmacists wish to deliver optimal services to their Indigenous patients in their own pharmacies they need to be more aware of the barriers Indigenous people experience generally and with respect to medicines in particular. Extra funding provided to subsidise the dispensing of prescriptions may overcome the pharmacists' perceived difficulties in servicing their Indigenous communities, but this will not necessarily lead to improved compliance with medication. What is also needed is a shift in the way services are offered through the pharmacy. This will require pharmacists to meet Indigenous people half way, by being willing to undergo training about Indigenous culture and by learning how to deliver appropriate services in surroundings which help Indigenous people feel culturally safe.
Pharmacists' awareness of and current interactions with AHWs were limited, but all participants could see the potential value of working more closely with these important members of the healthcare team. If the proposed extension of S100 goes ahead and financial barriers are removed, it then remains for pharmacists to take up the challenge of increasing their own understanding of Indigenous health issues and forming collaborative partnerships with their AHW counterparts. Then a real change for the better in mainstream pharmacy services may be achieved.
Acknowledgements
We would like to acknowledge all the pharmacists who gave generously of their precious time to participate in the interviews.
References
1. Australian Bureau of Statistics and Australian Institute of Health and Welfare. National Aboriginal and Torres Strait Islander Health Survey, 2004-05. Canberra, ACT: ABS and AIHW, 2005.
2. Australian Bureau of Statistics and Australian Institute of Health and Welfare. The Health and Welfare of Australia's Aboriginal and Torres Strait Islander Peoples 2005. Canberra, ACT: ABS and AIHW, 2005.
3. Walsh W. Cardiovascular hHealth in Indigenous Australians: a call for action. Medical Journal of Australia 2001; 175: 351-352.
4. National Aboriginal Community Controlled Health Organisations and Oxfam Australia. Close the gap: solutions to the indigenous health crisis facing Australia. Melbourne, VIC: Oxfam Australia, 2007.
5. Hamrosi K, Taylor S, Aslani P. Issues with prescribed medications in Aboriginal communities: Aboriginal health workers' perspectives. Rural and Remote Health 6: 557. (Online) 2006. Available: www.rrh.org.au (Accessed 25 July 2007).
6. Keys Young S Market Research. Keys Young market research into Aboriginal and Torres Strait Islander access to Medicare and The Pharmaceutical Benefits Scheme. Canberra, ACT: Keys Young S Market Research, 1997.
7. Emerson L, Bell K, Croucher K. Quality use of Medicines in Aboriginal Communities Project. Final report. Canberra, ACT: Pharmacy Guild of Australia, 2001.
8. Cousins C. The will to learn, not just teach: challenges and considerations for educators of Aboriginal adults. Australian Journal of Adult Learning 2003; 43: 101-114.
9. Murray R. Prescribing issues for Aboriginal people. Australian Prescriber 2003; 26: 106-109.
10. Couzos S, Murray R. Aboriginal primary health care: an evidence-based approach, 2nd edn. Melbourne, Vic: Oxford University Press, 2005.
11. National Aboriginal Community Controlled Health Organisation. About NACCHO. (Online) 2005. Available: http://www.naccho.org.au/home.htm (Accessed 15May 2006).
12. Kelaher M, Taylor-Thompson D, Harrison N, O'Donoghue L, Dunt D, Barnes T et al. Evaluation of PBS medicine supply arrangements for remote area Aboriginal health services under S100 of the National Health Act. Melbourne, VIC: Co-operative Research Centre for Aboriginal Health and Program Evaluation Unit, University of Melbourne, 2004.
13. HealthInfoNet. Summary of Australian Indigenous health. (Online) 2006. www.healthinfonet.ecu.edu.au/html/html_keyfacts/keyfacts_plain_lang_summary.htm (Accessed 19 June 2007).
14. McInman A. What Aboriginal people think about their access to health care. Sydney, NSW: McInman Research Centre, 2000.
15. *NACCHO, AMA, Pharmacy Guild. Summary of supporting evidence underlying the Position Paper on improving access to PBS medications for Aboriginal peoples and Torres Strait Islanders. (Online) 2004. Available: www.naccho.org/Reports.html (Accessed 25 July 2007).
16. Armour C, Taylor S, Hourihan F, Smith C, Krass I. Pharmacists leading the way in diabetes care - disease state management. Journal of the American Pharmacists Association 2004; 44: 455-466.
17. Krass I, Taylor SJ, McInman A, Armour C. The pharmacists' role in continuity of care in type 2 diabetes: an evaluation of a model. Journal of Pharmacy Technology 2006; 22: 3-8.
18. Saini B, Krass I, Armour C. Development, implementation, and evaluation of a community pharmacy-based asthma care model. Annals of Pharmacotherapy 2004; 38: 1954-1960.
19. Benrimoj SI, Langford JH, Berry G, Collins D, Lauchlan R, Stewart K et al. Clinical intervention rates in community pharmacy: a randomised trial of the effect of education and a professional allowance. International Journal of Pharmacy Practice 2003; 11: 71-80.
20. Whitehead PA, Soo WS, Tenni PC. An investigation of prescription interventions in Perth community pharmacies, Western Australia. Australian Pharmacist 2002; 21: 440-447.
21. Caleo S, Benrimoj S, Collins D, Lauchlan R, Stewart K. Clinical evaluation of community pharmacists' interventions. International Journal of Pharmacy 1996; 4: 221-227.
22. Couzos S. PBS medications - improving access for Aboriginal and Torres Strait Islander peoples. Australian Family Physician 2005; 34: 841-844.

